Abstract
Objective:
To determine the differential efficacy and safety of twice-weekly administration of 3 RDAs of iron and folic acid, with and without a complement of 2 RDAs of 11, and 1 RDA of 3 additional essential micronutrients as compared to a placebo control (PlbCON) given as foodLETs.
Subjects/Methods:
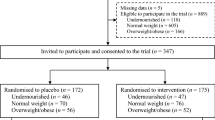
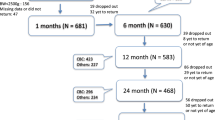
A total of 250 children aged 6–24 months were enrolled after recruitment by village health workers; 19 of them dropped out during the trial. Children were assigned to one of three treatment arms and followed for 20.5 weeks; 41 supervised twice-weekly dosings of 30 mg of iron plus folic acid, either with or without accompanying micronutrients or placebo were given as foodLETs, a tool for ready-to-eat fortification in infant food. Initial and final measurements of anthropometry and blood biomarkers for hematological, iron stores and inflammatory status, as well as for abnormal hemoglobin (Hb), were obtained. Symptoms of listlessness, vomiting, watery stools and acute respiratory infections were monitored weekly.
Results:
Iron-containing supplements increased Hb concentrations significantly (P<0.0001) and virtually eradicated any IDA, as compared to no change in hematological status in the PlbCON group (P=0.011). Iron stores, as reflected by ferritin, increased significantly with iron-containing treatments (P<0.0001). Responses were as effective in individuals with HbE as in those with exclusively HbA phenotypes. Watery stools (P=0.002) and listlessness (P=0.001) were significantly more frequent in those receiving iron and folic acid alone than in the PlbCON group. In contrast, acute respiratory infections (P=0.014) and listlessness (P=0.001) were significantly less frequent in those receiving the multiple micronutrient formulation than in the PlbCON group.
Conclusions:
Supplementation of micronutrients along with iron and folic acid mitigates the excess morbidity of iron-folate alone, without reducing its efficacy in correcting anemia and building iron stores. FoodLETs are a suitable vehicle to provide micronutrient supplementation to infants.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Algarin C, Peirano P, Garrido M, Pizarro F, Lozoff B (2003). Iron deficiency anemia in infancy: long-lasting effects on auditory and visual system functioning. Ped Res 53, 217–223.
Allen L, Shrimpton R (2005). The International Research on Infant Supplementation Study: implications for programs and further research. J Nutr 135, 666S–669S.
Allen LH (2001). Pregnancy and lactation. In: Bowman BA, Russell RM (eds). Present knowledge in nutrition. Chapter 37, 8th edn. ILSI Press: Washington DC, pp 403–415.
Allen LH, Rosado JL, Casterline JE, Lopez P, Munoz E, Garcia OP et al. (2000). Lack of hemoglobin response to iron supplementation in anemic Mexican preschoolers with multiple micronutrient deficiencies. Am J Clin Nutr 71, 1485–1494.
Angeles-Agdeppa I, Schultink W, Sastroamidjojo S, Gross R, Karyadi D (1997). Weekly micronutrient supplementation to build iron stores in female Indonesian adolescents. Am J Clin Nutr 66, 177–183.
Asobayire S, Adou P, Davidsson L, Cook JD, Hurrell RF (2001). Prevalence of iron deficiency with and without concurrent anemia in population groups with high prevalences of malaria and other infections: a study in Cote d'Ivoire. Am J Clin Nutr 74, 776–782.
Beard JL (1998). Weekly iron intervention: the case for intermittent iron supplementation. Am J Clin Nutr 68, 209–212.
Bhaskaram P (2002). Micronutrient malnutrition, infection, and immunity: an overview. Nutr Rev 60, S40–S45.
Bhutta ZA, Black RE, Brown KH, Gardner JM, Gore S, Hidayat A et al. (1999). Prevention of diarrhea and pneumonia by zinc supplementation in children in developing countries: pooled analysis of randomized controlled trials. Zinc Investigators' Collaborative Group. J Pediatr 135, 689–697.
Bloem MW (1995). Interdependence of vitamin A and iron: an important association for programmes of anaemia control. Proc Nutr Soc 54, 501–508.
Briend A, Solomons NW (2003). The evolving applications of spreads as a foofLET for improving the diets of infants and young children. Food Nutr Bull 24 (3 Suppl), S34–S38.
Brock C, Carry H, Hama C, Knipfel M, Taylor L (1985). Adverse effects of iron supplementation: a comparative trail of wax-matrix iron preparations and conventional ferrous sulfate tablets. Clin Ther 7, 568–573.
Brown KH, Dewey KG, Allen LH (1998). Complementary feeding of young children in developing countries: a review of current scientific knowledge. World Health Organization/UNICEF: Geneva.
