Abstract
Recently identified regulatory PMN control immune-driven dry eye disease (DED) in females by producing the arachidonic acid (ω-6)-derived specialized pro-resolving mediator (SPM), LXA4, in lymph nodes. Dietary ω-3 docosahexaenoic acid (DHA) is protective in DED but mechanisms of action remain elusive. DHA is converted to ω-3 SPMs by PMN via the same lipoxygenases (LOX) that generate LXA4. We investigated if dietary DHA amplifies SPM formation and affects T effector cell function and/or regulatory PMN in DED. DED was induced in mice on a DHA-enriched or ω-3-deficient diet. DHA deficiency amplified DED with marked sex-specific differences. Dietary DHA protection against dry eye disease correlated with increased PMN levels in lymph nodes, ocular tissues, and unexpectedly, selective amplification of LXA4 tissue levels. Dietary DHA increased 12/15-LOX and decreased 5-LOX expression in lymph nodes and isolated lymph node PMN, which correlated with amplified LXA4 formation. Acute DHA treatment rescued DHA-deficient females from exaggerated DED by amplifying lymph node LXA4 formation, increasing Treg and decreasing TH1 and TH17 effector cells. Our results identify DHA regulation of LXA4 producing PMN in ocular tissues and lymph nodes in health and immune disease as novel mechanism and determinant for T-cell responses to routine ocular injury or stress signals.
Similar content being viewed by others
Introduction
Paucity of dietary omega-3 polyunsaturated fatty acids (ω-3 PUFAs) correlates with higher incidence of diseases with an inflammatory component. Epidemiological, clinical, and/or animal studies provide strong evidence that dietary ω-3 PUFAs are protective in inflammatory and autoimmune diseases,1,2 which include diseases such as dry eye diseases and age-related macular degeneration.3,4,5,6 Docosahexaenoic acid (DHA) is the most abundant and terminal ω-3 PUFA and it is highly enriched in the brain, retina, and testis. The protective actions of dietary DHA in part have been attributed to formation of specialized pro-resolving lipid mediators (SPMs), namely resolvins, protectins, and maresins.7,8,9,10 These SPMs are generated primarily by the coordinated interaction of 5-lipoxygenase (LOX) and 12/15-LOX, two enzymes that are also essential for the formation of the founding member of the SPM family,11 namely the eicosanoid lipoxin A4 (LXA4), which is an arachidonic acid (ω-6 PUFA) product.
Increasing evidence indicates that tissue-resident SPM circuits are key factors in maintaining health in the eye’s immune-privileged tissues such as the cornea.7 The cornea is of particular interest as the corneal epithelium expresses an endogenous LXA4 circuit that regulates leukocyte function and epithelial wound healing. Treatment with LXA4 and ω-3-derived SPMs protects against inflammation and drives epithelial wound healing in the cornea.7,12 A key enzyme for LXA4 formation and for many DHA-derived SPM is 12/15-LOX (Alox15).7,13 Downregulation of 15-LOX and LXA4 formation in the cornea by estrogen has been identified as a factor for sex-specific difference in acute inflammation and wound healing in females.14,15,16 Immune-driven dry eye diseases (DEDs), such as Sjögren’s syndrome, is a ocular surface diseases with a striking 80% female prevalence. The etiology of immune-driven DED is unknown, but it is a chronic autoimmune disease that triggers T effector cell-driven responses against self-antigens in the lacrimal gland, goblet cells, ocular surface, and conjunctiva. We recently identified a 15-LOX-expressing population of regulatory polymorphonuclear neutrophils (PMN) that resides in draining lymph nodes, lacrimal glands, and the corneal limbus that generates LXA4.14 In females this population of LXA4-producing PMN is selectively regulated compared to males and their depletion causes a female-specific amplified TH1 and TH17 response and increased DED.
DHA-derived SPM resolvin D1 is a structural homolog of LXA4 and both mediated their action via FPR2/ALX in mice and humans. Topical and dietary DHA are protective in mouse models of dry disease.6,17,18,19 A likely mechanism for the protective actions of DHA in the eye and other organs is amplification of endogenous DHA-SPMs. It is unknown if dietary or topical DHA impacts T effector cell function or the recently identified tissue-resident regulatory PMN in immune-driven eye diseases. To this end, we placed mice on DHA-enriched or matched DHA-deficient diet and investigated the impact of dietary DHA on DED, SPM tissue levels, T effector cells, and regulatory PMN. Here we report that dietary DHA sex-specifically inhibits T effector cells and reduces DED. Unexpectedly, dietary and acute treatment with DHA did not markedly amplify DHA-series SPM but predominantly increased tissue levels of the eicosanoid SPM LXA4 and caused a marked increase in LXA4-producing PMNs in lymph nodes and expression of 12/15-LOX. Our findings identify a new mechanism of action for dietary DHA, namely amplification of an ω-6 SPM circuit.
Results
Dietary DHA is a determinant for the severity of DED in male and female mice
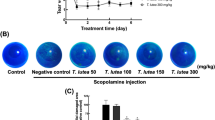
Effect of dietary DHA on dry eye pathogenesis was evaluated in an established mouse model of aqueous tear-deficient desiccating stress, which recapitulates key features of human autoimmune DED. Mice were placed on a balanced open source (AIN-76A, 6.2% fat) DHA-enriched (60% soybean oil and 40% DHA) or DHA-deficient (100% soybean oil) rodent diet 4 weeks prior to initiating desiccating stress and dry eye pathogenesis. Clinical fluorescence scoring (Fig. 1a, n = 10) demonstrated that epithelial defect after 10 days of desiccating stress was significantly amplified in mice on the DHA-deficient diet. Diet-induced exacerbation of dry eye pathogenesis (epithelial defect) was significantly greater (p = 0.0002) in females (clinical score = 10.2 ± 0.4) than males (clinical score 7.4 ± 0.4). The DHA diet group showed marked reduction in epithelial defect by 50.8 ± 5.9% (p < 0.0001) and 24.9 ± 7.6% (p = 0.0041) in females and males respectively, when directly compared to the DHA-deficient diet (Fig. 1a). A key feature of DED is the sex-specific difference that leads to amplified pathogenesis and effector T-cell responses in female mice.14 Hence, it is striking that dietary DHA eliminated sex-specific differences in dry eye-induced epithelial defects (Fig. 1a). Tear levels measured by Schirmer’s test (n = 10) confirmed desiccating stress. More importantly, only female mice in the DHA-enriched diet group (0.7 ± 0.18 mm) showed improved tear production (0.15 ± 0.07 mm) (Fig. 1b) after 10 days of desiccating stress. Our standard desiccating stress model uses scopolamine, a cholinergic antagonist, to inhibit lacrimal gland function. Cholinergic regulation of goblet cell-associated passages (GAPs) has recently been identified as an important mechanism for maintaining ocular surface immune tolerance.20 We did not investigate if dietary DHA regulates GAPs.
