Abstract
Background
Glucocorticoids (GCs) are highly effective yet problematic agents against bronchopulmonary dysplasia (BPD). The dimeric trans-activation of GCs induces unfavorable effects, while monomeric trans-repression suppresses inflammation-related genes. Recently, non-steroidal-selective glucocorticoid-receptor agonists and modulators (SEGRAMs) with only the trans-repressive action have been designed.
Methods
Using a bleomycin (Bleo)-induced alveolar simplification newborn rat model (recapitulating arrested alveolarization during BPD), we evaluated the therapeutic effects of compound-A (CpdA), a SEGRAM. Sprague-Dawley rats were administered Bleo from postnatal day (PD) 0 to 10 and treated with dexamethasone (Dex) or CpdA from PD 0 to 13. The morphological changes and mRNA expression of inflammatory mediators, including interleukin (IL)-1β, C–X–C motif chemokine ligand 1 (CXCL1), and C–C motif chemokine 2 (CCL2) were investigated.
Results
Similar to the effects of Dex, CpdA exerted protective effects on morphological derangements and inhibited macrophage infiltration and production of pro-inflammatory mediators in Bleo-treated animals. The effects of CpdA were probably mediated by GC receptor (GR)-dependent trans-repression, because unlike the Dex-treated group, anti-inflammatory genes specifically induced by GR-dependent trans-activation (such as “glucocorticoid-induced leucine zipper, GILZ”) were not upregulated.
Conclusions
CpdA improved lung inflammation, inhibited the arrest of alveolar maturation, and restored histological and biochemical changes in a Bleo-induced alveolar simplification model.
Impact
-
SEGRAMs have attracted widespread attention because they are expected to not exhibit unfavorable effects of GCs.
-
Compound A, one of the SEGRAMs, improved lung morphometric changes and decreased lung inflammation in a bleomycin-induced arrested alveolarization, a newborn rat model representing one of the main features of BPD pathology.
-
Compound A did not elicit bleomycin-induced poor weight gain, in contrast to dexamethasone treatment.
-
SEGRAMs, including compound A, may be promising candidates for the therapy of BPD with less adverse effects compared with GCs.
Similar content being viewed by others
Introduction
Advances in perinatal and neonatal care have increased the survival rate of extremely low gestational age newborns <28 weeks’ gestation (ELGANs).1,2 However, bronchopulmonary dysplasia (BPD) remains a major cause of morbidity for ELGANs, often leading to adverse sequelae, such as respiratory and neurodevelopmental disabilities. At present, ~40% of ELGANs experience some degree of BPD.3,4
BPD is a multifactorial disease induced by various insults such as intrauterine inflammatory processes, postnatal oxygen/ventilator-mediated injury, and infection.5,6 Most importantly, continuous and/or repetitive inflammation underlies the development of BPD.7 Accordingly, glucocorticoids (GCs) are widely used in the treatment of BPD as the first choice of anti-inflammatory drugs.8 However, GCs are known to have many side effects such as immunosuppression, causing hyperglycemia and delay in somatic growth and impairing neurodevelopment, all of which are particularly problematic in infants.9,10
GC is a ligand of the GC receptor (GR), a ligand-dependent transcription factor belonging to the nuclear receptor superfamily.11 GR resides in the cytoplasm in a ligand-free state, and bound to a multiprotein complex. Upon binding of a GC to GR, the complex is translocated into the nucleus and induces both stimulation and inhibition of gene expression through various mechanisms.12,13 Among these, trans-activation and trans-repression are well documented14 (Fig. 1). Trans-activation proceeds through a homo-dimeric GC-GR complex, binding to glucocorticoid-response elements (GREs) and upregulating anti-inflammatory genes including those for anti-inflammatory cytokines (interleukin (IL)-4, IL-10 etc.), annexin-1, dual-specificity phosphatase 1 (DUSP1), glucocorticoid-induced leucine zipper (GILZ), also known as TSC22 domain family member 3, and secretory leukocyte peptidase inhibitor (SLPI) etc. as well as those related to gluconeogenesis, protein degradation, and lipolysis.12 By contrast, trans-repression inhibits transcription of pro-inflammatory genes including pro-inflammatory cytokines (IL-1β, IL-6, TNF-α, IF-γ etc.), chemokines, adhesion molecules etc. by direct interaction between monomeric GC-GR complex and pro-inflammatory transcription factors, such as nuclear factor-κB (NF-κB), activator protein-1 (AP-1), p53, signal transducers and activators of transcription (STAT), interferon regulatory factor-3 (IRF-3), and cAMP response element binding protein (CREB).15 Trans-repression does not require GR dimerization.14,15
GR resides in the cytoplasm in the ligand-free state bound to a multiprotein complex. GC or SEGRAMs are principally lipophilic molecules, meaning that they can traverse plasma membranes and enter into cytoplasm. When GC binds to GR, the complex is translocated into the nucleus, where it induces both stimulation and inhibition of gene expression through various mechanisms. Among these, trans-activation and trans-repression are well documented. Trans-activation proceeds through homo-dimeric GC-GR complex, binding to glucocorticoid-response elements and upregulates anti-inflammatory mediators as well as genes related to several adverse effects of GCs. In contrast, trans-repression inhibits transcription of pro-inflammatory mediators by direct interaction between monomeric GC-GR complex and pro-inflammatory transcription factors. This process does not require GR dimerization. SEGRAMs act as a ligand for GRs and have anti-inflammatory properties via only trans-repression.
