Abstract
Animal and human studies have suggested that cannabidiol (CBD) may possess anxiolytic properties, but how these effects are mediated centrally is unknown. The aim of the present study was to investigate this using functional neuroimaging. Regional cerebral blood flow (rCBF) was measured at rest using 99mTc-ECD SPECT in 10 healthy male volunteers, randomly divided into two groups of five subjects. Each subject was studied on two occasions, 1 week apart. In the first session, subjects were given an oral dose of CBD (400 mg) or placebo, in a double-blind procedure. SPECT images were acquired 90 min after drug ingestion. The Visual Analogue Mood Scale was applied to assess subjective states. In the second session, the same procedure was performed using the drug that had not been administered in the previous session. Within-subject between-condition rCBF comparisons were performed using statistical parametric mapping (SPM). CBD significantly decreased subjective anxiety and increased mental sedation, while placebo did not induce significant changes. Assessment of brain regions where anxiolytic effects of CBD were predicted a priori revealed two voxel clusters of significantly decreased ECD uptake in the CBD relative to the placebo condition (p<0.001, uncorrected for multiple comparisons). These included a medial temporal cluster encompassing the left amygdala–hippocampal complex, extending into the hypothalamus, and a second cluster in the left posterior cingulate gyrus. There was also a cluster of greater activity with CBD than placebo in the left parahippocampal gyrus (p<0.001). These results suggest that CBD has anxiolytic properties, and that these effects are mediated by an action on limbic and paralimbic brain areas.
Similar content being viewed by others
INTRODUCTION
Cannabidiol (CBD) constitutes up to 40% of Cannabis sativa (Grlie, 1976) and has quite different psychological effects to the plant's best known constituent, Δ9-tetrahydrocannabinol (Δ9-THC) (Perez-Reyes et al, 1973; Zuardi et al, 1982). In particular, in animal studies CBD has effects similar to anxiolytic drugs in conditioned emotional paradigms (Zuardi and Karniol, 1983), the Vogel conflict test (Musty et al, 1984), and the elevated plus maze test (Guimaraes et al, 1990; Onaivi et al, 1990). Using the latter test, anxiolytic effects were also reported for three derivates of CBD, HU-219, HU-252, and HU-291 (Guimaraes et al, 1994). In humans, oral administration of CBD in healthy volunteers attenuates the anxiogenic effect of Δ9-tetrahydrocannabinol (Δ9-THC) (Zuardi et al, 1982). This effect does not seem to involve any pharmacokinetic interactions (Agurell et al, 1981; Zuardi et al, 1982), and CBD does not bind to the central known cannabinoid receptor, CB1, (Bisogno et al, 2001; Mechoulam et al, 2002) and hence cannot be a competitive antagonist (Howlett et al, 1992). CBD may thus possess inherent anxiolytic properties unrelated to THC-type activity. This is consistent with its anxiolytic effect on anxiety elicited by simulated public speaking (Zuardi et al, 1993a).
As the receptors that mediate the psychological effects of CBD are unknown, its mechanism of action on the brain is unclear. The aim of the present study was to use functional neuroimaging to investigate this. In view of its anxiolytic effect, we tested the hypothesis that CBD would affect neural activity in areas that normally mediate anxiety. We compared the effects of CBD and placebo on resting cerebral regional blood flow (rCBF) in healthy volunteers in a double-blind, cross-over design. Based on previous functional imaging studies of anxiety (Maddock and Buonocore, 1997; Fischer et al, 1996; Liotti et al, 2000; Ketter et al, 1996), we predicted that, relative to placebo, CBD would modulate rCBF in limbic and paralimbic areas: the orbitofrontal, cingulate and medial temporal cortex, and the insula.
MATERIALS AND METHODS
Subjects
A total of 10 healthy male postgraduate students were studied. None had undergone rCBF SPECT examinations or other nuclear medicine procedures before. All were right-handed as assessed by the Edinburgh Handedness Inventory (Oldfield, 1971), and were nonsmokers (of tobacco). Their mean age was 29.8 years (range 25–42 years, SD=5.1), their mean weight was 74.1 kg (67–85 kg, SD=6.05), and their body mass index ranged between 21 and 25 kg/m2. The subjects had not taken any medicines for at least 3 months before the study (Mathew et al, 1992). No subject had a history of head trauma, neurological, or major medical illnesses, based on a semistandardized medical questionnaire and physical examination. Neither the subjects (based on the Structured Clinical Interview for DSM-IV, First et al, 1997) nor their first-degree relatives (based on subjects' report) had a history of psychiatric illness. No subject had used marijuana more than five times in their lives (nor in the last year), and none had used any other illegal drug. The experiment was conducted with the understanding and consent of each subject, following approval by the local ethical committee.
Cannabidiol
CBD in powder, approximately 99.9% pure (supplied by THC-Pharm, Frankfurt, Germany), was dissolved in corn oil (Zuardi et al, 1993a, 1995). The same amount of corn oil was used as a placebo. The drug and placebo were packed inside identical gelatin capsules.
Self-Rating Scale
Subjective states were evaluated by means of the Visual Analogue Mood Scale (VAMS) of Norris (1971), translated into Portuguese by Zuardi and Karniol (1981b). It consists of 16 analogue scales to measure drug effects, which were arbitrarily divided by Norris into four factors: anxiety, physical sedation, mental sedation, and other feelings and attitudes. A factor analysis with the Portuguese version of this scale (Zuardi et al, 1993a) extracted four factors that can be identified with those of the Norris proposal. Prior to the experiment, each volunteer had performed a training session completing this scale.
Procedure
Subjects were told not to consume any alcohol for 24 h and caffeine for at least 4 h before each visit to the laboratory (Mathew et al, 1999). Subjects who reported having less than 6 h of sleep the previous night were excluded. After at least 8 h of fasting, subjects were instructed to have a light, standardized breakfast 2 h before the experiment. They were randomly divided into two groups of five subjects. Each subject was evaluated on two different occasions, 1 week apart. In the first session, after a 30-min period of adaptation, subjects were given a single dose of oral CBD (400 mg) or placebo, in a double-blind procedure. The sessions were held in the morning (between 0800 and 1200) to minimize the effects of circadian variation. SPECT image acquisition was performed 110 min after drug ingestion. Subjective ratings on the VAMS were made 30 min before drug ingestion, at the time of drug ingestion, and at 60 min and at 75 min afterwards. In the second session, an identical procedure was followed except that the other drug was administered (ie those given CBD in the first session received placebo in the second; and vice versa). Subjects were informed that they would receive CBD and placebo, but they were not told in which order. The investigators were also blind to the content of the capsules.
