Abstract
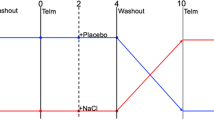
Hypertension is associated with impaired fibrinolysis. Both angiotensin receptor blockers (ARB) and the DASH (Dietary Approaches to Stop Hypertension) diet effectively lower blood pressure in hypertensive patients. Some evidence suggests that treatment with ARBs could increase fibrinolysis, however, data is conflicting. The impact of the DASH diet on fibrinolytic parameters is not known. Fifty-five hypertensive participants (35 African-American, 20 white) were randomly assigned to receive 8 weeks of either a control diet or the DASH diet. The diets did not differ in sodium content (approximately 3 g/day). Within each diet, individuals were randomly assigned to receive losartan or placebo for 4 weeks in double-blind, cross-over fashion. Tissue plasminogen activator (t-PA) antigen, t-PA activity, plasminogen activator inhibitor-1 (PAI-1) activity and plasma renin activity (PRA) were measured at the end of a 2-week run-in period on the control diet and after each treatment period. The DASH diet did not affect markers of fibrinolysis. Losartan significantly lowered t-PA antigen levels (−1.8 ng/mL, P = 0.045), but had no effect on t-PA or PAI-1 activities. This effect was more pronounced in whites (−4.1 ng/mL (P = 0.003)) compared with African-Americans (−0.3 ng/mL (P = 0.7), P-interaction = 0.03). Results were not materially affected by adjustment for basline values or changes in blood pressure. This study demonstrates that losartan reduces t-PA antigen levels in white, but not African-American hypertensive individuals. In contrast, the DASH diet had no significant effect on markers of fibrinolysis in whites or African-Americans.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 digital issues and online access to articles
$119.00 per year
only $9.92 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Pfeffer MA et al. Effect of captopril on mortality and morbidity inpatients with left ventricular dysfunction after myocardial infarction N Engl J Med 1992; 327: 669–677
Lewis EJ, Hunsicker LG, Bain RP, Rohde RD . The effect of angiotensin-converting enzyme inhibition on diabetic nephropathy. The Collaborative Study Group N Engl J Med 1993; 329: 1456–1462
Pitt B et al. Randomised trial of losartan versus capto-pril inpatients over 65 with heart failure (Evaluation of Losartan in the Elderly Study, ELITE) Lancet 1997; 349: 747–752
Sharma D, Buyse M, Pitt B, Rucinska EJ . Meta-analysis of observed mortality data from all-controlled, double-blind, multiple-dose studies of losartan in heart failure. Losartan Heart Failure Mortality Meta-analysis Study Group Am J Cardiol 2000; 85: 187–192
Heart Outcomes Prevention Evaluation Study Investigators. Effects of ramipril on cardiovascular and microvascular outcomes in people with diabetes mellitus: results of the HOPE study and MICRO-HOPE substudy Lancet 2000; 355: 253–259
Levy PJ et al. Inhibition of platelet aggregability by losartan in essential hypertension Am J Cardiol 2000; 86: 1188–1192
Lopez-Farre A et al. Angiotensin II AT(1) receptor antagonists and platelet activation Nephrol Dial Transplant 2001; 16 (Suppl 1): 45–49
Folsom AR et al. Prospective study of hemostatic factors and incidence of coronary heart disease: the Atherosclerosis Risk in Communities (ARIC) study Circulation 1997; 96: 1102–1108
Hamsten A, deFaire U, Walldius G . Plaminogen activator inhibitor in plasma: risk factor for recurrent myocardial infarction Lancet 1987; 2: 3–9
Juhan-Vague I et al. Fibrinolytic factors and the risk of myocardial infarction or sudden death inpatients with angina pectoris. ECAT Study Group. European Concerted Action on Thrombosis and Disabilities Circulation 1996; 94: 2057–2063
Meeade TW et al. Haemostatic function and cardiovascular death: early results of a prospective study Lancet 1980; 1: 1050–1054
Meeade TW et al. Haemostatic function and ischemic heart disease: principle results of the Northwick Park Heart Study Lancet 1986; 2: 533–537
Ridker PM et al. Stimulation of plasminogen activator inhibitor in vivo by infusion of angiotensin II. Evidence of a potential interaction between the renin-angiotensin system and fibrinolytic function Circulation 1993; 87: 1969–1973
Brown NJ, Agirbasli M, Vaughan DE . Comparative effect of angiotensin-converting enzyme inhibition and angiotensin II type 1 receptor antagonism on plasma fibrinolytic balance in humans Hypertension 1999; 34: 285–290
Brown NJ et al. Effect of activation and inhibition of the renin-angiotensin system of plasma PAI-1 Hypertension 1998; 32: 965–971
Goodfield NE, Newby DE, Ludlam CA, Flapan AD . Effects of acute angiotensin II type 1 receptor antagonism and angiotensin converting enzyme inhibition on plasma fibrinolytic parameters inpatients with heart failure Circulation 1999; 99: 2983–2985
Erdem Y et al. Effects of angiotensin converting enzyme and angiotensin II receptor inhibition on impaired fibrinolysis in systemic hypertension Am J Hypertens 1999; 12: 1071–1076
