Abstract
Rho-kinase (ROCK) inhibitors prevent pulmonary hypertension (PHT) in adult rodents, but little is known about their effects on the neonatal lung. Our objective was to examine the effects of ROCK inhibition on chronic hypoxia (CH)-induced PHT and abnormal lung structure in the neonatal rat. Pups were exposed to air or CH from postnatal d 1-14 while receiving Y-27632 (5 or 10 mg · kg−1 · d−1), fasudil (20 mg · kg−1 · d−1), or saline intraperitoneally. Relative to air, CH-exposed pups had increased pulmonary vascular resistance, right ventricular hypertrophy, arterial medial wall thickening, and abnormal distal airway morphology characterized by septal thinning and decreased secondary septation. Treatment with 10 mg/kg Y-27632 or fasudil attenuated the structural and hemodynamic changes of PHT while having no effect on septal thinning or inhibited secondary septation. In addition, Y-27632 (10 mg/kg) and fasudil augmented CH-induced somatic growth restriction. Pulmonary arteries of CH-exposed pups had increased ROCK activity, up-regulated expression of PDGF-BB and increased smooth muscle DNA synthesis, all of which were attenuated by treatment with 10 mg/kg Y-27632. Systemically administered ROCK inhibitors prevented PHT in the CH-exposed neonatal rat but at the cost of inhibited somatic growth. Limiting effects on vascular remodeling likely resulted, in major part, from attenuated vascular PDGF-BB/β-receptor signaling.
Similar content being viewed by others
Main
Chronic pulmonary hypertension (PHT) that has its origins during fetal or neonatal life is characterized pathologically in both humans (1) and experimental animals (2) by sustained vasoconstriction and rapid remodeling of pulmonary resistance arteries in which hyperplasia of medial wall smooth muscle is a major feature (3,4). Recent studies have implicated the RhoA/Rho-kinase (ROCK) pathway as central to the initiation and perpetuation of chronic PHT (5), based largely on the effects of two ROCK-specific kinase inhibitors: Y-27632 and fasudil (6). ROCK inhibitors have been reported to inhibit pulmonary artery myogenic responses in hypoxia-exposed adult rats (7) and fetal sheep (8) and to reverse sustained pulmonary vasoconstriction in response to hypoxia (9,10), bleomycin (10), or the infusion of vasoconstrictors, such as endothelin-1 (11). Systemic administration of ROCK inhibitors, commenced at the onset of injury, has been reported to prevent PHT induced either by hypoxia (9) or monocrotaline (12) in adult rodents. Finally, pilot studies in humans have shown that systemically administered fasudil acutely decreases pulmonary arterial pressure in adults with idiopathic PHT (13) and in children with PHT secondary to congenital heart disease (14). Together, these findings indicate that ROCK inhibitors hold great promise as a uniquely effective treatment for chronic PHT, however, little is known about their effects on the neonatal lung and pulmonary vasculature.
We have recently reported evidence of RhoA/ROCK pathway activation in the pulmonary arteries of neonatal rats with NO-unresponsive chronic PHT, secondary to either chronic hypoxia (CH) or bleomycin exposure (10). We have further shown that a single bolus of either Y-27632 (15 and 30 mg/kg) or fasudil (30 mg/kg) completely normalized pulmonary vascular resistance (PVR) in both models of chronic neonatal PHT (10). These findings suggest that ROCK is central to sustained vasoconstriction in chronic neonatal PHT, but the question about its role in the structural changes of chronic PHT remains unexplored. We hypothesized that sustained ROCK inhibition from birth would prevent CH-induced vascular remodeling through inhibition of smooth muscle cell (SMC) proliferation. Because growth factors, particularly PDGFs (15,16), are known to mediate smooth muscle proliferation in immature pulmonary vessels (16) and have been implicated in the persistence and progression of chronic PHT in humans (17), we also hypothesized that attenuation of hypoxia-induced SMC proliferation by inhibition of ROCK would be associated with changes in expression of PDGFs and their receptors. Finally, given that ROCK is highly expressed throughout the hypoxia-exposed neonatal rat lung (10) and has been shown to play a major role in proliferation of epithelial cells and other cell types (18,19), we examined whether sustained ROCK inhibition would impact lung growth and alveologenesis.
