Abstract
Bone marrow-derived cells exert anti-inflammatory actions and can migrate into the brain. However, their role in the development of neurogenic hypertension remains unclear. A hyperactive renin–angiotensin system and inflammation in the brain are mechanisms that contribute to angiotensin II-initiated neurogenic hypertension. We hypothesized that bone marrow-derived cells in the brain attenuate the overactive brain renin–angiotensin system and inflammation, thereby reducing neurogenic hypertension. We cultured plastic-adherent bone marrow-derived cells for 3 weeks. Seven days after initiation of vehicle or angiotensin II infusions, the rats underwent intracerebroventricular administration of either serum-free medium or autologous bone marrow-derived cells (106 cells). After 23 days of infusion, the mean arterial pressure was recorded, and the sympathetic tone was evaluated. Rats infused with angiotensin II demonstrated significant increases in the resting mean arterial pressure and the peak depressor response to ganglionic blockade (vehicle vs. angiotensin II infusion, 119 ± 4 vs. 178 ± 6 mmHg and −34 ± 6 vs. −74 ± 5 mmHg, respectively). Intracerebroventricularly administered bone marrow-derived cells attenuated the angiotensin II-mediated increases in the resting mean arterial pressure and peak depressor response (142 ± 11 and −52 ± 4 mmHg, respectively). The cells also reduced the angiotensin II-induced increases in angiotensin II type 1 receptor and transforming growth factor-β expression in the brain. In conclusion, bone marrow-derived cells in the brain may have a protective role against the development of angiotensin II-induced neurogenic hypertension by modulating angiotensin II type 1 receptor expression and inflammatory processes.
Similar content being viewed by others
Introduction
The central nervous system is a blood pressure control system that regulates sympathetic and parasympathetic nerve activity and releases hormones that control cardiac output and vascular resistance. An increase in sympathetic nerve activity and altered arterial baroreflex functions are associated with human primary hypertension as well as various animal models of hypertension [1]. Despite recent advances in therapeutic strategies targeting the various mechanisms of hypertension, regulation of these mechanisms in the brain remains unclear. Thus, a novel approach to neurogenic hypertension is needed.
Long-term infusion of subpressor doses of angiotensin II (Ang II) gradually induces hypertension [2]. A central mechanism was implicated in this slow pressor Ang II-induced hypertension [3,4,5]. Recent studies have suggested that activation of the brain renin–angiotensin system (RAS) and inflammation of the cardiovascular regulatory areas in the brain are important mechanisms involved in the development of neurogenic hypertension [4, 5]. Furthermore, the importance of T cell [6] and microglial [7] activation, which is related to brain inflammation, was reported to be essential for the development of neurogenic hypertension. Therefore, regulation of these mechanisms is a critical approach for controlling Ang II-induced neurogenic hypertension.
Bone marrow is a known source of circulating self-repairing cells [8, 9]. Tissue reconstruction and repair by bone marrow-derived cells have been reported in the brain. Postmortem assessments of leukemia patients who received sex-mismatched bone marrow transplantation revealed the presence of transgender neurons, astrocytes, and microglia [10]. Intravenously administered bone marrow-derived cells preferentially localized to the ipsilateral ischemic hemisphere and improved functional recovery after stroke in rats [11]. Furthermore, these cells have been clinically used for cell therapy in cardiovascular diseases, such as severe ischemic limb [12] and severe embolic stroke [13]. The anti-inflammatory and endothelial repair properties of the cells activate the microvasculature circulation, which has been suggested to improve ischemia [14].
Although bone marrow-derived cells can migrate into the brain [10], express an RAS modulatory enzyme [15], and secrete paracrine factors to promote anti-inflammation, the role of bone marrow-derived cells in the brain during the development of neurogenic hypertension has not been well elucidated. The abilities of bone marrow-derived cells, coupled with the importance of an overactive brain RAS and inflammation in the development of neurogenic hypertension, led us to hypothesize that an increase in the number of bone marrow-derived cells in the brain would attenuate Ang II-induced overactivation of these processes and reduce neurogenic hypertension. Our observations demonstrated that bone marrow-derived cells in the brain modulate the pathophysiological processes involved in the development of Ang II-induced neurogenic hypertension.
Methods
Animals
Five-week-old male Sprague–Dawley rats were purchased from Japan SLC Inc. (Hamamatsu-shi, Shizuoka, Japan) and housed in standard rodent cages with standard laboratory chow and tap water available ad libitum. The rats were kept in a room, maintained at a constant temperature (24 ± 2 °C) and humidity (55 ± 10%) with a 12-h light period between 08:00 and 20:00 h. The rats were given at least 1 week to acclimate to the environment after their arrival. The experimental protocol was approved by the Animal Care and Use Committee at the University of the Ryukyus. The details of the methods and the general protocol for animal experiments are provided in online supplementary information.
