Abstract
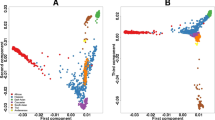
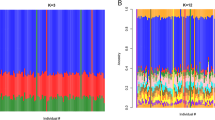
Africa is home to genetically diverse human populations. We compared the genetic structure of the Wolaita ethnic population from Southern Ethiopia (WETH, n=120) with HapMap populations using genome-wide variants. We investigated allele frequencies of 443 clinically and pharmacogenomically relevant genetic variants in WETH compared with HapMap populations. We found that WETH were genetically most similar to the Kenya Maasai and least similar to the Japanese in HapMap. Variant alleles associated with increased risk of adverse reactions to drugs used for treating tuberculosis (rs1799929 and rs1495741 in NAT2), thromboembolism (rs7294, rs9923231 and rs9934438 in VKORC1), and HIV/AIDS and solid tumors (rs2242046 in SLC28A1) had significantly higher frequencies in WETH compared with African ancestry HapMap populations. Our results illustrate that clinically relevant pharmacogenomic loci display allele frequency differences among African populations. We conclude that drug dosage guidelines for important global health diseases should be validated in genetically diverse African populations.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 6 print issues and online access
$259.00 per year
only $43.17 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Grossman I . ADME pharmacogenetics: current practices and future outlook. Expert Opin Drug Metab Toxicol 2009; 5: 449–462.
Ramos E, Doumatey A, Elkahloun AG, Shriner D, Huang H, Chen G et al. Pharmacogenomics, ancestry and clinical decision making for global populations. Pharmacogenomics J 2013; 14: 217–222.
Matimba A, Del-Favero J, Van Broeckhoven C, Masimirembwa C . Novel variants of major drug-metabolising enzyme genes in diverse African populations and their predicted functional effects. Hum Genomics 2009; 3: 169–190.
Campbell MC, Tishkoff SA . African genetic diversity: implications for human demographic history, modern human origins, and complex disease mapping. Annu Rev Genomics Hum Genet 2008; 9: 403–433.
Rotimi CN, Jorde LB . Ancestry and disease in the age of genomic medicine. N Engl J Med 2010; 363: 1551–1558.
Ngaimisi E, Habtewold A, Minzi O, Makonnen E, Mugusi S, Amogne W et al. Importance of ethnicity, CYP2B6 and ABCB1 genotype for efavirenz pharmacokinetics and treatment outcomes: a parallel-group prospective cohort study in two sub-Saharan Africa populations. PLoS One 2013; 8: e67946.
Ge D, Fellay J, Thompson AJ, Simon JS, Shianna KV, Urban TJ et al. Genetic variation in IL28B predicts hepatitis C treatment-induced viral clearance. Nature 2009; 461: 399–401.
Tekola Ayele F, Adeyemo A, Finan C, Hailu E, Sinnott P, Burlinson ND et al. HLA class II locus and susceptibility to podoconiosis. N Engl J Med 2012; 366: 1200–1208.
Altshuler DM, Gibbs RA, Peltonen L, Dermitzakis E, Schaffner SF, Yu F et al. Integrating common and rare genetic variation in diverse human populations. Nature 2010; 467: 52–58.
Rousset F . genepop'007: a complete re-implementation of the genepop software for Windows and Linux. Mol Ecol Resour 2008; 8: 103–106.
Weir BS, Cockerham CC . Estimating F-statistic for the analysis of population structure. Evolution 1984; 38: 1358–1370.
Pritchard JK, Stephens M, Donnelly P . Inference of population structure using multilocus genotype data. Genetics 2000; 155: 945–959.
Evanno G, Regnaut S, Goudet J . Detecting the number of clusters of individuals using the software STRUCTURE: a simulation study. Mol Ecol 2005; 14: 2611–2620.
Rosenberg NA . Distruct: a program for the graphical display of population structure. Mol Ecol Notes 2004; 4: 137–138.
Deeken J . The Affymetrix DMET platform and pharmacogenetics in drug development. Curr Opin Mol Ther 2009; 11: 260–268.
