Abstract
Nuclear hormone receptor liver X receptor-alpha (LXRα) has a vital role in cholesterol homeostasis and is reported to have a role in adipose function and obesity although this is controversial. Conversely, mesenchymal stem cells (MSCs) are suggested to be a major source of adipocyte generation. Accordingly, we examined the role of LXRα in adipogenesis of MSCs. Adult murine MSCs (mMSCs) were isolated from wild-type (WT) and LXR-null mice. Using WT mMSCs, we further generated cell lines stably overexpressing GFP-LXRα (mMSC/LXRα/GFP) or GFP alone (mMSC/GFP) by retroviral infection. Confluent mMSCs were differentiated into adipocytes by the established protocol. Compared with MSCs isolated from WT mice, MSCs from LXR-null mice showed significantly increased adipogenesis, as determined by lipid droplet accumulation and adipogenesis-related gene expression. Moreover, mMSCs stably overexpressing GFP-LXRα (mMSC/LXRα/GFP) exhibited significantly decreased adipogenesis compared with mMSCs overexpressing GFP alone (mMSC/GFP). Since Wnt/beta-catenin signaling is reported to inhibit adipogenesis, we further examined it. The LXR-null group showed significantly decreased Wnt expression accompanied by a decrease of cellular beta-catenin (vs WT). The mMSC/LXRα/GFP group exhibited significantly increased Wnt expression accompanied by an increase of cellular beta-catenin (vs mMSC/GFP). These data demonstrate that LXRα has an inhibitory effect on adipogenic differentiation in mMSCs with Wnt/beta-catenin signaling. These results provide important insights into the pathophysiology of obesity and obesity-related consequences such as metabolic syndrome and may identify potential therapeutic targets.
Similar content being viewed by others
Main
Liver X receptor-alpha (LXRα) is an oxysterol-regulated nuclear hormone receptor and has a vital role in cholesterol and lipid homeostasis.1, 2, 3, 4, 5, 6, 7, 8, 9 The expression of LXRα is restricted to tissues known to have important roles in lipid metabolism, such as the liver, adipose tissue, kidney, small intestine, skeletal muscle, and adrenal gland, whereas LXRβ is expressed ubiquitously.1, 3, 4, 10 The functions of LXRs in liver have been studied extensively. A recent study demonstrated that an LXR agonist attenuated endotoxin-induced liver injury in high-fat-diet-induced hepatic steatosis in mice.11 New evidence also points to an obesity-related effect of LXRs. Gao and Liu12 reported that an LXR agonist protected mice against the development of high-fat diet-induced obesity. In addition, recent studies imply a role for LXRα in adipose tissue because of the following evidence. First of all, the expression of LXRα is high in adipocytes.13 Second, the expression of LXRα is increased during adipogenesis.14, 15, 16 Finally, the expression levels of many LXRα target genes are also high in adipocytes.17 However, the role of LXRα in adipose tissue is not well defined. Interestingly, the role of LXRα in adipogenic differentiation is suggested by the studies using preadipocytes although those studies are limited and inconsistent.14, 15
Obesity is one of the most important risk factors of metabolic syndrome. Severe obesity is associated with both an increase in adipose cell size and increased adipose cell number.18, 19, 20 With respect to an increase in adipose cell number, mesenchymal stem cells (MSCs) are of note. Recent studies revealed that adult adipose tissue contains stem cells and they are much like bone marrow-derived MSCs.21, 22, 23 In addition, Liechty et al24 showed that human MSCs (hMSCs) transplanted into fetal sheep marrow differentiated and incorporated into normal adult adipose tissue. Moreover, Crossno et al25 reported that adipocyte progenitor cells originating from bone marrow contribute to an increase in adipocyte number. Taken together, MSCs are suggested to be a major source of adipocyte generation; however, the effect of LXRα on MSC differentiation to adipocyte is unknown.
Wnt/beta-catenin signaling is one of the most important regulators of MSC fate.26, 27 This signaling is also known to have a vital role in adipogenic differentiation of preadipocytes.28, 29 Activation of Wnt/beta-catenin signaling blocks adipogenesis,28, 29, 30 whereas inhibition of endogenous Wnt signaling promotes adipogenesis.29, 31 Thus Wnt/beta-catenin signaling is considered as a brake to adipogenic differentiation. Especially, Ross et al29 reported that Wnt 10b is the most important endogenous regulator of adipogenesis.
In this study, we test our hypothesis that LXRα has an important role in adipogenic differentiation of MSCs. Our data demonstrate that the deletion of LXR accelerates adipogenesis and the overexpression of LXRα inhibits adipogenic differentiation. Furthermore, this inhibitory effect of LXRα on adipogenesis is associated with Wnt/beta-catenin signaling, which has a vital role to inhibit adipogenesis.
