Abstract
Background
Anemia of prematurity is common in extremely preterm neonates, and oxygen exposure may participate to anemia by inhibiting erythropoietin secretion. We aimed to determine whether hyperoxia exerts an independent role in the occurrence of the anemia of prematurity.
Methods
Sprague-Dawley pups were exposed to 80% oxygen or room air from days 3 to 10 of life. Main outcome was the difference in hemoglobin and circulating erythropoietin levels in animals exposed to hyperoxia at 10 days of life. We performed a complete blood count analysis using fluorescent laser flow cytometry and measured circulating erythropoietin levels using ELISA.
Results
We found lower hemoglobin in the hyperoxia group, compared to the normoxia group, both in males (70 ± 3 versus 78 ± 2 g/l) and in females (71 ± 2 versus 81 ± 3 g/l) at 10 days of life. Reticulocyte count was not increased in the hyperoxia group. Circulating erythropoietin levels were lower at 10 days of life in the animals exposed to hyperoxia, both in males (33 ± 7 versus 73 ± 6 pg/ml) and in females (37 ± 5 versus 66 ± 3 pg/ml), but were similar at 28 days of life.
Conclusion
Neonatal exposure to hyperoxia decreases hematopoiesis in rats.
Impact
-
Mechanisms leading to anemia of prematurity are not well known and their study in humans is complicated due to multiple confounders.
-
This study shows for the first time that exposure to high concentrations of oxygen in the neonatal period decreases hematopoiesis in rats, providing insight on the pathophysiological mechanisms of the anemia of prematurity.
-
This research paves the way for future therapeutic developments aiming to reduce the burden of anemia of prematurity and the necessity of red blood cell transfusions in extremely preterm neonates.
Similar content being viewed by others
Introduction
Approximately 10% of all births are premature (before 37 weeks of gestation), and 1% occur extremely preterm (≤28 weeks of gestation).1 Although survival of neonates born extremely preterm has largely improved in the past decades,2 numerous complications occur following extremely preterm birth.
Infants born extremely preterm frequently present low levels of hemoglobin that may require red blood cell (RBC) transfusion.3 Multiple factors have been identified as contributors to anemia of prematurity. Neonates born preterm exhibit erythropoietin (EPO) deficiency, with low EPO levels for a given hemoglobin value, compared to full-term infants.4 Preterm infants are exposed to supraphysiological oxygen levels compared to fetal life and often receive oxygen supplementation, resulting in intermittent hyperoxia, which may further limit their EPO production. Other complications following premature birth, such as sepsis and necrotizing enterocolitis, may lead to increased inflammation furthering anemia. In addition, frequent blood draws participate to blood losses and iron deficiency in this population.
While chronic exposure to hypoxia is associated with increased hemoglobin levels in the general population,5 it is debated whether normobaric exposure to high levels of oxygen decreases EPO production and erythropoiesis in adults.6,7 Whether exposure to supplemental oxygen contributes to the anemia of prematurity has not been established.
A better understanding of the pathophysiological mechanisms leading to anemia of prematurity is important as it may help developing therapeutic strategies to reduce RBC transfusions in preterm neonates. We hypothesized that supplemental oxygen exposure may contribute to anemia of prematurity by decreasing EPO production and by increasing systemic inflammation.
Isolating the effects of supplemental oxygen while controlling for confounding factors in human studies is a challenge. Rats exposed to high levels of oxygen in the neonatal period are a well-established rodent model that replicates various conditions and complications associated with preterm birth, including bronchopulmonary dysplasia and right ventricle (RV) alterations,8 left ventricle alterations,9 vascular abnormalities,10 and renal abnormalities.11 We aimed to assess, in this model, whether neonatal exposure to hyperoxia was associated with decreased erythropoiesis.
Methods
Animals and experimental protocol
Animal experimental procedures were approved by the Animal Ethics Committee of the Sainte-Justine University Hospital Research Center (approval number 754) and followed the guidelines of the Canadian Council on Animal Care and the National Institutes of Health Guide for the Care and Use of Laboratory Animals. Animal experiments took place at the animal facility of Sainte-Justine University Hospital Research Center.