Bone marrow aspiration, cell culture, and labeling
The rats (200–230 g) were anesthetized with an intraperitoneal injection of 50 mg/kg sodium pentobarbital. The bilateral iliac crests of the rats were punctured with a 21-gauge needle and bone marrow was aspirated with a heparinized syringe to collect a total volume of 0.5 mL. A red blood cell lysis solution (1.5 mL; QIAGEN Sciences, Germantown, MD, USA) was added to the aspirated bone marrow, and filtered and phosphate-buffered saline (PBS)-washed cells were seeded in individual dishes of Dulbecco’s Modified Eagle’s Media (DMEM) with 10% fetal bovine serum and 2% penicillin/streptomycin, followed by incubation in a humidified incubator (5% CO2 at 37 °C) for 3 weeks. Prior to intracerebroventricular (icv) injection, the cells were collected and labeled with DiI (v-22885; Molecular Probes, Eugene, OR, USA) according to the manufacturer’s protocol. The number of cells was adjusted to 1 × 106 cells per 20 µL of serum-free medium for icv injection. The descending thoracic aorta of different sets of rats was obtained, and the aortic endothelial cells were cultured in a gelatin-coated culture dish.
Characterization of bone marrow-derived cells
Immunocytochemistry
Bone marrow-derived cells were immunostained with anti-CD29 (04-1109; Merck Millipore, Temecula, CA, USA) and anti-interleukin-10 (IL-10; ab9969, Abcam, Cambridge, MA, USA).
Western blotting
Western blotting was performed using previously described methods [16]. Cultured bone marrow-derived cells and rat aortic endothelial cells were collected and subjected to a protein isolation protocol. The proteins transferred onto polyvinylidene difluoride (PVDF) membranes were probed with antibodies against angiotensin-converting enzyme (ACE) (sc-12187; Santa Cruz Biotechnology, Dallas, TX, USA) and angiotensin-converting enzyme 2 (ACE2) (sc-20998; Santa Cruz Biotechnology).
BrdU uptake assay
Cultured cells secrete paracrine factors into the culture medium. We collected the conditioned media and applied it to serum-starved endothelial cells to examine cell proliferation. We assumed that an ability to influence endothelial cell proliferation is one of the paracrine effects of bone marrow-derived cells. Endothelial cell proliferation was examined by measuring BrdU incorporation during DNA synthesis using a colorimetric immunoassay kit (Roche; Mannheim, Germany). Fetal bovine serum (0.5%) was used as the control stimulant for endothelial cell proliferation.
Flow cytometric analysis
Flow cytometric analysis was performed with bone marrow-derived cells cultured for 3 weeks at the third passage. CD29 was used as a positive marker, and CD34 was used as a negative marker for rat mesenchymal stem cells.
Angiotensin II infusions
Two weeks after bone marrow aspiration, the rats were anesthetized with sodium pentobarbital. A small incision was made in the skin behind the neck, and the subcutaneous tissue was spread toward the interscapular space to create a pocket for an osmotic minipump (2004; Alzet, Cupertino, CA, USA), which was filled with either saline as a vehicle or Ang II (A9525; Sigma-Aldrich, St. Louis, MO, USA). The concentration of Ang II was adjusted to an infusion rate of 150 ng/kg/min for 4 weeks.
Intracerebroventricular injections
Intracerebroventricular injection of bone marrow-derived cells
The icv injections were performed using previously described methods [17]. One week after initiation of the infusions, the rats were anesthetized with sodium pentobarbital and placed on a stereotaxic frame in the prone position. The skin overlying the midline of the skull was incised, and a small hole was drilled into the dorsal surface of the cranium 0.8 mm posterior to Bregma and 1.5 mm lateral to the midline. The tip of a Hamilton syringe (10 µL) was advanced 4 mm vertically from the skull surface and either DiI-labeled autologous bone marrow-derived cells (1 × 106 cells/20 µL) or serum-free medium (20 µL) was injected bilaterally into the lateral ventricles over a 20-min injection time. Therefore, the cells were bilaterally implanted into the cerebrospinal fluid (CSF)-filled lateral ventricles. The following four groups were created: rats that received vehicle infusion with icv administration of medium (n = 7), rats that received vehicle infusion with icv administration of bone marrow-derived cells (n = 4), rats that received Ang II infusion with icv administration of medium (n = 5), and rats that received Ang II infusion with icv administration of bone marrow-derived cells (n = 6). The mortality rate of the rats during the experiment was 9%, which was not attributed to any particular experimental group.
