ABSTRACT
Although previous studies showed that the principal oncoprotein encoded by Epstein-Barr virus, latent membrane protein 1(LMP1), could induce the nasopharyngeal carcinoma cells in G2/M phase increased, little is known about the target molecules and mechanisms. The present study demonstrated that LMP1 could induce the accumulation of p53 protein and upregulate its transactivity in a dose dependent manner, which resulted in the decrease of the kinase activity of cdc2/cyclin B complex and inducing arrest at G2/M phase through the activation of NF-κB and AP-1 signaling pathways, and the effect of NF-κB was more obvious than that of AP-1. This study provided some significant evidence for further elucidating the molecular mechanisms that LMP1 had effects on the surveillance mechanism of cell cycle and promoting the survival of transformed cells and tumorigenesis.
Similar content being viewed by others
INTRODUCTION
Epstein-Barr virus (EBV) is a human gamma herpesvirus that is closely associated with several B-cell and epithelial cell malignancies, including the genesis of Burkitt's lymphoma, AIDS-associated lymphomas, and undifferentiated nasopharyngeal carcinoma (NPC)1. Among the products expressed by EBV during latent infection, Epstein-Barr virus encoded latent membrane protein 1(EBV-LMP1) is regarded as the principal oncoprotein of EBV2, 3. It has been reported that LMP1 participated in many basic life activities of the cell, such as proliferation, differentiation, transformation and apoptosis, through the activation of many distinct signal transduction pathways including the transcription factors NF-κB, AP-14 and STAT5, 6.
Our previous work has demonstrated that in nasopharyngeal carcinoma cell line, LMP1 could upregulate the transcription of cyclin D1 via NF-κB signaling pathway7, promoting the transition from G1 to S phase, and leading to the cells' entering S phase prematurely. On the other hand, LMP1 could induce the cells arrested at G2/M checkpoint, and the block of AP-1 transactivity would rescue the G2/M arrest induced by LMP1 partly. However, the target molecules and the signaling pathways that participated in the G2/M arrest induced by LMP1 remained obscure.
Recently, much evidence implicated that p53 could control the entry into mitosis when cells enter G2 phase with damaged DNA8. The main mechanism by which p53 regulates the G2/M transition involves the regulation of the cyclin B dependent kinase cdc2, which is essential for entry into mitosis. The p53 protein could repress the transcription of both the cyclin B and cdc2 genes. Also, several transcriptional targets of p53 can inhibit cdc2, including p219, which inhibits cdc2 directly, 14-3-3 σ, which anchors cdc2 in the cytoplasm where it can not induce mitosis, and Gadd45, which dissociates cdc2 from cyclin B.
The studies of p53 regulation demonstrated that except for post-translational modifications and ubiquitination, the transcription regulation of p53 gene is also a very important mechanism of p53 regulation. The NF-κB and AP-1 binding sites in p53 promoter region are particularly required for efficient transcription of the p53 gene10, 11. In fact, our previous study has shown that LMP1 could cause the accumulation of p53 protein in NPC cells via transcription factor NF-κB12. These triggered our suspect that LMP1 may induce p53-dependent G2/M arrest in NPC cells through the activation of NF-κB and/or AP-1 signaling pathways.
MATERIALS AND METHODS
Cell culture and treatment
MCF-7 (HTB-22; American Type Culture Collection) human mammary gland cell line, which can express wt p53 protein, was cultured in PRMI 1640-medium (Gibco Biocult, Paisley, UK), supplemented with 10% fetal calf serum (Sino-American Biotechnology Company, Luoyang, China). The Tet-on-LMP1-HNE2 is a dual-stable LMP1 integrated NPC cell line and the expression of LMP1 in which could be regulated by Tet system13. It was cultured in RPMI 1640 medium with 100 μg/ml G418 and 50 μg/ml hygromycin, supplemented with 10% fetal calf serum. Using the HNE2-LMP1 NPC cell line which can express LMP1 stably14, we established one stable cell line that expressed the dominant negative mutant of IκBα(DNM IκBα) and the transcriptional activity of NF-κB, which was inhibited efficiently, and named HNE2-LMP1-DNM I κBα. This was cultured in RPMI 1640 medium with 100 μg/ml G418 and 2 μg/ml pyromycin, supplemented with 10% fetal calf serum. Furthermore, the HNE2-LMP1-TAM67 nasopharyngeal carcinoma cell line, which can express the dominant negative mutant of c-Jun (TAM67) stabely and the transcriptional activity of AP-1, which was suppressed efficiently, was established. All cell lines grew at 37°C under 5% CO2, and 95% air at 99% humidity.
