Featured
-
-
Article |
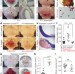 Endothelial TLR4 and the microbiome drive cerebral cavernous malformations
Endothelial TLR4 and the microbiome drive cerebral cavernous malformations
Lipopolysaccharide derived from gut bacteria can accelerate the formation of cerebral cavernous malformations by activating TLR4 on endothelial cells, and polymorphisms that increase expression of the genes encoding TLR4 or its co-receptor CD14 are associated with higher CCM lesion burden in humans.
- Alan T. Tang
- , Jaesung P. Choi
- & Mark L. Kahn
-
Letter |
 Cerebral cavernous malformations arise from endothelial gain of MEKK3–KLF2/4 signalling
Cerebral cavernous malformations arise from endothelial gain of MEKK3–KLF2/4 signalling
Gain of MEKK3 signalling is shown to cause cerebral cavernous malformations (CCMs) via activation of the target genes Klf2 and Klf4; endothelial-specific loss of MEKK3, KLF2 or KLF4 prevents lesion formation and lethality in a mouse CCM model.
- Zinan Zhou
- , Alan T. Tang
- & Mark L. Kahn
-
Outlook |
 Physiology: Beating stroke
Physiology: Beating stroke
New drugs and more focused therapy might cut down on atrial fibrillation and reduce the incidence of stroke.
- Neil Savage
-
Research Highlights |
 Nanoparticles home in to clear clots
Nanoparticles home in to clear clots
-
Letter |
 Apolipoprotein E controls cerebrovascular integrity via cyclophilin A
Apolipoprotein E controls cerebrovascular integrity via cyclophilin A
The APOE4-mediated proinflammatory pathway is shown to initiate blood–brain barrier breakdown and resulting neurodegeneration in transgenic mice.
- Robert D. Bell
- , Ethan A. Winkler
- & Berislav V. Zlokovic
-
Letter |
 Treatment of stroke with a PSD-95 inhibitor in the gyrencephalic primate brain
Treatment of stroke with a PSD-95 inhibitor in the gyrencephalic primate brain
Tat-NR2B9c, a PSD-95 inhibitor, is shown to reduce stroke-induced behavioural and neuroanatomical deficits in cynomolgous macaques when administered in the presence of an ischemic penumbra, suggesting the potential of PSD-95 inhibition as a neuroprotectant strategy for clinical investigation.
- Douglas J. Cook
- , Lucy Teves
- & Michael Tymianski
-
Research Highlights |
Cell source for brain disorder
-
Letter |
 Embolus extravasation is an alternative mechanism for cerebral microvascular recanalization
Embolus extravasation is an alternative mechanism for cerebral microvascular recanalization
Uninterrupted blood flow through the small vessels of the brain is essential for cerebral function and viability. Small clots that form in the vessels can be — but are not always — removed by haemodynamic forces and the fibrinolytic system. Here, a third mechanism for the removal of emboli is described: the endothelial cells that line the vessel walls send out membrane projections that envelop the emboli and move them into the perivascular parenchyma tissue. In aged mice, this process is markedly delayed.
- Carson K. Lam
- , Taehwan Yoo
- & Jaime Grutzendler
-

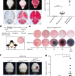 PIK3CA and CCM mutations fuel cavernomas through a cancer-like mechanism
PIK3CA and CCM mutations fuel cavernomas through a cancer-like mechanism