Abstract
Erythropoietin receptor (EpoR) has been reported to be overexpressed in tumours and has raised safety concerns regarding the use of erythropoiesis-stimulating agents (ESAs) to treat anaemia in cancer patients. To investigate the potential for EpoR to be overexpressed in tumours, we have evaluated human tumours for amplification of the EPOR locus, levels of EPOR transcripts, and expression of surface EpoR protein. Gene amplification analysis of 1083 solid tumours found that amplification of the EPOR locus was rare with frequencies similar to other non-oncogenes. EPOR transcript levels in tumours and tumour cell lines were low in comparison with bone marrow and were equivalent to, or lower than, levels in normal tissues of tumour origin. Although EpoR mRNA was detected in some tumour lines, no EpoR could be detected on the cell surface using 125I-Epo binding studies. This may be due to the lack of EpoR protein expression or lack of cell-surface-trafficking factors, such as Jak2. Taken together, we have found no evidence that EpoR is overexpressed in tumours or gets to the surface of tumour cells. This suggests that there is no selective advantage for tumours to overexpress EpoR and questions the functional relevance of EpoR gene transcription in tumours.
Similar content being viewed by others
Main
Erythropoiesis-stimulating agents (ESAs), epoetin-α, epoetin-β, and darbepoetin-α, regulate erythropoiesis by binding and activating the erythropoietin receptor (EpoR) on the surface of erythropoietic precursor cells, stimulating their survival, proliferation, and differentiation into mature red blood cells. Recently, off-label investigational clinical trials that aimed to prevent anaemia in breast and head and neck cancer patients undergoing chemotherapy and radiotherapy, respectively, reported a decrease in locoregional progression-free survival and overall survival in ESA-treated patients (Henke et al, 2003; Leyland-Jones et al, 2005). These findings have led to speculation that administration of ESAs to cancer patients may promote tumour growth through stimulating EpoR expressed on tumours. This hypothesis appeared to be supported by the literature, as some investigators have reported that tumour samples and cell lines transcribe the EPOR gene at high levels, that 90–100% of primary human tumours overexpress EpoR protein, and that recombinant human Epo (rHuEpo) induced proliferative, survival and migration effects on tumour cell lines (reviewed by Osterborg et al, 2007; Sinclair et al, 2007). In contrast, most clinical studies have found no increase in tumour progression or decrease in survival when ESAs are administered to cancer patients (Bohlius et al, 2006). Furthermore, many studies have found tumour cell lines are unresponsive to ESAs, including proliferation and survival of tumour cell lines in vitro (Berdel et al, 1991; Mundt et al, 1992; Rosti et al, 1993; Selzer et al, 2000; Westphal et al, 2002), and, of most physiological relevance, tumour growth in vivo (Silver and Piver, 1999; Mittelman et al, 2001; Stuben et al, 2001, 2003; Thews et al, 2001; Golab et al, 2002; Pinel et al, 2004; Sigounas et al, 2004; Ning et al, 2005). Thus, there is conflicting evidence for the role of EpoR in tumour growth.
Concerns have been raised about the lack of specificity of antibodies used by many studies to detect EpoR. Most studies used anti-EpoR peptide polyclonal antibodies (C-20; Santa Cruz Biotechnology, Santa Cruz, CA, USA) in immunoblotting and/or immunohistochemistry (IHC) experiments (Elliott et al, 2006). We and others have found that polyclonal antibodies C-20 detected a 66-kDa protein that was substantially larger than EpoR (59 kDa) and was identified to be heat-shock protein HSP70 (Elliott et al, 2006; Brown et al, 2007; Ragione et al, 2007). Owing to cross-reactivity with non-EpoR proteins (e.g., HSP70), C-20 was found unsuitable for IHC (Elliott et al, 2006; Brown et al, 2007). In addition, other anti-EpoR antibodies have been found to be nonspecific and insensitive and therefore inappropriate for EpoR detection (Della Ragione et al, 2007; Kirkeby et al, 2007; Laugsch et al, 2008; Sturiale et al, 2007).
Since the findings and conclusions from studies that used C-20 and other anti-EpoR antibodies to detect EpoR are inconclusive, we performed an extensive investigation of the potential for EpoR to be overexpressed in tumour cells through antibody-independent approaches.
Materials and methods
Cell lines and patient tissue samples
Human cell lines analysed were UT7/Epo (Epo-dependent megakaryoblastic leukaemia); MCF-7 (breast carcinoma); HeLa (cervical carcinoma); SHSY-5Y (neuroblastoma); CAKI-1, CAKI-2, 769P, A704, A498, SW-156, SK-NEP-1 (renal carcinomas); HT29, LS174T (colon carcinomas); and A549 (lung carcinoma). Tumour samples for representational oligonucleotide microarray analysis (ROMA) and quantitative PCR (Q-PCR) analysis were obtained from Cooperative Human Tissue Network (NCI Cancer Diagnosis Program), Duke University, University of Michigan, Asterand Inc. (Detroit, MI, USA), Cytomyx Inc. (Lexington, MA, USA), Genomics Collaborative (Cambridge, MA, USA), and as previously described (van der Horst et al, 2005). RNAs from paired normal and cancerous colon and lung tissue were from Ardais Corp. (Lexington, MA, USA). Other non-paired tissue mRNAs were obtained from Stratagene (La Jolla, CA, USA), Clontech (Mountainview, CA, USA), Asterand Inc., Ardais Corp., and Genpak Ltd (Brighton, UK).
Genomic amplification
DNA for ROMA, comparative genomic hybridisation (CGH) and Q-PCR was isolated from snap-frozen tumour samples using a proteinase K method. Representational oligonucleotide microarray analysis was performed as previously described (Lucito et al, 2003; van der Horst et al, 2005), and CGH was performed as previously described (Pei et al, 2002). Data were normalised using a modified global loss algorithm (Smyth and Speed, 2003) (data not shown), and amplicon boundaries were determined using the GLAD algorithm (Hupe et al, 2004) and assembled into a database (data on file at Amgen Inc.).
