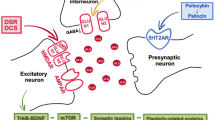
Abstract
Phencyclidine, ketamine, and other agents that block NMDA glutamate receptors trigger a schizophrenia-like psychosis in humans and induce pathomorphological changes in cerebrocortical neurons in rat brain. Accumulating evidence suggests that a complex network disturbance involving multiple transmitter receptor systems is responsible for the neuronal injury, and it is proposed that a similar network disturbance is responsible for the psychotomimetic effects of NMDA antagonists, and might also be involved in the pathophysiology of schizophrenia. In the present study we present evidence that serotonergic agents possessing 5HT2A agonist activity prevent NMDA antagonist neurotoxicity in rat brain. It is proposed that 5HT2A agonists may also prevent the psychotomimetic effects of NMDA antagonists. Among the 5HT2A agonists examined and found to be neuroprotective are LSD and related hallucinogens. The apparent contradiction in proposing that these agents might have antipsychotic properties is resolved by evidence linking their hallucinogenic activity to agonist action at 5HT2C receptors, whereas antipsychotic activity would be attributable to agonist action at 5HT2A receptors.
Similar content being viewed by others
Main
Phencyclidine (PCP) and ketamine cause a schizophrenia-like psychosis and cognitive impairments in normal humans (Luby et al. 1959; Rosenbaum et al. 1959; Cohen et al. 1962; Krystal et al. 1994; Newcomer et al. 1996), and a return to the acute exacerbated state in patients with chronic stabilized schizophrenia (Ban et al. 1961; Luby et al. 1962; Lahti et al. 1995). The discovery that these agents are noncompetitive antagonists of the NMDA subtype of glutamate receptor (Lodge and Anis 1982; Lodge et al. 1987) has led to the hypothesis that suppression or disruption of NMDA receptor activity is psychotogenic, and to the proposal that NMDA receptor hypofunction (NRH) is a candidate mechanism to explain symptom formation in schizophrenia (Olney 1988; Javitt and Zukin 1991; Olney and Farber 1995b). More recently it has been found that PCP and various other NMDA receptor antagonists, which trigger psychotic reactions in humans, also induce cytopathological changes in cerebrocortical neurons in the adult rat brain (Olney et al. 1989; Ellison and Switzer 1993; Ellison 1994; Fix et al. 1993; Fix et al. 1995; Corso et al. 1997). Based upon several lines of evidence we have hypothesized (Olney and Farber 1995b) that a common mechanism may underlie both the neurotoxic and psychotogenic actions of NMDA antagonists, and that this may be a complex mechanism involving not only a primary disruption of a major excitatory transmitter system (NMDA glutamate system), but a secondary impairment in at least one other major transmitter system (GABAA inhibitory system). If a common mechanism underlies the neurotoxic and psychotogenic actions of NMDA antagonists in rats and humans respectively, and the human psychosis induced by these agents has a schizophrenia-like quality, further elucidation of the specific transmitter receptor disturbances, that contribute to the NMDA antagonist neurotoxic syndrome in rats, may provide valuable clues to the complex transmitter disturbances that contribute to symptom formation in schizophrenia. With this prospect in mind, we have evaluated various neuroactive agents, including known and putative antipsychotic agents, for their ability to protect against NRH-induced neurotoxicity in rats. We have found that both traditional (for example, loxapine, haloperidol, and thioridazine) and novel (for example, clozapine and olanzapine) antipsychotics protect against NRH-induced neurotoxicity. However, the novel agents are approximately an order of magnitude more effective than the traditional agents in preventing the neurotoxic reaction (Farber et al. 1993; Farber et al. 1996). This is of considerable interest since the novel agents, through unknown mechanisms, appear to have a superior clinical profile in the treatment of schizophrenia.
