Abstract
Data sources
Ovid MEDLINE and Ovid OLDMEDLINE (January 1950 to January 2010), CINAHL (1982 to January 2010), Cochrane Library (up to 2010) and EMBASE (1981 to January 2010), bibliographies of potentially relevant reports and reviews, handsearching of Community Dentistry and Oral Epidemiology, Gerodontology, Journal of Disability and Oral Health and Special Care in Dentistry.
Study selection
Longitudinal prospective observational studies in individuals of all ages being hospitalised, that assessed changes of the following outcomes: tooth loss, any measures of periodontal health, dental caries and stomatological diseases. There were no language restrictions.
Data extraction and synthesis
One reviewer scanned the titles and abstracts to select studies. Potentially eligible studies were screened by two reviewers who also data extracted using specially designed forms. Quality was assessed by both reviewers using the Newcastle–Ottawa scale for cohort studies. The authors assessed whether a power calculation was reported for each study and, if so, the magnitude of a change that the study was powered to detect. Heterogeneity between studies was anticipated so a narrative review was planned.
Results
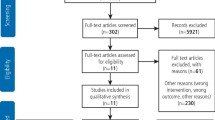
Five studies were included and all were assessed to be adequately representative and had sufficient follow-up. Outcome assessments were adequate but validity of the outcome measures was found to be subjective. One investigation included children only, whilst the remainder included adults only. Four of the studies were in intensive care units. Duration of hospitalisation was 5-20 days. This was insufficient a period for caries to develop. A power calculation was reported in only one study. Three out of four studies that reported on plaque accumulation found increasing levels of plaque accumulation during hospitalisation, whilst one did not. Two of three studies assessing gingival inflammation found a statistically significant increase. Two studies found a statistically significant increased incidence of mucositis in intubated patients but not in non-intubated patients.
Conclusions
Hospitalisation is associated with a deterioration in oral health, particularly in intubated patients.
Similar content being viewed by others
Commentary
This well-conducted systematic review addresses the impact of hospitalisation on oral health. Although daily oral hygiene measures are an important part of the care of hospitalised patients, it seems often to be given a low priority among the caregivers.1
The authors used an exhaustive database search strategy and handsearching to locate relevant studies. Two possibly relevant papers were not possible to retrieve, but the methodology of the review is well described, and in accordance with the recommendations for conducting systematic reviews.
In the five studies that fulfilled the inclusion criteria, the follow-up periods were long enough to be able to assess changes in oral hygiene and in gingival health. However, the validity of the outcome measurements was questionable due to the usage of subjective and epidemiological indices. There was also a substantial variation between the protocols, and in the frequencies of oral care provided.
The presented results indicate that dental plaque accumulation and gingival inflammation increases during hospitalisation, thus leading to deterioration of oral health among the included patient groups, especially among intubated patients.
In addition to deterioration of oral health, it has previously been shown that improved oral hygiene reduces the occurrence of respiratory tract diseases among elderly in ICUs.2 Moreover, approximately one out of ten cases of death from pneumonia among hospitalised elderly could be prevented by improving their oral hygiene.3
All of the included studies were, at least to some extent, conducted in ICU wards and often on intubated patients. Thus, the authors suggest that more studies are needed on non-intubated patients, and outside of ICU settings.
Practice points
-
Oral care needs to be improved and integrated into the care-chain of hospitalised individuals. This is not only a matter of oral health but may also lead to saving lives.
References
Grap MJ, Munro CL, Ashtiani B, et al. Oral care interventions in critical care: frequency and documentation. Am J Crit Care 2003; 12: 113–118.
Azarpazhooh A, Leake JL . Systematic review of the association between respiratory diseases and oral health. J Periodontol 2006; 77: 1465–1482.
Sjögren P, Nilsson E, Forsell M, Johansson O, Hoogstraate J . A systematic review of the preventive effect of oral hygiene on pneumonia and respiratory tract infection in elderly in hospitals and nursing homes: effect estimates and methodological quality of randomized controlled trials. J Am Geriatr Soc 2008; 56: 2124–2130.
Author information
Authors and Affiliations
Additional information
Address for correspondence: Unit of Periodontology and International, Centre for Evidence-Based Oral Health, UCL Eastman Dental Institute, London, UK.
Terezakis E, Needleman I, Kumar N, Moles D, Agudo E. The impact of hospitalization on oral health: a systematic review. J Clin Periodontol 2011; Apr 7. [Epub ahead of print]
Rights and permissions
About this article
Cite this article
Sjögren, P. Hospitalisation associated with a deterioration in oral health. Evid Based Dent 12, 48 (2011). https://doi.org/10.1038/sj.ebd.6400793
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.ebd.6400793
This article is cited by
-
Oral Management in Rehabilitation Medicine: Oral Frailty, Oral Sarcopenia, and Hospital-Associated Oral Problems
The journal of nutrition, health & aging (2020)