Abstract
Apoptotic cell death is initiated by a morphologically homogenous entity that was considered to be non-immunogenic and non-inflammatory in nature. However, recent advances suggest that apoptosis, under certain circumstances, can be immunogenic. In particular, some characteristics of the plasma membrane, acquired at preapoptotic stage, can cause immune effectors to recognize and attack preapoptotic tumor cells. The signals that mediate the immunogenicity of tumor cells involve elements of the DNA damage response (such as ataxia telangiectasia mutated and p53 activation), elements of the endoplasmic reticulum stress response (such as eukaryotic initiation factor 2α phosphorylation), as well as elements of the apoptotic response (such as caspase activation). Depending on the signal-transduction pathway, tumor cells responding to chemotherapy or radiotherapy can express ‘danger’ and ‘eat me’ signals on the cell surface (such as NKG2D ligands, heat-shock proteins and calreticulin) or can secrete/release immunostimulatory factors (such as cytokines and high-mobility group box 1) to stimulate innate immune effectors. Likewise, the precise sequence of such events influences the ‘decision’ of the immune system to mount a cognate response or not. We therefore anticipate that the comprehension of the mechanisms governing the immunogenicity of cell death will have a profound impact on the design of anticancer therapies.
Similar content being viewed by others
Main
Eukaryotic cells can die through different pathways and with distinct morphological changes, depending on the cell type and the precise cause of cell death. On the basis of our current understanding of cell death mechanisms, the fate of dying cells can be classified according to phenomenological and ultrastructural changes.1, 2 However imperfect, the classification of cell death modalities suggests the existence of at least three different types of cell death.
Apoptosis, or type 1 cell death, is primarily defined by its morphological hallmarks,3 including chromatin condensation, nuclear fragmentation, shrinkage of the cytoplasm and formation of apoptotic bodies. Apoptosis is usually, but not exclusively, associated with caspase activation4, 5 and mitochondrial membrane permeabilization.6, 7 Apoptotic cell death is a widespread and constantly occurring mechanism in living organisms, and is essential for normal development, tissue homeostasis and numerous other physiological processes. For example, during early development, up to 50% of existing cells undergo apoptosis in the human embryonic brain.8 Because of the vital role of apoptosis in development and homeostasis, the immunological consequences of cell death have been a major focus of research in the past decade. This is largely due to the numerous pathological phenomena that have been assigned to immunogenic cell death, including excessive immune responses (that cause autoimmune and chronic inflammatory diseases) or deficient immune response (that finally cause death by failure to control microbial or neoplastic disease).
Apoptosis in cancer cells can be induced by a panoply of distinct triggers as diverse as hypoxia, shortage of nutrients or growth factors, and radiotherapy or chemotherapy. As a means of protecting the host, physiological apoptosis is rapidly and specifically recognized by phagocytic cells9 (e.g., macrophages, immature dendritic cells (DCs), endothelial cells, fibroblasts). After recognition, apoptotic bodies are silently removed by phagocytosis; this event is associated with the release of potent anti-inflammatory mediators like transforming growth factor-β (TGF-β),10 prostaglandin E211 or platelet-activating factors12 in order to avoid local inflammatory reactions. Therefore, apoptosis has been unanimously considered as an immunologically silent type of cell death.11, 12, 13, 14 However, recent studies have revealed that apoptotic tumor cells induced by anthracyclines15 or ionizing irradiation16, 17, 18 were able to induce a potent immune response in vivo, opening new questions on the pretended non-immunogenicity of apoptotic cell death. Thus, the apparent morphological uniformity of apoptosis ‘hides’ a biochemical heterogeneity in thus far that some types of apoptosis are non-immunogenic while others are immunogenic.19, 20, 21
Autophagy, or type 2 cell death, is a slow process leading to the degradation of intracellular organelles after sequestration in double-membraned vacuoles.22 During autophagy, cells usually fail to manifest signs of apoptosis such as chromatin condensation, although sometimes apoptosis can follow an initial massive autophagic vacuolization.23 Interestingly, autophagy can lead either to cell death or to cell defense against acute stress. However, it is not clear whether cells can actually die through autophagy (meaning that autophagy would be responsible for cell death) or whether cells rather die with autophagy (meaning that autophagy would accompany cell death, yet would not participate in the lethal catabolic cascade). At present, the immunological impact of autophagic cell death is not well characterized.
Necrosis, or type 3 cell death, is morphologically characterized by swelling of the cytoplasm and oncosis, leading to the rupture of the plasma membrane, and the release of swollen and damaged organelles. Unlike apoptosis, the biochemical features of necrosis are poorly understood.24 Necrosis is usually considered to be immunologically harmful, because of the sudden release of proinflammatory mediators.25 Indeed, necrotic cell death often causes the release of proinflammatory cytokines, such as interleukin-8 (IL-8), IL-10, tumor necrosis factor-α (TNF-α),26 or of terminal mediators of inflammation, like high-mobility group box 1 (HMGB1).27, 28
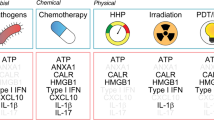
When considering normal, non-transformed cells, it is commonly assumed that the immunological consequences of cell death follow a classical dichotomy of immunogenic necrosis versus non-immunogenic (or even tolerogenic) apoptosis. This theory is supported by common sense. If each second several millions of cells succumb to apoptosis in the lifetime of an adult healthy individual, then it appears counterintuitive that apoptotic cell death would elicit an immune response.9, 29 Thus, one of the classical events associated to apoptosis is the exposure of phosphatidylserine residues on the plasma membrane leading to the silent removal of apoptotic bodies by macrophages.11, 12 Recent studies, however, have challenged this conceptual dichotomy and shed light on crucial interactions between apoptotic tumor cells and some components of the immune system.17, 30 Among these components, DCs have been shown to play a central role in the recognition of apoptotic cell death and in the initiation of an immune response, in response to various cell death-associated stimuli (Table 1). These events leading to the activation of the immune system can be mediated by the exposure of different proteins at the plasma membrane, by the release of inflammatory cytokines, or by the immunogenic properties of end-stage degradation products. The regulation of the immune response to dying cells is a crucial mechanism in living organisms. An example of excessive immune response to dying cells leading to the autoimmune pathology is systemic lupus erythematosus.31 In particular, it has been shown that apoptotic cell clearance defects related to C1q deficiency and other defects in the complement pathway lead to the development of autoantibodies to intracellular antigens bound on the surface of apoptotic cells. In contrast, escape from the immune-mediated surveillance of stressed or dying cells is one of the characteristics of tumor cells,32 leading to their uncontrolled proliferation.
This review will summarize the current state of the art of the connections between tumor cell death and the immune system, with special emphasis on cell death-related mechanisms involved in the induction of an immune response to dying tumor cells (Figure 1). We anticipate that the detailed molecular comprehension of immunogenicity of cancer cell death may open new strategies in cancer therapy.
Main steps of the induction of an antitumor immune response. Induction of tumor cell death leads to recognition of cell death by DCs. Apoptotic bodies are engulfed by APC, and tumor-derived antigens are processed and presented along with CMH and costimulatory molecules, after DC maturation, to naive T lymphocytes. This process can be amplified at different steps. Selection of immunogenic inducers of cell death allows enhancing of recognition and phagocytosis of apoptotic debris, maturation of DCs, processing and presentation of tumor-derived antigens. This leads to the induction of a cytotoxic immune response, involving CD4+ and CD8+ T lymphocytes, resulting in complete eradication of tumor cells. Additional immunotherapies targeting DCs and T lymphocytes can further enhance this immune response
Plasma Membrane Characteristics of Immunogenic Cell Death
Exposure of proteins on the plasma membrane is one of the crucial features of cell death.33 Some proteins can act as ‘eat me’ signals (such as phosphatidylserine) and facilitate the engulfment of dying cells33 by professional antigen-presenting cells (APCs) while others act as ‘don't eat me signal,34 (such as CD47) and mediate repulsion between the potential pray and its phagocyte. Such eat me and don't eat me signals exposed at the surface of dying cells are recognized by a specific set of APC receptors that in turn determine the appropriate immunological response.