Dietary DHA is a determinant for the severity of dry eye disease in male and female mice. Age-matched male and female C57BL/6J mice were place on a balanced DHA-enriched or DHA-deficient diet for 4 weeks prior to initiating desiccating stress. Desiccating stress consisted of scopolamine injections to reduce tear flow and housing in low-humidity environmental cubical with high airflow for 10 days. Images are representative fluorescein-stained corneas from females in each diet group. a Corneal epithelial defect, a marker of dry eye diseases severity, was assessed and quantified by clinical fluorescence scoring (n = 10) in healthy controls (no desiccating stress) and mice after 10 days of desiccating stress. b Tear production was measured by Schirmer’s test (n = 10). #P < 0.05, healthy versus dry eye; *P < 0.05, DHA-enriched versus DHA-deficient
Dietary DHA regulates tissue levels of the eicosanoid SPM LXA4 in healthy tissues
Dietary DHA modulates eicosanoid formation and can amplify ω-3 PUFA SPM pathways.10,21 Lipid mediator profiles of plasma (n = 4), corneas (n = 6), lacrimal glands (n = 6), and draining lymph nodes (n = 6) were established by liquid chromatography/tandem mass spectrometry (LC/MS/MS)-based lipidomics in healthy male and female mice on the DHA-deficient or DHA-enriched diet. DHA-SPM pathway markers 17-HDHA and 14-HDHA were significantly increased in all tissues but ω-3 PUFA-derived SPM (maresins, resolvins, and protectins) were below the limits of quantification for our instrument (AB SCIEX QTRAP 3200). Unexpectedly, dietary DHA significantly increased levels of the SPM eicosanoid LXA4 in males and females (Fig. 2a–c). LXA4 was identified by retention time, co-elution with deuterated internal standard, multiple reaction monitoring (MRM) of product ions and quantification of five diagnostic transitions.14 In females, dietary DHA increased LXA4 levels in plasma from below limits of detection to 325 ± 35 pg/200 μl, by 190 ± 41% in the cornea, by 150 ± 46% in the lacrimal gland, and by 194 ± 79% in draining lymph nodes. The effect of dietary DHA on eicosanoid levels was sex- and tissue-specific. LXA4 levels were significantly higher in male plasma and cornea compared to matched females, while females had significantly higher LXA4 levels in lacrimal glands and draining lymph nodes. The most striking sex-specific differences in LXA4 levels were observed in plasma where males had markedly higher levels of LXA4 both in the DHA-deficient (females = 0 ± 0 pg/200 μl versus males = 617 ± 161 pg/200 μl) and DHA-enriched diet (females = 325 ± 35 pg/200 μl versus males = 1248 ± 242 pg/200 μl). A similar marked sex-specific difference was observed for the PMN and lymphocyte chemoattractant LTB4. In both diet groups LTB4 was only present in the plasma of females but not males. The DHA-deficient diet significantly amplified (p = 0.049) female LTB4 plasma levels by 3.9-fold from 103 ± 26 pg/200 μl to 505 ± 204 pg/200 μl (Fig. 2a).
Dietary DHA regulates tissue levels and PMN production of the eicosanoid SPM LXA4 in healthy mice. Endogenous LXA4 and LTB4 tissue levels in plasma, cornea, lacrimal gland, and draining lymph nodes of healthy mice (males and females) on a DHA-enriched or DHA-deficient diet was quantified by LC/MS/MS-based lipidomics. a LXA4 and LTB4 plasma levels (n = 4). b LXA4 tissue levels (n = 6) in corneas, lacrimal glands, and draining lymph nodes. c PMN from draining lymph nodes were isolated from healthy males and females on the DHA-enriched or DHA-deficient diets. PMNs were activated with calcium ionophore at 37 °C for 15 min and endogenous LXA4 and LTB4 formation quantified by LC/MS/MS-based lipidomics (n = 5, pg/1 × 105 PMN). d qPCR analysis of 5-LOX and 15-LOX RNA expression in lymph node PMN (n = 4). a–d Values represent the mean ± SEM. *P < 0.05, DHA-enriched versus DHA-deficient; #P < 0.05, female versus male
Dietary DHA regulates the LXA4 circuit in resident lymph node PMN
Regulatory PMNs are resident in ocular tissues and draining lymph nodes.14 These regulatory PMNs highly express 15-LOX and have a high capacity of generating LXA4 compared to vascular inflammatory PMN.14 We isolated lymph node PMNs and activated them with calcium ionophore to determine if dietary DHA regulates their capacity for LXA4 and LTB4 generation. Lipidomic analysis established the endogenous formation of LXA4 and LTB4 by lymph node PMN from healthy male and female mice in both diet groups (Fig. 2c). Dietary DHA correlated with a marked increase in LXA4 formation by lymph node PMN from male and female mice, evidenced by a 2.8 ± 0.9-fold (p = 0.0018) and 4.6 ± 1.4 fold (p = 0.0027) increase, respectively. By contrast, DHA deficiency correlated with a marked increase in LTB4 formation in lymph node PMN in males (345% increase, p = 0.0110) and females (124% increase, p = 0.0273) compared to mice on the DHA-enriched diet. More importantly, LTB4 formation in lymph node PMN from females was 161 ± 68% higher compared to matched males in the DHA-deficient diet groups. LXA4 was the predominate LOX-derived eicosanoid generated by lymph node PMN in all DHA diet groups. PMN from females and males produced 567 and 851 pg of LXA4 in comparison to 73 and 14 pg of LTB4, respectively.