Experimental protocol for rat transient neonatal exposure to high concentration of oxygen was previously described.9,12 Litters of Sprague-Dawley pups obtained from Charles River laboratories (Saint-Constant, QC, Canada) were culled to 12 (6 females and 6 males) and kept with their mothers in 80% oxygen in a hyperoxia chamber (ProOx P110, Biosherix, Lacona, NY) from 3 to 10 days of life (“hyperoxia” group) or were kept in room air (control group). Mothers exposed to high levels of oxygen were interchanged every 12 h with a surrogate mother kept in room air to avoid maternal morbidity due to oxygen toxicity. Pup survival was monitored throughout the protocol.
Half of the litters were sacrificed at 10 days of life, immediately after exposure to high levels of oxygen for the hyperoxia group. The remaining pups were all kept in room air until sacrifice at 28 days of life. Pups were weaned at 3 weeks to regular chow. Both male and female pups were studied.
Collection of plasma and tissues
At 10 days of life, pups were sacrificed by decapitation, and trunk blood was obtained. At 28 days of life, rats were anesthetized using isoflurane with oxygen (5% for induction, 1–2% for maintenance, for a total duration of 1–2 min) and blood was obtained using cardiac puncture. Blood was collected in EDTA-coated tubes. The right kidney and the liver were collected upon sacrifice, immediately frozen in liquid nitrogen, and stored at −80 °C for later analysis.
Assessment of complete blood count
For complete blood count, whole-blood samples were immediately shaken and briefly stored at 4 °C before analysis. Complete blood count, including reticulocytes, was performed within 48 h of blood collection using a XT-2000i analyzer (Sysmex Corporation, Kobe, Japan) that uses fluorescent laser flow cytometry methods with rodent veterinary specific algorithms, available at IDEXX Reference Laboratories (Montréal, QC, Canada). Markedly abnormal results were reviewed by a clinical veterinarian pathologist, per the laboratory’s protocol.
Assessment of plasma EPO, ferritin, and interleukin-6 (IL-6)
Immediately after collection, whole-blood samples collected in EDTA-coated tubes were centrifuged (4000 rpm, 15 min at 4 °C) for plasma separation. Plasma was then aliquoted and stored at −80 °C for later analysis. Plasma EPO concentration was measured in non-diluted plasma samples using an enzyme-linked immunosorbent assay (ELISA) kit (BioLegend, catalog number 442807) validated in rats, with a sensitivity of 1 pg/ml and a detection range of 8–500 pg/ml. Intra-assay coefficient of variation (CV) was <7% and inter-assay CV <8%. Plasma ferritin concentration was measured in diluted plasma samples (1:4–1:40) using an ELISA kit (abcam, catalog number ab157732) validated in rats, with a sensitivity of 2.8 ng/ml and a detection range of 12.5–400 pg/ml. Intra-assay and inter-assay coefficients of variation were both <10%. Plasma IL-6 concentration was measured in non-diluted plasma samples using an ELISA kit (abcam, catalog number ab 100772) validated in rats, with a sensitivity of 30 pg/ml and a detection range of 41–10,000 pg/ml. Intra-assay CV was <10% and inter-assay CV <12%. All ELISA kits were used according to the manufacturer’s instructions.
Assessment of EPO gene expression by quantitative polymerase chain reaction (qPCR)
Reverse transcription of total RNA followed by qPCR was used to evaluate gene expression as reported in early experiments.9 Total RNA was isolated from sampled kidney (right) and liver snap-frozen in liquid nitrogen using the RNeasy Fibrous Tissue Mini Kit (Qiagen Inc., Toronto, Canada), as per the manufacturer’s protocol. One µg of total RNA was reverse transcribed using the Omniscript RT Kit (Qiagen Inc., Hilden, Germany) and qPCR was performed using SYBER Green PCR Master Mix (Applied Biosystems by ThermoFisher, Carlsbad, CA) with a LightCycler 96 from Roche PCR cycler (Roche Life Sciences, Penzerb, Germany). EPO cDNA was amplified in the following conditions: DNA was denatured for 10 min at 95 °C followed by 45 15-s cycles of denaturation at 95 °C and annealing/elongation at 60 °C for 1 min. The 40S ribosomal protein S16 (Rps16) was used as internal control.