Heat-shock proteins
Heat-shock proteins (HSPs) are a family of chaperone proteins that ensure the correct (re)folding of proteins in stress conditions. Although they are usually located in the intracellular compartment, at least two members of this family, HSP70 and HSP90, can be expressed at the surface of the plasma membrane and participate in the activation of the immune system. While many types of cellular stress can lead to the transcriptional and translational activation of inducible HSPs, it is not known through which mechanisms HSPs translocate to the cell surface. For the purpose of this discussion, it is important to note that many tumors overexpress HSPs, presumably as a response to a ‘stressful’ environment.35, 36 However, the mere overexpression of HSPs (which often mediate cytoprotective and apoptosis-inhibitory effects) within the cell is probably different, in immunological terms, from their presence on the cell surface.
HSP70 belongs to a family of an ATP-dependent chaperone protein that regulates the folding of newly synthesized polypeptides and the transport of these proteins to distinct subcellular compartments.37 When located inside cells, HSP70 inhibits apoptosis at multiple levels. HSP70 may interact with apoptosis protease-activating factor-1 (Apaf-1), thereby inhibiting the formation of the apoptosome (the caspase-9-activating complex) that is required for post-mitochondrial caspase activation.38 HSP70 can also inhibit caspase-independent apoptosis by blocking the translocation of apoptosis-inducing factor (AIF) into the nucleus, thereby preventing AIF-mediated chromatin condensation.39, 40 It has also been suggested that HSP70 can act at the premitochondrial level by inhibiting the proapoptotic transcription factor p5341 or stress kinases, including c-Jun N-terminal kinase 1 or ERK.42 Finally, HSP70 can block the translocation of Bax to the mitochondrial outer membrane, thereby preventing the Bax-dependent release of proapoptotic proteins from mitochondria.43
Intracellular HSP90 also exerts prominent cytoprotective functions. HSP90 can bind to numerous signaling proteins, including steroid receptors, MyoD,44 v-Src45 or Raf-1.46 When bound to these proteins, HSP90 ensures the correct conformational maturation of these receptors. HSP90 has also antiapoptotic properties, for instance by negatively effecting Apaf-1.47 HSP90 directly interacts with Apaf-1 and inhibits the formation of the apoptosome by blocking the recruitment of procaspase 9. Another role played by HSP90 in apoptosis inhibition is its interaction with phosphorylated Akt. Indeed, interaction of HSP90 and Akt leads to both promotion of cell survival through inactivation of Bad and caspase-9, and inhibition of apoptosis through NF-κB activation.48 Moreover, it has been reported that HSP90 would also have antiapoptotic properties by inhibiting the action of calpains in neuroblastoma cells exposed to ischemia/reperfusion stress.
Under some circumstances, HSP70 and HSP90 can also be found on the surface of the plasma membrane, where they can have immunostimulatory properties (Figure 2a). It has been reported that, in PC12 tumor cells, HSP70 can interact with phosphatidylserine.49 Indeed, the tight binding of HSP70 to phosphatidylserine residues on the membrane leads to an acceleration of apoptosis. Moreover, proteomic analysis of lipid rafts revealed the presence of HSP70 and HSP90 family members on the plasma membrane, along with trafficking factors.50, 51 The presence of HSP70 on the outer leaflet of the plasma membrane may be linked to its primary chaperone and transport function.
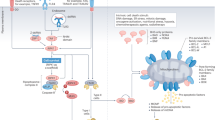
Overview of the main immunogenic determinants of dying tumor cells. (a) Plasma membrane characteristics of immunogenic cell death. Upon apoptotic cell death induced by anthracyclines or γ-irradiation, calreticulin is translocated to the membrane, thereby dictating the immunogenicity of tumor cell death by determining the phagocytosis by DCs. During tumor cell death, HSP70 and HSP90 can be transferred to the plasma membrane, and cross-present tumor-derived peptides to CD8+ T cells, leading to a cytotoxic response. HSP70 and HSP90 also stimulate NK cell lysis, through NKG2A ligands. In response to HSP family members, DCs are able to maturate and release proinflammatory cytokines. (b) Inflammatory cytokines released from dying cells. Necrotic cell death is associated with the release of numerous proinflammatory cytokines, including HSP family members, uric acid, which stimulates DCs and increases cytotoxic response, IL-6, IL-8, IL-10, TNF-α, and also HMGB1, which binds to TLR4, and regulates antigen processing and presentation. Of note, some of these components, such as HMGB1, can also be released during apoptotic cell death, leading to the induction of an immune response. (c) End-stage degradation products with proinflammatory properties. During late stages of cell death, cellular components with proinflammatory properties can be released from the cell debris. These include RNA molecules, which are recognized by TLR3 and lead to DC stimulation, DNA molecules, which interact with TLR9, or nucleotides. Importantly, late-stage apoptosis can be associated with the induction of PTX3, which interacts with the immunological synapse formed by DCs and apoptotic bodies. PTX3 modulates the immune response triggered by dying cells. (d) P53 activation in cancer cells and its immunological consequences. The DNA damage response pathway includes the activation of the protein p53, which leads to tumor cell apoptosis, but also to stimulation of the immune system through expression of NKG2D ligands, triggering NK-mediated lysis. Activation of p53 is also associated with the induction of tumor cell senescence, which is accompanied by secretion of various chemoattractants, and upregulation of inflammatory cytokines
When present at the plasma membrane, HSP70 and, to a lesser extent, HSP9052 are major determinants of the immunogenicity of stressed or dying cells. Reportedly, HSP70 and HSP90 play a major role in cross-presentation of tumor-derived antigenic peptides on major histocompatibility complex (MHC) class I molecules, leading to specific CD8+ T-cell responses.53, 54 It has been shown in mouse models that HSPs were essential for the cross-presentation of antigenic peptides by MHC class I.55, 56 The recognition of the HSP–peptide complex by DC is mediated by a complex formed by Toll-like receptor 4 (TLR4) and CD14.57, 58 TLR4 is also involved in intracellular antigen processing and presentation, as well as in the activation of the NF-κB pathway in DC.57, 58 This latter activation, which is perceived as a danger signal, results in the release of proinflammatory cytokines (TNF-α, IL-1β, IL-12, IL-6 and granulocyte macrophage colony-stimulating factor (GM-CSF) and hence in the cytokine-mediated activation of the host immune system.59, 60
In line with its immunostimulatory properties, HSP70 has also been shown to promote maturation of DCs, via the upregulation of CD86 and CD40.61 HSPs present on the surface of stressed or dying cells can interact with a number of receptors present on the surface of APCs. Thus, it has been suggested that HSP70 could interact with CD40, or scavenger receptors LOX-1 or SR-A.62 Recently, HSP90 has also been shown to directly bind to the CD91 receptor on APCs.63
Interestingly, HSP family members also stimulate another cell type of the innate immune system, the natural killer (NK) cells. The activity of NK cells is tightly regulated by means of inhibitory or activating receptors, including killer cell immunoglobulin-like receptors, immunoglobulin-like transcript receptors or C-type lectin receptors. The presence of HSP family members on the surface of stressed or dying cells leads to the activation of NK cells, by preventing the recognition of HLA-E peptide complexes by the inhibitory receptor complex CD94/NKG2A.64 As a result, stressed cells that bear HSP70 at their surface are efficiently destroyed by NK cells. HSP70 also plays a role in activating NK cells through their CD94 receptor. Indeed, HSP70 present on tumor cells can induce NK cell activation via its C-terminal substrate binding domain.65, 66 This NK activation could be partially prevented by blocking CD94.67
These mechanisms have a considerable importance for the recognition and destruction of tumor cells by the immune system. Systematic analyses of human tumors revealed that a large number of tumor cells were expressing HSP at their plasma membrane.68 This includes colon, pancreas, breast, head and neck tumors, and acute myeloid leukemia cells. Moreover, the expression of HSP could be increased when distinct cytotoxic stress69 was applied to tumor cells, leading to enhanced NK-mediated killing of malignant cells.