Several mechanisms, including antagonism of serotonin (5HT) receptors, have been proposed to explain clozapine's unique clinical profile. Recent advances in molecular pharmacology have led to the reclassification of the serotonergic system into several distinct receptor types (Martin and Humphrey 1994). The 5HT2 receptor in now recognized to be a family containing three separate molecular subtypes of receptors, two of which (5HT2A [previously named 5HT2] and 5HT2C [previously named 5HT1C]) are considered potentially relevant to clozapine's efficacy in treating schizophrenia (Hoenicke et al. 1992; Schmidt et al. 1995). Given the potential involvement of 5HT2A and 5HT2C receptors in schizophrenia, and in the therapeutic actions of clozapine, we undertook the present study to explore the role of 5HT2A and 5HT2C receptors in NRH-induced neurotoxicity.
METHODS
Adult female Sprague Dawley rats were injected intraperitoneally (ip) with a test agent followed, 15 minutes later, by an injection of MK-801 (0.5 mg/kg) subcutaneously (sc). Control animals (n = 88) received either dimethyl sulfoxide or saline, the vehicles used to dissolve the test agents, and MK-801 (0.5 mg/kg sc). For each test agent, at least 20 rats were used and at least 4 doses tested. The animals were sacrificed 4 hours after exposure to MK-801 and the severity of damage assessed by previously described methods (Olney et al. 1989; Farber et al. 1995). In a second set of experiments designed to further clarify the receptor site of action of the neuroprotective drugs, adult female rats (n = 70) received MK-801 (0.5 mg/kg sc) plus the 5HT2A/2C agonist DOI (ip) at one of several doses, and a fixed dose of either the 5HT2A/2C antagonist ritanserin (0.03 mg/kg ip) or the selective 5HT2C antagonist SDZ SER-082 (0.1 mg/kg ip). Results were analyzed by ANCOVA using the dose of DOI as the covariate and the treatment condition (ritanserin or SDZ SER-082) as the between subjects factor.
The Research Technology Branch of the National Institute on Drug Abuse provided (±)-1-(2,5-dimethoxy-4-bromophenyl)-2-aminopropane (DOB), (±)-1-(2,5-dimethoxy-4-methylphenyl)-2-aminopropane (DOM), and d-lysergic acid diethylamide (LSD). Research Biochemical International was the source of (±)-1-(2,5-dimethoxy-4-iodophenyl)-2-aminopropane (DOI), R(+)-lisuride, and ketanserin. Ritanserin and SDZ SER-082 were generously provided by Janssen Pharmaceuticals and Sandoz, respectively.
RESULTS
Combined 5HT2A/2C Antagonists
Ritanserin, a nonspecific 5HT2A/2C antagonist, administered at several doses between 0.001 mg/kg and 100 mg/kg (n = 34), showed no consistent evidence for protection against NRH-induced neurotoxicity (Fig. 1 ). However, at the extreme dose of 100 mg/kg it did show a moderate degree of protection (approximately 50%) while even higher doses were less effective (data not shown). The nonspecific 5HT2A/2C antagonist ketanserin (n = 33) also provided minimal to no protection over a broad range of dosages (0.001–10 mg/kg). At substantially higher doses (≥30 mg/kg; n = 18), where it would be binding to other receptors, possibly muscarinic (Leysen et al. 1981), it did consistently protect against MK-801 neurotoxicity with an ED50 of approximately 40 mg/kg (Fig. 1).
Inability of various 5HT2 antagonists to prevent MK-801 neurotoxicity. Data points represent the percent reduction in neurotoxicity for ritanserin, ketanserin, and SDZ SER-082. Neither ritanserin nor ketanserin show consistent protection in the dose range (0.01–1 mg/kg) where their serotonergic activity predominates. Supra-serotonergic doses of ketanserin are effective at blocking MK-801 neurotoxicity with an ED50 of approximately 40 mg/kg. Ritanserin at extremely high doses also provides some mild but fleeting protection. SDZ SER-082, a more selective 5HT2C antagonist, provides little or no protection over the dose range tested (0.01–10 mg/kg).
Combined 5HT2A/2C Agonists
DOI (n = 73), DOB (n = 48), DOM (n = 28) and LSD (n = 55), all 5HT2A/2C agonists, dose dependently prevented MK-801 neurotoxicity. DOB was the most potent with an ED50 of 0.36 mg/kg (Table 1). LSD, DOM, and DOI were also effective but slightly less potent with ED50s of 0.67 mg/kg, 0.81 mg/kg, and 0.98 mg/kg, respectively (Table 1).