Brown KH, Peerson IM, Rivery J, Allen LH (2002). Effect of supplemental zinc on the growth and serum zinc concentration of prepupertal children: a meta-analysis of randomized controlled trials. Am J Clin Nutr 75, 1062–1071.
Casanueva E, Erazo B, Rosales X, Tolentino M, Viteri F (2005). Anemia, oxidative stress and iron supplementation on pregnant women. FASEB Journal 19, A 846.11.
Chandra RK, Kumari S (1994). Nutrition and immunity: an overview. J Nutr 124 (Suppl), 1433–1435.
Christian P, West KP, Khatry SK, Leclerq SC, Pradhan EK, Katz J et al. (2003). Effects of maternal micronutrient supplementation on fetal loss and infant mortality: a cluster-randomized trial in Nepal. Am J Clin Nutr 78, 1194–1202.
Cook JD, Finch CA (1979). Assessing iron status of a population. Am J Clin Nutr 32, 2115–2119.
Dallman PR, Reeves JD, Drigger DA, Lo EY (1981). Diagnosis of iron deficiency: the limitations of laboratory tests in predicting responses to iron treatment in 1-year-old infants. J Pediatr 99, 376–381.
Dewey KG, Romero-Abal ME, Quan de Serrano J, Bulux J, Peerson JM, Eagle P et al. (1997). Effects of discontinuing coffee intake on iron status of iron-deficient Guatemalan toddlers: a randomized intervention study. Am J Clin Nutr 66, 168–176.
Eide WB, Kracht U (1999). Towards a definition of the right to food and nutrition: reflections on General Comment No. 12. SCN News 18, 39–40.
Failla ML (2003). Trace elements and host defense: recent advances and continuing challenges. J Nutr 133 (5 Suppl 1), 1443S–1447S.
Fang YZ, Yang S, Wu G (2002). Free radicals, antioxidants, and nutrition. Nutr 18, 872–879.
Fawzi WW, Msamanga GI, Spiegelman D, Wei R, Kapiga S, Villamor E et al. (2004). A randomized trial of multivitamin supplements and HIV disease progression and mortality. N Engl J Med 351, 23–31.
Flint J, Harding RM, Boyce AJ, Clegg JB (1993). The population genetics of the haemoglobinopathies. Baillieres Clin Haematol 6, 215–262.
Frazer DM, Wilkins SJ, Becker EM, Murphy TL, Vulpe CD, McKie AT et al. (2003). A rapid decrease in the expression of DMT1 and Dcytb but not Ireg1 or hephaestin explains the mucosal block phenomenon of iron absorption. Gut 52, 340–346.
Ganzoni AM, Töndung G, Rhyner K (1974). Orale Eisenmedikation. Dtsch Med Wochenschr 99, 1175–1178.
Gera G, Sachdev HPS (2002). Effect of iron supplementation on incidence of infectious illness in children: systematic review. BMJ 325, 1142–1152.
Giovannini M, Sala D, Usuelli M, Livio L, Francescato G, Braga M et al. (2006). Double blind, placebo-controlled trial comparing effects of supplementation with two different combinations of micronutrients delivered as sprinkles on growth, anemia, and iron-deficiency in Cambodian infants. J Pediatr Gastroenterol Nutr 42, 306–312.
Gross R, Bernade S, Lopez G (2005). The International Research on Infant Supplementation Initiative. J Nutr 135, 628S–630S.
Gross R (ed). (2001). Micronutrient supplementation throughout the life cycle. Report of a workshop held by the Ministry of Health, Brazil and UNICEF. UNICEF: New York.
Gross R, Solomons NW (2003). Research needs in micronutrient deficiencies. Food Nutr Bull 24, S42–S53.
Hadi H, Stoltzfus RJ, Dibley MJ, Moulton LH, West Jr KP, Kjolhede CL et al. (2000). Vitamin A supplementation selectively improves the linear growth of Indonesian preschool children: results from a randomized controlled trial. Am J Clin Nutr 71, 507–513.
Hallberg L (1998). Combating iron deficiency: daily administration of iron is far superior to weekly administration. Am J Clin Nutr 68, 213–217.
Helen Keller International (1999). Iron deficiency in Cambodia. A threat to the development of young Cambodian children and the country's future. HKI-Nut Bull 1, 1–3.
Herbert V (1973). The five possible causes of all nutrient deficiency: illustrated by deficiencies of vitamin B12. Am J Clin Nutr 26, 77–86.
Hoffman II HN, Phyliky RL, Fleming CR (1988). Zinc-induced copper deficiency. Gastroenterology 94, 508–512.
Hop LT, Berger J (2005). Multiple micronutrient supplementation improves anemia, micronutrient nutrient status, and growth of Vietnamese infants: double blind, randomized, placebo-controlled trial. J Nutr 135, 660–665.