MATERIALS AND METHODS
Murine MSC (mMSC) Isolation and Culture
All animal procedures were approved by the Duke University Institutional Animal Care and Use Committees. mMSCs were isolated by their adherence to plastic as previously described.32, 33, 34, 35, 36, 37, 38 Bone marrow was collected from 12-week-old male LXRα/LXRβ double knock out (LXRKO)39 and wild-type (WT) C57BL/6 mice by flushing femurs and tibias with the mMSC growth medium constituted of Minimum Essential Medium α (MEMα) with GlutaMAX (Invitrogen, Carlsbad, CA, USA), 20% fetal bovine serum (FBS), and penicillin/streptomycin (100 U/ml and 100 μg/ml, respectively). The bone marrow cells were then filtered through a 40-μm nylon mesh filter. Mononuclear cells were separated by gradient density using Ficoll-Paque Plus (Amersham Bioscience, Uppsala, Sweden). Cells were then washed twice with phosphate-buffered saline (PBS) and plated in plastic dishes. After 3 days, non-adherent cells were removed by two washes with PBS, and adherent cells were further cultured in the mMSC growth medium. Cells were then propagated in culture. Medium was changed every 3 days.
Confluent cells were incubated in adipogenic medium (Alpha-MEM–GlutaMax medium supplemented with 10 μg/ml insulin, 0.1 μmol/l dexamethasone, 50 μmol/l 3-isobutyl-1-methyl-xanthine (IBMX), 20 μmol/l indomethacin, 20% FBS, 100 U/ml penicillin, and 100 μg/ml streptomycin) for 9 days. Medium was changed every 3 days. Cells were harvested at day 9 after the initiation of differentiation.
To quantitate adipocyte differentiation, AdipoRed Assay Reagent (Cambrex, Walkersville, MD, USA) was employed following the manufacturer’s protocol. AdipoRed is a fluorescent dye that binds to lipid droplets. Total fluorescent signal was quantitated by fluorimeter.
Quantitative RT-PCR
Total RNA was isolated by the Tri Reagent (Sigma) and further purified using RNeasy columns (Qiagen, Valencia, CA, USA). The concentration of RNA was determined using spectrophotometry. First-strand cDNA was synthesized from total RNA using the High Capacity cDNA Archive Kit (Applied Biosystems, Foster City, CA, USA) following the manufacturer’s protocol. The Taqman probe primer system (Applied Biosystems) was used for quantitative RT-PCR. The primer and probe sets for murine peroxisome proliferator-activated receptor-gamma (PPAR-gamma), fatty acid synthase (FAS), Wnt1, Wnt3a, Wnt5a, Wnt10b, and the housekeeping gene glyceraldehyde-3-phosphate dehydrogenase (GAPDH) were purchased from Applied Biosystems. The primer and probe sets for human Wnt10b, LXRα, and GAPDH were also purchased from Applied Biosystems. TaqMan PCR was performed using ABI Prism 7700 Sequence Detection System as instructed by the manufacturer (Applied Biosystems). Target gene mRNA expression was normalized to GAPDH mRNA expression, and the relative amounts of all mRNAs were calculated using the comparative CT method.40
Cell Lines Stably Overexpressing GFP or GFP-LXRα
For the generation of mMSC lines stably expressing GFP or GFP-LXRα, LXRα cDNA was cloned into an MSCV-IRES-GFP plasmid backbone. Retroviral particles were then obtained by tripartite transfection in HEK 293T cells and concentrated by ultracentrifugation. WT C57BL/6 mMSCs were infected with retroviral particles in the presence of Polybrene (Sigma). Each infection was repeated twice. Pools of infected cells were then subcultured.
Immunoblotting
Cells were lysed at 4 °C with RIPA Lysis Buffer (Upstate, Lake Placid, NY, USA). Equal amounts of proteins (20 μg per lane) were separated by NuPAGE 4–12% Bis-Tris Gel (Invitrogen) electrophoresis. Protein fractions were then electrophoretically transferred onto a polyvinylidene difluoride membrane. The membrane was blocked with Blocker/Diluent solution (Western Blot Kit, Invitrogen). Then the membrane was incubated with rabbit polyclonal antibody to human beta-catenin (Cell Signaling Technology, Danvers, MA, USA) for 1 h at room temperature. After washing in wash buffer (Western Blot Kit, Invitrogen), the membrane was incubated with horseradish peroxidase-conjugated anti-rabbit immunoglobulin G (Western Blot Kit, Invitrogen) for 1 h at room temperature. The antigen antibody–peroxidase complex was visualized using the ECL chemiluminescence solution (Western Blot Kit, Invitrogen). The blot was subsequently stripped with Re-Blot Plus Western Blot Recycling Kit (Chemicon International, Temecula, CA, USA) and rehybridized with an anti-GAPDH antibody (Santa Cruz Biotechnology) as a control for protein loading. Densitometric quantitation was performed using the ImageJ software (NIH, Bethesda, MD, USA). Band intensity values of beta-catenin were standardized to those of GAPDH.