It is generally accepted that most unfavorable effects of GCs are brought about by the trans-activation process, although this also induces some anti-inflammatory proteins as listed above.12 To minimize adverse effects while retaining anti-inflammatory properties as much as possible, considerable attempts have been made to develop novel GR agonists that favor trans-repression with weak or negligible trans-activation properties. Such compounds possessing the ability to decouple trans-repression from trans-activation, are termed selective glucocorticoid-receptor agonists and modulators (SEGRAMs).13,14,16
One such SEGRAM is compound A (CpdA, 2-(4-acetoxyphenyl)-2-chloro-N-methyl-ethylammonium chloride).17,18 CpdA is a stable synthetic analog of hydroxy phenyl aziridine precursor, which has been isolated from tumbleweed and has been used historically as an oral contraceptive by San people living in southern Africa15 (Fig. 2b). CpdA exhibits favorable properties as a GC ligand, possessing sufficient trans-repression ability without apparent trans-activation.14,15,16 Thus, in theory, CpdA may exert less adverse effects of GCs.
Histologically, BPD is characterized by inflammation and alveolar maturation arrest during the early stage and by increasing wall thickness and fibrosis during the late stage of disease.5,19 In the present study, we used a bleomycin (Bleo)-induced lung injury model, commonly employed to investigate lung fibrosis.20 In immature neonatal rat, Bleo is known to result in alveolar simplification due to maturation arrest, which is thought to reproduce one of the typical BPD pathologies.21,22 Using this model, we aimed to confirm whether CpdA could improve histological abnormalities and reduce inflammatory response induced by Bleo administration.
Methods
All procedures were approved by the research animal committee of Osaka Medical and Pharmaceutical University (authorized number 29087, 30091 and 2019-092).
Subjects
Pregnant Sprague-Dawley rats were purchased from CREA Japan, Inc. (Tokyo, Japan). Pups were delivered naturally at 21 days of gestation and were nursed by the dam. The day of birth was described as postnatal day (PD) 0. Animals were fed ad libitum and exposed to 12:12-h light-dark cycles throughout the study period. CpdA was purchased from Santa Cruz Biotechnology, Inc. (Santa Cruz, CA), bleomycin sulfate was purchased from LKT Laboratories, Inc. (St. Paul, MN), and dexamethasone (Dex) was purchased from Fujifilm Wako Pure Chemical Corporation Inc. (Osaka, Japan). Anti- CD68 antibody (catalog no. ab31630) was obtained from Abcam, Inc. (Cambridge, UK).
Protocol
PD-0 rats from timed-pregnant dams were divided into four groups; 1) Control group: Normal saline-exposed and vehicle (distilled water)-treated, 2) Bleo group: Bleo-exposed (1 mg/kg) and vehicle-treated, 3) Dex group: Bleo-exposed and Dex-treated (0.1 mg/kg), and 4) CpdA group: Bleo-exposed and CpdA-treated (1 mg/kg). All reagents were administered by intraperitoneal injection. Bleo or normal saline were injected from PD 0 to 10. Vehicle, Dex, or CpdA were injected until PD-13. On PD-10 or 14, pups were euthanized with an intraperitoneal injection of pentobarbital sodium (100 mg/kg) (Fig. 2a).
Fixation of lung tissue
After rats were euthanized, their left lungs were removed, snap frozen in liquid nitrogen, and stored separately at −80 °C until use for subsequent RNA analysis. The right lung was air-inflated and perfusion-fixed at constant pressure, removed along with the heart, and fixed in 4% paraformaldehyde. These were then embedded in paraffin and lung tissues were cut into 4 μm sections for subsequent histological analyses of lung injury and immunohistochemical analysis.
Lung morphometry
Sections obtained from the right lung on PD-14 were stained with hematoxylin and eosin and the radial alveolar count (RAC) and mean linear intercept (MLI) length were measured. Each section was imaged on a Nikon Eclipse 80i microscope, using the 10× objective and captured by digital camera (DS-Ri1, Nikon, Tokyo, Japan). At least ten random lung fields were photographed from each animal. Measurements were carried out on three noncontiguous right lung sections per animal by a single observer blinded to the group identity.