Assessment of protein expression by western blot
Right kidney tissue was homogenized in lysis buffer (RIPA) supplemented with protease inhibitors (Na-deoxycholate 10%, EDTA 100 mM, sodium dodecyl sulfate 10%, cOmplete mini 0.05×; Roche, Germany), phenylmethanesulfonylfluoride 100 mM, Igepal), in the Precellys-24 tissue homogenizer (Bertin Instruments, Montigny-le-Bretonneux, France) and protein concentration was measured by Bradford as earlier experiments.9
Proteins extracted from the right kidney (40 µg) tissue were subjected to one-dimensional polyacrylamide gel electrophoresis (Invitrogen by ThermoFisher Bolt 4–12% Bis-Tris Plus, Carlsbad, CA). Immunodetection steps were processed using a primary antibody against vascular endothelial growth factor A (VEGF-A; 1/1000 dilution in 3% bovine serum albumin (BSA), ab231260, Abcam, Cambridge, MA) and glyceraldehyde 3-phosphate dehydrogenase (GAPDH; sc-20357, 1/1000 dilution in 3% BSA, Santa Cruz Biotechnology, Santa Cruz, CA) as a control for normalization. Bands were developed with an enhanced chemiluminescence substrate (PerkinElmer Inc., Waltham, MA) on a documentation system (Syngene, G:BOX, Cambridge, UK) and quantified using Image J (NIH). For VEGF-A, we used the average of 3 bands at 22, 35, and 45 kDa per the manufacturer’s instruction and provide the whole blots in Supplemental Figures. Results are shown as a ratio of VEGF-A/GAPDH. Equal protein loading was verified with Ponceau red stain.
Data analysis
Data are presented as mean ± standard deviation, and distribution of the data is shown in the figures as boxplots. Normality was assessed visually and using Kolmogorov–Smirnov test. Comparisons between groups were performed using a two-way analysis of variance to estimate the mean quantitative variable changes according to the levels of two independent variables (oxygen exposure and sex) and the interaction between these variables. The interaction term was removed from the model when non-significant. P values < 0.05 were considered statistically significant. Number of animals involved, as well as raw data for all figures, are provided as Supplemental Data. All analyses were performed using R version 3.6.0 (International Open Source collaborative).13
Results
Baseline characteristics
As previously reported,11 exposure to oxygen from 3 to 10 days of life (hyperoxia) did not alter male or female pup growth, with similar body weight in both groups at 10 and 28 days of life (Fig. 1). Pup survival to 28 days of life was >95% in both groups.
Body weight was obtained at (a) 10 and (b) 28 days of life. C: control group (open circles), H: animals exposed to hyperoxia from 3 to 10 days of life (open triangles). N = 9–13 per group. P values were determined using a two-way ANOVA. Psex, Pexposure, and Psex × expo represent the respective P values for the effect of sex, exposure, and the interaction between sex and exposure.
Hemoglobin and RBCs are altered by neonatal hyperoxia
Neonatal exposure to high level of oxygen induced lower level of hemoglobin with smaller RBCs, without an increase in reticulocytes at 10 days of life in rodents. We found significantly lower hemoglobin in the hyperoxia group, compared to the normoxia group, both in males (70 ± 3 versus 78 ± 2 g/l) and in females (71 ± 2 versus 81 ± 3 g/l). Mean cellular volume (MCV) was also lower in the hyperoxia group, while reticulocyte count and reticulocyte hemoglobin content were similar between groups. At 28 days of life, hemoglobin, MCV, reticulocyte count, and reticulocyte hemoglobin content were similar between groups (Fig. 2).
Hemoglobin at a 10 and b 28 days of life; mean cellular volume (MCV) at c 10 and d 28 days of life; reticulocyte count at e 10 and f 28 days of life; reticulocyte hemoglobin content at g 10 and h 28 days of life. C: control group (open circles), H: animals exposed to hyperoxia from 3 to 10 days of life (open triangles). N = 7–13 per group. P values were determined using a two-way ANOVA. Psex, Pexposure, and Psex × expo represent the respective P values for the effect of sex, exposure, and the interaction between sex and exposure.
