Key Points
-
Discusses the success rates of conventional local anaesthetic techniques when applied to the acutely inflamed pulp.
-
Outlines a staged approach that helps increase success rates of attaining pulpal anaesthesia in the acutely inflamed mandibular molar.
-
Discusses key variables (ie solutions, techniques, volume etc) that influence anaesthetic efficacy.
Abstract
Achieving profound pulpal anaesthesia in a mandibular molar diagnosed with irreversible pulpitis can be argued to be the most testing of dental anaesthetic challenges. Following discussion on the possible reasons for this occurrence in part 1, part 2 outlines the various local anaesthetic techniques that practitioners can use to overcome the acutely inflamed mandibular molar. They should then be able to apply these same principles to help anaesthetise any other tooth presenting with an acutely inflamed pulp. Techniques are discussed in detail along with key variables that have been associated with having an impact on the anaesthetic efficacy. This is to bring to light factors that can aid anaesthetic success as well as dispel common misnomers.
Similar content being viewed by others
Introduction
Difficulties in effectively anaesthetising an acutely inflamed mandibular molar (AIMM) are well documented. Conventional local anaesthetic techniques have shown to be unpredictable and sometimes ineffective, with success rates ranging between 20-50%.1,2,3,4,5,6 Part 1 outlined the clinical presentation and pathophysiology of an acutely inflamed pulp (AIP), defined what it meant to achieve pulpal anaesthesia and critically analysed theories as to why these teeth are more difficult to anaesthetise than their healthy counterparts. This section expands upon this by reviewing literature and drawing upon anecdotal experiences to outline a staged approach for attaining clinically acceptable pulpal anaesthesia in the AIMM (Fig. 1). Practitioners should then be able to apply these same principles to anaesthetising any other tooth presenting with an AIP.
Step one
a) Inferior alveolar nerve block with lingual block
As the first point of anaesthesia, an inferior alveolar nerve block (IANB) should be administered as infiltration techniques alone do not provide a sufficient degree of anaesthesia.7,8 This dental block technique is the commonest, but arguably, the most difficult and it anaesthetises tissues receiving sensory innervation from the inferior alveolar nerve (IAN). These are ipsilateral to the side of administration and include all mandibular teeth up to the midline, the buccal mucosa anterior to the first molar, and the skin and mucosa of the lower lip and chin (Fig. 2).9
Technique
1. Outline anatomical landmarks
Use the thumb to intra-orally palpate the deepest portion of the coronoid notch on the external oblique ridge (EOR). Simultaneously, place the index finger extra-orally in the indentation above the angle of the mandible. The maximum concavity of the coronoid notch corresponds to the height of the mandibular foramen and the distance between digits indicates its anteroposterior position.9 From this position, slide the thumb medially to palpate the internal oblique ridge (IOR) keeping a mental note of its position. Then slide it back to the coronoid notch on the EOR, stretching tissues taut and exposing the pterygomandibular depression (Fig. 3).
2. Insert needle
Direct the barrel across the occlusal plane of the contralateral premolars and insert a 27 gauge long needle into the mucosa medial to the IOR and lateral to the pterygomandibular raphe (Fig. 4). The height should coincide with the midpoint of the thumb and the anteroposterior distance slightly more than half way posteriorly between the digits.9 After advancing 20-25 mm, the needle should contact mandibular bone behind the lingula and above the mandibular foramen. Premature contact warrants repositioning and similarly, if the needle is placed too far posteriorly repositioning is advised to avoid inducing transient facial nerve palsy.
3. Aspirate syringe
Aspirate after withdrawing a few millimetres and if positive (that is, blood is seen entering into syringe) the needle must be repositioned and re-aspirated until a negative result is attained.
4. Deposit anaesthetic solution
When the needle is at the correct depth, height and there is no blood on aspiration, the anaesthetic should be deposited over the course of 30–60 seconds into the pterygomandibular space. Continuing to inject and straightening the needle on withdrawal to make it parallel to the medial aspect of the ramus, will anaesthetise the lingual nerve which runs anterior and parallel to the IAN (Fig. 5).9 This results in further anaesthesia to the lingual mucosa, anterior two-thirds of the tongue and the floor of mouth.9
Key variables
• Anaesthetic solution
Numerous clinical trials have failed to demonstrate any clinical superiority in efficacy of articaine 4%, prilocaine 4% or mepivocaine 3% preparations, in healthy and AIMMs, over lidocaine 2% preparations when administered via an IANB.1,10,11,12 However, despite the controversy surrounding the safety of 4% anaesthetic solutions (that is, articaine 4% and prilocaine 4%), there is no conclusive scientific evidence to support that they exhibit any more neurotoxicity than lidocaine 2%.13,14 Therefore although safe, their use over lidocaine 2% would provide no clinical advantage for the IANB technique.14 Research has yet to detail the impact of different vasoconstrictor concentrations on IANB success rates.