Tekola F, Bull SJ, Farsides B, Newport MJ, Adeyemo A, Rotimi CN et al. Tailoring consent to context: designing an appropriate consent process for a biomedical study in a low income setting. PLoS Negl Trop Dis 2009; 3: e482.
Tekola F, Bull S, Farsides B, Newport MJ, Adeyemo A, Rotimi CN et al. Impact of social stigma on the process of obtaining informed consent for genetic research on podoconiosis: a qualitative study. BMC Med Ethics 2009; 10: 13.
Toschi L, Finocchiaro G, Bartolini S, Gioia V, Cappuzzo F . Role of gemcitabine in cancer therapy. Future Oncol 2005; 1: 7–17.
Gray JH, Mangravite LM, Owen RP, Urban TJ, Chan W, Carlson EJ et al. Functional and genetic diversity in the concentrative nucleoside transporter, CNT1, in human populations. Mol Pharmacol 2004; 65: 512–519.
D'Andrea G, D'Ambrosio RL, Di Perna P, Chetta M, Santacroce R, Brancaccio V et al. A polymorphism in the VKORC1 gene is associated with an interindividual variability in the dose-anticoagulant effect of warfarin. Blood 2005; 105: 645–649.
Ben Mahmoud L, Ghozzi H, Kamoun A, Hakim A, Hachicha H, Hammami S et al. Polymorphism of the N-acetyltransferase 2 gene as a susceptibility risk factor for antituberculosis drug-induced hepatotoxicity in Tunisian patients with tuberculosis. Pathol Biol (Paris) 2012; 60: 324–330.
Garcia-Closas M, Hein DW, Silverman D, Malats N, Yeager M, Jacobs K et al. A single nucleotide polymorphism tags variation in the arylamine N-acetyltransferase 2 phenotype in populations of European background. Pharmacogenet Genomics 2011; 21: 231–236.
Pagani L, Kivisild T, Tarekegn A, Ekong R, Plaster C, Gallego Romero I et al. Ethiopian genetic diversity reveals linguistic stratification and complex influences on the Ethiopian gene pool. Am J Hum Genet 2012; 91: 83–96.
Bohonak AJ . IBD (Isolation by Distance): a program for analyses of isolation by distance. J Hered 2002; 93: 153–154.
CSA & ORC Macro. The 2007 Population and Housing Census of Ethiopia. CSA: Addis Ababa, 2007.
Fukunaga AK, Marsh S, Murry DJ, Hurley TD, McLeod HL . Identification and analysis of single-nucleotide polymorphisms in the gemcitabine pharmacologic pathway. Pharmacogenomics J 2004; 4: 307–314.
Soo RA, Wang LZ, Ng SS, Chong PY, Yong WP, Lee SC et al. Distribution of gemcitabine pathway genotypes in ethnic Asians and their association with outcome in non-small cell lung cancer patients. Lung Cancer 2009; 63: 121–127.
Takeuchi F, McGinnis R, Bourgeois S, Barnes C, Eriksson N, Soranzo N et al. A genome-wide association study confirms VKORC1, CYP2C9, and CYP4F2 as principal genetic determinants of warfarin dose. PLoS Genet 2009; 5: e1000433.
Yin T, Miyata T . Warfarin dose and the pharmacogenomics of CYP2C9 and VKORC1–rationale and perspectives. Thromb Res 2007; 120: 1–10.
Dandara C, Lombard Z, Du Plooy I, McLellan T, Norris SA, Ramsay M . Genetic variants in CYP (-1A2, -2C9, -2C19, -3A4 and -3A5), VKORC1 and ABCB1 genes in a black South African population: a window into diversity. Pharmacogenomics 2011; 12: 1663–1670.
Ross KA, Bigham AW, Edwards M, Gozdzik A, Suarez-Kurtz G, Parra EJ . Worldwide allele frequency distribution of four polymorphisms associated with warfarin dose requirements. J Hum Genet 2010; 55: 582–589.
Semino O, Santachiara-Benerecetti AS, Falaschi F, Cavalli-Sforza LL, Underhill PA . Ethiopians and Khoisan share the deepest clades of the human Y-chromosome phylogeny. Am J Hum Genet 2002; 70: 265–268.
