Abstract
Photodynamic therapy (PDT) has been shown in large studies to be capable of achieving closure of choroidal neovascularization (CNV), thereby resulting in stabilization of visual acuity. We report a series of four patients with classic CNV treated with PDT with good initial result but subsequent severe visual loss that may be related to a change in the morphology of the subretinal scar.
Similar content being viewed by others
Case report
A retrospective review of 52 patients who underwent PDT for a classic CNV over a 1-year period revealed four patients who developed severe visual loss following an initial satisfactory response to PDT. Three of these four patients had age-related macular degeneration (AMD) while in one patient CNV was idiopathic. The greatest linear dimension (GLD) of the CNV at baseline for the entire set of 52 patients ranged from 483 to 6199 μm; the four patients reported here had GLD between 2000 and 3000 μm at baseline. All patients were followed up at 3-monthly interval; LogMAR visual acuity was recorded using the modified ETDRS chart and fluorescein angiography (FA) was performed at every visit. PDT was administered using verteporfin at baseline and repeated, if necessary, as per the TAP protocol.1
Complete closure of the CNVs and initial visual stability was achieved in all four eyes (number of treatments ranged from 1 to 3). However, after a period ranging from 3 to 6 months following closure of the CNV, there was a sharp reduction in visual acuity (VA). The VA dropped by seven lines in patient 1, four lines in patients 2 and 3 and three lines in patient number 4 (mean drop of 20 letters, range 14–34 letters) (Figure 1). All patients were followed up for a period of 1 year; further FAs did not show leakage or residual active CNV in any of the patients and there was no further drop in the visual acuities.
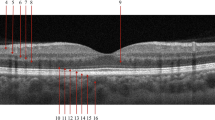
The typical fundus appearance seen in this series of patients is shown in Figures 2 and 3. Figure 2 shows persistently leaking classic CNV (patient 1). Photograph of the same patient taken 3 months later (Figure 3), shows a subretinal haemorrhage in spite of a complete closure of CNV as indicated by the absence of any fluorescein leakage. In all cases, there was late staining of the lesion indicating considerable fibrosis. Figures 2 and 3 illustrate the alteration in morphology of the fibrotic lesion, which we interpret as a contraction of the scar tissue and as a cause of the unexpected drop in visual acuity.
Same patient as in Figure 2. (a) Fundus photograph showing subretinal haemorrhage but (b) no leakage on fluorescein angiogram. Visual acuity had dropped by 7 lines (visual acuity 1.36 logMAR units).
Discussion
It is widely accepted that following PDT, if CNV closure is achieved, visual stability can be assured provided there is no recurrence of the CNV.1, 2 In our series of four patients despite having achieved successful closure of CNV and no evidence of its recurrence, there was a sharp decline in visual acuity that was likely to be related to contraction of the subretinal scar.
Previous histopathological studies of surgically excised membranes after PDT have shown thick fibrovascular membranes with areas of RPE metaplasia3 and collagenous avascular tissue with adherent fragments of Bruch's membrane and glial elements.4 We believe it is possible that contraction of the fibrous elements in the subretinal scar may account for the change in morphology of the subretinal scar in our patients.
A common clinical characteristic shared by the patients in our series was the large size of CNV; exceeding 2000 μm at baseline in all four cases and a fibrotic subretinal scar following PDT. This is similar to an earlier report that suggests CNVs larger than 1500 μm have a higher risk of subretinal fibrosis following PDT for subfoveal CNV in highly myopic eyes.5 As suggested earlier, perhaps large CNVs leak large amounts of cicatricial components from the bloodstream resulting in a greater fibrotic response;5 this subretinal scar tends to contract with time as seen in the four patients reported here and results in a sharp decline in visual acuity.
It is difficult to determine the statistical incidence of this complication from our small series. However, based on our experience, we recommend caution when reassuring patients regarding stabilization of visual acuity even after successful CNV closure by PDT especially in patients with a large lesion, which develop excessive fibrosis that could contract resulting in a severe drop in visual acuity.
References
Treatment of Age-Related Macular Degeneration with Photodynamic Therapy (TAP) Study Group. Photodynamic therapy of subfoveal choroidal neovascularisation in age related macular degeneration with verteporfin. Two-year results of two randomised clinical trials-TAP report. Arch Ophthalmol 2001; 119: 198–207.
Japanese Age-Related Macular Degeration Trial (JAT) Study Group. Japanese age-related macular degeneration trial: 1-year results of photodynamic therapy with verteporfin in Japanese patients with subfoveal choroidal neovascularization secondary to age-related macular degeneration. Am J Ophthalmol 2003; 136: 1049–1061.
Schnurrbusch UE, Welt K, Horn LC, Wiedemann P, Wolf S . Histological findings of surgically excised choroidal neovascular membranes after photodynamic therapy. Br J Ophthalmol 2001; 85(9): 1086–1091.
Stanga P, Hiscott P, Li K, Wong D . Macular relocation after photodynamic therapy for recurrent choroidal neovascular membrane: visual results and histopathological findings. Br J Ophthalmol 2003; 87(8): 975–976.
Ruiz-Moreno JM, Montero JA . Subretinal fibrosis after photodynamic therapy in subfoveal choroidal neovascularisation in highly myopic eyes. Br J Ophthalmol 2003; 87: 856–859.
Acknowledgements
The authors have no financial or other interest in any proprietary product or medication discussed in this article.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Bhatnagar, A., Musadiq, M. & Yang, Y. Late-onset visual decline following successful treatment of subfoveal choroidal neovascularisation with photodynamic therapy. Eye 20, 491–493 (2006). https://doi.org/10.1038/sj.eye.6701907
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.eye.6701907
Keywords
This article is cited by
-
The presentation of data relating to visual acuity
Eye (2007)
-
Reply to Doyle et al
Eye (2007)