• Volume
A recent systematic review, containing 319 patients, concluded there was no significant difference in success when administering 1.8 ml or 3.6 ml of lidocaine 2% to AIMMs.15 Neither provided an acceptable degree of pulpal anaesthesia, therefore, repeat injections would provide no benefit.15
• Technique
The limited evidence comparing the anaesthetic efficacy of alternative techniques, such as Gow-Gates and Vazirani-Akinosi techniques, on AIMMs have demonstrated that although they may provide marginally higher success rates over the conventional method, clinically acceptable rates of pulpal anaesthesia are still not achieved.16,17,18 For further details on these techniques please refer to Netter's head and neck anatomy for dentistry.9
• Mandibular foramen position
The commonest position of the mandibular foramen has been reported to be within the third quadrant of the ramus in both anterior-posterior and superior-inferior planes.19,20,21,22 This location is more posterior-inferiorly in children and more superior-anteriorly in the elderly, indicating the respective changes in the entry point of the needle.9,22 Furthermore, an oral panoramic radiograph can be used to determine this position in patients that may have an atypical foramen location.23
• Speed of administration
Studies have demonstrated IANBs lasting 60 seconds are more comfortable and have higher success rates in healthy mandibular molars when compared to those lasting 15 seconds.24 However, for AIMMs, the literature is conflicting as it suggests slow administration has no impact, but is still more comfortable.25
Summary
• Administer an IANB.
• Continue injecting on withdrawal for lingual block.
• Use lidocaine 2% anaesthetic with vasoconstrictor.
• Deposit 1.8 ml over 60 seconds.
• Repeat IANB if soft tissue anaesthesia has not been achieved – no lip numbness.
• When completed, proceed to administer a LBI.
b) Long buccal infiltration
Due to the poor success of conventional techniques, the long buccal infiltration (LBI) is recommended to supplement all IANBs to improve success rates from 20-50%, to 60-70%.1,2,3,4,5,6,10,26,27 It is relatively quick and simple and anaesthetises tissues receiving sensory innervation from the long buccal branch of the mandibular division of the trigeminal nerve.9 This includes the mandibular molars, skin of the cheek and the buccal muco-periosteum adjacent to the mandibular molars (Fig. 6).9 These tissues are not anaesthetised from an IANB.
Technique
1. Outline anatomical landmarks
Using a mirror, retract the cheek so the buccal mucosa adjacent to the molars is at 90 degrees to the mandible. This will keep the tissues taught and give a clear view of the mandibular molars and muco-buccal fold (Fig. 7).
2. Insert seedle
Insert a 2 gauge long needle into the mucosa at 45 degrees to the buccal cortical plate. The entry point should be below the muco-buccal fold and distal to the apices of the second mandibular molar at a depth of 2-4 mm in which bone should be contacted (Fig. 8). The use of topical anaesthetic before insertion is advised.
3. Aspirate syringe
Withdraw and aspirate and if blood is seen entering into the syringe, reposition needle and re-aspirate until negative results are attained.
4. Deposit anaesthetic solution
When at the correct site and there is no blood upon aspiration, inject 1-1.8 ml into the tissues. By depositing solution in this position, the long buccal nerve is anaesthetised as it crosses the anterior border of the mandibular ramus.9
Key variables
• Anaesthetic solution
In contrast to an IANB, clinical trials have demonstrated higher success rates of articaine 4% preparations (58-71%) over lidocaine 2% preparations (29-47%), when administering through a LBI to AIMMs.2,10,26,27 There is very little research that assesses the impact of varying vasoconstrictor concentrations on success rate.
• Volume
A recent randomised controlled trial found there was no statistically significant difference in the success rates between 1.8 ml and 3.6 ml of articaine 4% + adrenaline 1:100,000, suggesting increasing the volume past 1.8 ml would not improve success.28
• Lingual infiltration
One may consider a lingual infiltration, in addition to the long buccal infiltration, to improve the success rates of pulpal anaesthesia. However, clinical trials have failed to demonstrate any clinical advantage that this technique may provide over a solitary LBI following a failed IANB.2,29
Summary
-
Administer LBI with all IANBs.
-
Use articaine 4% anaesthetic with vasoconstrictor
-
Deposit 1-1.8 ml over 10-20 seconds
-
Objectively test the pulp and neighbouring teeth as outlined in part 1 and proceed cautiously if negative response attained
-
Repeat LBI if soft tissue anaesthesia has not been achieved – no pain on probing.
-
Proceed to next stage if presenting symptoms persist despite presence of soft tissue anaesthesia.
