Abstract
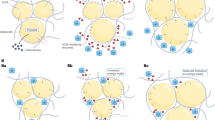
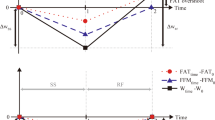
In people trying to lose weight, there are often repeated cycles of weight loss and regain. Weight cycling is, however, not limited to obese adults but affects people of normal weight, particularly young women, who are unhappy with their appearance. Furthermore, the onset of a pattern of weight cycling is shifting towards younger ages, owing to the increasing prevalence of overweight and obesity in children and adolescents, and the pressure from the media and society for a slim image even for normal weight children. Although there is still controversy whether weight cycling promotes body fat accumulation and obesity, there is mounting evidence from large population studies for increased cardiovascular risks in response to a behavior of weight cycling. Potential mechanisms by which weight cycling contributes to cardiovascular morbidity include hypertension, visceral fat accumulation, changes in adipose tissue fatty acid composition, insulin resistance and dyslipidemia. Moreover, fluctuations in blood pressure, heart rate, sympathetic activity, glomerular filtration rate, blood glucose and lipids that may occur during weight cycling – with overshoots above normal values during weight regain periods – put an additional load on the cardiovascular system, and may be easily overlooked if humans or animals are studied during a state of relatively stable weight. Overshoot of those risks factors, when repeated over time, will stress the cardiovascular system and probably contribute to the overall cardiovascular morbidity of weight cycling.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Weight Cycling. National task force on the prevention and treatment of obesity. JAMA 1994; 272: 1196–1202.
Elfhag K, Rossner S . Who succeeds in maintaining weight loss? A conceptual review of factors associated with weight loss maintenance and weight regain. Obes Rev 2005; 6: 67–85.
Williamson DF, Serdula MK, Anda RF, Levy A, Byers T . Weight loss attempts in adults: goals, duration, and rate of weight loss. Am J Public Health 1992; 82: 1251–1257.
Serdula MK, Mokdad AH, Williamson DF, Galuska DA, Mendlein JM, Heath GW . Prevalence of attempting weight loss and strategies for controlling weight. JAMA 1999; 282: 1353–1358.
Foreyt JP, Brunner RL, Goodrick GK, Cutter G, Brownell KD, St Jeor ST . Psychological correlates of weight fluctuation. Int J Eat Disord 1995; 17: 263–275.
Field AE, Byers T, Hunter DJ, Laird NM, Manson JE, Williamson DF et al. Weight cycling, weight gain, and risk of hypertension in women. Am J Epidemiol 1999; 150: 573–579.
Kroke A, Liese AD, Schulz M, Bergmann MM, Klipstein-Grobusch K, Hoffmann K et al. Recent weight changes and weight cycling as predictors of subsequent two year weight change in a middle-aged cohort. Int J Obes Relat Metab Disord 2002; 26: 403–409.
Lahti-Koski M, Mannisto S, Pietinen P, Vartiainen E . Prevalence of weight cycling and its relation to health indicators in Finland. Obes Res 2005; 13: 333–341.
Black DR, Pack DJ, Hovell MF . A time-series analysis of longitudinal weight changes in two adult women. Int J Obes 1991; 15: 623–633.
Brownell KD, Steen SN, Wilmore JH . Weight regulation practices in athletes: analysis of metabolic and health effects. Med Sci Sports Exerc 1987; 19: 546–556.
Bendixen H, Madsen J, Bay-Hansen D, Boesen U, Ovesen LF, Bartels EM et al. An observational study of slimming behavior in Denmark in 1992 and 1998. Obes Res 2002; 10: 911–922.
Janssen I, Katzmarzyk PT, Boyce WF, Vereecken C, Mulvihill C, Roberts C et al. Comparison of overweight and obesity prevalence in school-aged youth from 34 countries and their relationships with physical activity and dietary patterns. Obes Rev 2005; 6: 123–132.
Lazzer S, Boirie Y, Poissonnier C, Petit I, Duche P, Taillardat M et al. Longitudinal changes in activity patterns, physical capacities, energy expenditure, and body composition in severely obese adolescents during a multidisciplinary weight-reduction program. Int J Obes (London) 2005; 29: 37–46.
Lazzer S, Vermorel M, Montaurier C, Meyer M, Boirie Y . Changes in adipocyte hormones and lipid oxidation associated with weight loss and regain in severely obese adolescents. Int J Obes (London) 2005; 29: 1184–1191.