Quantitative PCR analysis of the EPOR locus was performed on DNA from 68 primary breast tumours in multiplex reactions with one of two sets of EPOR-specific primers and probes. Primer/probe set A amplified an EPOR fragment within exon 3 (Figure 1): forward primer, 5′-CTTCGTGCCCCTAGAGTTGC-3′; reverse primer, 5′-TGATGTGGATGACACGGTGAT-3′; and probe, 5′-TCACAGCAGCCTCCGGCGCT-3′. Primer/probe set C amplified an EPOR fragment within exon 8 that encodes the epitope for the M-20 anti-EpoR antibody (Figure 1): forward primer, 5′-TGCCAGCTTTGAGTACACTATCCT-3′; reverse primer, 5′-GCTCAGGGCACAGTGTCCAT-3′; and probe, 5′-CCCAGCTCCCAGCTCTTGCGTC-3′. Probes were labelled with 6-carboxyfluorescein (FAM) at the 5′ end and 6-carboxytetramethylrhodamine (TAMRA) at the 3′ end. A primer/probe set specific for a relatively invariant region of chromosome 6p22.2 (data on file at Amgen Inc.) was included in each multiplex reaction, as a non-amplified control: forward primer, 5′-GGTCTCTATTTGCACTTGGCTGAT-3′; reverse primer, 5′-TTTTCATTGTTGACCAAGCTAGACA-3′; and probe, 5′-TAGGGCATACTGCCTGCATATTTCCTGCT-3′ labelled with VIC at the 5′ end and TAMRA at the 3′ end. PCR products were quantified from standard curves generated with each primer/probe set using normal human genomic DNA (Novagen, Madison, WI, USA). Each 10 μl Q-PCR mixture contained 5 μl 2 × PCR master mix (Eurogentec, San Diego, CA, USA), 150 nM each primer and probe, and 15–20 ng genomic DNA. DNA amplification was performed using the ABI 7900 (Applied Biosystems, Foster City, CA, USA): denaturation at 95°C for 10 min, followed by 40 cycles of 15 s at 95°C and 1 min at 60°C. Reactions were performed in duplicate and repeated. Data were analysed using SDS software (Applied Biosystems). The relative copy number of EPOR using each primer/probe set is the ratio of the copy number at the EPOR locus to the copy number at the control locus; the mean relative copy number is presented.
Genomic organisation of the EPOR locus showing alternatively spliced transcripts and location of primers and probes. Light grey boxes represent coding regions of exons 1–8, open boxes represent untranslated 5′ and 3′ regions, and black boxes represent the transmembrane coding sequences. The three major EPOR transcripts are shown with dashed lines representing normal splicing sites. The hatched boxes represent intronic regions contained in some alternatively spliced forms. Primer/probe sets A, B, C, and D were designed to amplify EPOR fragments within exons 3, 6–7, 8, and 5–8, respectively.
Quantitative RT-PCR
For laser-dissected tumour and stroma RNA, sections were cut and placed directly into extraction buffer from Picopure RNA Isolation kit (sunnythanol (2 min), Accustain (30 s), dH2O (1 min), 75% EtOH, 95% EtOH, 100% Evale; Arcturus/Molecular Devices, Sunnyvale, CA, USA) or onto glass slides, then into a slide box on dry ice. Sections were stained as follows: treated with 75% EtOH ( × 2), dipped in xylene, and then air-dried. Laser dissection was performed on a Pixcell IIe System and RNA was extracted using PicoPure Isolation kit (Arcturus/Molecular Devices), according to the manufacturer's instructions. RNA was quantified using the Beckman DU640 Spectrophotometer at the following wavelengths: 260, 280, and 320 nm.
RNA was isolated from cells and tissues using the Absolutely RNA miniprep kit (Stratagene), treated with DNase I (Roche Biochemical, Indianapolis, In, USA), and cDNA synthesised using SuperScript II (Invitrogen, Carlsbad, CA, USA). Quantitative RT-PCR was performed using three sets of EPOR-specific primers and probes to amplify fragments within exons 3 (primer/probe set A), 6/7 (primer/probe set B), and 8 (primer/probe set C) (Figure 1). EPOR was amplified from exons 3 and 8 using primer/probe sets A and C, and from exon 6/7 using primer/probe set B: forward primer, 5′-ACCGCCGGGCTCTGAA-3′; reverse primer, 5′-TTCAAACTCGCTCTCTGGGC-3′; and probe, 5′-AGAAGATCTGGCCTGGCATCCCG-3′. Human cyclophilin was amplified using forward primer, 5′-TGCTGGACCCATCACAAATG-3′; reverse primer, 5′-TGCCATCCAACCACTCAGTC-3′; and probe, 5′-TTCCCAGTTTTTCATCTGCACTGCCA-3′. Probes were labelled with FAM (5′) and TAMRA (3′). PCR mixtures contained 50 ng cDNA, TaqMan Universal PCR Master Mix (Applied Biosystems), 450 nM primers, and 200 nM probe. An RNA control was included to confirm that samples were not contaminated with genomic DNA. The amplification programme was as follows: denaturation at 95°C for 10 min, followed by 40 cycles of 95°C for 15 s and 60°C for 1 min (ABI PRISM 7700 and PRISM 7900HT Sequence Detection Systems; Applied Biosystems). Levels of EPOR transcripts were normalised to cyclophilin. For brain samples and head and neck laser-dissected samples, cDNA was synthesised using Qiagen's OmniScript Reverse Transcriptase kit (Qiagen, Valencia, CA, USA), using 1 μ M oligo dT (Invitrogen), 0.5 U μl−1 RNase inhibitor (Roche Biochemical), 50 ng RNA, and 500 μ M dNTP in a 20 μl reaction. Equal amount (50 ng) of the DNase-treated RNA was used as a negative RT control, and quantitative RT-PCR was performed using Fast Start SYBR Green PCR Master Mix, according to the manufacturer's instructions (Roche Biochemical), using 0.5 μ M of forward and reverse primers. Lightcycler 1.5 (Roche Biochemical) parameters were as follows: EpoR, 10 min at 95°C, then 45 cycles of 15 s at 95°C, 5 s at 62°C, 20 s at 72°C, 90°C for 2 s with a reading at the end of the 2 s hold time. For human cyclophilin primers, parameters were as follows: 10 min at 95°C and 45 cycles of 15 s at 95°C, 5 s at 67°C, 20 s at 72°C and 2 s at 85°C with a reading at the end of the 2 s hold time. Lightcycler Detection software (versions 4.0) was used to analyse and graph the data. Primer set D (Figure 1) was EpoR 5′-CGTATGGCTGAGCCGAGCTT-3′ (exon 5) and 5′-CAGCCATCATTCTGGTACAGC-3′ (exon 8). Human cyclophilin primers were 5′-AGACGCCACCGCCGAGGAA-3′ (exon 1) and 5′-TGCCAGGACCCGTATGCTTTAGGA-3′ (exon 4).