Step two
Intra-ligamentary injection
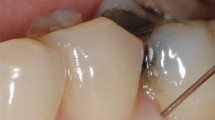
After a failed LBI, it is recommended that the intra-ligamentary injection (ILI) is the next supplemental technique that should be employed in the absence of an intra-osseous injection (IOI) kit. The overall success rate for endodontic procedures in AIMMs ranges between 56-96%.4,30,31,32 The technique itself is simple and requires a small volume of anaesthetic to produce rapid single tooth anaesthesia (Fig. 9). However, one must warn patients of the postoperative discomfort that can arise.33
Although the name suggests the solution is distributed across the periodontal ligament, it is in fact forced laterally intraosseusly into the bone marrow spaces, via cribiform plate, and systemically into the vasculature around the tooth.34,35 Conventional and high pressure syringes or computer controlled delivery systems (CCDS) are all modes of delivering an ILI.
Technique
1. Outline anatomical landmarks
Retract cheek so the buccal mucosa adjacent to the molars, is at almost 90 degrees to the mandible. This gives better access to the gingival sulcus of the mandibular molars.
2. Insert needle
Gently insert the tip of a 27 gauge short needle into the gingival sulcus of the mandibular molar at approximately 30 degrees. It should be then slowly advanced along the root surface using light hand pressure until resistance is met at the base of the sulcus. The mesial and distal points are recommended as the points of administration and should be approached buccally. Additionally, the buccal furcation is also recommended as it is easily accessible and permits the anaesthetic to diffuse more readily into the bone marrow spaces, via the inter-radicular septum, where the cortical bone is thin and porous.
3. Deposit anaesthetic solution
Administer 0.2 ml over a period of 10-20 seconds ensuring a high degree of back pressure is felt being careful not to shatter the glass cartridge. This pressure, along with soft tissue blanching, indicates the needle tip is in the correct position (Fig. 10).36,37,38 If solution flows readily into the patient's mouth, the needle should be repositioned until this resistance is felt.
Key variables
• Anaesthetic solution
The limited evidence available suggests no statistical superiority of mepivacaine 3%, prilocaine 3% and articaine 4% over lidocaine 2% preparations.39,40,41 However the use of solutions containing vasoconstrictors does appear to be a significant factor in gaining success.41,42
• Re-injection
Cohen et al. reported success of 74% on initial administration and 96% on reinjection for AIMMs, whereas Walton and Abbott found this to be 63% and 72% respectively in healthy mandibular molars.4,36,39 Therefore, if the initial ILI fails to achieve clinically acceptable anaesthesia, then a repeat injection is warranted.
• Mode of delivery
Clinical trials have yet to demonstrate any advantage of CCDS over conventional or high pressure syringes. The 56% success rate obtained by Nusstein et al. is comparable, and in some cases significantly lower, to that achieved in parallel studies that utilised conventional or high pressure syringes.4,32,36,38,43,44,45,46 Furthermore, there is conflicting evidence relating to the comfort of CCDS.45,47,48
• Type of tooth
Mandibular posterior teeth receive the greatest benefit from this technique, whereas the incisors obtain the least with success reported to be as low as 18%.31,33,49 Out of the posterior teeth, Jing et al. suggested it is the second molar that is significantly more likely to achieve pulpal anaesthesia following an ILI.31
Summary
-
Administer an ILI following a failed IANB and LBI
-
Use adrenaline containing anaesthetic solutions if not medically contraindicated
-
Deposit 0.2 ml over 20 seconds under back pressure mesially, distally and into buccal furcation
-
CCDS can be used but are not essential
-
Objectively test the pulp and neighbouring teeth as outlined in Part 1 and proceed cautiously if negative response attained
-
Repeat ILI if the initial administration fails
-
Proceed to next stage if presenting symptoms persist despite administration of repeated ILIs.
Intra-osseous injection
Although technically more difficult, the IOI is by far the most effective and predictable supplemental technique for anaesthetising AIMMs, with reports of success ranging between 80-100%.3,50,51,52,53,54,55,56,57,58 Specialised delivery systems (Stabident™ [Fairfax Dental Inc., Miami, FL] and X-tip™ [Dentsply, Tulsa, OK]) perforate the cortical plate adjacent to the tooth, allowing administration of anaesthetic directly into cancellous bone. It then bathes the periradicular region to rapidly induce profound pulpal anaesthesia (Fig. 9).
Verma et al. found 95% of patients experienced little to no discomfort on perforation.55 Reitz et al. reported an 11-16% incidence of moderate pain after soft tissue anaesthesia wore off.59 And in the 5% of sites that exhibited post injection swelling, complete resolution occurred over the course of several weeks.60,61
Technique
1. Preparation
Prior to perforation, disinfect the mucosa with chlorohexidine to minimise risk of secondary infections. Then infiltrate 0.1 ml of local anaesthetic into the attached gingiva at the site of perforation if not already anaesthetised (Fig. 11).