Plasmid
The dominant negative mutant of c-Jun, TAM67, deleted the nucleotides that encoded amino acids 3-122 of c-Jun. The mutant protein encoded by TAM67 thus retained the DNA-binding and leucine zipper domains of c-Jun, but lacked most of the amino-terminal end of the Jun protein, which contains the transactivation domain. This mutant c-Jun protein can dimerize and bind DNA, but failed to activate the transcription of an AP-1-responsive gene15. The human K14 promoter driven mutant c-Jun (TAM67) vector, which was constructed by inserting the TAM 67 sequence into the vector pGem3z, and the AP-1 luciferase reporter plasmid16, in which a sequence of the collagnease promoter region (−73 to +67 bp) containing one AP-1 binding site was inserted into a luciferase reporter vector pGL2- basic, were all kindly provided by Dr Li JJ (National Medical Center and Beckman Research Institute, USA). pRevTRE vector with a hygromycin resistance gene was obtained from Clontech Company (Cat No. 6137-1). The p53-pGL3 luciferase reporter plasmid, which contained the firefly luciferase gene under the control of p53-responsive elements17, was a generous gift of Prof. Yuan ZM (Department of Cancer Cell Biology, Harvard University School of Public Health, USA).
Cell transfection and establishment of stable clones
Transfections were performed using SuperFect\bigcircR Transfection Reagent (QIAGEN) method. Before transfection, cells (2 × 106 per well) were seeded in 6-well plates overnight. Plasmid DNA (2.0 μg) and SuperFect Transfection Reagent (10 μl), each were diluted in serum-free medium (100 μl). DNA and SuperFect¥bigcircR Transfection Reagent were then mixed and incubated for 15 min at room temperature to form transfection-complex. Cells were rinsed twice with PBS. Add 600 μl cell growth medium (containing serum and antibodies) to the transfection complexes. Mix and immediately transfer the whole volume to the cells. After 3 h of incubation at 37°C in CO2 incubator, the DNA-containing medium was replaced by fresh medium containing 10% serum.
To establishment of stable clones, the TAM67 and pRevTRE plasmids were co-transfected into HNE2-LMP1 cell lines as described above. Two days after the transfection, the transfected cells were distributed in 96-well plates and 50 μg/ml Hygromycin B (Calbiochem, San Diego, CA) was added to select stably transfected clones. After selection with Hygromycin for 3 weeks, individual clones were expanded to mass cultures and subsequently assayed for the transactivity of AP-1 using luciferase activity assay. The clone, which can express TAM67 plasmid stably and effectively suppress the transactivation induced by AP-1, was denominated HNE2-LMP1-TAM67 and maintained in culture medium supplemented with 50 μg/ml Hygromycin B.
Luciferase activity assay
Cells were co-transfected by the SuperFect Transfection Reagent (QIAGEN) method using luciferase reporter DNA and b-galactosidase reporter plasmids. The cells were lysed in Reporter Lysis Buffer (Promega, Madison, WI) 24 h after the transfection. We mixed 20 μl of cell lysate with 100 μl Luciferase Assay Reagent and the luciferase activity was measured by a luminometer (BIOSCAN LUMI-SCINT v3.2a). An aliquot of the same cell lysate of each cell line was used to measure β-galactosidase activity as an indicator of the transfection efficiency.
Cell lysate preparation
Cells were harvested and washed twice in cold phosphate-buffered saline (PBS), and then scraped into cell lysis buffer containing 50 mM Tris, pH 7.5, 1 mM EDTA, 25% SDS, 5 mM dithiothreitol, and 10 mM PMSF. The cells were incubated in lysis buffer for 30 min on ice and centrifuged at 15,000 g for 15 min. The supernatant was designed as the cell lysate.
Western blotting
Protein samples from the various cell preparations were subjected to 10% SDS-polyacrylamide gel electrophoresis and transferred onto nitrocellulose membrane. The membrane was then soaked in a blocking solution containing 5% (w/v) non-fat dry milk in phosphate-buffered saline containing 0.05% Tween 20 (PBST) for 1 h at room temperature. To assess p53 levels, the soaked membrane was then incubated with p53 monoclonal antibody (DO-1, catalog no. SC-126; Santa Cruz Biotechnology, Santa Cruz, CA) for 8 h at room temperature and then washed with PBST 3 times for 15 min each and incubated in horseradish peroxidase-conjugated goat anti-mouse IgG antibody at room temperature for 1 h. The membrane was washed 3 times with PBST buffer for 15 min each. Immunobands were detected by the enhanced chemiluminescence reaction (ECL PlusTM System, PIERCE, USK). Equal loading was assessed by protein concentration determinations using BCA Protein Assay Reagent Kit (PIERCE, USA) and by Ponceau S staining of the membrane. Quantification of immunoband intensities was determined by densitometic scanning using ImageMasterTM software (Pharmacia Biotechnology, USA).