SPECT
Subjects had a venous cannula inserted into their right arm, and rested supine with minimal environmental sensory stimulation. They were instructed to keep their eyes closed under eye pads and to relax for 15 min without falling asleep. Their ears were unplugged. VAMS ratings were made just before and 15 min after insertion of the venous cannula. At 30 min after insertion of the venous cannula, 740 MBq (20 mCi) of ethyl-cisteinate dimer (ECD) labeled with technetium-99 m (99mTc-ECD) was injected. Subjects rested for an additional period of 5 min postinjection, after which the venous cannula was removed.
Image acquisition started 20 min after the 99mTc-ECD injection, using a double-detector SOPHA® DST system (Sophy Medical Vision, Twinsburg, USA). High-resolution low-energy collimators were used, with 128 views acquired on a 128 × 128 matrix (30 s per view), with a total acquisition time of 30 min, and approximately 75 000 counts/frame/head. Raw images were prefiltered with a Butterworth filter (order number 4, cutoff frequency 0.16), and reconstructed by filtered back-projection as transaxial slices parallel to the long axis of the temporal lobe. Attenuation correction was performed considering a pixel size of 2.55 mm and using the first-order algorithm of Chang (coefficient 0.12/cm).
Image Processing and Analysis
Images were analyzed using Statistical Parametric Mapping software (SPM99) (Friston et al, 1995). Reconstructed transaxial datasets were transferred to a PC (Pentium IV, 2.2 GHz, 512 Mb RAM), converted to Analyze format and reoriented to neurological convention (ie left=left). Placebo images were realigned to CBD images using sinc interpolation. Linear (translations and rotations) and nonlinear (7 × 8 × 7 nonlinear basis functions) deformations were used to register images to the SPM SPECT template, which is based on the Montreal Neurological Institute (MNI) template (Mazziotta et al, 1995). Finally, an isotropic Gaussian filter of 12 mm was applied to diminish interindividual differences, and to conform data to the theory of Gaussian Random Fields (Friston et al, 1995), in order to allow the subsequent application of parametric statistical tests.
Between-condition (CBD vs placebo) comparisons of regional tracer uptake were performed on a voxel-by-voxel basis using paired t-tests. Before statistical testing, the regional ECD uptake of every voxel in each subject was standardized to the mean global uptake of the image in that subject, using proportional scaling. Only voxels with signal intensities above a threshold of 0.8 of the global mean (calculated using the standardized values) entered the statistical analysis. The resulting statistics at each voxel were transformed to Z-scores, thresholded at Z=2.33 (corresponding to p<0.01, one-tailed), and displayed as 3-D statistical parametric maps (SPM). These maps were first inspected for the presence of voxel clusters of significant difference in the regions where effects of CBD had been predicted a priori (medial temporal, cingulate, orbitofrontal, and insular cortices). Clusters in these regions were considered as significant if they included voxels with Z-scores of 3.09 or greater (corresponding to one-tailed p<0.001), and contained more than 20 voxels. Levels of p<0.001, uncorrected for multiple comparisons, have been frequently used in previous SPM analyses of positron emission tomography (PET) (Dougherty et al, 1999; Bremner et al, 1999b) and SPECT (Blackwood et al, 1999; Busatto et al, 2000) data, and are considered to provide good protection against false-positive results when there are clear hypotheses as to the location of findings. The SPMs were also inspected for differences in other, unpredicted regions. These areas were reported as significant if they survived a correction for multiple comparisons based on Gaussian random field theory (p<0.05) (Friston et al, 1995).
For each voxel cluster showing significant between-condition differences, estimates were calculated for the mean, median, and maximal percentages of ECD count rate change (and their variances) (Table 1). These indices were obtained by partitioning the Student's t-test value of each voxel into its main components, with the numerator of the t statistic used as an approximation of the magnitude of the signal change for each contrast (placebo>CBD or CBD>placebo), and the denominator (the standard error) used to calculate the variances. The MNI coordinates for the voxels of maximal statistical significance for each anatomical brain region included in a given cluster were converted to the Talairach and Tournoux (1988) system using the method described by Brett et al (2002).
The four VAMS factors were submitted to an ANOVA for repeated measures in both CBD and placebo sessions. The differences between CBD and placebo in each phase of the experimental session (−30, 0, 1′00, 1′15) were analyzed by t-tests. Correlations between the regional tracer uptake and each of the VAMS factors scores were also investigated with SPM99, at the same statistical significance levels as described above for the between-condition rCBF comparisons. The last point in which the VAMS was applied (75′ after drug intake) was chosen for these correlations due to its proximity to the injection of the SPECT tracer. Moreover, this is the point where CBD is expected to have its maximum anxiolytic effect among all the time points chosen for assessment during the experimental session (Zuardi et al, 1993a). The choice for this time point was also based on previous studies, which have shown that the plasma peak of an oral dose of CBD usually occurs between 1 and 2 h after ingestion (Agurell et al, 1981).
RESULTS
Visual Analogue Mood Scale
The administration of CBD was associated with significantly decreased subjective anxiety (F(3,27)=18.56, p<0.001) and increased mental sedation (F(3,27)=42.85, p<0.001), while placebo was not (F(3,27)=1.86, p=0.16 and F(3,27)=2.24, p=0.11, respectively) (Figure 1). In addition, an analysis at each time point indicated the following: (i) CBD was associated with significantly decreased anxiety at cannula insertion (60′ after drug intake, t=2.95, p=0.009) and resting phases (75′ after drug intake, t=5.50, p<0.001) as compared to placebo; (ii) CBD was associated with significantly increased feelings of mental sedation at cannula insertion (60′ after drug intake, t=−3.91, p=0.001) and resting phases (75′ after drug intake, t=−3.67, p=0.002) as compared to placebo.
Effect of CBD and placebo (PLCB) on the four factors of the VAMS. Points are means (±SEM) of 10 healthy subjects in the following phases of the experiment: predrug (−30), drug intake (0), prestress (60), and adaptation (75). Asterisk (*) indicates significant difference from placebo in each phase. Triangle (▴) indicates ANOVA significant changes.
Between-Condition rCBF Comparisons
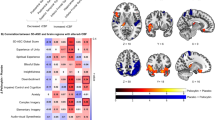
The SPM showing increases in ECD uptake in the CBD relative to placebo condition revealed only one cluster (>20 voxels) that surpassed the initial Z=2.33 statistical cutoff (Figure 2). This cluster, which achieved statistical significance at the p<0.001 level (uncorrected for multiple comparisons), was located in the medial temporal cortex, where the effects of CBD had been predicted a priori, and involved the left parahippocampal gyrus, extending inferiorly to encompass the left fusiform gyrus (Table 1).