Acute icv injection of Ang II
Different sets of rats (n = 15) were used to examine the pressor response to acute icv injection of Ang II (20 ng/2 µL of artificial CSF). Five rats received vehicle infusion and 10 rats received Ang II infusion (150 ng/kg/min) through an osmotic minipump (2002; Alzet). Five days after initiation of the infusions, the rats subjected to vehicle infusion received icv injection of medium and the rats subjected to Ang II infusion received icv injection of either medium or bone marrow-derived cells (106 cells). Twelve days after initiation of the infusions, the rats were anesthetized and underwent surgery to implant an arterial catheter and a guide cannula for icv injection [17] and were then allowed to recover for 48 h. Fourteen days after initiation of the infusions, acute icv injection of Ang II was performed in conscious, unrestrained rats.
Blood pressure measurements and acute ganglionic blockade
Before and during the first 3 weeks of infusion, body weight, and systolic blood pressure (SBP) were measured twice a week. SBP was measured by the tail-cuff method using a non-preheating, non-invasive blood pressure monitor (Model MK-2000; Muromachi Kikai Co., Ltd., Tokyo, Japan).
Three weeks after initiation of the infusions, the rats underwent surgery to implant arterial and venous catheters. After a 48-h recovery period, the rats were placed in an 18-cm-diameter plastic bowl and allowed to move freely. Arterial pressure was recorded using the Power Lab System (ML750; ADI Instruments, Castle Hill, Australia). The resting arterial pressure and heart rate (HR) were recorded for at least 30 min in conscious, unrestrained rats. After recording the resting blood pressure, 40 mg/kg of hexamethonium, a ganglionic blocker, was administered intravenously to examine the resting sympathetic tone. The effect of acute ganglionic blockade on blood pressure was monitored, and the degree of the peak depressor response was measured to evaluate the resting sympathetic tone.
Western blot analysis of the rat brain
Proteins were isolated from rat hypothalamus and brainstem samples using a standard protocol. The proteins transferred onto PVDF membranes were probed with antibodies against Ang II type 1 receptor (AT1, sc-31181; Santa Cruz Biotechnology, Dallas, TX, USA), Ang II type 2 receptor (AT2, sc48452, Santa Cruz Biotechnology), ACE (sc-12187; Santa Cruz Biotechnology), transforming growth factor β (TGF-β) (ab66043; Abcam), and IL-10 (ab9969; Abcam).
Histological examination
The fixation and immunostaining procedures used in this study have been described previously [18]. The DiI-labeled bone marrow-derived cells administered via icv injection were identified by red fluorescence. Some sections were immunostained with antibodies against IL-10 (ab9969; Abcam), ACE2 (sc-20998; Santa Cruz Biotechnology), or CD29 (04-1109; Merck Millipore).
Statistical analysis
The values are expressed as the mean ± SEM. Comparisons between the experimental groups were performed using ANOVA or Student’s t-test. P < 0.05 was considered statistically significant.
Results
Characteristics of cultured bone marrow-derived cells
Figure 1a shows a phase-contrast microscopic image of cultured bone marrow-derived cells. Spindle-shaped, plastic-adherent, and colony-forming bone marrow-derived cells were observed. The cells proliferated to >106 cells within 3 weeks in ~60% of the bone marrow samples. The cells expressed CD29 (Fig. 1b), a marker of mesenchymal stem cells, and IL-10 (Fig. 1c), an anti-inflammatory cytokine. Both CD29 and IL-10 had similar distribution patterns in the cytoplasm, mainly in the perinuclear area, with a slightly higher density at the edge of the cells. Figure 1d, e shows the western blotting of protein bands for the modulatory enzymes of RAS, ACE, and ACE2 in the bone marrow-derived cells. Quantification of these bands revealed that ACE expression was 0.13-times lower and ACE2 expression was 2.42-times higher in bone marrow-derived cells compared with the corresponding levels in endothelial cells. Furthermore, the paracrine effect of bone marrow-derived cells was examined using an endothelial cell proliferation assay with conditioned media from bone marrow-derived cells (Fig. 1f). The endothelial cell proliferation assay showed 1.52-times greater BrdU uptake with conditioned media from bone marrow-derived cells than that with media from endothelial cells, suggesting that bone marrow-derived cells secrete more endothelial cell proliferation factors than the endothelial cells themselves. Flow cytometric analysis was performed with bone marrow-derived cells cultured for 3 weeks at the third passage. Figure 1g depicts a representative plot of the flow cytometric analysis. Approximately 40% of the bone marrow-derived cells were CD29-positive and CD34-negative, which we considered mesenchymal stem cells.