Bellisle F, Monneuse MO, Steptoe A, Wardle J . Weight concerns and eating patterns: a survey of university students in Europe. Int J Obes Relat Metab Disord 1995; 19: 723–730.
Casper RC, Offer D . Weight and dieting concerns in adolescents, fashion or symptom? Pediatrics 1990; 86: 384–390.
Field AE, Cheung L, Wolf AM, Herzog DB, Gortmaker SL, Colditz GA . Exposure to the mass media and weight concerns among girls. Pediatrics 1999; 103: E36.
Taveras EM, Rifas-Shiman SL, Field AE, Frazier AL, Colditz GA, Gillman MW . The influence of wanting to look like media figures on adolescent physical activity. J Adolesc Health 2004; 35: 41–50.
Dittmar H, Halliwell E, Ive S . Does Barbie make girls want to be thin? The effect of experimental exposure to images of dolls on the body image of 5- to 8-year-old girls. Dev Psychol 2006; 42: 283–292.
Kazemi M, Shearer H, Choung YS . Pre-competition habits and injuries in Taekwondo athletes. BMC Musculoskelet Disord 2005; 6: 26.
Hall CJ, Lane AM . Effects of rapid weight loss on mood and performance among amateur boxers. Br J Sports Med 2001; 35: 390–395.
Horswill CA . Weight loss and weight cycling in amateur wrestlers: implications for performance and resting metabolic rate. Int J Sport Nutr 1993; 3: 245–260.
McCargar LJ, Crawford SM . Metabolic and anthropometric changes with weight cycling in wrestlers. Med Sci Sports Exerc 1992; 24: 1270–1275.
Melby CL, Schmidt WD, Corrigan D . Resting metabolic rate in weight-cycling collegiate wrestlers compared with physically active, noncycling control subjects. Am J Clin Nutr 1990; 52: 409–414.
Perriello Jr VA, Almquist J, Conkwright Jr D, Cutter D, Gregory D, Pitrezzi MJ et al. Health and weight control management among wrestlers. A proposed program for high school athletes. Va Med Q 1995; 122: 179–183, 185.
McCargar LJ, Simmons D, Craton N, Taunton JE, Birmingham CL . Physiological effects of weight cycling in female lightweight rowers. Can J Appl Physiol 1993; 18: 291–303.
Koutedakis Y, Jamurtas A . The dancer as a performing athlete: physiological considerations. Sports Med 2004; 34: 651–661.
Steen SN, Oppliger RA, Brownell KD . Metabolic effects of repeated weight loss and regain in adolescent wrestlers. JAMA 1988; 260: 47–50.
Prentice AM, Jebb SA, Goldberg GR, Coward WA, Murgatroyd PR, Poppitt SD et al. Effects of weight cycling on body composition. Am J Clin Nutr 1992; 56: 209S–216S.
Muls E, Kempen K, Vansant G, Saris W . Is weight cycling detrimental to health? A review of the literature in humans. Int J Obes Relat Metab Disord 1995; 19 (Suppl 3): S46–S50.
Wing RR . Weight cycling in humans: a review of the literature. Ann Behav Med 1992; 14: 113–119.
Blair SN, Shaten J, Brownell K, Collins G, Lissner L . Body weight change, all-cause mortality, and cause-specific mortality in the Multiple Risk Factor Intervention Trial. Ann Intern Med 1993; 119: 749–757.
Hamm P, Shekelle RB, Stamler J . Large fluctuations in body weight during young adulthood and twenty-five-year risk of coronary death in men. Am J Epidemiol 1989; 129: 312–318.
Lissner L, Odell PM, D'Agostino RB, Stokes III J, Kreger BE, Belanger AJ et al. Variability of body weight and health outcomes in the Framingham population. N Engl J Med 1991; 324: 1839–1844.
Peters ET, Seidell JC, Menotti A, Arayanis C, Dontas A, Fidanza F et al. Changes in body weight in relation to mortality in 6441 European middle-aged men: the Seven Countries Study. Int J Obes Relat Metab Disord 1995; 19: 862–868.
Diaz VA, Mainous III AG, Everett CJ . The association between weight fluctuation and mortality: results from a population-based cohort study. J Commun Health 2005; 30: 153–165.
Pasman WJ, Saris WH, Westerterp-Plantenga MS . Predictors of weight maintenance. Obes Res 1999; 7: 43–50.
Field AE, Manson JE, Taylor CB, Willett WC, Colditz GA . Association of weight change, weight control practices, and weight cycling among women in the Nurses' Health Study II. Int J Obes Relat Metab Disord 2004; 28: 1134–1142.