cdc2 kinase assay
The cdc2 kinase activity was detected with MESACUP cdc2 Kinase Assay Kit (MBL, LTD. Japan, Code No.5230). We suspended 2 × 107cells in cold sample buffer (50 mM Tris, pH 7.5, 0.5 M NaCl, 5 mM EDTA, 2 mM EGTA, 0.01 % Brij35, 1 mM PMSF, 0.05 mg/ml leupeptin, 50 mM 2-mercaptoethanol, 25 mM beta-glycerophosphate, and 1 mM Na-orthovanadate). After sonicated, cell extract was separated by centrifugation. We incubated 20 μl of HCK-gel suspension (MBL, Code No. 5236) with 300 μl of cell extract on ice for 1 h, followed by centrifugation and the pellets obtained were used as the enzyme source. Add reaction reagents into the HCK-gel pellets in the following order: 10 × cdc2 Reaction Buffer, Biotinylated MV Peptide, distilled water, and ATP. Sample Buffer was used to substitute for HCK-gel pellet as the negative control. Mix well the contents and incubate at 30°C for 30 min. Terminate the phosphorylation reaction and then detect the cdc2 kinase activity with ELISA. Transfer terminal reaction mixture to each microwell strip coated with Monoclonal Antibody (4A4). Incubate the microwell at 25°C for 60 min, and wash with Wash Solution. Then add POD conjugated Streptavidin to each well, incubate the microwell at 25°C for 30 min and wash 5 times. At last, add POD Substrate Solution to each well, incubate the microwell at 25°C for 5 min and add Stop Solution to each well. Read the O.D. of each well at 490 nm with a microplate reader (Bio-Tek Instruments, USA) immediately.
Cell cycle analysis
Cell cycle stage was analyzed by flow cytometry. Aliquots of 1 × 106 cells were harvested by centrifugation, washed in cold PBS, fixed with ice-cold 70% ethanol and treated with 1 μg/ml DNase-free RNase for 30 min. Propidium iodide (PI) was added to a final concentration of 50 μg/ml. The samples were then analyzed on a FACSort (Becton Dickinson, San Jose, CA), and cell cycle analysis was done with CELLQuest (version 3.3) software.
RESULTS
Both the protein and transactivity of p53 were up-regulated after the EBV-LMP1 expression
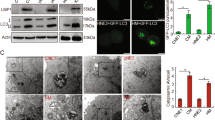
Twenty-four hours after treating the Tet-on-LMP1-HNE2 cells with different doses of doxycycline, the p53 protein levels increased in a dose-dependent manner, as is shown by immunoblotting experiment (Fig 1). When the dose of doxycycline was 0.6 μg/ml, p53 protein level was the highest, reaching about 1.8 times of that in the cells without doxycycline. To further investigate whether EBV-LMP1 could up-regulate the transactivity of p53 at the same time, the p53 luciferase reporter assay was performed. Parallel to the increase of p53 protein, the transactivity of p53 was also up-regulated by EBV-LMP1 in a dose-dependent manner (Fig 2). When the cells were treated with 0.6 μg/ml doxycycline for 24 h, the transactivity of p53 protein was about 1.86 times of that in the cells which was not treated with doxycycline. These indicated that the expression EBV-LMP1 would induce both the accumulation of p53 protein and up-regulation of its transactivity.
LMP1 induced p53 accumulation in a dose-dependent manner. The Tet-on-LMP1-HNE2 cells were harvested and lysed after they were treated with different doses of doxycycline for 24 h. Equal amounts of proteins were separated by 10% SDS-PAGE and blotted onto nitrocellulose membrane. The p53 protein was detected by Western blot using the specific antibody DO-1. Quantification of immunoband intensities was determined by densitometry scanning using ImageMasterTM software, and the amount of p53 protein obtained from the Tet-on-LMP1-HNE2 cells growing in the absence of doxycycline was normalized to one. MCF-7 cells, which can express wild type p53 protein, served as the positive control.