Recently, the role of HSP90 in increasing immunogenicity of tumor cells has been highlighted. In 29 patients with colorectal carcinoma, administration of autologous tumor-derived HSP90 resulted in increase of NKG2D or NKp46 receptors on NK cells, correlating with increased cytotoxic activity. In human myeloma, a recent study showed that treatment by bortezomib, a proteasome inhibitor, specifically induced apoptosis-associated exposure of HSP90 on the surface of tumor cells, whereas γ-irradiation or dexamethasone-induced apoptosis failed to do so. When tumor cell death was induced by bortezomib, apoptosis was associated with an increased DC-mediated immunogenicity as assessed by the phenotypic maturation of DC and their ability to activate human T cells in vitro.70
Altogether, these results suggest that the presence of proteins from the HSP family at the plasma membrane facilitates the recognition of stressed or dying cells, leading to their elimination by the immune system.
Calreticulin
Calreticulin (CRT) is a Ca2+-binding protein with a high capacity of buffering Ca2+ yet a low affinity for this divalent ion. CRT is mainly located in the lumen of the endoplasmic reticulum (ER) and is involved in the modulation of Ca2+ signaling and Ca2+ homeostasis.71, 72, 73 It chaperones several proteins and interacts in particular with the disulfide isomerase Erp57.74 The function of CRT in the cytoplasm is not entirely clear. However, CRT has been suggested to regulate nuclear protein transport,75 signaling via nuclear steroid receptors and integrin. As this is true for HSP, CRT can be found on the surface of stressed and dying cells. Again, the mechanisms accounting for its translocation from inside the cell (endo-CRT) to the cell surface are elusive.
When bound to the plasma membrane of cells upon apoptosis initiation, CRT is a crucial determinant of the phagocytosis of dying tumor cells by macrophages and DCs17 (Figure 1a). Moreover, cells that undergo apoptosis while lacking CRT are able to die unobstructed, but are not efficiently removed by phagocytes.33 Recently, CRT has been implicated in the immunogenicity of apoptosis elicited by anthracyclines or γ-irradiation.18 CT26 colon cancer or MCA205 fibrosarcoma cells translocate CRT to the cell surface after treatment with some cell death inducers (in particular, anthracyclines, γ-irradiation) or inhibitors of the PP1/GADD34 complex.16, 17, 18 In addition, CRT translocates to the cell surface of circulating tumor cells, in response to the intravenous injection of anthracyclines, as it has been shown for patients with acute myeloid leukemia.76
In response to anthracyclines or ionizing irradiation, CRT exposure occurs before the first morphological signs of apoptosis-related modifications and before cells expose phosphatidylserine residues on the outer leaflet of the plasma membrane. One similarity between the pathway elicited by anthracyclines and that elicited by PP1/GADD34 inhibitors is the phosphorylation of eukaryotic initiation factor 2α (eIF2α), a protein that is known to be phosphorylated as a result of the unfolded protein response of the ER.28, 77 This suggests that pleiotropic responses conditioned by eIF2α phosphorylation at the level of the ER control CRT exposure, which in turn determines the immunogenicity of cell death. However, direct induction of ER stress by tunicamycin or brefeldin A (which both induce eIF2α phosphorylation) does not provoke CRT exposure,17 indicating that eIF2α phosphorylation is required but not sufficient for CRT translocation to the plasma membrane surface. Caspase activation is also required for CRT exposure induced by anthracyclines because treatment with the pan-caspase inhibitor Z-VAD-fmk or transfection with the baculovirus IAP p35 (which is a direct and universal caspase inhibitor) prevents CRT exposure. At present, it is not known which caspase(s) are involved in the signal-transduction pathway that stimulates CRT exposure before the cells manifest signs of apoptosis.
When associated with apoptosis, CRT translocation is responsible for the induction of a potent antitumor immune response both in vitro and in vivo. This response is mediated by the rapid recognition and phagocytosis of tumor cells by DCs, leading to cytotoxic T-cell response both in vitro and in vivo. The immunogenicity of CRT expressing apoptotic cells could be abolished by CRT inhibition with blocking antibodies, or by CRT knockdown with specific small interfering RNAs.17, 18 Moreover, the immunogenicity of apoptotic cells that did not express CRT at their surface could be dramatically enhanced by the adsorption of recombinant CRT protein to the cell surface, underlining the pivotal role of this protein in determining the immunogenicity of tumor cell death.
Eat me signals versus peptide chaperoning as a mechanism for conferring immunogenicity
Distinct classes of chaperones including HSP70, HSP90 and CRT can act as eat me signals (see above) or may constitute a specific source of tumor-specific peptide antigen.61, 64 Thus, HSP70, HSP90 or CRT purified from tumors have been shown to elicit specific immune responses when injected into mice.78
Although CRT can interact with tumor-specific immunogenic peptides (as shown by Basu and Srivastava79), we believe that the immunogenicity of surface CRT exposure cannot be explained because CRT would act as a specific vehicle for transporting antigenic tumor peptides from the tumor to the APCs. Thus, exogenous addition of recombinant CRT protein (which has been produced in insect cells and hence cannot contain tumor-derived antigenic peptides) is sufficient to restore the immunogenicity of non-immunogenic apoptosis. We have performed additional experiments to address the possibility that the association of CRT protein with tumor-derived peptides might mediate the antitumor immune response. First, we provoked immunogenic cell death by treatment of cells with recombinant CRT protein plus mitomycin C or etoposide. Then, we vaccinated syngeneic mice, either with intact tumor cells or with their lysate (which was produced by freeze thaw cycles in conditions that did not lead to CRT degradation). Only intact tumor cells, but not their lysate, were immunogenic, suggesting that the mere presence of CRT (which could be associated with tumor-specific peptides) is not sufficient to elicit antitumor immunity. Second, we treated tumor cells with inhibitors of the proteasome, which according to Blachere et al.30 is required for the optimal generation of immunogenic peptides in dying cells and which induce a non-immunogenic variant of cell death. Addition of recombinant CRT protein still could restore the immunogenicity of proteasome inhibitor-induced cell death. This observation provides an argument in favor of the idea that the association of CRT with antigenic peptides on the surface of tumor cells is not responsible for the adjuvant effect of CRT. Rather, the effect of CRT would be mediated by its capacity to stimulate the uptake of tumor cells by DCs.
