Videofluoroscopic Swallow Study
The videofluoroscopic swallow study (VFSS) is the most commonly utilized instrumental assessment tool to determine the nature and extent of an oropharyngeal swallowing disorder. The studies are captured using fluoroscopy in video or digitized format that allows detailed analysis of the oropharyngeal swallowing process. The VFSS does not diagnose the etiology of the swallowing disorder; instead, it determines the details of oropharyngeal swallow dysfunction and helps guide decisions regarding behavioral swallow therapy based on those findings.
The American Speech-Language Hearing Association (ASHA) recently published Guidelines for Speech-Language Pathologists Performing Videofluoroscopic Swallowing Studies.1 Table 1 lists the indications, contraindications, and limitations of VFSS. These are reviewed prior to the study.
VFSS Protocol
The VFSS protocol can vary from facility to facility, and from clinician to clinician, but a standard protocol focused on oropharyngeal swallow physiology assessment with an eye toward possible management of pathophysiologies is the goal. Good clinical judgment is needed to determine the order of bolus presentation or modifications to the procedure if the individual appears unable to protect the airway even after the use of therapeutic intervention. Bolus presentation should be guided by patient performance, aspiration risks, abnormalities identified, and patient tolerance.
VFSS Protocol at VA Boston Healthcare
(Table 2)
At VA Boston Healthcare System (VA BHS) these studies are performed jointly by a speech-language pathologist and a radiologist.
Indications for the procedure reviewed. Once it is decided that the procedure is indicated, information is provided to the patient and caregiver regarding the VFSS procedure, safety, and the rationale for the examination. They are encouraged to ask questions and seek clarification. The next step is to work out the appropriate method of transport to the radiology department and to determine the patient's position to be used for the study.
A video imaging chair is primarily used. However, sometimes the study is performed with the patient in the standing position for a faster study, when it is safe and acceptable to the patient. The upright positioning may be precluded because of medical conditions such as low blood pressure, acute stroke, spinal cord injury bracing, or other skeletal limitations. Under such circumstances, the patient can also be placed in the side-lying position or in the patient's representative eating position.
Whenever possible, the patient is seated as upright as possible. All studies are started with the patient in the lateral view where aspiration is most efficiently detected, and then finished with an anterior-posterior view to assess swallow symmetry and vocal cord function. Observation of vocal cord movement on pronouncement of the vowel /ah/ by the patient is often used as the end point of the study.
With fluoroscopy, anatomic structures and landmarks are identified with mechanism at rest without contrast.
A standard protocol is utilized for administration of radiopaque material (usually barium) mixed with liquid and food of varying consistencies in smaller to larger amounts and thinner to thicker viscosities as tolerated. The typical protocol utilizes thin liquid, thick liquid (nectar), puree, and solid (graham cracker cookie) coated with puree as our standard administration, but this is altered pending any unique circumstance or request from patient or staff. Examination of the esophagus is at the discretion of the radiologist.
The current system of equipment and materials at VA Boston Healthcare System is listed in Table 3. The facility is now transitioning from standard S-VHS videotape format to a digital image capture and manipulations system.
Three minutes or less of fluoroscopy time are targeted, and often the studies are completed in 90 to 120 seconds. Knowledge of radiation safety cannot be stressed enough to keep radiation exposures "as low as reasonably achievable" (ALARA). The goal is always to practice safety factors of time (shortest necessary), distance (from x-ray tube), and shielding (led apron, thyroid shield, gloves glasses where appropriate).
The radiographic images are observed on a monitor during the procedure, some stills are taken, and images are simultaneously recorded on videotape or digitally for further detailed analysis.
Further review of these steps is illustrated in Video 1, which highlights procedures used during the VFSS protocol at VA Boston Healthcare System.
Analysis, Interpretation, and Reporting
The checklist analysis protocol used at VA Boston Healthcare System is shown in Table 4.
The worksheet incorporates use of comparative scales for both level of penetration (adapted from Rosenbek et al.2) seen in Table 5, and dysphagia severity rating (adapted from Waxman et al.3) seen in Table 6. These scales are helpful in comparing level of penetration and level of swallowing impairment within and across patients. They are also helpful in comparing any improvements in swallow impairment post-treatment.
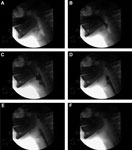
Simplified but accurate reporting is a critical part of communication with the primary physician and other caregivers and the patients, and the details of swallow dysfunction help clinicians guide specific treatments. Stills of the swallow events (Figure 1) may be very useful in quick representation of the swallowing events. The key normal swallowing events summarized in Table 7, and commonly observed abnormalities are summarized in Table 8.
Figure 1: Normal swallowing events in a young male viewed fluoroscopically.
a: Bolus hold position, glossopalatal seal maintained. b: Tongue tip elevation, soft palate elevates to closure, and bolus passes mandible ramus. c: Bolus moves posteriorly as tongue moves backward, hyoid and larynx begin to ascend, and epiglottis tilting. d: Larynx closed, epiglottis inverted, UES begins to open. e: Pharynx constricts, tongue base against pharynx, maximum hyoid elevation, UES open. f: Bolus tail through UES, structures returning to rest.
