Abstract
Data sources
PubMed, Embase, Cochrane Library, the World Health Organization (http://www.who.int/trialsearch) and Clinical Trials.gov (http://www.ClinicalTrials.gov.)
Study selection
Two reviewers independently selected studies. Randomised controlled trials (RCTs) in adults over the age of 18 with diabetes and periodontal disease undergoing non-surgical periodontal treatment with or without adjunctive antibiotics, with a follow up period of at least three months were considered.
Data extraction and synthesis
Data abstraction was carried out by two reviewers independently with study quality being assessed using the Cochrane risk of bias tool. The absolute difference of HbA1c percentage in each treatment arm was recorded or calculated. Weighted mean difference (WMD) was calculated and meta-analysis conducted. The primary outcome was hemoglobin A1c (HbA1c), and secondary outcomes were periodontal parameters which included probing pocket depth (PPD) and clinical attachment level (CAL).
Results
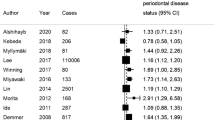
Ten RCTs involving a total of 1135 patients were included. Meta-analysis (ten studies) showed a mean change of HbA1c at three months = −0.36% (95%CI: −0.52% – 0.19%, P< 0.0001) with a change at six months = − 0.30%, (95%CI: −0.69% to 0.09%, P = 0.13). Clinically substantial and statistically significant reduction of PPD and CAL were found between subjects with and without treatment after periodontal therapy (PPD 20.42 mm, 95%CI: 20.60 to 20.23, P,0.00001; CAL 20.34 mm, 95%CI: 20.52 to 20.16, P = 0.0002).
Conclusions
This demonstrates that periodontal treatment leads to a reduction of HbA1c in diabetic patients with periodontitis, with improvement of periodontal status for three months after treatment. But the treatment may have no obvious effect on glycaemic control six months after treatment. So physicians and dentists should carefully interpret these results when they apply them in clinical practice.
Similar content being viewed by others
Commentary
The systematic review by Wang et al. is well conducted and satisfies the main methodological standards of the Cochrane Collaboration - although it is not a Cochrane systematic review per se. Most importantly, this is the first systematic review that takes into account the results from the ‘Diabetes and Periodontal Therapy Trial’ (DPTT), a large randomised controlled trial published in December 2013 in the Journal of the American Medical Association.1 Results from this sufficiently powered trial (n=514) failed to demonstrate a significant effect of periodontal treatment on glycaemic control among diabetic patients.
This topic has been much discussed in the literature during recent years, including in previous issues of Evidence-Based Dentistry.2,3,4 It is worth highlighting that effect sizes reported in successive meta-analyses during the last ten years have been globally decreasing over time. Until 2010, reported effects for the mean percentage difference in HbA1c for periodontal treatment ranged between −0.46% and −0.40%.5,6,7 In 2013, values reported in two meta-analyses decreased slightly, to between −0.38% and −0.36%.8,9 Finally, since 2014 and the publication of the DPTT,1 the decrease has continued, with values from two other meta-analyses, including the one by Wang et al., showing significant values of −0.36% to −0.27%.10,11 In these two most recent meta-analyses, the main result from the DPTT trial had a marked influence on the calculated mean differences, respectively 18.1%10 and 27%.11
Considering original trials, the decreasing trend in effect sizes with time is a well-known phenomenon. Time lag in the publication of negative findings has been reported as a possible explanation.12 Another more subtle explanation is the ‘Proteus phenomenon’,13 which describes the phenomenon of rapidly alternating extreme research claims and extremely opposite refutations.14
It is possible that the widespread attention given to the potential effect of periodontal treatment on HbA1c values led to major excitement in the scientific community. Then, ‘negative’ results may have become ‘attractive’.14 Inconsistent conclusions between results from meta-analyses and large trials create confusion in clinical guidelines.15 Today, in 2015, the topic is at the crossroads, and some key points should be kept in mind:
1) When all the available evidence is combined, the effect of periodontal treatment on HbA1c still points to benefits of periodontal treatment to improve glycaemic control in diabetic patients
2) Those concerned with health care should remain attentive to the evolution of these data because the trends are decreasing, and several trials are still ongoing
3) Researchers and clinicians should consider that patient-centred outcomes (such as assessment of quality of life) could also be of interest in the topic.