The brain region where there was significantly increased rCBF in healthy volunteers (n=10) during CBD vs placebo has been overlaid on coronal sections (−18, −16, −14, −12) and sagittal sections (−28, −30, −32, −34) of a reference brain, imaged with structural MRI and spatially normalized into an approximation to the Tailarach and Tornoux (1988) stereotactic atlas. The results are displayed in neurological convention (ie left=left). The numbers associated with each frame represent the standard coordinate in the y- (for the coronal frames) and x-axis (for the sagittal frames). The voxel cluster shown was located in the left parahippocampal gyrus extending inferiorly to encompass the left fusiform gyrus (peak Z-score=3.69, coordinatesx,y,z=−30, −14, −30; p<0.0001 uncorrected for multiple comparisons; 114 voxels).
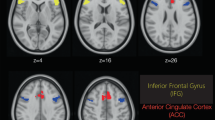
Significantly decreased (p<0.001, uncorrected for multiple comparisons), ECD uptake in the CBD relative to the placebo condition was evident in two regions where effects of CBD had been predicted a priori (Table 1). One cluster included the medial portion of the left amygdala–hippocampal complex and uncus, as well as the hypothalamus. The other was located in the superior portion of the left posterior cingulate gyrus (Brodmann area—BA31), extending towards the paracentral lobule (BA5/6). At the p<0.001 uncorrected level of significance, this SPM showed additional, unpredicted foci of decreased rCBF in the ECD relative to the placebo condition (>20 voxels) in the right cerebellum, medial occipital cortex, left inferior temporal, and posterior lateral frontal cortex, but none of these retained significance after correction for multiple comparisons.
Figure 3 displays, for each subject, the magnitude of tracer uptake changes between the CBD and placebo conditions at the voxel of maximal statistical significance in the regions where ECD uptake differences were observed (as summarized in Table 1). All 10 subjects showed greater ECD uptake values in the CBD condition relative to the placebo condition in the left parahippocampal/fusiform gyri. Of the 10 subjects, eight showed lower ECD activity in the CBD condition relative to the placebo condition in the left amygdala–hippocampal complex; eight in the left hypothalamus; and nine in the left posterior cingulate cortex/paracentral lobule (Figure 2). Similar patterns across individual subjects were observed when we used the mean tracer uptake values of all voxels included in the clusters of significant difference between the CBD and placebo conditions (data not shown).
Tracer uptake values during the CBD (filled circle) and PLCB (hollowed circle) conditions are plotted for the 10 subjects, using the voxel of maximal significant difference of each of the four regions reported in Table 1. From left to right and top to bottom: −4, −27, 47 (left posterior cingulate cortex/paracentral lobule), −6, −6, −8 (left hypothalamus), −16, −11, −21 (left amygdala–hippocampal complex), and −30, −15, −24 (left parahippocampal/fusiform gyri). Individual values were normalized to the global ECD uptake for each subject and condition. The graphs show that the large majority of individual subjects showed lower ECD activity in the CBD condition relative to the placebo condition in the left amygdala–hippocampus complex, hypothalamus, and posterior cingulate cortex/paracentral lobule, while all subjects had greater ECD uptake in the CBD condition relative to the placebo condition in the left parahippocampal/fusiform gyri.
Correlations with Subjective Status Ratings
No correlations were observed between subjective anxiety ratings and ECD uptake in the brain areas where the effects of CBD had been predicted a priori (p<0.001, uncorrected), or in other unpredicted areas after correction for multiple comparisons.
DISCUSSION
When undergoing neuroimaging procedures, such as PET or SPECT, subjects often report increased anxiety before scanning, which is greater than that during or after image acquisition (Grey et al, 2000; Gur et al, 1987; Giordani et al, 1990; Malizia, 1999). The results of the present study showed that a single dose of CBD induced significant decreases in state anxiety before SPECT scanning. Our data thus suggest that this compound has anxiolytic properties, consistent with the results from previous studies in both laboratory animals (Zuardi and Karniol, 1983; Musty et al, 1984; Guimaraes et al, 1990; Onaivi et al, 1990) and humans (Zuardi et al, 1982, 1993a).
The anxiolytic effects found in the present study were detected before the anxiety-evoking situation (the tracer injection and scanning procedure), indicating that CBD can affect anticipatory anxiety. In a previous study (Zuardi et al, 1993a), the anxiolytic effect of CBD was evident after the stress of public speaking. These antianxiety effects are in contrast to the anxiogenic effects of high doses of Δ9-THC (Malit et al, 1975; Zuardi et al, 1982; Mathew et al, 1999), and may help to reconcile apparently conflicting findings obtained with Cannabis sativa in relation to anxiety (Johns, 2001; Tournier et al, 2003).
Consistent with an anxiolytic effect, we found that CBD significantly modulated resting activity predominantly in limbic and paralimbic cortical areas, which are usually implicated in the pathophysiology of anxiety (Gray, 1982; Graeff, 1994). Thus, between-condition activity differences were detected in a left medial temporal cluster, which included portions of the amygdala and the hippocampus, as well as the hypothalamus, the left posterior cingulate gyrus, and the left parahippocampal gyrus.
The only brain region that showed significantly increased activity in the CBD relative to the placebo condition was the left parahippocampal gyrus. Deactivation of the parahippocampal region in healthy volunteers has been reported after panic attacks induced by lactate (Reiman et al, 1989) and CCK-4 (Javanmard et al, 1999), and with anxiety induced by presentation of combat-related images (Bremner et al, 1999b) and autobiographical memory scripts (Liotti et al, 2000). In addition, the abnormal asymmetry of resting activity in the parahippocampal gyri has been associated with panic disorder and with vulnerability to lactate-induced panic (Reiman et al, 1984, 1986; Nordahl et al, 1990, 1998; Bisaga et al, 1998; De Cristofaro et al, 1993). These studies suggest that anxiety can be associated with reduced parahippocampal activity, consistent with an anxiolytic effect of CBD and the increased activity in this region that we observed.