The RAC was determined as previously described.21,22,23 Respiratory bronchioles were identified as bronchioles lined by epithelia in one part of the wall. From the center of the respiratory bronchiole, a perpendicular line was drawn to the edge of the acinus (as defined by a connective tissue septum or the pleura), and septa intersected by this line were counted. The MLI was measured as previously reported.21,22,24 Large airways and vessels were avoided. Grids of horizontal and vertical lines were superimposed on an image and the number of times that lines intersected with the tissue was counted. The total length of grid lines was then divided by the number of intersections to afford the MLI in μm.
Immunohistochemical analysis
Tissue from right lungs on PD-14 was immunestained for CD68 to identify macrophages. Paraffin was removed from paraffin-embedded slices of formalin-fixed tissue using xylene. Sections were rehydrated by serial immersions in 100% ethanol, 90% ethanol, 70% ethanol, and water. Antigen retrieval was conducted with a microwave oven and subsequent washing with phosphate buffered saline (PBS). Endogenous peroxidase activity was reduced by immersion in 3% hydrogen peroxide. After rinsing, sections were covered with 3% goat serum for 30 min and incubated with anti-CD68 antibody diluted in PBS (1:800) overnight. After incubation, sections were rinsed with PBS and incubated with biotin-labeled secondary antibody diluted 1:300 in PBS for 2 h. After incubation with the secondary antibody, sections were rinsed with PBS, incubated in avidin-biotin complex staining kit (Vector Laboratories, Burlingame, CA) for 30 min at ~25 °C, rinsed in PBS, and developed with diaminobenzidine and hydrogen peroxide. Slides were lightly counterstained with hematoxylin and were then dehydrated by sequential immersion in 70% ethanol, 90% ethanol, 100% ethanol, and xylene before applying coverslips. Analysis of tissue macrophage (CD68-positive) numbers was conducted from ten random, non-overlapping, high-power fields captured from each section. Measurements were conducted on three noncontiguous right lung sections per animal by two observers blinded to the group identity.
Real-time PCR
The left lung tissue was used to analyze gene expression on PD-10 (at the termination of Bleo exposure) and PD-14 (at the termination of CpdA/Dex treatment) (Fig. 2a). Total RNA was extracted with ISOGEN (Nippon Gene, Tokyo, Japan), according to the manufacturers protocol. The RNA purity was verified by A260/A280 ratio. Total RNA was reverse transcribed into cDNA using an Omniscript Reverse Transcription Kit (Qiagen, Venlo, Netherlands). We measured mRNA levels of cytokines and chemokines with reverse transcription–polymerase chain reaction with TaqMan primers using a StepOnePlus real-time PCR system (Thermo Fisher Scientific, Waltham, MA), including IL-1β (Rn99999009_m1), C–X–C motif chemokine ligand 1 (CXCL1; Rn00578225_m1), C–C motif chemokine 2 (CCL2; Rn00580555_m1), DUSP1 (Rn00678341_g1), GILZ (Rn00580222_m1), and SLPI (Rn00670378_m1). Glyceraldehyde-3-phosphate dehydrogenase (GAPDH; Rn01775763_g1) was used as a standardizing control. These TaqMan primers (TaqMan Gene Expression Assays) were purchased from Thermo Fisher Scientific Inc. (Waltham, MA). The expression level of each mRNA was calculated using the 2−ΔΔCT method.
Statistics
All statistical analyses were carried out using JMP Pro Version 14.0 (SAS Institute Inc., Cary, NC). Data were expressed as mean ± SE and analyzed using one-way ANOVA with post-hoc Tukey test. A value of p < 0.05 was considered significant. The size of the effect was estimated from the distribution by calculation of Cohen’s d.
Results
Of the 56 animals studied, three animals died during the study: one in the Bleo group, one in the Dex group and one in the CpdA group.
Weight gain
The weight of pups at birth was the same within all groups. On PD-14, pups in the Dex group had significantly lower body weight gain since birth (18.8 ± 2.3 g, p < 0.05) compared with Control (26.6 ± 1.0), Bleo (26.0 ± 1.4), and CpdA groups (26.0 ± 1.9) (Fig. 3). The three groups other than the Dex group showed similar weight gain.
Histologic and morphometric analyses
Lungs from the Bleo group displayed impaired alveolarization as demonstrated by decreased septation, distal airspace enlargement, and a reduction in complexity compared with the Control group (Fig. 4a, b). Treatment with Dex or CpdA improved the alveolar structure and attenuated the lung injury (Fig. 4c, d). The MLI was significantly increased in rats of the Bleo group compared with the control group (Bleo: 111.5 ± 5.4 μm vs. Control: 69.5 ± 2.3, p < 0.01, Cohen’s d = 3.4, Fig. 4g). Dex significantly reduced MLI compared with the Bleo group (Dex: 93.4 ± 2.8, p < 0.01 vs. Bleo, Cohen’s d = 1.5, Fig. 4g). The MLI value of CpdA group (101.1 ± 4.5) was also lower than that of Bleo group, but the difference was not statistically significant (p = 0.07 vs. Bleo, Cohen’s d = 1.1). Similarly, another indicator, RAC, was significantly reduced in rats of the Bleo group compared with the control group (Bleo: 9.0 ± 0.6 vs. Control: 13.3 ± 0.3, p < 0.01, Cohen’s d = 3.1, Fig. 4h). Both Dex and CpdA significantly inhibited the reduction of RAC (Dex: 11.7 ± 0.1, p < 0.01, Cohen’s d = 2.2, and CpdA: 11.2 ± 0.7, p < 0.05, Cohen’s d = 1.2, vs. Bleo, Fig. 4h), although they were still lower than the control value. In addition, at least within our doses, neither Dex nor CpdA alone exerted any apparent effect on histological analysis (Fig. 4e, f), or quantitative measurements (MLI and RAC) (Fig. 4g, h).