Expression microarray analysis
Standard cRNA labelling and array processing were conducted according to the Affymetrix manual (Affymetrix, Santa Clara, CA, USA). First-strand synthesis used 5 μg total RNA, 10 pmol T7-(dT)24 primer, and Superscript II (Invitrogen). Double-stranded cRNA was purified using the MinElute Reaction Cleanup kit (Qiagen). Biotinylated cRNA was synthesised using the Bioarray High Yield RNA Transcript Labeling kit (Enzo Diagnostics, Farmingdale, NY, USA) for 6 h at 37°C and purified using the RNeasy Mini kit (Qiagen). The cRNA was hybridised to the Affymetrix Human Genome U133 Plus 2.0 array containing five unique EPOR probe sets: 209962_AT, 209963_S_AT, 215054_AT, 37986_AT, and 396_F_AT, each identifying different subregions within EPOR exon 8. The arrays were washed using the EukGE_WS2v4_450 protocol on a GeneChip Fluidic Station 450 and scanned using the Affymetrix GeneChip Scanner 3000. Raw signal intensities that met the recommended quality criteria were imported into the gene expression analysis system, Rosetta Resolver 5.0 (Rosetta Bio-software, Seattle, WA, USA; http://www.rosettabio.com/tech/default.htm). System processing, including normalisation, consisted of algorithms using an error-modelling approach (Rajagopalan, 2003).
A conventional two-way analysis of variance (ANOVA) was performed to determine if EPOR was differentially expressed in tumour vs normal tissues. Normalised intensity values were log transformed to achieve homoscedacity and used for the ANOVA calculations. An ANOVA calculation was performed for each tissue type with disease state and probe set as the two factors. If a difference was found, a post hoc comparison using the Dunn–Sidak test was performed. Statistical calculations were made using Matlab version 6.5.1 (Mathworks Inc., Natick, MA, USA).
Western blot analysis
Cell lysates and immunoblots were prepared as described previously (Elliott et al, 2006). Membranes were blocked with 5% milk in TBS containing 0.05% Tween-20, and incubated with 1 : 1000 dilution anti-Janus kinase 2 (Jak2) antibody (Cell Signaling Technologies, Danvers, MA, USA) for 2 h at room temperature. The secondary antibody was anti-rabbit IgG conjugated to horseradish peroxidase (Amersham Biosciences, Piscataway, NJ, USA). ECL-Plus (Amersham Biosciences) was used for detection. Blots were stripped and reprobed with 0.25 μg ml−1 anti-cyclophilin B (Abcam, Cambridge, MA, USA) as a loading control.
Epo-binding assays
Recombinant human Epo-binding studies were performed as previously described (Elliott et al, 1997) with some modifications. Cells were grown to confluency, dissociated with Versene (EDTA/EGTA), centrifuged, washed, and resuspended in binding buffer (RPMI, 1% BSA, 0.1% sodium azide, 50 mM HEPES, 10 μg ml−1 cytochalasin B), and 1 × 106 cells in 80 μl were incubated with 133 pM 125I-rHuEpo (specific activity, 2500 Ci mmol−1), with or without a 1500-fold excess (200 nM) unlabelled rHuEpo, for 2.5 h at 37°C. Reactions were quenched with 700 μl ice-cold PBS/0.5% BSA, and then centrifuged at 5000 g. Surface-bound 125I-rHuEpo was determined using a Packard Cobra II Auto Gamma Counter (Perkin-Elmer, Boston, MA, USA) and specific binding calculated as the difference in 125I-rHuEpo binding in the presence and absence of excess rHuEpo. For UT7/Epo Scatchard analysis, varying amounts of cold ligand (10 pg to 5 ng) in 40 μl binding buffer were added to 10 μl 125I-rHuEpo and 50 μl 5 × 105 UT7/Epo cells. Each reaction was performed in duplicate. Reaction tubes were incubated at 37°C for 1.5–2 h. Cell-bound and free 125I-rHuEpo were separated through 100% dibutyl phthalate oil in a fixed angle horizontal rotor at 12 000 g for 2 min at room temperature. The tubes were frozen in dry ice, the oil phase containing cell-bound 125I-rHuEpo was extracted, and the amount of 125I-rHuEpo was determined by scintillation counting. Nonspecific binding was determined by adding a 300-fold excess of cold rHuEpo to the reaction mix. Scatchard analyses were performed using Microsoft Excel.
Results
Genomic amplification of EPOR
Representational oligonucleotide microarray analysis and CGH data from 1083 tumour samples from 15 different tumour types were analysed for amplification of the EPOR locus. Amplification of EPOR in amplicons <10 Mb was identified in less than 0.7% of tumours (n=8) and was similar to the frequency of amplification of other established non-oncogenic loci such as glyceraldehyde-3-phosphate dehydrogenase (GAPDH), β-actin (ACTB), and β-glucuronidase (GUSB) (Figure 2A). None of the tumours with amplified EPOR contained EPOR in amplicons <1 Mb. Oncogenic loci cyclin D1 (CCND1), HER2, and EGFR were amplified in 3.5–6.7% of tumours and frequently contained amplicons <1 Mb (Figure 2A). Copy numbers of oncogenic loci were increased >9-fold in some tumours (Figure 2B). In contrast, the copy number of EPOR was increased to a maximum of 2–3-fold, concordant with other non-oncogenic loci (Figure 2B).
Erythropoietin receptor genomic amplification in tumour samples. Quantitative genomic microarray analysis was performed on 1083 tumours from 15 different tumour types. (A) Per cent of tumours demonstrating genomic amplification of oncogenes cyclin D1 (CCND1), EGFR, and HER2; non-oncogenes β-actin (ACTB), GUSB, and GAPDH; and test locus EPOR. The numbers of tumours with amplicons are shown below the x axis. (B) Per cent of tumours with genomic amplification of genes from panel A present in amplicons <10 Mb plotted against gene copy numbers. (C) Quantitative genomic PCR analysis of the EPOR locus in 68 breast tumour samples. The EPOR-specific primer/probe sets A and C were used to amplify EPOR fragments from exons 3 and 8, respectively. Breast tumour no. 29 had a gain in EPOR copy number (1.6-fold) and no. 50 had a deletion of one EPOR locus (0.4-fold).
To further analyse the frequency of EPOR amplification, Q-PCR was performed on genomic DNA isolated from 68 primary breast tumours. Copy numbers of EPOR were between 0.5 and 1.5 in all tumour samples, except one tumour with a copy gain and one with a copy deletion (Figure 2C). Both EPOR primer sets yielded concordant results. Taken together, these results demonstrated that the EPOR locus was rarely amplified in primary human tumours.