Analysis of Cellular Responses of hMSCs to LXR or Wnt Ligand
hMSCs were obtained from Cambrex. Cells were positive for CD105, CD166, CD29, and CD44 and negative for CD14, CD34, and CD45. hMSCs were grown in hMSC growth medium (Dulbecco’s modified Eagle’s medium supplemented with 10% fetal bovine serum, 4 mmol/l l-glutamine, 100 units/ml penicillin, and 100 μg/ml streptomycin). The growth medium was changed every 3 days. The natural LXR agonist 22-hydroxycholesterol (22OH-C) was purchased from Sigma. Recombinant human Wnt1 protein was purchased from Abcam (Cambridge, MA, USA). Cells were subjected to serum depletion for 16 h. Then cells were exposed to 22OH-C (0.01 μmol/l) or vehicle for 6 h, after which Wnt10b mRNA expression was determined using quantitative RT-PCR. For analysis of Wnt ligand, cells were serum depleted for 16 h, as above, before being exposed to human recombinant Wnt1 protein (final concentration 20 ng/ml) or vehicle for 6 h. Cells were then harvested and total RNA was analyzed by quantitative RT-PCR to determine the LXRα mRNA expression.
Statistical Analysis
All statistical procedures were carried out using the Statgraphics Plus version 5.0 software (StatPoint, Herndon, VA, USA). Comparisons between the two groups were made using Student's t test, and the differences were considered to be significant when P<0.05.
RESULTS
Deletion of LXR Promotes Adipocyte Differentiation of mMSCs
mMSCs were isolated from the bone marrow of WT and LXRKO mice. Cells were incubated in adipogenic medium (Alpha-MEM–GlutaMax medium supplemented with 10 μg/ml insulin, 0.1 μmol/l dexamethasone, 50 μmol/l 3-isobutyl-1-methyl-xanthine (IBMX), 20 μmol/l indomethacin, 20% FBS, 100 U/ml penicillin, and 100 μg/ml streptomycin) for 9 days. As shown in Figure 1a, differentiated adipocytes exhibited lipid droplets in cytoplasm. AdipoRed fluorescent dye (Cambrex) was employed to stain lipid droplets (Figure 1b). Adipogenesis was quantitated by measuring fluorescence using AdipoRed fluorescent dye. As shown in Figures 1c–e, lipid droplet accumulation was significantly greater in differentiated adipocytes from LXRKO mMSCs than those from the WT group (147.1±24.9%; n=12; P<0.05), suggesting an antiadipogenic effect of LXR on mMSCs.
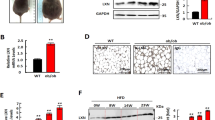
Deletion of LXR promotes adipocyte differentiation of murine MSCs. (a and b) Representative micrographs of differentiated adipocytes (day 9) from wild-type murine MSCs (a: phase contrast, b: AdipoRed fluorescence. Original magnification, × 400). (c and d) Representative AdipoRed fluorescent micrographs of differentiated adipocytes (day 9) from WT (c) and LXRKO (d). Original magnification, × 200. (e) Quantification of fluorescent lipid droplet accumulation. Relative percentage vs WT group. Data are mean±s.d. (n=12). *P<0.05 vs WT group.
Deletion of LXR Increases the Expression of Adipocyte-Related Genes
We also examined the expression of adipocyte-related genes by quantitative RT-PCR. mMSCs from WT and LXRKO mice were incubated in adipogenic medium for 9 days. Total RNA was analyzed by real-time RT-PCR for mRNA expression of PPAR-gamma and FAS on day 9. Consistent with the results regarding lipid droplet accumulation, PPAR-gamma and FAS expression was greater in the LXRKO compared with that in the WT group (2.33±0.45- and 1.60±0.24-fold increases, respectively; n=4; P<0.05; Figures 2a and b).
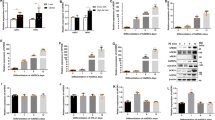
Expression of adipocyte-related genes. (a and b) Murine MSCs from wild-type (WT) and LXR-null (LXRKO) mice were incubated in adipogenic medium for 9 days. Total RNA was analyzed by quantitative RT-PCR for mRNA expression of PPAR-gamma (a) and fatty acid synthase (b) on day 9. Fold changes vs WT group. Data are mean±s.e.m. (n=4). *P<0.05 vs WT group. (c and d) Murine MSCs overexpressing GFP alone (mMSC/GFP) and mMSCs overexpressing GFP and LXRα (mMSC/LXRα/GFP) were incubated in adipogenic medium for 9 days. Total RNA was analyzed by quantitative RT-PCR for mRNA expression of PPAR-gamma (c) and fatty acid synthase (d) on day 9. Fold changes vs mMSC/GFP group. Data are mean±s.e.m. (n=4). *P<0.05 vs mMSC/GFP group.
Overexpression of LXRα Inhibits Adipocyte Differentiation of mMSCs
We next generated mMSC cell lines stably expressing GFP-LXRα (mMSC/LXRα/GFP) by retroviral infection. Cell lines expressing GFP alone (mMSC/GFP) were also generated as control. Cells were incubated in adipogenic medium for 9 days.
Adipogenesis was quantitated by assessing lipid droplet accumulation using AdipoRed fluorescent dye. As shown in Figures 3a–c, lipid droplet accumulation was significantly lower in differentiated adipocytes from the mMSC/LXRα/GFP group compared with that from the control mMSC/GFP group (59.2±8.2%; n=12; P<0.05), suggesting an antiadipogenic effect of LXRα on mMSCs.