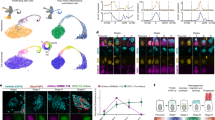
a–f Lung histology stained with hematoxylin and eosin. a control group, b Bleo group, c Dex group, d CpdA group, e Dex alone group, and f CpdA alone group. Magnification ×100. Scale bar is 200 μm. g Mean linear intercept (MLI). h Radial alveolar counts (RACs). White bar: Control group, Black bar: Bleo group, Horizontal striped bar: Dex group, Polka dot bar: CpdA group. Mean ± SE. N = 5–8/group. *p < 0.05, **p < 0.01. Bleo group displayed impaired alveolarization, increased MLI, and decreased RACs compared with the control group (a, b, g, h). Treatment with Dex or CpdA improved the alveolar structure (c, d, g, h). Neither Dex nor CpdA alone exerted any apparent effect on histological or morphometric analyses (e, f, g, h).
Immunohistochemical analysis
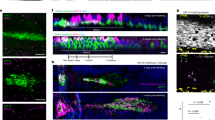
Previous studies have reported that macrophages were infiltrated in the lung of Bleo-exposure models,25,26 and Dex effectively prevented macrophage recruitment.27,28 Similarly, in the present study, immunostaining revealed that the Bleo group had significantly increased recruitment of macrophages compared to those of the control group (Bleo: 46.3 ± 1.7 cells/10 HPF vs. Control: 34.7 ± 3.3, p < 0.01, Cohen’s d = 0.9, Fig. 5a, b, e). CpdA treatment inhibited macrophage infiltration significantly (40.2 ± 1.8, p < 0.05 vs. Bleo, Cohen’s d = 0.5, Fig. 5d, e), while Dex showed no effect (45.7 ± 2.0, p = 0.98 vs. Bleo, Cohen’s d < 0.1, Fig. 5c, e).
CpdA decreased the extent of macrophage infiltration, while Dex showed no effect. a–d anti-CD68 immunostaining, a control group, b Bleo group, c Dex group, and d CpdA group. Magnification ×400. Scale bar is 50 μm. Brown stained cells are CD68-positive macrophage (arrow). e the number of macrophages per 10 HPF. White bar: Control group, Black bar: Bleo group, Horizontal striped bar: Dex group, Polka dot bar: CpdA group. Mean ± SE. N = 5–8/group. *p < 0.05, **p < 0.01, NS not significant.
mRNA expression of cytokines and chemokines
Inflammatory mediators have been reported to increase in either bronchoalveolar lavage or homogenized lung tissues from BPD.29,30,31,32 Therefore, we investigated the changes of some pro-inflammatory mediators. We chose IL-1β as a major inflammatory cytokine, CXCL1 as a neutrophil attractant, and CCL2 as a potent chemoattractant for inflammatory cells. On PD-10 (Fig. 6a, upper panels), the mRNA expression of CXCL1 and CCL2 were significantly elevated by Bleo treatment relative to those in Control group. Both Dex and CpdA effectively prevented Bleo-induced up-regulation of these mediators, although statistical significance was not always achieved. Four days after (PD-14, Fig. 6a, lower panels), chemokine expressions levels were returned to the control level regardless of any treatment. Unexpectedly, the expression of IL-1β was reduced by Bleo relative to the control group. These findings may be related to our protocol wherein Bleo injection was discontinued by d-10 (Fig. 2a).
a Relative mRNA expression of IL-1β, CXCL1, and CCL2 at PD-10 (upper panels) and PD-14 (lower panels). At PD-10, both Dex and CpdA effectively prevented Bleo-induced up-regulation of these mediators. However, inhibitory effects disappeared at PD-14. b Relative mRNA expression of DUSP1, GILZ and SLPI at PD-10. These anti-inflammatory mediators are likely induced by GC through the homo-dimeric trans-activation mechanism. None were induced or else were rather decreased in the CpdA group, while Dex increased DUSP-1. White bar: Control group, Black bar: Bleo group, Horizontal striped bar: Dex group, Polka dot bar: CpdA group. Mean ± SE. N = 5–8/group. *p < 0.05, **p < 0.01.
mRNA expression of anti-inflammatory proteins related to GC-dependent trans-activation
DUSP1, GILZ and SLPI are representative anti-inflammatory genes, which are thought to be upregulated through a trans-activation process dependent on homo-dimeric GC-GR complex.12,15 None of these were induced or rather were decreased (GILS and SLPI) in the CpdA group, while Dex increased DUSP-1 (Fig. 6b). In addition, the expression of DUSP-1 was significantly lower in the CpdA group than in the Dex group.