To assess if dietary DHA had a significant effect on the expression of obligatory enzymes for lipoxin and/or leukotriene formation, we assessed RNA expression of 5-LOX (Alox5) and 12/15-LOX (Alox15) in lymph node PMN from healthy male and female mice in both diet groups (Fig. 2d). 5-LOX mRNA expression in PMN was significantly higher in females (108 ± 45%, p = 0.0075) in the DHA-deficient diet group, which correlated with amplified LTB4 formation (Fig. 2c). Consistent with the observed protective effects of dietary DHA, 5-LOX expression was abrogated in lymph node PMN from both males and females in the DHA-enriched diet group. 12/15-LOX mRNA expression, an obligatory enzyme for de novo LXA4 formation by PMN, was significantly higher in males compared to females in all diet groups. Dietary DHA reduced PMN 12/15-LOX expression in females by 55 ± 11% (p = 0.0002) and in sharp contrast markedly increased expression in males by 50 ± 20% (p = 0.0144). The results indicate that dietary DHA sex-specifically regulates 5-LOX (Alox5) and 12/15-LOX (Alox15) expression and LXA4 and LTB4 formation by lymph node PMN. Specifically, dietary DHA had a greater effect on male PMN in terms of amplifying Alox15 expression and LXA4 formation.
Sex-specific differences in regulation of tissue PMN levels by dietary DHA in health and DED
Tissue PMNs sex-specifically generate and regulate LXA4 tissue levels.14 To assess the impact of dietary DHA on these tissue PMNs they were quantified in healthy mice and 10 days after desiccating stress by immunohistochemistry (IHC) and myeloperoxidase (MPO) assay. CD45+/Ly6g+ PMNs were manually counted in sections of the limbus region of the cornea (Fig. 3a, b). IHC quantification (n = 6) demonstrated higher PMN numbers in the healthy limbus of males (p = 0.0074) and females (p < 0.0001) in the DHA diet group compared with the DHA-deficient diet group (Fig. 3a). PMN numbers in healthy female and male mice were higher by 114 ± 25% and 50 ± 18%, respectively, compared with the DHA-deficient diet group (Fig. 3a). Dietary DHA did not impact the number of PMN in the limbus of females. However, in male mice dietary DHA correlated with a 11 ± 2-fold increase in PMN in the limbus.
Sex-specific regulation of tissue PMN levels by dietary DHA in health and dry eye disease. Tissues were collected from males and females on the DHA-enriched or DHA-deficient diet. a IHC quantification of CD45+Ly6g+ PMN in flat-mounted corneas with limbus (n = 6). The total number of corneal PMN was counted in nine, ×40 fields of view that comprised the diameter of a cornea (from limbus to limbus). b Representative images of corneal limbus region measured with scale bars at 20 μm. PMN levels quantified by myeloperoxidase (MPO) activity (n = 6) in the lacrimal gland (c) and in the draining lymph nodes (d). *P < 0.05, DHA-enriched versus DHA-deficient, unpaired t test; #P < 0.05, female versus male
PMNs were quantified in the lacrimal glands and draining lymph nodes by measuring MPO activity (n = 6). There were marked sex-specific differences in PMN numbers in the lacrimal gland (Fig. 3c), which is a primary target for T cells in DED.22,23 In healthy females, unlike in males, DHA diet correlated with 2.1 ± 0.6-fold (p < 0.0001) increase in PMNs in the lacrimal glands compared to the DHA-deficient diet group. Desiccating stress in females eliminated the dietary effect of elevated lacrimal gland PMN as numbers returned to basal level (77 558 ± 22 067/10 mg). In males, the DHA-enriched diet did not result in higher PMN number in healthy mice, on the contrary PMN levels were lower compared to the DHA-deficient diet group. However, with desiccating stress lacrimal PMN levels in the DHA diet group increased by 64 ± 18% and were the same as in the DHA-deficient diet group. In draining lymph nodes (Fig. 3d) DHA diet correlated with marked increase in PMN levels in both females and males 110 ± 53% and 128 ± 70%, respectively (Fig. 3d). Dietary DHA further increased lymph node PMN levels in female mice by 76 ± 39% with DED. In contrast, in males DED had no impact on numbers of PMN in lymph nodes in either the DHA-deficient or DHA-enriched diet group.
Dietary DHA amplifies cornea and lymph node LXA4 circuits in DED
A key feature of dry eye pathogenesis is epithelial defect in the cornea (Fig. 1a). The healthy cornea highly expresses a 12/15-LOX-LXA4 protective circuit that promotes re-epithelialization and controls effector cell function.24,25,26 Impact of dietary DHA on expression and activity of the corneal 15-LOX/LXA4 circuit was assessed 10 days after initiating DEDs (Fig. 4). Dietary DHA markedly upregulated the primary 12/15-LOX DHA products 14-HDHA and 17-HDHA (Fig. 4a). 14-HDHA increased by 125 ± 37% and 1369 ± 620% and 17-HDHA increased by 225 ± 111% and 105 ± 61% in males and females, respectively. Despite dietary amplification of DHA-series SPM pathway markers (14-HDHA and 17-HDHA), resolvins, protectins, or maresins were not consistently detected in single mouse corneas. In health and DED PMNs are not an abundant cell type in the cornea and are largely restricted to the vascular limbus region14 but the mouse cornea and human corneal epithelial cells can generate LXA4 endogenously.15,24 Consistent with dietary DHA amplification of LXA4 in healthy mouse corneas, corneas from mice with DED on the DHA diet also demonstrated a marked upregulation of corneal LXA4 levels (Fig. 4a) in both males and females by 109 ± 39% and 480 ± 158% (p = 0.0038 and 0.0023), respectively. Dietary DHA deficiency correlated with a significant increase in expression of Alox5 and Alox15 in both males and females (Fig. 4b). Corneal expression of Alox5 and Alox15 was 1.6 ± 0.7 to 3.4 ± 1.2- and 2.2 ± 0.5 to 2.7 ± 1.0-fold higher (male–female), respectively, in the DHA-deficient versus the DHA-enriched diet group.
