Abstract
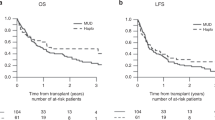
Allogeneic transplantation is successful in a minority of patients with primary refractory acute leukemia (PRAL). An HLA-matched sibling donor (MSD) is available only in 30–40% of the patients, whereas a partially mismatched related donor (PMRD) is available for most. We compared the outcome of 24 MSD (median age 24 years) and 19 PMRD (median age 34 years; P = 0.04) allograft recipients with PRAL. All MSD patients received non-T cell-depleted marrow whereas all PMRD patients received partially T cell-depleted marrow. All evaluable PMRD patients and 90% of the evaluable MSD patients attained CR. Six patients in each group with recurrent/persistent disease died. Ten PMRD (3-year probability 70%) and 14 MSD (3-year probability 63%) patients died of treatment-related causes. At the last follow-up, three PMRD (18–50 months; 3-year probability 14%) and four MSD (20–166 months; 3-year probability 20%) patients were alive and well. We conclude that allogeneic transplantation is a viable therapeutic option for PRAL. PMRD transplantation is a reasonable alternative in patients with no MSD, and results in similar outcome. In terms of identifying a donor and harvesting cells, a PMRD transplant is significantly quicker than an unrelated donor transplant – a point of great practical importance in the setting of failed induction chemotherapy where time is of the essence.
Bone Marrow Transplantation (2002) 29, 291–295. doi:10.1038/sj.bmt.1703373
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Linker CA, Levitt LJ, O'Donnell M et al. Treatment of adult acute lymphoblastic leukemia with intensive cyclical chemotherapy: a follow-up report Blood 1991 78: 2814 2822
Wiernik PH, Banks PL, Case DCJ et al. Cytarabine plus idarubicin or daunorubicin as induction and consolidation therapy for previously untreated adult patients with acute myeloid leukemia Blood 1992 79: 313 319
Hann IM, Stevens RF, Goldstone AH et al. Randomized comparison of DAT versus ADE as induction chemotherapy in children and younger adults with acute myeloid leukemia. Results of the Medical Research Council's 10th AML trial (MRC AML10) Blood 1997 89: 2311 2318
Mehta J, Powles R, Treleaven J et al. The impact of karyotype on remission rates in adult patients with de novo acute myeloid leukemia receiving high-dose cytarabine-based induction chemotherapy Leuk Lymphoma 1999 34: 553 560
Grever MR . Treatment of patients with acute nonlymphocytic leukemia not in remission Semin Oncol 1987 14: 416 424
Powles R, Treleaven J, Singhal S et al. Total therapy of acute myeloid leukemia: 7-year follow-up Blood 1997 90 (Suppl. 1): 227a
Zander AR, Dicke KA, Keating M et al. Allogeneic bone marrow transplantation for acute leukemia refractory to induction chemotherapy Cancer 1985 56: 1374 1379
Forman SJ, Schmidt GM, Nademanee AP et al. Allogeneic bone marrow transplantation as therapy for primary induction failure for patients with acute leukemia J Clin Oncol 1991 9: 1570 1574
Biggs JC, Horowitz MM, Gale RP et al. Bone marrow transplants may cure patients with acute leukemia never achieving remission with chemotherapy Blood 1992 80: 1090 1093
Mehta J, Powles R, Horton C et al. Bone marrow transplantation for primary refractory acute leukaemia Bone Marrow Transplant 1994 14: 415 418
Chiang KY, van Rhee F, Godder K et al. Allogeneic bone marrow transplantation from partially mismatched related donors as therapy for primary induction failure acute myeloid leukemia Bone Marrow Transplant 2001 27: 507 510
Mehta J . Graft-versus-leukemia reactions in clinical bone marrow transplantation Leuk Lymphoma 1993 10: 427 432
Henslee-Downey PJ, Abhyankar SH, Parrish RS et al. Use of partially mismatched related donors extends access to allo-geneic marrow transplant Blood 1997 89: 3864 3872
Mehta J, Singhal S, Chiang KY et al. Haploidentical BMT for acute leukemia: single-center experience of 220 patients Blood 2000 96 (Suppl. 1): 840a
Lee C, Brouillette M, Lamb L et al. Use of a closed system for Vαβ-positive T cell depletion of marrow for use in partially mismatched related donor (PMRD) transplantation Prog Clin Biol Res 1994 389: 523 532
Powles R, Mehta J, Kulkarni S et al. Allogeneic blood and bone-marrow stem-cell transplantation in haematological malignant diseases: a randomised trial Lancet 2000 355: 1231 1237
Singhal S, Powles R, Treleaven J et al. A low CD34+ cell dose results in higher mortality and poorer survival after blood or marrow stem cell transplantation from HLA-identical siblings: should 2 × 106 CD34+ cells/kg be considered the minimum threshold? Bone Marrow Transplant 2000 26: 489 496
Henslee-Downey PJ, Parrish RS, MacDonald JS et al. Combined in vitro and in vivo T lymphocyte depletion for the control of graft-versus-host disease following haploidentical marrow transplant Transplantation 1996 61: 738 745
Aversa F, Tabilio A, Velardi A et al. Treatment of high-risk acute leukemia with T-cell-depleted stem cells from related donors with one fully mismatched HLA haplotype New Engl J Med 1998 339: 1186 1193
Henslee-Downey PJ . Allogeneic related partially mismatched transplantation In: Barrett J, Treleaven JG (eds) The Clinical Practice of Stem Cell Transplantation Isis Medical Media: Oxford 1998 pp 392 417
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Singhal, S., Powles, R., Henslee-Downey, P. et al. Allogeneic transplantation from HLA-matched sibling or partially HLA-mismatched related donors for primary refractory acute leukemia. Bone Marrow Transplant 29, 291–295 (2002). https://doi.org/10.1038/sj.bmt.1703373
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.bmt.1703373
Keywords
This article is cited by
-
Thiotepa and antithymocyte globulin-based conditioning prior to haploidentical transplantation with posttransplant cyclophosphamide in high-risk hematological malignancies
Bone Marrow Transplantation (2020)
-
Clinical outcome of FLAG-IDA chemotherapy sequential with Flu–Bu3 conditioning regimen in patients with refractory AML: a parallel study from Shanghai Institute of Hematology and Institut Paoli-Calmettes
Bone Marrow Transplantation (2019)
-
Fludarabine-treosulfan compared to thiotepa-busulfan-fludarabine or FLAMSA as conditioning regimen for patients with primary refractory or relapsed acute myeloid leukemia: a study from the Acute Leukemia Working Party of the European Society for Blood and Marrow Transplantation (EBMT)
Journal of Hematology & Oncology (2019)
-
Prevention of relapse using granulocyte CSF-primed PBPCs following HLA-mismatched/haploidentical, T-cell-replete hematopoietic SCT in patients with advanced-stage acute leukemia: a retrospective risk-factor analysis
Bone Marrow Transplantation (2012)
-
Improved outcome in relapsed and refractory myeloid malignancies for unrelated vs related donor allogeneic peripheral blood-derived hematopoietic cell transplantation
Bone Marrow Transplantation (2010)