Inflammatory Cytokines Released from Dying Cells
Dying tumor cells can release proinflammatory cytokines during their agony, and these factors can be instrumental in eliciting an immune response (Figure 2b). It is generally assumed that necrotic cell death would be the type of cell death that is associated with the indiscriminate extracellular release of soluble intracellular constituents through the permeabilized plasma membrane.80 Indeed, necrotic cells are able to act on fibroblasts, macrophages and DCs, activating NF-κB and inducing the expression of genes that are involved in inflammatory responses and tissue repair,81 perhaps in a TLR2-dependent manner.82 Such genes include the cytokine-induced neutrophil chemoattractant (KC) and macrophage inflammatory protein-2, metalloproteinase 3 and vascular endothelial growth factor,83 but also TNF-α, IL-8, IL 10, and IL-6.29 This general proinflammatory feature seems to be absent from apoptotic cell death.29 Among the numerous components released into the extracellular matrix during necrotic cell death, some components mediate important immunological effects. Interestingly, necrotic cells release HSP (see above) as well as uric acid,84 which also can elicit proinflammatory effects through TLR285 or by stimulating the NALP3 inflammasome.86
HMGB1
When cells succumb to necrosis, they release HMGB1, which is well known for its proinflammatory properties27 (Figure 2b). HMGB1 is a non-histone chromatin-binding protein that influences transcription and other nuclear functions.87 HMGB1 is either secreted actively from inflammatory cells28 or passively released as a soluble molecule from necrotic cells.27 Once present in the extracellular space, HMGB1 can signal tissue injury and initiate inflammatory response through binding to a range of receptors, including the receptor for advanced glycosylation end products (RAGE), TLR2 or TLR4.88, 89 HMGB1 is a terminal mediator of sepsis28 and can induce hepatic injury during ischemia/reperfusion in a TLR4-dependent manner.90
HMGB1 release has been considered as a potential way of inducing an immune response against dying tumor cells undergoing necrosis. However, several studies showed that necrotic cells were unable to trigger an immune response91, 92 when injected in vivo, in contrast to the initial expectations. Recently, it has been found that tumor cells that undergo apoptosis in vitro, in response to anthracyclines, could mediate a potent antitumor vaccination effect when they were injected subcutaneously into syngeneic immunogenic mice. This antitumor vaccination effect did not require any addition of immunostimulatory compounds (such as adjuvants) and conferred long-term protection against further challenge with live tumor cells.15 This system of antitumor vaccination involves the obligatory recognition and phagocytosis of dying tumor cells by DCs, because depletion of DCs in vivo abolishes the antitumor immune response.15, 93 DCs then process and present tumor-derived antigens to cytotoxic T cells, which in turn mediate a cytolytic response against tumor cells.
Importantly, the immune response against dying tumor cells involves the release of HMGB1 by dying tumor cells.93 Once released, HMGB1 binds to TLR4 on DCs and controls the initiation of the immune response through processing and presentation of tumor-derived antigens.93 TLR4 has been shown to control antigen presentation by inhibiting fusion between phagosomes and lysosomes.94, 95 When HMGB1 is blocked by neutralizing antibodies, or when its expression in tumor cells is silenced by RNA interference, the initiation of the immune response is blunted both in vitro and in vivo. We found that mouse or human cells dying in response to various lethal stimuli in vitro released HMGB1 into the extracellular medium at a late stage, when apoptotic bodies were formed and cells underwent secondary necrosis. After extracellular release, HMGB1 binds to TLR4 on DCs and plays an indispensable role in the DC-dependent T-cell activation in response to dying tumor cells.93 Apparently, HMGB1 has to bind to TLR4 to allow for optimal antigen processing in DCs. When either HMGB1 or TLR4 is absent from the system, dying tumor cells are still normally engulfed by DCs. However, the phagosomes containing tumor cell material rapidly fuse with lysosomes, meaning that the phagocytic cargo is degraded rather then presented in the form of antigenic peptides that bind to MHC molecules. This defect in antigen presentation can be corrected by inhibiting lysosomes, for instance with chloroquine of bafilomycin A1.
The relevance of these findings has also been addressed in humans. Breast cancer patients bearing a TLR4 allele (Asp299Gly variant96) that reduces the affinity of TLR4 for HMGB1 demonstrated a markedly increased incidence of metastases after primary treatment when compared to those patients bearing the normal TRL4 allele.93 DCs from patients bearing the deficient TLR4 allele also are poor presenters of antigen from dying tumor cells unless their lysosomes are inhibited with chloroquine.93
In addition to interacting with TLR2 and TLR4, HMGB1, combined with self-DNA, could stimulate the production of interferon-α by stimulating TLR9.97, 98 Moreover, a complex associating HMGB1 and DNA can bind the RAGE receptor.27 In turn, this complex stimulates intracellular TLR9 and activates IFN-α secretion through a MyD88-dependent pathway.98
The question whether HMGB1 is released during apoptotic cell death has been a matter of debate ever since. Primarily, it was suggested that HMGB1 was released by necrotic, but not by apoptotic cells, even at late apoptosis stages. Two findings have challenged this question. First, many investigators have found that nuclear DNA is released in a time-dependent manner during apoptosis.99 Second, binding of HMGB1 to DNA was increased during apoptosis, in line with the fact that late-stage apoptotic cells can release both DNA and HMGB1. Recent studies98, 100 have confirmed that HMGB1 could also be released from apoptotic tumor cells, at least at late stages of the lethal process, and that this release could be blocked by the pan-caspase inhibitor Z-VAD-fmk, which delays secondary necrosis.
The difference in the immunogenicity of primary necrosis (which is non-immunogenic) versus secondary necrosis (necrosis after apoptosis, which can be immunogenic) might reside in the difference of the components that are released after loss of membrane integrity. As secondary necrosis follows apoptosis, caspase activation may have dismantled some of the cell's major immunosuppressive components, and/or might facilitate the release of immunostimulatory agents. Future investigation will have to identify caspase substrates that regulate the immune response, once they come into contact with innate immune effectors.
End-stage Degradation Products with Proinflammatory Properties
Like early stages of cell death (for instance, CRT exposure at the plasma membrane during apoptotic cell death), end-stage degradation of cells could confer immunostimulation (Figure 2c). Indeed, plasma membrane collapse during primary or secondary necrosis is associated with the release of RNA molecules, which interact with TLR3 on DCs,101 with the release of double-stranded DNA,102 which stimulates both macrophages and DCs, as well as that of nucleotides, leading to the maturation of DCs103 along with the activation of the NF-κB pathway.104
End-stage degradation products from dying tumor cells are able to modulate their recognition by the immune system through a family of innate immunity receptors, the pentraxins.105 Short pentraxins, like C-reactive protein or serum amyloid protein, are secreted in response to IL-6 and play an important role in the clearance of cellular debris. Late-stage apoptotic cells stimulate mature DCs (but not immature DCs) to produce the long pentraxin, pentraxin-3 (PTX3).106 Once secreted, PTX3 binds to the membranes of apoptotic cells and maturing DCs. When it is recruited to this immunological synapse, PTX3 modulates the immune response to late apoptotic cells. Indeed, when apoptotic murine fibroblasts expressing MelanA/MART1 are cultured with DCs, such DCs are able to activate specific CD8 T cell through cross-presentation on tumor-derived antigen. However, addition of PTX3 directly inhibits T-cell activation, by inhibiting the cross-presentation of tumor-derived antigens to cytotoxic T cells.107
P53 Activation in Cancer Cells and Its Immunological Consequences
In response to oncogene-driven DNA damage, ionizing irradiation or chemotherapy, a specific pathway, called the DNA damage response pathway, can be activated in tumor cells.108, 109 This response involves, among others, the proteins ataxia telangiectasia mutated (ATM, which detects DNA damage), checkpoint kinase-1 (Chk1, which mediates cell cycle arrest) and p53 (which mediates cell cycle arrest and apoptosis). In addition of inducing apoptosis of transformed cells,109 the activation of the DNA damage response can also activate the expression of ligands of the activating NK and T-cell receptors NKG2D110 (Figure 2d). Tumor cells that have activated the DNA damage response pathway express NKGD2 ligands, such as the MHC class I polypeptide-related sequence A or the retinoic acid early transcript 1, in an ATM- and Chk1 (but not p53)-dependent manner. Such NKG2D ligands expressing cancer cells can be efficiently recognized by NK, NKT and some cytolytic T cells, meaning that the tumor cells are actively destroyed. The activation of the DNA damage response pathway therefore links the DNA damage response to the immune-mediated eradication of tumor cells.