Dietary DHA amplifies cornea LXA4 circuits in dry eye disease. Corneas were isolated from males and females on the DHA-enriched or DHA-deficient diet after 10 days of desiccating stress (n = 5). Corneas were processed for lipidomic or qPCR analysis. a 12/15-LOX DHA-derived products and LXA4 levels (pg/cornea). b qPCR analysis of 5-LOX and 15-LOX RNA expression in corneas (n = 5). Values represent the mean ± SEM. *P < 0.05, DHA-enriched versus DHA-deficient, unpaired t test; #P < 0.05, female versus male
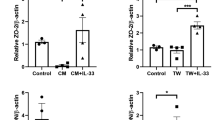
Regulatory PMN in draining lymph nodes generates significant levels of LXA4 (Fig. 2c). We next assessed the impact of dietary DHA on endogenous formation of lymph node LXA4 or DHA-derived SPM levels at the peak of DED (Fig. 5a). Dietary DHA markedly amplified 14-HDHA and 17-HDHA levels, pathway markers for DHA-derived SPM in both males and females by 6.6 ± 1.8 to 45.8 ± 23.0 (14-HDHA)- and 5.3 ± 0.7 to 6.1 ± 0.9 (17-HDHA)-fold, respectively. We did not consistently detect and were able to quantify DHA-derived SPM. In contrast male and female mice on the DHA-enriched diet had markedly higher levels of LXA4 in draining lymph nodes compared to mice on a DHA-deficient diet, amplification of lymph node LXA4 levels was greater in females than in males, 292 ± 121% versus 105 ± 69% (p = 0.0117 and 0.0559). Consistent with results obtained with draining lymph node PMN, dietary DHA correlated with minimized Alox5 and amplified Alox15 RNA expression in draining lymph nodes during DEDs (Fig. 5b). However, lymph node Alox15 expression was higher in males in both diet groups and only in males did dietary DHA significantly amplify lymph nodes Alox15 RNA levels (67 ± 32%, p = 0.0224).
Dietary DHA amplifies lymph node LXA4 circuits in dry eye disease. Draining lymph nodes were isolated from males and females on the DHA-enriched or DHA-deficient diet after 10 days of desiccating stress (n = 5). Pooled lymph nodes from each mouse were processed for lipidomic or qPCR analysis. a 12/15-LOX DHA-derived products and LXA4 levels (pg/lymph node/mouse). b qPCR analysis of 5-LOX and 15-LOX RNA expression in draining lymph nodes (n = 5). a, b Values represent the mean ± SEM. *P < 0.05, DHA-enriched versus DHA-deficient, unpaired t test; #P < 0.05, female versus male
Acute DHA treatment rescues females from amplified immune-driven DED
The protective effect of long-term dietary DHA is multifactorial. We set out to determine if acute treatment with DHA alone would rescue mice on the DHA-deficient diet from exacerbated DED. Female mice were selected since they have amplified DED,14 which correlates with a striking female disease prevalence in humans. Female mice were placed on a 4-week DHA-deficient diet prior to initiating desiccating stress. On day 1 of desiccating stress mice were treated with a combined approach of subconjunctival (SC) injection (50 ng DHA/5 μl, every 4 days) and intravenous (IV) injection (250 nmol/kg, qd) or sterile saline alone.
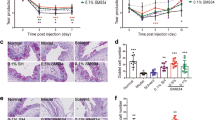
Acute DHA treatment rescued mice on the DHA-deficient diet from amplified epithelial defect (Fig. 6a). Epithelial defect was reduced by 57 ± 13% and DHA treatment increased tear production by 140 ± 83% (n = 6, p < 0.05). A key feature of autoimmune dry eye pathogenesis is the activation and infiltration of CD4+ effector T cells.27,28 Dietary DHA deficiency markedly decreased PMN in the corneal limbus and draining lymph nodes (Fig. 3) and LXA4 tissue levels (Figs. 4 and 5). Acute DHA treatment rescued female mice with dietary DHA deficiency from an amplified immune response by increasing PMN levels 150 ± 29% and decreasing CD4+ T cells by 38 ± 7% (Fig. 6).
Acute DHA treatment rescues females from amplified immune-driven dry eye disease. Female mice on the DHA-deficient diet (4 weeks) were treated locally and systemically with DHA or saline alone (vehicle control) starting at day 1 of desiccating stress. After 10 days of desiccating stress dry eye disease was assessed and corneas with limbus region isolated for IHC analysis. a Representative corneal fluorescein staining images. Bar graphs show clinical scoring of epithelial defect and tear production measured by Schirmer’s strip (n = 6). b IHC representation images (left) and quantification (right) of PMN (CD45+, Ly6g+) and CD3+, CD4+ T cells in corneas (n = 6), measured with scale bars at 20 μm. The total number of corneal PMN and T cells was counted in nine, ×40 magnification fields of view that comprised the diameter of a cornea (from limbus to limbus). Values represent the mean ± SEM. *P < 0.05, saline versus DHA
PMNs were quantified by flow cytometry in draining lymph nodes (Fig. 7a). Acute DHA treatment increased lymph node PMN numbers by 190 ± 105% (p = 0.0116) in the DHA-deficient diet mice. We have established that lymph node PMNs have key roles in regulating T effector and Treg cells in autoimmune DED.14 To determine if DHA treatment could rescue mice on the DHA-deficient diet from an amplified effector T-cell and impaired Treg response, we quantified CD4+ TH1 (IFNγ+), TH17 (IL17+), and Treg (Foxp3+) cells in draining lymph nodes by flow cytometry (Fig. 7b). DHA treatment caused a marked increase (289 ± 41%, p = 0.0002) in Treg and abrogated TH1 and TH17 cells in draining lymph nodes as evidenced by 84 ± 1% (p < 0.0001) and 81 ± 2% (p = 0.0004) decrease, respectively. Collectively these finding establish that acute DHA treatment can rescue female mice from amplified effector T-cell-driven DEDs.
