Abstract
Calcification, a phenomenon often regarded by pathologists little more than evidence of cell death, is becoming recognized to be important in the dynamics of a variety of diseases from which millions of beings suffer in all ages. In calcification, all that is needed for crystal formation to start is nidi (nuclei) and an environment of available dissolved components at or near saturation concentrations, along with the absence of inhibitors for crystal formation. Calcifying nanoparticles (CNP) are the first calcium phosphate mineral containing particles isolated from human blood and were detected in numerous pathologic calcification related diseases. Controversy and critical role of CNP as nidi and triggering factor in human pathologic calcification are discussed.
Similar content being viewed by others
PATHOLOGIC CALCIFICATION RELATED DISEASES: A MAJOR HEALTH PROBLEM IN HUMANS IN ALL AGE GROUPS
The mineral phase of many kinds of hard tissue in organisms is called biologic apatite (BA). Pure hydroxyapatite (HA) has the formula Ca10(PO4)6(OH)2. BA additionally contains several other ions, mainly carbonate but also trace amounts of other anions such as HPO42−, Cl−, and F−. Other cation elements are also present in minor amounts including Mg2+, Na+, and Fe2+. BA is the primary mineral of normal bone and teeth (1). By definition, pathologic calcification refers to the deposition of calcium phosphates (CaP) or other calcific salts at sites, which would not normally have become mineralized. Abnormal accumulation can occur in areas of tissue damage (dystrophic calcification), in hypercalcemic or hyperparathyroid states (2). Apatite deposition is not a rare phenomenon in pediatry. Calcification is most often seen in children who had prenatal infections. It is also found in association with or as a consequence of toxic or hypoxic damage, intracranial bleed, metabolic, and hereditary diseases like mitochondrial encephalopathy, biotinidase deficiency, and in certain conditions of unknown cause (3).
Kidney and bladder stones, dental pulp stones, some gall stones, salivary gland stones, chronic calculous prostatitis, testicular microliths, calcification in hemodialysis patients, atherosclerosis, malacoplakia, scleroderma (systemic sclerosis), calcinosis cutis, calcific aortic stenosis, several malignancies, some dementias, calcific tenditis, synovitis and arthritis, diffuse interstitial skeletal hyperostosis, juvenile dermatomyositis, systemic lupus erythematosus are the most common diseases involving extraskeletal calcification (4,5). BA deposits also occur in association with inflammation in a variety of other tissues including the eye after implantation of ocular lenses (6) or the breast after breast implants (7). In each case, these deposits contribute to the morbidity and mortality of the underlying condition. Although the sizes of the mineral crystals in pathologic calcification are similar to those in bone, there is much more mineral in the deposits than there is in bone. Bone matrix proteins also accumulate associated with the deposits. The reasons for the formation of these deposits are not known. It was hypothesized that persistent inflammation is a component of BA and other HA deposition diseases. Other contributing factors are genetic, environmental, and physical chemical (5). Since inflammation has been the proposed trigger for the calcification, what is the underlying cause of the triggering inflammation?
We first consider the formation of kidney stones (KS), a major and increasing health problem. Approximately 5% of American women and 12% of men will have a KS at some time in life, at an annual cost of $2.1 billion (8). The prevalence of KS in the USA rose by 37% between 1976–1980 and 1988–1994 in both genders (9). Studies on the geographic variation in the USA in the prevalence of KS disease have shown a 50% higher prevalence in the southeast than the northwest (10), possibly associated with a changing state of dehydration related to high summertime temperatures and resulting in a low urine volume. Given the temperature rise worldwide due to the effects of global warming, it has been predicted that there could be an increase of 1.6–2.2 million lifetime cases of KS by 2050, particularly in the southeast regions of the USA (11,12). Rule et al. (13) have shown that KS are a risk factor for chronic kidney disease, and studies are warranted to assess screening and preventive measures for chronic kidney disease in stone formers. Urinary macromolecules in children show stronger inhibition of Ca oxalate (CaOx) crystal growth, aggregation and adhesion than in adults. Furthermore osteopontin and calgranulin B expression is down-regulated in children due to this inhibitory effect and, thus, stone nidus formation is controlled (14). What happens in adults to make them more suseptable to KS formation? Could it be the acquisition of an infectious agent?
Another observation may be important. A strong association has been identified between the numbers of sessions of extracorporeal shock wave lithotripsy (SWL) the patient received with conversion of CaOx stones to increasing levels of CaP in recurring stones (15). The presence of CaP stones raises clinical concern, especially those stones containing brushite (calcium monohydrogen phosphate dihydrate, CaHPO4), because of their increased hardness and, thus, greater resistance to communition by SWL (16). Why does SWL increase CaP KS formation? Is it possible that an infectious agent acquired over time enhances the formation of CaP rather than CaOx in recurring stones?
Another example of pathologic calcification occurs in cardiovascular disease. Surprisingly, cardiovascular disease is the leading cause of death in patients with chronic kidney disease. A growing body of data points to nontraditional risk factors, including disturbances in mineral metabolism, as important determinants of the extremely high cardiovascular morbidity and mortality rates in these patients. Disturbances in mineral metabolism, especially elevated calcium and phosphate levels, have been linked to vascular and valvular calcification, both of which are associated with poor prognosis in chronic kidney disease patients. New studies indicate that not only vascular intimal calcification (associated with atherosclerosis) but also vascular medial calcification are correlated with decreased survival in chronic kidney disease patients (17).
Calcification of cardiovascular prosthetic implants is a common and important problem. A variety of cardiovascular prostheses are affected clinically by calcification, including bioprosthetic heart valves, aortic homografts, and trileaflet polymeric valve prostheses. In addition, experimental studies have demonstrated calcification of artificial heart devices in ventricular assist systems in long-term calf studies. The pathophysiology of this disease process is incompletely understood (18). Is calcification on those devices form by the same mechanism of pathologic calcification in the soft tissue? Is the association of calcification-releated cardiovascular disease and KS formation closely related and perhaps caused by the same agent acquired like a bacterium or virus?
NUCLEATION AND GROWTH OF CaP IN THE HUMAN BODY
Pathologic calcification is a complicated, actively regulated process of mineralization that is similar to bone formation and remodeling (19,20). Mineralogists explain that all that is needed for crystal formation to start is nidi (nucleus) and an environment of available dissolved components at or near saturation concentrations, along with the absence of inhibitors for crystal formation (21). Bacteria or other agents producing such nidi, if present in blood and in urine, are very likely candidates to launch and accelerate pathologic calcification in vivo (22,23). This is clinically important since blood contains phosphate near its saturation level (24).
Matrix vesicles (MV), which are membranous structures derived from the surfaces of hypertrophic chondrocytes, are thought to initiate calcification at the mineralization front by focally concentrating calcium within their already phosphate-rich structures (25). These vesicles have high levels of alkalinephosphatase and have the ability to concentrate calcium and increase phosphorus during mineralization. Electron microscope studies have indicated that biologic calcification occurs in the MVs in two steps, the first related to the initial deposition of HA within the lumen of the MVs and the second to the propagation of mineral outside the vesicles (26).
Acidic phospholipids are present at high levels in cells at the mineralizing front in bone and in pathologic calcifications (27). Detergent pretreatment of bioprosthetic heart valves, shown to inhibit mineralization, likely acts by the detergent-mediated extraction of phospholipids and other proteolipids, which takes place under these conditions (28).
THE PREVIOUSLY UNSUSPECTED ROLE OF NANOPARTICLES
Human exposure to nanoparticles is inevitable as nanoparticles become more widely used and, as a result, nanotoxicology research is now gaining attention. Although the number of nanoparticle types and applications continues to increase, studies to characterize their effects after exposure and to address their potential toxicity are few in comparison. In the medical field in particular, nanoparticles are being used in diagnostic and therapeutic tools to better understand, detect, and treat human diseases (29). When size-dependent cytotoxicity is studied, it has been shown that the smaller the particle is more cytotoxic it gets (30), and they may act as a nidus for pathologic calcification.