Recently, evidence for a link between p53 and immune-mediated eradication of tumor cells has been described. In a mouse model of hepatocellular carcinoma, restoration of p53 expression in vivo, in the tumor cells, demonstrated a rapid regression and clearance of cancers.111 The putative mechanism involved in this process is the p53-mediated induction of senescence in tumor cells. Senescence has been associated with the upregulation of inflammatory cytokines such as MCP-1, IL-1β, IL-15 or TLR4.112 In hepatocellular carcinoma, p53 reactivation induced a marked increase in proinflammatory cytokines, including chemoattractants for macrophages (Csf1 and Mcp1), neutrophils (Cxcl1) or NK cells (IL-15).111 An increase in inflammatory transcripts (NCF2 and NCF4 for neutrophils, MgL2 and MSR2 for macrophages and KLRB1 and KLRD1 for NK cells) was also noted. In this model, the participation of the innate immune system was shown to be determinant for the efficient clearance of senescent tumor cells because the removal of T cells, NK cells or granulocytes abolished the therapeutic potential of p53 reactivation in vivo.
These results show that the protective activation of p53 in transformed cells can lead to intrinsic, but also to extrinsic, immune-mediated removal of abnormal cells. This mechanism has a major relevance in cancer immunosurveillance, but also in cancer treatment, as it enhances the recognition and elimination of cancer cells by the immune system.
Conclusion
One of the hallmarks of cancer cells is the resistance to cell death.113 Logically, one of the first strategies in the fight against cancer has been to restore the sensibility to death. It has been suggested that cancer cells also have the capacity to evade the surveillance by the immune system.32 Therefore, it would be of highest therapeutic value to restore the immune recognition of poorly immunogenic cancer cells. One particularly attractive solution might consist in combining two approaches, namely restoration of cell death and restoration of tumor immunosurveillance and to take advantage of the immunogenic properties of cancer cell death (Figure 3). This may be achieved by favoring chemotherapies that induce immunogenic cell death, and by avoiding chemotherapies that induce immunologically silent cell death or that mediate immunosuppressive side effects, such as myelosuppression or thymolysis. In addition, active strategies for stimulating the immune response should be employed. This includes the use of drugs with immunostimulatory effects114 and the manipulation of cell death to ensure optimal immunogenicity (surface exposure of HSP and CRT, release of HMGB1, inhibition of pentraxins). In addition, it may be useful to screen patients for genetic or acquitted defects that may compromise the immune response against dying tumor cells.
Proposed strategies for efficient immunochemotherapy. The concept of immunochemotherapy is the association of both direct cytotoxic drugs effects and indirect immune-mediated cytotoxic effects. This causes the generation of an immunogenic tumor cell death, through induction of calreticulin (e.g., anthracyclines), or HSP family members at the plasma membrane (e.g., bortezomib), through the release of inflammatory mediators, such as chemoattractants, proinflammatory cytokines or HMGB1, through the release of late-stage cell death mediators or through the activation of p53. This also supposes the relative preservation of the immune system, and the elimination of inhibitory components such as PTX3 as a mandatory step for the induction of an antitumor immune response. Upon immunogenic tumor cell death, the immune system generates an antitumor immune response that will permanently eradicate remaining tumor cells
More than the meaning of life, the meaning of death has become a crucial question for biomedical research. The recent advances in the understanding of biochemical mechanisms accounting for the immunogenicity of cell death have potential implications in many fields of medicine, including cancer biology, virology and autoimmunity.
Abbreviations
- AIF:
-
apoptosis-inducing factor
- Apaf-1:
-
apoptosis protease-activating factor-1
- APC:
-
antigen-presenting cell
- CRT:
-
calreticulin
- DC:
-
dendritic cell
- ER:
-
endoplasmic reticulum
- HMGB1:
-
high-mobility group box 1
- HSP:
-
heat-shock protein
- IL:
-
interleukin
- MHC:
-
major histocompatibility complex
- PTX3:
-
pentraxin-3
- RAGE:
-
receptor for advanced glycosylation end products
- TLR4:
-
Toll-like receptor 4
References
Kroemer G, El-Deiry WS, Golstein P, Peter ME, Vaux D, Vandenabeele P et al. Classification of cell death: recommendations of the Nomenclature Committee on Cell Death. Cell Death Differ 2005; 12 (Suppl 2): 1463–1467.
Galluzzi L, Maiuri MC, Vitale I, Zischka H, Castedo M, Zitvogel L et al. Cell death modalities: classification and pathophysiological implications. Cell Death Differ 2007; 14: 1237–1243.
Kerr JF, Wyllie AH, Currie AR . Apoptosis: a basic biological phenomenon with wide-ranging implications in tissue kinetics. Br J Cancer 1972; 26: 239–257.
Kroemer G, Martin SJ . Caspase-independent cell death. Nat Med 2005; 11: 725–730.
Kroemer G, Galluzzi L, Brenner C . Mitochondrial membrane permeabilization in cell death. Physiol Rev 2007; 87: 99–163.
Brenner C, Kroemer G . Apoptosis. Mitochondria – the death signal integrators. Science 2000; 289: 1150–1151.
Green DR, Kroemer G . The pathophysiology of mitochondrial cell death. Science 2004; 305: 626–629.
de la Rosa EJ, de Pablo F . Cell death in early neural development: beyond the neurotrophic theory. Trends Neurosci 2000; 23: 454–458.
Savill J, Dransfield I, Gregory C, Haslett C . A blast from the past: clearance of apoptotic cells regulates immune responses. Nat Rev Immunol 2002; 2: 965–975.
Chen W, Frank ME, Jin W, Wahl SM . TGF-beta released by apoptotic T cells contributes to an immunosuppressive milieu. Immunity 2001; 14: 715–725.
Fadok VA, Bratton DL, Konowal A, Freed PW, Westcott JY, Henson PM . Macrophages that have ingested apoptotic cells in vitro inhibit proinflammatory cytokine production through autocrine/paracrine mechanisms involving TGF-beta, PGE2, and PAF. J Clin Invest 1998; 101: 890–898.
Savill J, Fadok V . Corpse clearance defines the meaning of cell death. Nature 2000; 407: 784–788.
Voll RE, Herrmann M, Roth EA, Stach C, Kalden JR, Girkontaite I . Immunosuppressive effects of apoptotic cells. Nature 1997; 390: 350–351.
Steinman RM, Turley S, Mellman I, Inaba K . The induction of tolerance by dendritic cells that have captured apoptotic cells. J Exp Med 2000; 191: 411–416.
Casares N, Pequignot MO, Tesniere A, Ghiringhelli F, Roux S, Chaput N et al. Caspase-dependent immunogenicity of doxorubicin-induced tumor cell death. J Exp Med 2005; 202: 1691–1701.
Obeid M, Panaretakis T, Joza N, Tufi R, Tesniere A, van Endert P et al. Ecto-calreticulin in immunogenic chemotherapy. Immunol Rev 2007 (in press).
Obeid M, Tesniere A, Ghiringhelli F, Fimia GM, Apetoh L, Perfettini JL et al. Calreticulin exposure dictates the immunogenicity of cancer cell death. Nat Med 2007; 13: 54–61.