EPOR transcripts in tumours and tumour cell lines
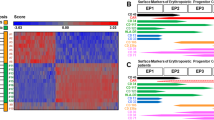
To investigate EPOR overexpression through mechanisms other than genomic amplification, levels of EPOR transcripts in tumours and cell lines were compared with levels in normal tissues of tumour origin. Analysis of 24 normal tissues showed that EPOR was transcribed at high levels in bone marrow, medium levels in adrenal, and low levels in all other tissues (Figure 3A). Comparative analysis of EPOR transcription in tumour vs non-tumour tissues determined that transcript levels in kidney, stomach, colon, and lung tumours and cell lines were lower than those found in corresponding normal tissues (Figure 3B). Levels of EPOR transcripts were also not elevated in brain tumours relative to normal brain (Figure 3C), colon and lung adenocarcinomas relative to patient-matched normal tissue (Figure 3D), and laser-dissected tumour epithelia from head and neck tumours relative to stroma (samples collected from three different regions from each tumour A–C, Figure 3E).
Levels of EPOR transcripts in normal vs tumour tissues. Quantitative RT-PCR was used to determine levels of EPOR transcripts in normal and tumour tissues relative to levels of cyclophilin B transcripts. (A) Levels of EPOR transcripts in a panel of normal tissues obtained using primer/probe set B (corroborated with primer/probe set A). EPOR transcript levels relative to cyclophilin were analysed: (B) normal tissues vs tumour tissues and cell lines; (C) brain tumours and normal brain (not patient-matched samples); (D) patient-matched normal vs colon and lung tumour samples; (E) patient-matched head and neck tumour and stroma (A–C indicate different preparations from the same tumour). Bone marrow samples were included as a positive haematopoietic control in all analyses (clear bars). Results obtained using primer/probe set B (Figure 1) are shown for panels A, B, and D and primer set D for panels C and E.
Levels of EPOR transcripts were further examined in microarray analyses of 121 tumour and 170 normal tissues. For each of the five probe sets for EPOR on the HG-U133 Plus 2.0 array, levels of EPOR transcripts in tumours were not significantly elevated above levels found in the normal tissue counterpart (Figure 4; data not shown). Interestingly, a statistically significant (P<0.05) decrease in levels of EPOR transcripts in kidney tumours, lung squamous cell carcinoma, lymphomas, and prostate adenocarcinoma relative to normal tissues was identified (Figure 4). This result was confirmed with five different probe sets. These data demonstrate that EPOR transcription is not elevated in tumour samples or cell lines compared with EPOR transcript levels in the normal, non-tumour counterpart.
Microarray analysis of levels of EPOR transcripts in normal vs oncogenic samples. Comparative microarray analysis of 121 tumour and 170 normal tissues from breast, colon, kidney, lung, lymph node, ovary, pancreas, prostate, and skin samples. Closed circles represent transcript levels from individual samples using EPOR probe 396_F_AT (EPOR exon 8). Other EPOR probe sets yielded similar intensity profiles. Horizontal, double-headed arrows indicate no statistical difference in EPOR levels between normal and tumour tissues. A single-headed arrow indicates a significant (P<0.05) reduction in levels of EPOR transcripts in tumour tissues compared with normal tissues. No statistical analyses were performed on pancreatic samples because of the lack of a normal control, or on ovary and melanoma samples because of their small sample sizes.
EPOR transcript levels and surface expression in tumour cell lines
Since EPOR transcripts were detected in tumour cells, albeit at low levels, we investigated the association between transcript levels and expression of EpoR at the cell surface. The particular cell lines used in this study were selected because of reports that they responded to Epo. The six cell lines included megakaryoblastic leukaemia line UT7/Epo cells (known to be Epo responsive; Laugsch et al, 2008) as a positive control; a renal carcinoma line 769P (with extremely low levels of EpoR mRNA) (Elliott et al, 2006) as a negative control; and four cell lines in which rHuEpo has been reported to induce an in vitro response: breast carcinoma line MCF-7 (Acs et al, 2001), cervical carcinoma line HeLa (Acs et al, 2003; Pajonk et al, 2004), renal carcinoma line CAKI-2 (Westenfelder and Baranowski, 2000), and neuroblastoma line SHSY-5Y (Um et al, 2007). Relatively high levels of EPOR transcripts were observed in UT7/Epo cells, very low levels in MCF-7, HeLa, SHSY-5Y, and CAKI-2 cells, and negligible levels in 769P cells (Figure 5A). While UT7/Epo cells bound high levels, none of the solid tumour cell lines bound detectable levels above background of 125I-rHuEpo, (Figure 5B). Scatchard analysis demonstrated that UT7/Epo cells expressed ∼11 700 cell-surface receptors per cell with a binding affinity of 68 pM (Figure 5C). In contrast, 32D cells expressing murine EpoR expressed relatively low levels of cell-surface receptors (0.58±0.10% total c.p.m.; ∼760 receptors per cell; data not shown), demonstrating the assay was sensitive. These data indicate that synthesis of EpoR mRNA in solid tumour cell lines does not predict surface expression; EpoR protein may not be synthesised in these solid tumour cell lines and/or may be trapped in the cytoplasm and may not be trafficked to the surface of the cell.
Lack of correlation between levels of EPOR transcripts and EpoR surface expression in tumour cell lines. (A) Quantitative RT-PCR of EPOR in tumour cell lines using primer/probe set C (Figure 1). Similar data were obtained with primer/probe sets A and B (Figure 1; data not shown). (B) Specific binding of 125I-rHuEpo to cell lines (combined data from three to four experiments with n=11–17 per bar). Error bars represent s.e.m. (C) Scatchard analysis of rHuEpo binding to UT7/Epo cells. Each point represents the average of three samples. (D) Western blot analysis of Jak2 expression levels. Cyclophilin B is shown as a loading control for western blot analysis.
Janus kinase 2 is required for surface expression of EpoR in haematopoietic cells (Huang et al, 2001). Variable levels of Jak2 expression were observed in cell lines (Figure 5D), and lack of Jak2 in some may account for, in part, lack of surface EpoR. However, other cell lines (e.g., CAKI-2) expressed Jak2 protein but still no surface expression was observed (Figure 5B). These data suggest that if EpoR protein is synthesised in these cells, it does not get to the surface of tumour cell lines at detectable levels due to potential limiting surface-trafficking factors, such as Jak2.
