Abstract
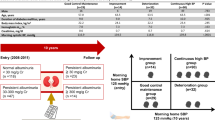
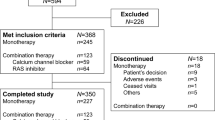
We investigated the effects of aggressive antihypertensive therapy based on hydrochlorothiazide, candesartan or lisinopril on urinary albumin excretion, endothelial function and inflammatory activity in hypertensive type II diabetic individuals. A total of 70 hypertensive type II diabetic individuals were treated with three antihypertensive strategies in a randomized, double-blind, double-dummy design. Blood pressure was titrated to levels below 130/85 mmHg or a decrease in systolic pressure of 10% with a diastolic pressure below 85 mmHg. After titration, patients were treated for 12 months. Mean blood pressures changed from 157/93, 151/94 and 149/93 at baseline to 135/80, 135/82 and 131/80 mmHg after titration in the hydrochlorothiazide (n=24), candesartan (n=24) and lisinopril (n=22) groups. About 70% reached target blood pressures. However, only 45% had blood pressures <130/85 mmHg. Urinary albumin excretion and levels of soluble vascular cell adhesion molecule-1 and intercellular adhesion molecule-1 decreased (GEE regression coefficients, −2.40 mg/24 h (P<0.001), −85 ng/ml (P=0.01) and −50 ng/ml (P=0.02)), but brachial artery endothelium-dependent and -independent vasodilation and levels of von Willebrand factor and C-reactive protein did not change (GEE regression coefficients, 0.21 mm (P=0.07), 0.04 mm (P=0.43), 0.04 IU/ml (P=0.33) and −1.15 mg/l (P=0.64)). No differences in outcome variables between treatment groups were observed. These data show that achievement of target blood pressures below 130/85 mmHg in hypertensive type II diabetes is difficult. Aggressive antihypertensive therapy can improve urinary albumin excretion, endothelial function and inflammatory activity in hypertensive type II diabetic individuals, regardless of the type of antihypertensive therapy used.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 digital issues and online access to articles
$119.00 per year
only $9.92 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Estacio RO et al. The effect of nisoldipine as compared with enalapril on cardiovascular outcomes in patients with non-insulin-dependent diabetes and hypertension. N Engl J Med 1998; 338: 645–652.
Lewis EJ et al. Renoprotective effect of the angiotensin-receptor antagonist irbesartan in patients with nephropathy due to type 2 diabetes. N Engl J Med 2001; 345: 851–860.
Tatti P et al. Outcome results of the Fosinopril Versus Amlodipine Cardiovascular Events Randomized Trial (FACET) in patients with hypertension and NIDDM. Diabetes Care 1998; 21: 597–603.
Staessen JA et al. Risks of untreated and treated isolated systolic hypertension in the elderly: meta-analysis of outcome trials. Lancet 2000; 355: 865–872.
Chobanian AV et al. The seventh report of the Joint National Committee on prevention, detection, evaluation, and treatment of high blood pressure: the JNC 7 report. JAMA 2003; 289: 2560–2572.
Stehouwer CD et al. Increased urinary albumin excretion, endothelial dysfunction, and chronic low-grade inflammation in type 2 diabetes: progressive, interrelated, and independently associated with risk of death. Diabetes 2002; 51: 1157–1165.
Rahman ST et al. Effects of eprosartan versus hydrochlorothiazide on markers of vascular oxidation and inflammation and blood pressure (rennin–angiotensin system antagonists, oxidation, and inflammation). Am J Cardiol 2002; 89: 686–690.
Gasic S et al. Fosinopril decreases levels of soluble vascular cell adhesion molecule-1 in borderline hypertensive type II diabetic patients with microalbuminuria. Am J Hypertens 1999; 12: 217–222.
Rajagopalan S et al. Effect of losartan in aging-related endothelial impairment. Am J Cardiol 2002; 89: 562–566.
Jilma B et al. Effects of enalapril and losartan on circulating adhesion molecules and monocyte chemotactic protein-1. Clin Sci (Lond) 2002; 103: 131–136.
van Dijk RA et al. Determinants of brachial artery mean 24 h pulse pressure in individuals with Type II diabetes mellitus and untreated mild hypertension. Clin Sci (Lond) 2002; 102: 177–186.