Acute DHA treatment rescues females from amplified T-cell responses and amplifies endogenous LXA4 formation in tissues. Female mice on the DHA-deficient diet (4 weeks) were treated locally and systemically with DHA or saline alone starting at day 1 of desiccating stress. After 10 days of desiccating stress draining lymph nodes were collected for analysis by flow cytometry. a Bar graph PMN (CD45highLy6ghigh) in draining lymph nodes (n = 3, with pooled cervical lymph nodes from 1 mouse for each group). b Frequencies of Treg cells (CD4+Foxp3+), TH1 cells (CD4+IFNγ+), and TH17 (CD4+IL17+) cells among absolute number of lymphocytes. c LXA4 levels were measured by LC/MS/MS-based lipidomics in plasma (n = 4), cornea (n = 5), lacrimal gland (n = 5), and draining lymph nodes (n = 5). d qPCR analysis of 5-LOX, 15-LOX, and LXA4 receptor (ALX) RNA expression in draining lymph nodes. Values represent the mean ± SEM. *P < 0.05, saline versus DHA
Acute DHA treatment restores expression and activity of the LXA4 circuit in dietary DHA deficiency
We next assessed if acute DHA treatment could restore expression and activity of SPM circuits, specifically LXA4 formation, in mice subjected to long-term dietary DHA deficiency. Lipidomic analysis demonstrated that acute DHA treatment markedly increased LXA4 levels (Fig. 7c) in plasma, cornea, and draining lymph nodes compared to saline-treated mice by 2300 ± 1982% (p = 0.0319), 246 ± 126% (p = 0.0231), and 404 ± 240% (p = 0.0154), respectively. To assess the impact of DHA treatment on expression of the LXA4 pathway, we focused on lymph nodes as they are the main site for regulating effector T cells and initiating adaptive immune responses. The increase in lymph node LXA4 levels caused by acute DHA treatment correlated with a significant decrease in 5-LOX RNA levels and a concurrent increase in 15-LOX RNA levels (Fig. 7d). These results provide evidence that acute treatment with DHA can rapidly restore LXA4 circuit expression and activity in lymph nodes and reverse amplified adaptive immune responses caused by dietary DHA deficiency
Discussion
Immune-driven DED is characterized by an imbalance in immunoregulatory and pro-inflammatory pathways (Fig. 8). Current treatment options are palliative to restore tear film or are aimed at blocking essential immune pathways. Our experiments demonstrate that depletion of dietary ω-3 PUFA significantly exacerbates effector T-cell-driven DED in mice while dietary DHA supplementation is protective (Fig. 8). These finding are consistent with a post hoc clinical study, which established that dietary ω-3 PUFAs in women is associated with a decreased incidence of dry eye syndrome.29 More importantly, our data demonstrate that dietary amplification of dry eye pathogenesis due to ω-3 PUFA depletion was greater in females than in males, which support our previous findings of sex-specific differences in corneal wound healing15 and immune-driven DED.14 There is compelling evidence for significant roles of essential PUFAs in regulating ocular surface immunity and physiology. ω-3 PUFA dietary deficiency in mice reduces tear volume while supplementation stimulates tear production,17 and topical treatment with ω-3 and ω-6 PUFA reduces dry eye pathogenesis and markers of inflammation.6 DHA is a major PUFA in human tears and we have reported that decreased tear levels of DHA are associated with tear film dysfunction and DED.30 DHA is of particular interest as it is the most prevalent ω-3 PUFA in tissues and its tissue levels are highly regulated, especially in the retina, brain, and testis. Animal studies have established that topical application of DHA increases nerve density and corneal epithelial cell proliferation and accelerates wound healing after corneal surgery.31,32
Summary scheme illustrating docosahexaenoic acid (DHA)-mediated increase in tissue PMN numbers, 15-LOX expression, PMN LXA4 formation, and tissue LXA4 levels as a proposed mechanism for inhibiting effector T-cell responses (TH1 and TH17) and reducing pathogenesis in immune-driven dry eye disease. Male and female symbols and relative symbol size indicate pathways that demonstrated marked sex-specific differences
Beneficial actions of DHA in the ocular surface are multifactorial and include modulation of inflammatory and immune responses. A mechanism for dietary and therapeutic DHA treatment is amplification of DHA-derived resolvins, protectins, and maresins. These SPMs regulate PMN, macrophage, and T effector cell function in many tissues, including the cornea and retina.33,34,35,36 Studies using dietary fish oil supplementation or the fat-1 transgenic mouse have demonstrated that increased tissue levels of DHA or eicosapentaenoic acid (EPA) can result in increased ω-3 SPM levels or its pathway markers.10,21,37,38,39 Hence, our findings that dietary DHA significantly and selectively increased levels of the arachidonic acid-derived LXA4, in lymph nodes, cornea, and lacrimal glands at first glance seem counterintuitive. However, LXA4 is formed by the same enzymes, identical mechanisms, and analogous ω-6 intermediates as ω-3 PUFA-derived SPM. It is important to recognize that arachidonic acid is the most abundant substrate for LOX and COX enzymes in most cells and tissues, a fact that is not changed by dietary supplementation with fish oils in humans or mice. Our current findings in mice are in agreement with results from a clinical study where we analyzed serum from human infants that received parenteral nutrition.40 We analyzed serum from a small cohort of human infants where the IV lipid emulsion was switched from soybean to fish oil, unexpectedly LXA4 serum levels dramatically increased at 1 and/or 4 weeks after switching the patients to the fish oil emulsion.
The molecular mechanism for dietary DHA amplification of endogenous LXA4 formation in multiple tissue, including draining lymph nodes, remains to be fully defined. Studies have reported dietary DHA regulation of leukocyte function and pro-inflammatory mediator expression.41,42,43,44 This includes a clinical study, which demonstrated that a high DHA and EPA diet changed the expression of more than 1000 genes in monocytes included a marked decrease in pro-inflammatory and induction of anti-inflammatory pathways.45 We have previously identified a population of regulatory PMN that reside in lymph nodes and the limbus regions of the cornea.14 These specialized PMN control DED in females by producing LXA4, a key feature of these PMN is high expression of 15-LOX and low expression of 5-LOX. Dietary DHA markedly reduced 5-LOX expression in the lymph node PMN population in both males and females, which correlated with a marked increase in LXA4 formation. More importantly, acute local and systemic treatment with DHA rescued female on a DHA-deficient diet from amplified DED, abrogated T effector cell responses and restored the lymph node regulatory PMN population. All of these protective actions of DHA treatment correlated with decreased 5-LOX and increased 15-LOX expression and a marked increase in lymph node LXA4 levels. Multiple mechanisms have been proposed for direct actions of DHA1,2,43,44 but how dietary or acute systemic treatment with DHA regulates gene expression or the levels of regulatory PMN in lymph nodes remains to discovered. Several studies9,46 have established that DHA-derived SPM regulate 5-LOX activity and expression and induce M2-like phenotypes in macrophages. Hence, even though we did not directly detect DHA-derived SPMs their pathways were clearly upregulated in the DHA diet group and it is possible that DHA-derived SPMs have a role in amplifying the LXA4 pathway and regulatory PMN in tissues.
Emerging evidence indicates that SPMs such as lipoxins are not just formed during the resolution phase of acute inflammation or that their primary bioaction is regulation of inflammation. Specific cells such as regulatory PMN and astrocytes14,47,48 as part of their homeostatic function maintain a basal tissue tone of LXA4 in draining lymph nodes, retina, optic nerve head, and corneal limbus. This local tissue tone of LXA4 has important roles in controlling the response of T cells or neurons to routine stress/injury signals in the ocular surface or retina. DHA directly or indirectly regulates the expression of the LXA4 biosynthetic pathway and increases tissue levels of LXA4 producing regulatory PMN in the corneal limbus and draining lymph nodes (Fig. 8). DHA regulation of 5-LOX and 15-LOX expression and regulatory PMN and LXA4 levels demonstrated marked and diverse sex- and tissue-specific difference, which underscores that regulation of routine immune responses and protective roles of DHA is distinct in males and females.