Discussion
In our Bleo-induced alveolar simplification model, CpdA exerted protective effects on morphological derangements, inhibited macrophage infiltration and production of pro-inflammatory mediators. In particular, the inhibition of morphological changes was shown to be biologically sufficient, and the effect sizes were very large as estimated by Cohen’s d (1.1–3.6). These effects were probably based on GR-dependent trans-repression activity, since anti-inflammatory genes specifically induced by GR-dependent trans-activation (DUSP1, GILZ, and SLPI) were not upregulated (Figs. 1 and 6). This interpretation is consistent with previous studies showing the inability of CpdA to stimulate GILZ or DUSP gene expression.33,34,35 It is generally accepted that the anti-inflammatory effects of GCs are mainly due to trans-repression. However, a counter-augment emphasizes the importance of the trans-activation process as the anti-inflammatory mechanism of GCs.12 Aforementioned molecules induced by GC-dependent trans-activation, especially GILZ, are known to demonstrate considerable anti-inflammatory effects in various situations.36 Therefore, whether SEGRAMs including CpdA exert anti-inflammatory properties comparable to GCs in clinical settings is still uncertain.
Various animal model studies have reported the efficacy of CpdA on inflammatory processes, such as collagen-induced arthritis,37 autoimmune encephalomyelitis, type I diabetes, acute colitis, Duchenne muscular dystrophy,38 or a Th2-driven asthma.39 Therefore, CpdA may exhibit clinical effectiveness against some inflammatory disorders. Recently, some SEGRAMs, such as ADZ7594 and Mapracorat, have been approved for use in clinical trials. ADZ7594 has been reported to improve lung function and symptoms in adult patients with asthma without any severe adverse effects.40 Mapracorat is used as a topical treatment for inflammatory skin disorders and has been reported to reduce the severity of psoriasis without any serious adverse effects.41
The mechanism of action of GCs is highly complex and is not completely understood. It is not restricted to trans-activation and trans-repression, as shown simply in Fig. 1. In addition to a tethering mechanism (Fig. 1), composite or competitive suppression of transcription factors are further examples of trans-repression.14 Dimeric and monomeric GR do not necessarily show opposing effects; monomeric GR may also induce gene activation.11,12,13,14 Whether favorable or unfavorable, each clinical effect of a GC is a final phenotype resulting from the complex interplay of many upregulated and down-regulated genes. Therefore, we ought not to suppose that monomeric GR-SEGRAM complex is free from any or all adverse effects of GR.
Nevertheless, CpdA did not influence weight gain, in contrast to poor weight gain resulting from Dex treatment in the present study. In this sense, CpdA is superior to GCs, although it should be noted that the observation period in this case was too short. To give an example, AL-438, one of the SEGRAMs, was reported to show escape from GC-mediated adverse effects on chondrocyte proliferation and bone growth, while maintaining anti-inflammatory properties.42
Other than growth retardation, CpdA did not induce enzymes relating to gluconeogenesis, protein degradation, and lipolysis15 (Fig. 1). It failed to induce the regulated in development and DNA-damage response 1 (REDD1),15 which is thought to be a key player in GC-mediated cutaneous atrophy and a regulator of skeletal muscle metabolism.43,44 These molecular findings were likely responsible for the results of model studies showing CpdA ability to escape from hyperglycemia, muscular and skin atrophy38 and osteoporosis.45 In addition, CpdA possibly showed a lesser degree of resistance phenomenon, observed in long-standing GC treatment.15 This is partly explained by the studies showing that CpdA did not induce GR degradation by proteasomes, and did not activate expression of the FK506-binding protein 51 (FKBP51), which is known to prevent GR nuclear translocation.46 However, in terms of neurodevelopmental disability, the most serious sequela of GC exposure in infants, it is unclear whether SEGRAMs avoid this consequence, since the underlying mechanisms are unclear.
Until recently, pathological findings of BPD were dichotomized into so-called “old” and “new” BPD, corresponding to the pre- and post-surfactant eras, respectively.5,47 “Old” BPD demonstrated non-homogeneous findings including severe airway injury (i.e., airway epithelial lesions and smooth muscle hyperplasia) and fibrotic change (i.e., fibroproliferation with bundles of myofibroblasts and collagen in the thickened alveolar septa). In contrast, the main feature of “new” BPD is reduced alveolar development characterized by fewer, larger, and simplified alveoli (arrest of alveolarization) with less prominent airway injury and fibrotic change. However, this apparent dichotomy may be too simplistic. Practically speaking, both features may be mixed to various degrees in any era. Recently, Wu et al. reported that BPD could be classified clinically into several phenotypic subgroups according to the most affected regions: large airway disease, parenchymal lung disease, and pulmonary hypertension.48 It may be difficult to apply these phenotypes clearly into respective pathology, because BPD presents as a mixture of each clinical phenotype and pathological finding. Therefore, it is unrealistic to expect that some single animal model will precisely reproduce all the complex and heterogeneous pathological features at the same time. Instead, each model should be considered as representative of a specific pathological finding.19 Our early Bleo-exposure model at least recapitulated arrest of alveolarization, one of the important pathological events of BPD. CpdA accelerated alveolar maturation in this model, which means that CpdA has the potential to secure gas exchange area and improve alveolar ventilation/perfusion ratio against BPD-inducible derangement.