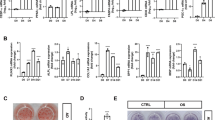
Overexpression of LXRα inhibits adipocyte differentiation of murine MSCs. (a and b) Reperesentative AdipoRed fluorescent micrographs of differentiated adipocytes (day 9) from mMSCs overexpressing GFP alone (a: mMSC/GFP) and mMSCs overexpressing GFP and LXRα (b: mMSC/LXRα/GFP). Original magnification, × 200. (c) Quantification of fluorescent lipid droplet accumulation. Relative percentage vs mMSC/GFP group. Data are mean±s.d. (n=12). *P<0.05 vs mMSC/GFP group.
Overexpression of LXRα Decreases the Expression of Adipocyte-Related Genes
mMSCs overexpressing GFP alone (mMSC/GFP) and mMSCs overexpressing GFP-LXRα (mMSC/LXRα/GFP) were incubated in adipogenic medium for 9 days. Total RNA was analyzed by quantitative RT-PCR for mRNA expression of PPAR-gamma and FAS on day 9. Consistent with the results regarding lipid droplet accumulation, PPAR-gamma and FAS expression was decreased in the mMSC/LXRα/GFP group compared with that in the control mMSC/GFP group (0.75±0.04- and 0.36±0.02-fold changes vs the mMSC/GFP group, respectively; n=4; P<0.05; Figures 2c and d).
Deletion of LXR Decreases Wnt Expression
As Wnt/beta-catenin signaling, especially Wnt 10b, is reported to inhibit adipogenesis, we examined the expression of Wnt genes by quantitative RT-PCR. mMSCs from WT and LXRKO mice were incubated in adipogenic medium for 9 days. Total RNA was analyzed by real-time RT-PCR for mRNA expression of Wnt1, Wnt3a, Wnt5a, and Wnt10b on day 9. As shown in Figures 4a–c, the LXRKO group showed a decreased expression of Wnt1, Wnt5a, and Wnt10b compared with that in the WT group (0.63±0.14-, 0.54±0.04-, and 0.25±0.03-fold changes vs the WT group, respectively; n=4; P<0.05). Especially, Wnt10b expression was remarkably decreased in the LXRKO group (Figure 4c). Wnt 3a was not expressed in any samples (data not shown).
Deletion of LXR decreases Wnt expression and cellular beta-catenin. Murine MSCs from wild-type (WT) and LXR-null (LXRKO) mice were incubated in adipogenic medium for 9 days. (a–c) Total RNA was analyzed by quantitative RT-PCR for mRNA expression of Wnt1 (a), Wnt5a (b), and Wnt10b (c) on day 9. Fold changes vs WT group. Data are mean±s.e.m. (n=4). *P<0.05 vs WT group. (d and e) Cell lysates were isolated and subjected to immunoblotting analysis using antibodies for beta-catenin and GAPDH. (d) A representative immunoblot from three independent experiments. Densitometric quantitation from three independent experiments is shown in the bar graph (e). Data are mean±s.e.m.; *P<0.05 vs WT group.
Deletion of LXR Decreases Cellular Beta-Catenin
To confirm the suppression of Wnt/beta-catenin signaling in the LXRKO group, we further examined cellular beta-catenin protein expression by immunoblotting. mMSCs from WT and LXRKO mice were incubated in the adipogenic medium for 9 days. Cell lysates were isolated and subjected to immunoblotting analysis using antibodies for beta-catenin and GAPDH. As shown in Figure 4d, cellular beta-catenin protein expression was decreased in the LXRKO group compared with that in the WT group. Densitometric quantification from three independent experiments revealed that cellular beta-catenin protein expression was significantly suppressed in the LXRKO compared with that in the WT group (Figure 4e), suggesting that the inhibitory effect of LXR on the adipogenesis of mMSCs is associated with Wnt/beta-catenin signaling.
Overexpression of LXRα Increases Wnt Expression
We also examined the expression of Wnt genes in the mMSC/LXRα/GFP and mMSC/GFP groups by quantitative RT-PCR. mMSC/GFP and mMSC/LXRα/GFP were incubated in adipogenic medium for 9 days. Total RNA was analyzed by real-time RT-PCR for mRNA expression of Wnt1, Wnt3a, Wnt5a, and Wnt10b on day 9. As shown in Figures 5a–c, the mMSC/LXRα/GFP group showed an increased expression of Wnt1, Wnt5a, and Wnt10b compared with that in the control mMSC/GFP group (3.45±1.05-, 1.75±0.14-, and 7.35±0.90-fold increases, respectively; n=4; P<0.05). Especially, Wnt10b expression was remarkably increased in the mMSC/LXRα/GFP group (Figure 5c). Wnt3a was not expressed in any samples (data not shown).
Overexpression of LXRα increases Wnt expression and cellular beta-catenin. Murine MSCs overexpressing GFP alone (mMSC/GFP) and mMSCs overexpressing GFP and LXRα (mMSC/LXRα/GFP) were incubated in adipogenic medium for 9 days. (a–c) Total RNA was analyzed by quantitative RT-PCR for mRNA expression of Wnt1 (a), Wnt5a (b), and Wnt10b (c) on day 9. Fold changes vs WT group. Data are mean±s.e.m. (n=4). *P<0.05 vs mMSC/GFP group. (d and e) Cell lysates were isolated and subjected to immunoblotting analysis using antibodies for beta-catenin and GAPDH. (d) A representative immunoblot from three independent experiments. Densitometric quantitation from three independent experiments is shown in the bar graph (e). Data are mean±s.e.m.; *P<0.05 vs mMSC/GFP group.
