Abstract
Objective:
To investigate whether low-carbohydrate diets are efficient for reduction of body weight and through which mechanism.
Design:
A couple of studies using low-carbohydrate diets in the treatment of obesity are reviewed. Mechanisms for explaining the reduced appetite are described in relation to knowledge on regulation of appetite for fat and carbohydrate.
Results:
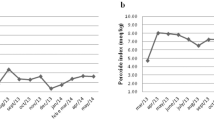
Studies with low-carbohydrate diets demonstrate a rapid weight loss, being more pronounced after 3 and 6 months compared to low-fat diets. After 12 months there is no difference between the low-carbohydrate and the conventional low-fat diet on weight loss. Both diets lead to improvements in risk factors for coronary heart disease, the low-carbohydrate diet leading to a greater decrease in serum triglycerides and increase in HDL cholesterol compared to the low-fat diet. Blood pressure, insulin sensitivity and LDL cholesterol were improved to a similar degree by the two diets. The mechanism for the rapid weight loss with the low-carbohydrate diet is a suppressed appetite, first through the high-protein content of the diet, second through the ketogenic nature of the diet with satiety signals for fat being active and third through the absence of hunger-promoting carbohydrate components like sucrose and/or fructose.
Conclusion:
A rapid initial weight loss occurs with a low-carbohydrate diet due to a suppressed appetite. There is as yet no indication of an increased metabolic rate and an increased thermogenesis by the low-carbohydrate diet. The safety and efficacy of low-carbohydrate diets have to await further studies.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Serdula MK, Mokdad AH, Williamson DF, Galuska DA, Mendlein JM, Heath GW . Prevalence of attempting weight loss and strategies for controlling weight. JAMA 1999; 282: 1353–1358.
Brehm BJ, Seeley RJ, Daniels SR, D’Alessio DA . A randomized trial comparing a very low carbohydrate diet and a calorie-restricted low fat diet on body weight and cardiovascular risk factors in healthy women. J Clin Endocrinol Metab 2003; 88: 1617–1623.
Westerterp-Plantenga MS, Rolland V, Wilson SA, Westerterp KR . Satiety related to 24 h diet-induced thermogenesis during high protein/carbohydrate vs high fat diets measured in a respiration chamber. Eur J Clin Nutr 1999; 53: 495–502.
Foster GD, Wyatt HR, Hill JO, McGuckin BG, Brill C, Mohammed BS, Szapary PO, Rader DJ, Edman JS, Klein S . A randomized trial of a low-carbohydrate diet for obesity. N Engl J Med 2003; 348: 2082–2090.
Brehm BJ, Spang SE, Lattin BL, Seeley RJ, Daniels SR, D’Alessio DA . The role of energy expenditure in the differential weight loss in obese women on low-fat and low-carbohydrate diets. J Clin Endocrinol Metab 2005; 90: 1475–1482.
Johnston CS, Tjonn SL, Swan PD . High-protein, low-fat diets are effective for weight loss and favorably alter biomarkers in healthy adults. J Nutr 2004; 134: 586–591.
Fischer K, Colombani PC, Wenk C . Metabolic and cognitive coefficients in the development of hunger sensations after pure macronutrient ingestion in the morning. Appetite 2004; 42: 49–61.
Melanson KJ, Westerterp-Plantenga MS, Saris WH, Smith FJ, Campfield LA . Blood glucose patterns and appetite in time-blinded humans: carbohydrate vs fat. Am J Physiol 1999; 277: R337–R345.
Koutsari C, Sidossis LS . Effect of isoenergetic low- and high-carbohydrate diets on substrate kinetics and oxidation in healthy men. Br J Nutr 2003; 90: 413–418.
Blundell JE, Cooling J, King NA . Differences in postprandial responses to fat and carbohydrate loads in habitual high and low fat consumers (phenotypes). Br J Nutr 2002; 88: 125–132.
Wenk C . Implications of dietary fat for nutrition and energy balance. Physiol Behav 2004; 83: 565–571.
Leonhardt M, Langhans W . Fatty acid oxidation and control of food intake. Physiol Behav 2004; 83: 645–651.