In contrast, activity in the left amygdala–hippocampal complex, hypothalamus, and posterior cingulate cortex decreased with CBD relative to placebo. The amygdala is thought to play a key role in mediating fear and anxiety (Deakin and Graeff, 1991; LeDoux, 1998; Gorman et al, 2000), being activated during fear conditioning (Furmark et al, 1997; Morris et al, 1998; LaBar et al, 1998; Buchel et al, 1998), while processing anxious faces (Breiter et al, 1996; Morris et al, 1996; Whalen et al, 1998; Hariri et al, 2002) and during pharmacologically induced anxiety (Ketter et al, 1996; Benkelfat et al, 1995; Servan-Schreiber et al, 1998). Functional and structural changes in the amygdala have also been reported in PTSD (Pitman et al, 2001; Rauch et al, 1996; Shin et al, 1997; Rauch et al, 2000; Liberzon et al, 1999), panic disorder (Uchida et al, 2003; Bystritsky et al, 2001), generalized anxiety disorder (Thomas et al, 2001; De Bellis et al, 2000), and in social (Birbaumer et al, 1998; Tillfors et al, 2001; Furmark et al, 2002) and simple phobias (Wik et al, 1997). The reduction in amygdala activity that we observed with CBD is thus consistent with the anxiolytic effect that it had in our subjects. The hippocampus has also been implicated in the processing of anxiety. Functional neuroimaging studies have shown increased activity in the hippocampus in association with anxiety in OCD (McGuire et al, 1994), panic disorder (Bisaga et al, 1998; Bystritsky et al, 2001; Boshuisen et al, 2002), PTSD (Osuch et al, 2001), and in social phobia (Schneider et al, 1999). However, other studies have reported either decreased or no difference in activity in the hippocampus in association with normal anxiety or anxiety disorders (Schuff et al, 2001; Schneider et al, 1999; Bremner et al, 1997; Fredrikson et al, 1997; Fischer et al, 1996; Paradiso et al, 1997; Liotti et al, 2000).
The hypothalamus is a major component of the central autonomic nervous system, and is often involved in mediating the effects of stress and anxiety (Afifi and Bergman, 1998). Functional imaging studies during fear and anxiety induction in healthy subjects (Fredrikson et al, 1995b; Javanmard et al, 1999) and in panic disorder patients (Boshuisen et al, 2002) have reported increases in the activity of the hypothalamic region, and hypothalamic–pituitary–adrenal axis abnormalities have been commonly reported in anxiety disorders (Hageman et al, 2001). The reduced hypothalamic activity that we observed is thus consistent with the anxiolytic effect of CBD.
The posterior cingulate cortex is strongly linked to temporolimbic structures (Vogt et al, 1992; Maddock, 1999; Afifi and Bergman, 1998), and is thought to play a central role in emotion and anxiety (MacLean, 1993; Maddock, 1999). Increased activity in the posterior cingulate gyrus has been associated with watching anxiety-provoking videos (Fischer et al, 1996, Fredrikson et al, 1995a), and with experimentally provoked obsessions and anxiety in patients with obsessive–compulsive disorder (OCD) (McGuire et al, 1994). Untreated patients with OCD show increased metabolism in the posterior cingulate (Perani et al, 1995) that decreases with treatment, with the change in posterior cingulate rCBF correlated with symptomatic improvement (Rauch et al, 2001, 2002). There have also been reports of increased posterior cingulate activation during symptom provocation in post-traumatic stress disorder (Bremner et al, 1999a) and panic disorder (Bystritsky et al, 2001). However, anxiety induction in phobic patients has been associated with deactivation in the posterior cingulate region (Wik et al, 1993) and Busatto et al (2000) reported a negative correlation between rCBF in the left posterior cingulate cortex and severity of symptoms in OCD.
We did not observe a correlation between the severity of anxiety and rCBF in the areas where activity was modulated by CBD, but this may have been difficult to detect because there was a 15-min gap between the points when the ratings were made and the SPECT tracer was injected.
While the areas where we found modulatory effects of CBD are thus implicated in mediating anxiety, and have also been associated with the anxiolytic effects of diazepam (Di Piero et al, 2001), citalopram (Van der Linden et al, 2000; Furmark et al, 2002), sertraline, and desipramine (Hoehn-Saric et al, 2001), these effects of CBD could be related to an effect other than on anxiety. For instance, we also observed sedative effects of CBD, confirming former findings in animals (Pickens, 1981; Monti, 1977; Colasanti et al, 1984; Zuardi et al, 1981a, 1991) and humans (Carlini et al, 1979; Zuardi et al, 1982, 1993b). This effect has been reported to be dose-related (Pickens, 1981) and CBD has also been shown to decrease wakefulness (Monti, 1977) and to cause longer sleep duration in insomniacs (Carlini and Cunha, 1981). Thus, the reduced hypothalamic activity observed after CBD use in our study could equally be related to sedative effects of CBD, as suggested to occur with other sedative compounds (Tung et al, 2001).
Other pharmacological effects of CBD have been reported in studies in laboratory animals and humans, such as anti-inflammatory (Malfait et al, 2000), anticonvulsant (Carlini et al, 1973; Izquierdo et al, 1973; Cunha et al, 1980), neuroprotective (Hampson et al, 1998), and hormonal effects (Zuardi et al, 1984, 1993a). In addition, the pharmacological profile of CBD is similar to that of clozapine, an ‘atypical’ antipsychotic drug (Zuardi et al, 1991, 1995), and both CBD and clozapine induce c-fos expression in the prefrontal cortex and lateral septal nucleus in rats (Zuardi et al, 2001). The mechanism(s) of action whereby CBD produces all these effects remains obscure. This is largely in contrast with the effects of Δ9-THC, which mimics the endogenous cannabinoids in many of its actions. CBD does not act through the known cannabinoid receptors, but the stereospecificity previously observed may indicate that CBD binds to another type of receptor in the brain (Mechoulam et al, 2002).
In conclusion, our results suggest that CBD has anxiolytic effects that are mediated through an action on limbic and paralimbic areas of the brain. However, the findings need to be seen as preliminary, given the limitations of the study. Firstly, it would have been desirable to measure plasma levels of CBD and relate them to the magnitude of change in rCBF. Without a dose–response curve, uncertainty about the regional cerebral effects of CBD remains. Nevertheless, it should be pointed out that it is not clear whether there is a relation between plasma levels of cannabinoids—especially CBD—and their clinical effects (Agurell et al, 1986). In addition, the subject sample was modest and the use of SPECT limited the study's statistical power. Finally, given the limited spatial resolution of the SPECT technique and the smoothing procedure, the interpretation of large foci of tracer uptake changes as involving different brain structures of small size (such as the amygdala, hippocampus, and hypothalamus) should be made with caution. These limitations could be overcome by examining a larger sample and using functional magnetic resonance imaging, which would permit the acquisition of greater numbers of images with a better spatial and temporal resolution.
References
Afifi AK, Bergman RA (1998). Functional Neuroanatomy: Text and Atlas. McGraw-Hill: New York.