Hormonal and biochemical changes associated with neonatal hyperoxia
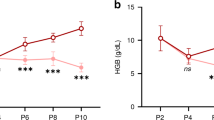
Circulating EPO levels were lower at 10 days of life in the animals exposed to hyperoxia, both in males (33 ± 7 versus 73 ± 6 pg/ml) and in females (37 ± 5 versus 66 ± 3 pg/ml), but were similar at 28 days of life. Similarly, ferritin levels were lower at 10 days of life, but not at 28 days of life, in both male and female animals exposed to hyperoxia. Expression of VEGF-A, a protein induced by hypoxia14 and downregulated by hyperoxia,15 was decreased in the kidneys of rats exposed to hyperoxia at 10 days of life. In contrast, we found a trend toward a mild increase in kidney VEGF-A expression in the hyperoxia group, compared to the control group, at 28 days of life (Fig. 3 and Supplemental Fig. 1).
Plasma erythropoietin (EPO) at (a) 10 and (b) 28 days of life; plasma ferritin at (c) 10 and (d) 28 days of life; ratio of densitometric analysis of vascular endothelial growth factor A (VEGF-A)/GAPDH, used as a loading control, measured in the kidney at (e) 10 and (f) 28 days of life. C: control group (open circles), H: animals exposed to hyperoxia from 3 to 10 days of life (open triangles). N = 4–5 per group. P values were determined using a two-way ANOVA. Psex, Pexposure, and Psex × expo represent the respective P values for the effect of sex, exposure, and the interaction between sex and exposure.
Increase in markers of inflammation associated with neonatal hyperoxia
Platelet count did not differ between groups. We found a higher white blood cell count in rats exposed to hyperoxia, and this difference was not observed at 28 days of life. We also found increased plasma IL-6 levels in the hyperoxia group at 10 days of life, while IL-6 levels were below the detection limit (40 pg/ml) in all animals from both groups at 28 days of life (Fig. 4).
Platelet count at (a) 10 and (b) 28 days of life; white blood cell (WBC) count at (c) 10 and (d) 28 days of life; e plasma interleukin-6 (IL-6) measured at 10 days of life. C: control group (open circles), H: animals exposed to hyperoxia from 3 to 10 days of life (open triangles). N = 7–13 per group. P values were determined using a two-way ANOVA. Psex, Pexposure, and Psex × expo represent the respective P values for the effect of sex, exposure, and the interaction between sex and exposure.
EPO expression in the kidney and the liver
Kidney EPO expression was decreased in the hyperoxia group at 10 days of life, while we found no difference in the expression of EPO in the liver between groups. Sex did not influence the expression of EPO in the kidney or in the liver (Fig. 5).
EPO expression, measured by qPCR, measured at 10 days of life in the kidney (a) and in the liver (b); C: control group (open circles), H: animals exposed to hyperoxia from 3 to 10 days of life (open triangles). N = 9 per group. P values were determined using a two-way ANOVA. Psex, Pexposure, and Psex × expo represent the respective P values for the effect of sex, exposure, and the interaction between sex and exposure.
Discussion
In this study, we explored neonatal erythropoiesis in rats exposed to high levels of oxygen in the neonatal period, a model that recapitulates some of the conditions associated with preterm birth. We found that neonatal exposure to high levels of oxygen was associated with lower hemoglobin levels without increase in reticulocyte count, smaller RBCs, lower EPO and ferritin levels, increased systemic inflammation, and lower VEGF-A expression in the kidney at 10 days of life. All these abnormalities were corrected at 28 days of life. EPO expression in the kidney, but not in the liver, was decreased following exposure to neonatal hyperoxia.
Anemia of prematurity is very common in extremely preterm neonates. Previous studies in the late 1990s have reported rates of transfusions as high as 80% in infants born <1500 g and 95% in infants born <1000 g.3 Low oxygen tension is a key regulator of erythropoiesis,16 but whether oxygen supplementation is independently associated with decreased erythropoiesis could not be determined by retrospective observational clinical studies. We, thus, measured parameters of erythropoiesis in rats exposed to high levels of oxygen in the neonatal period. As opposed to humans, organ development is not complete at birth in rodents.17 This rodent model therefore is clinically relevant, reproducing some of the complications that are associated with preterm birth.9,18,19,20 However, because we did not perform any blood draw prior to sacrifice, and the rats did not present other complications of preterm birth such as sepsis and necrotizing enterocolitis, we could specifically study the effect of increased oxygen tension on erythropoiesis.