Reversal of DOI's Protection by Ritanserin
To further confirm the involvement of the 5HT2A/2C receptor system, a fixed dose of ritanserin (0.03 mg/kg ip) was administered together with various doses of DOI to MK-801-treated rats (n = 36) to see if ritanserin would reverse DOI's protection. Consistent with the hypothesis that the 5HT2A/2C system is the site of DOI's protective action, ritanserin significantly (p < 0.0005) shifted DOI's protection curve to the right in a manner consistent with a competitive interaction (Fig. 2 ). Similar findings were seen with ritanserin + LSD (n = 4) and ketanserin + DOI (n = 5), but full dose response data were not generated (data not shown). Confirming our impression that ketanserin's protective action against MK-801 neurotoxicity is not due to its 5HT2A/2C activity, the dose of ketanserin (0.03 mg/kg ip) that reversed DOI's protection is 3 orders of magnitude lower than the dose of ketanserin (≥30 mg/kg) required to appreciably block MK-801’s neurotoxic effect.
Inhibition by ritanserin of DOI's protection against MK-801 neurotoxicity. Data points represent the percent reduction in neurotoxicity. DOI, a 5HT2A/2C agonist, dose-dependently prevents the neurotoxic effect of MK-801. Ritanserin, a 5HT2A/2C antagonist, significantly interferes with DOI's protection [F(1,100) = 25.95, p < 0.0005] as is indicated by shifting of the dose-response curve to the right. Squares: MK-801 (0.5 mg/kg) plus DOI. Diamonds: MK-801 (0.5 mg/kg) plus DOI plus ritanserin (0.03 mg/kg).
5HT2A vs. 5HT2C Receptor
To explore initially whether the protection provided by LSD, DOI, DOB, and DOM can be attributed to activity at the 5HT2A receptor, the 5HT2C receptor, or both, we tested the LSD analog lisuride, which has been reported to be a 5HT2A agonist, but a 5HT2C antagonist (Burris et al. 1991). Lisuride (n = 45) also potently protected against MK-801’s neurotoxic action (Table 1), indicating that the 5HT2A receptor might be the site of action for lisuride and the several 5HT2A/2C agonists as well. To determine if agonism at 5HT2C receptors could contribute also to the protection against the neurotoxic effects of MK-801, we tested whether SDZ SER-802, a selective 5HT2C antagonist, could inhibit DOI's blocking action. Consistent with the hypothesis that 5HT2A receptor interaction is solely responsible for the neuroprotective action of these agents, SDZ SER-082 (0.1 mg/kg ip; n = 34) was ineffective (p = 0.5) in reversing DOI's blocking action (Fig. 3 ). When used alone and across a wide dose range, SDZ SER-082 (n = 22) did not affect MK-801 neurotoxicity (Fig. 1).
Inability of SDZ SER-082 to inhibit DOI's protection against MK-801 neurotoxicity. Data points represent the percent reduction in neurotoxicity. DOI, a 5HT2A/2C agonist, dose-dependently prevents the neurotoxic effect of MK-801. SDZ SER-802, a 5HT2C antagonist, is unable to interfere with DOI's protection [F(1,98) = 0.43, p = 0.5] as is indicated by the two curves being superimposed. Squares: MK-801 (0.5 mg/kg) plus DOI. Diamonds: MK-801 (0.5 mg/kg) plus DOI plus SDZ SER-082 (0.1 mg/kg).