Idjradinata P, Watkins WE, Pollitt E (1994). Adverse effects of iron supplementation on weight gain of iron-replete young children. Lancet 343, 1252–1254.
Institute of Medicine, Food and Nutrition Board (1998). Dietary Reference Intakes for Thiamine, Riboflavin, Niacin, Vitamin B6, folate, Vitamin B12, Pantothenic Acid, Biotin and Choline. National Academy Press: Washington, DC.
Institute of Medicine, Food and Nutrition Board (2001). Dietary Reference Intakes for vitamin A, vitamin K, arsenic, boron, chromium, copper, iodine, iron, manganese, molybdenum, nickel, silicon, vanadium and zinc. National Academy of Science Press: Washington DC.
IRIS Study Group: Smuts CM, Lombard CJ, Bernade AJS, Dhansay MA, Berger J, Hop LT et al. (2005). Efficacy of a foodlet-based multiple micronutrient supplement for preventing growth faltering, anemia, and micronutrient deficiency of infants: the four country IRIS trial pooled data analysis. J Nutr 135, 631–638.
Jack S, Monchy D, Hem N, Hok P, Anderson V, Bailey K et al. (2004). Zinc deficiency amongst stunted children in Phnom Penh, Cambodia (abst.). IZiNCG Symposium Lima, Peru, Program and Abstract: 16.
Kordas K, Stoltzfus RJ (2004). New evidence of iron and zinc interplay at the enterocyte and neural tissue. J Nutr 134, 1295–1298.
Lock G (2003). The foodLET vehicle designed for and used in the IRIS I intervention. Food Nutr Bull 24 (3 Suppl), S16–S19.
Longfils P, Heang HK, Soeng H, Sinuon M (2005). Weekly iron and folic acid supplementation as a tool to reduce anemia among primary school children in Cambodia. Nutr Rev 63, S139–S145.
Lopez de Romaña G, Cusirramos S, Lopez de Romaña D, Gross R (2005). Efficacy of multiple micronutrient supplementation for improving anemia, micronutrient status, growth, and morbidity of Peruvian infants. J Nutr 135, 646S–6652.
Lozoff B, Jimenez E, Wolf AW (1991). Long-term developmental outcome of infants with iron deficiency. New Engl J Med 325, 687–694.
Majumdar I, Paul P, Talib VH, Ranga S (2003). The effect of iron therapy on growth of iron-replete and iron-depleted children. J Trop Pediatr 49, 84–88.
Nestel P, Briend A, de Benoist B, Decker E, Ferguson E, Fontaine O et al. (2003). Complementary food supplements to achieve micronutrient adequacy for infants and young children. J Pediatr Gastroenterol Nut 36, 316–328.
Oates PS, Thomas C, Freitas E, Callow MJ, Morgan EH (2000). Gene expression of divalent metal transporter 1 and transferrin receptor in duodenum of Belgrade rats. Am J Physiol 278, G930–G936.
Penny ME, Marin RM, Duran A, Peerson JM, Lanata CF, Lönnerdal B et al. (2004). Randomized controlled trial of the effect of daily supplementation with zinc or multiple micronutrients on the morbidity, growth, and micronutrient status of young Peruvian children. Am J Clin Nutr 79, 457–465.
Pollitt E (2001). The developmental and probabilistic nature of the functional consequences of iron-deficiency anemia in children. J Nutr 131, 669S–675S.
Powers HJ (1995). Riboflavin-rich interactions with particular emphasis on the gastrointestinal tract. Proc Nutr Soc 54, 509–517.
Powers HJ (2003). Riboflavin (vitamin B-2) and health (2003). Am J Clin Nutr 77, 1352–1360.
Rongguang Z, Kent G (2004). Human rights and the governance of food quality and safety in China. Asia Pacific J Clin Nutr 13, 178–183.
Sazawal S, Black RE, Ramsan M, Chwaya HM, Stoltzfus RJ, Dutta A et al. (2006). Effects of routine prophylactic supplementation with iron and folic acid on admission to hospital and mortality in preschool children in a high malaria transmission setting: community-based, randomized, placebo-controlled trial. Lancet 367, 133–143.
Schultink W, Gross R (1999). Use of daily compared with weekly iron supplementation: apples and pears. Am J Clin Nutr 69, 739–742.
Schultink W, Gross R, Gliwitzki M, Karyadi D, Matulessi P (1995). Effect of daily vs twice weekly iron supplementation in Indonesian preschool children with a low iron status. Am J Clin Nutr 61, 111–115.
Schultink W, Gross R, Smuts CM, Lombard CH, Swanevelder SA (2002). International research on infant supplementation: analysis of the multi-centre study in the efficacy of multi-micronutrient supplementation on small children. Draft report. UNICEF: New York.
Schümann K (2001). Safety aspects of iron in food. Ann Nutr Metab 45, 91–101.