Similarly to what is observed in human neonates born preterm, we found that rats exposed to hyperoxia had a significantly lower hemoglobin level, both in males and females. Previous studies have shown that EPO production in response to low hemoglobin levels is decreased in preterm infants compared to full-term infants,4 while their erythroid progenitors remain highly sensitive to EPO,21 suggesting that EPO deficiency, but not resistance to EPO, contributes to anemia of prematurity.
In our study, we show that neonatal exposure to high levels of oxygen resulted in decreased plasma EPO levels in rodents, and reticulocyte count was not increased, thus reproducing the non-regenerative anemia observed in human preterm neonates.
We previously reported that hyperoxia in rodents decreased levels of hypoxia-induced factor 1 expression during the hyperoxia period.22 Similarly, in our study, kidney VEGF-A expression was decreased at 10 days of life. However, we found a trend toward an increase in VEGF-A at 28 days of life in the hyperoxia group. Hypoxia was shown to increase VEGF-A expression in the inner medulla of the kidney.23 Considering that neonatal hyperoxia impairs nephrogenesis, changes in VEGF-A expression in the kidney in time following neonatal hyperoxia exposure may reflect an ensuing relative state of tissue hypoxia at the level of the kidneys. Although we did not observe any significant difference at 28 days of life in hemoglobin and in plasma EPO levels between groups, these results may explain previous reports from our group and others of increased hemoglobin levels in children24 and adults25 born very preterm that were associated with EPO levels similar to those of subjects born term, reflective of a relative excessive EPO production for a given hemoglobin.25 Whether an increase in circulating EPO and hemoglobin levels would also be observed later in life in this rodent model remains to be assessed.
We further found that plasma ferritin levels were decreased in animals exposed to hyperoxia, which may explain the microcytosis observed in the complete blood count. Low plasma ferritin reflects low iron store and iron deficiency is a common feature of the anemia of prematurity usually attributed to insufficient intake and blood losses rather than supplemental oxygen. Current results are consistent with the fact that the effect of iron on ferritin synthesis is highly dependent on oxygen tension. Indeed, a study showed in mouse peritoneal macrophages that, while iron strongly induced ferritin synthesis in hypoxia (2% oxygen), this effect was blunted in hyperoxic conditions (80% oxygen).26 Considering that reticulocyte hemoglobin content was similar between groups, both at 10 and 28 days of life, these results suggest that EPO deficiency may have a larger role than iron deficiency/unavailability in the lower hemoglobin levels observed in the animals exposed to high levels of oxygen.
EPO originates from the liver and the kidneys, both in humans and in rats. While the transition from a predominantly hepatic to renal production occurs in utero between gestational ages 30 and 40 weeks in humans,27 this switch is observed within the first days of life in rodents.28 We thus investigated whether the decrease in EPO production was due to a decrease in EPO expression in the kidneys, the liver, or both and found lower EPO expression in the kidneys but not in the liver at 10 days of life in animals exposed to hyperoxia. This is in line with the fact that liver EPO production is less sensitive to oxygen tension than kidney production.29
Very preterm birth is associated with increased systemic oxidative stress30 and inflammation31 during the neonatal period in humans. Whereas newborn rats have a mature antioxidant system at their birth,32 in this experimental model, we previously reported in the heart of hyperoxia-exposed rats an increase in the expression of toll-like receptor 4, which is involved in inflammation and oxidative stress signaling, as well as an increase in the expression of pro-inflammatory cytokines IL-1β and IL-18, that was observed both at 10 days and 12 weeks of life.18 In the lungs, a previous study found an increase in lung mRNA chemokines monocyte chemoattractant protein-1, macrophage inflammatory protein-2, and interferon gamma-induced protein-10 immediately following neonatal exposure to hyperoxia in mice.33 In the current study, we found an increase in white blood cell count and IL-6, which are markers of systemic inflammation, at 10 days of life, suggesting that exposure to supplemental oxygen could participate to the inflammatory status observed in preterm neonates. We did not find a persistent systemic inflammation at 28 days of life, as opposed to the persistent inflammation observed in the myocardium at 12 weeks of life in this model.18 These results are consistent with those found in human young adults born very preterm, who did not display an increase in systemic inflammation despite a high prevalence of cardiovascular risk factors.34