Methods
Animals
Age-matched (6–10 weeks old) C57BL/6J male and female mice were purchased from Jackson Laboratory (Bar Harbor, ME). Mice were maintained on a 12-h day/night cycle and received ad libitum a standard rodent diet (Rat/Mouse diet LM-485, Harlan Tekland, Madison, WI) prior to initiating the dietary study. All mice were placed on a balanced open source (AIN-76A, 6.2% fat) DHA-enriched (60% soybean oil and 40% DHA) or DHA-deficient (100% soybean oil) rodent diet (Research Diets, New Brunswick, NJ) for 4 weeks prior to initiating desiccating stress and dry eye pathogenesis. We did not control for estrogen fluctuations due to the normal 4- to 5-day estrous cycle of females. DHA ethyl ester (DHA ethyl ester 71.5% and EPA ethyl ester 12%) for preparing the balanced custom diets was a kind gift from Solutex (Madrid, Spain). All animal studies were approved by the University of California Berkeley Animal Care and Use Committee and follow the NIH Guide for the Care and Use of Laboratory Animals.
Dry eye tear-deficient mouse model
DED was induced using an established model of desiccating stress as previously described.14 Briefly, mice were placed in cages with a perforated screen wall and exposed to continuous airflow from fans in a low-humidity (20–30%) cubicle. Lacrimal gland function was inhibited by injection with scopolamine hydrobromide (0.1 mL of 10 mg/mL, formulated in sterile saline; Sigma-Aldrich Corp., St Louis, MO) for 3 or 5 consecutive days, and a reduced dose (0.1 mL of 5 mg/mL) for 10 days, respectively. Scopolamine hydrobromide injections were performed three times per day (9 a.m., 2 p.m., and 7 p.m.), subcutaneously into alternating hindquarters of mice. Healthy controls were age- and sex-matched untreated mice on a DHA-enriched or DHA-deficient rodent diet housed in a standard animal facility environment.
Tissue isolation
Healthy mice or mice with DED were euthanized. Corneas with complete limbus, lacrimal glands (weighed upon extraction), and cervical draining lymph nodes (diameter controlled 1.8–2.0 mm) were surgically removed using a stainless steel surgical blade. Isolated tissues were washed in ice-cold sterile phosphate-buffered saline (PBS) under a dissecting microscope and immediately snap-frozen for RNA, lipidomic, MPO analyses, or immediately processed for flow cytometry/IHC.14
PMN isolation
PMNs were isolated from cervical draining lymph nodes from male and female mice on the DHA-enriched or DHA-deficient diet. Briefly, lymph nodes were minced and filtered through a 40-mm cell strainer (BD Falcon; BD Biosciences, San Diego, CA). After preparation of single-cell suspension, cells were negatively separated and isolated using PMN isolation kits (Miltenyi Biotec, Bergisch-Gladbach, Germany), according to the manufacturer’s instructions. Cells were stained with trypan blue and counted using light microscopy. The cell suspension was pelleted by centrifugation, followed by washing in RPMI 1640 with 5% FBS. The cell pellet was resuspended (5 × 105 PMN/ml) in 200 μl RPMI 1640 with 5% FBS and activated with calcium ionophore (37 °C, 15 min, 5 μM). Media were collected to establish endogenous lipid mediator formation by LC/MS/MS-based lipidomics. Unactivated freshly isolated PMN were used to quantify gene expression.
Clinical assessment of DED
Epithelial damage was qualitatively assessed by fluorescence microcopy by staining corneas with 0.5 μL of 2.5% Fluorescein Sodium (Bausch & Lomb) before further quantitative assessment was conducted in accordance with the standard NEI scoring system. Using a phenol red thread (Zone-Quick; Showa Yakuhin Kako Co., Tokyo, Japan), the cotton thread test measured tear production by placing the thread in the lateral canthus of the conjunctiva fornix of each eye for 30 s after excess tears had been removed 30 s prior. Light microscopy (Carl Zeiss, Jena, Germany) was used to measure and read the tear fluid distance (in millimeters).
MPO assay
Tissue PMNs were quantitated by measuring MPO activity in lacrimal glands and lymph nodes as previously described.14,24,25 Total tissue PMN numbers were established through calibration curves of PMN exudates from zymosan A-induced peritonitis in C57BL/6J mice.
Flow cytometry analysis
PMNs and lymphocyte cell populations within lacrimal glands, draining lymph nodes, and corneas were assessed by flow cytometry as previously described.14 Anti-FcR mAB (BD PharMingen, San Diego, CA) was used to block Fc receptors for 10 min before samples were incubated for 30 min in titrated amounts of fluorescent-labeled antibodies: fluorescein isothiocyanate (FITC)-conjugated anti-Ly6g (1A8 clone; BD PharMingen, San Diego, CA, USA) for PMN; phycoerythrin (PE)-conjugated anti-CD45 (MEC 13.3 clone; BD PharMingen) for leukocytes; PE-conjugated anti-CD3 (500A2 clone; BD PharMingen) for T cells; FITC-conjugated anti-CD4 (RM4-5 clone; BD PharMingen) for activated CD4+ T cells; allophycocyanin (APC)-conjugated anti-IFN-γ (XMG1.2; TONBO biosciences); FITC- or APC-conjugated anti-IL17 (eBio17B7; ebioscience); and APC-conjugated anti-Foxp3 (3G3; TONBO biosciences). Live cells were sorted using a high-speed sorter (MoFlo, SX DakoCytomation, Inc., Fort Collins, CO, USA).
Quantitative PCR
mRNA from lymph node PMN was isolated using a RNA Easy Mini Kit (Qiagen Sciences, Germantown, MD, USA) and quantified via spectrophotometry. mRNA was then reverse transcribed using a High-Capacity cDNA Kit (Applied Biosystems, Foster City, CA, USA). All samples were run in duplicates using a StepOne Plus qPCR system (Applied Biosystems) β-actin was used as a reference gene and universal mouse reference RNA was used to calculate relative mRNA expression of our samples as previously described.14,15
Lipid mediator lipidomics
Corneas, lacrimal glands, and draining lymph nodes were rapidly homogenized using a refrigerated bead homogenizer in 66% MeOH containing deuterated internal standards (PGE2-d4, LTB4-d4, 15-HETE-d8, LXA4-d5, DHA-d5, and AA-d8). Tissue supernatants were extracted using Accubond ODS-C18 cartridges (Agilent Technologies, Santa Clara, CA). Lipid mediators were identified and quantified by LC/MS/MS-based lipidomics using a AB Sciex QTRAP 3200 MS as previously described.14,15 Analysis was carried out in negative ion mode, and lipid mediators and PUFA were quantitated using scheduled MRM using 4–6 specific transition ions for each analyte. Prominent fragment ions (m/z) for identification of LXA4 (351.2 m/z, retention time 10.5 min) included 115.1, 135.1, 189.2, 217.3, and 235.3.