Apatite is generally not toxic to human cells. However, when apatite is present somewhere other than in bones and teeth, it may cause adverse effects (31–33). Other studies have concluded that in vivo apatite applications are generally safe (34–37). Although these disagreements have not been completely resolved, both BA and non-BA materials have been continuously used in drug delivery and transplantation (38–41). What has not been well studied, however, is the cytotoxcity of nanophase apatite and related particles.
REPLICATING, CALCIFYING NANOPARTICLES, AND THEIR RELATION TO PATHOLOGIC CALCIFICATION
Most pathologic calcifications throughout the body contain mixtures of carbonate-substituted HA and octacalcium phosphate. According to the Merck Manuel, these ultramicroscopic crystals occur in snowball-like clumps. Those clumps can cause severe inflammation (42). Structures similar to these nanometer-sized snowballs were discovered almost two decades ago in blood and blood products (43). These structures, called calcifying nanoparticles (CNP), were detected in numerous pathologic calcification related diseases (44–47). CNP are the first CaP mineral containing particles isolated from human blood.
CNP have the following unusual properties: bacteria-like (48), pleomorphic (49), infectious (50), self replicating (51), capable of passing sterilization filters because of their small size (80–500 nm) (52), resistance to heat and γ irradiation at doses typically fatal for conventional bacteria (53), capable of forming a calcific coating at physiologic pH and mineral concentrations (49), lacking inherent DNA (54), sensitive to certain antibiotics (55), and capable of causing the formation of lipid compounds (un published data).
CNP have now been linked to pathologic calcification related diseases such as arteriosclerosis (44–46), KS (47,56–59), gall stone (60,61), dental pulp stone formation (62–64), prostatitis (65–67), Alzheimer's (Kajander et al. Do Autonomously replicating sterile-filterable particles have an association with amyloid accumulation? Viruses and virus-like agents in disease. Second Karger Symposium, March 7–9, 1993, Basel, Switzerland, Abstract 41), polycystic kidney (PKD) (68,69), and cancer (70,71). CNP exert cytotoxic effects on some mammalian cells in vitro (72) and on living organisms in vivo (73).
The incidence of KS formation and recurrences may continue to rise every year. Thus, new approaches in treatment and prevention could have a huge economic effect apart from benefits in terms of reduced morbidity. Over seventy years ago, Randall examined the papillae of cadaveric renal units and demonstrated that interstitial crystal plaques in the papillary tip were common in stone formers (74). These crystals were composed not of CaOx, the most common solid phase found in patients with nephrolithiasis, but of CaP. He believed that the CaP crystals serve as a nucleation surface for CaOx. Recently, Matlaga et al. (75) analyzed Randall's plaques (RP) and confirmed that they are formed of spherical CaP deposits with a multilaminated internal morphology. With the CNP detection methodologies we developed (59), important features of CNP and their triggering effect on nephrolithiasis have been suggested (47,59). In our study, there was evidence of a link between detection of CNP and presence of RP. Although causality was not demonstrated, the results we obtained suggest that further studies with negative control samples should be made to explore the etiology of RP formation, thus leading to a better understanding of the pathogenesis of stone formation. Additionally, this hypothesis may bring an explanation to the reason of the increase on CaP KS formation after SWL.
Another urinary disease, PKD, is the most common autosomal dominant lethal disease in humans. Interestingly, a higher prevalence of kidney calcifications is observed in PKD than in the normal population (76). It has been proposed that the currently known cellular toxicities, tissue distribution, and pharmacology of CNP are plausibly related to the known pathology and pharmacology of PKD (68). Hjelle et al. (68) evaluated 13 PKD cyst fluids and detected CNP antigen positivity in each sample as well as in liver cystic fluid from affected individuals. This may explain the reason of high rate calcification problem in patients with PKD.
The presence of prostatic calculi in younger men is associated with both inflammation and symptoms of chronic pelvic pain syndrome (77). Biopsies, urine, and prostatic secretion cultures fail to demonstrate bacterial pathogens, however inflammation is often detected in chronic prostatitis (78). The core of prostatic calculi is typically CaP (79), which is the hallmark of CNP action. Wood and Shoskes (66) proposed that there is a potential role of CNP in chronic prostatitis. Recent clinical research targeting these agents has proven effective in treating some patients with refractory category III prostatitis (chronic pelvic pain syndrome) (67). In that research, CNP antigen or antibody was found in 60% of serum and 40% of urine samples. In 10 patients who underwent transrectal ultrasound after therapy, prostatic stones were decreased in size or resolved in 50% (67).
Testicular microlithiasis (TM) is an uncommon pathologic condition of unclear etiology, which is characterized by calcium deposits within the seminiferous tubules. Zhang et al. has studied infertility patients with and without TM. Their results have showed that CNP may be linked to the development of TM, which may provide a potential target for the diagnosis and treatment of infertility with TM (80).
Mechanisms mediating vascular calcification remain incompletely understood. Some have hypothesized the potential role of CNP in arterial calcification (44,45). Miller et al. cultured nano-sized particles from calcified but not from noncalcified aneurysms. These particles were stained with CNP-specific MAb, recognized by a DNA-specific dye and incorporated radiolabeled uridine, and, after decalcification, they appeared via electron microscopy to contain cell walls (45). Puskas et al. propagated CNP- like spherical particles from 26 of 42 sclerotic aorta and carotid samples and confirmed their nature by dot immunoblot by using CNP-specific MAb, light microscopy, and transmission electronmicroscopy (TEM). [3H]l-aspartic acid was incorporated into high molecular weight compounds of demineralized particles. PCR amplification of 16S rDNA sequences from the particles was unsuccessful using traditional protocols (44). Identification of CNP-like particles at the lesion supports but does not by itself prove the hypothesis that these agents contribute to the pathogenesis of atherosclerosis, especially vascular calcifications. Specific therapies targeting these particles has demonstrated reduced plaque formation, regression of plaques, and improved lipid profiles (81). The potential of anti-CNP treatments are controversial and await larger clinical trials. Epidemiologic studies have implicated antibodies made by the body against CNP to be a strong independent risk factor for coronary artery calcification. Also Hu et al. (82) has cultured CNP-like material from calcified cardiac valves with rheumatic heart disease.
Apatite deposition is not a rare phenomena in pediatry. In an infant with idiopathic arterial calcification of infancy, prenatal diagnosis of arterial calcification was made by ultrasonography and allowed initiation of therapy in utero. Etidronate therapy produced apparent radiographic and ultrasonographic improvement in the degree of vascular calcification (83). Etidronate is a compound, which inhibits CNP replication (55).
Originally, Sedivy and Battistutti (84) reported that CNP promoted crystallization of psammoma bodies in ovarian cancer. Hudelist et al. soon verified the 100% concordance between the expression of CNP and the presence of psammoma bodies in malignant ovarian tumors. In their research, several lines of evidence suggest the involvement of these organisms in the process of biomineralization. Therefore they have concluded that CNP infection of malignant ovarian tissue contributes to mechanisms leading to the formation of calcified deposits known as psammoma bodies (70).
In addition, CNP have been shown to be detected at higher rates in serum of patients with gallstone disease (60), and mitral valve calcification (85), dental calculus, and periodontitis (46,62,63). Others have suggested that CNP may contribute to the development of peripheral neutropathy in HIV-positive patients (86,87) and even osteoporosis (88). All these hypothetical approaches require further investigation.
DETECTION METHODS FOR CNP AND THEIR IN VITRO EFFECT ON MAMMALIAN CELL CULTURES
Methods to diagnose CNP in biologicals, cells, tissues, blood, and urine include immunodetection with CNP-specific MAb, electron microscopy, and culture techniques (89). Because CNP pass through 0.22-μm pore size filters, which exclude most common microbes, filtration is often used to clean up fluid specimens before culture for CNP (89). Replication can be measured by particle counting and OD at 650 nm (55). It has been also shown that growth of the CNP could be detected by specific methods, such as ELISA and turbidity (43).