Characteristics of cultured bone marrow-derived cells. a Phase-contrast microscopic image of bone marrow-derived cells. The scale bar denotes 100 µm. b Immunoreactivity of CD29. A negative control image is shown in the left upper corner. The scale bar denotes 20 µm. c Immunoreactivity of interleukin-10 (IL-10). A negative control image is shown in the left upper corner. The scale bar denotes 20 µm. d Western blotting of angiotensin-converting enzyme (ACE) from endothelial cells and bone marrow-derived cells and quantification of the protein bands. The data are shown as the mean ± SEM, n = 4 each, *p < 0.01 vs. endothelial cells. e Western blotting of angiotensin-converting enzyme 2 (ACE2) from endothelial cells and bone marrow-derived cells and quantification of the protein bands. The data are shown as the mean ± SEM, n = 4 each, *p < 0.01 vs. endothelial cells. f BrdU uptake assay in endothelial cells. The conditioned media from bone marrow-derived cells, which contain paracrine factors, were collected and the effect of the media on endothelial cell proliferation was examined by measuring BrdU incorporation during DNA synthesis. FBS (0.5%) was used as a control. The data are shown as the mean ± SEM, n = 4–12 each, *p < 0.01 vs. endothelial cells. g A representative plot from the flow cytometric analysis. The bone marrow-derived cells that were CD29-positive and CD34-negative were considered mesenchymal stem cells. EC rat aortic endothelial cells; BMC bone marrow-derived cells; FBS fetal bovine serum
Effects of icv administration of bone marrow-derived cells on angiotensin II-induced neurogenic hypertension
To determine whether an increase in the number of bone marrow-derived cells in the brain attenuates Ang II-induced neurogenic hypertension, we administered autologous bone marrow-derived cells to Ang II-infused rats and monitored their blood pressure. Figure 2 shows the effects of bone marrow-derived cells on the resting mean arterial pressure (MAP) (Fig. 2a) and resting sympathetic tone (Fig. 2b) in Ang II-infused rats. In vehicle-infused rats, icv administration of bone marrow-derived cells did not affect the resting MAP or the peak depressor response to ganglionic blockade. The rats that received Ang II infusion for 23 days and icv injection of serum-free medium had a significantly higher resting MAP (178 ± 6 mmHg) and a larger depressor response to ganglionic blockade (−74 ± 5 mmHg) compared with the rats that received vehicle infusion and icv injection of serum-free medium (119 ± 4 and −34 ± 6 mmHg, respectively). The bone marrow-derived cells significantly attenuated both the Ang II-mediated increase in the resting MAP and the increase in the peak depressor response (142 ± 11 and −52 ± 4 mmHg, respectively, p < 0.05). The time-dependent changes in body weight gain (Supplementary Fig. 2A), SBP (Supplementary Fig. 2B), resting HR (Supplementary Fig. 3A), and the MAP after ganglionic blockade (Supplementary Fig. 3B) did not differ between the rats that received either saline infusions or icv administration. Only the rats that received Ang II infusions with serum-free medium icv injection showed a trend toward increasing SBP (Supplementary Fig. 2B).
The resting arterial pressure and depressor response to acute ganglionic blockade in conscious rats. a Representative traces of arterial pressure (top panel) and the resting mean arterial pressure (MAP) of each group of rats (lower panel). Angiotensin II (Ang II) infusion significantly increased the resting MAP in the rats that received intracerebroventricular (icv) injection of serum-free medium. Icv administration of bone marrow-derived cells attenuated the Ang II-mediated increase in the resting MAP. The scale bar in the top panel denotes 3 min. b Representative traces of arterial pressure changes in response to acute ganglionic blockade (top panel) and the peak depressor responses of each group of rats (lower panel). Ang II infusion significantly increased the peak depressor response to acute ganglionic blockade. Icv administration of bone marrow-derived cells attenuated the increase in the depressor response. The scale bar in the top panel denotes 1 min. The numbers in parentheses indicate the number of rats tested; *p < 0.05 vs. the other group, two-way ANOVA followed by Tukey’s honestly significant difference (HSD) test
Distribution and morphology of icv-implanted bone marrow-derived cells in the brain
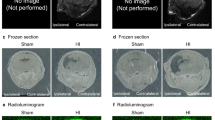
Figure 3a shows a low-magnification photo of a forebrain section containing the subfornical organ, lateral ventricle with the choroid plexus, and dorsal third ventricle. A schematic illustration of Fig. 3a is shown in Fig. 3b. DiI-positive cells were detected 4 weeks after icv administration of DiI-labeled bone marrow-derived cells. DiI-positive cells (red fluorescence) were distributed throughout the choroid plexus both on the surface of the ventricles and in the subventricular zone. DiI-positive cells were not detected in the subfornical organ (Fig. 3a) or other cardiovascular regulatory areas, such as the hypothalamic paraventricular nucleus (Supplementary Fig. 4A), the rostral ventrolateral medulla (Supplementary Fig. 4B), the area postrema, or the nucleus tractus solitarius (Supplementary Fig. 4C). Higher magnification of the choroid plexus area revealed that the DiI-positive cells (white arrows in Fig. 3c–h) located on the apical side of the epithelial cells of the choroid plexus, exhibited an oval shape, were smaller than surrounding epithelial cells and expressed IL-10 (3D), ACE2 (3F), and CD29 (3H). An IL-10-positive cell without DiI staining (red arrow head in Fig. 3d) was observed on the basal side of the epithelial cells near the DiI-positive cells.