Practice point
-
The available evidence in 2015 points to benefits of periodontal treatment to improve glycaemic control in diabetic patients.
References
Engebretson SP, Hyman LG, Michalowicz BS, et al. The effect of nonsurgical periodontal therapy on hemoglobin A1c levels in persons with type 2 diabetes and chronic periodontitis: a randomized clinical trial. JAMA 2013; 310: 2523–2532.
Garcia R . Periodontal treatment could improve glycaemic control in diabetic patients. Evid Based Dent 2009; 10: 20–21.
Vergnes JN . Treating periodontal disease may improve metabolic control in diabetics. Evid Based Dent 2010; 11: 73–74.
Engebretson S . Periodontal disease and glycemic control in diabetics. Evid Based Dent 2014; 15: 93–94.
Simpson TC, Needleman I, Wild SH, Moles DR, Mills EJ . Treatment of periodontal disease for glycaemic control in people with diabetes. Cochrane Database Syst Rev 2010; 5:CD004714 (2010). doi:10.1002/14651858.CD004714.pub2
Teeuw WJ, Gerdes VE, Loos BG . Effect of periodontal treatment on glycemic control of diabetic patients: a systematic review and meta-analysis. Diabetes Care 2010; 33: 421–427.
Darré L, Vergnes JN, Gourdy P, Sixou M . Efficacy of periodontal treatment on glycaemic control in diabetic patients: A meta-analysis of interventional studies. Diabetes Metab 2008; 34: 497–506.
Corbella S, Francetti L, Taschieri S, De Siena F, Fabbro M D . Effect of periodontal treatment on glycemic control of patients with diabetes: A systematic review and meta-analysis. J Diabetes Investig 2013; 4: 502–509.
Engebretson S, Kocher T . Evidence that periodontal treatment improves diabetes outcomes: a systematic review and meta-analysis. J Periodontol 2013; 84: S153–169.
Wang X, Han X, Guo X, Luo X, Wang D . The effect of periodontal treatment on hemoglobin a1c levels of diabetic patients: a systematic review and meta-analysis. PloS One 2014; 9:e 108412.
Li Q, Hao S, Fang J, Xie J, Kong XH, Yang JX . Effect of non-surgical periodontal treatment on glycemic control of patients with diabetes: a meta-analysis of randomized controlled trials. Trials 2015; 16: 291.
Ioannidis JP . Effect of the statistical significance of results on the time to completion and publication of randomized efficacy trials. JAMA 1998; 279: 281–286.
Ioannidis J, Trikalinos TA . Early extreme contradictory estimates may appear in published research: the Proteus phenomenon in molecular genetics research and randomized trials. J Clin. Epidemiol 2005; 58: 543–549.
Ioannidis JP . Why most published research findings are false. PLoS Med 2005; 2:e124 (2005).
Ioannidis JA, Cappelleri JC, Lau J . Issues in comparisons between meta-analyses and large trials. JAMA 1998; 279:1089–1093.
Author information
Authors and Affiliations
Additional information
Address for correspondence: Dr X Wang, Department of Stomatology, Changhai Hospital, The Second Military Medical University, Shanghai, China. Email: Wang_Dento@163.com
Wang X, Han X, Guo X, Luo X, Wang D. The effect of periodontal treatment on hemoglobin a1c levels of diabetic patients: a systematic review and meta-analysis. PLoS One. 2014; 9: e108412. doi:10.1371/journal.pone.0108412
Rights and permissions
About this article
Cite this article
Vergnes, JN. Review finds periodontal treatment has short term benefits for diabetics. Evid Based Dent 16, 78–79 (2015). https://doi.org/10.1038/sj.ebd.6401114
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.ebd.6401114