Overexpression of LXRα Increases Cellular Beta-Catenin
To confirm the activation of Wnt/beta-catenin signaling in the mMSC/LXRα/GFP group, we examined cellular beta-catenin protein expression by immunoblotting. mMSC/GFP and mMSC/LXRα/GFP were incubated in the adipogenic medium for 9 days. Cell lysates were isolated and subjected to immunoblotting analysis using antibodies for beta-catenin and GAPDH. As shown in Figure 5d, cellular beta-catenin protein expression was increased in the mMSC/LXRα/GFP group compared with that in the control mMSC/GFP group. Densitometric quantification from three independent experiments revealed that cellular beta-catenin protein expression was increased significantly in the mMSC/LXRα/GFP compared with that in the control mMSC/GFP group (Figure 5e). These results suggest that LXRα inhibits the adipogenesis of mMSCs in association with Wnt/beta-catenin signaling.
LXR Agonist 22-Hydroxycholesterol Upregulates Wnt10b Expression in hMSCs
Because an association between LXRα and Wnt/beta-catenin signaling was suggested in murine genetic models, we further examined cellular responses to LXR or Wnt ligand in hMSCs. After 16 h of serum depletion, hMSCs were exposed to 0.01 μmol/l 22OH-C for 6 h, and Wnt10b mRNA expression was evaluated using quantitative RT-PCR. As shown in Figure 6a, Wnt10b expression increased significantly in 22OH-C-treated hMSCs compared with that in vehicle-treated hMSCs (1.6±0.2-fold increase; n=3; P<0.05). Next, the effects of human recombinant Wnt1 protein (final concentration 20 ng/ml) on LXRα expression in hMSCs were evaluated. After 16 h of serum depletion and 6 h of exposure to 20 ng/ml human recombinant Wnt1 protein, there was no significant change in LXRα expression in hMSCs compared with vehicle treatment (Figure 6b; 1.0±0.1-fold change vs vehicle treatment; n=3).
Cellular responses to LXR or Wnt ligand in human MSCs. After human MSCs had been serum starved for 16 h, LXR ligand 22OH-C (final concentration 0.01 μmol/l) or human recombinant Wnt1 protein (final concentration 20 ng/ml) was added to the medium, and cells were cultured for a further 6 h before being harvested. Total RNA was analyzed by quantitative RT-PCR to determine Wnt10b (a) or LXRα (b) mRNA expression. Data show fold changes vs the vehicle-treated group (Vehicle). Data are mean±s.e.m. (n=3). *P<0.05 vs vehicle-treated group. NS, statistically non-significant.
DISCUSSION
In this study, we have shown that the deletion of LXR accelerates adipogenesis and the overexpression of LXRα inhibits adipogenesis of mMSCs, demonstrating that LXRα has an inhibitory effect of adipogenesis of mMSCs. Furthermore, we have demonstrated that the inhibitory effect of LXRα on adipogenesis is associated with Wnt/beta-catenin signaling, which has a vital role to inhibit adipocyte differentiation. Our data would suggest that the high level of expression of LXRα in adipose tissue13 and the increase in LXRα mRNA levels during adipogenesis14, 15, 16 contribute to the modulation of adipogenesis and obesity.
Increased adiposity predisposes individuals to both type 2 diabetes and metabolic syndrome. Severe obesity is associated with both an increase in adipose cell size and increased adipose cell number.18, 19, 20 Recent studies demonstrate that adipose tissue contains stem cells, much like bone marrow stromal MSCs.21, 22, 23 New fat cells arise from a preexisting pool of adipose stem cells irrespective of age.23, 41 In addition, Crossno et al25 reported that adipocyte progenitor cells originating from bone marrow contribute to development of new adipocytes in adult animals. Taken together, MSCs are suggested to have an important role in the maintenance of mass and function of adult adipose tissue. Accordingly, in vitro differentiation of MSCs toward the adipogenic lineage provides a useful means for studying in tissue culture the regulation of adipogenesis.42, 43
Nuclear hormone receptor LXRα has a vital role to control lipid and cholesterol homeostasis.1, 2, 3, 4, 5, 6, 7, 8, 9 The roles of LXRα in the liver and in macrophages have been studied extensively. In a recent study, an LXR agonist attenuated endotoxin-induced liver injury in high-fat-diet-induced hepatic steatosis in mice.11 In addition, Gao and Liu12 reported that an LXR agonist protected mice against the development of high-fat-diet-induced obesity. With regard to the relationship between adipocytes and cholesterol, adipocytes contain the largest pool of free cholesterol in the body,44 and recent studies have demonstrated high levels of LXRα expression in adipocytes,13 increased LXRα mRNA levels during adipogenesis14, 15, 16 and high levels of expression of many LXRα target genes in adipocytes.17 However, the role of LXRα in adipose tissue is not well defined. Despite the fact that the expression of LXRα increases during adipogenesis, the role of LXRα in adipose differentiation has remained conflicting. The studies using preadipocytes reported the function of LXRα as both positive and negative regulator of adipocyte differentiation.14, 15 Ross et al15 have reported that LXR activity inhibits adipocyte differentiation and lipid accumulation in cultured preadipocytes. They showed that ectopic expression of a constitutively active VP16-LXR-alpha fusion protein inhibited the differentiation of preadipocytes 3T3-L1 cells. In contrast to Ross et al,15 Juvet et al14 reported that LXR agonist treatment of differentiating adipocytes led to increased lipid accumulation. Our observation that LXRα has inhibitory effects on adipogenesis is consistent with the former report. These inconsistent data may reflect differences in cell types, cell line variations, and culture conditions. In this study, we used MSCs instead of preadipocytes. Developmentally, MSCs are at the step between the undifferentiated multipotent embryonic stem cells and the preadipocytes.45, 46, 47, 48 Our data could suggest the effect of LXRα on the first step of adipogenesis.