Examples of Swallow Studies
Video 2 shows a normal VFSS in an healthy adult. Figure 1 shows elements of the sequence in stills. Note the key normal events listed in Table 7. Aging is accompanied by many subtle changes in swallowing function. Changes in swallowing function in otherwise healthy subjects over the age of 85 years are listed in Table 9. It is important to note that normal aging is never associated with dysphagia or aspiration.
Video 2: Interpretation, normal.
(Source: Gates J, Hartnell GG, Gramigna GD. Videofluoroscopy and swallowing studies for neurologic disease: a primer. RadioGraphics 2006;26:e22., with permission)
Video 3 shows a disordered swallow pattern by VFSS for a patient with traumatic brainstem injury. Note many of the abnormalities as summarized in Table 8.
Note the large number of swallowing abnormalities (Table 9) including aspiration and absent opening of the upper esophageal sphincter due to the lack of anterior displacement of the cricoid cartilage.
Behavioral Swallow Treatment
The observed functional abnormalities are utilized in designing behavioral treatment plans for patients. Table 10 summarizes some of the treatments based on the observed abnormalities. As a single study, VFSS provides the most physiologic information in oral and pharyngeal stages and may be considered a physiologic standard of assessment.
A list of suggested readings is provided below.
Suggested Readings
American Speech-Language-Hearing Association. Clinical indicators for instrumentation assessment of dysphagia. In: Swallowing and Swallowing Disorders, 1998. Rockville, MD: Special Interest Division on Dysphagia, American Speech-Language-Hearing Association, 1998.
American Speech-Language-Hearing Association. Clinical indicators for instrumental assessment of dysphagia (guidelines). ASHA 2000; suppl 20:18–19.
Bisch EM, Logemann JA, Rademaker AW, Kahrilas PJ, Lazarus CL. Pharyngeal effects of bolus volume, viscosity, and temperature in patients with dysphagia resulting from neurologic impairment and in normal subjects. J Speech Hearing Res 1994;37:1041–1059.
Bucholz DW, Robbins J. Neurologic diseases affecting oropharyngeal swallowing. In: Perlman AL, Schulze-Delrieu KS, eds. Deglutition and Its Disorders Anatomy, Physiology, Clinical Diagnosis and Management. San Diego: Singular, 1997:319–342.
Cook IJ, Kahrilas PJ. AGA technical review on management of oropharyngeal dysphagia. Gastroenterology 1999;116:455–478.
Dantas RO, Kern MK, Massey BT, et al. Effect of swallowed bolus variables on oral and pharyngeal phases of swallowing. Am J Physiol 1990;258:G675–G681.
Donner MW, Jones B. Editorial. Gastrointest Radiol 1983;10:194–195.
Donner MW, Siegel CI. The evaluation of pharyngeal neuromuscular disorders by cineradiography. AJR 1965;94:299>–307.
Eisenhuber E, Schima W, Schober E, et al. Videofluoroscopic assessment of patients with dysphagia: pharyngeal retention is a predictive factor for aspiration. AJR 2002;178:393–398.
Ekberg O, Hamdy S, Woisard V, Wutte-Hannig A, Ortega P. Social and psychological burden of dysphagia: its impact on diagnosis and treatment. Dysphagia 2002;17:139–146.
Feinberg M, Ekberg O. Videofluoroscopy in elderly patients with aspiration: importance of evaluating both oral and pharyngeal stages of deglutition. AJR 1991;156:293–296.
Gates J, Hartnell GG, Gramigna GD. Videofluoroscopy and swallowing studies for neurologic disease: a primer. RadioGraphics 2006;26:e22. doi:10.1148/rg.e22. Published November 8, 2005.
Kahrilas PJ, Logemann JA. Volume accommodations during swallowing. Dysphagia 1993;8:259–265.
Logemann JA. Evaluation and Treatment of Swallowing Disorders, 2nd ed. San Diego, CA: College Hill, 1998.
Logemann JA. Manual for the Videofluoroscopic Study of Swallowing, 2nd ed. Austin TX: Pro-Ed, 1993.
Logemann JA. Screening, diagnosis, and management of neurogenic dysphagia. Semin Neurol 1996;16(4):319–327.
Marik PE, Kaplan D. Aspiration pneumonia and dysphagia in the elderly. Chest 2003;124:328–336.
Miller RM, Langmore SE. Treatment efficacy for adults with oropharyngeal dysphagia. Arch Phys Med Rehabil 1994;75:1256–5662.
Odderson IR, Keaton JC, McKenna BS. Swallow management in patients on an acute stroke pathway: quality is cost effective. Arch Phys Med Rehabil 1995;76(12):1130–1133.
Palmer JB, Kuhlemeier KV, Tippett DC, Lynch C. A protocol for the videofluorographic swallowing study. Dysphagia 1993;8:209–214.
Pikus L, Levine MS, Yang YX, et al. Videofluoroscopic studies of swallowing and the relative risk of pneumonia. AJR 2003;190:1613–1616.
Shaker R, Ren J, Podvrsan B, et al. Effects of aging and bolus variables on pharyngeal and upper esophageal sphincter motor function. Am J Physiol 1993;264:G427–G432.
Veterans Health Administration, Department of Defense. VA/DoD Clinical Practice Guideline for the Management of Stroke Rehabilitation in the Primary Care Setting. Washington (DC): Department of Veteran Affairs; 2003.