2. Identify site of perforation
Using the pre-operative radiograph, evaluate root proximity and the site of perforation. This should be distal to the tooth in question, with an exception of second molars where a mesial site is adequate, and 2-4 mm apical to the alveolar crest in the attached gingiva where the buccal cortical bone is approximately 3-4 mm thick.59,60,61,62,63,64,65,66,67
3. Perforate cortical plate
Connect the perforating component to the slow hand piece and orientate the tip 90° to the site of perforation. Apply light pressure and activate in a series of two second bursts to prevent overheating of the bone to reduce the risk of post-operative swelling. A characteristic give should be felt after four to five seconds indicating penetration through the cortical plate and into the cancellous bone (Fig. 12). If this sensation is not felt after five seconds, select another penetration site.
4. Deposit anaesthetic solution
Guide a 27 gauge ultra-short needle, via conventional syringe, into the perforation site (Fig. 13). Finally, administer between 0.9-1.8ml over a three to four minute period to ensure patient comfort and reduced tachycardia.57 Flow of anaesthetic into the cancellous bone is important for success and if seen flowing back out into the mouth, perforation into another site should be considered.51
Key variables
• Anaesthetic solution
Studies show no difference in anaesthetic efficacy between lidocaine 2%, articaine 4% preparations and different adrenaline concentrations when administered to AIMMs.51,52,53,54,55,56,57 However, mepivacaine 3% is an effective substitute for patients with cardiovascular diseases and long acting anaesthetics (bupivicaine) should be avoided due to their cardio-toxic potential.50,52,57,62,68,69
• Re-injection
Jensen et al. demonstrated that administering a second IOI 30 minutes after the first, which produced 100% success, prolonged effectiveness and duration of pulpal anaesthesia by 15 minutes.70 Additional studies have documented further increases in anaesthetic efficacy after the second IOI in AIMMs.50
• Mode of delivery
To date, the StabidentTM and X-TipTM systems have become the most popular and most researched IO techniques. Unfortunately, there are no direct comparative studies when applied to AIMMs, however, parallel studies conclude similar success rates.3,51,52,53,54,55,56,57,66,67,71
Summary
-
Administer IOI following failed IANB, LBI and/or repeated ILIs if equipment available
-
Use lidocaine 2% anaesthetic with vasoconstrictor
-
Use mepivocaine 3% plain in patients with cardiovascular diseases and avoid bupivicaine
-
Deposit 0.9-1.8 ml over three to four minutes ensuring no backflow of solution into oral cavity
-
StabidentTM and X-tipTM have similar efficacy, however, localising the perforation site is easier with X-tipTM
-
Objectively test the pulp and neighbouring teeth as outlined in part 1 and proceed cautiously if negative response attained
-
Repeat IOI if initial administration fails or wears off
-
Proceed to next stage if presenting symptoms persist despite repeated IOIs.
Step Three
Intra-pulpal injection
Unfortunately, there are some patients that do not achieve adequate pulpal anaesthesia even after administering a combination of supplemental techniques. For these cases an intra-pulpal injection (IPI) is indicated and conventional methods dictate the anaesthesia to be deposited, via conventional syringe, into a small opening in the pulp chamber, that is the, pulp horn (Fig. 14). A high degree of back pressure is required to induce immediate onset and the patient should be pre-emptively warned of the short-lasting moderate to severe pain they will experience upon administration.72,73
However, the conventional IPI technique may not always allow for the anaesthesia to spread throughout the entire pulp. For example, it can be difficult to gain the necessary back pressure when there is persistent bleeding from a hyperaemic pulp or an unintentionally large access cavity. Therefore, despite comfortable removal of coronal pulp tissue, extirpation of the radicular pulp can be a painful process. To counteract this, a variation of the conventional IPI technique has been developed and used by the restorative team at the Leeds Dental Institute and is described below.
Technique
1. Stabilise coronal tooth structure
Administer a conventional IPI and under rubber dam, stabilise the coronal portion of the tooth by conservatively removing all soft caries and failed restorations without involving the pulp.
2. Access pulp and achieve haemostasis
Using a high speed cooled bur, de-roof the pulp chamber so that all pulp horns and undercuts are removed. If this is too painful then administer another IPI and incrementally de-roof the pulp until completely removed. Curette the coronal pulp and then use a local anaesthetic soaked cotton wool pledge (CWP) or other haemostatic agents, such as Racellet® pellets or aluminium chloride to achieve haemostasis. Sodium hypochlorite may also be used.