Discussion
Although ESAs have been used safely for numerous years, results from several recent off-label, investigational clinical trials have raised concerns that ESAs may have direct tumour-stimulating effects and promote tumour progression in anaemic cancer patients (Henke et al, 2003; Leyland-Jones et al, 2005; Bohlius et al, 2006). The notion that EpoR was overexpressed in tumours and that rHuEpo enhanced tumour progression has been confounded by the finding that antibodies used to detect EpoR are nonspecific and additionally bind non-EpoR proteins, including HSP70 (Elliott et al, 2006; Brown et al, 2007; Della Ragione et al, 2007; Kirkeby et al, 2007; Laugsch et al, 2008; Ragione et al, 2007; Sturiale et al, 2007). Therefore, a recent study suggesting high-level EpoR expression in head and neck tumours correlated with tumour progression and worse survival in patients administered ESAs (Henke et al, 2006) most likely identified the well-know association of HSP70 and worse prognosis (Schmitt et al, 2007). Furthermore, there are a large number of studies that find that ESAs do not stimulate tumour progression in preclinical models (reviewed by Osterborg et al, 2007; Sinclair et al, 2007). Since specific anti-EpoR antibodies have yet to be identified, we investigated if EpoR was overexpressed in tumours by performing a systematic analysis of EPOR genomic amplification and transcription in more than 15 different primary tumour types, and EpoR transcript and surface EpoR expression analysis in representative tumour cell lines in which rHuEpo has been reported to induce responses (Westenfelder and Baranowski, 2000; Acs et al, 2001, 2003; Pajonk et al, 2004; Um et al, 2007).
A common phenomenon of tumour formation is the amplification of proto-oncogenes such as HER2 (Parkes et al, 1990), EGFR (Reissmann et al, 1999), CCND1 (Szepetowski et al, 1992; Reissmann et al, 1999), and c-MET (Rege-Cambrin et al, 1992), which provide a selective advantage for tumour cell growth and survival through overexpression. Genomic analysis of 1083 tumours showed that the EPOR locus was amplified in <0.7% tumours, only in large amplicons, and less than 2–3 times the normal copy number. In contrast, EGFR, CCND1, and HER2 were amplified in 3.5–6.7% of tumours, often >9 times the normal copy number and frequently amplified in small amplicons indicative of the selective amplification of these genes. These data demonstrate that EPOR amplification is a rare event in solid tumours and not a primary driver of tumour formation and progression.
Although the EPOR locus was rarely amplified in tumours, it was possible that EPOR was overexpressed through other mechanisms. Here, we report the first comprehensive, quantitative analysis of EPOR transcript levels in multiple tumour types compared to tissues of tumour origin. In this analysis, we found that levels of EPOR transcripts in tumour samples and cell lines from more than 15 different tumour types were equivalent to, or lower than, levels in normal tissues. In concordance with our study, it was recently reported that levels of EPOR transcripts in prostate (Feldman et al, 2006) and head and neck tumours (Winter et al, 2005) were similar to levels in normal tissues. High levels of EPOR transcripts were reported in kidney tumours compared with normal kidney (Lee et al, 2005) and in melanoma cell lines compared with normal melanocytes (Selzer et al, 2000). However, these latter studies used small numbers of samples, and levels of transcripts were not quantified. In the present study, we examined 11 kidney and 9 melanoma tumour samples and found no increase in levels of EPOR transcripts relative to normal tissues.
Most solid tumour cell lines we examined expressed EpoR mRNA; however, the levels were substantially lower compared to that found in Epo-responsive cells (UT7/Epo) or tissues (bone marrow). In addition, we were unable to detect EpoR on the cell surface of the same cells. Owing to non-specificities and insensitivity of antibodies available for EpoR protein detection (Elliott et al, 2006; Brown et al, 2007; Della Ragione et al, 2007; Kirkeby et al, 2007; Laugsch et al, 2008; Sturiale et al, 2007), we have been unable to determine EpoR protein expression in these lines. However, the lack of detectable surface binding of 125I-Epo to intact cells suggests that EpoR protein levels may be low if expressed at all. Translocation of EpoR to the cell surface is an inefficient process (less than 1% of total cellular EpoR molecules are produced on the cell surface); thus, EPOR transcription and EpoR protein synthesis does not always lead to cell-surface expression of functional EpoR in tumour cells (Migliaccio et al, 1991; Neumann et al, 1993; Sawyer and Hankins, 1993; Hilton et al, 1995; Hermine et al, 1996; Kurten et al, 1996; Supino-Rosin et al, 1999). Thus, an alternative explanation may be inefficient transport of EpoR protein to the cell surface. Janus kinase 2 is essential for surface expression of EpoR; in haematopoietic cells, it binds EpoR in the endoplasmic reticulum, induces correct protein folding, and localises EpoR to the cell surface (Huang et al, 2001). Some of the cell lines investigated had no or very low Jak2 expression and may, in part, account for the lack of detectable EpoR on the surface in some cells if protein is synthesised. Interestingly, murine 32D-Epo-independent cells expressed Jak2 (DaSilva et al, 1994) and EpoR, but EpoR was not detected at the cell surface (Migliaccio et al, 1991). This suggests that accessory proteins other than Jak2 may also be required to modulate surface expression of EpoR or may alter the affinity of EpoR for Epo (Dong and Goldwasser, 1993; Masuda et al, 1993; Nagao et al, 1993; Hermine et al, 1994). Recently, it has been hypothesised that an alternative receptor for rHuEpo, a heterodimer of EpoR and the β-common chain, mediates tissue-protective effects in non-haematopoietic tissues (Brines et al, 2004). However, these data were not reproduced by other investigators (Um et al, 2007). Taken together, these data suggest that Epo responses in these cells, if any, may be weak.
It is possible that very low levels of surface receptor on the tumour cell lines we examined are present and they mediate a response to rHuEpo, thereby explaining the responses to rHuEpo reportedly detected by some investigators (Westenfelder and Baranowski, 2000; Acs et al, 2001, 2003; Um et al, 2007). Differentiated neuroblastoma cell line SHSY-5Y was reported to express extremely low (∼17) EpoR homodimers on the cell surface (Um et al, 2007). This level of surface receptor was reportedly sufficient to induce low-level signalling and survival responses (Um et al, 2007). A proliferative effect of rHuEpo was reported in MCF-7 cells (Acs et al, 2001), but seven other studies reported no proliferative effect in MCF-7 cells (Berdel et al, 1991, 1992; Mundt et al, 1992; Rosti et al, 1993; Gewirtz et al, 2006; Li et al, 2006; Laugsch et al, 2008). Also, rHuEpo reportedly increased the survival of parental HeLa cells in one study (Acs et al, 2003) but not in another study (Pajonk et al, 2004). Renal carcinoma cell line CAKI-2 was reported to bind 125I-Epo and proliferate in vitro a maximum of 2.5-fold (Westenfelder and Baranowski, 2000). Since most of these studies had technical concerns (e.g., performed in the absence of serum, lack of critical controls (e.g., vehicle to control for contaminating carrier proteins), use of suprapharmacologic doses of rHuEpo, modest proliferative responses for established cell lines), the results from these studies are inconclusive and inconsistent. In one such study, the direct effect of rHuEpo to induce signalling and protect a rat mammary carcinoma cell line from Taxol-induced apoptosis in vitro did not translate to an effect on Taxol-induced tumour inhibition in vivo, despite a reported impact on signalling pathways in the tumour (Hardee et al, 2006). The conclusion that ESAs promote tumour cell growth is not supported by in vivo studies in rodent tumour models: in 23 published studies, there was no tumour-promoting effect of ESAs either alone or in combination with radiotherapy or chemotherapy (Sinclair et al, 2007). In some studies, ESAs were reported to enhance the efficiency of tumour-ablative therapy (Silver and Piver, 1999; Mittelman et al, 2001; Thews et al, 2001; Golab et al, 2002; Pinel et al, 2004; Sigounas et al, 2004; Ning et al, 2005) and induce tumour regression (Mittelman et al, 2001). Therefore, the most physiologically relevant tumour models that directly examined effects of ESAs in vivo do not support a tumour-promoting effect of ESAs.