The p53-luciferase reporter plasmid activity was increased in a dose-dependent manner when the expression of EBV-LMP1 was induced by different doses of doxycycline. The Tet-on-LMP1-HNE2 cells were cotransfected with p53-luciferase reporter plasmid and β-galactosidase reporter vector as an internal control. At 24 h after treating the cells with different doses of doxycycline, cellular extracts were prepared and assayed for luciferase and β-galactosidase activities as described in the Materials and Methods section. Fold activation was determined by dividing the luciferase activity of each sample by the basal luciferase activity in the absence of doxycycline. Bars, means of triplicates±SD.
EBV-LMP1 up-regualted p53 via NF-kB and AP-1 signal pathways
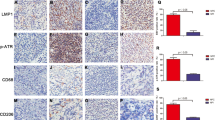
Our previous work has shown that EBV-LMP1 expression could activate the transcriptional activities of NF-κB18 and AP-119 in NPC cell lines. Recently, it was reported that the NF-κB and AP-1 binding sites in p53 gene promoter region were required for efficient transcription of the p53 protein10, 11. It was suspected that LMP1 might induce the accumulation of p53 protein and up-regulate its transactivity via NF-κB and/or AP-1 signal transduction pathways. Using the HNE2-LMP1-DNM IκBα and HNE2-LMP1-TAM67 NPC cell lines, in which the transcriptional activity of NF-κB or AP-1 was efficiently suppressed, it could be explored that whether NF-κB and/or AP-1 participated in the up-regulation of p53 protein induced by LMP1. Comparison the p53 protein levels in the HNE2-LMP1-DNM IκBα cell line and HNE2-LMP1-TAM 67 cell line with that in Tet-on-LMP1-HNE2 cells treated with 0.6 mg/ml doxycycline for 24 h showed that block of the NF-κB or AP-1 signal transduction pathway resulted in the reduction of p53 protein level to 17% and 65%, respectively (Fig 3). With the change of the protein levels, the transactivities of p53 in the HNE2-LMP1-DNM IκBα and HNE2-LMP1-TAM67 cell lines also reduced to 26% and 54% of that in Tet-on-LMP1-HNE2 cells treated with doxycycline, respectively (Fig 4). These data indicated that both the NF-κB and AP-1 signal transduction pathways participated in the up-regulation of p53 induced by EBV-LMP1 and the effect of NF-κB on p53 was more notable than that of AP-1.
Block of the AP-1 or NF-κB signaling pathways resulted in the decrease of p53 protein. Tet-on-LMP1-HNE2 cells were treated with 0 μg/ml or 0.6 μg/ml doxycycline for 24 h. HNE2-LMP1-TAM67 (in which the transactivation induced by intracellular AP-1 was suppressed effectively) and HNE2-LMP1-DNM I κ B α (in which the transactivation induced by intracellular NF-κB was inhibited effectively) cells were then washed and lysated with lysis buffer. Equal amounts of proteins were separated by 10% SDS-PAGE and blotted onto nitrocellulose membrane. The p53 protein was detected by Western blot using the specific antibody DO-1. Quantification of immunoband intensities was determined by densitometry scanning. Relative correction was determined by dividing the intensity of each sample by the amount of p53 protein obtained from Tet-on-LMP1-HNE2 cells growing in 0.6 μg/ml doxycycline for 24 h. MCF-7 cells, which can express wild type p53 protein, served as the positive control.
Block of the AP-1 or NF-κB signaling pathways resulted in decrease of the transactivity of p53 protein. Tet-on-LMP1-HNE2, HNE2-LMP1-TAM67 and HNE2-LMP1-DNM IκBα cells were cotransfected with p53-luciferase reporter plasmid and β-galactosidase reporter vector as an internal control. After transfection, the Tet-on-LMP1-HNE2 cells were tread with 0 μg/ml or 0.6 μg/ml doxycycline for 24 h. Cellular extracts were then prepared and assayed for luciferase and β- galactosidase activities as described in the Materials and Methods section. Bars, means of triplicates±SD.
LMP1 induced the p53-dependent G 2 /M arrest
It is clear that p53 could induce G2/M arrest through down-regulating the transcription of both cdc2 and cyclin B directly and inhibiting the kinase activity of cdc2/cyclin B complex indirectly8. After we have discovered that EBV-LMP1 could induce the accumulation of p53 protein and up-regulate its transactivies via NF-κB and AP-1 signal transduction pathways, we would like to further study whether EBV-LMP1 could induce the p53-dependent G2/M arrest in NPC cells through the activation of NF-κB and AP-1.