Distribution and morphology of icv-implanted bone marrow-derived cells in the forebrain. a A coronal brain section containing the subfornical organ, lateral ventricle with the choroid plexus, and dorsal third ventricle of a rat that received icv administration of DiI-labeled autologous bone marrow-derived cells. DiI-positive cells (red fluorescence) were distributed along the choroid plexus, the surface of the ventricle, and in the subventricular zone. DiI-positive cells were not detected in the subfornical organ. Sections were counterstained with 4ʹ,6-diamidino-2-phenylindole (DAPI) (blue fluorescence). The scale bar denotes 1 mm. b Schematic illustration of a. Chp choroid plexus; CPu caudate putamen; D3V dorsal third ventricle; LV lateral ventricle; SFO subfornical organ; vhc ventral hippocampal commissure. c, d Higher magnification of the choroid plexus area with a DiI-positive cell (c) with IL-10 staining (d, green fluorescence). e, f The choroid plexus area with a DiI-positive cell (e) with ACE2 staining (f). g, h The choroid plexus area with a DiI-positive cell (g) with CD29 staining (h). The DiI-positive cells (white arrows) on the apical side of the epithelial cells had a round shape and were smaller than the surrounding epithelial cells, which were large, cuboidal-lining cells. A non-DiI-positive IL-10-expressing cell (red arrow head in d) was observed on the basal side of the epithelial cells and located near the DiI-positive cell. The scale bar denotes 30 µm in c–h
Expression of RAS components and inflammation-related cytokines in the brains of Ang II-infused rats
To determine whether bone marrow-derived cells modulated the brain RAS and inflammation, we examined the expression of RAS components and inflammation-related cytokines in the brains of Ang II-infused rats. Figure 4 shows the western blotting results of RAS components and inflammation-related cytokines in the hypothalamus and brainstem of Ang II-infused rats. The rats that received Ang II infusions and icv injection of serum-free medium showed significantly higher AT1 receptor and TGF-β expression (2.35-times and 2.46-times, respectively) compared with the rats that received vehicle infusions and icv injection of serum-free medium. Icv administration of bone marrow-derived cells attenuated the Ang II-mediated increases in ATI receptor and TGF-β expression. Ang II infusions with or without icv administration of bone marrow-derived cells did not affect the expression levels of the AT2 receptor, ACE, or IL-10 in the brain.
Expression of renin–angiotensin system (RAS) components and inflammation-related cytokines in the brains of Ang II-infused rats. a, b, c Representative western blots of RAS components and quantification of the protein bands. Ang II infusion significantly increased the expression of angiotensin II type 1 receptors (AT1Rs) in the brain. Icv administration of bone marrow-derived cells attenuated this increased expression. Ang II infusion with or without icv administration of bone marrow-derived cells did not affect the expression of angiotensin II type 2 receptors (AT2Rs) or ACE. d, e Representative western blots of inflammation-related cytokines and quantification of the protein bands. Ang II infusion significantly increased the expression of transforming growth factor β (TGF-β). Icv administration of bone marrow-derived cells attenuated this increased expression. Ang II infusion with or without icv administration of bone marrow-derived cells did not affect IL-10 expression. The data are presented as the mean ± SEM, n = 4 each; *p < 0.05 vs. the other group
Pressor response to acute icv injection of Ang II in conscious Ang II-infused rats
To examine augmentation of the brain RAS on blood pressure regulation in Ang II-infused rats, we performed acute icv injection of 20 ng of Ang II to evoke a pressor response in this animal model. Figure 5 shows the resting MAP levels and a change in these levels after acute icv injection of ANG II in Ang II-infused rats. Fourteen days after the infusions, the resting MAP did not differ between the rats that received either infusions or icv administration. The pressor response to acute icv injection of Ang II was significantly greater in the rats that received Ang II infusion with icv injection of medium (23 ± 2 mmHg) compared with the rats that received vehicle infusion with icv injection of medium (15 ± 1 mmHg). Icv administration of bone marrow-derived cells attenuated the enhanced pressor response to acute icv injection of Ang II (18 ± 2 mmHg) (Fig. 5b).