MATERIALS AND METHODS
Materials.
Y-27632 and fasudil were from Alexis Biochemicals (San Diego, CA) and Enzo Life Sciences (Plymouth Meeting, PA), respectively. Plexiglas animal exposure chambers and automated O2 controllers (Oxy Cycler model A84XOV) were from BioSpherix Ltd. (Redfield, NY). Acids, alcohols, organic solvents, paraformaldehyde, Permount, and Superfrost/Plus microscope slides were from Fisher Scientific (Whitby, ON, Canada). 5-Bromo-2′-deoxyuridine (BrdU) and an in situ BrdU immunostaining kit were from BD Biosciences (Mississauga, ON, Canada). Rabbit polyclonal anti-glyceraldehyde-3-phosphate dehydrogenase (GAPDH, EC 1.2.1.12; sc-25778), PDGF-receptor β (PDGF-Rβ; sc-339), phospho-tyrosine 1021 PDGF-Rβ (sc-12909-R) PDGF-Rα (sc-338), anti-myosin regulatory light chain (MLC20; sc-15370), and goat anti-mouse and -rabbit IgG-biotin secondary antibodies were from Santa Cruz Biotechnology (Santa Cruz, CA). Rabbit polyclonal anti-human PDGF-BB (RB-9257) was from Neomarkers (Fremont, CA). Polyclonal goat anti-human PDGF-AA (AB-221-NA) was from R&D Systems (Minneapolis, MN). A goat anti-rabbit IgG-peroxidase antibody was from Cell Signaling Technology (Beverly, MA). Phos-tag acrylamide was from NARD Institute (Amagasaki City, Japan).
Animal exposures and interventions.
All procedures involving animals were performed in accordance with the standards of the Canadian Council on Animal Care and were approved by the Animal Care Committee of the Sunnybrook Research Institute. Each litter, maintained at n = 10-12 pups to control for nutritional effects, was nursed in either air (21% O2) or hypoxia (13% O2) from postnatal d 1-14, as previously described in detail (2). Pups received either Y-27632 (1 or 2 mg/mL suspended in 0.9% saline vehicle; 5 μL/g body weight = 5 or 10 mg/kg) or an equivalent volume of vehicle by daily intraperitoneal injection. In initial experiments, a higher dose of Y-27632 (15 mg · kg−1 · d−1) previously found to be acutely effective in reversing sustained pulmonary vasoconstriction (10) was found to be fatal in ∼40% of pups by d 14. In additional studies, treatment with a structurally dissimilar and ∼50% less potent ROCK inhibitor (6), fasudil (20 mg · kg−1 · d−1), was also found to increase mortality (∼20% by 14 d). At the end of each 14-d exposure period, pups were either killed by pentobarbital overdose or exsanguinated after anesthesia. Some pups received 20 mg/kg BrdU intraperitoneally 2 h before sacrifice.
Right ventricular hypertrophy (RVH).
RVH was quantified by measuring the right ventricle to left ventricle and septum dry weight ratio, as previously described (20).
Two-dimensional echocardiographic analyses.
Evaluation of PVR was performed in anesthetized animals spontaneously breathing room air, as previously described in detail (2,10). Briefly, a short axis view at the level of the aortic valve was obtained and the pulmonary artery was identified using color flow Doppler. The pulmonary arterial acceleration time (PAAT) was measured as the time from the onset of systolic flow to peak pulmonary outflow velocity and the right ventricular ejection time (RVET) as the time from onset to completion of systolic pulmonary flow. A surrogate of PVR was calculated according to the formula: [1/(PAAT/RVET)].
Immunohistochemistry.
Lungs were inflation-fixed, embedded in paraffin, cut into 5-μm sections and immunostained using an avidin-biotin-peroxidase method, as previously described (2,20). Concentrations of the primary antisera were 1:1000 for PDGF-BB, 1:200 for PDGF-AA, 1:200 for PDGF-Rβ and -Rα, and 1:100 for phospho-PDGF-Rβ. For PDGF-BB, PDGF-Rβ, and phospho-PDGF-Rβ, negative controls were generated by preadsorption with a 10-fold excess of blocking peptide. For quantitation of BrdU-labeled SMC nuclei, eight BrdU-stained sections were examined from each animal (four from the right lung and four from the left), also as previously described (16).