Agurell S, Carlsson S, Lindgren JE, Ohlsson A, Gillespie H, Hollister L (1981). Interactions of delta 1-tetrahydrocannabinol with cannabinol and cannabidiol following oral administration in man. Assay of cannabinol and cannabidiol by mass fragmentography. Experientia 37: 1090–1092.
Agurell S, Halldin M, Lindgren JE, Ohlsson A, Widman M, Gillespie H et al (1986). Pharmacokinetics and metabolism of delta 1-tetrahydrocannabinol and other cannabinoids with emphasis on man. Pharmacol Rev 38: 21–43.
Benkelfat C, Bradwejn J, Meyer E, Ellenbogen M, Milot S, Gjedde A et al (1995). Functional neuroanatomy of CCK4-induced anxiety in normal healthy volunteers. Am J Psychiatry 152: 1180–1184.
Birbaumer N, Grodd W, Diedrich O, Klose U, Erb M, Lotze M et al (1998). fMRI reveals amygdala activation to human faces in social phobics. Neuroreport 9: 1223–1226.
Bisaga A, Katz JL, Antonini A, Wright CE, Margouleff C, Gorman JM et al (1998). Cerebral glucose metabolism in women with panic disorder. Am J Psychiatry 155: 1178–1183.
Bisogno T, Hanus L, De Petrocellis L, Tchilibon S, Ponde DE, Brandi I et al (2001). Molecular targets for cannabidiol and its synthetic analogues: effect on vanilloid VR1 receptors and on the cellular uptake and enzymatic hydrolysis of anandamide. Br J Pharmacol 134: 845–852.
Blackwood DH, Glabus MF, Dunan J, O'Carroll RE, Muir WJ, Ebmeier KP (1999). Altered cerebral perfusion measured by SPECT in relatives of patients with schizophrenia. Correlations with memory and P300. Br J Psychiatry 175: 357–366.
Boshuisen ML, Ter Horst GJ, Paans AM, Reinders AA, den Boer JA (2002). rCBF differences between panic disorder patients and control subjects during anticipatory anxiety and rest. Biol Psychiatry 52: 126–135.
Breiter HC, Etcoff NL, Whalen PJ, Kennedy WA, Rauch SL, Buckner RL et al (1996). Response and habituation of the human amygdala during visual processing of facial expression. Neuron 17: 875–887.
Bremner JD, Narayan M, Staib LH, Southwick SM, McGlashan T, Charney DS (1999a). Neural correlates of memories of childhood sexual abuse in women with and without posttraumatic stress disorder. Am J Psychiatry 156: 1787–1795.
Bremner JD, Randall P, Vermetten E, Staib L, Bronen RA, Mazure C et al (1997). Magnetic resonance imaging-based measurement of hippocampal volume in posttraumatic stress disorder related to childhood physical and sexual abuse—a preliminary report. Biol Psychiatry 41: 23–32.
Bremner JD, Staib LH, Kaloupek D, Southwick SM, Soufer R, Charney DS (1999b). Neural correlates of exposure to traumatic pictures and sound in Vietnam combat veterans with and without posttraumatic stress disorder: a positron emission tomography study. Biol Psychiatry 45: 806–816.
Brett M, Johnsrude IS, Owen AM (2002). The problem of functional localization in the human brain. Nat Rev Neurosci 3: 243–249.
Buchel C, Morris J, Dolan RJ, Friston KJ (1998). Brain systems mediating aversive conditioning: an event-related fMRI study. Neuron 20: 947–957.
Busatto GF, Zamignani DR, Buchpiguel CA, Garrido GE, Glabus MF, Rocha ET et al (2000). A voxel-based investigation of regional cerebral blood flow abnormalities in obsessive–compulsive disorder using single photon emission computed tomography (SPECT). Psychiatry Res 99: 15–27.
Bystritsky A, Pontillo D, Powers M, Sabb FW, Craske MG, Bookheimer SY (2001). Functional MRI changes during panic anticipation and imagery exposure. Neuroreport 12: 3953–3957.
Carlini EA, Cunha JM (1981). Hypnotic and antiepileptic effects of cannabidiol. J Clin Pharmacol 21(Suppl 8–9): 417–427.
Carlini EA, Leite JR, Tanhauser M, Berardi AC (1973). Cannabidiol and Cannabis sativa extract protect mice and rats against convulsive agents. J Pharm Pharmacol 25: 664–665.
Carlini EA, Masur J, Magalhães CCPB (1979). Possível efeito hipnótico do cannabidiol no ser humano. Estudo preliminar. Ciência e Cultura 31: 315–322.
Colasanti BK, Brown RE, Craig CR (1984). Ocular hypotension, ocular toxicity and neurotoxicity in response to marihuana extract and cannabidiol. Gen Pharmacol 15: 479–484.
Cunha J, Carlini EA, Pereira AE, Ramos OL, Pimentel C, Gagliardi R et al (1980). Chronic administration of cannabidiol to healthy volunteers and epileptic patients. Pharmacology 21: 175–185.
De Bellis MD, Casey BJ, Dahl RE, Birmaher B, Williamson DE, Thomas KM et al (2000). A pilot study of amygdala volumes in pediatric generalized anxiety disorder. Biol Psychiatry 48: 51–57.
De Cristofaro MT, Sessarego A, Pupi A, Biondi F, Faravelli C (1993). Brain perfusion abnormalities in drug-naive, lactate-sensitive panic patients: a SPECT study. Biol Psychiatry 33: 505–512.
Deakin JWF, Graeff FG (1991). 5-HT and mechanisms of defense. J Psychopharmacol 5: 305–315.
Di Piero V, Ferracuti S, Sabatini U, Tombari D, Di Legge S, Pantano P et al (2001). Diazepam effects on the cerebral responses to tonic pain: a SPET study. Psychopharmacology (Berl) 158: 252–258.
Dougherty DD, Shin LM, Alpert NM, Pitman RK, Orr SP, Lasko M et al (1999). Anger in healthy men: a PET study using script-driven imagery. Biol Psychiatry 46: 466–472.
First MB, Spitzer RL, Gibbon M, Williams JBW (1997). Structured Clinical Interview for DSM-IV Axis I Disorders—Clinician Version (SCID-CV). American Psychiatric Press: Washington, DC.
Fischer H, Wik G, Fredrikson M (1996). Functional neuroanatomy of robbery re-experience: affective memories studied with PET. Neuroreport 7: 2081–2086.
Fredrikson M, Fischer H, Wik G (1997). Cerebral blood flow during anxiety provocation. J Clin Psychiatry 58(Suppl 16): 16–21.