Nevertheless, this study has several limitations. First, CpdA and Dex treatment was initiated on the same day as the Bleo-exposure began. In other words, CpdA and Dex were used as a prophylactic medicine in this study. In clinical practice, GCs are only administered to infants suffering from severe BPD. Thus, it is necessary to verify whether CpdA shows a similar effect during chronic stages of BPD. Second, we evaluated both CpdA and Dex in a single dosage only and did not investigate their dose-dependency. When determining the supplemental dose of CpdA, we referenced previous works investigating CpdA effect on various animal models. We found several rodent model studies, the majority of which dealt with mice models. The dose of CpdA extended over the range of 0.8 to 15 mg/kg/day.39,49 At first, we chose a minimal dose of 1 mg/kg/day and as that dose of CpdA showed an apparent effect, we did not try other doses of CpdA. Therefore, we cannot provide the optimal dose range of CpdA from these experiments on our Bleo-model. The dose of Dex was determined based on clinical management of severe BPD; usually administered at the range of 0.1 to 0.5 mg/kg/day. The final doses of both CpdA and Dex in this study cannot be equivalent in anti-inflammatory effect, which makes it difficult to compare these two agents. However, we used Dex as a positive control, representative of GCs, and did not intend to compare Dex and CpdA. In the future, it will be necessary to study the effect of various dosages of CpdA on chronic-stage BPD models. Third, we have assessed Bleo-induced changes of cytokines/chemokines in mRNA levels only, although this should be sufficient for confirming the GR dependence of anti-inflammatory proteins. The changes in mRNA levels of cytokines/chemokines over time may differ from those at the protein levels, and future studies are needed. Finally, In the present study, we only confirmed the efficacy of RvD1 against arrested alveolarization. We believe that other BPD models are necessary to confirm effectiveness of RvD1 against BPD.
In conclusion, our results clearly showed that CpdA decreased lung inflammation and improved lung morphometric changes in Bleo-induced alveolar maturation arrest, a newborn rat model representing one of the main features of BPD pathology. We also confirmed that CpdA may act through a monomeric trans-repression mechanism and showed that it possibly escaped from growth-impairing effects, unlike GCs. SEGRAMs, including CpdA, may be promising candidates for the therapy of BPD as GC mimics with less severe adverse effects.
Data availability
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Norman, M. et al. Association between year of birth and 1-year survival among extremely preterm infants in Sweden during 2004–2007 and 2014–2016. JAMA 321, 1188-1199 (2019).
Kusuda, S., Bennett, M. & Gould, J. Neonatal Research Network of Japan and the California Perinatal Quality Care Collaborative. Outcomes of Infants with Very Low Birth Weight Associated with Birthplace Difference: A Retrospective Cohort Study of Births in Japan and California. J. Pediatr. 229, 182–190 (2021).
Stoll, B. J. et al. Trends in care practices, morbidity, and mortality of extremely preterm neonates, 1993-2012. JAMA 314, 1039–1051 (2015).
Nakashima, T. et al. Neonatal Research Network of Japan. Trends in Bronchopulmonary Dysplasia Among Extremely Preterm Infants in Japan, 2003-2016. J. Pediatr. 230, 119–125 (2021).
Thébaud, B. et al. Bronchopulmonary dysplasia. Nat. Rev. Dis. Prim. 14, 78 (2019).
Álvarez-Fuente, M. et al. Preventing bronchopulmonary dysplasia: new tools for an old challenge. Pediatr. Res. 85, 432–441 (2019).
Papagianis, P. C., Pillow, J. J. & Moss, T. J. Bronchopulmonary dysplasia: Pathophysiology and potential anti-inflammatory therapies. Paediatr. Respir. Rev. 30, 34–41 (2019).
Filippone, M., Nardo, D., Bonadies, L., Salvadori, S. & Baraldi, E. Update on Postnatal corticosteroids to prevent or treat bronchopulmonary dysplasia. Am. J. Perinatol. 36, S58–S62 (2019).
Yeh, T. F. et al. Outcomes at school age after postnatal dexamethasone therapy for lung disease of prematurity. N. Engl. J. Med. 350, 1304–1313 (2004).