Calcified and noncalcified forms of CNP have been observed as free, cell-attached, and internalized particles in mammalian cell cultures in vitro (43,72). In our experiments, we have chosen six different fibroblast lines as experimental models, because they are the most ubiquitous cells in the animal body and might be most accessible in wound tissue for invading pathogens with the exception of professional phagocytic leukocytes (72). We have shown that CNP were bound as clusters on the cell surfaces within 15 min. It is concluded that CNP are internalized either by receptor-mediated endocytosis or by a closely related pathway within 12 h (72). We showed that cytotoxicity was dependent on CNP concentration and exposure time. Dying cells always contained numerous ingested CNP. Hybridomas and many lymphocytes were found to be affected by CNP, but considerably higher doses were needed (72).
IN VIVO EFFECTS OF CNP (ANIMAL EXPERIMENTS)
Åkerman et al. reported that radiolabeled (99mTc) viable CNP accumulated in the kidney and appeared in urine after 15 min of their i.v. injection into rabbits. This could be due to the fact that kidneys are the preferred sites for this agent, unlike other known nanoparticles, and the presence of injured epithelium or a nucleus in the kidney/urinary tract provides a preferable niche for CNP to adhere and grow, resulting in biocrystallization (73). A control study in rabbit was performed administering a similar dose of 99mTc-labeled albumin cross-linked particles or tin-technetium nanoparticles as nanocolloids. Nanocolloids were not targeted to kidneys as CNP were (72). Shiekh et al. too observed that CNP, when injected i.v. into rats, were localized in kidneys. In their research they observed regions of chronic inflammation infiltrated in the cortex and medulla, which could be due to damage induced by CNP. The research team has also shown CNP adhering to the surface of the epithelium and their penetration into the epithelial cells (58).
In a small study, Garcia Cuerpo et al. (90) found that translumbar, percutaneous intrarenal injection of CNP (isolated from KS) into rats resulted in KS formation. In addition, Shiekh et al. has examined CNP's role in biocrystallization and in vivo effects on kidney pathology. CaOx monohydrate assay was carried out in the presence of CNP to study biocrystallization. Wistar rats were given an i.v. injection of CNP and the kidneys were examined for pathologic changes. The assay showed accelerated biocrystallization of CaOx in the presence of CNP, indicating them to be efficient candidates for biomineralization. Histopathological studies revealed bacteria induced renal tubular calcifications and various manifestations of infection (58). Their studies confirm that CNP may be involved in the pathogenesis of renal tubular calcification. Such findings are required to prove Koch's postulates linking CNP to other pathologic calcification related diseases.
Schwartz et al. designed an experiment to test the hypothesis that the systemic delivery of planktonic forms of CNP derived from calcified, diseased human tissue, or bovine blood are transmissible particles that exacerbate arterial response to injury. New Zealand White rabbits in which the endothelium was mechanically removed from one carotid artery were injected i.v. with either saline (control), lipopolysaccharide, HA crystals. HA crystals exposed to culture media, or planktonic forms of bovine- or human-derived CNP. They have shown that the systemic administration of planktonic forms of human-derived CNP exacerbated arterial response to injury distinct from that of bovine-derived CNP and other inflammatory agents (91).
BIOLOGIC CLASSIFICATION OF CNP
Despite their potential role in major medical health problems, CNP have not been classified in any taxonomic group due to limited information on their biologic characteristics. Although the biologic characterization of CNP is yet to be fully understood, the precipitation and growth of CaP readily occurs in systems containing trace amounts of CNP, but not in identical control systems lacking CNP (51,54).
Chemical analysis using energy-dispersive x-ray microanalysis (EDX) of these mineral layers shows Ca and P peaks (43). The effectiveness of CNP biomineralization is remarkable: apatite formation in vitro stopped only when the calcium level decreased by 50% from 1.8 to 0.9 mM, and the phosphate levels fell to near zero (47). Our results indicate that the CNP CaP phase can be formed at pH 7.4 consistent with human physiologic phosphate and calcium concentrations. This can be also monitored by 85Sr incorporation and provides a unique model for in vitro studies on calcification (43,47,92).
EVIDENCE FOR SELF-REPLICATION OF CNP
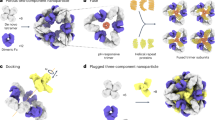
To enhance our understanding of the self-replicating nature of CNP, we investigated their growth using inverted light microscope and BioStation IM time-lapse imaging system (51). The results are in conjunction with previous findings of metabolic activity (54) antibiotic sensitivity (55), antibody specificity (72), morphologic aspects, and infectivity (49,50), all concomitantly validate CNP as live-like self-replicators (51). We found a systematic increase in both the cell-like nanoparticles and the apatite coatings and apatite “igloos” (Fig. 1A). The preferred formation of igloos over apatite-coated cell-like particles occurred when the serum or protein in the nutrient solution was depleted. With sufficient protein, the igloos did not readily form but the cell-like nanoparticles (Fig. 1B) rapidly increased along a flattening growth curve (51). Although the mechanism for the formation of both the cell-like nanoparticles and the apatite crystals and igloos may be entirely nonbiologic, it mimics in many ways the life cycle of typical bacteria. As long as serum proteins, calcium, and phorphorous are present, new cell-like nanoparticles continue to form and apatite continues to precipitate as coatings on these nanoparticles. Igloos continue to form in serum protein depleted media. Controls lacking an initial charge of CNP do not form either the cell-like nanoparticles or the apatite precipitates, even under identical conditions of chemistry and environmental conditions (43,51). Controls salted with inorganic apatite dust particles or albumin addition also do not produce the formation and growth of either the CNP or new apatite precipitates of any type. The “life cycle” of CNP is more complex than previously realized, and includes the formation of pleomorphic cell-like nanoparticles, their acquisition of precipitated apatite coatings built up from extremely small particles of apatite, the formation under a depleted protein environment of much larger apatite structures or igloos, the production of new cell-like nanoparticles within the igloos, the release of these nanoparticles, and a repeat of this cycle (see Fig. 1A). In the case of abundant protein in the media, the igloo phase may be bypassed and the cell-like nanoparticles may be reproduced by budding or by fission (51). This “life cycle” is reproducible, relatively invariant, and predictable and has been observed over more than three decades in “cultures” inoculated with a small amount of initial CNP identical to those on file with the German cell bank (DSM no. 5819–5821; Braunschweig), although some of the details are still being elucidated.
Scanning electron microscopic image of CNP cultured in serum-free condition (A), and in serum containing condition (B). On the left (A), an “igloo” is seen. White arrow shows the igloo opening, and black arrows show the small CNP released from the igloo. On the B, coccobacillar shaped small CNP “cells” are seen. Bars, 1 μm.
CNP BIOFILM
CNP also produce a slime-like biofilm, which may contribute to the “stickiness” of the CNP complex (cell-like vesicles and associated apatite precipitates) in human tissue, circulatory systems, the obstruction of blood flow in arteries (43,45), and on catheter or stent-like artificial prosthesis (unpublished data). This biofilms links together the cell-like nanoparticles and provides anchoring to fixed structures such as arterial walls or kidney tissue. Detailed TEM imaging shows that this biofilms is usually present along with the cell-like vesicles and the precipating apatite (55). The formation of this induced apatitic biofilm formation is dependent on the presence of oxygen (43,93). Additional studies have shown that the formation and growth of this biofilm can be prevented with several antibiotics and antimetabolites, and by high gamma irradiation at sterilizing doses (55,90). Schwartz et al. (94) has shown that CNP biofilm retains some characteristics of conventional bacterial biofilm and requires protein-calcium interactions, although extracellular RNA is not required.
FORMATION OF APATITE
Previous studies have shown that CNP form two distinct forms of apatite. The early-formed apatite consists of extremely small (10's of nanometer) flakes, plates, and crystals, which coat the cell-like organic nanoparticles. Under conditions of serum or protein depletion, these apatite crystals coalesce to form much larger structures (1–10 μm) which are usually concentrically zoned in texture (igloos) (51). These larger structures often contain a central cavity which typically contain multiple cell-like nanoparticles. In some cases, the igloo is partially open allow the egress of these cell-like particles which can then repeat the cycle (43,51). These subspherical units or igloos were identified in most human KS examined (47,95,96). Fourier Transform Infrared Spectroscopy of CNP revealed the mineral as almost identical to bone and apatite KS mineral (54).