SC and IV DHA injections
Two days prior to inducing desiccating stress, female mice on a 4-week DHA-deficient diet received local DHA treatment (50 ng) via a SC injection. The local treatment was repeated on day 3 and day 7 of desiccating stress. Control mice received 5 μL PBS SC injection. SC injections were carried out under a Zeiss AxioCam microscope with a 10 μL hamilton syringe. Systemic treatment with DHA (250 nmol/kg) was started on day 1 of desiccating stress by tail vein (IV) injections. The control group received vehicle alone (20 μL sterile PBS) daily. DHA (Cayman Chemical Company, Ann Arbor, MI) was dried under a stream of nitrogen to remove all EtOH and immediately resuspended in sterile PBS for IV or SC injections.
Statistical analysis
One-tailed, unpaired Student’s t test was used to determine differences between males and females. One-way analysis of variance with Tukey’s post hoc testing was used to determine differences between multiple experimental groups. Overall comparisons were made by significant statistical P values of <0.05. Unless otherwise noted, all data reported as ± SEM.
References
Simopoulos, A. P. Omega-3 fatty acids in inflammation and autoimmune diseases. J. Am. Coll. Nutr. 21, 495–505 (2002).
Calder, P. C. Marine omega-3 fatty acids and inflammatory processes: effects, mechanisms and clinical relevance. Biochim. Biophys. Acta 1851, 469–484 (2015).
Christen, W. G., Schaumberg, D. A., Glynn, R. J. & Buring, J. E. Dietary ω-3 fatty acid and fish intake and incident age-related macular degeneration in women. Arch. Ophthalmol. 129, 921–929 (2011).
Kawakita, T. et al. Effects of dietary supplementation with fish oil on dry eye syndrome subjects: randomized controlled trial. Biomed. Res. 34, 215–220 (2013).
McCusker, M. M., Durrani, K., Payette, M. J. & Suchecki, J. An eye on nutrition: the role of vitamins, essential fatty acids, and antioxidants in age-related macular degeneration, dry eye syndrome, and cataract. Clin. Dermatol. 34, 276–285 (2016).
Rashid, S. et al. Topical omega-3 and omega-6 fatty acids for treatment of dry eye. Arch. Ophthalmol. 126, 219–225 (2008).
Wei, J. & Gronert, K. The role of pro-resolving lipid mediators in ocular diseases. Mol. Aspects Med. 58, 37–43 (2017).
Norling, L. V., Ly, L. & Dalli, J. Resolving inflammation by using nutrition therapy: roles for specialized proresolving mediators. Curr. Opin. Clin. Nutr. Metab. Care 20, 145–152 (2017).
Buckley, C. D., Gilroy, D. W. & Serhan, C. N. Proresolving lipid mediators and mechanisms in the resolution of acute inflammation. Immunity 40, 315–327 (2014).
Hassan, I. R. & Gronert, K. Acute changes in dietary -3 and -6 polyunsaturated fatty acids have a pronounced impact on survival following ischemic renal injury and formation of renoprotective docosahexaenoic acid-derived protectin D1. J. Immunol. 182, 3223–3232 (2009).
Chiang, N., Arita, M. & Serhan, C. N. Anti-inflammatory circuitry: lipoxin, aspirin-triggered lipoxins and their receptor ALX. Prostaglandins Leukot. Essent. Fatty Acids 73, 163–177 (2005).
Kenchegowda, S. & Bazan, H. E. Significance of lipid mediators in corneal injury and repair. J. Lipid Res. 51, 879–891 (2010).
Calandria, J. M. et al. Selective survival rescue in 15-lipoxygenase-1-deficient retinal pigment epithelial cells by the novel docosahexaenoic acid-derived mediator, neuroprotectin D1. J. Biol. Chem. 284, 17877–17882 (2009).
Gao, Y. et al. Female-specific downregulation of tissue polymorphonuclear neutrophils drives impaired regulatory T cell and amplified effector T cell responses in autoimmune dry eye disease. J. Immunol. 195, 3086–3099 (2015).
Wang, S. B. et al. Estrogen negatively regulates epithelial wound healing and protective lipid mediator circuits in the cornea. FASEB J. 26, 1506–1516 (2012).
Krishnan, T. et al. Gender differences in re-epithelialisation time in fungal corneal ulcers. Br. J. Ophthalmol. 96, 137–138 (2012).
Harauma, A., Saito, J., Watanabe, Y. & Moriguchi, T. Potential for daily supplementation of n-3 fatty acids to reverse symptoms of dry eye in mice. Prostaglandins Leukot. Essent. Fatty Acids 90, 207–213 (2014).
Cortina, M. S. & Bazan, H. E. Docosahexaenoic acid, protectins and dry eye. Curr. Opin. Clin. Nutr. Metab. Care 14, 132–137 (2011).
Barabino, S. et al. The role of systemic and topical fatty acids for dry eye treatment. Prog. Retin. Eye Res. 61, 23–34 (2017).
Barbosa, F. L. et al. Goblet cells contribute to ocular surface immune tolerance-implications for dry eye disease. Int. J. Mol. Sci. 18, E978 (2017).
Barden, A. E., Mas, E., Croft, K. D., Phillips, M. & Mori, T. A. Specialized proresolving lipid mediators in humans with the metabolic syndrome after n-3 fatty acids and aspirin. Am. J. Clin. Nutr. 102, 1357–1364 (2015).
Stevenson, W., Chauhan, S. K. & Dana, R. Dry eye disease: an immune-mediated ocular surface disorder. Arch. Ophthalmol. 130, 90–100 (2012).
Niederkorn, J. Y. et al. Desiccating stress induces T cell-mediated Sjogren's syndrome-like lacrimal keratoconjunctivitis. J. Immunol. 176, 3950–3957 (2006).
Gronert, K. et al. A role for the mouse 12/15-lipoxygenase pathway in promoting epithelial wound healing and host defense. J. Biol. Chem. 280, 15267–15278 (2005).
