Summary:
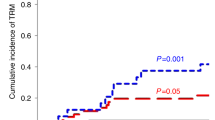
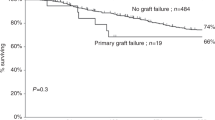
For many children with life-threatening hematological diseases, hematopoietic stem cell transplantation (HSCT) is the only curative option. In children lacking a matched related or unrelated donor and with the certainty that, left untreated, death will ensue alternative donors must be sought. Haplo-identical peripheral blood stem cell transplantation (PBSCT) from a healthy parent is a feasible alternative. To reduce the risk of fatal graft-versus-host disease (GvHD) as a complication of transplant across major histocompatibility antigens, intense T-cell depletion is required. Large numbers of purified, cytokine mobilized peripheral stem cells (the so-called mega-dose concept) are required to compensate for the significantly increased risk of either graft failure or early rejection. In our unit, despite this approach, graft dysfunction has, in a significant group of children, proved problematic and, despite salvage attempts at re-transplantation, usually fatal. In children with hematological malignant disease, our overall relapse-free survival is 41%. However, successful transplant outcome has been associated with considerable delays in immune reconstitution that can be implicated in subsequent viral reactivation. We are investigating new strategies to improve the outcome of haplo-identical PBSCT, which may allow us to offer this form of treatment to more children requiring urgent HSCT.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Beatty PG, Mori M, Milford E . Impact of racial genetic polymorphisms on the probability of finding an HLA matched donor. Transplantation 1995; 60: 778–783.
Casper J, Cannita B, Truitt R et al. Unrelated bone marrow donor transplants for children with leukemia or myelodysplasia. Blood 1995; 85: 2354–2363.
Rubinstein P, Carrier C, Scaradavou A et al. Outcomes of 562 recipients of placental-blood transplants from unrelated donors. The New Engl J Med 1998; 339: 1565–1577.
Rowe JM, Lazarus HM . Genetically haploidentical stem cell transplantation for acute leukemia. Bone Marrow Transplant 2001; 27: 669–676.
Aversa F, Tabalio A, Terenzi A et al. Successful engraftment of T-cell depleted haploidentical ‘three loci’ incompatible transplants in leukemia patients by addition of recombinant human granulocyte colony-stimulating factor mobilized peripheral blood progenitor cells to bone marrow inoculum. Blood 1994; 84: 3948–3955.
Handgretinger R, Klingebiel T, Lang P et al. Megadose transplantation of purified peripheral blood CD34+ progenitor cells from HLA mismatched parental donors in children. Bone Marrow Transplant 2001; 27: 777–783.
Kook H, Goldma F, Padley D et al. Reconstruction of the immune system after unrelated or partially matched T-cell depleted bone marrow transplantation in children: immunophenotypic analysis and factors affecting the speed of recovery. Blood 1996; 88: 1089–1097.
Eyrich M, Lang P, Shangara L et al. A prospective analysis of the pattern of immune reconstitution in a pediatric cohort following transplantation of positively selected human leucocyte antigen-disparate haematopoietic stem cells from parental donors. Br J Haematol 2001; 114: 422–432.
Lang P, Handgretinger R, Niethammer D et al. Transplantation of highly purified CD34+ progenitor cells from unrelated donors in pediatric leukemia. Blood 2003; 101: 1630–1636.
Klingebiel T, Handgretinger R, Lang P et al. Haploidentical transplant for acute lymphoblastic leukemia in childhood. Blood Rev 2004; 18: 181–192.
Bornhauser M, Platzbecker U, Theuser C et al. CD34+-enriched peripheral blood progenitor cells from unrelated donors for allografting of adult patients: high risk of graft failure, infection and relapse despite donor lymphocyte add-back. Br J Haematol 2002; 118: 1095–1103.
Veys P . The role of haploidentical stem cell transplantation in the management of children with hematological disorders. Br J Haematol 2003; 123: 193–206.
Platzbecker U, Ehninger G, Bornhauser M . Allogeneic transplantation of CD34+ selected hematopoietic cells – clinical problems and current challenges. Leuk Lymphoma 2004; 45: 447–453.
McDonough CH, Jacobson DA, Vogelsang GB et al. High incidence of graft failure in children receiving CD34+ augmented elutriated allografts for non-malignant disease. Bone Marrow Transplant 2003; 31: 1073–1080.
Lang P, Handgretinger R, Griel J et al. Transplantation of CD34+ enriched allografts in children with nonmalignant disease: does graft manipulation necessarily result in high incidence of graft failure. Bone Marrow Transplant 2004; 33: 125–126.
Passweg JR, Kuhne T, Gregor M et al. Increased stem cell dose, as obtained using currently available technology, may not be sufficient for engraftment of haploidentical stem cell transplantation. Bone Marrow Transplant 2000; 26: 1033–1036.
Martelli MF, Reisner Y . Haploidenical ‘mega dose’ CD34+ cell transplants for patients with acute leukemia. Leukemia 2002; 16: 404–405.
Maitra B, Szekely E, Gjini K et al. Human mesenchymal stem cells support unrelated donor hematopoietic stem cells and suppress T cell activation. Bone Marrow Transplant 2004; 33: 597–604.
Acknowledgements
The medical, nursing and ancillary staff of the IHOBA, Willem-Alexander Kinder en Jeugd Centrum, Leiden University Medical Center, Leiden, the Netherlands. The staff of the Europdonor Foundation, Leiden, the Netherlands. JDJ Bakker-Steeneveld and CM Jol-van der Zijde, Data Managers, IHOBA, Willem-Alexander Kinder en Jeugd Centrum, Leiden University Medical Center, Leiden, the Netherlands. Professor Dr Dietrich Niethammer, Klinik für Kinderheilkunde und Jugendmedizin, Abteilung der Universität Tubingen, Tubingen, Germany. Professor Dr Thomas Klingebiel, Klinik für Kinderheilkunde III, Zentrum für Kinderheilkunde und Jugendmedizin der Universität Frankfurt, Frankfurt, Germany.
Author information
Authors and Affiliations
Corresponding author
Additional information
Conflict of interest and financial support: None.
Rights and permissions
About this article
Cite this article
Ball, L., Lankester, A., Bredius, R. et al. Graft dysfunction and delayed immune reconstitution following haploidentical peripheral blood hematopoietic stem cell transplantation. Bone Marrow Transplant 35 (Suppl 1), S35–S38 (2005). https://doi.org/10.1038/sj.bmt.1704842
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.bmt.1704842
Keywords
This article is cited by
-
Favorable immune recovery and low rate of GvHD in children transplanted with partially T cell-depleted PBSC grafts
Bone Marrow Transplantation (2019)
-
A low thymic function is associated with leukemia relapse in children given T-cell-depleted HLA-haploidentical stem cell transplantation
Leukemia (2012)
-
Feasibility and outcome of haploidentical SCT in pediatric high-risk hematologic malignancies and Fanconi anemia in Uruguay
Bone Marrow Transplantation (2012)
-
Subclinical GvHD in non-irradiated F1 hybrids: severe lymphoid-tissue GvHD causing prolonged immune dysfunction
Bone Marrow Transplantation (2011)
-
Assessment of CD4 T-lymphocyte reactivity by the Cylex ImmuKnow assay in patients following allogeneic hematopoietic SCT
Bone Marrow Transplantation (2010)