Ridker PM et al. Prospective study of endogenous tissue plasminogen activator and risk of stroke Lancet 1994; 343: 940–943
Ridker PM et al. Endogenous tissue-type plasminogen activator and risk of myocardial infarction Lancet 1993; 341: 1165–1168
Macko RF et al. Elevated tissue plasminogen activator antigen and stroke risk: The Stroke Prevention In Young Women Study Stroke 1999; 30: 7–11
Mallion JM, Goldberg AI . Global efficacy and tolerability of losartan, an angiotensin II subtype 1-receptor antagonist, in the treatment of hypertension Blood Press Suppl 1996; 2: 82–86
Appel LJ et al. A clinical trial of the effects of dietary patterns on blood pressure N Engl J Med 1997; 336: 1117–1124
Miller ER III, Appel LJ, Risby TH . Effect of dietary patterns on measures of lipid peroxidation: results from a randomized clinical trial Circulation 1998; 98: 2390–2395
Appel LJ et al. Effect of dietary patterns on serum homocysteine: results of a randomized, controlled feeding study Circulation 2000; 102: 852–857
Marckmann P, Toubro S, Astrup A . Sustained improvement in blood lipids, coagulation, and fibrinolysis after major weight loss in obese subjects Eur J Clin Nutr 1998; 52: 329–333
Marckmann P, Sandstrom B, Jespersen J . Favorable long-term effect of a low-fat/high-fiber diet on human blood coagulation and fibrinolysis Arterioscler Thromb 1993; 13: 505–511
Marckmann P, Sandstrom B, Jespersen J . Fasting blood coagulation and fibrinolysis of young adults unchanged by reduction in dietary fat content Arterioscler Thromb 1992; 12: 201–205
Lopez-Segura F et al. Monounsaturated fatty acid-enriched diet decreases plasma plasminogen activator inhibitor type 1 Arterioscler Thromb Vasc Biol 1996; 16: 82–88
Mehrabian M, Peter JB, Barnard RJ, Lusis AJ . Dietary regulation of fibrinolytic factors Atherosclerosis 1990; 84: 25–32
He J et al. The renin-angiotensin system and blood pressure: differences between blacks and whites Am J Hypertens 1999; 12: 555–562
Materson BJ et al. Single-drug therapy for hypertension in men. A comparison of six antihypertensive agents with placebo. The Department of Veterans Affairs Cooperative Study Group on Antihypertensive Agents N Engl J Med 1993; 328: 914–921
Sacks FM et al. Rationale and design of the Dietary Approaches to Stop Hyptertension trial (DASH): a multi-center controlled-feeding study of dietary patterns to lower blood pressure Ann Epidemiol 1995; 5: 108–118
Zeger SL, Liang KY . An overview of methods for the analysis of longitudinal data Stat Med 1992; 11: 1825–1839
Chandler WL et al. Clearance of tissue plasminogen activator (tPA) and tPA/plasminogen activator inhibitor type I (PAI-1) complex relationship to elevated tPA antigen inpatients with high PAI-1 activity levels Circulation 1997; 96: 761–768
Kerins DM, Hao Q, Vaughan DE . Angiotensin induction of PAI-1 expression in endothelial cells is mediated by the hexapeptide angiotensin IV J Clin Invest 1995; 96: 2515–2520
Iso H, Folsom AR et al. Hemostatic variables in Japanese and Caucasian men. Tissue plasminogen activator, antithrombin III, and protein C and their relations to coronary risk factors Am J Epidemiol 1990; 132: 41–46
Lip GY et al. Relation of endothelium, thrombogenesis, and hemorheology in systemic hypertension to ethnicity and left ventricular hypertrophy Am J Cardiol 1997; 80: 1566–1571
Ridker PM, Hennekens CH, Stampfer MJ, Manson JE, Vaughan DE . Prospective study of endogenous tissue plasminogen activator and risk of stroke Lancet 1994; 343: 940–943
Ridker PM . Plasma concentration of endogenous tissue plasminogen activator and the occurrence of future cardiovascular events J Thromb Thrombolysis 1994; 1: 35–40
Mutanen M, Aro A . Coagulation and fibrinolysis factors in healthy subjects consuming high stearic or trans fatty acid diets Thromb Haemost 1997; 77: 99–104
Thompson SG et al for the European Concerted Action on Thrombosis and Disabilities Angina Pectoris Study Group. Hemostatic factors and the risk of myocardial infarction or sudden death inpatients with angina pectoris N Engl J Med 1999; 332: 635–641
Acknowledgements
We would like to thank the participants and staff, whose hard work and dedication made this work possible. We would also like to acknowledge the Baltimore VA Geriatrics Research, Education, and Clinical Center (GRECC). This work was supported by a grant from the National Institutes of Health (T32PE10025) and a grant from Merck and Company, Inc.
Author information
Authors and Affiliations
Corresponding author
Additional information
5Endocrinology-Hypertension Division, Brigham and Women’s Hospital, Harvard Medical School, Boston, MA, USA
Rights and permissions
About this article
Cite this article
Erlinger, T., Conlin, P., Macko, R. et al. The impact of angiotensin II receptor blockade and the DASH diet on markers of endogenous fibrinolysis. J Hum Hypertens 16, 391–397 (2002). https://doi.org/10.1038/sj.jhh.1001401
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.jhh.1001401