Abstract
Alzheimer's and Parkinson's diseases are associated with the formation in the brain of amyloid fibrils from β-amyloid and α-synuclein proteins, respectively. It is likely that oligomeric fibrillization intermediates (protofibrils), rather than the fibrils themselves, are pathogenic, but the mechanism by which they cause neuronal death remains a mystery. We show here that mutant amyloid proteins associated with familial Alzheimer's and Parkinson's diseases form morphologically indistinguishable annular protofibrils that resemble a class of pore-forming bacterial toxins, suggesting that inappropriate membrane permeabilization might be the cause of cell dysfunction and even cell death in amyloid diseases.
Similar content being viewed by others
Main
The possibility that a molecular species other than the amyloid fibril could be pathogenic arose when oligomeric species rich in β-sheet structure (protofibrils) were found to be discrete intermediates in the fibrillization of β-amyloid (Aβ) and of α-synuclein in vitro1,2. An intermediate protofibril might therefore be pathogenic and be 'detoxified' by conversion to a fibril, as suggested by three general observations: there is no correlation between the quantity of fibrillar deposits at autopsy and the clinical severity of Alzheimer's or Parkinson's disease; transgenic mouse models of these conditions have disease-like phenotypes before fibrillar deposits can be detected1,2; and non-fibrillar Aβ oligomers are toxic in cell culture3,4 and have activity in vivo5.
Toxic protofibrils have been implicated in other neurodegenerative diseases as well as in systemic amyloidoses such as type II diabetes (in which the amyloid protein is IAPP)6 and familial amyloidotic polyneuropathy (in which it is transthyretin)7. Strikingly, protofibrils comprising proteins that are not associated with any disease are also toxic, suggesting that toxicity might arise from a shared structural feature of these intermediates8.
The pathogenic-protofibril hypothesis is supported by biophysical studies of variants of Aβ and α-synuclein linked to autosomal-dominant forms of Alzheimer's and Parkinson's diseases, respectively. The 'Arctic' mutation in amyloid-precursor protein, unlike all other mutations associated with Alzheimer's disease, reduces the total concentration of circulating Aβ, but mutant AβARC forms protofibrils in vitro more rapidly and to a greater extent than the wild-type form9.
The A30P and A53T α-synuclein mutations associated with Parkinson's disease (in which an alanine residue is replaced by phenylalanine at position 30 or by threonine at position 53, respectively) both promote protofibril formation in vitro relative to wild-type α-synuclein2. We examined the structural properties of A30P, A53T and AβARC protofibrils for shared structural features that might be related to their toxicity.
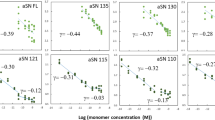
Heterogeneous populations of A30P, A53T and AβARC protofibrils were fractionated by gel-filtration chromatography (H.A.L. et al., unpublished results). The fraction with the smallest A30P and A53T protofibrils contained β-sheet-rich (as measured by circular dichroism) oligomers comprising 20–25 α-synuclein molecules (relative molecular mass, 320K–380K; 22–26 monomers; H.A.L. et al., unpublished results). Analysis of this fraction by electron microscopy revealed annular species (diameter 8–12 nm; inner diameter 2.0–2.5 nm) and coiled species, both of which seemed to be related to the spherical and chain-like species reported earlier2. Protofibrillar AβARC, fractionated by a similar method, contained many annular species of similar appearance (Fig. 1), diameter (7–10 nm; inner diameter 1.5–2.0 nm) and relative molecular mass (150K–250K, 40–60 AβARC molecules).
Projection averages of annular protofibrils formed by the Parkinson's-disease-linked α-synuclein mutants A53T and A30P and by the Alzheimer's-disease-linked Aβ(1–40)ARC 'Arctic' mutant (E22G). The images were calculated from a total of about 5,000–6,000 particles, which were obtained from 25–31 digitized electron micrographs of purified (by gel filtration on Superdex-200 (α-synuclein) or Superose-6 (Aβ)) protofibrillar fractions corresponding to the lowest-Mr fraction of each mutant. Each panel shows an original area of 30.5×30.5 nm.
The pore-like morphology of a subpopulation of amyloid protofibrils might explain the pore activity of α-synuclein protofibrils in vesicle-permeabilization models10 and the channel-like properties of Aβ (ref. 11). Other amyloid proteins, including huntingtin (in Huntington's disease)12 and IAPP6,12, also have pore-like activity in vitro. The small annular Aβ and α-synuclein protofibrils (Fig. 1) resemble the cytolytic β-barrel pore-forming toxins from bacteria such as Clostridium perfringens13.
As expected, amyloid pores are formed much less efficiently than bacterial pores, which during the course of evolution have optimized their ability to puncture host membranes. However, amyloid pores might be wholly or partly responsible for the cytotoxicity associated with the formation of amyloid fibrils in Alzheimer's and Parkinson's diseases and in other age-associated degenerative amyloid diseases.
References
Lansbury, P. T. Proc. Natl Acad. Sci. USA 96, 3342–3344 (1999).
Goldberg, M. S. & Lansbury, P. T. Nature Cell Biol. 2, E115–E119 (2000).
Hartley, D. M. et al. J. Neurosci. 19, 8876–8884 (1999).
Lambert, M. P. et al. Proc. Natl Acad. Sci. USA 95, 6448–6453 (1998).
Walsh, D. M. et al. Nature 416, 535–539 (2002).
Janson, J. et al. Diabetes 48, 491–498 (1999).
Sousa, M. M. et al. Am. J. Pathol. 159, 1993–2000 (2001).
Bucciantini, M. et al. Nature 416, 507–511 (2002).
Nilsberth, C. et al. Nature Neurosci. 4, 887–893 (2001).
Volles, M. J. & Lansbury, P. T. Biochemistry 41, 4595–4602 (2002).
Lin, H., Bhatia, R. & Lal, R. FASEB J. 15, 2433–2444 (2001).
Kagan, B. L., Hirakura, Y., Azimov, R. & Azimova, R. Brain Res. Bull. 56, 281–284 (2001).
Hotze, E. M. et al. J. Biol. Chem. 277, 11597–11605 (2002).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Rights and permissions
About this article
Cite this article
Lashuel, H., Hartley, D., Petre, B. et al. Amyloid pores from pathogenic mutations. Nature 418, 291 (2002). https://doi.org/10.1038/418291a
Issue Date:
DOI: https://doi.org/10.1038/418291a
This article is cited by
-
Altered neural cell junctions and ion-channels leading to disrupted neuron communication in Parkinson’s disease
npj Parkinson's Disease (2022)
-
Conformational strains of pathogenic amyloid proteins in neurodegenerative diseases
Nature Reviews Neuroscience (2022)
-
Carrying Excess Baggage Can Slowdown Life: Protein Clearance Machineries That Go Awry During Aging and the Relevance of Maintaining Them
Molecular Neurobiology (2022)
-
Modeling of mutant superoxide dismutase 1 octamers with cross-linked disulfide bonds
Journal of Molecular Modeling (2022)
-
Reverse engineering Lewy bodies: how far have we come and how far can we go?
Nature Reviews Neuroscience (2021)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.