DISCUSSION
Accumulating evidence (reviewed in Olney and Farber 1995a and b; Farber et al. 1997; Kim et al. 1997) suggests that NMDA antagonist neurotoxicity is mediated by an indirect mechanism involving disturbances in multiple transmitter receptor systems subserving a complex neural network in which major excitatory pathways are ordinarily held under inhibitory restraint by glutamate acting tonically at NMDA receptors on inhibitory (GABAergic or noradrenergic) neurons. Blockade of these NMDA receptors inactivates the inhibitory mechanism thereby disinhibiting the excitatory pathways, and unleashing excitotoxic activity that serves as the proximal cause of neuronal injury. Given evidence for serotonergic innervation of GABAergic interneurons via 5HT2A receptors (Mengod et al. 1990; Sheldon and Aghajanian 1990; Cornea-Hebert et al. 1996; Mathews et al. 1996; Shen and Andrade 1996), we postulate that a 5HT2A receptor is located on one or more of the GABAergic neurons in the NRH neurotoxicity circuit, and that activation of this receptor by the 5HT2A agonist restores inhibition to the network and prevents neuronal injury. A potentially important implication of our findings is that 5HT2A agonists could be used to prevent the neurotoxic side effects of NMDA antagonists, thus improving the safety of NMDA antagonists for the treatment of nervous system conditions such as stroke, trauma, and neuropathic pain. In addition, if a common mechanism does underlie the neurotoxic and psychotomimetic effects of NMDA antagonists, then coadministration of a selective 5HT2A agonist with an NMDA antagonist could also prevent the psychotomimetic effects of NMDA antagonists.
It seems contradictory to propose that drugs such as LSD and its analogs, which are notorious hallucinogens, might possess properties that could counteract the psychosis induced by PCP and other NMDA antagonists. However, this is a reasonable proposal when viewed in light of the findings of Burris et al. (1991) that agonist action at 5HT2C receptors is responsible for the hallucinogenic effects of LSD. Our evidence, when taken together with the findings of Burris et al. (1991), suggests that stimulation of 5HT2C receptors may promote one type of psychotic activity (LSD hallucinosis), and stimulation of 5HT2A receptors may suppress another type (PCP psychosis). Perhaps this might explain the findings that PCP exacerbates a schizophrenic psychosis, and LSD does not (Erard et al. 1980; Domino and Luby 1981). For further clarification it will be important to evaluate drugs that are selective 5HT2A antagonists or agonists. Similar studies of agonists and antagonists specific for the 5HT2C receptor would also be of benefit. Since LSD has significant affinity not only for 5HT2A and 5HT2C receptors but for the recently described 5ht5A, 5ht5B, 5ht6 and 5ht7 receptors (Martin an Humphrey 1994), the potential involvement of all such receptors should be explored once selective ligands become available.
References
Ban TA, Lohrena JJ, Lehmann HE . (1961): Observations on the action of Sernyl—A new psychotropic drug. Can Psychiatr Assoc J 6: 150–157
Burris KD, Breeding M, Sanders-Bush E . (1991): (+)lysergic acid diethylamide, but not its nonhallucinogenic congeners, is a potent serotonin 5-HT1C receptor agonist. J Pharmacol Exp Ther 258: 891–896
Cohen BD, Rosenbaum G, Luby ED, Gottlieb JS . (1962): Comparison of phencyclidine hydrochloride (Sernyl) with other drugs. Arch Gen Psychiatry 6: 395–401
Cornea-Hebert V, Riad M, Zerari F, Garcia S, Descarries L, Wu C, Singh S . (1996): Cellular mapping of 5-HT2A receptor protein in adult rat CNS. Soc Neurosci Abstr 22: 1775