Fredrikson M, Wik G, Annas P, Ericson K, Stone-Elander S (1995a). Functional neuroanatomy of visually elicited simple phobic fear: additional data and theoretical analysis. Psychophysiology 32: 43–48.
Fredrikson M, Wik G, Fischer H, Andersson J (1995b). Affective and attentive neural networks in humans: a PET study of Pavlovian conditioning. Neuroreport 7: 97–101.
Friston KJ, Holmes AP, Worsley KJ, Poline JB, Frith CD, Frackowiak RSJ (1995). Statistical parametric maps in functional imaging: a general linear approach. Hum Brain Mapp 2: 189–210.
Furmark T, Fischer H, Wik G, Larsson M, Fredrikson M (1997). The amygdala and individual differences in human fear conditioning. Neuroreport 8: 3957–3960.
Furmark T, Tillfors M, Marteinsdottir I, Fischer H, Pissiota A, Langstrom B et al (2002). Common changes in cerebral blood flow in patients with social phobia treated with citalopram or cognitive-behavioral therapy. Arch Gen Psychiatry 59: 425–433.
Giordani B, Boivin MJ, Berent S, Betley AT, Koeppe RA, Rothley JM et al (1990). Anxiety and cerebral cortical metabolism in normal persons. Psychiatry Res 35: 49–60.
Gorman JM, Kent JM, Sullivan GM, Coplan JD (2000). Neuroanatomical hypothesis of panic disorder, revised. Am J Psychiatry 157: 493–505.
Graeff FG (1994). Neuroanatomy and neurotransmitter regulation of defensive behaviors and related emotions. Braz J Med Biol Res 27: 811–829.
Gray JA (1982). Precis of the neuropsychology of anxiety. An enquiry into the functions of the septohippocampal system. Behav Brain Sci 5: 469–534.
Grey SJ, Price G, Mathews A (2000). Reduction of anxiety during MR imaging: a controlled trial. Magn Reson Imaging 18: 351–355.
Grlie L (1976). A comparative study on some chemical and biological characteristics of various samples of cannabis resin. Bull Narcot 14: 37–46.
Guimaraes FS, Chiaretti TM, Graeff FG, Zuardi AW (1990). Antianxiety effect of cannabidiol in the elevated plus-maze. Psychopharmacology (Berl) 100: 558–559.
Guimaraes FS, de Aguiar JC, Mechoulam R, Breuer A (1994). Anxiolytic effect of cannabidiol derivatives in the elevated plus-maze. Gen Pharmacol 25: 161–164.
Gur RC, Gur RE, Resnick SM, Skolnick BE, Alavi A, Reivich M (1987). The effect of anxiety on cortical cerebral blood flow and metabolism. J Cereb Blood Flow Metab 7: 173–177.
Hageman I, Andersen HS, Jorgensen MB (2001). Post-traumatic stress disorder: a review of psychobiology and pharmacotherapy. Acta Psychiatr Scand 104: 411–422.
Hampson AJ, Grimaldi M, Axelroad J, Wink D (1998). Cannabidiol and (-)Δ9-tetrahydrocannabinol are neuroprotective antioxidants. Proc Nat Acad Sci USA 95: 8268–8273.
Hariri AR, Tessitore A, Mattay VS, Fera F, Weinberger DR (2002). The amygdala response to emotional stimuli: a comparison of faces and scenes. Neuroimage 17: 317–323.
Hoehn-Saric R, Schlaepfer TE, Greenberg BD, McLeod DR, Pearlson GD, Wong SH (2001). Cerebral blood flow in obsessive–compulsive patients with major depression: effect of treatment with sertraline or desipramine on treatment responders and non-responders. Psychiatry Res 108: 89–100.
Howlett AC, Evans D, Houston DB (1992). The cannabinoid receptor. In: Murphy L, Bartke A (eds) Marijuana/Cannabinoids: Neurobiology and Neurophysiology. CRC Press: Boca Raton, FL. pp 35–72.
Izquierdo I, Orshinger OA, Berardi AC (1973). Effect of cannabidiol and other Cannabis sativa compounds on hippocampal seizures discharges. Psychopharmacology 28: 95–102.
Javanmard M, Shlik J, Kennedy SH, Vaccarino FJ, Houle S, Bradwejn J (1999). Neuroanatomic correlates of CCK-4-induced panic attacks in healthy humans: a comparison of two time points. Biol Psychiatry 45: 872–882.
Johns A (2001). Psychiatric effects of cannabis. Br J Psychiatry 178: 116–122.
Ketter TA, Andreason PJ, George MS, Lee C, Gill DS, Parekh PI et al (1996). Anterior paralimbic mediation of procaine-induced emotional and psychosensory experiences. Arch Gen Psychiatry 53: 59–69.
LaBar KS, Gatenby JC, Gore JC, LeDoux JE, Phelps EA (1998). Human amygdala activation during conditioned fear acquisition and extinction: a mixed-trial fMRI study. Neuron 20: 937–945.
LeDoux J (1998). Fear and the brain: where have we been, and where are we going? Biol Psychiatry 44: 1229–1238.
Liberzon I, Taylor SF, Amdur R, Jung TD, Chamberlain KR, Minoshima S et al (1999). Brain activation in PTSD in response to trauma-related stimuli. Biol Psychiatry 45: 817–826.
Liotti M, Mayberg HS, Brannan SK, McGinnis S, Jerabek P, Fox PT (2000). Differential limbic-cortical correlates of sadness and anxiety in healthy subjects: implications for affective disorders. Biol Psychiatry 48: 30–42.
MacLean PD (1993). Perspectives on cingulate cortex in the limbic system. In: Vogt BA, Gabriel M (eds) Neurobiology of Cingulate Cortex and Limbic Thalamus. Birkhäuser: Basel. pp 1–15.
Maddock RJ (1999). The retrosplenial cortex and emotion: new insights from functional neuroimaging of the human brain. Trends Neurosci 22: 310–316.
Maddock RJ, Buonocore MH (1997). Activation of left posterior cingulate gyrus by the auditory presentation of threat-related words: an fMRI study. Psychiatry Res 75: 1–14.
Malfait AM, Gallily R, Sumariwalla PF, Malik AS, Andreakos E, Mechoulam R et al (2000). The nonpsychoactive cannabis constituent cannabidiol is an oral anti-arthritic therapeutic in murine collagen-induced arthritis. Proc Natl Acad Sci USA 97: 9561–9566.
Malit LA, Johnstone RE, Bourke DI, Kulp RA, Klein V, Smith TC (1975). Intravenous delta9-Tetrahydrocannabinol: effects of ventilatory control and cardiovascular dynamics. Anesthesiology 42: 666–673.