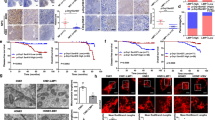
Through detection of the kinase activity of cdc2/cyclin B complex as described in the Materials and Methods section, it was discovered that the O.D. at 490 nm of the Tet-on-LMP1-HNE2 cells without doxycycline treatment was 0.334 while that of the Tet-on-LMP1-HNE2 cells treated with doxycycline reduced to 0.003. Block of the NF-κB or AP-1 signal transduction pathway caused the O.D. at 490 nm to rise to 0.050 and 0.030, respectively, which implied partial recovery of the kinase activity (Fig 5). The results indicated that EBV-LMP1 could induce the down-regulation of the kinase activity of cdc2/cyclin B complex via activation of the NF-κB and AP-1 signal transduction pathways. The effect of NF-κB on cdc2/cyclin B was more apparent than that of AP-1.
Decrease of cdc2 kinase activity induced by EBV-LMP1 and block of NF-κ B or AP-1 signaling pathway results in the increase of cdc2 kinase activity partly. At 24 h after treating the Tet-on-LMP1-HNE2 with 0 μg/ml or 0.6 μg/ml doxycycline, cellular extracts from Tet-on-LMP1-HNE2, HNE2-LMP1-TAM67 and HNE2-LMP1-DNM IkBa cells were prepared and assayed for cdc2 kinase activity as described in Materials and Methods. Bars, means of triplicates±SD.
Further analysis of cell cycle distribution showed that 9.27% of the cells stayed in G2/M phage when the Tet-on-LMP1-HNE2 cells were treated with doxycycline and only 2.04% of the cells in G2/M phage without doxycycline treatment. As shown in the kinase assay experiment, block of the NF-κB or AP-1 signal transduction pathway led to partial rescue of the G2/M arrest induced by EBV-LMP1, the percentages of cells staying in G2/M stage were 4.64% and 6.16%, respectively (Fig 6).
EBV-LMP1 induced the NPC cell arrested at G2/M checkpoint and blocking AP-1 or NF-κB signaling pathway resulted in the rescue of G2/M arrest partly. At 24 h after treating the Tet-on-LMP1-HNE2 with 0 μg/ml or 6 μg/ml doxycycline, Tet-on-LMP1-HNE2, HNE2-LMP1-TAM67 and HNE2-LMP1-DNM IkBa cells were harvested and fixed with ethanol, and stained with propidium iodide, as described in the Materials and Methods section. The data were presented as number of cells (Y-axis) having a certain PI fluorescence (DNA content; X-axis). The percentage of each cell cycle stage was indicated in each panel.
From the above-mentioned experiments, it could be concluded that EBV-LMP1 could induce the accumulation of p53 protein and up-regulate the transactivity of p53, which resulted in the down-regualtion of the kinase activity of cdc2/cyclin B complex and induced NPC cell arrest at G2/M checkpoint, through activation of the NF-κB and AP-1 signal transduction pathways. Furthermore, the effect of NF-κB on p53-dependent G2/M arrest induced by EBV-LMP1 was more obvious than that of AP-1.
DISCUSSION
NPC is one of the most common malignant tumors in Southern China. Genetic factors, and EBV infection as well as environmental factors have been reported to be associated with the etiology of NPC20, 21. However, the molecular mechanism for NPC tumorigenesis remains unclear.
The p53 protein is associated with 50-70% of human tumors22, 23. There are at least 3500 kinds of mutation in the p53 gene24. However, the frequency of p53 gene mutation in NPC is lower than 10 percent25, 26. Previous work has shown that the mRNA27 and protein of p53 were overexpressed in NPC and it has been speculated that the accumulation of p53 protein in NPC cells may be related to the infection of EBV28, 29, 30. Our previous study showed that the oncoprotein LMP1 encoded by EBV could cause the accumulation of p53 protein in NPC cells via transcription factor NF-κB12. In this study, we further confirmed that LMP1 induced the accumulation of p53 protein and up-regulated its transactivity at the same time.