Resting MAP levels and changes in the MAP after acute icv injection of ANG II in conscious Ang II-infused rats. a Resting MAP levels before acute icv injection of Ang II. No significant difference was identified in the resting MAP between the rats subjected to either 14 days of Ang II infusions or icv injection of bone marrow-derived cells. b Changes in the MAP after acute icv injection of Ang II. Ang II infusion significantly enhanced the pressor response to acute icv injection of Ang II in the rats that received icv injection of medium. Icv administration of bone marrow-derived cells attenuated the enhanced pressor response to acute icv injection of Ang II. The data are presented as the mean ± SEM. *p < 0.05 vs. the vehicle-medium icv group. The numbers in parentheses indicate the number of rats tested. One-way ANOVA followed by Tukey’s HSD test
Discussion
In this study, we provided evidence that icv administration of autologous bone marrow-derived cells attenuated Ang II-induced sympathetic overactivation and increased blood pressure. The icv-implanted cells expressed ACE2 and IL-10 and reduced the Ang II-induced increases in AT1 receptor and TGF-β expression in the brain. These results suggest that icv-implanted bone marrow-derived cells have a protective role against the development of Ang II-induced neurogenic hypertension by modulating an overactive brain RAS and inflammatory processes.
Studies have suggested that a hyperactive brain RAS [19], neuroinflammation [20, 21] and vascular inflammation in the brain [22] are involved in the development of Ang II-induced neurogenic hypertension. In our current study, Ang II-infused rats exhibited increased AT1 receptor expression in the hypothalamus and brainstem (Fig. 4a). The pressor response to acute icv injection of Ang II was enhanced in the Ang II-infused rats before significant elevation of the resting blood pressure (Fig. 5). These observations support those of the previous studies [4, 5, 19] and suggest that a hyperactive brain RAS was present in our animal model. Icv administration of autologous bone marrow-derived cells attenuated Ang II-induced sympathetic overactivation and increased blood pressure in rats (Fig. 2) as well as the hyperactive brain RAS (Figs. 4, 5). A strategy that increases bone marrow-derived cells or enhances the activity of endogenous cells in the brain may have a preventive and therapeutic potential to control neurogenic hypertension.
Although, the mechanisms mediating attenuation of Ang II-induced changes are not fully understood, the RAS modulatory enzymes expressed in bone marrow-derived cells may play a role. We found that the expression patterns of ACE and ACE2 in the bone marrow-derived cells were very unique and that low levels of ACE and high levels of ACE2 were present in bone marrow-derived cells compared with those in endothelial cells (Fig. 1d, e). Cultured human mononuclear cells, a cell source used to treat severe ischemic limb [12], exhibited higher ACE2 protein expression than human umbilical vein endothelial cells (Supplementary Fig. 5). We and others have reported that overexpression of ACE2 improved the neurogenic components of hypertension [16, 18] by attenuating the hyperactive brain RAS [23] and inflammation [24], and these observations led us to speculate that bone marrow-derived cells may have negative RAS modulatory roles in local corresponding sites.
In the present study, the implanted cells were distributed in CSF-accessible sites, including the choroid plexus and subarachnoid space (Fig. 3a). However, cells were not found in the brain parenchyma, including cardiovascular regulatory areas. An important question that arises from this observation is how the implanted cells affect cardiovascular regulatory neurons. The morphology of DiI-labeled implanted cells showed a monocyte-like appearance and expressed IL-10 (Fig. 3d), ACE2 (Fig. 3f), and CD29 (Fig. 3h). These cells were clearly different from the surrounding cells, suggesting that implanted cells may retain characteristics similar to those observed in cultured bone marrow-derived cells (Fig. 1). Therefore, we propose that the implanted cells had at least partial mesenchymal stem cell-like characteristics and actions. The mesenchymal stem cell secretes various paracrine factors that promote immunomodulatory actions [8, 14]. For example, these cells were reported to boost differentiation of the M2 subtype of macrophages [25], which have an anti-inflammatory phenotype that reduces the release of proinflammatory cytokines. Immune surveillance cells in the CSF have crucial functions, including monitoring, influencing, and amplifying the communication between the peripheral and central nervous systems in the initiation of neuroinflammation as well as resolving inflammation [26]. Regarding Ang II-induced neurogenic hypertension, recent studies have indicated that both activated T cells in the periphery [6, 27] and microglial activation related to brain inflammation [7, 21] were essential for the development of this disease. However, little is known about the role of immune cells from the CSF in neurogenic hypertension. We propose that immune cells in the CSF, including perivascular macrophages, play an important role in the development of neurogenic hypertension. In the present study, we observed endogenous IL-10-positive cells (red arrow head in Fig. 3d) located on the basal side of the choroid plexus epithelium and near the DiI-positive implanted cells in the choroid plexus area. Therefore, we assume that the implanted bone marrow-derived cells affected endogenous immune cells in the CSF to reduce inflammatory stimulation of peripheral Ang II, which in turn attenuated Ang II-induced overactivation of the brain RAS and inflammation in the cardiovascular regulatory areas of the brain parenchyma. Further studies are needed to elucidate this proposed mechanism.
