Abstract
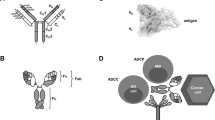
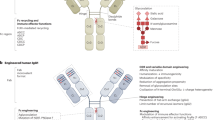
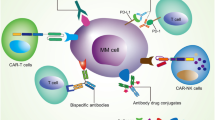
The potential for disease-specific targeting and low toxicity profiles have made monoclonal antibodies attractive therapeutic drug candidates. Antibody-mediated target cell killing is frequently associated with immune effector mechanisms such as antibody-directed cellular cytotoxicity, but they can also be induced by apoptotic processes. Antibody-directed mechanisms, including antigen crosslinking, activation of death receptors, and blockade of ligand-receptor growth or survival pathways, can elicit the induction of apoptosis in targeted cells. Depending on their mechanism of action, monoclonal antibodies can induce targeted cell-specific killing alone or can enhance target cell susceptibility to chemo- or radiotherapeutics by effecting the modulation of antiapoptotic pathways. This review will focus on the mechanisms by which antibodies are capable of eliciting programmed cell death either directly or indirectly within tumor cells.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 50 print issues and online access
$259.00 per year
only $5.18 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
Abbreviations
- ADCC:
-
antibody-dependent cellular cytotoxicity
- CDC:
-
complement-dependent cellular cytotoxicity
- IAP:
-
inhibitor of apoptosis
- RTK:
-
receptor tyrosine kinase
- TNFR:
-
tumor necrosis factor receptor
- TRAIL:
-
TNF-related apoptosis-inducing ligand receptor
- EGFR:
-
epidermal growth factor receptor
- IGF-1R:
-
insulin-like growth factor-1 receptor
- FGFR:
-
fibroblast growth factor receptor
- PDGFR:
-
platelet-derived growth factor receptor
- VEGF:
-
vascular endothelial growth factor
- PI3K:
-
phosphoinositol 3-kinase
- PLCγ:
-
phospholipase C gamma
- MAPK:
-
mitogen-activated protein kinase
- TGF-α:
-
transforming growth factor-α
- IR:
-
ionizing radiation
- SCCHN:
-
squamous cell carcinoma of the head and neck
- DNA-PK:
-
DNA-dependent protein kinase
- JNK:
-
c-jun N-terminal protein kinase
- NHL:
-
non-Hodgkin's lymphoma
- AML:
-
acute myelogenous leukemia
- CLL:
-
chronic lymphocytic leukemia
- ADEPT:
-
antibody-directed enzyme prodrug therapy
References
Alimandi M, Romano A, Curia MC, Muraro R, Fedi P, Aaronson SA, Di Fiore PP and Kraus MH . (1995). Oncogene, 10, 1813–1821.
Arteaga CL . (2002). Oncologist, 7S4, 31–39.
Ashkenazi A and Dixit VM . (1998). Science, 281, 1305–1308.
Baek JH, Jang JE, Kang CM, Chung HY, Kim ND and Kim KW . (2000). Oncogene, 19, 4621–4631.
Baetu TM and Hiscott J . (2002). Cytokine Growth Factor Rev., 13, 199–207.
Bagshawe KD and Begent RHJ . (1996). Adv. Drug Deliv. Rev., 22, 365–367.
Bandyopadhyay D, Mandal M, Adam L, Mendelsohn J and Kumar R . (1998). J. Biol. Chem., 273, 1568–1573.
Baselga J . (2002). Oncologist, 7S4, 2–8.
Baselga J, Norton L, Masui H, Pandiella A, Coplan K, Miller Jr WH and Mendelsohn J . (1993). J. Natl. Cancer Inst., 85, 1327–1333.
Benini S, Manara MC, Baldini N, Cerisano V, Massimo Serra, Mercuri M, Lollini PL, Nanni P, Picci P and Scotlandi K . (2001). Clin. Cancer Res., 7, 1790–1797.
Bianco C, Bianco R, Tortora G, Damiano V, Guerrieri P, Montemaggi P, Mendelsohn J, De Placido S, Bianco AR and Ciardiello F . (2000). Clin. Cancer Res., 6, 4343–4350.
Boulianne GL, Hozumi N and Shulman MJ . (1984). Nature, 312, 643–646.