Morphometric analyses.
For all analyses, measurements were carried out on four sections per animal and four animals (representing two litters) per treatment group by an observer blinded to group identity. For assessment of percentage arterial medial wall thickness (%MWT), pulmonary arteries were identified by the presence of both inner and outer elastic lamina using Hart's stain, as previously described in detail (2). Analyses of distal airway structure, including tissue density, mean linear intercept, and secondary crest volume density were carried out on hematoxylin and eosin stained sections, as previously described (21).
Western blot analyses.
Third or fourth generation intrapulmonary arteries were dissected from four litters per group (the pooled vessels of 2-3 animals from each litter representing one sample), lysed in RIPA buffer containing protease and phosphatase inhibitors, fractionated by SDS-PAGE, transferred to polyvinylidene difluoride membranes, blotted and band densities measured as previously described (16). Compensation for differences in protein loading was achieved by reblotting for GAPDH. Dilutions of primary antisera were 1:1000 for PDGF-BB and PDGF-Rβ and 1:5000 for GAPDH. MLC20 phosphorylation, used as a marker of ROCK activity (22), was quantified by Phos-tag acrylamide SDS-PAGE (23), according to a method previously reported in detail (24). After electrophoresis and transfer, membranes were blotted with anti-MLC20 (dilution 1:1000), yielding two bands with Phos-tag (an upper band representing phosphorylated and a lower band representing unphosphorylated MLC20) and only one band when Phos-tag was omitted from the resolving gel. Density of the upper band was expressed as a percentage of the combined densities of both upper and lower bands.
Data presentation and analysis.
All values are expressed as means ± SEM. Statistical significance (p < 0.05) was determined by two-way ANOVA followed by pair-wise multiple comparisons using the Tukey test (SigmaStat, Systat software, San Jose, CA).
RESULTS
Body weight and lung weight.
As shown in Table 1, and reported previously (2), neonatal rats chronically exposed to hypoxia had reduced body weight compared with air-exposed controls. Daily treatment with 10 mg/kg Y-27632 or 20 mg/kg fasudil augmented hypoxia-induced somatic growth restriction but had no effect on body weight in air-exposed animals (Table 1). In contrast, inhibitory effects on growth were not observed in hypoxia-exposed animals treated with 5 mg · kg−1 · d−1 Y-27632. Lung weight was significantly decreased in CH-exposed animals treated with vehicle or 5 mg · kg−1 · d−1 Y-27632, when compared with air, but not in animals treated with 10 mg · kg−1 · d−1 Y-27632 or 20 mg · kg−1 · d−1 fasudil (Table 1).
Right ventricular hypertrophy.
Chronic exposure to hypoxia led to significant RVH, which was almost completely attenuated by treatment with 10 mg · kg−1 · d−1 Y-27632 (Fig. 1A). A similar degree of attenuation of hypoxia-induced RVH was observed after treatment with 20 mg · kg−1 · d−1 fasudil. In contrast, treatment with 5 mg · kg−1 · d−1 Y-27632 had no significant effect on this parameter.
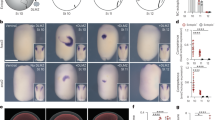
Structural changes of chronic PHT. (A) Right ventricle (RV)/left ventricle + septum (LV + S) weight ratio (n = 8 animals/group), as a marker of RVH, and (B) % arterial medial wall thickness in either air- (open bars) or 13% O2-exposed (closed bars) animals (n = 4 animals/group). *p < 0.05, by two-way ANOVA, compared with air-exposed groups. †p < 0.05, by two-way ANOVA, compared with vehicle-treated hypoxia-exposed group. (C) Representative photomicrographs of Hart's elastin stain in the lungs of pups that were exposed to 21% O2 (air) or 13% O2 (hypoxia) and treated with either 0.9% saline (vehicle), 5 mg · kg−1 · d−1 Y-27632 [Y-27632 (5)] or 10 mg · kg−1 · d−1 Y-27632 [Y-27632 (10)] from postnatal d 1-14. Bar lengths = 25 μm.