Doyle, L. W. Postnatal corticosteroids to prevent or treat bronchopulmonary dysplasia. Neonatology 118, 244–251 (2021).
Vettorazzi, S., Nalbantoglu, D., Gebhardt, J. C. M., & Tuckermann, J. A guide to changing paradigms of glucocorticoid receptor function—a model system for genome regulation and physiology. FEBS J. (2021) (epub ahead of print).
Vandevyver, S. et al. New insights into the anti-inflammatory mechanism of glucocorticoids: an emerging role for glucocorticoid-receptor-mediated trans-activation. Endocrinology 154, 993–1007 (2013).
Reichardt, S. D. et al. The role of glucocorticoids in inflammatory diseases. Cells 10, 2921 (2021).
Sundahl, N. et al. Selective glucocorticoid receptor modulation: new directions with non-steroidal scaffolds. Pharmacol. Ther. 152, 28–41 (2015).
Lesovaya, E. et al. Discovery of compound A—a selective activator of the glucocorticoid receptor with anti-inflammatory and anti-cancer activity. Oncotarget 6, 30730–30744 (2015).
Safy, M. et al. Efficacy and safety of selective glucocorticoid receptor modulators in comparison to glucocorticoids in arthritis, a systematic review. PLoS ONE 12, e0188810 (2017).
Louw, A. & Swart, P. Salsola tuberculatiformis Botschantzev and an aziridine precursor analog mediate the in vivo increase in free corticosterone and decrease in corticosteroid-binding globulin in female Wistar rats. Endocrinology 140, 2044–2053 (1999).
Bosscher, K. D. et al. A fully dissociated compound of plant origin for inflammatory gene repression. Proc. Natl Acad. Sci. USA 102, 15827–15832 (2005).
Alvira, C. M. & Morty, R. E. Can we understand the pathobiology of bronchopulmonary dysplasia? J. Pediatr. 190, 27–37 (2017).
Kolb, P. et al. The importance of interventional timing in the bleomycin model of pulmonary fibrosis. Eur. Respir. J. 55, 1901105 (2020).
Tourneux, P. et al. Inhaled nitric oxide improves lung structure and pulmonary hypertension in a model of bleomycin-induced bronchopulmonary dysplasia in neonatal rats. Am. J. Physiol. Lung Cell. Mol. Physiol. 297, L1103–L1111 (2009).
Sewing, A. C. et al. Therapeutic hypercapnia prevents bleomycin-induced pulmonary hypertension in neonatal rats by limiting macrophage-derived tumor necrosis factor-α. Am. J. Physiol. Lung Cell. Mol. Physiol. 303, L75–L87 (2012).
Cooney, T. P. & Thurlbeck, W. M. The radial alveolar count method of Emery and Mithal: a reappraisal 2—intrauterine and early postnatal lung growth. Thorax 37, 580–583 (1982).
Shivanna, B. et al. Omeprazole attenuates pulmonary aryl hydrocarbon receptor activation and potentiates hyperoxia-induced developmental lung injury in newborn mice. Toxicol. Sci. 148, 276–287 (2015).
Lee, A. H. et al. Pho-inase inhibitor prevents bleomycin-induced injury in neonatal rats independent of effects on lung inflamemation. Am. J. Respir. Cell. Mol. Biol. 50, 61–73 (2014).
Ee, M. T. et al. Leukotriene B4 mediates macrophage influx and pulmonary hypertension in bleomycin-induced chronic neonatal lung injury. Am. J. Physiol. Lung Cell. Mol. Physiol. 311, L292–L302 (2016).
Li, H. P., Li, X., He, G. J., Yi, X. H. & Kaplan, A. P. The influence of dexamethasone on the proliferation and apoptosis of pulmonary inflammatory cells in bleomycin-induced pulmonary fibrosis in rats. Respirology 9, 25–32 (2004).
Bai, L., Li, A., Gong, C., Ning, X. & Wang, Z. Protective effect of rutin against bleomycin induced lung fibrosis: Involvement of TGF-β1/α-SMA/Col I and III pathway. Biofactors 46, 637–644 (2020).
Ryan, R. M., Ahmed, Q. & Lakshminrusimha, S. Inflammatory mediators in the immunobiology of bronchopulmonary dysplasia. Clin. Rev. Allergy Immunol. 34, 174–190 (2008).
Groneck, P., Reuss, D., Gotze-Speer, B. & Speer, C. P. Effects of dexamethasone on chemotactic activity and inflammatory mediators in tracheobronchial aspirates of preterm infants at risk for chronic lung disease. J. Pediatr. 122, 938–944 (1993).
D’Angio, C. T. et al. Discordant pulmonary proinflammatory cytokine expression during acute hyperoxia in the newborn rabbit. Exp. Lung Res. 25, 443–456 (1999).
Londhe, V. A. et al. CXCR2/CXCR2 ligand biological axis impairs alveologenesis during ds RNA- induced lung inflammation in mice. Pediatr. Res. 58, 919–926 (2005).