Obeid M, Panaretakis T, Joza N, Tufi R, Tesniere A, van Endert P et al. Calreticulin exposure is required for the immunogenicity of γ-irradiation and UVC light-induced apoptosis. Cell Death Differ 2007; 14: 1848–1850.
Albert ML, Sauter B, Bhardwaj N . Dendritic cells acquire antigen from apoptotic cells and induce class I-restricted CTLs. Nature 1998; 392: 86–89.
Zitvogel L, Casares N, Pequignot MO, Chaput N, Albert ML, Kroemer G . Immune response against dying tumor cells. Adv Immunol 2004; 84: 131–179.
Banchereau J, Steinman RM . Dendritic cells and the control of immunity. Nature 1998; 392: 245–252.
Maiuri MC, Zalckvar E, Kimchi A, Kroemer G . Self-eating and self-killing: crosstalk between autophagy and apoptosis. Nat Rev Mol Cell Biol 2007; 8: 41–52.
Gonzalez-Polo RA, Boya P, Pauleau AL, Jalil A, Larochette N, Souquere S et al. The apoptosis/autophagy paradox: autophagic vacuolization before apoptotic death. J Cell Sci 2005; 118 (Part 14): 3091–3102.
Golstein P, Kroemer G . Cell death by necrosis: towards a molecular definition. Trends Biochem Sci 2007; 32: 37–43.
Vakkila J, Lotze MT . Inflammation and necrosis promote tumour growth. Nat Rev Immunol 2004; 4: 641–648.
Fadok VA, Bratton DL, Guthrie L, Henson PM . Differential effects of apoptotic versus lysed cells on macrophage production of cytokines: role of proteases. J Immunol 2001; 166: 6847–6854.
Scaffidi P, Misteli T, Bianchi ME . Release of chromatin protein HMGB1 by necrotic cells triggers inflammation. Nature 2002; 418: 191–195.
Wang H, Bloom O, Zhang M, Vishnubhakat JM, Ombrellino M, Che J et al. HMG-1 as a late mediator of endotoxin lethality in mice. Science 1999; 285: 248–251.
Krysko DV, D'Herde K, Vandenabeele P . Clearance of apoptotic and necrotic cells and its immunological consequences. Apoptosis 2006; 11: 1709–1726.
Blachere NE, Darnell RB, Albert ML . Apoptotic cells deliver processed antigen to dendritic cells for cross-presentation. PLoS Biol 2005; 3: e185.
Walport MJ . Lupus, DNase and defective disposal of cellular debris. Nat Genet 2000; 25: 135–136.
Zitvogel L, Tesniere A, Kroemer G . Cancer despite immunosurveillance: immunoselection and immunosubversion. Nat Rev Immunol 2006; 6: 715–727.
Gardai SJ, Bratton DL, Ogden CA, Henson PM . Recognition ligands on apoptotic cells: a perspective. J Leukoc Biol 2006; 79: 896–903.
Kharitonenkov A, Chen Z, Sures I, Wang H, Schilling J, Ullrich A . A family of proteins that inhibit signalling through tyrosine kinase receptors. Nature 1997; 386: 181–186.
Jaattela M . Over-expression of hsp70 confers tumorigenicity to mouse fibrosarcoma cells. Int J Cancer 1995; 60: 689–693.
Garrido C, Fromentin A, Bonnotte B, Favre N, Moutet M, Arrigo AP et al. Heat shock protein 27 enhances the tumorigenicity of immunogenic rat colon carcinoma cell clones. Cancer Res 1998; 58: 5495–5499.
Shi Y, Thomas JO . The transport of proteins into the nucleus requires the 70-kilodalton heat shock protein or its cytosolic cognate. Mol Cell Biol 1992; 12: 2186–2192.
Beere HM, Wolf BB, Cain K, Mosser DD, Mahboubi A, Kuwana T et al. Heat-shock protein 70 inhibits apoptosis by preventing recruitment of procaspase-9 to the Apaf-1 apoptosome. Nat Cell Biol 2000; 2: 469–475.
Creagh EM, Carmody RJ, Cotter TG . Heat shock protein 70 inhibits caspase-dependent and -independent apoptosis in Jurkat T cells. Exp Cell Res 2000; 257: 58–66.
Ravagnan L, Gurbuxani S, Susin SA, Maisse C, Daugas E, Zamzami N et al. Heat-shock protein 70 antagonizes apoptosis-inducing factor. Nat Cell Biol 2001; 3: 839–843.
Wadhwa R, Yaguchi T, Hasan MK, Mitsui Y, Reddel RR, Kaul SC . Hsp70 family member, mot-2/mthsp70/GRP75, binds to the cytoplasmic sequestration domain of the p53 protein. Exp Cell Res 2002; 274: 246–253.
Lee JS, Lee JJ, Seo JS . HSP70 deficiency results in activation of c-Jun N-terminal kinase, extracellular signal-regulated kinase, and caspase-3 in hyperosmolarity-induced apoptosis. J Biol Chem 2005; 280: 6634–6641.
Stankiewicz AR, Lachapelle G, Foo CP, Radicioni SM, Mosser DD . Hsp70 inhibits heat-induced apoptosis upstream of mitochondria by preventing Bax translocation. J Biol Chem 2005; 280: 38729–38739.
Nathan DF, Lindquist S . Mutational analysis of Hsp90 function: interactions with a steroid receptor and a protein kinase. Mol Cell Biol 1995; 15: 3917–3925.
Hartson SD, Matts RL . Association of Hsp90 with cellular Src-family kinases in a cell-free system correlates with altered kinase structure and function. Biochemistry 1994; 33: 8912–8920.
Wartmann M, Davis RJ . The native structure of the activated Raf protein kinase is a membrane-bound multi-subunit complex. J Biol Chem 1994; 269: 6695–6701.
Pandey P, Saleh A, Nakazawa A, Kumar S, Srinivasula SM, Kumar V et al. Negative regulation of cytochrome c-mediated oligomerization of Apaf-1 and activation of procaspase-9 by heat shock protein 90. EMBO J 2000; 19: 4310–4322.
Ozes ON, Mayo LD, Gustin JA, Pfeffer SR, Pfeffer LM, Donner DB . NF-kappaB activation by tumour necrosis factor requires the Akt serine-threonine kinase. Nature 1999; 401: 82–85.
Arispe N, Doh M, Simakova O, Kurganov B, De Maio A . Hsc70 and Hsp70 interact with phosphatidylserine on the surface of PC12 cells resulting in a decrease of viability. FASEB J 2004; 18: 1636–1645.
Foster LJ, De Hoog CL, Mann M . Unbiased quantitative proteomics of lipid rafts reveals high specificity for signaling factors. Proc Natl Acad Sci USA 2003; 100: 5813–5818.
Li N, Shaw AR, Zhang N, Mak A, Li L . Lipid raft proteomics: analysis of in-solution digest of sodium dodecyl sulfate-solubilized lipid raft proteins by liquid chromatography-matrix-assisted laser desorption/ionization tandem mass spectrometry. Proteomics 2004; 4: 3156–3166.
Udono H, Srivastava PK . Comparison of tumor-specific immunogenicities of stress-induced proteins gp96, hsp90, and hsp70. J Immunol 1994; 152: 5398–5403.
Doody AD, Kovalchin JT, Mihalyo MA, Hagymasi AT, Drake CG, Adler AJ . Glycoprotein 96 can chaperone both MHC class I- and class II-restricted epitopes for in vivo presentation, but selectively primes CD8+ T cell effector function. J Immunol 2004; 172: 6087–6092.
Schild H, Arnold-Schild D, Lammert E, Rammensee HG . Stress proteins and immunity mediated by cytotoxic T lymphocytes. Curr Opin Immunol 1999; 11: 109–113.