3. Deposit solution and create bung
Following haemostasis, use a conventional syringe to deposit anaesthetic into the canal orifices and the pulp chamber under back pressure, flooding it to half full (Fig. 15). Then use a packing instrument to condense a small ball of warm thermoplastic gutta-percha (GP) or silicone putty into the pulp chamber for an intimate adaption to the pulpal floor (Fig. 16). GP is the preferred method as it is easily adaptable, sets quickly, and can be easily adjusted and subsequently removed. A thermoplastic backfilling gun (that is, ObturaTM) is ideal, but multiple heated conventional GP cones may also be used.
4. Use bung
When condensed, the bung should be left in the pulp chamber for 60 seconds before its removal (Fig. 17). This produces the necessary pressure to force the solution down into the root canal system creating immediate and profound anaesthesia, particularly in the radicular pulp. The bung can be placed back into the pulp chamber if the anaesthesia wears off during treatment, removing the need to remove the rubber dam.
Summary
-
Administer an IPI when all supplemental techniques fail
-
For conventional IPIs, adequate backpressure into a small opening is required
-
When using the bung, ensure complete removal of the pulp chamber roof and achieve adequate haemostasis before anaesthetic deposition.
Conclusion
The basic strategy proposed above is one of many that aim to help practitioners approach the AIMM in a more predictable manner. These principles are not exclusive to the mandibular molars and they can be applied to all teeth diagnosed with acute irreversible pulpitis. An underlying understanding of the aetiology, combined with an awareness of the various supplemental techniques, will help practitioners overcome most cases of failed anaesthesia.
References
Claffey E, Reader A, Nusstein J, Beck M, Weaver J . Anaesthetic efficacy of articaine for inferior alveolar nerve blocks in patients with irreversible pulpitis. J Endod 2004; 30: 568–571.
Aggarwal V, Jain A, Kabi D . Anaesthetic efficacy of supplemental buccal and lingual infiltrations of articaine and lidocaine after an inferior alveolar nerve block in patients with irreversible pulpitis. J Endod 2009; 35: 925–929.
Nusstein J, Reader A, Nist R, Beck M, Meyers W J . Anaesthetic efficacy of the supplemental intraosseous injection of 2% lidocaine with 1:100,000 epiniphrine in irreversible pulpitis. J Endod 1998; 24: 487–491.
Cohen H, Cha B, Spångberg L S . Endodontic anaesthesia in mandibular molars: a clinical study. J Endod 1993; 19: 370–373.
Kennedy S, Reader A, Nusstein J, Beck M, Weaver J . The significance of needle deflection in success of the inferior alveolar nerve block in patients with irreversible pulpitis. J Endod 2003; 29: 630–633.
Reisman D, Reader A, Nist R, Beck M, Weaver J . Anaesthetic efficacy of the supplemental intraosseous injection of 3% mepivacaine in irreversible pulpitis. Oral Surg Oral Med, Oral Pathol Oral Radiol Endod 1997; 84: 676–682.
Abdulwahab M, Boynes S, Moore P, Seifikar S, Al-Jazzaf A, Alshuraidah A, et al. The efficacy of six local anaesthetic formulations used for posterior mandibular buccal infiltration anaesthesia. J Am Dent Assoc. 2009; 140: 1018–1024.
Monteiro M R, Groppo F C, Haiter-Neto F, Volpato M C, Almeida JF . 4% articaine buccal infiltration versus 2% lidocaine inferior alveolar nerve block for emergency root canal treatment in mandibular molars with irreversible pulpits: a randomized clinical study. Int Endod J 2015; 48: 145–152.
Norton N S, Netter F H . Netter's head and neck anatomy for dentistry. Philadelphia: Saunders Elsevier, 2007.
Ashraf H, Kazem M, Dianat O, Noghrehkar F . Efficacy of articaine versus lidocaine in block and infiltration anaesthesia administered in teeth with irreversible pulpitis: a prospective, randomized, double-blind study. J Endod 2013; 39: 6–10.
Mikesell P, Nusstein J, Reader A, Beck M, Weaver J . A comparison of articaine and lidocaine for inferior alveolar nerve blocks. J Endod 2005; 31: 265–270.
Kambalimath D H, Dolas R S, Kambalimath H V, Agrawal S M . Efficacy of 4 % articaine and 2 % lidocaine: a clinical study. J Maxillofac Oral Surg. 2013; 12: 3–10.
Garisto G A, Gaffen A S, Lawrence H P, Tenenbaum H C, Haas D A . Occurrence of paresthesia after dental local anaesthetic administration in the United States. J Am Dent Assoc. 2010; 141: 836–844.
Yapp K E, Hopcraft M S, Parashos P . Articaine: a review of the literature. Br Dent J. 2011; 210: 323–329.