Previous studies have indicated that EBV-LMP1 could activate the cell cycle regulators via NF-κB and AP-1 signaling pathways, resulting in disturbance of cell cycle and promoting proliferation of NPC cells31, 32, 33. To further elucidate the mechanism underlying induction of p53 by LMP1, we established 2 stable cell lines, namely HNE2-LMP1-DNM IkBa and HNE2-LMP1-TAM67, in which the dominant negative mutant of IkBa (DNM IκBα) or c-Jun (TAM67) was expressed permanently by Western blot(data not shown) and the transcriptional activity of NF-κB or AP-1 has been inhibited efficiently. At the same time, we used a dual-stable LMP1 integrated NPC cell line Tet-on-LMP1-HNE2 cells, in which the expression of LMP1 could be tightly regulated by doxycycline in a dose dependent manner13. Since the three kinds of cell line we used are all established from the HNE2-LMP1 nasopharyngeal carcinoma cell line, comparison of the amounts and transactivity of p53 protein, kinase activity of cdc2/cyclin B complex and the distribution of cell cycle stage in the HNE2-LMP1-TAM67 and the HNE2-LMP1-DNM I κ B α cell lines with those in Tet-on-LMP1-HNE2 cells treated with doxycycline, can indicate that EBV-LMP1 could induce the accumulation of p53 and up-regulate its transactivity, which resulted in the down-regulation of the kinase activity of cdc2/cyclin B complex and increased cells in G2/M phase, via the activation of NF-κB and AP-1 signaling pathways. The effect of NF-κB was more obvious than that of AP-1.
Many stimulation signals such as DNA damage, hypoxia, ribonucleotide deletion and activation of oncogene (adenovirus E1A, Ras, c-Myc et al) can activate p5334, 35, 36, 37, followed by cell cycle arrest or apoptosis. The studies of p53 regulation demonstrated that except for post-translational modifications and ubiquitination, the transcriptional regulation of p53 gene was also a very important mechanism of p53 regulation. The NF-κB and AP-1 binding sites in p53 promoter region, which were localized in -163 ∼ -155 bp and -288 ∼ -282 bp upstream from the transcriptional starting site, were required for efficient transcription of the p53 protein10. A recent study also indicated that p53 transactivated its own promoter in a dose-dependent manner while NF-κB had an additive effect on p53 in HCT 116 (human colon carcinoma cells), SK-OV-3 (human ovarian adenocarcinoma cells) and Saos-2 (human osteogenic sarcoma cells), thus resulting in a positive feedback of the p53 expression11.
This implied that the accumulation of p53 protein induced by LMP1 was mostly likely the result from up-regulation of p53 transcription via NF-κB and AP-1, and the effect of NF-κB was more notable. However, it is still possible that NF-κB and AP-1 signaling pathways have effect on the stabilization and activity of p53 by other mechanisms.
G2/M checkpoint is a very important restriction point before mitosis in eukaryotic cell, which is closely associated with the genomic instability, tumorigenesis and treatment of tumor38, 39, 40, 41, 42. G2/M arrest provides an essential period for DNA repair before the segregation of chromosomes, which may decrease the chromosomal aberrations, provent the failure in mitosis and increase the tolerance to DNA damage agents such as some chemotherapeutic compounds and ionizing radiation.
Radiation therapy is the main treatment for NPC. Our previous work has shown that while inducing apoptosis of NPC cells, irradiation activated the activity of NF-κB at the same time which led to the resistance to radiation and block of NF-κB activity through the introduction of the dominant negative mutant of IκBα that can sensitize cells to the radiation. The present study demonstrated that LMP1 induce p53-dependent G2/M arrest via NF-κB and AP-1 signaling pathways, and provided one of the possible mechanisms underlying NPC cells' resistance to ionizing radiation. This will help improve the therapy strategy for NPC, although it need further study to confirm the effectiveness.
The respective block of NF-κB or AP-1 signaling pathway just rescue the G2/M arrest induced by LMP1 partly, which suggested that NF-κB and AP-1 signaling pathways may have synergetically to mediated G2/M arrest induced by LMP1. Further study may provide new clues for better understanding of the distinct mechanism of how EBV-LMP1 participates in the disturbance of cell cycle and tumorigenesis.
References
Kawa, K . Epstein-Barr virus-associated diseases in humans. International Journal of Hematology 2000; 71:108–17.
Fahraeus R, Rymo L, Rhim JS et al. Morphological transformation of human keratinocytes expressing the LMP gene of Epstein-Barr virus. Nature 1990; 345:447–9.
Peng M and Lundgren E . Transient expression of the Epstein-Barr virus LMP1 gene in human primary B cells induces cellular activation and DNA synthesis. Oncogene 1992; 7:1775–82.
Zhang W and Liu HT . MAPK signal pathways in the regulation of cell proliferation in mammalian cells. Cell Research 2002; 12(1):9–18.
He Z, Xin B, Yang X, Chan. C et al. Nuclear factor-kB activation is involved in LMP1-mediated transformation and tumorigenesis of rat-1 fibroblasts. Cancer Research 2000; 60:1845–8.