In the present study, the altered AT1 receptor and TGF-β protein expression in the brain (Fig. 4a, d) suggested that tissue-level inflammatory processes may be affected by Ang II infusion and administration of bone marrow-derived cells; however, we could not identify any difference in IL-10 protein expression in the tissues (Fig. 4e). IL-10 is an anti-inflammatory cytokine that affects several immune cells that trigger and amplify inflammatory stimulation in the brain. We believe that IL-10-expressing cells, including the injected bone marrow-derived cells, triggered anti-inflammatory processes and that IL-10 expression was diluted in the tissue to such a level that we were unable to detect any differences in the brain at the time of sampling, which was at the end of the experiment.
One of the limitations of this study was that we could not identify the type of main effector cell in our observations. The bone marrow-derived cells used in this study had similar characteristics to those described by Friedenstein et al. [28] who first developed the concept of mesenchymal stem cells as plastic-adherent, spindle-shaped, in vitro colony-forming cells. However, the flow cytometric analysis showed that ~40% of the cells used in the experiment were CD29-positive and CD34-negative; therefore, we considered them to be mesenchymal stem cells. Characterization of the cultured cells revealed that the bone marrow-derived cells used in the icv experiments expressed the RAS modulatory enzyme (ACE2) with active paracrine function, included mesenchymal stem cells and were not uniform cells (Fig. 1). Because of the heterogeneous nature of the cultured cells, we used term bone marrow-derived cells in the present study. Furthermore, use of single-cell clones or a purer mesenchymal stem cell population would be advantageous for identifying cell types; however, most available cells are allogeneic or xenogeneic cells. In the present study, we intended to use autologous cells to minimize the risk of adverse immunological reactions. Adipose derived-mesenchymal stem cells may be a purer stem cell population than the bone marrow-derived cells and may be used as a cell source for autologous transplantation in a future study. Although we could not identify the type of main effector cell, we believe that the bone marrow-derived cells, including mesenchymal stem cells, exerted some functions accounting for the observed beneficial effects.
In summary, we explored the role of bone marrow-derived cells in the brain in Ang II-induced neurogenic hypertension. Bone marrow-derived cells secrete various paracrine factors to promote anti-inflammation. These cells have therapeutic potential for various refractory diseases, including cardiovascular disease, and clinical applications have been explored. We demonstrated that icv administration of autologous bone marrow-derived cells attenuated sympathetic overactivation and increases in blood pressure. Understanding the role of bone marrow-derived cells in neurogenic hypertension will provide new insight into preventive and therapeutic strategies to control this prevalent disease. A drug or intervention that increases the number of self-repairing stem cells in the brain may serve as a preventive strategy against the development of hypertension, although further studies are needed to elucidate the role of bone marrow-derived cells in neurogenic hypertension.
References
Malpas SC. Sympathetic Nervous System Overactivity and its role in the development of cardiovascular disease. Physiol Rev. 2010;90:513–57.
Dickinson CJ, Lawrence JR. A slowly developing pressor response to small concentrations of angiotensin Its bearing on the pathogenesis of chronic renal hypertension. Lancet. 1963;1:1354–6.
Severs WB, Daniels-Severs AE. Effects of angiotensin on the central nervous system. Pharmacol Rev. 1973;25:415–49.
Veerasingham SJ, Raizada MK. Brain renin-angiotensin system dysfunction in hypertension: recent advances and perspectives. Br J Pharmacol. 2003;139:191–202.
Leenen FH. Actions of circulating angiotensin II and aldosterone in the brain contributing to hypertension. Am J Hypertens. 2014;27:1024–32.
McMaster WG, Kirabo A, Madhur MS, Harrison DG. Inflammation, immunity, and hypertensive end-organ damage. Circ Res. 2015;116:1022–33.
Shen XZ, Li Y, Li L, Shah KH, Bernstein KE, Lyden P, Shi P. Microglia participate in neurogenic regulation of hypertension. Hypertension. 2015;66:309–16.
Kuroda Y, Kitada M, Wakao S, Dezawa M. Bone marrow mesenchymal cells: how do they contribute to tissue repair and are they really stem cells? Arch Immunol Ther Exp. 2011;59:369–78.
Vahidy FS, Rahbar MH, Zhu H, Rowan PJ, Bambhroliya AB, Savitz SI. Systematic review and meta-analysis of bone marrow-derived mononuclear cells in animal models of ischemic stroke. Stroke. 2016;47:1632–9.
Cogle CR, Yachnis AT, Laywell ED, Zander DS, Wingard JR, Steindler DA, et al. Bone marrow transdifferentiation in brain after transplantation: a retrospective study. Lancet. 2004;363:1432–7.
Chen J, Li Y, Katakowski M, Chen X, Wang L, Lu D, et al. Intravenous bone marrow stromal cell therapy reduces apoptosis and promotes endogenous cell proliferation after stroke in female rat. J Neurosci Res. 2003;73:778–86.