In summary, we found no evidence that EpoR mRNA was overexpressed in the solid tumour types analysed in this study (through genomic amplification or other mechanisms). Erythropoietin receptor transcript levels were low and EpoR protein was not trafficked to the cell surface at detectable levels. These data suggest that primary tumour samples and tumour cell lines did not overexpress EpoR. Taken together, these results question the hypothesis that there is functional relevance to EpoR mRNA transcription in tumours.
Change history
16 November 2011
This paper was modified 12 months after initial publication to switch to Creative Commons licence terms, as noted at publication
References
Acs G, Acs P, Beckwith SM, Pitts RL, Clements E, Wong K, Verma A (2001) Erythropoietin and erythropoietin receptor expression in human cancer. Cancer Res 61: 3561–3565
Acs G, Zhang PJ, McGrath CM, Acs P, McBroom J, Mohyeldin A, Liu S, Lu H, Verma A (2003) Hypoxia-inducible erythropoietin signaling in squamous dysplasia and squamous cell carcinoma of the uterine cervix and its potential role in cervical carcinogenesis and tumor progression. Am J Pathol 162: 1789–1806
Berdel WE, Danhauser-Riedl S, Oberberg D, Zafferani M (1992) Effects of hematopoietic growth factors on malignant nonhematopoietic cells. Semin Oncol 19: 41–45
Berdel WE, Oberberg D, Reufi B, Thiel E (1991) Studies on the role of recombinant human erythropoietin in the growth regulation of human nonhematopoietic tumor cells in vitro. Ann Hematol 63: 5–8
Bohlius J, Wilson J, Seidenfeld J, Piper M, Schwarzer G, Sandercock J, Trelle S, Weingart O, Bayliss S, Djulbegovic B, Bennett CL, Langensiepen S, Hyde C, Engert A (2006) Recombinant human erythropoietins and cancer patients: updated meta-analysis of 57 studies including 9353 patients. J Natl Cancer Inst 98: 708–714
Brines M, Grasso G, Fiordaliso F, Sfacteria A, Ghezzi P, Fratelli M, Latini R, Xie QW, Smart J, Su-Rick CJ, Pobre E, Diaz D, Gomez D, Hand C, Coleman T, Cerami A (2004) Erythropoietin mediates tissue protection through an erythropoietin and common beta-subunit heteroreceptor. Proc Natl Acad Sci USA 101: 14907–14912
Brown WM, Maxwell P, Graham AN, Yakkundi A, Dunlop EA, Shi Z, Johnston PG, Lappin TR (2007) Erythropoietin receptor expression in non-small cell lung carcinoma: a question of antibody specificity. Stem Cells 25: 718–722
DaSilva L, Howard OM, Rui H, Kirken RA, Farrar WL (1994) Growth signaling and JAK2 association mediated by membrane-proximal cytoplasmic regions of prolactin receptors. J Biol Chem 269: 18267–18270
Della Ragione F, Cucciolla V, Borriello A, Oliva A, Perrotta S (2007) Erythropoietin receptors on cancer cells: a still open question. J Clin Oncol 25: 1812–1813; author reply 1815
Dong YJ, Goldwasser E (1993) Evidence for an accessory component that increases the affinity of the erythropoietin receptor. Exp Hematol 21: 483–486
Elliott S, Busse L, Bass MB, Lu H, Sarosi I, Sinclair AM, Spahr C, Um M, Van G, Begley CG (2006) Anti-Epo receptor antibodies do not predict Epo receptor expression. Blood 107: 1892–1895
Elliott S, Lorenzini T, Chang D, Barzilay J, Delorme E (1997) Mapping of the active site of recombinant human erythropoietin. Blood 89: 493–502
Feldman L, Wang Y, Rhim JS, Bhattacharya N, Loda M, Sytkowski AJ (2006) Erythropoietin stimulates growth and STAT5 phosphorylation in human prostate epithelial and prostate cancer cells. Prostate 66: 135–145
Gewirtz DA, Di X, Walker TD, Sawyer ST (2006) Erythropoietin fails to interfere with the antiproliferative and cytotoxic effects of antitumor drugs. Clin Cancer Res 12: 2232–2238
Golab J, Olszewska D, Mroz P, Kozar K, Kaminski R, Jalili A, Jakobisiak M (2002) Erythropoietin restores the antitumor effectiveness of photodynamic therapy in mice with chemotherapy-induced anemia. Clin Cancer Res 8: 1265–1270
Hardee ME, Rabbani ZN, Arcasoy MO, Kirkpatrick JP, Vujaskovic Z, Dewhirst MW, Blackwell KL (2006) Erythropoietin inhibits apoptosis in breast cancer cells via an Akt-dependent pathway without modulating in vivo chemosensitivity. Mol Cancer Ther 5: 356–361
Henke M, Laszig R, Rube C, Schafer U, Haase KD, Schilcher B, Mose S, Beer KT, Burger U, Dougherty C, Frommhold H (2003) Erythropoietin to treat head and neck cancer patients with anaemia undergoing radiotherapy: randomised, double-blind, placebo-controlled trial. Lancet 362: 1255–1260
Henke M, Mattern D, Pepe M, Bezay C, Weissenberger C, Werner M, Pajonk F (2006) Do erythropoietin receptors on cancer cells explain unexpected clinical findings? J Clin Oncol 24: 4708–4713
Hermine O, Dong YJ, Goldwasser E (1994) Effects of butyrate on the erythropoietin receptor of cell line IW201. Blood 84: 811–814
Hermine O, Dubart A, Porteux F, Mayeux P, Titeux M, Dumenil D, Vainchenker W (1996) Inhibition of the erythropoietin-induced erythroid differentiation by granulocyte–macrophage colony-stimulating factor in the human UT-7 cell line is not due to a negative regulation of the erythropoietin receptor. Blood 87: 1746–1753
Hilton DJ, Watowich SS, Murray PJ, Lodish HF (1995) Increased cell surface expression and enhanced folding in the endoplasmic reticulum of a mutant erythropoietin receptor. Proc Natl Acad Sci USA 92: 190–194
Huang LJ, Constantinescu SN, Lodish HF (2001) The N-terminal domain of Janus kinase 2 is required for Golgi processing and cell surface expression of erythropoietin receptor. Mol Cell 8: 1327–1338