Hatzivassiliou E and Mosialos G . Cellular signaling pathways engaged by the Epstein-Barr virus transforming protein LMP1. Frontiers in Bioscience 2002; 7:d319–29.
Zhao XR, Wang CX, Luo FJ et al. The Epstein-Barr virus encoded latent membrane protein 1 (EBV-LMP1) activates expression of cyclin D1. Progress in Inorganic Biochemistry And Biophysics 2001; 28:704–9.
Taylor WR and Stark GR . Regulation of the G2/M transition by p53. Oncogene 2001; 20:1803–15.
Chen X, Zhang W, Gao YF et al. Senescence-like changes induced by expression of p21Waf1/Cip1 in NIH3T3 cell line. Cell Research 2002; 12(3):229–33.
Kirch HC, Flaswinkel S, Rumpf H et al. Expression of human p53 requires synergistic activation of transcription from the p53 promoter by AP-1, NF-kappaB and Myc/Max. Oncogene 1999; 18:2728–38.
Benoit V, Hellin AC, Huygen S et al. Additive effect between NF-kappaB subunits and p53 protein for transcriptional activation of human p53 promoter. Oncogene 2000; 19:4787–94.
Liao W, Tang M, Yin L et al. EBV latent membrane protein 1 induces p53 expression via NF-kappa B in nasopharyngeal carcinoma Zhonghua Zhong Liu Za Zhi 2001; 23:199–201.
Liao W, Yi H, Li XY et al. Doxycycline dependent expression of Epstein-Barr virus latent membrane protein 1 with Tet regulating system in nasopharyngeal carcinoma cell line. Acta Biochimica et Biophysica Sinica 1999; 31:309–312.
Wang CX, Li XY, Gu HH et al. Preliminary study on the activation of TRAFs mediated by Epstein-Barr virus encoded LMP1 in nasopharyngeal carcinoma. Virologica Sinica 2001; 16:6–10.
Li JJ, Rhim JS, Schlegel R et al. Expression of dominant negative Jun inhibits elevated AP-1 and NF-κB transactivation and suppresses anchorage independent growth of HPV immortalized human keratinocytes. Oncogene 1998; 16:2711–21.
Li JJ, Westergaard C, Ghosh P et al. Inhibitors of both nuclear factor-kappaB and activator protein-1 activation block the neoplastic transformation response. Cancer Research 1997; 57:3569–76.
Wiederschain D, Gu J and Yuan ZM . Evidence for a distinct inhibitory factor in the regulation of p53 functional activity. Journal of Biological Chemistry 2001; 276:27999–8005.
Yin L, Liao W, Deng X et al. LMP1 activates NF-kappa B via degradation of I kappa B alpha in nasopharyngeal carcinoma cells. Chinese Medical Journal (English) 2001; 114:718–22.
Luo FJ, Hu Z, Deng XY et al. Epstein-Barr virus LMP1 activated AP-1 mediated by JNK in nasopharyngeal cell line. Chinese Journal of Biochemical. Molecular. Biology 2001; 17:381–5.
Hildesheim A and Levine PH . Etiology of nasopharyngeal carcinoma: a review. Epidemiologic Reviews 1993; 15:466–85.
Chen DL, Huang TB . A case-control study of risk factors of nasopharyngeal carcinoma. Cancer Letter 1997; 117:17–22.
Hollstein M, Shomer B, Greenblatt M et al. Somatic point mutations in the p53 gene of human tumors and cell lines: updated compilation. Nucleic Acids Research 1996; 24:141–6.
Wang G, Huang CH, Zhao Y et al. Genetic aberration in primary hepatocellular carcinoma: correlation between p53 gene mutation and loss-of-heterozygosity on chromosome 16q21-q23 and 9p21-p23. Cell Research 2000; 10(4):311–23.
Walker DR, Bond JP, Tarone. RE et al. Evolutionary conservation and somatic mutation hotspot maps of p53: correlation with p53 protein structural and functional features. Oncogene 1999; 18:211–8.
Sun Y, Hegamyer G, Cheng YJ et al. An infrequent point mutation of the p53 gene in human nasopharyngeal carcinoma. Proceedings of the National Academy of Sciences of the United States of America 1992; 89:6516–20.
Lo KW, Mok CH, Huang DP et al. p53 mutation in human nasopharyngeal carcinomas. Anticancer Research 1992; 12:1957–63.
Li H, Han W and Zhang L . cDNA expression array in the differential expression profiles of p53 regulated genes in nasopharyngeal carcinoma and the human normal nasopharynx. Zhonghua Zhong Liu Za Zhi 2001; 23:448–50.