Srivastava PK, Menoret A, Basu S, Binder RJ, McQuade KL . Heat shock proteins come of age: primitive functions acquire new roles in an adaptive world. Immunity 1998; 8: 657–665.
Binder RJ, Blachere NE, Srivastava PK . Heat shock protein-chaperoned peptides but not free peptides introduced into the cytosol are presented efficiently by major histocompatibility complex I molecules. J Biol Chem 2001; 276: 17163–17171.
Asea A, Rehli M, Kabingu E, Boch JA, Bare O, Auron PE et al. Novel signal transduction pathway utilized by extracellular HSP70: role of Toll-like receptor (TLR) 2 and TLR4. J Biol Chem 2002; 277: 15028–15034.
Asea A, Kraeft SK, Kurt-Jones EA, Stevenson MA, Chen LB, Finberg RW et al. HSP70 stimulates cytokine production through a CD14-dependant pathway, demonstrating its dual role as a chaperone and cytokine. Nat Med 2000; 6: 435–442.
Wang Y, Kelly CG, Singh M, McGowan EG, Carrara AS, Bergmeier LA et al. Stimulation of Th1-polarizing cytokines, C-C chemokines, maturation of dendritic cells, and adjuvant function by the peptide binding fragment of heat shock protein 70. J Immunol 2002; 169: 2422–2429.
Lehner T, Wang Y, Whittall T, McGowan E, Kelly CG, Singh M . Functional domains of HSP70 stimulate generation of cytokines and chemokines, maturation of dendritic cells and adjuvanticity. Biochem Soc Trans 2004; 32 (Part 4): 629–632.
Singh-Jasuja H, Toes RE, Spee P, Munz C, Hilf N, Schoenberger SP et al. Cross-presentation of glycoprotein 96-associated antigens on major histocompatibility complex class I molecules requires receptor-mediated endocytosis. J Exp Med 2000; 191: 1965–1974.
Becker T, Hartl FU, Wieland F . CD40, an extracellular receptor for binding and uptake of Hsp70–peptide complexes. J Cell Biol 2002; 158: 1277–1285.
Binder RJ, Srivastava PK . Essential role of CD91 in re-presentation of gp96-chaperoned peptides. Proc Natl Acad Sci USA 2004; 101: 6128–6133.
Hickman-Miller HD, Hildebrand WH . The immune response under stress: the role of HSP-derived peptides. Trends Immunol 2004; 25: 427–433.
Botzler C, Li G, Issels RD, Multhoff G . Definition of extracellular localized epitopes of Hsp70 involved in an NK immune response. Cell Stress Chaperones 1998; 3: 6–11.
Multhoff G, Mizzen L, Winchester CC, Milner CM, Wenk S, Eissner G et al. Heat shock protein 70 (Hsp70) stimulates proliferation and cytolytic activity of natural killer cells. Exp Hematol 1999; 27: 1627–1636.
Gross C, Schmidt-Wolf IG, Nagaraj S, Gastpar R, Ellwart J, Kunz-Schughart LA et al. Heat shock protein 70-reactivity is associated with increased cell surface density of CD94/CD56 on primary natural killer cells. Cell Stress Chaperones 2003; 8: 348–360.
Shin BK, Wang H, Yim AM, Le Naour F, Brichory F, Jang JH et al. Global profiling of the cell surface proteome of cancer cells uncovers an abundance of proteins with chaperone function. J Biol Chem 2003; 278: 7607–7616.
Gehrmann M, Marienhagen J, Eichholtz-Wirth H, Fritz E, Ellwart J, Jaattela M et al. Dual function of membrane-bound heat shock protein 70 (Hsp70), Bag-4, and Hsp40: protection against radiation-induced effects and target structure for natural killer cells. Cell Death Differ 2005; 12: 38–51.
Spisek R, Charalambous A, Mazumder A, Vesole DH, Jagannath S, Dhodapkar MV . Bortezomib enhances dendritic cell (DC)-mediated induction of immunity to human myeloma via exposure of cell surface heat shock protein 90 on dying tumor cells: therapeutic implications. Blood 2007; 109: 4839–4845.
Groenendyk J, Lynch J, Michalak M . Calreticulin, Ca2+, and calcineurin – signaling from the endoplasmic reticulum. Mol Cells 2004; 17: 383–389.
Coppolino MG, Woodside MJ, Demaurex N, Grinstein S, St-Arnaud R, Dedhar S . Calreticulin is essential for integrin-mediated calcium signalling and cell adhesion. Nature 1997; 386: 843–847.
Kwon MS, Park CS, Choi K, Ahnn J, Kim JI, Eom SH et al. Calreticulin couples calcium release and calcium influx in integrin-mediated calcium signaling. Mol Biol Cell 2000; 11: 1433–1443.
Oliver JD, Roderick HL, Llewellyn DH, High S . ERp57 functions as a subunit of specific complexes formed with the ER lectins calreticulin and calnexin. Mol Biol Cell 1999; 10: 2573–2582.
Holaska JM, Black BE, Rastinejad F, Paschal BM . Ca2+-dependent nuclear export mediated by calreticulin. Mol Cell Biol 2002; 22: 6286–6297.
Chaput N, De Botton S, Obeid M, Apetoh L, Ghiringhelli F, Panaretakis T et al. Molecular determinants of immunogenic cell death: surface exposure of calreticulin makes the difference. J Mol Med 2007; 85: 1069–1076.
Boyce M, Bryant KF, Jousse C, Long K, Harding HP, Scheuner D et al. A selective inhibitor of eIF2alpha dephosphorylation protects cells from ER stress. Science 2005; 307: 935–939.
Blachere NE, Li Z, Chandawarkar RY, Suto R, Jaikaria NS, Basu S et al. Heat shock protein–peptide complexes, reconstituted in vitro, elicit peptide-specific cytotoxic T lymphocyte response and tumor immunity. J Exp Med 1997; 186: 1315–1322.
Basu S, Srivastava PK . Calreticulin, a peptide-binding chaperone of the endoplasmic reticulum, elicits tumor- and peptide-specific immunity. J Exp Med 1999; 189: 797–802.
Matzinger P . The danger model: a renewed sense of self. Science 2002; 296: 301–305.
Basu S, Binder RJ, Suto R, Anderson KM, Srivastava PK . Necrotic but not apoptotic cell death releases heat shock proteins, which deliver a partial maturation signal to dendritic cells and activate the NF-kappa B pathway. Int Immunol 2000; 12: 1539–1546.
la Sala A, Ferrari D, Corinti S, Cavani A, Di Virgilio F, Girolomoni G . Extracellular ATP induces a distorted maturation of dendritic cells and inhibits their capacity to initiate Th1 responses. J Immunol 2001; 166: 1611–1617.
Li M, Carpio DF, Zheng Y, Bruzzo P, Singh V, Ouaaz F et al. An essential role of the NF-kappa B/Toll-like receptor pathway in induction of inflammatory and tissue-repair gene expression by necrotic cells. J Immunol 2001; 166: 7128–7135.
Shi Y, Evans JE, Rock KL . Molecular identification of a danger signal that alerts the immune system to dying cells. Nature 2003; 425: 516–521.
Binder RJ, Vatner R, Srivastava P . The heat-shock protein receptors: some answers and more questions. Tissue Antigens 2004; 64: 442–451.
Martinon F, Petrilli V, Mayor A, Tardivel A, Tschopp J . Gout-associated uric acid crystals activate the NALP3 inflammasome. Nature 2006; 440: 237–241.