Hupe P, Stransky N, Thiery JP, Radvanyi F, Barillot E (2004) Analysis of array CGH data: from signal ratio to gain and loss of DNA regions. Bioinformatics 20: 3413–3422
Kirkeby A, van Beek J, Nielsen J, Leist M, Helboe L (2007) Functional and immunochemical characterisation of different antibodies against the erythropoietin receptor. J Neurosci Methods 164: 50–58
Kurten RC, Cadena DL, Gill GN (1996) Enhanced degradation of EGF receptors by a sorting nexin, SNX1. Science 272: 1008–1010
Laugsch M, Metzen E, Svensson T, Depping R, Jelkmann W (2008) Lack of functional erythropoietin receptors on cancer cell lines. Int J Cancer 122 (5): 1005–1011
Lee YS, Vortmeyer AO, Lubensky IA, Vogel TW, Ikejiri B, Ferlicot S, Benoit G, Giraud S, Oldfield EH, Linehan WM, Teh BT, Richard S, Zhuang Z (2005) Coexpression of erythropoietin and erythropoietin receptor in von Hippel–Lindau disease-associated renal cysts and renal cell carcinoma. Clin Cancer Res 11: 1059–1064
Leyland-Jones B, Semiglazov V, Pawlicki M, Pienkowski T, Tjulandin S, Manikhas G, Makhson A, Roth A, Dodwell D, Baselga J, Biakhov M, Valuckas K, Voznyi E, Liu X, Vercammen E (2005) Maintaining normal hemoglobin levels with epoetin alfa in mainly nonanemic patients with metastatic breast cancer receiving first-line chemotherapy: a survival study. J Clin Oncol 23: 5960–5972
Li Y, Zhang J, Long Y (2006) Effect of erythropoietin on the proliferation of human cancer cell line MCF-7. Wuhan Daxue Xuebao (Yixue Ban) 27: 429–432
Lucito R, Healy J, Alexander J, Reiner A, Esposito D, Chi M, Rodgers L, Brady A, Sebat J, Troge J, West JA, Rostan S, Nguyen KC, Powers S, Ye KQ, Olshen A, Venkatraman E, Norton L, Wigler M (2003) Representational oligonucleotide microarray analysis: a high-resolution method to detect genome copy number variation. Genome Res 13: 2291–2305
Masuda S, Nagao M, Takahata K, Konishi Y, Gallyas Jr F, Tabira T, Sasaki R (1993) Functional erythropoietin receptor of the cells with neural characteristics. Comparison with receptor properties of erythroid cells. J Biol Chem 268: 11208–11216
Migliaccio AR, Migliaccio G, D'Andrea A, Baiocchi M, Crotta S, Nicolis S, Ottolenghi S, Adamson JW (1991) Response to erythropoietin in erythroid subclones of the factor-dependent cell line 32D is determined by translocation of the erythropoietin receptor to the cell surface. Proc Natl Acad Sci USA 88: 11086–11090
Mittelman M, Neumann D, Peled A, Kanter P, Haran-Ghera N (2001) Erythropoietin induces tumor regression and antitumor immune responses in murine myeloma models. Proc Natl Acad Sci USA 98: 5181–5186
Mundt D, Berger MR, Bode G (1992) Effect of recombinant human erythropoietin on the growth of human tumor cell lines in vitro. Micro-titertec-tetrazolium assay. Arzneimittelforschung 42: 92–95
Nagao M, Matsumoto S, Masuda S, Sasaki R (1993) Effect of tunicamycin treatment on ligand binding to the erythropoietin receptor: conversion from two classes of binding sites to a single class. Blood 81: 2503–2510
Neumann D, Wikstrom L, Watowich SS, Lodish HF (1993) Intermediates in degradation of the erythropoietin receptor accumulate and are degraded in lysosomes. J Biol Chem 268: 13639–13649
Ning S, Hartley C, Molineux G, Knox SJ (2005) Darbepoetin alfa potentiates the efficacy of radiation therapy in mice with corrected or uncorrected anemia. Cancer Res 65: 284–290
Osterborg A, Aapro M, Cornes P, Haselbeck A, Hayward CR, Jelkmann W (2007) Preclinical studies of erythropoietin receptor expression in tumour cells: impact on clinical use of erythropoietic proteins to correct cancer-related anaemia. Eur J Cancer 43: 510–519
Pajonk F, Weil A, Sommer A, Suwinski R, Henke M (2004) The erythropoietin-receptor pathway modulates survival of cancer cells. Oncogene 23: 8987–8991
Parkes HC, Lillycrop K, Howell A, Craig RK (1990) C-erbB2 mRNA expression in human breast tumours: comparison with c-erbB2 DNA amplification and correlation with prognosis. Br J Cancer 61: 39–45
Pei L, Peng Y, Yang Y, Ling XB, Van Eyndhoven WG, Nguyen KC, Rubin M, Hoey T, Powers S, Li J (2002) PRC17, a novel oncogene encoding a Rab GTPase-activating protein, is amplified in prostate cancer. Cancer Res 62: 5420–5424
Pinel S, Barberi-Heyob M, Cohen-Jonathan E, Merlin JL, Delmas C, Plenat F, Chastagner P (2004) Erythropoietin-induced reduction of hypoxia before and during fractionated irradiation contributes to improvement of radioresponse in human glioma xenografts. Int J Radiat Oncol Biol Phys 59: 250–259
Ragione FD, Cucciolla V, Borriello A, Oliva A (2007) Erythropoietin receptors on cancer cells: still an open question. J Clin Oncol 25: 1812–1813
Rajagopalan D (2003) A comparison of statistical methods for analysis of high density oligonucleotide array data. Bioinformatics 19: 1469–1476
Rege-Cambrin G, Scaravaglio P, Carozzi F, Giordano S, Ponzetto C, Comoglio PM, Saglio G (1992) Karyotypic analysis of gastric carcinoma cell lines carrying an amplified c-met oncogene. Cancer Genet Cytogenet 64: 170–173
Reissmann PT, Koga H, Figlin RA, Holmes EC, Slamon DJ (1999) Amplification and overexpression of the cyclin D1 and epidermal growth factor receptor genes in non-small-cell lung cancer. Lung Cancer Study Group. J Cancer Res Clin Oncol 125: 61–70
