Abstract
Extract: The total body plethysmograph method of DuBois et al. [7] for measurement of lung volume and airway resistance was adapted to the study of newborn infants. A Rendell-Baker mask directly controlled by the operator proved by trial and error to minimize the chances of pressure leaks and undesirable pressure on the nose and allowed the mandible to be pulled forward to minimize pharyngeal obstruction. Use of an oscilloscope for direct visualization of flow and pressure tracings was essential in order to detect immediately pressure leaks, artifacts, and abnormal patterns during measurements of both lung volume and airway resistance.
Interpretation of the measurements of airway resistance and of the relation of conductance to lung volume over a wide range of age and lung volumes requires that the flow rates at which measurements are made be recorded, along with lung volumes.
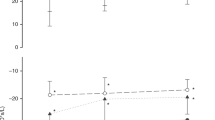
In 51 newborn infants, an airway resistance value of 19.2±5.6 cm H2O/l/s was observed. Thoracic gas volume at functional residual capacity was 89.9±15.5 ml. The resulting mean value for conductance (reciprocal of airway resistance), 0.052 l/s/cm H2O, fell above the calculated regressions of conductance versus lung volume determined by Briscoe and DuBois [3], who used data obtained from older children and adults. Direct comparison is limited since airway resistance in the older subjects was usually obtained using panting flow rates of 0.5 l/s, while the infants in this study had flow rates of approximately 0.1 l/s at the time airway resistance was measured.
Speculation: Confirmation of the presence of the major expiratory flow-limiting segment in the nasal airway of newborn and small infants is needed. This location suggests a physiologic means for slowing expiratory flow and thus maintaining expiratory intraluminal pressure in the tracheobronchial tree, which might protect the compliant trachea and major bronchi from compression by positive intrapleural pressure in obstructive pulmonary disease. It is possible that there is an airflow-lung volume-airway resistance relation throughout life; however, a wide range of control data will be required to establish such a relation.
Similar content being viewed by others
Article PDF
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Doershuk, C., Matthews, L. Airway Resistance and Lung Volume in the Newborn Infant. Pediatr Res 3, 128–134 (1969). https://doi.org/10.1203/00006450-196903000-00004
Issue Date:
DOI: https://doi.org/10.1203/00006450-196903000-00004
Keywords
This article is cited by
-
Assessment of lung ventilation of premature infants with bronchopulmonary dysplasia at 1.5 Tesla using phase-resolved functional lung magnetic resonance imaging
Pediatric Radiology (2023)
-
Studies of wall shear and mass transfer in a large scale model of neonatal high-frequency jet ventilation
Annals of Biomedical Engineering (1990)