Various experimental protocols have been used to reproduce the adverse conditions of preterm birth. In the study by Shaffer et al., animals exposed from 1 to 8 days of life to 96–100% FiO2 displayed pulmonary and vascular changes that resembled bronchopulmonary dysplasia.8 In a study by Goss et al.,35 animals exposed from 1 to 10 days of life to 90% FiO2 displayed elevated RV systolic pressure. Kumari et al.20 exposed neonatal rats from 1 to 14 days of life to 85% FiO2 and showed severe pulmonary hypertension and RV dysfunction. In this research, we used a model of neonatal exposure from 3 to 10 days of life to 80% FiO2. We have previously shown in this model cardiac9,12,18,36 and vascular10,37 abnormalities, compared to control animals, that were very similar to the alterations found by Benny et al.38 who used a different experimental protocol of exposure to high levels of O2 (85% FiO2 for 3 weeks, from day 1 to day 22 of life). In this experimental model, the high levels of oxygen exposure (80–100% FiO2 depending on the study) aim to mimic the supraphysiological levels of exposure to breathing and circulating oxygen concentration experienced by preterm neonates upon birth compared to much lower fetal levels. Overall, these studies show that neonatal exposure of rats to high levels of oxygen, despite slight changes in the duration and intensity of exposure, all lead to similar and reproducible alterations that closely reproduce pulmonary and cardiovascular changes observed in humans born preterm, both in the neonatal period39 and later in life.40,41,42,43,44
This study has several limitations. First, only one condition of neonatal exposure to high levels of oxygen (80% O2 from P3 to P10) was used in this study. However, other groups who used different models of exposure have found similar outcomes in terms of cardiac and vascular function,38 suggesting that neonatal exposure to high levels of oxygen result in specific abnormalities that are consistent independently of minor changes in the exposure protocol. Second, we did not measure EPO-R expression in the erythroid progenitors, and thus we cannot rule out a reduced expression of EPO-R that would result in a lower sensitivity of erythroid progenitors to EPO, that may also contribute to decreased hemoglobin levels.
In conclusion, exposure to high levels of oxygen during the neonatal period, recapitulating preterm birth deleterious conditions, induced in rodents a decrease in hemoglobin levels, associated with reduced ferritin, increased systemic inflammation, and EPO deficiency due to decreased kidney EPO production, and therefore reproduced the main characteristics of the anemia of prematurity observed in humans born extremely preterm. Whether neonatal exposure of immature erythropoietic system to supraphysiological oxygen levels contributes to longer-term reprogramming of erythropoiesis observed in children and adults born preterm remains to be evaluated.
Data availability
Raw data are available in Supplemental Materials.
References
Shah, P. S. et al. The Canadian Preterm Birth Network: a study protocol for improving outcomes for preterm infants and their families. CMAJ Open 6, E44–E49 (2018).
Helenius, K. et al. Survival in very preterm infants: an international comparison of 10 national neonatal networks. Pediatrics 140, e20171264 (2017).
Widness, J. A. et al. Changing patterns of red blood cell transfusion in very low birth weight infants. J. Pediatr. 129, 680–687 (1996).
Stockman, J. A. et al. Anemia of prematurity: determinants of the erythropoietin response. J. Pediatr. 105, 786–792 (1984).
Lundby, A.-K. M., Keiser, S., Siebenmann, C., Schäffer, L. & Lundby, C. Kidney-synthesized erythropoietin is the main source for the hypoxia-induced increase in plasma erythropoietin in adult humans. Eur. J. Appl. Physiol. 114, 1107–1111 (2014).
Balestra, C., Germonpré, P., Poortmans, J. R. & Marroni, A. Serum erythropoietin levels in healthy humans after a short period of normobaric and hyperbaric oxygen breathing: the ‘normobaric oxygen paradox’. J. Appl Physiol. 100, 512–518 (2006).
Keramidas, M. E. et al. Acute normobaric hyperoxia transiently attenuates plasma erythropoietin concentration in healthy males: evidence against the ‘normobaric oxygen paradox’ theory. Acta Physiol. 202, 91–98 (2011).
Shaffer, S. G., O’Neill, D., Bradt, S. K. & Thibeault, D. W. Chronic vascular pulmonary dysplasia associated with neonatal hyperoxia exposure in the rat. Pediatr. Res. 21, 14–20 (1987).