Importantly, Beaven et al49 recently reported that LXRKO mice, when bred onto the OB background (ob/ob LXRαβ−/− mice), exhibited increased total body adiposity compared with OB mice. Conversely, LXRKO mice are likely to be protected against diet-induced obesity through increased energy expenditure.50 However, adipose tissue-specific LXR-null mice have not yet been generated. Therefore, it is difficult to identify the precise roles of LXR in adipose tissue. Future studies are needed to elucidate the involvement of LXR in adipocyte differentiation and adipose biology.
We also studied the mechanism of the inhibitory effect of LXRα on adipogenesis of MSCs. Wnt/beta-catenin signaling is reported to be an important regulator of MSC fate.26, 27 This signaling is also known to have a vital role in adipogenic differentiation of preadipocytes.28, 29 Activation of Wnt/beta-catenin signaling blocks adipogenesis.28, 29, 30 On the other hand, inhibition of endogenous Wnt signaling is reported to promote adipogenesis.29, 31 Therefore, Wnts are considered as a brake to adipogenic differentiation. In particular, Ross et al29 reported that Wnt10b is the most important endogenous regulator of adipogenesis. Longo et al30 created transgenic mice in which Wnt10b is expressed from the FABP4 promoter (FABP4-Wnt10b mice) and found that these mice had reduced adiposity and were resistant to diet-induced obesity. In addition, Wright et al51 reported that expression of Wnt10b in adipose tissue reduces adiposity in the ob/ob obesity model. Those authors also reported that Wnt10b protected against genetic obesity in mice owing to ectopic expression of agouti (Ay).51 In this study, the deletion of LXR decreases Wnt1, Wnt5a, and Wnt10b expression. Especially, Wnt10b expression is remarkably decreased. Moreover, the deletion of LXR decreases cellular beta-catenin protein expression, confirming that Wnt/beta-catenin signaling is suppressed. Consistent with the data of LXR deletion, overexpression of LXRα increases the mRNA expression of Wnts, especially Wnt10b. Overexpression of LXRα also increases cellular beta-catenin protein expression. The results of the present study suggest that the mechanism underlying the inhibitory effect of LXRα on the adipogenesis of MSCs is associated with Wnt/beta-catenin signaling. Furthermore, the data suggest that the action may be LXR ligand dependent. However, the precise mechanisms underlying the association between LXRα and Wnt/beta-catenin signaling remain unclear. Whether LXRα acts as a heterodimer or not and the role of LXRβ are unknown. In addition, there are a number of molecules that regulate adipogenesis, even though Wnt/beta-catenin signaling has been suggested as one of the most important pathways. Therefore, further experiments are needed to elucidate the mechanism(s) underlying the antiadipogenic effect of LXRα more clearly.
In conclusion, the present study demonstrates that LXRα inhibits adipocyte differentiation of mMSCs with Wnt/beta-catenin signaling. Such a role of LXRα might be physiologically important in the maintenance of the mass and function of adult adipose tissue. Our results support a role for LXRα in adipose tissue, and further characterization of the role of LXRα in adipocyte biology is important for future research on obesity, with possible therapeutic implications for treatment of obesity and obesity-related consequences, such as metabolic syndrome.
References
Jakobsson T, Treuter E, Gustafsson JA et al. Liver X receptor biology and pharmacology: new pathways, challenges and opportunities. Trends Pharmacol Sci 2012;33:394–404.
Janowski BA, Willy PJ, Devi TR et al. An oxysterol signalling pathway mediated by the nuclear receptor LXR alpha. Nature 1996;383:728–731.
Kidani Y, Bensinger SJ . Liver X receptor and peroxisome proliferator-activated receptor as integrators of lipid homeostasis and immunity. Immunol Rev 2012;249:72–83.
Parikh M, Patel K, Soni S et al. Liver X receptor: a cardinal target for atherosclerosis and beyond. J Atheroscler Thromb 2014;21:519–531.
