Abstract
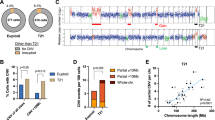
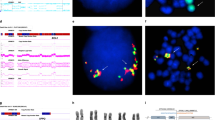
Trisomic cells in neoplasms may represent abnormal clones originated from a tissue-confined mosaicism, and arise therefore by a meiotic error. We report on a 16-month-old child with erythroleukaemia (AML-M6), whose marrow karyotype at onset was 48,XX,del(13)(q12q14),del(14)(q22q32),+21,+21. The parental origin of the supernumerary chromosomes 21 was investigated by comparing 10 polymorphic loci scattered along the whole chromosome on the patient's marrow and her parents’ leukocytes. Three loci were informative for the presence of three alleles, two of which were of maternal origin; two further loci showed a maternal allele of higher intensity. Lymphocytes and skin fibroblasts showed a normal karyotype, and molecular analysis on leukocytes at remission, buccal smear and urinary sediment cells consistently showed only one maternal allele, whereas neonatal blood from Guthrie spot showed two maternal alleles as in the marrow. An accurate clinical re-evaluation confirmed a normal phenotype. Our results indicate that tetrasomy 21 arose from a marrow clone with trisomy 21 of meiotic origin. To the best of our knowledge, this is the first evidence that supernumerary chromosomes in neoplastic clones may in fact be present due to a meiotic error. This demonstrates that a tissue-confined constitutional mosaicism for a trisomy may indeed represent the first event in multistep carcinogenesis.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Heim S, Mitelman F . Cancer Cytogenetics, 2nd edn Wiley-Liss: New York 1995
United Kingdom Cancer Cytogenetics Group . Primary, single, autosomal trisomies associated with haematological disorders Leuk Res 1992 16: 841–851
Haas OA, Seyger M . Hypothesis: meiotic origin of trisomic neoplasms Cancer Genet Cytogenet 1993 70: 112–116
Mark HFL . Phenotypic variability in trisomy 8 mosaicism is consistent with the hypothesis of meiotic origin of trisomic neoplasms Cancer Genet Cytogenet 1994 76: 158
Lampert F . On the ‘Keimversprengungs’ origin of embryonic tumors Cancer Genet Cytogenet 1994 78: 242
Hecht F . Trisomy and disomy in tumors Cancer Genet Cytogenet 1995 80: 171
Antonarakis SE, Avramopoulos D, Blouin J-L, Conover Talbot Jr C, Schinzel AA . Mitotic errors in somatic cells cause trisomy 21 in about 4.5% of cases and are not associated with advanced maternal age Nat Genet 1993 3: 146–150
Mitelman Database of Chromosome Aberrations in Cancer Mitelman F, Johansson B, Mertens F (eds) . 2000 http://cgap.nci.nih.gov/Chromosomes/Mitelman
Harris DJ, Begleiter ML, Chamberlin J, Hankins L, Magenis RE . Parental trisomy 21 mosaicism Am J Hum Genet 1982 34: 125–133
Hook EB . Exclusion of chromosomal mosaicism: tables of 90%, 95%, and 99% confidence limits and comments on use Am J Hum Genet 1977 29: 94–97
Wiemels JL, Cazzaniga G, Daniotti M, Eden OB, Addison GM, Masera G, Saha V, Biondi A, Greaves MF . Prenatal origin of acute lymphoblastic leukaemia in children Lancet 1999 354: 1499–1503
Robinson WP, Binkert F, Bernasconi F, Lorda-Sanchez I, Werder EA, Schinzel AA . Molecular studies of chromosomal mosaicism: relative frequency of chromosome gain or loss and possible role of cell selection Am J Hum Genet 1995 56: 444–451
Jenkins EC, Schupf N, Genovese M, Ye LL, Kapell D, Canto B, Harris M, Devenny D, Lee JH, Brown WT . Increased low-level chromosome 21 mosaicism in older individuals with Down syndrome Am J Med Genet 1997 68: 147–151
Bhatt S, Schreck R, Graham JM, Korenberg JR, Hurvitz CG, Fischel-Ghodsian N . Transient leukemia with trisomy 21: description of a case and review of the literature Am J Med Genet 1995 58: 310–314
Satge D, Van Den Berghe H . Aspects of the neoplasms observed in patients with constitutional autosomal trisomy Cancer Genet Cytogenet 1996 87: 63–70
Seghezzi L, Maserati E, Minelli A, Dellavecchia C, Addis P, Locatelli F, Angioni A, Balloni P, Miano C, Cavalli P, Danesino C, Pasquali F . Constitutional trisomy 8 as first mutation in multistep carcinogenesis: clinical, cytogenetic, and molecular data on three cases Genes Chromosom Cancer 1996 17: 94–101
Acknowledgements
We thank ABEO-Liguria for technical support. CCD and PowerGene Systems (Perceptive Scientific Instruments, UK) were a gift from AICODS (Vésenaz, CH). This work was supported by IGG grant ‘Studio delle anomalie cromosomiche nei tumori solidi pediatrici’ and by grants from MURST-COFIN 2000 to CD and FP. CM is a research fellow supported by Eredità Laura Capursi. DNA samples were stored thank to a Telethon grant (C30) to CD for the Cell and DNA Bank.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Minelli, A., Morerio, C., Maserati, E. et al. Meiotic origin of trisomy in neoplasms: evidence in a case of erythroleukaemia. Leukemia 15, 971–975 (2001). https://doi.org/10.1038/sj.leu.2402123
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.leu.2402123