Bertagnolli, M. et al. Transient neonatal high oxygen exposure leads to early adult cardiac dysfunction, remodeling, and activation of the renin-angiotensin system. Hypertension 63, 143–150 (2014).
Huyard, F. et al. Remodeling of aorta extracellular matrix as a result of transient high oxygen exposure in newborn rats: implication for arterial rigidity and hypertension risk. PLoS ONE 9, e92287 (2014).
Sutherland, M. R. et al. Age- and sex-related changes in rat renal function and pathology following neonatal hyperoxia exposure. Physiol. Rep. 4, e12887 (2016).
Yzydorczyk, C. et al. Neonatal oxygen exposure in rats leads to cardiovascular and renal alterations in adulthood. Hypertension 52, 889–895 (2008).
R Core Team. R: A Language and Environment for Statistical Computing (R Foundation for Statistical Computing, 2019).
Minchenko, A., Bauer, T., Salceda, S. & Caro, J. Hypoxic stimulation of vascular endothelial growth factor expression in vitro and in vivo. Lab. Invest. 71, 374–379 (1994).
Dong, D. et al. Hyperoxia sensitizes hypoxic HeLa cells to ionizing radiation by downregulating HIF‑1α and VEGF expression. Mol. Med. Rep. 23, 62 (2021).
Stockmann, C. & Fandrey, J. Hypoxia-induced erythropoietin production: a paradigm for oxygen-regulated gene expression. Clin. Exp. Pharmacol. Physiol. 33, 968–979 (2006).
Clubb, F. J. & Bishop, S. P. Formation of binucleated myocardial cells in the neonatal rat. An index for growth hypertrophy. Lab. Invest. 50, 571–577 (1984).
Mian, M. O. R. et al. TLR (toll-like receptor) 4 antagonism prevents left ventricular hypertrophy and dysfunction caused by neonatal hyperoxia exposure in rats. Hypertension 74, 843–853 (2019).
Ladha, F. et al. Sildenafil improves alveolar growth and pulmonary hypertension in hyperoxia-induced lung injury. Am. J. Respir. Crit. Care Med. 172, 750–756 (2005).
Kumari, S. et al. Bimodal right ventricular dysfunction after postnatal hyperoxia exposure: implications for the preterm heart. Am. J. Physiol. Heart Circ. Physiol. 317, H1272–H1281 (2019).
Rhondeau, S. M., Christensen, R. D., Ross, M. P., Rothstein, G. & Simmons, M. A. Responsiveness to recombinant human erythropoietin of marrow erythroid progenitors from infants with the ‘anemia of prematurity’. J. Pediatr. 112, 935–940 (1988).
Popescu, C. R. et al. Hyperoxia exposure impairs nephrogenesis in the neonatal rat: role of HIF-1α. PLoS ONE 8, e82421 (2013).
Marti, H. H. & Risau, W. Systemic hypoxia changes the organ-specific distribution of vascular endothelial growth factor and its receptors. Proc. Natl Acad. Sci. USA 95, 15809–15814 (1998).
Pechlaner, R. et al. Very preterm birth results in later lower platelet activation markers. Pediatr. Res. https://doi.org/10.1038/s41390-020-1070-8 (2020).
Flahault, A. et al. Duration of neonatal oxygen supplementation, erythropoiesis and blood pressure in young adults born preterm. Thorax 75, 494–502 (2020).
Kuriyama-Matsumura, K., Sato, H., Suzuki, M. & Bannai, S. Effects of hyperoxia and iron on iron regulatory protein-1 activity and the ferritin synthesis in mouse peritoneal macrophages. Biochim. Biophys. Acta 1544, 370–377 (2001).
Dame, C. et al. Erythropoietin mRNA expression in human fetal and neonatal tissue. Blood 92, 3218–3225 (1998).
Clemons, G. K., Fitzsimmons, S. L. & DeManincor, D. Immunoreactive erythropoietin concentrations in fetal and neonatal rats and the effects of hypoxia. Blood 68, 892–899 (1986).
Tan, C. C., Eckardt, K. U., Firth, J. D. & Ratcliffe, P. J. Feedback modulation of renal and hepatic erythropoietin mRNA in response to graded anemia and hypoxia. Am. J. Physiol. 263, F474–F481 (1992).