Peet DJ, Turley SD, Ma W et al. Cholesterol and bile acid metabolism are impaired in mice lacking the nuclear oxysterol receptor LXR alpha. Cell 1998;93:693–704.
Steffensen KR, Gustafsson JA . Putative metabolic effects of the liver X receptor (LXR). Diabetes 2004;53:S36–S42.
Tobin KA, Steineger HH, Alberti S et al. Cross-talk between fatty acid and cholesterol metabolism mediated by liver X receptor-alpha. Mol Endocrinol 2000;14:741–752.
Venkateswaran A, Laffitte BA, Joseph SB et al. Control of cellular cholesterol efflux by the nuclear oxysterol receptor LXR alpha. Proc Natl Acad Sci USA 2000;97:12097–12102.
Zelcer N, Tontonoz P . Liver X receptors as integrators of metabolic and inflammatory signaling. J Clin Invest 2006;116:607–614.
Annicotte JS, Schoonjans K, Auwerx J . Expression of the liver X receptor alpha and beta in embryonic and adult mice. Anat Rec A Discov Mol Cell Evol Biol 2004;277:312–316.
Liu Y, Han X, Bian Z et al. Activation of liver X receptors attenuates endotoxin-induced liver injury in mice with nonalcoholic fatty liver disease. Dig Dis Sci 2012;57:390–398.
Gao M, Liu D . The liver X receptor agonist T0901317 protects mice from high fat diet-induced obesity and insulin resistance. AAPS J 2013;15:258–266.
Willy PJ, Umesono K, Ong ES et al. LXR, a nuclear receptor that defines a distinct retinoid response pathway. Genes Dev 1995;9:1033–1045.
Juvet LK, Andresen SM, Schuster GU et al. On the role of liver X receptors in lipid accumulation in adipocytes. Mol Endocrinol 2003;17:172–182.
Ross SE, Erickson RL, Gerin I et al. Microarray analyses during adipogenesis: understanding the effects of Wnt signaling on adipogenesis and the roles of liver X receptor alpha in adipocyte metabolism. Mol Cell Biol 2002;22:5989–5999.
Steffensen KR, Schuster GU, Parini P et al. Different regulation of the LXRalpha promoter activity by isoforms of CCAAT/enhancer-binding proteins. Biochem Biophys Res Commun 2002;293:1333–1340.
Soukas A, Socci ND, Saatkamp BD et al. Distinct transcriptional profiles of adipogenesis in vivo and in vitro. J Biol Chem 2001;276:34167–34174.
Brook CG, Lloyd JK, Wolf OH . Relation between age of onset of obesity and size and number of adipose cells. Br Med J 1972;2:25–27.
Faust IM, Johnson PR, Stern JS et al. Diet-induced adipocyte number increase in adult rats: a new model of obesity. Am J Physiol 1978;235:E279–E286.
Hirsch J, Batchelor B . Adipose tissue cellularity in human obesity. Clin Endocrinol Metab 1976;5:299–311.
De Ugarte DA, Morizono K, Elbarbary A et al. Comparison of multi-lineage cells from human adipose tissue and bone marrow. Cells Tissues Organs 2003;174:101–109.
Lee RH, Kim B, Choi I et al. Characterization and expression analysis of mesenchymal stem cells from human bone marrow and adipose tissue. Cell Physiol Biochem 2004;14:311–324.
Zuk PA, Zhu M, Mizuno H et al. Multilineage cells from human adipose tissue: implications for cell-based therapies. Tissue Eng 2001;7:211–228.
Liechty KW, MacKenzie TC, Shaaban AF et al. Human mesenchymal stem cells engraft and demonstrate site-specific differentiation after in utero transplantation in sheep. Nat Med 2000;6:1282–1286.
Crossno JT Jr, Majka SM, Grazia T et al. Rosiglitazone promotes development of a novel adipocyte population from bone marrow-derived circulating progenitor cells. J Clin Invest 2006;116:3220–3228.
Davis LA, Zur Nieden NI . Mesodermal fate decisions of a stem cell: the Wnt switch. Cell Mol Life Sci 2008;65:2658–2674.
Satija NK, Gurudutta GU, Sharma S et al. Mesenchymal stem cells: molecular targets for tissue engineering. Stem Cells Dev 2007;16:7–23.
Bennett CN, Ross SE, Longo KA et al. Regulation of Wnt signaling during adipogenesis. J Biol Chem 2002;277:30998–31004.
Ross SE, Hemati N, Longo KA et al. Inhibition of adipogenesis by Wnt signaling. Science 2000;289:950–953.
Longo KA, Wright WS, Kang S et al. Wnt10b inhibits development of white and brown adipose tissues. J Biol Chem 2004;279:35503–35509.
Christodoulides C, Laudes M, Cawthorn WP et al. The Wnt antagonist Dickkopf-1 and its receptors are coordinately regulated during early human adipogenesis. J Cell Sci 2006;119 (Pt 12):2613–2620.
Bruder SP, Jaiswal N, Haynesworth SE . Growth kinetics, self-renewal, and the osteogenic potential of purified human mesenchymal stem cells during extensive subcultivation and following cryopreservation. J Cell Biochem 1997;64:278–294.