Zhang H, Tamakoshi K, Yatsuya H, Murata C, Wada K, Otsuka R et al. Long-term body weight fluctuation is associated with metabolic syndrome independent of current body mass index among Japanese men. Circ J 2005; 69: 13–18.
Saarni SE, Rissanen A, Sarna S, Koskenvuo M, Kaprio J . Weight cycling of athletes and subsequent weight gain in middleage. Int J Obes (London) 2006; 30: 1639–1644.
Colditz GA, Willett WC, Rotnitzky A, Manson JE . Weight gain as a risk factor for clinical diabetes mellitus in women. Ann Intern Med 1995; 122: 481–486.
Huang Z, Willett WC, Manson JE, Rosner B, Stampfer MJ, Speizer FE et al. Body weight, weight change, and risk for hypertension in women. Ann Intern Med 1998; 128: 81–88.
Willett WC, Manson JE, Stampfer MJ, Colditz GA, Rosner B, Speizer FE et al. Weight, weight change, and coronary heart disease in women. Risk within the ‘normal’ weight range. JAMA 1995; 273: 461–465.
Calle EE, Rodriguez C, Walker-Thurmond K, Thun MJ . Overweight, obesity, and mortality from cancer in a prospectively studied cohort of US adults. N Engl J Med 2003; 348: 1625–1638.
Trentham-Dietz A, Newcomb PA, Egan KM, Titus-Ernstoff L, Baron JA, Storer BE et al. Weight change and risk of postmenopausal breast cancer (United States). Cancer Cause Control 2000; 11: 533–542.
Manore MM, Berry TE, Skinner JS, Carroll SS . Energy expenditure at rest and during exercise in nonobese female cyclical dieters and in nondieting control subjects. Am J Clin Nutr 1991; 54: 41–46.
Rodin J, Radke-Sharpe N, Rebuffe-Scrive M, Greenwood MR . Weight cycling and fat distribution. Int J Obes 1990; 14: 303–310.
Lauer JB, Reed GW, Hill JO . Effects of weight cycling induced by diet cycling in rats differing in susceptibility to dietary obesity. Obes Res 1999; 7: 215–222.
Reed GW, Cox G, Yakubu F, Ding L, Hill JO . Effects of weight cycling in rats allowed a choice of diet. Am J Physiol 1993; 264: R35–R40.
Lim K, Murakami E, Lee S, Shimomura Y, Suzuki M . Effects of intermittent food restriction and refeeding on energy efficiency and body fat deposition in sedentary and exercised rats. J Nutr Sci Vitaminol (Tokyo) 1996; 42: 449–468.
Ernsberger P, Koletsky RJ, Baskin JS, Collins LA . Consequences of weight cycling in obese spontaneously hypertensive rats. Am J Physiol 1996; 270: R864–R872.
Prevot A, Dulloo A, Montani JP . Weight cycling per se, independently of excess weight gain, promotes fat accumulation and insulin resistance [Abstract]. FASEB J 2005; 19: A988.
Kochan Z . Increased lipogenic potential of rat adipose tissue after repeated dieting – the role of SREBP-1 transcription factor. Cell Mol Biol Lett 2003; 8: 901–909.
Stelmanska E, Korczynska J, Swierczynski J . Tissue-specific effect of refeeding after short- and long-term caloric restriction on malic enzyme gene expression in rat tissues. Acta Biochim Pol 2004; 51: 805–814.
Karbowska J, Kochan Z, Swierczynski J . Increase of lipogenic enzyme mRNA levels in rat white adipose tissue after multiple cycles of starvation-refeeding. Metabolism 2001; 50: 734–738.
Sea MM, Fong WP, Huang Y, Chen ZY . Weight cycling-induced alteration in fatty acid metabolism. Am J Physiol Regul Integr Comp Physiol 2000; 279: R1145–R1155.
Guagnano MT, Ballone E, Pace-Palitti V, Vecchia RD, D'Orazio N, Manigrasso MR et al. Risk factors for hypertension in obese women. The role of weight cycling. Eur J Clin Nutr 2000; 54: 356–360.
Guagnano MT, Pace-Palitti V, Carrabs C, Merlitti D, Sensi S . Weight fluctuations could increase blood pressure in android obese women. Clin Sci (London) 1999; 96: 677–680.