Corso TD, Sesma MA, Tenkova TI, Der TC, Wozniak DF, Farber NB, Olney JW . (1997): Multifocal brain damage induced by phencyclidine is augmented by pilocarpine. Brain Res 752: 1–14
Domino EF, Luby ED . (1981): Abnormal mental states induced by phencyclidine as a model of schizophrenia. In Domino EF (ed), PCP (Phencyclidine): Historical and Current Perspectives. Ann Arbor, NPP Books, pp 401–418
Ellison G, Switzer RC . (1993): Dissimilar patterns of degeneration in brain following four different addictive stimulants. Neuroreport 5: 17–20
Ellison G . (1994): Competitive and non-competitive NMDA antagonists induce similar limbic degeneration. Neuroreport 5: 2688–2692
Erard R, Luisada PV, Peele R . (1980): The PCP psychosis: prolonged intoxication or drug-precipitated functional illness? J Psychedelic Drugs 12: 235–251
Farber NB, Price MT, Labruyere J, Nemnich J, St Peter H, Wozniak DF, Olney JW . (1993): Antipsychotic drugs block phencyclidine receptor-mediated neurotoxicity. Biol Psychiatr 34: 119–121
Farber NB, Wozniak DF, Price MT, Labruyere J, Huss J, St Peter H, Olney JW . (1995): Age specific neurotoxicity in the rat associated with NMDA receptor blockade: potential relevance to schizophrenia? Biol Psychiatr 38: 788–796
Farber NB, Foster J, Duhan NL, Olney JW . (1996): Olanzapine and fluperlapine mimic clozapine in preventing MK-801 neurotoxicity. Schizophr Res 21: 33–37
Farber NB, Kim SH, Olney JW . (1997): Costimulation of muscarinic and non-NMDA glutamate receptors reproduces NMDA antagonist neurotoxicity. Soc Neurosci Abstr 23: 2308
Fix AS, Horn JW, Wightman KA, Johnson CA, Long GG, Storts RW, Farber N, Wozniak DF, Olney JW . (1993): Neuronal vacuolization and necrosis induced by the noncompetitive N-methyl-D-aspartate (NMDA) antagonist MK(+)801 (dizocilpine maleate): a light and electron microscopic evaluation of the rat retrosplenial cortex. Exp Neurol 123: 204–215
Fix AS, Wozniak DF, Truex LL, McEwen M, Miller JP, Olney JW . (1995): Quantitative analysis of factors influencing neuronal necrosis induced by MK-801 in the rat posterior cingulate/retrosplenial cortex. Brain Res 696: 194–204
Hoenicke EM, Vanecek SA, Woods JH . (1992): The discrimitive stimulus effects of clozapine in pigeons: Involvement of 5-hydroxytryptamine1C and 5-hydroxytryptamine2 receptors. J Pharmacol Exp Ther 263: 276–284
Javitt DC, Zukin SR . (1991): Recent advances in the phencyclidine model of schizophrenia. Am J Psychiatr 148: 1301–1308
Kim SH, Farber NB, Price MT, Olney JW . (1997): Clonidine suppresses MK801-induced acetylcholine release in rat posterior cingulate cortex: in vivo microdialysis study. Soc Neurosci Abstr 23: 2308
Krystal JH, Karper LP, Seibyl JP, Freeman GK, Delaney R, Bremner JD, Heninger GR, Bowers MB Jr, Charney DS . (1994): Subanesthetic effects of the noncompetitive NMDA antagonist, ketamine, in humans. Psychotomimetic, perceptual, cognitive, and neuroendocrine responses. Arch Gen Psychiatr 51: 199–214
Lahti AC, Koffel B, LaPorte DJ, Tamminga CA . (1995): Subanesthetic doses of ketamine stimulate psychosis in schizophrenia. Neuropsychopharmacology 13: 9–19
Leysen JE, Awouters F, Kennis L, Laduron PM, Vandenberk J, Janssen PAJ . (1981): Receptor binding profile of R 41 468, a novel antagonist at 5-HT2 receptors. Life Sci 28: 1015–1022
Lodge D, Anis NA . (1982): Effects of phencyclidine on excitatory amino acid activation of spinal interneurones in the cat. Eur J Pharmacol 77: 203–204
Lodge D, Aram JA, Church J, Davies SN, Martin D, O'Shaughnessey CT, Zeman S . (1987): Excitatory amino acids and phencyclidine-like drugs. In Hicks TP, Lodge D, McLennan H (eds), Excitatory Amino Acid Transmission. New York, Alan R. Liss Inc., pp 83–90