Ishida A, Ohya Y, Sakuda H, Ohshiro K, Higashiuesato Y, Nakaema M, et al. Autologous peripheral blood mononuclear cell implantation for patients with peripheral arterial disease improves limb ischemia. Circ J. 2005;69:1260–5.
Taguchi A, Sakai C, Soma T, Kasahara Y, Stern DM, Kajimoto K, et al. Intravenous Autologous bone marrow mononuclear cell transplantation for stroke: phase1/2a clinical trial in a homogeneous group of stroke patients. Stem Cells Dev. 2015;24:2207–18.
Karantalis V, Hare JM. Use of mesenchymal stem cells for therapy of cardiac disease. Circ Res. 2015;116:1413–30.
Strawn WB, Richmond RS, Ann Tallant E, Gallagher PE, Ferrario CM. Renin-angiotensin system expression in rat bone marrow haematopoietic and stromal cells. Br J Haematol. 2004;126:120–6.
Yamazato M, Ferreira AJ, Yamazato Y, Diez-Freire C, Yuan L, Gillies R, et al. Gene transfer of angiotensin-converting enzyme 2 in the nucleus tractus solitarius improves baroreceptor heart rate reflex in spontaneously hypertensive rats. J Renin Angiotensin Aldosterone Syst. 2011;12:456–61.
Yamazato M, Ohya Y, Nakamoto M, Sakima A, Tagawa T, Harada Y, et al. Sympathetic hyperreactivity to air-jet stress in the chromosome 1 blood pressure quantitative trait locus congenic rats. Am J Physiol Regul Integr Comp Physiol. 2006;290:R709–R714.
Yamazato M, Yamazato Y, Sun C, Diez-Freire C, Raizada MK. Overexpression of angiotensin-converting enzyme 2 in the rostral ventrolateral medulla causes long-term decrease in blood pressure in the spontaneously hypertensive rats. Hypertension. 2007;49:926–31.
Xue B, Zhang Z, Johnson RF, Johnson AK. Sensitization of slow pressor angiotensin II (Ang II)-initiated hypertension: induction of sensitization by prior Ang II treatment. Hypertension. 2012;59:459–66.
Cardinale JP, Sriramula S, Mariappan N, Agarwal D, Francis J. Angiotensin II-induced hypertension is modulated by nuclear factor-κB in the paraventricular nucleus. Hypertension. 2012;59:113–21.
Shi P, Diez-Freire C, Jun JY, Qi Y, Katovich MJ, Li Q, et al. Brain microglial cytokines in neurogenic hypertension. Hypertension. 2010;56:297–303.
Biancardi VC, Son SJ, Ahmadi S, Filosa JA, Stern JE. Circulating angiotensin II gains access to the hypothalamus and brain stem during hypertension via breakdown of the blood-brain barrier. Hypertension. 2014;63:572–9.
Feng Y, Yue X, Xia H, Bindom SM, Hickman PJ, Filipeanu CM, et al. Angiotensin-converting enzyme 2 overexpression in the subfornical organ prevents the angiotensin II-mediated pressor and drinking responses and is associated with angiotensin II type 1 receptor downregulation. Circ Res. 2008;102:729–36.
Sriramula S, Xia H, Xu P, Lazartigues E. Brain-targeted angiotensin-converting enzyme 2 overexpression attenuates neurogenic hypertension by inhibiting cyclooxygenase-mediated inflammation. Hypertension. 2015;65:577–86.
Yamazato Y, Yamazato M, Ishida A, Fujita J, Ohya Y. Intratracheal administration of autologous bone marrow-derived cells ameliorates monocrotaline-induced pulmonary vessel remodeling and lung inflammation in rats. Lung. 2018;196:147–55.
Brendecke SM, Prinz M. Do not judge a cell by its cover--diversity of CNS resident, adjoining and infiltrating myeloid cells in inflammation. Semin Immunopathol. 2015;37:591–605.
Harrison DG. The immune system in hypertension. Trans Am Clin Climatol Assoc. 2014;125:130–8.
Friedenstein AJ, Piatetzky-Shapiro II, Petrakova KV. Osteogenesis in transplants of bone marrow cells. J Embryol Exp Morphol. 1966;16:381–90.
Acknowledgements
We thank Sakiko Hatoma, Morihiro Ota, and Masato Nohara for their excellent technical assistance.
Funding:
This work was supported by the Grants-in-Aid for Scientific Research from the Japan Society for the Promotion of Science (grant numbers 21591059 and 24591232).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Electronic supplementary material
Rights and permissions
About this article
Cite this article
Yamazato, M., Ishida, A., Yamazato, Y. et al. Intracerebroventricular administration of bone marrow-derived cells attenuates angiotensin II-initiated neurogenic hypertension in rats. Hypertens Res 41, 828–838 (2018). https://doi.org/10.1038/s41440-018-0088-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41440-018-0088-3