Abstract
Objective:
To establish beginning evidence of clinical validity and reliability of the Neonatal Pain, Agitation and Sedation Scale (N-PASS) in neonates with prolonged pain postoperatively and during mechanical ventilation.
Study Design:
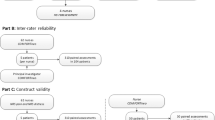
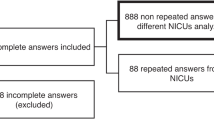
Prospective psychometric evaluation. Two nurses administered the N-PASS simultaneously and independently before and after pharmacologic interventions for pain or sedation. One nurse also administered the premature infant pain profile (PIPP) concurrently with the N-PASS. The setting consisted of 50-bed level III neonatal intensive care unit. Convenience sample of 72 observations of 46 ventilated and/or postoperative infants, 0 to 100 days of age, gestational age 23 to 40 weeks was used. Outcome measures comprised convergent and construct validity, interrater reliability and internal consistency.
Result:
Interrater reliability measured by intraclass coefficients of 0.85 to 0.95 was high (P<0.001 to 0.0001). Convergent validity was demonstrated by correlation with the PIPP scores (Spearman's rank correlation coefficient of 0.83 at high pain scores, 0.61 at low pain scores). Internal consistency, measured by Cronbach's α, was evident with pain scores (0.82), and with sedation scores (0.87). Construct validity was established via the Wilcoxon signed-rank test, comparing the distribution of N-PASS scores before and after pharmacologic intervention showing pain scores of 4.86 (3.38) and 1.81 (1.53) (mean (s.d.), P<0.0001) and sedation scores of 0.85 (1.66) and −2.78 (2.81) (P<0.0001) for pre- and postintervention assessments, respectively.
Conclusions:
This research provides beginning evidence that the N-PASS is a valid and reliable tool for assessing pain/agitation and sedation in ventilated and/or postoperative infants 0 to 100 days of age, and 23 weeks gestation and above.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Anand KJS, Aranda JV, Berde CB, Buckman S, Capparelli EV, Carlo W et al. The Newborn Drug Development Initiative (NDDI) workshop: summary proceedings from the neonatal pain control group. Pediatrics 2006; 117: 9–22.
American Academy of Pediatrics and Canadian Paediatric Society, Batton DG, Barrington KJ, Wallman C . Prevention and management of pain in the neonate: an update. Pediatrics 2006; 118: 2231–2241.
Ng E, Taddio A, Ohlsson A . Intravenous midazolam infusion for sedation of infants in the neonatal intensive care unit. Cochrane Database Syst Rev 2000; CD002052.
Stevens BJ, Pillai RR, Oberlander TE, Gibbins S . Assessment of pain in neonates and infants. In: Anand KJS, Stevens BJ, McGrath PJ (eds). Pain in Neonates and Infants. 3rd edn. Elsevier: Edinburgh, 2007; 67–90.
Curley MA, Harris SK, Fraser KA, Johnson RA, Arnold JH . State behavioral scale: a sedation assessment instrument for infants and young children supported on mechanical ventilation. Pediatr Crit Care Med 2006; 7: 107–114.
American Society of Anesthesiology House of Delegates. Continuum of depth of sedation. http://www.asahq.org/publicationsAndServices/standards/20.pdf. Accessed July 18, 2007.
Stevens B, Johnston C, Petryshen P, Taddio A . Premature infant pain profile: development and initial validation. Clin J Pain 1996; 12: 13–22.
Lawrence J, Alcock D, McGrath P, Kay J, MacMurray SB, Dulberg C . The development of a tool to assess neonatal pain. Neonat Netw 1993; 12: 59–66.
Krechel SW, Bildner J . CRIES: a new neonatal postoperative pain measurement score. Initial testing of validity and reliability. Paediatr Anaesth 1995; 5: 53–61.
Debillon T, Zupan V, Ravault N, Magny JF, Dehan M . Development and initial validation of the EDIN scale, a new tool for assessing prolonged pain in preterm infants. Arch Dis Child Fetal Neonatal Ed 2001; 85: F36–F41.
Duhn LJ, Medves JM . A systematic integrative review of infant pain assessment tools. Adv Neonat Care 2004; 4: 126–140.
Stevens BJ, Johnston CC, Horton L . Factors that influence the behavioral pain responses of premature infants. Pain 1994; 59: 101–109.
Hummel P, van Dijk M . Pain assessment: current status and challenges. Semin Fetal Neonat Med 2006; 11: 237–245.
