Abstract
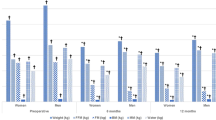
Objective: The gastric bypass-induced quantitative and qualitative modifications of energy intake (En In, kcal/day) and their impact on body weight (bw) loss were evaluated. The factors influencing energy intake and body weight loss were also investigated.
Design: Longitudinal study.
Setting: University Hospital of Geneva.
Subjects: Fifty obese women undergoing a Roux-en-Y gastric bypass.
Results: The reduction of EnIn was significantly related to bw loss expressed either in kg or as percentage correction of excess bw (P<0.01 for both), whereas the post-operative modifications of diet composition did not play a role. Age and initial bw significantly influenced bw loss (P<0.0001 and P<0.001, respectively), as shown by multiple regression analysis. Patients were divided into four sub-groups according to their age (under or over 35 y) and initial bw (under or over 120 kg). ANOVA showed that under 35-y-old subjects reduced their EnIn significantly more than their older counterparts having similar bw (P<0.02 and P<0.05); consequently, bw loss, expressed in kg, was significantly (P<0.0001 and P<0.0005) larger in younger patients. Subjects with an initial bw over 120 kg lost significantly (P<0.001 and P<0.02) more weight as compared to patients with a smaller degree of obesity (under 120 kg) and similar age.
Conclusions: Gastric bypass-induced body weight loss is mainly due to the reduction of EnIn, whereas the qualitative modifications of the diet do not play a role. Younger subjects have a greater capacity to reduce EnIn and, therefore, lose more weight. Pre-operative high degree of obesity leads to a larger weight reduction, probably because of a greater energy deficit.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Alford BB, Blankenship AC, Hagen RD . 1990 The effects of variation in carbohydrate, protein and fat content of the diet upon weight loss J. Am. Diet. Assoc. 90: 534–540
Blaak EE . 2000 Adrenergically stimulated fat utilization and ageing Ann. Med. 32: 380–382
Bloomston M, Zervos EE, Camps MA, Goode SE, Rosemurgy AS . 1997 Outcome following bariatric surgery in super versus morbidly obese patients: does weight matter? Obes. Surg. 7: 414–419
Brolin RE, Robertson LB, Kenler HA, Cody RP . 1994 Weight loss and dietary intake after vertical banded gastroplasty and Roux-en-Y gastric bypass Ann. Surg. 220: 782–790
Dixon JB, Dixon ME, O'Brien PE . 2001 Pre-operative predictors of weight loss at one year after lap-band surgery Obes. Surg. 11: 200–207
Donnelly JE, Jacobsen DJ, Whatley JE . 1994 Influence of degree of obesity on loss of fat-free mass during very-low-energy diets Am. J. Clin. Nutr. 60: 874–878
Dwyer JT . 1992 Treatment of obesity In Conventional Programs and Fat Diets in Obesity ed. P Björntorp & NN Brodoff, Vol 57: pp 662–676 Philadelphia, PA: JB Lippincott
Ferrannini E . 1988 The theoretical basis of indirect calorimetry: a review Metabolism 37: 287–301
Golay A, Allaz AF, Morel Y, de Tonnac N, Tankova S, Reaven G . 1996 Similar weight loss with low- or high-carbohydrate diets Am. J. Clin. Nutr. 63: 174–178
Hall JC, Watts JM, O'Brien PE, Dustan RE, Walsh JF, Slavotinek AH, Elmslie RG . 1990 Gastric surgery for morbid obesity: the Adelaide study Ann. Surg. 211: 419–427
Howatt MP, Mohan R, Champagne C, Monlezun C, Wozniak P, Bray GA . 1994 Validity and reliability of reported dietary intake data J. Am. Diet. Assoc. 94: 169–173
Jéquier E, Felber JP . 1987 Indirect calorimetry Baillière's Clin. Endocrinol. Metab. 1: 911–935
Kenler HA, Brolin RE, Cody RP . 1990 Changes in eating behaviour after horizontal gastroplasty and Roux-en-Y gastric bypass Am. J. Clin. Nutr. 52: 87–92
Klesges RC, Eck LH, Ray JW . 1995 Who underreports dietary intake in a dietary recall? Evidence from the Second National Health and Nutrition Examination Survey J. Consult. Clin. Psychol. 63: 438–444
Kral JC . 1992 Surgical treatment of obesity In Obesity ed. P Björntorp & BN Bronoff pp 731–741 Philadelphia, PA: JB Lipincott