In one interesting study, we examined CNP cultures in High Aspect Rotating Vessels designed at the National Aeronautics and Space Administration's Johnson Space Center, which are designed to simulate some aspects of microgravity (97). CNP cultured in that system multiplied 4.6 times faster than under stationary conditions and 3.2 times faster than in shaker flask incubation. Interestingly, the results demonstrated that the degree of apatite crystal formation on the cell-like nanoparticles, and the properties of the apatite are strongly affected by the gravity and other specific culture conditions used (97). Although some researchers believe that microgravity does not affect crystal formation and biomineralization (98), it has been shown that long periods in a microgravity environment does cause loss of bone, and enhance KS formation-like biomineralization disorders in astronauts (99–102). Our data from the experiments would support the hypothesis that reduced gravity may enhance the development of KS by enhancing the growh of CNP (103).
THE CONTROVERSY
CNP were originally called “nanobacteria” because they behaved like known bacteria yet were very small (43). That terminology prompted a search for nucleic acid. (RNA or DNA) (104–107). DNA fragments identified early subsequently were shown to be contamination or DNA absorbed by the particles from their environment (107). As of the present time, no undisputed DNA has been associated with these particles. The original term nanobacteria was therefore dropped by our group as misleading and controversial. We have subsequently used the terms CNP. As we have learned more about their life cycle, we now realize that they consist of a membrane-enclosed vesicle or cell-like particle which has the ability to cause or catalyze precipitation of extremely small HA particles or crystals on the membrane surfaces, and to combine the precipitated apatite into more complex layered concentric structures, which we call igloos because they are often hollow containing newly formed membrane-enclosed vesicles (51). In one version of the life cycle, the hollow igloo is breached and releases the cell-like nanoparticles, which continue to reproduce and precipitate new apatite. In another version of the life cycle, the cell-like nanoparticles precipate fresh apatite on their membrane surfaces but do not form igloos. In both versions, a biofilm may link the nanoparticles together, link them to the igloo, or form an anchor against fluid movement and dispersion. The term CNP refers only to the membrane-enclosed cell-like particle. The associated apatite (both membrane coatings and igloos) and biofilms are separate, but the whole association is termed by us the CNP complex. No previous definition made clear that the membrane-enclosed cell-like particles are not apatite but can exist alone, but are closely associated with both a precipitated apatite coating and with a much larger apatite igloo. Previous definition did not always include the biofilms as separate and distinct part of the complex.
The very small size (50–200 nm) raises the critical question of whether these particles can contain sufficient DNA to operate as a true replicating and metabolizing cell. Maniloff's work suggests that to contain the DNA and proteins needed to function, a cell must be at least 140 nm across (108). However, recently it has been shown that a genome constructed to encode 387 protein coding and 43 structural RNA genes could sustain a viable synthetic cell, a Mycoplasma laboratorium, which can shrink its size below that limitation (109). CNP are also incredibly resistant to heat and other methods that would normally kill bacteria, which makes some scientists wonder if they might be an unusual form of crystal rather than organisms (53). Cisar et al. (107) and Martel et al. (105) presented alternative theories for the experimental findings of earlier CNP studies. They stated that biomineralization previously attributed to CNP may be initiated by nonliving macromolecules and transferred on “subculture” by self-propagating microcrystalline apatite. We are unaware of any report showing the nucleation and growth of inorganic apatite under physiologic conditions. In addition, for inorganic crystallization to continue over prolonged periods of time, conditions of nonequilibrium must exist and be maintained.
Martel et al. (105) have investigated a purported similar material which they termed nanobacteria-like particles (NLP) in their research. It is not clear what the relationship of these NLP is to the original culture deposited by us in the German cell bank, so it is not possible to directly compare results. Cisar et al. also cultured similar particles from serum and human saliva sources and named them nanobacteria with no test comparing them to the original material deposited by us in the cell bank (107). His team verified our findings, and also confirmed the extreme difficulties in performing PCR, but finally suggested his opinion that the culturable particles cannot be bacteria, since they were too small, were not inhibited with a respiratory poison, nucleic acids could not be detected with standard procedures and their protein patterns revealed only few proteins, much less than one would expect from a common bacterium. CNP could not be lysed with lysozyme, proteinase K, several other proteinases, lipases, amylases, alkali, ultrasound, X-press, detergents or solvents (93). In our experiments we needed to use acid or EDTA-like chelators before the analysis, which were the factors for structural change in nucleic acid. It has been our experience that CNP actually inhibit the amplification of added exogeneous classical bacterial DNA by polymerase chain reaction methods. We currently conclude that no convincing evidence exists for the presence of inherent nucleic acid within CNP. PCR analysis using universal primers practically impossible and worthless.
Cisar et al. has not sequenced any proteins. They did not do any DNA work besides staining with Hoechst 33258, where they got the same weakly positive result than we did. Contrary to Dr. Cranton's claims (110), Cisar et al. did not do a PCR phylogenetic analysis using 16S rRNA sequences (107).
As pointed out by Dr. Cranton, apatite can be formed under super-saturating concentrations of calcium and phosphate via several mechanisms (110). To our knowledge, CNP-mediated calcification is the only mechanism to make apatite at nonsaturating levels of calcium and phosphate. Cisar et al. did not follow saturation degree analysis in his studies although saliva is known to be highly super-saturated with calcium and phosphate.
In the study by Martel et al., electron microscopic images from so called NLP morphologically look like the serum protein precipitation formed in long-term serum cultures we have described earlier (89) and are not comparable with our earlier findings (Figs. 2 and 3). Therefore, we find their entire report not comparable with our findings, and the immunostaining tests that they have pursued in their research cannot be comparable with the results we and other laboratories obtained in earlier years. As they have claimed, if the MAb raised for CNP would cross react with a major component of serum, in every experiment containing serum component, the results would be positive. We would recommend using negative controls with no primary antibody and nonspecific MAb in every immunostaining experiments to eliminate false-positive possibilities. Vali et al. (111) have also shown that nanoforms contain apatite-protein complexes and immuno electron microscopy reveals protein antigens in proximity to apatite suggesting a novel form of protein-associated mineralization.
The claims that CNP must be a nonbiogenic (albumin, fetuin-A, and apolipoprotein A1) crystallization still cannot explain the biogenic-like properties of CNP. Some examples of those properties are
-
1
CNP cannot be cultured from every serum sample although each serum contains albumin, fetuin, and apolipopretein.
-
2
TEM examination of CNP cultures have always shown a close association of apatite with submicrometer vesicles (cell-like bodies) enclosed within membraneous structures (51). We and others have always found the presence of these membranous vesicles remaining after the apatite has been chelated and dissolved away with acid or EDTA (51,112,113). Nonbiogenic apatite has larger crystals that are easily dissolved in acidic solution but CNP dissolves very slowly (43).
-
3
When inorganic apatite is added to culture medium (DMEM), it dissolves but CNP introduced to identical media begins and continues to self propagate (51).
-
4
CNP can be cultured in serum-free conditions and be passaged for years with no serum addition (43,51). Therefore, CNP cannot be simple serum protein-derived vesicles with associated crystal formation.
-
5
Inorganic apatite crystals do not stimulate immune response and cause pathologic calcification as CNP do (50,112,114).
-
6
CNP has specific staining properties (72,113). Other components of the serum or growth media do not stain using the same stain.
-
7
CNP are cytotoxic and they have a specific route in vivo (72,73). Serum proteins do not have these properties. Serum protein coated inorganic apatite crystals have been cultured and injected to animals but their route in animals was different (73,112,114).
-
8
CNP have and release endotoxin (72) and thereby stimulate and mediate chronic local inflammatory reactions in atherosclerotic plaque (44). Other suggested explanations (albumin, fetuin-A, and apolipoprotein A1, inorganically precipitated apatite particles) lack this property.
-
9
CNP growth could be prevented with tetracycline, high doses of aminoglycoside antibiotics, EDTA, cytosine arabinoside, 5-fluorouracil, and gamma-irradiation (55).
-
10
CNP structures have been isolated from many diseased tissues and when found, are always similar to other structures from other unrelated patients (44,47,59,60).
-
11
The metabolic potential of CNP was confirmed using a tetrazolium salt detecting dehydrogenase activity (113), and S-methionine incorporation (54). Also, β-mercaptoethanol, known to enhance growth of certain microorganisms and mammalian cells, promoted CNP metabolism and growth (113).
