Abstract
Objective:
To compare the characteristics of infants born at 22 weeks gestational age (GA) who were resuscitated at birth with those of infants who were not resuscitated.
Study Design:
We reviewed records of all the infants with a GA of 22 0/7 through 22 6/7 weeks who were born alive at William Beaumont Hospital from 1990 through 2009. Deliveries were attended by a neonatologist if they were in the hospital at the time of delivery or requested by the obstetrician and otherwise were attended by a pediatric resident or neonatal nurse practitioner.
Result:
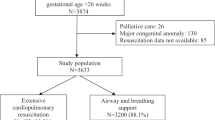
There were 85 infants born alive at 22 weeks GA during the study period. Thirty-six were intubated in the delivery room and defined as having been resuscitated. Two of them survived. On multivariate analysis, a higher birth weight (odds ratio 2.39 per 100 g increase, 95% confidence interval 1.21 to 4.73) and the presence of a neonatologist at delivery (odds ratio 6.72, 95% confidence interval 1.72 to 26.2) were each associated with an increased likelihood of resuscitation.
Conclusion:
Infants born at 22 weeks GA were more likely to be resuscitated if they were larger or if the delivery was attended by a neonatologist. We encourage neonatal groups to follow the recommendations of the American Academy of Pediatrics Committee on the Fetus and Newborn regarding initiation of resuscitation in these infants: inform parents that a good outcome is very unlikely and respect the parents’ choice of whether resuscitation should be initiated.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Iijma S, Arai H, Ozawa Y, Kawase Y, Uga N . Clinical patterns in extremely preterm (22 to 24 weeks of gestation) infants in relation to survival time and prognosis. Am J Perinatol 2009; 26: 399–406.
Nishida H, Sakuma I . Limit of viability in Japan: ethical consideration. J Perinat Med 2009; 37: 457–460.
Donohue PK, Boss RD, Shepard J, Graham E, Allen MC . Intervention at the border of viability: perspective over a decade. Arch Pediatr Adolesc Med 2009; 163: 902–906.
Stoll BJ, Hansen NI, Bell EF, Shankaran S, Laptook AR, Walsh MC et al. Neonatal outcomes of extremely preterm infants from the NICHD neonatal research network. Pediatrics 2010; 126: 443–456.
Itabashi K, Horiuchi T, Kusuda S, Kabe K, Itani Y, Nakamura T et al. Mortality rates for extremely low birth weight infants born in Japan in 2006. Pediatrics 2009; 123: 445–450.
The EXPRESS Group. One-year survival of extremely preterm infants after active perinatal care in Sweden. JAMA 2009; 301: 2225–2233.
Riley K, Roth S, Selwood M, Wyatt JJ . Survival and neurodevelopmental morbidity at 1 year of age following extremely preterm delivery over a 20-year period: a single centre cohort study. Acta Pediatrica 2008; 97: 159–165.
Tyson JE, Parikh NA, Langer J, Green C, Higgins RD . Intensive care for extreme prematurity – moving beyond gestational age. N Engl J Med 2008; 358: 1672–1681.
Peerzada JM, Richardson DK, Burns JP . Delivery room decision-making at the threshold of viability. J Pediatr 2004; 145: 492–498.
Peerzada JM, Schollin J, Hakansson S . Delivery room decision-making for extremely preterm infants in Sweden. Pediatrics 2006; 117: 1988–1995.
Bell EF . Noninitiation or withdrawal of intensive care for high-risk newborns. Pediatrics 2007; 119: 401–403.
Batton DG . Clinical report- antenatal counseling regarding resuscitation at an extremely low gestational age. Pediatrics 2009; 124: 422–427.
Mercurio MR . Physicians refusal to resuscitate at borderline gestational age. J Perinatol 2005; 25: 685–689.
American Academy of Pediatrics, Committee on Fetus and Newborn. Levels of neonatal care. Pediatrics 2004; 114: 1341–1347.
Papille LA, Burstein J, Burstein R, Koffler H . Incidence and evolution of subependymal and intraventricular hemorrhage: a study of infants with birth weights less than 1500 grams. J Pediatr 1978; 92: 529–534.
Committee for the Classification of Retinopathy of Prematurity. An international classification of retinopathy of prematurity. Arch Ophthalmol 1984; 102: 1130–1134.
Singh J, Fanaroff J, Andrews B, Caldarelli L, Lagatta J, Plesha-Troyke S et al. Resuscitation in the ‘gray zone’ of viability: determining physician preferences and predicting infant outcomes. Pediatrics 2007; 120: 519–526.
Meadow W . 500 gram infants – and 800-pound gorillas – in the delivery room. Pediatrics 2006; 117: 2276.
Hadlock FP, Harrist RB, Martinez-Poyer J . In utero analysis of fetal growth: a sonographic weight standard. Radiology 1991; 181: 129–133.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Holtrop, P., Swails, T., Riggs, T. et al. Resuscitation of infants born at 22 weeks gestation: a 20-year retrospective. J Perinatol 33, 222–225 (2013). https://doi.org/10.1038/jp.2012.88
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jp.2012.88
Keywords
This article is cited by
-
Outcomes following a comprehensive versus a selective approach for infants born at 22 weeks of gestation
Journal of Perinatology (2019)
-
Frameworks are pretty on paper but often do not fit reality: Reply to Lemyre et al.
Journal of Perinatology (2016)
-
Perinatal factors associated with active intensive treatment at the border of viability: a population-based study
Journal of Perinatology (2015)