Mestan, K. et al. Cord blood 8-isoprostane in the preterm infant. Early Hum. Dev. 88, 683–689 (2012).
Romero, R. et al. Evidence of perturbations of the cytokine network in preterm labor. Am. J. Obstet. Gynecol. 213, 836.e1–836.e18 (2015).
Tanswell, A. K. & Freeman, B. A. Pulmonary antioxidant enzyme maturation in the fetal and neonatal rat. I. Developmental profiles. Pediatr. Res. 18, 584–587 (1984).
D’Angio, C. T., Johnston, C. J., Wright, T. W., Reed, C. K. & Finkelstein, J. N. Chemokine mRNA alterations in newborn and adult mouse lung during acute hyperoxia. Exp. Lung Res. 24, 685–702 (1998).
Flahault, A. et al. Increased incidence but lack of association between cardiovascular risk factors in adults born preterm. Hypertension 75, 796–805 (2020).
Goss, K. N. et al. Neonatal hyperoxic lung injury favorably alters adult right ventricular remodeling response to chronic hypoxia exposure. Am. J. Physiol. Lung Cell. Mol. Physiol. 308, L797–L806 (2015).
Bertagnolli, M. et al. Activation of the cardiac renin-angiotensin system in high oxygen-exposed newborn rats: angiotensin receptor blockade prevents the developmental programming of cardiac dysfunction. Hypertension 67, 774–782 (2016).
Mivelaz, Y. et al. Neonatal oxygen exposure leads to increased aortic wall stiffness in adult rats: a Doppler ultrasound study. J. Dev. Orig. Health Dis. 2, 184–189 (2011).
Benny, M. et al. Neonatal hyperoxia exposure induces aortic biomechanical alterations and cardiac dysfunction in juvenile rats. Physiol. Rep. 8, e14334 (2020).
Altit, G., Bhombal, S., Feinstein, J., Hopper, R. K. & Tacy, T. A. Diminished right ventricular function at diagnosis of pulmonary hypertension is associated with mortality in bronchopulmonary dysplasia. Pulm. Circ. 9, 2045894019878598 (2019).
Telles, F. et al. Changes in the preterm heart from birth to young adulthood: a meta-analysis. Pediatrics 146, e20200146 (2020).
Lewandowski, A. J. et al. Right ventricular systolic dysfunction in young adults born preterm. Circulation 128, 713–720 (2013).
Flahault, A. et al. Arterial structure and stiffness are altered in young adults born preterm. Arterioscler. Thromb. Vasc. Biol. https://doi.org/10.1161/ATVBAHA.120.315099 (2020).
Dartora, D. R. et al. Association of bronchopulmonary dysplasia and right ventricle systolic function in young adults born preterm. Chest https://doi.org/10.1016/j.chest.2021.01.079 (2021).
Flahault, A. et al. Left ventricle structure and function in young adults born very preterm and association with neonatal characteristics. J. Clin. Med. 10, 1760 (2021).
Acknowledgements
The authors would like to thank the staff of the animal facility of the Sainte Justine Research Center for their support.
Funding
This work was supported by a Fonds de recherche du Québec – Santé (FRQS)/Fondation des Étoiles fellowship award to A.F. DRD was awarded fellowships from the Société Québecoise d’Hypertension Artérielle, Canadian Vascular Network, and FRQS. C.N.R.P. received a visiting research fellowship from Coordenação de Aperfeiçoamento de Pessoal de Nível Superior – Brazil (CAPES – process number 23038.017466/2018-50).
Author information
Authors and Affiliations
Contributions
A.F., D.R.D., C.N.R.P., and Y.H. performed research. A.F. performed data analysis. A.F. and A.M.N. wrote the first version of the manuscript. A.F., C.L., T.M.L., and A.M.N. participated in the interpretation of the results. T.M.L. and A.M.N. supervised the study. All authors revised the manuscript.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethics approval and consent to participate
Patient consent was not required for this study, as it did not involve human participants.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Flahault, A., Dartora, D.R., Pontes, C.N.R. et al. Exposure to high levels of oxygen in neonatal rats induce a decrease in hemoglobin levels. Pediatr Res 92, 430–435 (2022). https://doi.org/10.1038/s41390-021-01802-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41390-021-01802-1