Drebert, Z., Bracke, M. & Beck, I. M. Glucocorticoids and the non-steroidal selective glucocorticoid receptor modulator, compound A, differentially affect colon cancer-derived myofibroblasts. J. Steroid Biochem. Mol. Biol. 149, 92–105 (2015).
Malaise, O. et al. Glucocorticoid-induced leucine zipper (GILZ) is involved in glucocorticoid- induced and mineralocorticoid-induced leptin production by osteoarthritis synovial fibroblasts. Arthritis Res. Ther. 18, 219 (2016).
Desmet, S. J. et al. Compound A influences gene regulation of the Dexamethasone-activated glucocorticoid receptor by alternative cofactor recruitment. Sci. Rep. 7, 8063 (2017).
Bereshchenko, O., Migliorati, G., Bruscoli, S. & Riccardi, C. Glucocorticoid-induced leucine zipper: a novel anti-inflammatory molecule. Front. Pharmacol. 10, 308 (2019).
Dewint, P. et al. A plant-derived ligand favoring monomeric glucocorticoid receptor conformation with impaired trans-activation potential attenuates collagen-induced arthritis. J. Immunol. 180, 2608–2615 (2008).
Huynh, T. et al. Selective modulation through the glucocorticoid receptor ameliorates muscle pathology in mdx mice. J. Pathol. 231, 223–235 (2013).
Reber, L. L. et al. A dissociated glucocorticoid receptor modulator reduces airway hyperresponsiveness and inflammation in a mouse model of asthma. J. Immunol. 188, 3478–3487 (2012).
Brown, M. N. et al. Efficacy and safety of ADZ7594, an inhaled non-steroidal selective glucocorticoid receptor modulator, in patients with asthma: a phase 2a randomized, double blind, placebo-controlled crossover trial. Respir. Res. 20, 37 (2019).
Wigger-Alberti, W. et al. Comparison of occlusive and open application in a psoriasis plaque test design, exemplarily using investigations of mapracorat 0.1% ointment versus vehicle and reference drugs. Ski. Pharmacol. Physiol. 30, 102–114 (2017).
Owen, H. C., Miner, J. N., Ahmed, S. F. & Farquharson, C. The growth plate sparing effects of the selective glucocorticoid receptor modulator, AL-438. Mol. Cell. Endocrinol. 264, 164–170 (2007).
Baida, G. et al. REDD1 functions at the crossroads between the therapeutic and adverse effects of topical glucocorticoids. EMBO Mol. Med. 7, 42–58 (2015).
Britto, F. A. et al. REDD1 deletion prevents dexamethasone-induced skeletal muscle atrophy. Am. J. Physiol. Endocrinol. Metab. 307, E983–E993 (2014).
Rauner, M. et al. Dissociation of osteogenic and immunological effects by the selective glucocorticoid receptor agonist, compound A, in human bone marrow stromal cells. Endocrinology 152, 103–112 (2011).
Lesovaya, E. et al. Combination of a selective activator of the glucocorticoid receptor Compound A with a proteasome inhibitor as a novel strategy for chemotherapy of hematologic malignancies. Cell Cycle 12, 133–144 (2013).
Day, C. L. & Ryan, R. M. Bronchopulmonary dysplasia: new becomes old again! Pediatr. Res. 81, 210–213 (2017).
Wu, K. Y. et al. Characterization of disease phenotype in very preterm infants with severe bronchopulmonary dysplasia. Am. J. Respir. Crit. Care. Med. 201, 1398–1406 (2020).
Zhang, Z., Zhang, Z. Y. & Schluesener, H. J. Compound A, a plant origin ligand of glucocorticoid receptors, increases regulatory T cells and M2 macrophages to attenuate experimental autoimmune neuritis with reduced side effects. J. Immunol. 183, 3081–3091 (2009).
Acknowledgements
The authors would like to thank Kazumi Honda and Yumiko Yoshimura for assistance with the biochemical analysis, and Yusuke Onishi and Yasuhiro Ogino for assistance with the immunohistochemical analysis.
Funding
The authors have no financial relationships relevant to this article to disclose.
Author information
Authors and Affiliations
Contributions
S.I., T.O., and J.S. conceived and designed the research. S.I., J.S., and S.K. performed experiments and acquired data. S.I. prepared the manuscript. T.O. revised and edited the manuscript. D.N. helped in executing the statistical analysis. S.Y., Y.H., and A.A. critically reviewed the manuscript for important intellectual content. All authors have approved the final manuscript and agreed to be accountable for all aspects of the work.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Ishikawa, S., Ogihara, T., Yamaoka, S. et al. A glucocorticoid-receptor agonist ameliorates bleomycin-induced alveolar simplification in newborn rats. Pediatr Res 93, 1551–1558 (2023). https://doi.org/10.1038/s41390-022-02257-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41390-022-02257-8
This article is cited by
-
Effects of postnatal corticosteroids on lung development in newborn animals. A systematic review
Pediatric Research (2024)