Rosti V, Pedrazzoli P, Ponchio L, Zibera C, Novella A, Lucotti C, Della Cuna GR, Cazzola M (1993) Effect of recombinant human erythropoietin on hematopoietic and non-hematopoietic malignant cell growth in vitro. Haematologica 78: 208–212
Sawyer ST, Hankins WD (1993) The functional form of the erythropoietin receptor is a 78-kDa protein: correlation with cell surface expression, endocytosis, and phosphorylation. Proc Natl Acad Sci USA 90: 6849–6853
Schmitt E, Gehrmann M, Brunet M, Multhoff G, Garrido C (2007) Intracellular and extracellular functions of heat shock proteins: repercussions in cancer therapy. J Leukoc Biol 81 (1): 15–27
Selzer E, Wacheck V, Kodym R, Schlagbauer-Wadl H, Schlegel W, Pehamberger H, Jansen B (2000) Erythropoietin receptor expression in human melanoma cells. Melanoma Res 10: 421–426
Sigounas G, Sallah S, Sigounas VY (2004) Erythropoietin modulates the anticancer activity of chemotherapeutic drugs in a murine lung cancer model. Cancer Lett 214: 171–179
Silver DF, Piver MS (1999) Effects of recombinant human erythropoietin on the antitumor effect of cisplatin in SCID mice bearing human ovarian cancer: a possible oxygen effect. Gynecol Oncol 73: 280–284
Sinclair AM, Todd MD, Forsythe K, Knox SJ, Elliott S, Begley CG (2007) Expression and function of erythropoietin receptors in tumors: implications for the use of erythropoiesis-stimulating agents in cancer patients. Cancer 110: 477–488
Smyth GK, Speed T (2003) Normalization of cDNA microarray data. Methods 31: 265–273
Stuben G, Thews O, Pottgen C, Knuhmann K, Sack H, Stuschke M, Vaupel P (2003) Impact of anemia prevention by recombinant human erythropoietin on the sensitivity of xenografted glioblastomas to fractionated irradiation. Strahlenther Onkol 179: 620–625
Stuben G, Thews O, Pottgen C, Knuhmann K, Vaupel P, Stuschke M (2001) Recombinant human erythropoietin increases the radiosensitivity of xenografted human tumours in anaemic nude mice. J Cancer Res Clin Oncol 127: 346–350
Sturiale A, Campo S, Crasci E, Coppolino G, Bolignano D, Grasso G, Buemi M (2007) Erythropoietin and its lost receptor. Nephrol Dial Transplant 22: 1484–1485
Supino-Rosin L, Yoshimura A, Altaratz H, Neumann D (1999) A cytosolic domain of the erythropoietin receptor contributes to endoplasmic reticulum-associated degradation. Eur J Biochem 263: 410–419
Szepetowski P, Simon MP, Grosgeorge J, Huebner K, Bastard C, Evans GA, Tsujimoto Y, Birnbaum D, Theillet C, Gaudray P (1992) Localization of 11q13 loci with respect to regional chromosomal breakpoints. Genomics 12: 738–744
Thews O, Kelleher DK, Vaupel P (2001) Erythropoietin restores the anemia-induced reduction in cyclophosphamide cytotoxicity in rat tumors. Cancer Res 61: 1358–1361
Um M, Gross AW, Lodish HF (2007) A ‘classical’ homodimeric erythropoietin receptor is essential for the antiapoptotic effects of erythropoietin on differentiated neuroblastoma SH-SY5Y and pheochromocytoma PC-12 cells. Cell Signal 19: 634–645
van der Horst EH, Degenhardt YY, Strelow A, Slavin A, Chinn L, Orf J, Rong M, Li S, See LH, Nguyen KQ, Hoey T, Wesche H, Powers S (2005) Metastatic properties and genomic amplification of the tyrosine kinase gene ACK1. Proc Natl Acad Sci USA 102: 15901–15906
Westenfelder C, Baranowski RL (2000) Erythropoietin stimulates proliferation of human renal carcinoma cells. Kidney Int 58: 647–657
Westphal G, Niederberger E, Blum C, Wollman Y, Knoch TA, Rebel W, Debus J, Friedrich E (2002) Erythropoietin and G-CSF receptors in human tumor cells: expression and aspects regarding functionality. Tumori 88: 150–159
Winter SC, Shah KA, Campo L, Turley H, Leek R, Corbridge RJ, Cox GJ, Harris AL (2005) Relation of erythropoietin and erythropoietin receptor expression to hypoxia and anemia in head and neck squamous cell carcinoma. Clin Cancer Res 11: 7614–7620
Acknowledgements
We thank Gene Cutler, Nicki Chin, Daniel M Baker, Mike Damore, Amy Lafayette for assistance with data acquisition; Barbra Sasu for critically reviewing and Kathryn Boorer, PhD, for assistance with writing this manuscript.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
From twelve months after its original publication, this work is licensed under the Creative Commons Attribution-NonCommercial-Share Alike 3.0 Unported License. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-sa/3.0/
About this article
Cite this article
Sinclair, A., Rogers, N., Busse, L. et al. Erythropoietin receptor transcription is neither elevated nor predictive of surface expression in human tumour cells. Br J Cancer 98, 1059–1067 (2008). https://doi.org/10.1038/sj.bjc.6604220
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.bjc.6604220
Keywords
This article is cited by
-
ΗΙF1α, EGR1 and SP1 co-regulate the erythropoietin receptor expression under hypoxia: an essential role in the growth of non-small cell lung cancer cells
Cell Communication and Signaling (2019)
-
Erythropoietin promoted the proliferation of hepatocellular carcinoma through hypoxia induced translocation of its specific receptor
Cancer Cell International (2017)
-
Progress in detecting cell-surface protein receptors: the erythropoietin receptor example
Annals of Hematology (2014)
-
The erythropoietin receptor is a downstream effector of Klotho-induced cytoprotection
Kidney International (2013)
-
Effects of erythropoietin receptors and erythropoiesis-stimulating agents on disease progression in cancer
British Journal of Cancer (2012)