Fowler S, Reader A . Is a Volume of 3.6 mL Better than 1.8 mL for Inferior Alveolar Nerve Blocks in Patients with Symptomatic Irreversible Pulpitis? J Endod; 39: 970–972.
Click V, Drum M, Reader A, Nusstein J, Beck M . Evaluation of the Gow-Gates and Vazirani-Akinosi techniques in patients with symptomatic irreversible pulpitis: a prospective randomized study. J Endod 2014; 41: 16–21.
Aggarwal V, Singla M, Kabi D . Comparative evaluation of anaesthetic efficacy of Gow-Gates mandibular conduction anaesthesia, Vazirani-Akinosi technique, buccalpluslingual infiltrations, and conventional inferior alveolar nerve anaesthesia in patients with irreversible pulpitis. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2010; 109: 303–308.
Goldberg S, Reader A, Drum M, Nusstein J, Beck M . Comparison of the anaesthetic efficacy of the conventional inferior alveolar, Gow-Gates, and Vazirani-Akinosi techniques. J Endod. 2008; 34: 1306–1311.
Ennes J P, Medeiros R M . Localization of mandibular foramen and clinical implications. Int J Morphol 2009; 27: 1305–1311.
Hayward J, Richardson E R, Malhotra S K . The mandibular foramen: Its anteroposterior position. Oral Surg, Oral Med Oral Pathol 1977; 44: 837–843.
Hetson G, Share J, Frommer J, Kronman J H . Statistical evaluation of the position of the mandibular foramen. Oral Surg, Oral Med Oral Pathol 1988; 65: 32–34.
Hwang T J, Hsu S C, Huang Q F, Guo M K . Age changes in location of mandibular foramen. Zhonghua Ya Yi Xue Hui Za Zhi, 1990; 9: 98–103.
Dharmar S . Locating the mandibular canal in panoramic radiographs. Int J Oral Maxillofac Implants 1997; 12: 113–117.
Kanaa M D, Meechan J G, Corbett I P, Whitworth J M . Speed of injection influences efficacy of inferior alveolar nerve blocks: A double-blind randomized controlled trial in volunteers. J Endod 2006; 32: 919–923.
Aggarwal V, Singla M, Miglani S, Kohli S, Irfan M . A prospective, randomized single-blind evaluation of effect of injection speed on anaesthetic efficacy of inferior alveolar nerve block in patients with symptomatic irreversible pulpitis. J Endod 2012; 38: 1578–1580.
Rogers B S, Botero T M, McDonald N J, Gardner R J, Peters M C . Efficacy of articaine versus lidocaine as a supplemental buccal infiltration in mandibular molars with irreversible pulpitis: a prospective, randomized, double-blind study. J Endod 2014; 40: 753–758.
Matthews R, Drum M, Reader A, Nusstein J, Beck M . Articaine for supplemental buccal mandibular infiltration anaesthesia in patients with irreversible pulpitis when the inferior alveolar nerve block fails. J Endod 2009; 35: 343–346.
Singla M, Subbiya A, Aggarwal V, Vivekanandhan P et al. Comparison of the anaesthetic efficacy of different volumes of 4% articaine (1.8 and 3.6 mL) as supplemental buccal infiltration after failed inferior alveolar nerve block. Int Endod J 2015; 48: 103–108.
Dou L, Luo J, Yang D . Anaesthetic efficacy of supplemental lingual infiltration of mandibular molars after inferior alveolar nerve block plus buccal infiltration in patients with irreversible pulpitis. Int Endod J 2013; 46: 660–665.
Zarei M, Ghoddusi J, Sharifi E, Forghani M, Afkhami F, Marouzi P . Comparison of the anaesthetic efficacy of and heart rate changes after periodontal ligament or intraosseous XTip injection in mandibular molars: a randomized controlled clinical trial. Int Endod J 2012; 45: 921–926.
Jing Q, Wan K, Wang X J, Ma L . Effectiveness and safety of computer-controlled periodontal ligament injection system in endodontic access to the mandibular posterior teeth. Chin Med Sci J 2014; 29: 23–27.
Nusstein J, Claffey E, Reader A, Beck M, Weaver J . Anaesthetic effectiveness of the supplemental intraligamentary injection, administered with a computer-controlled local anaesthetic delivery system, in patients with irreversible pulpitis. J Endod 2005; 31: 354–358.
White J J, Reader A, Beck M, Meyers W J . The periodontal ligament injection: A comparison of the efficacy in human maxillary and mandibular teeth. J Endod 1988; 14: 508–514.
Walton R E . Distribution of solutions with the periodontal ligament injection: clinical, anatomical, and histological evidence. J Endod 1986; 12: 492–500.