Kretsch MJ, Fong AK, Green MW . 1999 Behavioural and body size correlates of energy intake underreporting by obese and normal-weight women J. Am. Diet. Assoc. 99: 300–306
Lindroos AK, Lissner L, Sjöstrom L . 1996 Weight change in relation to intake of sugar and sweet foods before and after weight reducing gastric surgery Int. J. Obes. Relat. Metab. Disord. 20: 634–643
Lissner L, Lindroos AK, Sjöström L . 1998 Swedish obese subjects (SOS): an obesity intervention study with nutritional perspective Eur. J. Clin. Nutr. 52: 316–322
Lusk G . 1924 Animal calorimetry: analysis of the oxidation of mixtures of carbohydrates and fat J. Biol. Chem. 59: 41–42
Näslund I, Wickbom G, Christofferson E, Agren G . 1986 A prospective randomized comparison of gastric bypass and gastroplasty: complications and early results Acta. Chir. Scand. 152: 681–689
Näslund I, Järnmark I, Andersson H . 1988 Dietary intake before and after gastric bypass and gastroplasty for morbid obesity Int. J. Obes. 12: 503–513
Nickals BJ, Rogus EM, Goldberg AP . 1997 Exercise blunts declines in lipolysis and fat oxidation after dietary-induced weight loss in obese older women Am. J. Physiol. Endocrinol. Metab. 273: E149–E155
Pasquali R, Casimiri F, Melchionda N . 1987 Protein metabolism in obese patients during very low-calorie mixed diets containing different amounts of proteins and carbohydrates Metabolism 36: 1141–1148
Pories WJ, Flickinger EG, Meehleim D, Van Rij AM, Thomas FT . 1982 The effectiveness of gastric bypass over gastric partition in morbid obesity Ann. Surg. 196: 398–399
Rabast U, Vomberger KH, Ehl M . 1981 Loss of weight, sodium and water in obese persons consuming a high or low carbohydrate diet Ann. Nutr. Metab. 25: 342–349
Sugerman HJ, Starkey JV, Birkenhauer RA . 1987 A randomized prospective trial of gastric bypass vs vertical banded gastroplasty Roux-en-Y gastric bypass and their effects on sweet vs non-sweet eaters Ann. Surg. 205: 613–624
Sugerman HJ, Londrey GL, Kellum JM, Wolf L, Liszka T, Engle KM, Birkenhauer RA, Starkey JV . 1989 Weight loss with vertical banded gastroplasty and Roux-en-Y gastric bypass for morbid obesity with selective vs random assignement Am. J. Surg. 157: 93–102
Talieh J, Kirgan D, Fisher BL . 1997 Gastric bypass for morbid obesity: a standard surgical technique by consensus Obes. Surg. 7: 518–520
Toth MJ, Tcherof A . 2000 Lipid metabolism in elderly Eur. J. Clin. Nutr. 54: (Suppl 3): S121–S125
Zhang J, Temme EH, Sasaki S, Kesteloot H . 2000 Under- and overreporting of energy intake using urinary cations as biomarkers: relation to body mass index Am. J. Epidemiol. 152: 453–462
Acknowledgements
This study was partially supported by the Swiss National Funds for Scientifical Research, grant no. 32-61339.00 and by a grant from the Ernst and Lucie Schmidheiny Foundation.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Bobbioni-Harsch, E., Huber, O., Morel, P. et al. Factors influencing energy intake and body weight loss after gastric bypass. Eur J Clin Nutr 56, 551–556 (2002). https://doi.org/10.1038/sj.ejcn.1601357
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.ejcn.1601357
Keywords
This article is cited by
-
Associations between diet composition, dietary pattern, and weight outcomes after bariatric surgery: a systematic review
International Journal of Obesity (2023)
-
Dietary Macronutrient Composition and Quality, Diet Quality, and Eating Behaviors at Different Times Since Laparoscopic Sleeve Gastrectomy
Obesity Surgery (2023)
-
Association Between Energy and Macronutrient Intakes and Weight Change After Bariatric Surgery: a Systematic Review and Meta-analysis
Obesity Surgery (2023)
-
Gut Factors Mediating the Physiological Impact of Bariatric Surgery
Current Diabetes Reports (2022)
-
Nutrition, Physical Activity, and Prescription of Supplements in Pre- and Post-bariatric Surgery Patients: a Practical Guideline
Obesity Surgery (2019)