Bruns CJ, Liu W, Davis DW, Shaheen RM, McConkey DJ, Wilson MR, Bucana CD, Hicklin DJ and Ellis LM . (2000). Cancer, 89, 488–499.
Bruns CJ, Shrader M, Harbison MT, Portera C, Solorzano CC, Jauch KW, Hicklin DJ, Radinsky R and Ellis LM . (2002). Int. J. Cancer, 102, 101–108.
Burgering BM and Coffer PJ . (1995). Nature, 376, 599–602.
Byrd JC, Kitada S, Flinn IW, Aron JL, Pearson M, Lucas D and Reed JC . (2002). Blood, 99, 1038–1043.
Cantley LC . (2002). Science, 296, 1655–1657.
Cardarelli PM, Quinn M, Buckman D, Fang Y, Colcher D, King DJ, Bebbington C and Yarranton G . (2002). Cancer Immunol. Immunother., 51, 15–24.
Carmeliet P and Jain RK . (2000). Nature, 407, 249–257.
Carter P . (2001). Nat. Rev: Cancer, 1, 118–129.
Carter P, Presta L, Gorman CM, Ridgway JB, Henner D, Wong WL, Rowland AM, Kotts C, Carver ME and Shepard HM . (1992). Proc. Natl. Acad. Sci. USA, 89, 4285–4289.
Ciardiello F, Bianco R, Damiano V, De Lorenzo S, Pepe S, De Placido S, Fan Z, Mendelsohn J, Bianco AR and Tortora G . (1999). Clin. Cancer Res., 5, 909–916.
Clynes RA, Towers TL, Presta LG and Ravetch JV . (2000). Nat. Med., 6, 443–446.
Danielsen AJ and Maihle NJ . (2002). Growth Factors, 20, 1–15.
Datta SR, Brunet A and Greenberg ME . (1999). Genes Dev., 13, 2905–2927.
Deardon C . (2002). Biodrugs, 16, 283–301.
de Bono JS and Rowinsky EK . (2002). Trends Mol. Med., 8S4, S19–S26.
de Haard HJ, van Neer N, Reurs A, Hufton SE, Roovers RC, Henderikx P, de Bruine AP, Arends JW and Hoogenboom HR . (1999). J. Biol. Chem., 274, 18218–18230.
De Vries C, Escobedo JA, Ueno H, Houck K, Ferrara N and Williams LT . (1992). Science, 255, 989–991.
Dias S, Hattori K, Heissig B, Zhu Z, Wu Y, Witte L, Hicklin DJ, Tateno M, Bohlen P, Moore MA and Rafii S . (2001). Proc. Natl. Acad. Sci. USA, 98, 10857–10862.
Dias S, Hattori K, Zhu Z, Heissig B, Choy M, Lane W, Wu Y, Chadburn A, Hyjek E, Gill M, Hicklin DJ, Witte L, Moore MA and Rafii S . (2000). J. Clin. Invest., 106, 511–521.
Dougall WC, Qian X, Peterson NC, Miller MJ, Samanta A and Greene MI . (1994). Oncogene, 9, 2109–2123.
Ekedahl J, Joseph B, Grigoriev MY, Muller M, Magnusson C, Lewensohn R and Zhivotovsky B . (2002). Exp. Cell Res., 279, 277–290.
Ferrara N . (1995). Breast Cancer Res. Treat., 36, 127–137.
Findley HW and Zhou M . (1999). Leukemia, 13, 147–149.
Fischer-Colbrie J, Witt A, Heinzl H, Speiser P, Czerwenka K, Sevelda P and Zeillinger R . (1997). Anticancer Res., 17, 613–619.
Folkman J . (1991). J. Natl. Cancer Inst., 82, 4–6.
Folkman J . (1995). Nat. Med., 1, 27–31.
Gerber HP, Dixit V and Ferrara N . (1998a). J. Biol. Chem., 273, 13313–13316.
Gerber HP, McMurtrey A, Kowalski J, Yan M, Keyt BA, Dixit V and Ferrara N . (1998b). J. Biol. Chem., 273, 30336–30343.
Ghetie MA, Bright H and Vitetta ES . (2001). Blood, 97, 1392–1398.