Malizia AL (1999). What do brain imaging studies tell us about anxiety disorders? J Psychopharmacol 13: 372–378.
Mathew RJ, Wilson WH, Chiu NY, Turkington TG, Degrado TR, Coleman RE (1999). Regional cerebral blood flow and depersonalization after tetrahydrocannabinol administration. Acta Psychiatr Scand 100: 67–75.
Mathew RJ, Wilson WH, Humphreys DF, Lowe JV, Wiethe KE (1992). Regional cerebral blood flow after marijuana smoking. J Cereb Blood Flow Metab 12: 750–758.
Mazziotta JC, Toga AW, Evans A, Fox P, Lancaster J (1995). A probabilistic atlas of the human brain: theory and rationale for its development. The International Consortium for Brain Mapping (ICBM). Neuroimage 2: 89–101.
McGuire PK, Bench CJ, Frith CD, Marks IM, Frackowiak RS, Dolan RJ (1994). Functional anatomy of obsessive–compulsive phenomena. Br J Psychiatry 164: 459–468.
Mechoulam R, Parker LA, Gallily R (2002). Cannabidiol: an overview of some pharmacological aspects. J Clin Pharmacol 42(Suppl 11): 11–19.
Monti JM (1977). Hypnoticlike effects of cannabidiol in the rat. Psychopharmacology (Berl) 55: 263–265.
Morris JS, Frith CD, Perrett DI, Rowland D, Young AW, Calder AJ et al (1996). A differential neural response in the human amygdala to fearful and happy facial expressions. Nature 383: 812–815.
Morris JS, Ohman A, Dolan RJ (1998). Conscious and unconscious emotional learning in the human amygdala. Nature 393: 467–470.
Musty RE, Conti LH, Mechoulam R (1984). Anxiolytic properties of cannabidiol. In: Harvey DJ (eds) Marihuana ‘84. Proceedings of the Oxford Symposium on Cannabis. IRL Press Limited: Oxford. pp 713–719.
Nordahl TE, Semple WE, Gross M, Mellman TA, Stein MB, Goyer P et al (1990). Cerebral glucose metabolic differences in patients with panic disorder. Neuropsychopharmacology 3: 261–272.
Nordahl TE, Stein MB, Benkelfat C, Semple WE, Andreason P, Zametkin A et al (1998). Regional cerebral metabolic asymmetries replicated in an independent group of patients with panic disorders. Biol Psychiatry 44: 998–1006.
Norris H (1971). The action of sedatives on brain stem oculomotor systems in man. Neuropharmacology 10: 181–191.
Oldfield RC (1971). The assessment and analysis of handedness: the Edinburgh inventory. Neuropsychologia 9: 97–113.
Onaivi ES, Green MR, Martin BR (1990). Pharmacological characterization of cannabinoids in the elevated plus maze. J Pharmacol Exp Ther 253: 1002–1009.
Osuch EA, Benson B, Geraci M, Podell D, Herscovitch P, McCann UD et al (2001). Regional cerebral blood flow correlated with flashback intensity in patients with posttraumatic stress disorder. Biol Psychiatry 50: 246–253.
Paradiso S, Robinson RG, Andreasen NC, Downhill JE, Davidson RJ, Kirchner PT et al (1997). Emotional activation of limbic circuitry in elderly normal subjects in a PET study. Am J Psychiatry 154: 384–389.
Perani D, Colombo C, Bressi S, Bonfanti A, Grassi F, Scarone S et al (1995). [18F]FDG PET study in obsessive–compulsive disorder. A clinical/metabolic correlation study after treatment. Br J Psychiatry 166: 244–250.
Perez-Reyes M, Timmons MC, Davis KH, Wall EM (1973). A comparison of the pharmacological activity in man of intravenously administered delta9-tetrahydrocannabinol, cannabinol, and cannabidiol. Experientia 29: 1368–1369.
Pickens JT (1981). Sedative activity of cannabis in relation to its Δ9-tetrahydrocannabinol and cannabidiol content. Br J Pharmacol 72: 649–656.
Pitman RK, Shin LM, Rauch SL (2001). Investigating the pathogenesis of posttraumatic stress disorder with neuroimaging. J Clin Psychiatry 62(Suppl 17): 47–54.
Rauch SL, Dougherty DD, Cosgrove GR, Cassem EH, Alpert NM, Price BH et al (2001). Cerebral metabolic correlates as potential predictors of response to anterior cingulotomy for obsessive compulsive disorder. Biol Psychiatry 50: 659–667.
Rauch SL, Shin LM, Dougherty DD, Alpert NM, Fischman AJ, Jenike MA (2002). Predictors of fluvoxamine response in contamination-related obsessive compulsive disorder: a PET symptom provocation study. Neuropsychopharmacology 27: 782–791.
Rauch SL, van der Kolk BA, Fisler RE, Alpert NM, Orr SP, Savage CR et al (1996). A symptom provocation study of posttraumatic stress disorder using positron emission tomography and script-driven imagery. Arch Gen Psychiatry 53: 380–387.
Rauch SL, Whalen PJ, Shin LM, McInerney SC, Macklin ML, Lasko NB et al (2000). Exaggerated amygdala response to masked facial stimuli in posttraumatic stress disorder: a functional MRI study. Biol Psychiatry 47: 769–776.
Reiman EM, Raichle ME, Butler FK, Herscovitch P, Robins E (1984). A focal brain abnormality in panic disorder, a severe form of anxiety. Nature 310: 683–685.
Reiman EM, Raichle ME, Robins E, Butler FK, Herscovitch P, Fox P et al (1986). The application of positron emission tomography to the study of panic disorder. Am J Psychiatry 143: 469–477.
Reiman EM, Raichle ME, Robins E, Mintun MA, Fusselman MJ, Fox PT et al (1989). Neuroanatomical correlates of a lactate-induced anxiety attack. Arch Gen Psychiatry 46: 493–500.
Schneider F, Weiss U, Kessler C, Muller-Gartner HW, Posse S, Salloum JB et al (1999). Subcortical correlates of differential classical conditioning of aversive emotional reactions in social phobia. Biol Psychiatry 45: 863–871.
Schuff N, Neylan TC, Lenoci MA, Du AT, Weiss DS, Marmar CR et al (2001). Decreased hippocampal N-acetylaspartate in the absence of atrophy in posttraumatic stress disorder. Biol Psychiatry 50: 952–959.
Servan-Schreiber D, Perlstein WM, Cohen JD, Mintun M (1998). Selective pharmacological activation of limbic structures in human volunteers: a positron emission tomography study. J Neuropsychiatry Clin Neurosci 10: 148–159.