Wallner SJ, Luschnigg N, Schnedl WJ, Lahousen T, Sudi K, Crailsheim K et al. Body fat distribution of overweight females with a history of weight cycling. Int J Obes Relat Metab Disord 2004; 28: 1143–1148.
van der Kooy K, Leenen R, Seidell JC, Deurenberg P, Hautvast JG . Effect of a weight cycle on visceral fat accumulation. Am J Clin Nutr 1993; 58: 853–857.
Rebuffe-Scrive M, Hendler R, Bracero N, Cummunigs N, McCarthy S, Rodin J . Biobehavioral effects of weight cycling. Int J Obes Relat Metab Disord 1994; 18: 651–658.
Leyton J, Drury PJ, Crawford MA . Differential oxidation of saturated and unsaturated fatty acids in vivo in the rat. Br J Nutr 1987; 57: 383–393.
Hudgins LC, Hirsch J . Changes in abdominal and gluteal adipose-tissue fatty acid compositions in obese subjects after weight gain and weight loss. Am J Clin Nutr 1991; 53: 1372–1377.
Riemersma RA, Wood DA, Butler S, Elton RA, Oliver M, Salo M et al. Linoleic acid content in adipose tissue and coronary heart disease. BMJ (Clin Res Ed) 1986; 292: 1423–1427.
Field AE, Manson JE, Laird N, Williamson DF, Willett WC, Colditz GA . Weight cycling and the risk of developing type 2 diabetes among adult women in the United States. Obes Res 2004; 12: 267–274.
Yatsuya H, Tamakoshi K, Yoshida T, Hori Y, Zhang H, Ishikawa M et al. Association between weight fluctuation and fasting insulin concentration in Japanese men. Int J Obes Relat Metab Disord 2003; 27: 478–483.
Olson MB, Kelsey SF, Bittner V, Reis SE, Reichek N, Handberg EM et al. Weight cycling and high-density lipoprotein cholesterol in women: evidence of an adverse effect: a report from the NHLBI-sponsored WISE study. Women's Ischemia Syndrome Evaluation Study Group. J Am Coll Cardiol 2000; 36: 1565–1571.
Rubins HB, Robins SJ, Collins D, Fye CL, Anderson JW, Elam MB et al. Gemfibrozil for the secondary prevention of coronary heart disease in men with low levels of high-density lipoprotein cholesterol. Veterans Affairs High-Density Lipoprotein Cholesterol Intervention Trial Study Group. N Engl J Med 1999; 341: 410–418.
Kajioka T, Tsuzuku S, Shimokata H, Sato Y . Effects of intentional weight cycling on non-obese young women. Metabolism 2002; 51: 149–154.
Miller GD, Dimond AG, Stern JS . The effect of repeated episodes of dietary restriction and refeeding on systolic blood pressure and food intake in exercise-trained normotensive rats. Obes Res 2000; 8: 324–336.
Ernsberger P, Nelson DO . Refeeding hypertension in dietary obesity. Am J Physiol 1988; 254: R47–R55.
Ernsberger P, Koletsky RJ, Baskin JS, Foley M . Refeeding hypertension in obese spontaneously hypertensive rats. Hypertension 1994; 24: 699–705.
Contreras RJ, Williams VL . Dietary obesity and weight cycling: effects on blood pressure and heart rate in rats. Am J Physiol 1989; 256: R1209–R1219.
Van Vliet BN, Chafe LL, Antic V, Schnyder-Candrian S, Montani JP . Direct and indirect methods used to study arterial blood pressure. J Pharmacol Toxicol Methods 2000; 44: 361–373.
Dobrian AD, Davies MJ, Prewitt RL, Lauterio TJ . Development of hypertension in a rat model of diet-induced obesity. Hypertension 2000; 35: 1009–1015.
Mizelle HL, Edwards TC, Montani JP . Abnormal cardiovascular responses to exercise during the development of obesity in dogs. Am J Hypertens 1994; 7: 374–378.
Hall JE, Brands MW, Dixon WN, Smith Jr MJ . Obesity-induced hypertension. Renal function and systemic hemodynamics. Hypertension 1993; 22: 292–299.
Antic V, Tempini A, Montani JP . Serial changes in cardiovascular and renal function of rabbits ingesting a high-fat, high-calorie diet. Am J Hypertens 1999; 12: 826–829.
Schulz M, Liese AD, Boeing H, Cunningham JE, Moore CG, Kroke A . Associations of short-term weight changes and weight cycling with incidence of essential hypertension in the EPIC-Potsdam Study. J Hum Hypertens 2005; 19: 61–67.
Graci S, Izzo G, Savino S, Cattani L, Lezzi G, Berselli ME et al. Weight cycling and cardiovascular risk factors in obesity. Int J Obes Relat Metab Disord 2004; 28: 65–71.