Gille H, Kowaski J, Li B, Lecouter J, Moffat B, Zioncheck TF, Pelletier N and Ferrara N . (2001). J. Biol. Chem., 276, 3222–3230.
Glennie MJ and Johnson PW . (2001). Immunol. Today, 21, 403–410.
Gupta VK, Jaskowiak NT, Beckett MA, Mauceri HJ, Grunstein J, Johnson RS, Calvin DA, Nodzenski E, Pejovic M, Kufe DW, Posner MC and Weichselbaum RR . (2002). Cancer J., 8, 47–54.
Harmey JH and Bouchier-Hayes D . (2002). BioEssays, 24, 280–283.
Hengartner MO . (2000). Nature, 407, 770–776.
Hoogenboom HR and Chames P . (2000). Immunol. Today, 21, 371–378.
Hu L, Hofmann J, Zaloudek C, Ferrara N, Hamilton T and Jaffe RB . (2002). Am. J. Pathol., 161, 1917–1924.
Huang SM, Bock JM and Harari PM . (1999). Cancer Res., 59, 1935–1940.
Huang SM and Harari PM . (1999). Invest. New Drugs, 17, 259–269.
Huang SM and Harari PM . (2000). Clin. Cancer Res., 6, 2166–2174.
Ichikawa K, Liu W, Zhao L, Wang Z, Liu D, Ohtsuka T, Zhang H, Mountz JD, Koopman WJ, Kimberly RP and Zhou T . (2001). Nat. Med., 7, 954–960.
Igney FH and Krammer PH . (2002). Nat. Rev. Cancer, 2, 277–288.
Inoue K, Slaton JW, Davis DW, Hicklin DJ, McConkey DJ, Karashima T, Radinsky R and Dinney CP . (2001). Clin. Cancer Res., 6, 2635–2643.
Irmler M, Thome M, Hahne M, Schneider P, Hofmann K, Steiner V, Bodmer JL, Schroter M, Burns K, Mattmann C, Rimoldi D, French LE and Tschopp J . (1997). Nature, 388, 190–195.
Jain RK . (2002). Semin. Oncol., 29, 3–9.
Jones PT, Dear PH, Foote J, Neuberger MS and Winter G . (1986). Nature, 321, 522–525.
Kandasamy K and Srivastava RK . (2002). Cancer Res., 62, 4929–4937.
Kennedy SG, Wagner AJ, Conzen SD, Jordan J, Bellacosa A, Tsichlis PN and Hay N . (1997). Genes Dev., 11, 701–713.
Keppler-Hafkemeyer A, Kreitman RJ and Pastan I . (2000). Int. J. Cancer, 87, 86–94.
Kim ES, Khuri FR and Herbst RS . (2001). Curr. Opin. Oncol., 13, 506–513.
Kim J, Li B, Winer J, Armanini M, Gillett N, Phillip HS and Ferrara N . (1993). Nature, 362, 841–844.
Knappik A, Ge L, Honegger A, Pack P, Fischer M, Wellnhofer G, Hoess A, Wolle J, Pluckthun A and Virnekas B . (2000). J. Mol. Biol., 296, 57–86.
Kozin SV, Boucher Y, Hicklin DJ, Bohlen P, Jain RK and Suit HD . (2001). Cancer Res., 61, 39–44.
Kreitman RJ . (2001). Curr. Pharmacol. Biotechnol., 2, 313–325.
Kreitman RJ, Wilson WH, Robbins D, Margulies I, Stetler-Stevenson M, Waldmann TA and Pastan I . (1999). Blood, 94, 3340–3348.
Kreitman RJ, Wilson WH, White JD, Stetler-Stevenson M, Jaffe ES, Giardina S, Waldmann TA and Pastan I . (2000). J. Clin. Oncol., 18, 1622–1636.
Lee S, Yang W, Lan KH, Sellappan S, Klos K, Hortobagyi G, Hung MC and Yu D . (2002). Cancer Res., 62, 5703–5710.
Li B, Fuh G, Meng G, Xin X, Gerritsen ME, Cunningham B and De Vos AM . (2000). J. Biol. Chem., 275, 29823–29828.
Liu B and Fan Z . (2001). Oncogene, 20, 3726–3734.