McLaughlin J, Grazia Luca M, Jones MN, D’Amato M, Dockray GJ, Thompson DG . Fatty acid chain length determines cholecystokinin secretion and effect on human gastric motility. Gastroenterology 1999; 116: 46–53.
Tso P, Liu M . Ingested fat and satiety. Physiol Behav 2004; 81: 275–287.
Berger K, Winzell MS, Mei J, Erlanson-Albertsson C . Enterostatin and its target mechanisms during regulation of fat intake. Physiol Behav 2004; 83: 623–630.
Lawton CL, Burley VJ, Wales JK, Blundell JE . Dietary fat and appetite control in obese subjects: weak effects on satiation and satiety. Int J Obes Relat Metab Disord 1993; 17: 409–416.
Raben A, Vasilaras TH, Moller AC, Astrup A . Sucrose compared with artificial sweeteners: different effects on ad libitum food intake and body weight after 10 wk of supplementation in overweight subjects. Am J Clin Nutr 2002; 76: 721–729.
Elliott SS, Keim NL, Stern JS, Teff K, Havel PJ . Fructose, weight gain, and the insulin resistance syndrome. Am J Clin Nutr 2002; 76: 911–922.
Lindqvist A, de la Cour CD, Stegmark A, Hakanson R, Erlanson-Albertsson C . Overeating of palatable food is associated with blunted leptin and ghrelin responses. Regul Pept 2005; 130: 123–132.
Erlanson-Albertsson C . How palatable food disrupts appetite regulation. Basic Clin Pharmacol Toxicol 2005; 97: 61–73.
Kong MF, Chapman I, Goble E, Wishart J, Wittert G, Morris H, Horowitz M . Effects of oral fructose and glucose on plasma GLP-1 and appetite in normal subjects. Peptides 1999; 20: 545–551.
Rayner CK, Park HS, Wishart JM, Kong M, Doran SM, Horowitz M . Effects of intraduodenal glucose and fructose on antropyloric motility and appetite in healthy humans. Am J Physiol Regul Integr Comp Physiol 2000; 278: R360–R366.
Teff KL, Elliott SS, Tschop M, Kieffer TJ, Rader D, Heiman M, Townsend RR, Keim NL, D’Alessio D, Havel PJ . Dietary fructose reduces circulating insulin and leptin, attenuates postprandial suppression of ghrelin, and increases triglycerides in women. J Clin Endocrinol Metab 2004; 89: 2963–2972.
Raben A . Should obese patients be counselled to follow a low-glycaemic index diet? No. Obes Rev 2002; 3: 245–256.
Pawlak DB, Ebbeling CB, Ludwig DS . Should obese patients be counselled to follow a low-glycaemic index diet? Yes. Obes Rev 2002; 3: 235–243.
Wurtman RJ, Wurtman JJ . Carbohydrates and depression. Sci Am 1989; 260: 68–75.
Rogers PJ, Smit HJ . Food craving and food ‘addiction’: a critical review of the evidence from a biopsychosocial perspective. Pharmacol Biochem Behav 2000; 66: 3–14.
Colantuoni C, Schwenker J, McCarthy J, Rada P, Ladenheim B, Cadet JL, Schwartz GJ, Moran TH, Hoebel BG . Excessive sugar intake alters binding to dopamine and mu-opioid receptors in the brain. Neuroreport 2001; 12: 3549–3552.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
This article is cited by
-
Ketosis and appetite-mediating nutrients and hormones after weight loss
European Journal of Clinical Nutrition (2013)
-
The biochemistry of ketogenesis and its role in weight management, neurological disease and oxidative stress
Journal of Physiology and Biochemistry (2012)
-
Lifestyle Intervention Leading to Moderate Weight Loss Normalizes Postprandial Triacylglycerolemia Despite Persisting Obesity
Obesity (2011)
-
Short-Term Carbohydrate-Restricted Diet for Weight Loss in Severely Obese Women
Obesity Surgery (2011)
-
Popular weight-loss diets: from evidence to practice
Nature Clinical Practice Cardiovascular Medicine (2007)