Luby ED, Cohen BD, Rosenbaum G, Gottlieb JS, Kelley R . (1959): Study of a new schizophrenomimetic drug—Sernyl. Arch Neurol Psychiatr 81: 363–369
Luby ED, Gottlieb JS, Cohen BD, Rosenbaum G, Domino EF . (1962): Model psychoses and schizophrenia. Am J Psychiatr 119: 61–67
Martin GR, Humphrey PPA . (1994): Receptors for 5-hydroxytryptamine: Current perspectives on classification and nomenclature. Neuropharmacology 33: 261–273
Mathews GA, Sofroniew MV, Rattray M . (1996): Differential expression of 5HT2A and 5HT2C serotonin receptor subtype mRNAs by hippocampal interneurons. Soc Neurosci Abstr 22: 1775
Mengod G, Pompeiano M, Martinez-Mir MI, Palacios JM . (1990): Localization of the mRNA for the 5-HT2 receptor by in situ hybridization histochemistry. Correlation with the distribution of receptor sites. Brain Res 524: 139–143
Newcomer JW, Farber NB, Jevtovic-Todorovic V, Selke G, Kelly A, Williams F, Craft S, Olney JW . (1996): NMDA glutamate receptor hypofunction: A model for schizophrenia-like cognitive and behavioral symptoms. Soc Neurosci Abstr 22: 240
Olney JW . (1988): Excitatory transmitters and neuropsychiatric disorders. In Ferrendelli JA, Collins RC, Johnson EM (eds), Neurobiology of Amino Acids, Peptides, and Trophic Factors. Boston, Kluwer Academic Publishers, pp 51–61
Olney JW, Labruyere J, Price MT . (1989): Pathological changes induced in cerebrocortical neurons by phencyclidine and related drugs. Science 244: 1360–1362
Olney JW, Farber NG . (1995a): NMDA antagonists as neuroprotectants, psychotogens, neurotoxins and instructive research tools. Neuropsychopharmacology 13: 335–345
Olney JW, Farber NB . (1995b): Glutamate receptor dysfunction and schizophrenia. Arch Gen Psychiatr 52: 998–1007
Rosenbaum G, Cohen BD, Luby ED, Gottlieb JS, Yelen D . (1959): Comparison of Sernyl with other drugs. Arch Gen Psychiatr 1: 651–656
Schmidt CJ, Sorensen SM, Kehne JH, Carr AA, Palfreyman MG . (1995): The role of 5-HT2A receptors in antipsychotic activity. Life Sci 56: 2209–2222
Sheldon PW, Aghajanian GK . (1990): Serotonin (5-HT) induces IPSPs in pyramidal layer of rat piriform cortex: Evidence for the involvement of a 5-HT2-activated interneuron. Brain Res 506: 62–69
Shen R, Andrade R . (1996): Facilitation of GABAergic neurotransmission by 5-HT2 receptor activation in hippocampus CA1 region. Soc Neurosci Abstr 22: 1775
Acknowledgements
Supported by a research award from the Scottish Rite Benevolent Foundation's Schizophrenia Research Program (NBF), Scientist Development Award DA 00290 (NBF), DA 05072 (JWO), AG 11355 (JWO) and a Research Scientist Award MH 38894 (JWO).
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Farber, N., Hanslick, J., Kirby, C. et al. Serotonergic Agents That Activate 5HT2A Receptors Prevent NMDA Antagonist Neurotoxicity. Neuropsychopharmacol 18, 57–62 (1998). https://doi.org/10.1016/S0893-133X(97)00127-9
Received:
Revised:
Accepted:
Issue Date:
DOI: https://doi.org/10.1016/S0893-133X(97)00127-9
Keywords
This article is cited by
-
Increased spontaneous MEG signal diversity for psychoactive doses of ketamine, LSD and psilocybin
Scientific Reports (2017)
-
Glutamate as a therapeutic target in psychiatric disorders
Molecular Psychiatry (2004)
-
Effects of the 5-HT2A Agonist Psilocybin on Mismatch Negativity Generation and AX-Continuous Performance Task: Implications for the Neuropharmacology of Cognitive Deficits in Schizophrenia
Neuropsychopharmacology (2003)
-
Receptor mechanisms and circuitry underlying NMDA antagonist neurotoxicity
Molecular Psychiatry (2002)
-
Treatment of negative and cognitive symptoms
Current Psychiatry Reports (1999)