Schümann K, Romero-Abal ME, Mäurer A, Luck T, Beard J, Murray-Kolb L et al. (2005). Haematological response to haem iron or ferrous sulphate mixed with refried beans in moderately anemic Guatemalan preschool children. PHN 8, 572–581.
Scrimshaw NS (2004). The SCN and the Millenium Developments Goals. Keynote address. SCN News 28, 19–23.
Semba RD, Bloem MW (2002). The anemia of vitamin A deficiency: epidemiology and pathogenesis. Eur J Clin Nutr 56, 271–281.
Smuts CM, Benadé AJS, Berger J, Hop LT, Lopez de Romaña G, Untoro J et al. (2003). IRIS I: a foodlet-based multiple micronutrient in 6- to 12-month-old infants at high risk of micronutrient malnutrition in four contrasting populations: description of a multicenter field trial. Food Nutr Bull 24, S27–S33.
Smuts CM, Dhansay MA, Faber M, van Stuijvenberg ME, Swanevelder S, Gross R et al. (2005). Efficacy of multiple micronutrient supplementation or improving anemia, micronutrient status, and growth in South African infants. J Nutr 135, 653–659.
Solomons NW (1986). Competitive interaction of iron and zinc in the diet: consequences for human nutrition. J Nutr 16, 927–935.
Solomons NW, Jacob RA (1981). Studies on the bioavailability of zinc in humans: effects of heme and non-heme iron on the absorption of zinc. Am J Clin Nutr 34, 475–482.
Thu BD, Schultink JW, Dillon D, Gross R, Leswara ND, Khoi HH (1999). Effect of daily and weekly micronutrient supplementation on micronutrient deficiencies and growth of young Vietnamese children. Am J Clin Nutr 69, 80–86.
Troost FJ, Saris WH, Haenen GRMM, Bast A, Brummer RJM (2003). New method to study oxidative damage and oxidation of the human small bowel: effects of iron application. Am J Physiol 285, G354–G359.
Untoro J, Karyidi E, Wibowo L, Erhard MW, Gross R (2005). Multiple micronutrient supplementation improves micronutrient status and anemia but not growth and morbidity of Indonesian infants. A randomized, double-blind, placebo-controlled trial. J Nutr 135, 639S–645S.
Verhoef H, West CE, Ndeto P, Burema J, Beguin Y, Kok FJ (2001). Serum transferrin receptor concentration indicates increased erythropoiesis in Kenyan children with asymptomatic malaria. Am J Clin Nutr 74, 767–775.
Viteri FE (1997). Iron supplementation for the control of iron deficiency in populations at risk. Nutr Rev 55, 195–209.
Weinberg ED (1993). The development of awareness of iron-withholding defense. Perspect Biol Med 36, 215–221.
Yip R (2001). Iron. In: Bowman BA, Russell RM (eds). Present Knowledge in Nutrition. Chapter 30, 8th edn. ILSI Press: Washington DC, pp 311–351.
Yip R, Reeves JD, Lönnerdal B, Keen CL, Dallman PR (1985). Does iron supplementation compromise zinc nutrition in healthy infants? Am J Clin Nutr 42, 683–687.
Zlotkin S, Arthur P, Antwi KY, Yeung G (2001). Treatment of anemia with microencapsulated ferrous fumarate plus ascorbic acid supplied as sprinkles to complementary (weaning) foods. Am J Clin Nutr 74, 791–795.
Acknowledgements
The authors acknowledge the inspiration of a vision on multiple nutrient interventions to resolve micronutrient malnutrition gained from our association with the late Dr Rainer Gross. The study was organized and funded by FSNPSP–GTZ. We thank Ung Kim Heang and Hay Soeng for assistance in the field. Our thanks go to Lomapharm for custom-tailored production and supply of the foodLETs and to Roche for donation of the vitamin mix. We are indebted to Jenny Bush-Hallen for her input in this study and to UNICEF Cambodia for additional financial support. The study was organized and funded by FSNPSP-GTZ with additional financial support from UNICEF Cambodia.
Author information
Authors and Affiliations
Corresponding author
Additional information
Guarantor: K Schümann.
Contributions: KS and NWS designed the study and drafted the manuscript; PL organized and supervised the study in the field; DM performed the laboratory analysis; SvX helped with the study design and with its gearing to local and international requirements; HW did the statistical evaluation. All contributors wrote respective parts of the manuscript.
Rights and permissions
About this article
Cite this article
Schümann, K., Longfils, P., Monchy, D. et al. Efficacy and safety of twice-weekly administration of three RDAs of iron and folic acid with and without complement of 14 essential micronutrients at one or two RDAs: a placebo-controlled intervention trial in anemic Cambodian infants 6 to 24 months of age. Eur J Clin Nutr 63, 355–368 (2009). https://doi.org/10.1038/sj.ejcn.1602930
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.ejcn.1602930