Leedom, A. J., Sullivan, A. B., Dong, B., Lau, D. & Gronert, K. Endogenous LXA4 circuits are determinants of pathological angiogenesis in response to chronic injury. Am. J. Pathol. 176, 74–84 (2010).
Gronert, K. Lipid autacoids in inflammation and injury responses: a matter of privilege. Mol. Interv. 8, 28–35 (2008).
El Annan, J. et al. Characterization of effector T cells in dry eye disease. Invest. Ophthalmol. Vis. Sci. 50, 3802–3807 (2009).
De Paiva, C. S. et al. IL-17 disrupts corneal barrier following desiccating stress. Mucosal Immunol. 2, 243–253 (2009).
Miljanovic, B. et al. Relation between dietary n-3 and n-6 fatty acids and clinically diagnosed dry eye syndrome in women. Am. J. Clin. Nutr. 82, 887–893 (2005).
Walter, S. D. et al. omega-3 tear film lipids correlate with clinical measures of dry eye. Invest. Ophthalmol. Vis. Sci. 57, 2472–2478 (2016).
Cortina, M. S., He, J., Li, N., Bazan, N. G. & Bazan, H. E. Recovery of corneal sensitivity, calcitonin gene-related peptide-positive nerves, and increased wound healing induced by pigment epithelial-derived factor plus docosahexaenoic acid after experimental surgery. Arch. Ophthalmol. 130, 76–83 (2012).
Pham, T. L. et al. Defining a mechanistic link between pigment epithelium-derived factor, docosahexaenoic acid, and corneal nerve regeneration. J. Biol. Chem. 292, 18486–18499 (2017).
Krishnamoorthy, S. et al. Resolvin D1 binds human phagocytes with evidence for proresolving receptors. Proc. Natl Acad. Sci. USA 107, 1660–1665 (2010).
Jin, Y. et al. Anti-angiogenesis effect of the novel anti-inflammatory and pro-resolving lipid mediators. Invest. Ophthalmol. Vis. Sci. 50, 4743–4752 (2009).
Hua, J. et al. The resolvin D1 analogue controls maturation of dendritic cells and suppresses alloimmunity in corneal transplantation. Invest. Ophthalmol. Vis. Sci. 55, 5944–5951 (2014).
Bazan, N. G. Neuroprotectin D1-mediated anti-inflammatory and survival signaling in stroke, retinal degenerations, and Alzheimer’s disease. J. Lipid Res. 50(Suppl), S400–S405 (2009).
Jones, M. L. et al. Maternal dietary omega-3 fatty acid intake increases resolvin and protectin levels in the rat placenta. J. Lipid Res. 54, 2247–2254 (2013).
Bilal, S. et al. Fat-1 transgenic mice with elevated omega-3 fatty acids are protected from allergic airway responses. Biochim. Biophys. Acta 1812, 1164–1169 (2011).
Mas, E., Croft, K. D., Zahra, P., Barden, A. & Mori, T. A. Resolvins D1, D2, and other mediators of self-limited resolution of inflammation in human blood following n-3 fatty acid supplementation. Clin. Chem. 58, 1476–1484 (2012).
Kalish, B. T. et al. Intravenous fish oil lipid emulsion promotes a shift toward anti-inflammatory proresolving lipid mediators. Am. J. Physiol. Gastrointest. Liver Physiol. 305, G818–G828 (2013).
Matsumoto, K., Morita, I., Hibino, H. & Murota, S. Inhibitory effect of docosahexaenoic acid-containing phospholipids on 5-lipoxygenase in rat basophilic leukemia cells. Prostaglandins Leukot. Essent. Fatty Acids 49, 861–866 (1993).
Stanke-Labesque, F. et al. Effect of dietary supplementation with increasing doses of docosahexaenoic acid on neutrophil lipid composition and leukotriene production in human healthy volunteers. Br. J. Nutr. 100, 829–833 (2008).
Chilton, F. H., Patel, M., Fonteh, A. N., Hubbard, W. C. & Triggiani, M. Dietary n-3 fatty acid effects on neutrophil lipid composition and mediator production. Influence of duration and dosage. J. Clin. Invest. 91, 115–122 (1993).
Calder, P. C. Omega-3 polyunsaturated fatty acids and inflammatory processes: nutrition or pharmacology? Br. J. Clin. Pharmacol. 75, 645–662 (2013).
Bouwens, M. et al. Fish-oil supplementation induces antiinflammatory gene expression profiles in human blood mononuclear cells. Am. J. Clin. Nutr. 90, 415–424 (2009).
Chiang, N. & Serhan, C. N. Structural elucidation and physiologic functions of specialized pro-resolving mediators and their receptors. Mol. Aspects Med. 58, 114–129 (2017).
Livne-Bar, I. et al. Astrocyte-derived lipoxins A4 and B4 promote neuroprotection from acute and chronic injury. J. Clin. Invest. 127, 4403–4414 (2017).
Biteman, B. et al. Interdependence of lipoxin A4 and heme-oxygenase in counter-regulating inflammation during corneal wound healing. FASEB J. 21, 2257–2266 (2007).
Acknowledgements
This project was funded in part by National Institutes of Health Grants (EY022208 and P30EY003176)
Author information
Authors and Affiliations
Contributions
K.G. and Y.G. conceived the study, designed the experiments, interpreted the data, and wrote the paper; J.S., Y.Z., A.C., J.H.S., D.W. and K.M. carried out most of the experiments, analyzed data, generated figures, discussed results, and commented on the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Rights and permissions
About this article
Cite this article
Gao, Y., Su, J., Zhang, Y. et al. Dietary DHA amplifies LXA4 circuits in tissues and lymph node PMN and is protective in immune-driven dry eye disease. Mucosal Immunol 11, 1674–1683 (2018). https://doi.org/10.1038/s41385-018-0070-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41385-018-0070-z
This article is cited by
-
Dysregulation of neuroprotective lipoxin pathway in astrocytes in response to cytokines and ocular hypertension
Acta Neuropathologica Communications (2024)
-
Pro- and anti-inflammatory bioactive lipids imbalance contributes to the pathobiology of autoimmune diseases
European Journal of Clinical Nutrition (2023)
-
Gut-derived butyrate suppresses ocular surface inflammation
Scientific Reports (2022)
-
Loss of 15-lipoxygenase disrupts Treg differentiation altering their pro-resolving functions
Cell Death & Differentiation (2021)