Liu B, Fang M, Schmidt M, Lu Y, Mendelsohn J and Fan Z . (2000). Br. J. Cancer, 82, 1991–1999.
Mallat Z and Tedgui Z . (2000). Br. J. Pharmacol., 130, 947–962.
Maloney DG . (2001). Anticancer Drugs, 12S2, S1–S4.
Mandal M, Adam L, Mendelsohn J and Kumar R . (1998). Oncogene, 27, 999–1007.
Maung ZT, MacLean FR, Reid MM, Pearson AD, Proctor SJ, Hamilton PJ and Hall AG . (1994). Br. J. Haematol., 88, 105–109.
Mendelsohn J . (1990). Semin. Cancer Biol., 1, 339–344.
Mendelsohn J . (1997). Clin. Cancer Res., 3, 2703–2707.
Mendelsohn J . (2000). Clin. Cancer Res., 6, 747–753.
Mendez MJ, Green LL, Corvalan JR, Jia XC, Maynard-Currie CE, Yang XD, Gallo ML, Louie DM, Lee DV, Erickson KL, Luna J, Roy CM, Abderrahim H, Kirschenbaum F, Noguchi M, Smith DH, Fukushima A, Hales JF, Klapholz S, Finer MH, Davis CG, Zsebo KM and Jakobovits A . (1997). Nat. Genet., 15, 146–156.
Mesri M, Morales-Ruiz M, Ackermann EJ, Bennett CF, Pober JS, Sessa WC and Altieri DC . (2001). Am. J. Pathol., 158, 1757–1765.
Milas L, Mason K, Hunter N, Petersen S, Yamakawa M, Ang K, Mendelsohn J and Fan Z . (2000). Clin. Cancer Res., 6, 701–708.
Millauer B, Wizigmann-Voos S, Schnurch H, Martinez R, Moller NPH, Risau W and Ullrich A . (1993). Cell, 72, 835–846.
Miyashita T and Reed JC . (1993). Blood, 81, 151–157.
Monks NR, Blakey DC, Curtin NJ, East SJ, Heuze A and Newell DR . (2001). Br. J. Cancer, 85, 764–771.
Morrison SL, Johnson MJ, Herzenberg LA and Oi VT . (1984). Proc. Natl. Acad. Sci. USA, 81, 6851–6855.
Nagata S . (1997). Cell, 88, 355–365.
Nagata S and Golstein P . (1995). Science, 267, 1449–1456.
Napier MP, Sharma SK, Springer CJ, Bagshawe KD, Green AJ, Martin J, Stribbling SM, Cushen N, O'Malley D and Begent RH . (2000). Clin. Cancer Res., 6, 765–772.
Nicholson S, Sainsbury JR, Halcrow P, Chambers P, Farndon JR and Harris AL . (1989). Lancet, 1, 182–185.
Nor JE, Christensen J, Liu J, Peters M, Mooney DJ, Strieter RM and Polverini PJ . (2001). Cancer Res., 61, 2183–2188.
O'Connor DS, Schechner JS, Adida C, Mesri M, Rothermel AL, Li F, Nath AK, Pober JS and Altieri DC . (2000). Am. J. Pathol., 156, 393–398.
Ogasawara J, Watanabe-Fukunaga R, Adachi M, Matsuzawa A, Kasugai T, Kitamura Y, Itoh N, Suda T and Nagata S . (1993). Nature, 364, 806–809.
Ohtsuka T and Zhou T . (2002). J. Biol. Chem., 277, 29294–29303.
Ong SH, Hadari YR, Gotoh N, Guy GR, Schlessinger J and Lax I . (2001). Proc. Natl. Acad. Sci. USA, 98, 6074–6079.
Overholser JP, Prewett MC, Hooper AT, Waksal HW and Hicklin DJ . (2000). Cancer, 89, 74–82.
Pan G, Ni J, Wei YF, Yu G, Gentz R and Dixit VM . (1997). Science, 277, 815–818.
Pan G, Ni J, Yu G, Wei YF and Dixit VM . (1998). FEBS Lett., 424, 41–45.
Parrizas M, Saltiel AR and LeRoith D . (1997). J. Biol. Chem., 272, 154–161.
