Abstract
Data sources
The Cochrane Oral Health Group's Trials Register, Cochrane Central Register of Controlled Trials (CENTRAL), Medline and Embase databases were searched with no language or date restrictions.
Study selection
Three reviewers independently selected studies. Randomised controlled trials (RCTs) involving interventions to treat patients with neurosensory defect of the inferior alveolar or lingual nerve or both as a sequela of iatrogenic injury were considered.
Data extraction and synthesis
Standard Cochrane methodological procedures were followed.
Results
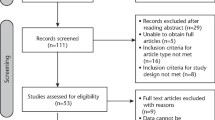
Two studies considered at high risk of bias, reporting data from 26 analysed patients were included. Both studies investigated the effectiveness of low-level laser treatment compared to placebo laser therapy on inferior alveolar sensory deficit as a result of iatrogenic injury. Two studies assessed as at high risk of bias, reporting data from 26 analysed participants were included in this review. The age range of participants was from 17 to 55 years. Both trials investigated the effectiveness of low-level laser treatment compared to placebo laser therapy on inferior alveolar sensory deficit as a result of iatrogenic injury.
Patient-reported altered sensation was partially reported in one study and fully reported in another. Following treatment with laser therapy, there was some evidence of an improvement in the subjective assessment of neurosensory deficit in the lip and chin areas compared to placebo, though the estimates were imprecise: a difference in mean change in neurosensory deficit of the chin of 8.40 cm (95% confidence interval (CI) 3.67 to 13.13) and a difference in mean change in neurosensory deficit of the lip of 21.79 cm (95% CI 5.29 to 38.29). The overall quality of the evidence for this outcome was very low. No studies reported on the effects of the intervention on the remaining primary outcomes of pain, difficulty eating, speaking or taste. No studies reported on quality of life or adverse events.
Conclusions
There is clearly a need for randomised controlled clinical trials to investigate the effectiveness of surgical, medical and psychological interventions for iatrogenic inferior alveolar and lingual nerve injuries. Primary outcomes of this research should include: patient-focused morbidity measures including altered sensation and pain, pain, quantitative sensory testing and the effects of delayed treatment.
Similar content being viewed by others
Commentary
Every surgery and treatment in the human body may have associated risks and side effects. Iatrogenic nerve injury in the head and neck area is uncommon, however the consequences can permanently or temporarily traumatise the patient's normal daily functions such as eating and smiling.
Many dental and non-dental procedures and trauma can affect and injure the nerves. Surgical procedures such as third molar extractions, orthognathic surgeries and implant placement are mostly associated with the occurrence of nerve injury. Local anaesthetic injection and endodontic treatment could cause nerve injuries as well.
The authors had a very clear question, which was to address the effectiveness of any surgical, medical or psychological treatment for the management of iatrogenic nerve injury, which was accomplished in a well done methodological review.
The extensive search for randomised clinical trials resulted in the selection of two articles included and selected for the final analysis. The two high risk of bias studies as they were categorised by the authors examined the use of lower-level laser for the treatment of iatrogenic nerve injuries compared to placebo.
The limitations of the studies and the imprecision of the data provided very low quality evidence and no therapy can be indicated or preferred for the treatment of idiopathic nerve injury.
Operative and post-operative complications seem commonly rare during dental procedures. However due to the long- or short-term impact and severity it is important to take them into account in planning any dental procedure, and having a knowledge of the patient's risk factors that could be associated with the complications such as age, surgical difficulty, medical status and smoking.
It appears that the skills of the operator and the proximity to the inferior alveolar nerve are the risk factors associated with injury to the inferior alveolar and lingual nerves following third molar extractions.1
Since there is no definitive answer on how to treat nerve injuries, the best recommendation is to try as much as possible to avoid the risks for nerve injury since the successful management is unclear at this time.
References
Jerjes W, Upile T, Shah P, et al. Risk factors associated with injury to the inferior alveolar and lingual nerves following third molar surgery-revisited. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2010; 109: 335–345.
Author information
Authors and Affiliations
Additional information
Address for correspondence: Luisa Fernandez Mauleffinch, Review Group Co-ordinator, Cochrane Oral Health Group, School of Dentistry, The University of Manchester, Coupland III Building, Oxford Road, Manchester, M13 9PL, UK. E-mail: luisa.fernandez@manchester.ac.uk
Coulthard P, Kushnerev E, Yates JM, Walsh T, Patel N, Bailey E, Renton TF. Interventions for iatrogenic inferior alveolar and lingual nerve injury. Cochrane Database Syst Rev 2014; 4: Art. No.: CD005293. DOI: 10.1002/14651858.CD005293.pub2.
Rights and permissions
About this article
Cite this article
Veitz-Keenan, A., Keenan, J. Trials needed to identify best management of iatrogenic inferior alveolar and lingual nerve injuries. Evid Based Dent 16, 29 (2015). https://doi.org/10.1038/sj.ebd.6401085
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.ebd.6401085
This article is cited by
-
Surgical treatment of painful inferior alveolar nerve injuries following endodontic treatment: a consecutive case series of seven patients
Oral and Maxillofacial Surgery (2017)