Bianchi ME, Beltrame M, Paonessa G . Specific recognition of cruciform DNA by nuclear protein HMG1. Science 1989; 243 (4894 Part 1): 1056–1059.
Park JS, Gamboni-Robertson F, He Q, Svetkauskaite D, Kim JY, Strassheim D et al. High mobility group box 1 protein interacts with multiple Toll-like receptors. Am J Physiol Cell Physiol 2006; 290: C917–C924.
Rovere-Querini P, Capobianco A, Scaffidi P, Valentinis B, Catalanotti F, Giazzon M et al. HMGB1 is an endogenous immune adjuvant released by necrotic cells. EMBO Rep 2004; 5: 825–830.
Tsung A, Sahai R, Tanaka H, Nakao A, Fink MP, Lotze MT et al. The nuclear factor HMGB1 mediates hepatic injury after murine liver ischemia–reperfusion. J Exp Med 2005; 201: 1135–1143.
Ronchetti A, Rovere P, Iezzi G, Galati G, Heltai S, Protti MP et al. Immunogenicity of apoptotic cells in vivo: role of antigen load, antigen-presenting cells, and cytokines. J Immunol 1999; 163: 130–136.
Gamrekelashvili J, Kruger C, von Wasielewski R, Hoffmann M, Huster KM, Busch DH et al. Necrotic tumor cell death in vivo impairs tumor-specific immune responses. J Immunol 2007; 178: 1573–1580.
Apetoh L, Ghiringhelli F, Tesniere A, Obeid M, Ortiz C, Criollo A et al. Toll-like receptor 4-dependent contribution of the immune system to anticancer chemotherapy and radiotherapy. Nat Med 2007; 13: 1050–1059.
Blander JM, Medzhitov R . Regulation of phagosome maturation by signals from Toll-like receptors. Science 2004; 304: 1014–1018.
Shiratsuchi A, Watanabe I, Takeuchi O, Akira S, Nakanishi Y . Inhibitory effect of Toll-like receptor 4 on fusion between phagosomes and endosomes/lysosomes in macrophages. J Immunol 2004; 172: 2039–2047.
Arbour NC, Lorenz E, Schutte BC, Zabner J, Kline JN, Jones M et al. TLR4 mutations are associated with endotoxin hyporesponsiveness in humans. Nat Genet 2000; 25: 187–191.
Ivanov S, Dragoi AM, Wang X, Dallacosta C, Louten J, Musco G et al. A novel role for HMGB1 in TLR9-mediated inflammatory responses to CpG-DNA. Blood 2007; 110: 1970–1981.
Tian J, Avalos AM, Mao SY, Chen B, Senthil K, Wu H et al. Toll-like receptor 9-dependent activation by DNA-containing immune complexes is mediated by HMGB1 and RAGE. Nat Immunol 2007; 8: 487–496.
Choi JJ, Reich III CF, Pisetsky DS . Release of DNA from dead and dying lymphocyte and monocyte cell lines in vitro. Scand J Immunol 2004; 60: 159–166.
Bell CW, Jiang W, Reich III CF, Pisetsky DS . The extracellular release of HMGB1 during apoptotic cell death. Am J Physiol Cell Physiol 2006; 291: C1318–C1325.
Kariko K, Ni H, Capodici J, Lamphier M, Weissman D . mRNA is an endogenous ligand for Toll-like receptor 3. J Biol Chem 2004; 279: 12542–12550.
Ishii KJ, Suzuki K, Coban C, Takeshita F, Itoh Y, Matoba H et al. Genomic DNA released by dying cells induces the maturation of APCs. J Immunol 2001; 167: 2602–2607.
Krysko DV, Leybaert L, Vandenabeele P, D'Herde K . Gap junctions and the propagation of cell survival and cell death signals. Apoptosis 2005; 10: 459–469.
Ferrari D, Wesselborg S, Bauer MK, Schulze-Osthoff K . Extracellular ATP activates transcription factor NF-kappaB through the P2Z purinoreceptor by selectively targeting NF-kappaB p65. J Cell Biol 1997; 139: 1635–1643.
Bottazzi B, Garlanda C, Salvatori G, Jeannin P, Manfredi A, Mantovani A . Pentraxins as a key component of innate immunity. Curr Opin Immunol 2006; 18: 10–15.
Rovere P, Peri G, Fazzini F, Bottazzi B, Doni A, Bondanza A et al. The long pentraxin PTX3 binds to apoptotic cells and regulates their clearance by antigen-presenting dendritic cells. Blood 2000; 96: 4300–4306.
Baruah P, Propato A, Dumitriu IE, Rovere-Querini P, Russo V, Fontana R et al. The pattern recognition receptor PTX3 is recruited at the synapse between dying and dendritic cells, and edits the cross-presentation of self, viral, and tumor antigens. Blood 2006; 107: 151–158.
Bartkova J, Horejsi Z, Koed K, Kramer A, Tort F, Zieger K et al. DNA damage response as a candidate anti-cancer barrier in early human tumorigenesis. Nature 2005; 434: 864–870.
Gorgoulis VG, Vassiliou LV, Karakaidos P, Zacharatos P, Kotsinas A, Liloglou T et al. Activation of the DNA damage checkpoint and genomic instability in human precancerous lesions. Nature 2005; 434: 907–913.
Gasser S, Orsulic S, Brown EJ, Raulet DH . The DNA damage pathway regulates innate immune system ligands of the NKG2D receptor. Nature 2005; 436: 1186–1190.
Xue W, Zender L, Miething C, Dickins RA, Hernando E, Krizhanovsky V et al. Senescence and tumour clearance is triggered by p53 restoration in murine liver carcinomas. Nature 2007; 445: 656–660.
Shelton DN, Chang E, Whittier PS, Choi D, Funk WD . Microarray analysis of replicative senescence. Curr Biol 1999; 9: 939–945.
Hanahan D, Weinberg RA . The hallmarks of cancer. Cell 2000; 100: 57–70.
Zitvogel L, Apetoh L, Ghiringhelli F, Kroemer G . Immunological aspects of anti-cancer chemotherapy. Nat Rev Immunol 2007 (in press).
Acknowledgements
GK is supported by a special grant from Ligue contre le Cancer (équipe labellisée) as well as by grants from European Commission (Active p53, RIGHT, Trans-Death, Death-Train, ChemoRes) and by Institut National contre le Cancer (INCa). LZ is supported by grants from INCa and from European DC THERA. AT receives a fellowship from Fondation pour la Recherche Medicale. TP receives a fellowship from the Swedish Research Council. LA is supported by Ligue contre le Cancer, and FG by Poste d'Accueil INSERM.
Author information
Authors and Affiliations
Corresponding author
Additional information
Edited by G Melino
Rights and permissions
About this article
Cite this article
Tesniere, A., Panaretakis, T., Kepp, O. et al. Molecular characteristics of immunogenic cancer cell death. Cell Death Differ 15, 3–12 (2008). https://doi.org/10.1038/sj.cdd.4402269
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.cdd.4402269
Keywords
This article is cited by
-
Exploiting immunostimulatory mechanisms of immunogenic cell death to develop membrane-encapsulated nanoparticles as a potent tumor vaccine
Journal of Nanobiotechnology (2023)
-
Afzelin induces immunogenic cell death against lung cancer by targeting NQO2
BMC Complementary Medicine and Therapies (2023)
-
Immune-based combination therapy to convert immunologically cold tumors into hot tumors: an update and new insights
Acta Pharmacologica Sinica (2023)
-
SIRPα blockade improves the antitumor immunity of radiotherapy in colorectal cancer
Cell Death Discovery (2023)
-
Cuproptosis in lung cancer: mechanisms and therapeutic potential
Molecular and Cellular Biochemistry (2023)