Montani JP, Antic V, Yang Z, Dulloo A . Pathways from obesity to hypertension: from the perspective of a vicious triangle. Int J Obes Relat Metab Disord 2002; 26 (Suppl 2): S28–S38.
Verdecchia P, Clement D, Fagard R, Palatini P, Parati G . Blood Pressure Monitoring. Task force III: Target-organ damage, morbidity and mortality. Blood Press Monit 1999; 4: 303–317.
Antic V, Van Vliet BN, Montani JP . Loss of nocturnal dipping of blood pressure and heart rate in obesity-induced hypertension in rabbits. Auton Neurosci 2001; 90: 152–157.
Pelat M, Verwaerde P, Merial C, Galitzky J, Berlan M, Montastruc JL et al. Impaired atrial M(2)-cholinoceptor function in obesity-related hypertension. Hypertension 1999; 34: 1066–1072.
Landsberg L, Saville ME, Young JB . Sympathoadrenal system and regulation of thermogenesis. Am J Physiol 1984; 247: E181–E189.
Ernsberger P, Koletsky RJ, Kilani A, Viswan G, Bedol D . Effects of weight cycling on urinary catecholamines: sympathoadrenal role in refeeding hypertension. J Hypertens 1998; 16: 2001–2005.
Antic V, Kiener-Belforti F, Tempini A, Van Vliet BN, Montani JP . Role of the sympathetic nervous system during the development of obesity-induced hypertension in rabbits. Am J Hypertens 2000; 13: 556–559.
Antic V, Dulloo A, Montani JP . Short-term (5-day) changes in food intake alter daily hemodynamics in rabbits. Am J Hypertens 2003; 16: 302–306.
Van Vliet BN, Montani JP . Baroreflex stabilization of the double product. Am J Physiol 1999; 277: H1679–H1689.
Frattola A, Parati G, Cuspidi C, Albini F, Mancia G . Prognostic value of 24-hour blood pressure variability. J Hypertens 1993; 11: 1133–1137.
Parati G, Pomidossi G, Albini F, Malaspina D, Mancia G . Relationship of 24-hour blood pressure mean and variability to severity of target-organ damage in hypertension. J Hypertens 1987; 5: 93–98.
Sega R, Corrao G, Bombelli M, Beltrame L, Facchetti R, Grassi G et al. Blood pressure variability and organ damage in a general population: results from the PAMELA study (Pressioni Arteriose Monitorate E Loro Associazioni). Hypertension 2002; 39: 710–714.
Pringle E, Phillips C, Thijs L, Davidson C, Staessen JA, De Leeuw PW et al. Systolic blood pressure variability as a risk factor for stroke and cardiovascular mortality in the elderly hypertensive population. J Hypertens 2003; 21: 2251–2257.
Gehrig Jr JJ, Jamison RL, Baylis C, Troy JL, Brenner BM, Jamison RL . Effect of intermittent feeding on renal hemodynamics in conscious rats. Am J Physiol 1986; 250: F566–F572.
Anderson S, Brenner BM . The role of intraglomerular pressure in the initiation and progression of renal disease. J Hypertens Suppl 1986; 4: S236–S238.
Anderson S, King AJ, Brenner BM . Hyperlipidemia and glomerular sclerosis: an alternative viewpoint. Am J Med 1989; 87: 34N–38N.
Acknowledgements
The authors' studies discussed in this review were supported by the Swiss National Science Foundation and the Swiss Heart Foundation.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Montani, JP., Viecelli, A., Prévot, A. et al. Weight cycling during growth and beyond as a risk factor for later cardiovascular diseases: the ‘repeated overshoot’ theory. Int J Obes 30 (Suppl 4), S58–S66 (2006). https://doi.org/10.1038/sj.ijo.0803520
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.ijo.0803520
Keywords
This article is cited by
-
Weight regain, but not weight loss exacerbates hepatic fibrosis during multiple weight cycling events in male mice
European Journal of Nutrition (2024)
-
Premature Death in Bodybuilders: What Do We Know?
Sports Medicine (2023)
-
Weight cycling in combat sports: revisiting 25 years of scientific evidence
BMC Sports Science, Medicine and Rehabilitation (2021)
-
Body mass index trajectories and the risk for Alzheimer’s disease among older adults
Scientific Reports (2021)
-
Weight trajectories and abdominal adiposity in COVID-19 survivors with overweight/obesity
International Journal of Obesity (2021)