Colter DC, Class R, DiGirolamo CM et al. Rapid expansion of recycling stem cells in cultures of plastic-adherent cells from human bone marrow. Proc Natl Acad Sci USA 2000;97:3213–3218.
Ip JE, Wu Y, Huang J et al. Mesenchymal stem cells use integrin beta1 not CXC chemokine receptor 4 for myocardial migration and engraftment. Mol Biol Cell 2007;18:2873–2882.
Mangi AA, Noiseux N, Kong D et al. Mesenchymal stem cells modified with Akt prevent remodeling and restore performance of infarcted hearts. Nat Med 2003;9:1195–1201.
Mirotsou M, Zhang Z, Deb A et al. Secreted frizzled related protein 2 (Sfrp2) is the key Akt-mesenchymal stem cell-released paracrine factor mediating myocardial survival and repair. Proc Natl Acad Sci USA 2007;104:1643–1648.
Pereira RF, Halford KW, O'Hara MD et al. Cultured adherent cells from marrow can serve as long-lasting precursor cells for bone, cartilage, and lung in irradiated mice. Proc Natl Acad Sci USA 1995;92:4857–4861.
Prockop DJ . Marrow stromal cells as stem cells for nonhematopoietic tissues. Science 1997;276:71–74.
Schuster GU, Parini P, Wang L et al. Accumulation of foam cells in liver X receptor-deficient mice. Circulation 2002;106:1147–1153.
Livak KJ, Schmittgen TD . Analysis of relative gene expression data using real-time quantitative PCR and the 2(-Delta Delta C(T)) Method. Methods 2001;25:402–408.
Phillips BW, Vernochet C, Dani C . Differentiation of embryonic stem cells for pharmacological studies on adipose cells. Pharmacol Res 2003;47:263–268.
Matsushita K, Wu Y, Okamoto Y et al. Local renin angiotensin expression regulates human mesenchymal stem cell differentiation to adipocytes. Hypertension 2006;48:1095–1102.
Mogi M, Iwai M, Horiuchi M . Emerging concept of adipogenesis regulation by the renin-angiotensin system. Hypertension 2006;48:1020–1022.
Krause BR, Hartman AD . Adipose tissue and cholesterol metabolism. J Lipid Res 1984;25:97–110.
Billon N, Monteiro MC, Dani C . Developmental origin of adipocytes: new insights into a pending question. Biol Cell 2008;100:563–575.
Bost F, Aouadi M, Caron L et al. The role of MAPKs in adipocyte differentiation and obesity. Biochimie 2005;87:51–56.
Hausman DB, DiGirolamo M, Bartness TJ et al. The biology of white adipocyte proliferation. Obes Rev 2001;2:239–254.
Scavo LM, Karas M, Murray M et al. Insulin-like growth factor-I stimulates both cell growth and lipogenesis during differentiation of human mesenchymal stem cells into adipocytes. J Clin Endocrinol Metab 2004;89:3543–3553.
Beaven SW, Matveyenko A, Wroblewski K et al. Reciprocal regulation of hepatic and adipose lipogenesis by liver X receptors in obesity and insulin resistance. Cell Metab 2013;18:106–117.
Kalaany NY, Gauthier KC, Zavacki AM et al. LXRs regulate the balance between fat storage and oxidation. Cell Metab 2005;1:231–244.
Wright WS, Longo KA, Dolinsky VW et al. Wnt10b inhibits obesity in ob/ob and agouti mice. Diabetes 2007;56:295–303.
Acknowledgements
We thank Hui Mu for her technical assistance. This work was supported, in whole or in part, by grants from the National Heart, Lung, and Blood Institute (RO1 HL35610, HL58516, HL72010, and HL73219 to Victor J Dzau), the Edna Mandel Foundation (to Victor J Dzau), the Leducq Foundation (to Victor J Dzau), the Ministry of Education, Culture, Sports, Science, and Technology of Japan (KAKENHI 21790745 to Kenichi Matsushita), the Japan Society for the Promotion of Science (KAKENHI 26461086 to Kenichi Matsushita), the Uehara Memorial Foundation (to Kenichi Matsushita), the Inoue Foundation for Science (to Kenichi Matsushita), and the Swedish Science Council (to Jan-Åke Gustafsson).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
This study demonstrates that the nuclear hormone receptor LXRα has an inhibitory effect on adipogenic differentiation in murine mesenchymal stem cells with active Wnt/beta-catenin signaling. These data provide important insights into the pathophysiology of obesity and obesity related consequences such as metabolic syndrome and may identify potential therapeutic targets.
Rights and permissions
About this article
Cite this article
Matsushita, K., Morello, F., Zhang, Z. et al. Nuclear hormone receptor LXRα inhibits adipocyte differentiation of mesenchymal stem cells with Wnt/beta-catenin signaling. Lab Invest 96, 230–238 (2016). https://doi.org/10.1038/labinvest.2015.141
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/labinvest.2015.141
This article is cited by
-
Signaling pathways in obesity: mechanisms and therapeutic interventions
Signal Transduction and Targeted Therapy (2022)
-
Mesenchymal stem cells in obesity: insights for translational applications
Laboratory Investigation (2017)