Smith G N, Walton R E . Periodontal ligament injection: distribution of injected solutions. Oral Surg, Oral Med & Oral Pathol 1983; 55: 232–238.
Walton R E, Abbott B J . Periodontal ligament injection: a clinical evaluation. J Am Dent Assoc 1981; 103: 571–575.
Smith G N, Walton R E, Abbott B J . Clinical evaluation of periodontal ligament anaesthesia using a pressure syringe. J Am Dent Assoc 1983; 107: 953–956.
Kaufman E, Galili D, Garfunkel A A . Intraligamentary anaesthesia: a clinical study, J Prosth Dent 1983; 49: 337–339.
Grey RJ, Lomax A M, Rood J P . Periodontal ligament injection: alternative solutions. Anesth Prog 1990; 37: 293–295.
Berlin J, Nusstein J, Reader A, Beck M, Weaver J . Efficacy of articaine and lidocaine in a primary intraligamentary injection administered with a computer-controlled local anaesthetic delivery system. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2005; 99: 361–366.
Schleder J R, Reader A, Beck M, Meyers W J . The periodontal ligament injection: A comparison of 2% lidocaine, 3% mepivacaine, and 1:100,000 epiniphrine to 2% lidocaine with 1:100,000 epiniphrine in human mandibular premolars. J Endod 1988; 14: 397–404.
Grey R J, Lomax A M, Rood J P . Periodontal ligament injection: with or without a vasoconstrictor? Br Dent J 1987; 162: 263–265.
Parirokh M, Sadr S, Nakhaee N, Abbott PV, Askarifard S . Efficacy of supplementary buccal infiltrations and intraligamentary injections to inferior alveolar nerve blocks in mandibular first molars with asymptomatic irreversible pulpitis: a randomized controlled trial. Int Endod J 2014; 47: 926–933.
Berlin J, Nusstein J, Reader A, Beck M, Weaver J . Efficacy of articaine and lidocaine in a primary intraligamentary injection administered with a computer-controlled local anaesthetic delivery system. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2005; 99: 361–366.
Kämmerer P W, Schiegnitz E, von Haussen T, B et al. Clinical efficacy of a computerised device (STA™) and a pressure syringe (VarioJect INTRA™) for intraligamentary anaesthesia. Euro J Dent Ed 2015; 19: 16–22.
Malamed S F . The periodontal ligament (PDL) injection: an alternative to inferioralveolar nerve block. Oral Surg Oral Med Oral Pathol 1982; 53: 117–121.
Rosenberg ES . A computer-controlled anaesthetic delivery system in a periodontal practice: patient satisfaction and acceptance. J Esth Rest Dent 2002; 14: 39–46.
Grace E G, Barnes D M, Reid B C, Flores M, George D L . Computerized local dental anaesthetic systems: patient and dentist satisfaction. J Dent 2003; 31: 9–12.
Meechan J G, Ledvinka J I . Pulpal anaesthesia for mandibular central incisor teeth: a comparison of infiltration and intraligamentary injections. Int Endod J 2002; 35: 629–634.
Reader A, Nist R, Beck M, Weaver J . Anaesthetic efficacy of the supplemental intraosseous injection of 3% mepivacaine in irreversible pulpitis. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 1997; 84: 676–682.
Nusstein J, Kennedy S, Reader A, Beck M, Weaver J . Anaesthetic efficacy of the supplemental Xtip intraosseous injection in patients with irreversible pulpitis. J Endod 2003; 29: 724–728.
Bigby J, Reader A, Nusstein J, Beck M, Weaver J . Articaine for supplemental intraosseous anaesthesia in patients with irreversible pulpitis. J Endod 2006; 32: 1044–1047.
Parente S A, Anderson R W, Herman W W, Kimbrough W F, Weller R N . Anaesthetic efficacy of the supplemental intraosseous injection for teeth with irreversible pulpitis. J Endod 1998; 24: 826–828.
Bhuyan A C, Latha S S, Jain S, Kataki R . Anaesthetic efficacy of the supplemental Xtip intraosseous injection using 4% articaine with 1:100,000 adrenaline in patients with irreversible pulpitis: An in vivo study. J Con Dent 2014; 17: 522–525.
Verma P K, Srivastava R, Ramesh K M . Anaesthetic efficacy of Xtip intraosseous injection using 2% lidocaine with 1:80,000 epiniphrine in patients with irreversible pulpitis after inferior alveolar nerve block: a clinical study. J Con Dent 2013; 16: 162–166.
Pereira L A, Groppo F C, Bergamaschi Cde C, et al. Articaine (4%) with epiniphrine (1:100,000 or 1:200,000) in intraosseous injections in symptomatic irreversible pulpitis of mandibular molars: anaesthetic efficacy and cardiovascular effects. Oral Surg Oral Med Oral Pathol Oral Radiol 2013; 116: 85–91.