-
12
Polarized light was shown to reduce CNP biofilm formation indicating a light induced metabolic process within the CNP complex (115). Apparently, CNP have metabolic activity, which clearly differentiates them from inorganic crystal formation. Alternatively, the behavior of these nanoparticles closely mimics metabolic activity using a mechanism not understood despite decades of research.
ARE CNP LIVE OR DEAD?
We summarized the properties of CNP that resemble the characteristics of living bacteria and also point out the differences that set them aside as a different and distinct type of small cell-like objects. We raise the question of whether they should be considered living entities. We conclude that CNPs do not fit the typical definition of life, but we suggest that perhaps the typical definition is too restrictive, and a broader definition is required, which encompasses the properties of CNPs.
One property of living systems is their ability to pass on to subsequent generations some information that restricts the new structure and properties to those of the earlier generation. Mutations are allowed, but basic properties should be passed on to subsequent generations. Bullard et al. put to test the “crystals-as-genes” hypothesis. For crystals to resemble genes, there must be more inheritance than mutation in successive generations. However, despite the greatest of care taken to not expose the fresh crystal seeds to atmosphere, and even in the absence of cleavage, new hillocks, “mutations” proliferated so that the detailed structure and morphology of the new crystals differed considerably from the original structure (116). An antibody analog that recognized external structural morphology of the parent crystals would not recognize morphology of the subsequent crystals. By contrast, for more than a decade, CNP have been cultured and passaged under physiologic conditions similar to mammalian culture conditions, without any change in their growth characteristics and specific MAb recognizing epitopes (43,51), a property analogous to the morphology of the crystal surfaces of Bullard et al.
There is truly no universally agreed definition of life. Although the theme of DNA has permeated so deeply in the scientific world, lately, there have also been some contrary publications questioning the concept of the gene as the unit of life (117,118). The theory that life could have started with very simple heterotrophic primordial cells is currently gaining recognition (119). Such could be the case with CNP. These particles consist of an organic membrane surrounding a vesicle. This membrane seems to have the ability to induce apatite precipitation and the formation of complex external structures embodied by the concentric layered larger precipitates including the igloos. The membrane-encased cell-like nanoparticles seem to have the ability to self-replicate while maintaining a complex set of characteristics which are passed on to subsequent generations (51). One hypothesis for the origin of life is that it started with a simple membrane-enclosed vesicle, which allowed or promoted simple chemical reactions across the or through a membrane so that the interior chemistry was somewhat different from the exterior chemistry (119). The membrane may also have had catalytic properties so that it promoted chemical reactions not normally found in its surrounding environment. At some point, the membrane-enclosed vesicle split or budded and a new vesicle was formed. If one of the chemical reactions induced at the membrane surface consisted of precipitation of a salt such as CaP, the system might resemble what we now call CNP. Continuation of this process would lead to growth, increase in complexity, and eventually to the formation of simple DNA. If life began in such a system, the early cell-like version would lack DNA, but would still be considered a living system. Perhaps the CNP can be considered a modern-day analog of such a primitive system, and could be considered a primitive form of life lacking nucleic acid, but still possessing self-replication, membrane-induced chemical reactions, the ability to maintain distinctive characteristics over multiple generations, and the ability to exist and grow over a range of environmental conditions. It is evident that CNP involved in pathologic biomineralization with their distinctive characteristics defy the old standard scientific expectations and definitions of life. Perhaps, an expanded definition of life is appropriate.
CONCLUSIONS
CNP and their associated apatite precipitates and biofilms make up an extremely interesting complex found in many humans. In some ways, it might be considered to be an analog of a possible hypothetical early primitive life form, which developed and reproduced without the benefit of DNA. However, naming an agent as nanoparticles or nanobacteria, living or nonliving but self-replicating, has relatively little meaning with respect to causing disease. The fundamental importance is that these self-replicating special particles that we call CNP are found in blood and in pathogenic calcification and their properties of promoting ready crystallization and growth of Ca minerals are well established. These self-replicating particles may induce calcification and stone formation in vivo because: CNP a) have been detected in human blood, b) are transported from blood into urine and bile as living organisms, c) are renotropic, d) cause apoptotic cell death, e) are present in human stone-isolates, and tissues with calcification, and f) clearly cause KS formation in rats within one month when injected in an intrarenal route. CNP may be the potential reason of poorly understood inflammation that is detected in many pathologic calcification related diseases.
Because CNP have been detected in blood and “sterile” blood products, they should be of interest to the biopharmaceutical industry. For example, CNP have been isolated and cultured from the cultured nasopharyngeal carcinoma epithelia HNE1 cell supernatant (120). Safety of vaccines produced in cell culture by using (bovine) serum or serum-derived materials in culture of the cells, sterilized by filtration is an issue needing thorough risk analysis, and method validation (121).
Only continued research will reveal the nature of CNP and their impact on health and disease. CNP are a good model system to use in developing drugs to alter the likely diverse pathways involved in tissue calcification. The evidence that CNP exist in the human body and are closely associated with many kinds of disease is now overwhelming. Although interesting, future investigations of CNP should not be side tracked by controversies over whether they are alive or not; their potentially very detrimental effect on human health should be the focus of future effort.
Abbreviations
- BA:
-
biological apatite
- CNP:
-
calcifying nanoparticles
- HA:
-
hydroxyapatite
- KS:
-
kidney stone
- MV:
-
matrix vesicles
- NLP:
-
nanobacteria-like particles
- PKD:
-
polycystic kidney disease
- RP:
-
Randall's plaques
- SWL:
-
extracorporeal shock wave lithotripsy
- TEM:
-
transmission electron microscopy
- TM:
-
testicular microlithiasis
References
Tadic D, Peters F, Epple M 2002 Continuous synthesis of amorphous carbonated apatites. Biomaterials 23: 2553–2559
Zaidi AN, Ceneviva GD, Phipps LM, Dettorre MD, Mart CR, Thomas NJ 2005 Myocardial calcification caused by secondary hyperparathyroidism due to dietary deficiency of calcium and vitamin D. Pediatr Cardiol 26: 460–463
Ray M, Dixit A, Singhi P 2002 Nephrogenic diabetes insipidus with intracranial calcification. Indian Pediatr 39: 197–202
Carson DA 1998 An infectious origin of extraskeletal calcification. Proc Natl Acad Sci USA 95: 7846–7847
Pachman LM, Boskey AL 2006 Clinical manifestations and pathogenesis of hydroxyapatite crystal deposition in juvenile dermatomyositis. Curr Rheumatol Rep 8: 236–243
Rezaei-Kanavi M, Javadi MA, Mirbabaei-Ghafghazi F 2009 Intraocular lens calcification; a clinicopathologic report. J Ophthalmic Vis Res 4: 122–124