Arterial wall remodeling.
As shown in Figure 1B, chronic exposure to hypoxia led to arterial wall remodeling, as demonstrated by increased %MWT. Treatment with 10 mg · kg−1 · d−1 Y-27632 or 20 mg · kg−1 · d−1 fasudil almost completely attenuated the hypoxia-induced increase in %MWT, whereas 5 mg · kg−1 · d−1 Y-27632 had no significant effect. Differences in medial wall thickness between vehicle- and Y-27632-treated groups are further illustrated by Hart's elastin staining in Figure 1C.
Pulmonary vascular resistance.
Chronic exposure to hypoxia increased PVR (Fig. 2), even while breathing room air, as previously reported (2,10). Treatment with either dose of Y-27632 or 20 mg · kg−1 · d−1 fasudil significantly attenuated PVR when compared with hypoxia-exposed vehicle-treated pups but with 10 mg · kg−1 · d−1 Y-27632 having a greater effect than 5 mg · kg−1 · d−1 Y-27632 or fasudil (Fig. 2).
Pulmonary vascular resistance. Inverse PAAT:RVET [1/(PAAT:RVET)] ratio as a surrogate marker of PVR in either air- (open bars) or 13% O2-exposed (closed bars) animals (n = 8 animals/group). *p < 0.01, by two-way ANOVA, compared with respective air group. **p < 0.05, by two-way ANOVA, compared with respective air group. †p < 0.01, by two-way ANOVA, compared with hypoxia groups.
ROCK activity.
As shown in Figure 3, increased % MLC20 phosphorylation (as a marker of increased ROCK activity) was observed in the lungs of animals chronically exposed to hypoxia. Treatment with 10 mg · kg−1 · d−1 Y-27632 normalized ROCK activity in hypoxia-exposed pups, whereas 5 mg · kg−1 · d−1 Y-27632 had no significant effect. A complete attenuation of ROCK activity was also observed in the lungs of animals treated with 20 mg · kg−1 · d−1 fasudil (data not shown).
Rho-kinase activity. (A) Western blot analyses of % myosin regulatory light chain (MLC20) phosphorylation, as a marker of Rho-kinase activity in lung tissue from either air- (open bars) or 13% O2-exposed (closed bars) animals (n = 4 samples/group). *p < 0.01, by two-way ANOVA, compared with respective air-exposed group. †p < 0.05, by two-way ANOVA, compared with other hypoxia-exposed groups. (B) Representative immunoblots for MLC20 either with Phos-tag (upper phosphorylated band and lower unphosphorylated band, both highlighted by arrows) or without Phos-tag (single band).
Arterial smooth muscle proliferation.
As shown in Figure 4, we observed increased SMC proliferation in the medial wall of pulmonary arteries from animals chronically exposed to hypoxia, as demonstrated by increased BrdU labeling. Increased proliferation was completely attenuated by treatment with 10 mg · kg−1 · d−1 Y-27632.
Arterial wall smooth muscle proliferation. (A) Bromodeoxyuridine-labeled medial wall nuclear counts in pulmonary arteries, expressed as a percentage of total medial wall nuclei in either air- (open bars) or 13% O2-exposed (closed bars) animals (n = 4 animals/group). *p < 0.001, by two-way ANOVA, compared with all other groups. (B) Representative high-power photomicrograph of a lung section from a hypoxia-exposed vehicle-treated pup, demonstrating BrdU-positive nuclei (brown stain), highlighted by arrows, two of which are located in the medial wall of a pulmonary artery (pa). Bar length = 25 μm.
PDGF ligand and receptor expression.