Ambuel B, Hamlett KW, Marx CM, Blumer JL . Assessing distress in pediatric intensive care environments: the COMFORT scale. J Pediatr Psychol 1992; 17: 95–109.
Reilly PL, Simpson DA, Sprod R, Thomas L . Assessing the conscious level of infants and young children: a paediatric version of the Glasgow Coma Scale. Childs Nerv Syst 1988; 4: 30–33.
Hadjistavropoulos HD, Craig KD, Grunau RV, Johnston CC . Judging pain in newborns: facial and cry determinants. J Pediatr Psychol 1994; 19: 485–491.
Craig KD, Gilbert CA, Lilley CM . Cry as an indicator of pain in infants. In: Barr RG, Hopkins B, Green J (eds). Crying as a Signal, a Sign, and a Symptom. MacKeigh Press: London, 2000; 23–40.
Craig KD, Whitfield MF, Grunau RV, Linton J, Hadjistavropoulos HD . Pain in the preterm neonate: behavioural and physiological indices. Pain 1993; 52: 287–299.
Howard VA, Thurber FW . The interpretation of infant pain: physiological and behavioral indicators used by NICU nurses. J Pediatr Nurs 1998; 13: 164–174.
Gedaly-Duff V, Huff-Slankard J . Sleep as an indicator for pain relief in an infant: a case study. J Pediatr Nurs 1998; 13: 32–40.
Grunau RV, Craig KD . Pain expression in neonates: facial action and cry. Pain 1987; 28: 395–410.
Grunau RE, Holsti L, Whitfield MF, Ling E . Are twitches, startles, and body movements pain indicators in extremely low birth weight infants? Clin J Pain 2000; 16: 37–45.
Holsti L, Grunau RE, Oberlander TF, Whitfield MF, Weinberg J . Body movements: an important additional factor in discriminating pain from stress in preterm infants. Clin J Pain 2005; 21: 491–498.
Pokela ML . Pain relief can reduce hypoxemia in distressed neonates during routine treatment procedures. Pediatrics 1994; 93: 379–383.
Alexander SM, Todres ID . The use of sedation and muscle relaxation in the ventilated infant. Clin Perinatol 1998; 25: 63–78.
Shrout PE, Fleiss JL . Intraclass correlations: uses in assessing rater reliability. Psychol Bull 1979; 86: 420–428.
Johnston CC, Stevens BJ, Yang F, Horton L . Differential response to pain by very premature neonates. Pain 1995; 61: 471–479.
Craig KD, Korol CT, Pillai RR . Challenges of judging pain in vulnerable infants. Clin Perinatol 2002; 29: 445–457.
Johnston CC, Stevens BJ, Franck LS, Jack A, Stremler R, Platt R . Factors explaining lack of response to heel stick in preterm newborns. J Obstet Gynecol Neonatal Nurs 1999; 28: 587–594.
Holsti L, Grunau RE, Oberlander TF, Whitfield MF . Prior pain induces heightened motor responses during clustered care in preterm infants in the NICU. Early Hum Dev 2005; 81: 293–302.
Acknowledgements
We thank the NICU staff nurses, nurse practitioners and physicians in the Ronald McDonald Children's Hospital at Loyola University Medical Center for their cooperation in this research, especially those nurses who collected data. We also thank KJS Anand, MBBS, D.Phil for manuscript review. This research was supported via internal research funds, Loyola University Medical Center.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Hummel, P., Puchalski, M., Creech, S. et al. Clinical reliability and validity of the N-PASS: neonatal pain, agitation and sedation scale with prolonged pain. J Perinatol 28, 55–60 (2008). https://doi.org/10.1038/sj.jp.7211861
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.jp.7211861
Keywords
This article is cited by
-
High-flow nasal cannula (HFNC) vs continuous positive airway pressure (CPAP) vs nasal intermittent positive pressure ventilation as primary respiratory support in infants of ≥ 32 weeks gestational age (GA): study protocol for a three-arm multi-center randomized controlled trial
Trials (2023)
-
Current pain management practices for preterm infants with necrotizing enterocolitis: a European survey
Pediatric Research (2023)
-
COMFORTneo scale: a reliable and valid instrument to measure prolonged pain in neonates?
Journal of Perinatology (2023)
-
RETRACTED ARTICLE: The Neonatal Withdrawal Assessment Tool (NWAT): pilot inter-rater reliability and content validity
Journal of Perinatology (2023)
-
Analgesia and sedation in critically ill pediatric patients: an update from the recent guidelines and point of view
European Journal of Pediatrics (2023)