Abstract
Data sources
Medline, CINAHL, PsycINFO, SCI, SSCI, Cochrane Database of Systematic Reviews, Business Source Premier, Google scholar.
Study selection
Primary or secondary reports and studies, published in English, after 1993, likely to include data relevant to direct access, report on empirical data relating to the operation of that system.
Data extraction and synthesis
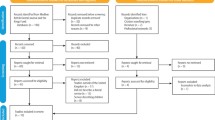
After initial screening, titles and abstracts were assessed by two reviewers, and disagreements resolved by the third. Full texts of these eligible ones were then assessed by the team until consensus reached. Data extraction by one reviewer was checked by a second and disagreements resolved by discussion with the third. Study quality was assessed through reference to CASP or SIGN checklists. Descriptive analyses and synthesis of findings were given.
Results
From the 1,733 studies yielded from the search, over 100 research dental and other health-related papers were identified as relevant. Thirty-five studies were eligible for inclusion under dental health care direct access and 57 under non-dental health care direct access literature. The quality of the evidence was varied but on the whole assessed as moderately good quality.
There was no evidence of increased risk to patient safety in any of the included seven studies. Four studies on appropriateness of DCP referrals reported a high proportion of over-referral, one study found under-referral and one good agreement regarding referral decisions.
Six of the seven studies looking at DCPs' knowledge or support to patients for smoking cessation, diabetes, child abuse and domestic violence found deficiencies in DCPs' knowledge or support to patients, but these studies didn't have evidence to suggest how this compared to dentists.
Increasing access to dental therapists and hygienists (whether indirect, general or without supervision of a dentist) according to ten studies, resulted in greater access to and use of dental services by underserved populations. Three studies suggested variable and, at most, modest cost savings to patients and service providers. High levels of patient satisfaction were found in all eight studies reporting this, and DCP job satisfaction was reported to be higher with direct access.
Conclusions
Although over-referral of patients to dentists was suggested and a need for training on assessment and referral skills, there was no evidence of significant issues of patient safety from the clinical activities of DCPs. There was strong evidence of improved access to dental care with direct access arrangements, cost benefits to patients/service providers and high levels of patient satisfaction.
Similar content being viewed by others
Commentary
In the UK, up until March 2013, any patient attending for dental treatment to be provided by a Dental Care Professional (DCP), firstly had to see a dentist for treatment planning, and then referral on to the DCP. DCPs include dental nurses, dental hygienists, dental therapists, dental technicians, clinical dental technicians and orthodontic therapists, and make up around 60% of the dental workforce. However, in May 2012 the Office of Fair Trading (OFT) report on Dentistry in the UK (Dentistry, OFT1414: www.oft.gov.uk) made the case for deregulation of the requirement for patients to see a registered dentist before having access to a DCP, by calling on the General Dental Council (GDC), ‘to review and urgently remove restrictions on direct patient access to dental care professionals’.1 In some countries it is already legal for patients to be seen directly by various DCPs without seeing a dentist first.
In response, the GDC commissioned this rapid evidence review in April 2012 (completed 29th June 2012) to help inform their Direct Access Task and Finish Group, which made recommendations to the GDC. The aim of the review was to find, assess, appraise and synthesise the evidence on likely impact, including benefits and risks, of introducing direct access for patients to have treatment by DCPs without having to see a dentist first. It was carried out over a very short period of time (around two months), and synthesised a large amount of disparate evidence into a succinct report. The studies came from a variety of countries including USA, UK, Australia, Norway, New Zealand, Sweden, Spain, Italy and Canada. The findings helped inform the GDC Group's decision in May 2013 in favour of deregulation and direct access for DCPs.2
So, what is a rapid review and why was it carried out in this case? There is no single definition of a rapid review; they can take a variety of forms3 but are generally considered to be literature reviews that use methods to speed up or rationalise the traditional systematic review process.4 Although high quality systematic reviews such as Cochrane reviews are generally viewed as the gold standard, they are not without their drawbacks, one of which is that they can take a minimum of six months and up to two years to complete. Rapid reviews can be carried out in a short timeframe (often one to two months), and although they are an emerging approach to synthesising knowledge, they are becoming more commonly used to provide evidence for decision makers (policy makers, patient groups and clinicians) quickly. Their choice over systematic reviews can be driven by a clinical urgency, or where there is limited time or resources to carry out a full systematic review. It seems likely that the urgency of the OFT call led to the need for a rapid review as part of the GDC's decision-making around deregulation. In addition to the speed of their production, rapid reviews tend to answer broader questions than that characteristic of the single focused systematic review question. However, rapid reviews have a number of limitations and, as a result of the streamlining that is carried out in order to speed up the review process and broaden the evidence categories that are included, there can be a loss of the results through reduced rigour and introduction of bias. Despite this concern, one comparison of recommendations from rapid reviews and systematic reviews suggested that their ‘essential conclusions …do not differ extensively’.5
This appears to be a thorough rapid review in many ways but with some significant limitations. The authors have methodically presented the data in a comprehensive distillation of findings from numerous settings, with a variety of DCPs, and against the background of many different healthcare settings. The methodologies that have been altered to expedite the review process are detailed to some extent, for example only articles in English were included, no grey literature was sought, and although the authors made ‘extensive enquires… to dental organisations worldwide’, they did not attempt to obtain articles that they could not gain immediate access to. Unfortunately there is no information on the number of non-English articles that were excluded or how many items could not be obtained, to allow assessment of the potential impact of the omission of these from the review. The language limitation may have been particularly relevant given that Norway, Sweden, Spain and Italy are among the main countries evidence was expected to come from. In addition, it was decided that literature should only be sought from 1993 onwards. One of the comments that the authors make is the lack of data from New Zealand relevant to their questions in the literature. However, in New Zealand, the School Dental Nurse Program (now known as Dental Therapy) was first established in 1923 (providing diagnostic, preventive and treatment services directly) and programme assessments are likely to have taken place before 1993.