Immunohistochemistry was used to screen for changes in pulmonary arterial expression of PDGF-AA and its -Rα, which were found not to differ between air- and hypoxia-exposed groups (data not shown). In contrast, a marked hypoxia-mediated increase in PDGF-BB immunoreactivity on pulmonary arteries was observed (Fig. 5A). Increased PDGF-BB immunoreactivity was attenuated by treatment with 10 mg · kg−1 · d−1, but not by 5 mg · kg−1 · d−1, Y-27632 (Fig. 5A). These findings were confirmed by Western blot analyses on pulmonary arterial tissue-derived protein (Fig. 5B). Chronic exposure to hypoxia also led to increased arterial wall expression of PDGF-Rβ (Fig. 6A and B). In hypoxia-exposed animals, overall expression of PDGF-Rβ (as shown by Western blot analyses; Fig. 6B) was decreased to levels similar to air controls by treatment with 10 mg · kg−1 · d−1 Y-27632. Treatment with 5 mg · kg−1 · d−1 Y-27632 had no effect on PDGF-Rβ expression (data not shown). As shown in Figure 6C, PDGF-Rβ activation, using immunohistochemistry for phospho-tyrosine PDGF-Rβ as a marker (17), was increased by chronic exposure to hypoxia and completely attenuated by treatment with 10 mg · kg−1 · d−1 Y-27632.
PDGF-BB expression. (A) Representative photomicrographs of PDGF-BB immunohistochemistry (brown stain) in pups that were exposed to 21% O2 (air) or 13% O2 (hypoxia) and treated with either 0.9% saline (vehicle) or Y-27632 (5 or 10 mg · kg−1 · d−1) from postnatal d 1-14. Markedly increased arterial wall expression was evident in a hypoxia-exposed vehicle-treated pup, which was completely attenuated by treatment with 10 mg · kg−1 · d−1 Y-27632 [Y-27632 (10)] but not 5 mg · kg−1 · d−1 Y-27632 [Y-27632 (5)]. Inset: lack of staining in a section from a hypoxia-exposed vehicle-treated pup in which the primary antibody was preadsorbed with blocking peptide. Bar lengths = 25 μm. (B) Western blot analyses of arterial PDGF-BB expression, normalized to GAPDH, in either air- (open bars) or 13% O2-exposed (closed bars) animals (n = 4 samples/group). *p < 0.05, by two-way ANOVA, compared with air vehicle and hypoxia-exposed Y-27632-treated group.
PDGF-Rβ expression and activation. (A) Representative photomicrographs of PDGF-Rβ immunohistochemistry (brown stain) in pups that were exposed to 21% O2 (air) or 13% O2 (hypoxia) and treated with either 0.9% saline (vehicle) or Y-27632 (10 mg · kg−1 · d−1) from postnatal d 1-14. Markedly increased arterial wall expression is evident in a hypoxia-exposed vehicle-treated pup. Intensity of staining in the arterial wall was reduced by treatment with Y-27632. Inset: lack of staining in a section from a hypoxia-exposed vehicle-treated pup in which the primary antibody was preadsorbed with blocking peptide. Bar lengths = 50 μm. (B) Western blot analyses of arterial PDGF-Rβ expression, normalized to GAPDH, in either air- (open bars) or 13% O2-exposed (closed bars) animals (n = 4 samples/group). *p < 0.05, by two-way ANOVA, compared with respective air-exposed group. †p < 0.05, by two-way ANOVA, compared with hypoxia-exposed vehicle-treated group. (C) Representative photomicrographs of phospho-tyrosine PDGF-Rβ immunohistochemistry (brown stain), as a marker of PDGF-Rβ activation. Markedly increased immunoreactivity is evident in a hypoxia-exposed vehicle-treated pup, which was completely attenuated by treatment with Y-27632. Inset: lack of staining in a section from a hypoxia-exposed vehicle-treated pup in which the primary antibody was preadsorbed with blocking peptide. Bar lengths = 25 μm.
Distal airway morphology.
We observed septal thinning and “emphysematous” distal airspaces (Fig. 7A) in the lungs of pups chronically exposed to hypoxia, as evidenced by significantly decreased tissue density (Fig. 7B) and increased mean linear intercept (Fig. 7C), consistent with impaired alveolar formation, as previously reported by others (25). Neither Y-27632 nor fasudil had any effect on decreased tissue density induced by hypoxia (Fig. 7B). In contrast, there was a trend toward decreased mean linear intercept (suggestive of augmented secondary septation) in hypoxia-exposed animals treated with Y-27632 (p = 0.065 versus hypoxia-exposed vehicle-treated group). In comparison, treatment with fasudil led to a greater, and statistically significant, decrease in mean linear intercept. These findings led us to examine secondary crest number/unit area (mm2) as a more sensitive marker of secondary septation. As shown in Figure 7D, neither Y-27632 nor fasudil had any impact on decreased secondary crest counts in hypoxia-exposed animals.