Lambert J et al. Endothelium-dependent and -independent vasodilation of large arteries in normoalbuminuric insulin-dependent diabetes mellitus. Arterioscler Thromb Vasc Biol 1996; 16: 705–711.
Henry RM et al. Left ventricular mass increases with deteriorating glucose tolerance, especially in women: independence of increased arterial stiffness or decreased flow-mediated dilation: the Hoorn study. Diabetes Care 2004; 27: 522–529.
Ingerslev J . A sensitive ELISA for von Willebrand factor (vWf:Ag). Scand J Clin Lab Invest 1987; 47: 143–149.
Schalkwijk CG et al. Plasma concentration of C-reactive protein is increased in type I diabetic patients without clinical macroangiopathy and correlates with markers of endothelial dysfunction: evidence for chronic inflammation. Diabetologia 1999; 42: 351–357.
Zeger SL, Liang KY . Longitudinal data analysis for discrete and continuous outcomes. Biometrics 1986; 42: 121–130.
Adler AI et al. Development and progression of nephropathy in type 2 diabetes: the United Kingdom Prospective Diabetes Study (UKPDS 64). Kidney Int 2003; 63: 225–232.
Schiffrin EL . Effects of antihypertensive drugs on vascular remodeling: do they predict outcome in response to antihypertensive therapy? Curr Opin Nephrol Hypertens 2001; 10: 617–624.
Ridker PM et al. C-reactive protein and other markers of inflammation in the prediction of cardiovascular disease in women. N Engl J Med 2000; 342: 836–843.
Jager A et al. von Willebrand factor, C-reactive protein, and 5-year mortality in diabetic and nondiabetic subjects: the Hoorn Study. Arterioscler Thromb Vasc Biol 1999; 19: 3071–3078.
UK Prospective Diabetes Study Group. Tight blood pressure control and risk of macrovascular and microvascular complications in type 2 diabetes: UKPDS 38. BMJ 1998; 317: 703–713.
Parving HH et al. The effect of irbesartan on the development of diabetic nephropathy in patients with type 2 diabetes. N Engl J Med 2001; 345: 870–878.
Brenner BM et al. Effects of losartan on renal and cardiovascular outcomes in patients with type 2 diabetes and nephropathy. N Engl J Med 2001; 345: 861–869.
Heart Outcomes Prevention Evaluation Study Investigators. Effects of ramipril on cardiovascular and microvascular outcomes in people with diabetes mellitus: results of the HOPE study and MICRO-HOPE substudy. Lancet 2000; 355: 253–259.
Acknowledgements
AstraZeneca provided funding for this clinical trial (to CDAS), but had no influence on the data analyses or manuscript preparation. We thank Teri Brouwer for her valuable contribution and Ellen Bulterijs, Greetje de Vries and Harry Twaalfhoven for their excellent assistance.
Author information
Authors and Affiliations
Corresponding author
Additional information
Conflicts of interest: None.
Rights and permissions
About this article
Cite this article
Schram, M., van Ittersum, F., Spoelstra-de Man, A. et al. Aggressive antihypertensive therapy based on hydrochlorothiazide, candesartan or lisinopril as initial choice in hypertensive type II diabetic individuals: effects on albumin excretion, endothelial function and inflammation in a double-blind, randomized clinical trial. J Hum Hypertens 19, 429–437 (2005). https://doi.org/10.1038/sj.jhh.1001812
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.jhh.1001812
Keywords
This article is cited by
-
Potential Protective Role of Blood Pressure-Lowering Drugs on the Balance between Hemostasis and Fibrinolysis in Hypertensive Patients at Rest and During Exercise
American Journal of Cardiovascular Drugs (2019)
-
First-line renin–angiotensin system inhibitors vs. other first-line antihypertensive drug classes in hypertensive patients with type 2 diabetes mellitus
Journal of Human Hypertension (2018)
-
Blood pressure management in patients with type 2 diabetes mellitus
Hypertension Research (2017)
-
Effect of erythropoietin-stimulating agent on uremic inflammation
Journal of Inflammation (2012)
-
Updated Report on Comparative Effectiveness of ACE inhibitors, ARBs, and Direct Renin Inhibitors for Patients with Essential Hypertension: Much More Data, Little New Information
Journal of General Internal Medicine (2012)