Zarei M, Ghoddusi J, Sharifi E, Forghani M, Afkhami F, Marouzi P . Comparison of the anaesthetic efficacy of and heart rate changes after periodontal ligament or intraosseous X-Tip injection in mandibular molars: a randomized controlled clinical trial. Int Endod J 2012; 45: 921–926.
Kanaa M D, Whitworth J M, Meechan J G . A prospective randomized trial of different supplementary local anaesthetic techniques after failure of inferior alveolar nerve block in patients with irreversible pulpitis in mandibular teeth. J Endod 2012 38: 421–425.
Reitz J, Reader A, Nist R, Beck M, Meyers WJ . Anaesthetic efficacy of a repeated intraosseous injection given 30 min following an inferior alveolar nerve block/intraosseous injection. Anesth Prog 1998; 45: 143–149.
Coggins R, Reader A, Nist R, Beck M, Meyers W J . Anaesthetic efficacy of the intraosseous injection in maxillary and mandibular teeth. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 1996; 81: 634–641.
Dunbar D, Reader A, Nist R, Beck M, Meyers W J . Anaesthetic efficacy of the intraosseous injection after an inferior alveolar nerve block. J Endod 1996; 22: 481–486.
Gallatin E, Stabile P, Reader A, Nist R, Beck M . Anaesthetic efficacy and heart rate effects of the intraosseous injection of 3% mepivacaine after an inferior alveolar nerve block. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2000; 89: 83–87.
Talaat W M, Al-Bayatti S W, Dohair D E, Zobeidi M A, Hannouneh KM . A CBCT measurement of the mandibular buccal bone thickness in dentate adults. Oral Surg 2015; 8: 38–41.
Leong D J, Li J, Moreno I, Wang H L . Distance between external cortical bone and mandibular canal for harvesting ramus graft: a human cadaver study. J Perio 2010; 81: 239–243.
Al-Jandan B A, Al-Sulaiman A A, Marei H F, Syed F A, Almana M . Thickness of buccal bone in the mandible and its clinical significance in mono-cortical screws placement. A CBCT analysis. Int J Oral Maxillofac Surg 2013; 42: 77–81.
Razavian H, Kazemi S, Khazaei S, Jahromi M Z . Xtip intraosseous injection system as a primary anaesthesia for irreversible pulpitis of posterior mandibular teeth: A randomized clinical trial. Dent Res J 2013; 10: 210–213.
Guglielmo A, Reader A, Nist R, Beck M, Weaver J . Anaesthetic efficacy and heart rate effects of the supplemental intraosseous injection of 2% mepivacaine with 1:20,000 levonordefrin. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 1999; 87: 284–293.
Bacsik C, Swift J, Hargreaves K . Toxic systemic reactions of bupivacaine and etidocaine. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 1995; 79: 18–23.
Hull T, Rothwell B . Intraosseous anaesthesia comparing lidocaine and etidocaine. J Dent Res 1998; 77: 197.
Jensen J, Nusstein J, Drum M, Reader A, Beck M . Anaesthetic efficacy of a repeated intraosseous injection following a primary intraosseous injection. J Endod 2008; 34: 126–130.
Gallatin J, Reader A, Nusstein J, Beck M, Weaver J . A comparison of two intraosseous anaesthetic techniques in mandibular posterior teeth. J Am Dent Assoc 2003; 134: 1476–1484.
Birchfield J, Rosenberg P A . Role of the anaesthetic solution in intrapulpal anaesthesia. J Endod 1975; 1: 26–27.
VanGheluwe J, Walton R . Intrapulpal injection—factors related to effectiveness. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 1997; 18: 38–40.
Acknowledgements
I owe sincere and earnest thankfulness to staff members in the Restorative Department of the Leeds Dental Institute for their inspirational guidance and support throughout this project. Furthermore, I am truly indebted and thankful to Mr Collin Sullivan (Clinical Photographer at Leeds Dental Institute) and the Leeds Dental Institute Medical and Dental Illustrative Department for the detailed clinical photographs and illustrations depicted in both parts of this series. Finally, I would like to express my warm thanks to my friends and family who have supported me with their encouraging words.
Author information
Authors and Affiliations
Corresponding author
Additional information
Refereed Paper
Rights and permissions
About this article
Cite this article
Virdee, S., Bhakta, S. & Seymour, D. Effective anaesthesia of the acutely inflamed pulp: part 2. Clinical strategies. Br Dent J 219, 439–445 (2015). https://doi.org/10.1038/sj.bdj.2015.843
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.bdj.2015.843