Murono S, Yoshizaki T, Park CS et al. Association of Epstein-Barr virus infection with p53 protein accumulation but not bcl-2 protein in nasopharyngeal carcinoma. Histopathology 1999; 34:432–8.
Leung SY, Chau KY, Yuen ST et al. p53 overexpression is different in Epstein-Barr virus-associated and Epstein-Barr virus-negative carcinoma. Histopathology 1998; 33:311–7.
Gulley ML, Burton MP, Allred DC et al. Epstein-Barr virus infection is associated with p53 accumulation in nasopharyngeal carcinoma. Human Pathology 1998; 29:252–9.
Spender LC, Cannell EJ, Hollyoake M et al. Control of cell cycle entry and apoptosis in B lymphocytes infected by Epstein-Barr virus. Journal of Virology 1999; 73:4678–88.
Miller WE, Mosialos G, Kieff E et al. Epstein-Barr virus LMP1 induction of the epidermal growth factor receptor is mediated through a TRAF signaling pathway distinct from NF-κB activation. Journal of Virology 1997; 71:586–94.
Arvanitakis L, Yaseen N and Sharma S . Latent membrane protein-1 induces cyclin D2 expression, pRb hyperphosphorylation, and loss of TGF-beta 1-mediated growth inhibition in EBV-positive B cells. Journal of Immunology 1995; 155:1047–56.
Levine AJ . p53, the cellular gatekeeper for growth and division. Cell 1997; 88:323–31.
Somasundaram K . Tumor suppressor p53: regulation and function. Frontiers in Bioscience 2000; 5:D424–37.
Lowe SW . Activation of p53 by oncogenes. Endocr. Relat. Cancer 1999; 6:45–8.
Vogelstein B, Lane D and Levine AJ . Surfing the p53 network. Nature 2000; 408:307–10.
Zhou BB and Elledge SJ . The DNA damage response: putting checkpoints in perspective. Nature 2000; 408:433–9.
Khanna KK and Jackson SP . DNA double-strand breaks: signaling, repair and the cancer connection. Nature Genetics 2001; 27:247–54.
O'onnell MJ, Walworth NC and Carr AM . The G2-phase DNA-damage checkpoint. Trends in Cell Biology 2000; 10:296–303.
Hoeijmakers JH . Genome maintenance mechanisms for preventing cancer. Nature 2001; 411:366–74.
Nigg EA . Mitotic kinases as regulators of cell division and its checkpoints. Nature Reviews Molecular cell Biology 2001; 2:21–32.
Acknowledgements
We would like to thank Professor Gong JP and Dr. Sheng ML (Molecular Medical Center, Huazhong University of Science and Technology) for their technological instructions on flow cytometry. We would also thank Professor Yuan ZM (Department of Cancer Cell Biology, Harvard University School of Public Health) and Professor Li JJ (Laboratory of Biochemical Physiology, National Cancer Institute, Frederick, Maryland) for their generous presents of p53 and AP-1 luciferase reporter plasmids. The work was supported by the Special Funds for Major State Basic Research (973) of China (No. G1998051201), the National Natural Science Foundation of China (No. 30100005) and the National Natural Science Foundation of China for Distinguished Young Scholars (No. 39525022).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
DENG, L., YANG, J., ZHAO, X. et al. Cells in G2/M phase increased in human nasopharyngeal carcinoma cell line by EBV-LMP1 through activation of NF-κB and AP-1. Cell Res 13, 187–194 (2003). https://doi.org/10.1038/sj.cr.7290163
Received:
Revised:
Accepted:
Issue Date:
DOI: https://doi.org/10.1038/sj.cr.7290163
Keywords
This article is cited by
-
Precision medicine in nasopharyngeal carcinoma: comprehensive review of past, present, and future prospect
Journal of Translational Medicine (2023)
-
Current approach and novel perspectives in nasopharyngeal carcinoma: the role of targeting proteasome dysregulation as a molecular landmark in nasopharyngeal cancer
Journal of Experimental & Clinical Cancer Research (2021)
-
Mitogen- and stress-activated Kinase 1 mediates Epstein-Barr virus latent membrane protein 1-promoted cell transformation in nasopharyngeal carcinoma through its induction of Fra-1 and c-Jun genes
BMC Cancer (2015)
-
EBV-LMP1-targeted DNAzyme restrains nasopharyngeal carcinoma growth in a mouse C666-1 xenograft model
Medical Oncology (2011)
-
Mechanisms of cell immortalization mediated by EB viral activation of telomerase in nasopharyngeal carcinoma
Cell Research (2006)