Sominsky S, Korostishevsky M, Kurnik D, Aklillu E, Cohen Y, Ken-Dror G et al. The VKORC1 Asp36Tyr variant and VKORC1 haplotype diversity in Ashkenazi and Ethiopian populations. J Appl Genet 2014; 55: 163–171.
Aklillu E, Leong C, Loebstein R, Halkin H, Gak E . VKORC1 Asp36Tyr warfarin resistance marker is common in Ethiopian individuals. Blood 2008; 111: 3903–3904.
Loebstein R, Dvoskin I, Halkin H, Vecsler M, Lubetsky A, Rechavi G et al. A coding VKORC1 Asp36Tyr polymorphism predisposes to warfarin resistance. Blood 2007; 109: 2477–2480.
Tostmann A, Boeree MJ, Aarnoutse RE, de Lange WC, van der Ven AJ, Dekhuijzen R . Antituberculosis drug-induced hepatotoxicity: concise up-to-date review. J Gastroenterol Hepatol 2008; 23: 192–202.
Wang PY, Xie SY, Hao Q, Zhang C, Jiang BF . NAT2 polymorphisms and susceptibility to anti-tuberculosis drug-induced liver injury: a meta-analysis. Int J Tuberc Lung Dis 2012; 16: 589–595.
Ho HT, Wang TH, Hsiong CH, Perng WC, Wang NC, Huang TY et al. The NAT2 tag SNP rs1495741 correlates with the susceptibility of antituberculosis drug-induced hepatotoxicity. Pharmacogenet Genomics 2013; 23: 200–207.
Yew WW, Leung CC . Antituberculosis drugs and hepatotoxicity. Respirology 2006; 11: 699–707.
Yimer G, Aderaye G, Amogne W, Makonnen E, Aklillu E, Lindquist L et al. Anti-tuberculosis therapy-induced hepatotoxicity among Ethiopian HIV-positive and negative patients. PLoS One 2008; 3: e1809.
Hassen Ali A, Belachew T, Yami A, Ayen WY . Anti-tuberculosis drug induced hepatotoxicity among TB/HIV co-infected patients at Jimma University Hospital, Ethiopia: nested case-control study. PLoS One 2013; 8: e64622.
Yimer G, Ueda N, Habtewold A, Amogne W, Suda A, Riedel KD et al. Pharmacogenetic & pharmacokinetic biomarker for efavirenz based ARV and rifampicin based anti-TB drug induced liver injury in TB-HIV infected patients. PLoS One 2011; 6: e27810.
Mekonnen T, Abseno M, Meressa D, Fekde B . Prevalence and management outcomes of anti TB drugs induced hepatotocicity, St.Peter TB Specialized Hospital. J Ethiopia Med Pract 2002; 4: 32–38.
WHO. Global Tuberculosis Report 2012. WHO: Geneva, 2012.
Acknowledgements
The research project was supported by the Wellcome Trust (grant no.079791), and the Intramural Research Program of the National Human Genome Research Institute, National Institutes of Health, in the Center for Research on Genomics and Global Health (CRGGH). The CRGGH is also supported by the National Institute of Diabetes and Digestive and Kidney Diseases. We thank staff of the Mossy Foot Treatment and Prevention Association of Ethiopia for coordinating the fieldwork.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Supplementary Information accompanies the paper on the The Pharmacogenomics Journal website
Supplementary information
Rights and permissions
About this article
Cite this article
Tekola-Ayele, F., Adeyemo, A., Aseffa, A. et al. Clinical and pharmacogenomic implications of genetic variation in a Southern Ethiopian population. Pharmacogenomics J 15, 101–108 (2015). https://doi.org/10.1038/tpj.2014.39
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/tpj.2014.39
This article is cited by
-
Pharmacogenomic implications of the evolutionary history of infectious diseases in Africa
The Pharmacogenomics Journal (2017)
-
Novel genomic signals of recent selection in an Ethiopian population
European Journal of Human Genetics (2015)