Peters W, Smith D, Lugowski S, Pritzker K, Holmyard D 2001 Calcification properties of saline-filled breast implants. Plast Reconstr Surg 107: 356–363
Pearle MS, Calhourn EA, Curhan GC 2005 Urologic diseases in America project: urolithiasis. J Urol 173: 848–857
Stamatelou KK, Francis ME, Jones CA, Curhan GC 2003 Time trends in reported prevalence of kidney stones in the United Sates: 1976–1994. Kidney Int 63: 1817–1823
Soucie JM, Coates R, McClellan W, Austin H, Thun M 1996 Relation between geographic variability in kidney stones prevalence and risk factors for stones. Am J Epidemiol 143: 487–495
Brikowski TH, Lotan Y, Pearle MS 2008 Climate-related increase in the prevalence of urolithiasis in the United States. Proc Natl Acad Sci USA 105: 9841–9846
Evan AP 2009 Physiopathology and etiology of stone formation in the kidney and the urinary tract. Pediatr Nephrol. Available at: http://www.springerlink.com/content/41507435785w4261/fulltext.pdf. Accessed January 12, 2010
Rule AD, Bergstralh EJ, Melton LJ III, Li X, Weaver AL, Lieske JC 2009 Kidney stones and the risk for chronic kidney disease. Clin J Am Soc Nephrol 4: 804–811
Momohara C, Tsujihata M, Yoshioka I, Tsujimura A, Nonomura N, Okuyama A 2009 Mechanism underlying the low prevalence of pediatric calcium oxalate urolithiasis. J Urol 182: 1201–1209
Parks JH, Coe FL, Evan AP, Worcester EM 2009 Urine pH in renal calcium stone formers who do and do not increase stone phosphate content with time. Nephrol Dial Transplant 24: 130–136
Klee LW, Brito CG, Lingeman JE 1991 The clinical implications of brushite calculi. J Urol 145: 715–718
El-Abbadi M, Giachelli CM 2005 Arteriosclerosis, calcium phosphate deposition and cardiovascular disease in uremia: current concepts at the bench. Curr Opin Nephrol Hypertens 14: 519–524
Levy RJ, Schoen FJ, Anderson HC, Harasaki H, Koch TH, Brown W, Lian JB, Cumming R, Gavin JB 1991 Cardiovascular implant calcification: a survey and update. Biomaterials 12: 707–714
Demer LL 1995 A skeleton in the atherosclerosis closet. Circulation 92: 2029–2032
Wexler L, Brundage B, Crouse J, Detrano R, Fuster V, Maddahi J, Rumberger J, Stanford W, White R, Taubert K 1996 Coronary artery calcification: pathophysiology, epidemiology, imaging methods, and clinical implications. A statement for health professionals from the American Heart Association. Writing Group. Circulation 94: 1175–1192
Jono S, Shioi A, Ikari Y, Nishizawa Y 2006 Vascular calcification in chronic kidney disease. J Bone Miner Metab 24: 176–181
Blair B, Fabrizio M 2000 Pharmacology for renal calculi. Expert Opin Pharmacother 1: 435–441
Sohshang HL, Singh MA, Singh NG, Singh SR 2000 Biochemical and bacteriological study of urinary calculi. J Commun Dis 32: 216–221
Driessens FC, Verbeeck RM, van Dijk JW 1989 Plasma calcium difference between man and vertebrates. Comp Biochem Physiol A Comp Physiol 93: 651–654
Chen NX, O'Neill KD, Chen X, Moe SM 2008 Annexin-mediated matrix vesicle calcification in vascular smooth muscle cells. J Bone Miner Res 23: 1798–1805
Poole AR, Matsui Y, Hinek A, Lee ER 1989 Cartilage macromolecules and the calcification of cartilage matrix. Anat Rec 224: 167–179
Bailey MT, Pillarisetti S, Xiao H, Vyavahare NR 2003 Role of elastin in pathologic calcification of xenograft heart valves. J Biomed Mater Res A 66: 93–102
Dewanjee MK, Solis E, Lanker J, Mackey ST, Lombardo GM, Tidwell C, Ellefsen RD, Kaye MP 1986 Effect of diphosphonate binding to collagen upon inhibition of calcification and promotion of spontaneous endothelial cell coverage on tissue valve prostheses. ASAIO Trans 32: 24–29
Lewinski N, Colvin V, Drezek R 2008 Cytotoxicity of Nanoparticles. Small 4: 26–49
Pan Y, Neuss S, Leifert A, Fischler M, Wen F, Simon U, Schmid G, Brandau W, Jahnen-Dechent W 2007 Size-Dependent Cytotoxicity of Gold Nanoparticles. Small 3: 1941–1949
Inayat-Hussain SH, Rajab NF, Roslie H, Hussin AA, Ali AM, Annuar BO 2004 Cell death induced by hydroxyapatite on L929 fibroblast cells. Med J Malaysia 59: 176–177
Barroug A, Kuhn LT, Gerstenfeld LC, Glimcher MJ 2004 Interactions of cisplatin with calcium phosphate nanoparticles: in vitro controlled adsorption and release. J Orthop Res 22: 703–708
Telli C, Serper A, Dogan A, Guc D 1999 Evaluation of the cytotoxicity of calcium phosphate root canal sealers by MTT assay. J Endod 25: 811–813
Rauschmann MA, Wichelhaus TA, Stirnal V, Dingeldein E, Zichner L, Schnettler R, Alt V 2005 Nanocrystalline hydroxyapatite and calcium sulphate as biodegradable composite carrier material for local delivery of antibiotics in bone infections. Biomaterials 26: 2677–2684
Tamai N, Myoui A, Tomita T, Nakase T, Tanaka J, Ochi T, Yoshikawa H 2002 Novel hydroxyapatite ceramics with an interconnective porous structure exhibit superior osteoconduction in vivo. J Biomed Mater Res 59: 110–117
Albiar E, Holds JB 1992 Hydroxyapatite orbital implants: indications for use and nursing considerations. J Ophthalmic Nurs Technol 11: 71–76
Mizushima Y, Ikoma T, Tanaka J, Hoshi K, Ishihara T, Ogawa Y, Ueno A 2006 Injectable porous hydroxyapatite microparticles as a new carrier for protein and lipophilic drugs. J Control Release 110: 260–265
Bouladjine A, Al-Kattan A, Dufour P, Drouet C 2009 New advances in nanocrystalline apatite colloids intended for cellular drug delivery. Langmuir 25: 12256–12265
Tazaki J, Murata M, Akazawa T, Yamamoto M, Ito K, Arisue M, Shibata T, Tabata Y 2009 BMP-2 release and dose-response studies in hydroxyapatite and beta-tricalcium phosphate. Biomed Mater Eng 19: 141–146
Matsushima A, Kotobuki N, Tadokoro M, Kawate K, Yajima H, Takakura Y, Ohgushi H 2009 In vivo osteogenic capability of human mesenchymal cells cultured on hydroxyapatite and on beta-tricalcium phosphate. Artif Organs 33: 474–481
Chang WC, Tsou HK, Chen WS, Chen CC, Shen CC 2009 Preliminary comparison of radiolucent cages containing either autogenous cancellous bone or hydroxyapatite graft in multilevel cervical fusion. J Clin Neurosci 16: 793–796
McCarty DJ 2008 Basic Ca phosphate and calcium oxalate crystal deposition diseases. In: Porter RS, Kaplan JL (eds) The Merck Manual Online. Merck & Co., Inc., Whitehouse Station. Available at: http://www.merck.com/mmpe/sec04/ch035/ch035d.html. Accessed at December 5, 2009
Kajander EO, Çiftçioglu N 1998 Nanobacteria: An alternative mechanism for pathogenic intra- and extracellular calcification and stone formation. Proc Natl Acad Sci USA 95: 8274–8279
Puskás LG, Tiszlavicz L, Rázga Z, Torday LL, Krenács T, Papp JG 2005 Detection of nanobacteria-like particles in human atherosclerotic plaques. Acta Biol Hung 56: 233–245
Miller VM, Rodgers G, Charlesworth JA, Kirkland B, Severson SR, Rasmussen TE, Yagubyan M, Rodgers JC, Cockerill FR III, Folk RL, Rzewuska-Lech E, Kumar V, Farell-Baril G, Lieske JC 2004 Evidence of nanobacterial-like structures in calcified human arteries and cardiac valves. Am J Physiol Heart Circ Physiol 287: H1115–H1124
Çiftçioğlu N, McKay DS, Kajander EO 2003 Association between nanobacteria and periodontal disease. Circulation 108: e58–e59
Çiftçioglu N, Björklund M, Kuorikoski K, Bergström K, Kajander EO 1999 Nanobacteria: an infectious cause for kidney stone formation. Kidney Int 56: 1893–1898
Kajander EO, Tahvanien E, Kuronen I, Çiftçioğlu N 1994 Comparison of Staphylococci and novel bacteria-like particles from blood. Zentralbl Bakteriol Suppl 26: 147–149
Çiftçioğlu N, Pelttari A, Kajander EO 1997 Extrardinary growth phases of Nanobacteria isolated from mammalian blood. In: Hoover RB (ed) Instruments, Methods, and Missions for Astrobiology. Proceedings of SPIE, San Diego, CA, 3111: 429–435
Çiftçioğlu N, Aho KM, McKay DS, Kajander EO 2007 Are apatite nanoparticles safe?. Lancet 369: 2078
Mathew G, McKay DS, Ciftçioglu N 2008 Do blood-borne calcifying nanoparticles self-propagate?. Int J Nanomedicine 3: 265–275
Kajander EO, Björklund M, Çiftçioğlu N 1999 Suggestions from observations on nanobacteria isolated from blood. Size Limits of Very Small Microorganisms: Proceedings of a Workshop, Steering Group on Astrobiology of the Space Studies Board, National Research Council, Washington DC, pp 50–55.