Pegram M, Hsu S, Lewis G, Pietras R, Beryt M, Sliwkowski M, Coombs D, Baly D, Kabbinavar F and Slamon D . (1999). Oncogene, 18, 2241–2251.
Peltenburg LT . (2000). Q. J. Nucl. Med., 44, 355–364.
Penuel E, Schaefer G, Akita RW and Sliwkowski MX . (2001). Semin. Oncol., 28, 36–42.
Pietras RJ, Poen JC, Gallardo D, Wongvipat PN, Lee HJ and Slamon DJ . (1999). Cancer Res., 59, 1347–1355.
Pollak M . (2000). Eur. J. Cancer, 36, 1224–1228.
Posey J, Yang B, Khazaeli M, Fox F, Engel J, Needle M and Wasksal H . (2002). Am. Soc. Clin. Oncol, (Proceedings of the 38th Annual meeting) 21, 17a (Abstract 63).
Press OW, Eary JF, Gooley T, Gopal AK, Liu S, Rajendran JG, Maloney DG, Petersdorf S, Bush SA, Durack LD, Martin PJ, Fisher DR, Wood B, Borrow JW, Porter B, Smith JP, Mathews DC, Appelbaum FR and Bernstein ID . (2000). Blood, 96, 2934–2942.
Presta LG . (2002). Curr. Pharmacol. Biotechnol., 3, 237–256.
Prewett M, Huber J, Li Y, Santiago A, O'Connor W, King K, Overholser J, Hooper A, Pytowski B, Witte L, Bohlen P and Hicklin DJ . (1999). Cancer Res., 59, 5209–5218.
Reed JC . (2002). Nat. Rev. Drug Discov., 1, 111–121.
Rosen LS . (2002). Cancer Control, 9, 36–44.
Rowan W, Tite J, Topley P and Brett SJ . (1998). Immunology, 95, 427–436.
Sasaki M, Kumazaki T, Tanimoto K and Nishiyama M . (2003). Int. J. Oncol., 22, 181–186.
Sato JD, Kawamoto T, Le AD, Mendelsohn J, Polikoff J and Sato GH . (1983). Mol. Biol. Med., 1, 511–529.
Scaffidi C, Schmitz I, Zha J, Korsmeyer SJ, Krammer PH and Peter ME . (1998). J. Biol. Chem., 274, 22532–22538.
Schier R, McCall A, Adams GP, Marshall KW, Merritt H, Yim M, Crawford RS, Weiner LM, Marks C and Marks JD . (1996). J. Mol. Biol., 263, 551–567.
Senter PD and Springer CJ . (2001). Adv. Drug Deliv. Rev., 53, 247–264.
Shaheen RM, Tseng WW, Vellagas R, Liu W, Ahmad SA, Jung YD, Reinmuth N, Drazan KE, Bucana CD, Hicklin DJ and Ellis LM . (2001). Int. J. Oncol., 18, 221–226.
Shan D, Ledbetter JA and Press OW . (2000). Cancer Immunol. Immunother., 48, 673–683.
Sheridan MT, O'Dwyer T, Seymour CB and Mothersill CE . (1997). Radiat. Oncol. Invest., 5, 180–186.
Shibuya M, Yamaguchi S, Yamane A, Ikeda T, Tojo A, Matsushime H and Sato M . (1990). Oncogene, 5, 519–524.
Sievers EL . (2000). Cancer Chemother. Pharmacol., 46, 18–22.
Sievers EL, Appelbaum FR, Spielberger RT, Forman SJ, Flowers D, Smith FO, Shannon-Dorcy K, Berger MS and Bernstein ID . (1999). Blood, 93, 3678–3684.
Slamon DJ, Clark GM, Wong SG, Levin WJ, Ullrich A and McGuire WL . (1987). Science, 235, 177–182.
Slamon DJ, Leyland-Jones B, Shak S, Fuchs H, Paton V, Bajamonde A, Fleming T, Eiermann W, Wolter J, Pegram M, Baselga J and Norton L . (2001). N. Engl. J. Med., 344, 783–792.
Soffer SZ, Moore JT, Kim E, Huang J, Yokoi A, Manley C, O'Toole K, Stolar C, Middlesworth W, Yamashiro DJ and Kandel JJ . (2001). J. Pediatr. Surg., 36, 1177–1181.