The information on benefits and risks of direct access to DCPs around healthcare systems, and the lack of evidence for increased patient risk seem to be consistent in the same direction of benefit/lack of risk. Mechanisms currently regulating and monitoring the practice of hygienists and therapists with direct patient access are detailed in the review, including limitation of clinical remit, patient groups or settings, prescribed levels of experience, qualification or training, formal supervision (for example by a dentist such as is found in the ‘named dentist’ models in New Zealand and Alaska) and audit/inspection. Regulation and monitoring of dentists and DCPs might be developed in common rather than independently of one another. It may be purposeful that there was no review panel member with clinical dental expertise (perhaps with a view to independence), but this limitation shows in one or two areas. Although the process implications of over-referral of patients by DCPs to dentists are mentioned (increasing burden on dentists and increasing cost), there is no mention of the clinical implications of this. It is also of concern that the significant gaps in the evidence base are mentioned only once in the report and don't seem to feature at all in the conclusions. For example, despite the safety remit, the review was unable to cite robust clinical evidence on the comparative effectiveness of direct access DCPs with dentists, yet this lack of evidence is hardly mentioned.
The deregulation of dental access will be a major change for dentistry in the UK. This decision seems to have been driven by the OFT's feeling that restrictions were ‘likely to dampen competition in the dentistry market, reduce innovation, limit patient choice and lead to inefficient use of resources in the provision of dental treatment’, but it is worth remembering that this rapid review is just one piece of the evidence that the GDC took into consideration in their decision-making on direct access. Other evidence included a number of different stakeholder meetings, consultation and qualitative research carried out by Ipsos Mori. The information in the rapid report on benefits and risks of direct access around healthcare systems and the lack of evidence on increasing patient risk seem to be consistent findings through the evidence presented in the review. However, there is a significant lack of evidence for some key areas, and care should be taken that absence of evidence is not taken to mean evidence of absence. There should be careful interpretation of the data that exist against the background of what is not known. It is imperative that this new landscape in oral health care provision in the UK is monitored over time for DCPs (just as it should be for dentists), to maintain confidence in the high standard of care and levels of satisfaction that patients expect and report from their oral health care providers.6
References
http://www.oft.gov.uk/shared_oft/market-studies/Dentistry/OFT1414.pdf
Khangura S, Konnya K, Cushman, R, Grimshaw J and Moher D . Evidence summaries: the evolution of a rapid review approach. Syst Rev 2012; 1: 10.
Ganann R, Ciliska D, Thomas H . Expediting systematic reviews: methods and implications of rapid reviews. Implement Sci 2010; 5: 56.
Watt A, Cameron A, Sturm L, et al. Rapid versus full systematic reviews: validity in clinical practice? ANZ J Surg 2008; 78: 1037–1040.
Executive Summary: Adult Dental Health Survey 2009, Pub. The NHS Information Centre for health and social care ISBN 978-1-84636-492-1.
Author information
Authors and Affiliations
Additional information
Address for correspondence Steven Turner, Dental Health Services Research Unit, University of Dundee. E mail: s.turner@dundee.ac.uk
Turner S, Tripathee S, MacGillvray S. Benefits and risks of direct access to treatment by dental care professionals: A rapid evidence review. Final Report to the General Dental Council. (available on-line http://www.gdc-uk.org/newsandpublications/research/documents/finalversionofliteraturereviewondirectaccess.pdf).
Rights and permissions
About this article
Cite this article
Innes, N., Evans, D. Evidence of improved access to dental care with direct access arrangements. Evid Based Dent 14, 36–37 (2013). https://doi.org/10.1038/sj.ebd.6400926
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.ebd.6400926