Björklund M, Çiftçioğlu N, Kajander EO 1998 Extraordinary survival of nanobacteria under extreme conditions. In: Hoover RB (ed) Instruments, Methods, and Missions for Astrobiology. Proceedings of SPIE, San Jose, CA 3441: 123–129.
Çiftçioğlu N, McKay DS, Mathew G, Kajander EO 2006 Nanobacteria: Nanobacteria: fact or fiction? Characteristics, detection, and medical importance of novel self-replicating, calcifying nanoparticles. J Investig Med 54: 385–394
Çiftçioğlu N, Miller-Hjelle MA, Hjelle JT, Kajander EO 2002 Inhibition of nanobacteria by antimicrobial drugs as measured by a modified microdilution method. Antimicrob Agents Chemother 46: 2077–2086
Çiftçioğlu N 2002 Kidney stone formation: an infectious disease?. Japanese Journal of Urological Surgery 15: 228–232
Kajander EO, Çiftçioğlu N, Aho K, Garcia-Cuerpo E 2003 Characteristics of Nanobacteria and their possible role in stone formation. Urol Res 31: 47–54
Shiekh FA, Khullar M, Singh SK 2006 Lithogenesis: induction of renal calcifications by nanobacteria. Urol Res 34: 53–57
Ciftçioğlu N, Vejdani K, Lee O, Mathew G, Aho KM, Kajander EO, McKay DS, Jones JA, Stoller ML 2008 Association between Randall's plaque and calcifying nanoparticles. Int J Nanomedicine 3: 105–115
Wen Y, Li YG, Yang ZL, Wang XJ, Wei H, Liu W, Miao XY, Wang QW, Huang SF, Yang J, Kajander EO, Çiftçioğlu N 2005 Detection of nanobacteria in serum, bile and gallbladder mucosa of patients with cholecystolithiasis. Chin Med J 118: 421–424
Wen Y, Li YG, Yang ZL, Wang XJ, Wei H, Liu W, Tan AL, Miao XY, Wang QW, Huang SF, Kajander EO, Çiftçioğlu N 2003 Nanobacteria in serum, bile and gallbladder mucosa of cholecystolithiasis patients. Zhonghua Wai Ke Za Zhi 41: 267–270
Çiftçioğlu N, Çiftçioğlu V, Vali H, Turcott E, Kajander EO 1998 Sedimentary rocks in our mouth: Dental pulp stones made by Nanobacteria. In: Hoover RB (ed) Instruments, Methods, and Missions for Astrobiology. Proceedings of SPIE, 3441: 130–135
Zhang SM, Tian F, Jiang XQ, Li J, Xu C, Guo XK, Zhang FQ 2009 Evidence for calcifying nanoparticles in gingival crevicular fluid and dental calculus in periodontitis. J Periodontol 80: 1462–1470
Zeng JF, Zhang W, Jiang HW, Ling JQ 2006 [Isolation, cultivation and initial identification of Nanobacteria from dental pulp stone.]. Zhonghua Kou Qiang Yi Xue Za Zhi 41: 498–501
Zhou Z, Hong L, Shen X, Rao X, Jin X, Lu G, Li L, Xiong E, Li W, Zhang J, Chen Z, Pan J, Song B 2008 Detection of nanobacteria infection in type III prostatitis. Urology 71: 1091–1095. Erratum in: Urology 72:723
Wood HM, Shoskes DA 2006 The role of nanobacteria in urologic disease. World J Urol 24: 51–54
Shoskes DA, Thomas KD, Gomez E 2005 Anti-nanobacterial therapy for men with chronic prostatitis/chronic pelvic pain syndrome and prostatic stones: preliminary experience. J Urol 173: 474–477
Hjelle JT, Miller-Hjelle MA, Poxton IR, Kajander EO, Çiftçioğlu N 2000 Endotoxin and nanobacteria in polycystic kidney disease. Kidney Int 57: 2360–2374
Kajander EO, Çiftçioğlu N, Miller-Hjelle MA, Hjelle JT 2001 Nanobacteria: controversial pathogens in nephrolithiasis and polycystic kidney disease. Curr Opin Nephrol Hypertens 10: 445–452
Hudelist G, Singer CF, Kubista E, Manavi M, Mueller R, Pischinger K, Czerwenka K 2004 Presence of nanobacteria in psammoma bodies of ovarian cancer: evidence for pathogenetic role in intratumoral biomineralization. Histopathology 45: 633–637
Wainwright M 1999 Nanobacteria and associated ‘elementary bodies' in human disease and cancer. Microbiology 145: 2623–2624
Çiftçioglu N, Kajander EO 1998 Interaction of nanobacteria with cultured mammalian cells. Pathophysiology 4: 259–270
Åkerman KK, Kuikka JT, Çiftçioglu N, Parkkinen J, Bergström KA, Kuronen I, Kajander EO 1997 Radiolabeling and in vivo distribution of nanobacteria in rabbit. In: Hoover RB (ed) Instruments, Methods, and Missions for Astrobiology. The International Society for Optical Engineering, Proceedings of SPIE, San Diego, CA, 3111: 436–442.
Randall A 1937 The origin and growth of renal calculi. Ann Surg 105: 1009–1027
Matlaga BR, Coe FL, Evan AP, Lingeman JE 2007 The role of Randall's palques in the pathogenesis of calcium stones. J Urol 177: 31–38
Burton EM, Hanna JD, Mercado-Deane MG 1995 Nephrocalcinosis in a child with autosomal dominant polycystic kidney disease and a prolapsing ectopic ureterocele. Pediatr Radiol 25: 462–465
Muezzinoglu B, Gurbuz Y 2001 Stromal microcalcification in prostate. Malays J Pathol 23: 31–33
Anim JT, Kehinde EO, Prasad A, Prasad A, Mojiminiyi OA, Ali Y, Al-Awadi KA 2006 Relationship between serum prostate specific antigen and the pattern of inflammation in both benign and malignant prostatic disease in Middle Eastern men. Int Urol Nephrol 38: 27–32
Torres Ramirez C, Aguilar Ruiz J, Zuluaga Gomez A 1981 Ultrastructure of primary or endogenous prostatic calculi. Scanning electron microscopic study. Arch Esp Urol 34: 13–22
Zhang QH, Lu GS, Shen XC, Zhou ZS, Fang Q, Zhang X, Li LK, Jin XY, Song B 2009 Nanobacteria may be linked to testicular microlithiasis in infertility. J Androl, in press
Maniscalco BS, Taylor KA 2004 Calcification in coronary artery disease can be reversed by EDTA-tetracycline long-term chemotherapy. Pathophysiology 11: 95–101
Hu YR, Zhao Y, Sun YW, Lü WD, Liu ZL, Li JM, Wu ZS, Tang H, Gao F, Zhou XM 2009 Detection of nanobacteria-like material from calcified cardiac valves with rheumatic heart disease. Cardiovasc Pathol, in press
Bellah RD, Zawodniak L, Librizzi RJ, Harris MC 1992 Idiopathic arterial calcification of infancy: Prenatal and postnatal effects of therapy in an infant. J Pediatr 121: 930–933
Sedivy R, Battistutti WB 2003 Nanobacteria promote crystallization of psammoma bodies in ovarian cancer. APMIS 111: 951–954
Jelic TM, Malas AM, Groves SS, Jin B, Mellen PF, Osborne G, Roque R, Rosencrance JG, Chang HH 2004 Nanobacteria-caused mitral valve calciphylaxis in a man with diabetic renal failure. South Med J 97: 194–198
Sommer AP, Pavlath AE 2005 Primordial proteins and HIV. J Proteome Res 4: 633–636
Pretorius AM, Sommer AP, Aho KM, Kajander EO 2004 HIV and nanobacteria. HIV Med 5: 391–393
Sommer AP 2004 Could reduced bone mineral densities in HIV be caused by nanobacteria?. J Proteome Res 3: 670–672
Miller-Hjelle MA, Hjelle JT, Çiftçioğlu N, Kajander EO 2003 Nanobacteria: methods for growth and identification of this recently discovered calciferous agent. In: Olson WP (ed) Rapid Analytical Microbiology, the Chemistry and Physics of Microbial Identification. Davis Horwood International Publishing, Surrey, United Kingdom, pp 297–312