Tedder TF and Engel P . (1994). Immunol. Today, 15, 450–454.
Terman BI, Dougher-Vermazen M, Carrion ME, Dimtrov D, Armellino DC, Gospodarowicz D and Bohlen P . (1992). Biochem. Biophys. Res. Commun., 187, 1579–1586.
Tortora G, Caputo R, Pomatico G, Pepe S, Bianco AR, Agrawal S, Mendelsohn J and Ciardiello F . (1999). Clin. Cancer Res., 5, 875–881.
Tran J, Rak J, Sheehan C, Saibil SD, LaCasse E, Korneluk RG and Kerbel RS . (1999). Biochem. Biophys. Res. Commun., 264, 781–788.
Trauth BC, Klas C, Peters AM, Matzku S, Moller P, Falk W, Debatin KM and Krammer PH . (1989). Science, 245, 301–305.
van der Kolk LE, Evers LM, Omene C, Lens SM, Lederman S, van Lier RA, van Oers MH and Eldering E . (2002). Leukemia, 16, 1735–1744.
Vaughan TJ, Osbourn JK and Tempest PR . (1998). Nat. Biotechnol., 16, 535–539.
Volm M, Efferth T and Mattern J . (1992). Anticancer Res., 12, 11–20.
Waltenberger J, Claesson-Welsh L, Siegbahn A, Shibuya M and Heldin CH . (1994). J. Biol. Chem., 269, 26988–26995.
Ward ES and Ghetie V . (1995). Ther. Immunol., 2, 77–94.
Winter G and Milstein C . (1991). Nature, 349, 293–299.
Witte L, Hicklin DJ, Zhu Z, Pytowski B, Kotanides H, Rockwell P and Bohlen P . (1998). Cancer Metast. Rev., 17, 155–161.
Witzig TE, Gordon LI, Cabanillas F, Czuczman MS, Emmanouilides C, Joyce R, Pohlman BL, Bartlett NL, Wiseman GA, Padre N, Grillo-Lopez AJ, Multani P and White CA . (2002). J. Clin. Oncol., 20, 2453–2463.
Witzig TE, White CA, Wiseman GA, Gordon LI, Emmanouilides C, Raubitschek A, Janakiraman N, Gutheil J, Schilder RJ, Spies S, Silverman DH, Parker E and Grillo-Lopez AJ . (1999). J. Clin. Oncol., 17, 3793–3803.
Wu X, Fan Z, Masui H, Rosen N and Mendelsohn J . (1995). J. Clin. Invest., 95, 1897–1905.
Yakes FM, Chinratanalab W, Ritter CA, King W, Seelig S and Arteaga CL . (2002). Cancer Res., 62, 4132–4141.
Yarnold S and Fell HP . (1994). Cancer Res., 54, 506–512.
Zhang L, Yu D, Hicklin DJ, Hannay JAF, Ellis LM and Pollock RE . (2002). Cancer Res., 62, 2034–2042.
Zhu Z, Bohlen P and Witte L . (2002). Curr. Cancer Drug Targets, 2, 135–156.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ludwig, D., Pereira, D., Zhu, Z. et al. Monoclonal antibody therapeutics and apoptosis. Oncogene 22, 9097–9106 (2003). https://doi.org/10.1038/sj.onc.1207104
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.onc.1207104
Keywords
This article is cited by
-
Excess reactive oxygen species production mediates monoclonal antibody-induced human embryonic stem cell death via oncosis
Cell Death & Differentiation (2017)
-
Role of Bruton’s tyrosine kinase inhibitors in HIV-1-infected cells
Journal of NeuroVirology (2015)
-
Separation of SSEA-4 and TRA-1–60 Labelled Undifferentiated Human Embryonic Stem Cells from A Heterogeneous Cell Population Using Magnetic-Activated Cell Sorting (MACS) and Fluorescence-Activated Cell Sorting (FACS)
Stem Cell Reviews and Reports (2009)
-
Tumor specificity and in vivo targeting of an antibody against exon 9 deleted E-cadherin in gastric cancer
Journal of Cancer Research and Clinical Oncology (2007)
-
Monoclonal antibody mechanisms of action in cancer
Immunologic Research (2007)