Shin LM, Kosslyn SM, McNally RJ, Alpert NM, Thompson WL, Rauch SL et al (1997). Visual imagery and perception in posttraumatic stress disorder. A positron emission tomographic investigation. Arch Gen Psychiatry 54: 233–241.
Talairach J, Tournoux P (1988). Co-planar Stereotaxic Atlas of the Human Brain. Thieme: Stuttgart.
Thomas KM, Drevets WC, Dahl RE, Ryan ND, Birmaher B, Eccard CH et al (2001). Amygdala response to fearful faces in anxious and depressed children. Arch Gen Psychiatry 58: 1057–1063.
Tillfors M, Furmark T, Marteinsdottir I, Fischer H, Pissiota A, Langstrom B et al (2001). Cerebral blood flow in subjects with social phobia during stressful speaking tasks: a PET study. Am J Psychiatry 158: 1220–1226.
Tournier M, Sorbara F, Gindre C, Swendsen JD, Verdoux H (2003). Cannabis use and anxiety in daily life: a naturalistic investigation in a non-clinical population. Psychiatry Res 118: 1–8.
Tung A, Bluhm B, Mendelson WB (2001). The hypnotic effect of propofol in the medial preoptic area of the rat. Life Sci 69: 855.
Uchida RR, Del-Ben CM, Santos AC, Araujo D, Crippa JA, Guimaraes FS et al (2003). Decreased left temporal lobe volume of panic patients measured by magnetic resonance imaging. Braz J Med Biol Res 36: 925–929.
Van der Linden G, van Heerden B, Warwick J, Wessels C, van Kradenburg J, Zungu-Dirwayi N et al (2000). Functional brain imaging and pharmacotherapy in social phobia: single photon emission computed tomography before and after treatment with the selectiveserotonin reuptake inhibitor citalopram. Prog Neuropsychopharmacol Biol Psychiatry 24: 419–438.
Vogt BA, Finch DM, Olson CR (1992). Functional heterogeneity in cingulate cortex: the anterior executive and posterior evaluative regions. Cereb Cortex 2: 435–443.
Whalen PJ, Rauch SL, Etcoff NL, McInerney SC, Lee MB, Jenike MA (1998). Masked presentations of emotional facial expressions modulate amygdala activity without explicit knowledge. J Neurosci 18: 411–418.
Wik G, Fredrikson M, Ericson K, Eriksson L, Stone-Elander S, Greitz T (1993). A functional cerebral response to frightening visual stimulation. Psychiatry Res 50: 15–24.
Wik G, Fredrikson M, Fischer H (1997). Evidence of altered cerebral blood-flow relationships in acute phobia. Int J Neurosci 91: 253–263.
Zuardi AW, Cosme RA, Graeff FG, Guimarães FS (1993a). Effects of ipsapirone and cannabidiol on human experimental anxiety. J Psychopharmacol 7: 82–88.
Zuardi AW, Finkelfarb E, Bueno OFA, Musty RE, Karniol IG (1981a). Characteristics of the stimulus produced by the mixture of cannabidiol with Δ9-tetrahydrocannabinol. Arch Int Pharmacodyn 249: 137–146.
Zuardi AW, Guimarães FS, Guimarães VMC, Del Bel EA (2001). Cannabidiol. In: Grotenhermen F (ed) Cannabis Und Cannabinoide. Verlag Hans Huber: Bern. pp 381–393.
Zuardi AW, Guimaraes FS, Moreira AC (1993b). Effect of cannabidiol on plasma prolactin, growth hormone and cortisol in human volunteers. Braz J Med Biol Res 26: 213–217.
Zuardi AW, Karniol IG (1981b). Estudo transcultural de uma escala de auto-avaliação para estados subjetivos. J Bras Psiq 31: 403–406.
Zuardi AW, Karniol IG (1983). Changes in the conditioned emotional response of rats induced by Δ9-THC, CBD and mixture of the two cannabinoids. Arq Biol Tecnol 26: 391–397.
Zuardi AW, Morais SL, Guimaraes FS, Mechoulam R (1995). Antipsychotic effect of cannabidiol. J Clin Psychiatry 56: 485–486.
Zuardi AW, Rodrigues JA, Cunha JM (1991). Effects of cannabidiol in animal models predictive of antipsychotic activity. Psychopharmacology (Berl) 104: 260–264.
Zuardi AW, Shirakawa I, Finkelfarb E, Karniol IG (1982). Action of cannabidiol on the anxiety and other effects produced by delta 9-THC in normal subjects. Psychopharmacology (Berl) 76: 245–250.
Zuardi AW, Teixeira NA, Karniol IG (1984). Pharmacological interaction of the effects of Δ9-tetrahydrocannabinol and cannabidiol on serum corticosterone levels in rats. Arch Int Pharmacodyn 269: 12–19.
Acknowledgements
JASC and AWZ are recipients of Conselho Nacional de Desenvolvimento Científico e Tecnológico fellowships (Grants 200984/01-2 and 303770/85-6, respectively). This research was supported in part by the Fundação de Amparo à Pesquisa do Estado de São Paulo fellowship (Grants 02/13197-2, 01/00189-9, 99/12205-7, 99/09547-3, and 95/06195-8). We are grateful to Professor Dr José Antonio Marin Neto (Department of Medical Clinic, University of São Paulo, Ribeirão Preto, Brazil), for technical and logistic assistance. We also thank Professor Dr Frederico G Graeff (Department of Neuropsychiatry and Medical Psychology, University of São Paulo, Ribeirão Preto, Brazil) for comments and suggestions on the manuscript.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Crippa, J., Zuardi, A., Garrido, G. et al. Effects of Cannabidiol (CBD) on Regional Cerebral Blood Flow. Neuropsychopharmacol 29, 417–426 (2004). https://doi.org/10.1038/sj.npp.1300340
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.npp.1300340
Keywords
This article is cited by
-
Neuroimaging studies of cannabidiol and potential neurobiological mechanisms relevant for alcohol use disorders: a systematic review
Journal of Cannabis Research (2024)
-
The therapeutic potential of purified cannabidiol
Journal of Cannabis Research (2023)
-
Hippocampal circuit dysfunction in psychosis
Translational Psychiatry (2022)
-
The Effectiveness and Safety of Cannabidiol in Non-seizure-related Indications: A Systematic Review of Published Randomized Clinical Trials
Pharmaceutical Medicine (2022)
-
A double-blind, randomized, placebo-controlled test of the effects of cannabidiol on fear elicited by a 10% carbon dioxide-enriched air breathing challenge
Psychopharmacology (2022)