Garcia-Cuerpo E, Kajander EO, Çiftçioğlu N, Castellano FJ, Correa C, Gonzales J, Mampaso F, Liano F, De Gabiola EG, Berrilero YA 2000 Nanobacteria: un modelo de neo-litogenesis experimental. Arch Esp Urol 53: 291–303
Schwartz MK, Lieske JC, Hunter LW, Miller VM 2009 Systemic injection of planktonic forms of mammalian-derived nanoparticles alters arterial response to injury in rabbits. Am J Physiol Heart Circ Physiol 296: H1434–H1441
Çiftçioğlu N, Björklund M, Kajander EO 1998 Stone formation and calcification by nanobacteria in human body. In: Hoover RB (ed) Instruments, Methods, and Missions for Astrobiology. Proceedings of SPIE, San Jose, CA, 3441: 105–111
Kajander EO, Kuronen I, Åkerman K, Pelttari A, Çiftçioğlu N 1997 Nanobacteria from blood, the smallest culturable autonomously replicating agent on earth. In: Hoover RB (ed) Instruments, Methods, and Missions for the Investigation of Extraterrestrial Microorganisms, Proceedings of SPIE, San Diego, CA, 3111: 420–428
Schwartz MK, Hunter LW, Huebner M, Lieske JC, Miller VM 2009 Characterization of biofilm formed by human-derived nanoparticles. Nanomedicine 4: 931–941
Evan AP, Bledsoe SB, Connors BA, Deng L, Liang L, Shao C, Fineberg NS, Grynpas MD, Stambrook PJ, Youzhi S, Sahota A, Tischfield JA 2001 Sequential analysis of kidney stone formation in the Aprt knockout mouse. Kidney Int 60: 910–923
Naito Y, Ohtawara Y, Kageyama S, Nakano M, Ichiyama A, Fujita M, Suzuki K, Kawabe K, Kino I 1997 Morphological analysis of renal cell culture models of calcium phosphate stone formation. Urol Res 25: 59–65
Çiftçioglu N, Haddad RS, Golden DC, Morrison DR, McKay DS 2005 A potential cause for kidney stone formation during space flights: enhanced growth of nanobacteria in microgravity. Kidney Int 67: 483–491
Becker W, Marxen J, Epple M, Reelsen O 2000 Influence of microgravity on crystal formation in biomineralization. J Appl Physiol 89: 1601–1607
Whitson PA, Pietrzyk RA, Sams CF 2001 Urine volume and its effects on renal stone risk in astronauts. Aviat Space Environ Med 72: 368–372
Pak CY, Hill K, Cintron NM, Huntoon C 1989 Assessing applicants to the NASA flight program for their renal stone-forming potential. Aviat Space Environ Med 60: 157–161
McCarthy ID 2005 Fluid shifts due to microgravity and their effects on bone: a review of current knowledge. Ann Biomed Eng 33: 95–103
Jones JA, Jennings R, Pietryzk R, Ciftcioglu N, Stepaniak P 2005 Genitourinary issues during spaceflight: a review. Int J Impot Res 17: S64–S67
Jones JA, Çiftçioğlu N, Schmid JF, Barr YR, Griffith D 2009 Calcifying nanoparticles (nanobacteria): an additional potential factor for urolithiasis in space flight crews. Urology 73: 210.e11–210.e13
Young JD, Martel J, Young L, Wu CY, Young A, Young D 2009 Putative nanobacteria represent physiological remnants and culture by-products of normal calcium homeostasis. PLoS One 4: e4417
Martel J, Young JD 2008 Purported nanobacteria in human blood as calcium carbonate nanoparticles. Proc Natl Acad Sci USA 105: 5549–5554
Raoult D, Drancourt M, Azza S, Nappez C, Guieu R, Rolain JM, Fourquet P, Campagna B, La Scola B, Mege JL, Mansuelle P, Lechevalier E, Berland Y, Gorvel JP, Renesto P 2008 Nanobacteria are mineralo fetuin complexes. PLoS Pathog 4: e41
Cisar JO, Xu DQ, Thompson J, Swaim W, Hu L, Kopecko DJ 2000 An alternative interpretation of nanobacteria-induced biomineralization. Proc Natl Acad Sci USA 97: 11511–11515
Maniloff J, Nealson KH, Psenner R, Loferer M, Folk RL 1997 Nannobacteria: size limits and evidence. Science 276: 1773–1776
Glass JI, Assad-Garcia N, Alperovich N, Yooseph S, Lewis MR, Maruf M, Hutchison CA 3rd, Smith HO, Venter JC 2006 Essential genes of a minimal bacterium. Proc Natl Acad Sci USA 103: 425–430
Cranton E Rest in peace nanobacteria, you were not alive after all. Available at: http://www.drcranton.com/nanobacteria.htm. Accessed December 5, 2009
Vali H, McKee MD, Çiftçioğlu N, Sears SK, Plows FL, Chevet E, Ghiasi P, Plavsic M, Kajander EO, Zare RN 2001 Nanoforms: a new type of protein-associated mineralization. Geochim Cosmochim Acta 65: 63–74
Miller VM, Hunter LW, Chu K, Kaul V, Squillace PD, Lieske JC, Jayachandran M 2009 Biologic nanoparticles and platelet reactivity. Nanomed 4: 725–733
Kumar V, Farell G, Harrington S, Fitzpatrick L, Rzewuska E, Miller VM, Lieske JC 2006 Cell biology of pathologic renal calcification: contribution of crystal transcytosis, cell-mediated calcification, and nanoparticles. J Investig Med 54: 412–424
Shiekh FA, Miller VM, Lieske JC 2009 Do calcifying nanoparticles promote nephrolithiasis? A review of the evidence. Clin Nephrol 71: 1–8
Sommer AP, Hassinen HI, Kajander EO 2002 Light induced replication of nanobacteria: A preliminary report. J Clin Laser Med Surg 20: 241–244
Bullard T, Freudenthal J, Avagyan S, Kahr B 2007 Test of Cairns-Smith's ‘crystals-as-genes' hypothesis. Faraday Discuss 136: 231–245; discussion 309–328.
Pereto J 2005 Controversies on the origin of life. Int Microbiol 8: 23–31
Pennisi E 2007 DNA study forces rethink of what it means to be a gene. Science 316: 1556–1557
Shapiro R 2006 Small molecule interactions were central to the origin of life. Q Rev Biol 81: 105–125
Zhou HD, Li GY, Yang YX, Li XL, Sheng SR, Zhang WL, Zhao J 2006 Intracellular co-localization of SPLUNC1 protein with nanobacteria in nasopharyngeal carcinoma epithelia HNE1 cells depended on the bactericidal permeability increasing protein domain. Mol Immunol 43: 1864–1871
Çiftçioğlu N, Kuronen I, Åkerman K, Hiltunen E, Laukkanen J, Kajander EO 1997 A new potential threat in antigen and antibody products: nanobacteria. In: Brown F, Burton D, Doherty P, Mekalanos J, Norrby E (eds) Vaccines 97. Cold Spring Harbor Laboratory Press, Cold Spring Harbor, NY, pp 99–103
Author information
Authors and Affiliations
Corresponding author
Additional information
Supported by the National Aeronautics and Space Administration Exobiology Program.
Rights and permissions
About this article
Cite this article
Çiftçioğlu, N., McKay, D. Pathological Calcification and Replicating Calcifying-Nanoparticles: General Approach and Correlation. Pediatr Res 67, 490–499 (2010). https://doi.org/10.1203/PDR.0b013e3181d476ce
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/PDR.0b013e3181d476ce
This article is cited by
-
Calcium orthophosphates (CaPO4): occurrence and properties
Progress in Biomaterials (2016)