Distal airway morphology. (A) Representative low-power photomicrographs of hematoxylin and eosin-stained sections from pups that were exposed to 21% O2 (air) or 13% O2 (hypoxia) and treated with either 0.9% saline (vehicle) or Y-27632 (10 mg · kg−1 · d−1) or fasudil (20 mg · kg−1 · d−1) from postnatal d 1-14. Bar lengths = 250 μm. Morphometric analyses of (B) tissue density, (C) mean linear intercept and (D) secondary crests/mm2 in either air- (open bars) or 13% O2-exposed (closed bars) animals (n = 4 animals/group). *p < 0.05, by two-way ANOVA, compared with respective air-exposed groups. †p < 0.001, by two-way ANOVA, compared with air-exposed groups (n = 4 animals/group).
DISCUSSION
We have previously shown that a single bolus of ROCK inhibitor completely normalized PVR in neonatal rats with established chronic PHT (10). In this study, we extended these findings by examining the effects of sustained ROCK inhibition from birth in preventing the structural changes of chronic hypoxic PHT. We found that systemic treatment with Y-27632 or fasudil at doses, which completely attenuated hypoxia-induced up-regulation of ROCK activity in the lung, attenuated RVH and increased arterial medial wall thickening, but had no impact on changes in distal airways characterized by septal thinning and inhibited secondary septation.
A novel insight from this study was that attenuating effects of Y-27632 on SMC hyperplasia and arterial wall remodeling were paralleled by attenuated hypoxia-induced up-regulation of arterial PDGF-BB and PDGF-Rβ expression and consequently decreased PDGF-Rβ activation. PDGF is made up of homo or heterodimers consisting of A and B chains. PDGF-AA binds exclusively to the PDGF-Rα, whereas PDGF-Rβ binds all isoforms. We have previously reported that PDGF-BB (and not -AA) stimulates proliferation of neonatal rat primary cultured pulmonary arterial smooth muscle (16). Furthermore, we have shown, taking a soluble receptor approach, that increased expression of PDGF-Rβ ligands are critical to pathologic proliferation of neonatal rat pulmonary arterial smooth muscle in vivo (16). Coupled with these earlier observations, our current findings implicate inhibitory effects on the PDGF-BB/Rβ pathway as a major mechanism by which ROCK inhibitors limit pulmonary vascular remodelling. A caveat is that reversal of sustained vasoconstriction, which may be expected to reduce mechanical strain on vascular wall smooth muscle, can itself contribute to changes in PDGF receptor expression/activation and consequent SMC proliferation (26). Therefore, it is not possible, taking the present pharmacological approach, to distinguish indirect consequences of ROCK inhibitor-induced vasodilatation from limiting effects on other ROCK-mediated pathways. Other mechanisms, not explored in this study, by which ROCK inhibitors may have limited vascular remodeling include attenuated vascular production of endothelin-1 (27), inhibited downstream signaling of G-protein-coupled receptor ligands (11,28), and augmented function of the NO/cyclic GMP pathway (29).
Importantly, we observed worsened somatic growth restriction in hypoxia-exposed pups receiving ROCK inhibitors, which has not been reported in mature rodents receiving either Y-27632 or fasudil. In addition, mortality was increased in neonatal rat pups at doses much lower than that previously reported to be nonlethal in adult rodents (9,30,31). Fagan et al. (9) reported increased mortality in adult mice given Y-27632 60 mg · kg−1 · d−1 by s.c. infusion, with no apparent adverse effects reported at 30 mg · kg−1 · d−1. Similarly, Hyvelin et al. treated adult rats with daily enteral boluses of Y-27632 30 mg/kg for up to 3 wk, without apparent toxic effects. Finally, Abe et al. (31) treated hypoxia-exposed mice with daily boluses of fasudil 100 mg/kg, also for 3 wk, without apparent toxicity. Our observation that a dose of Y-27632 (5 mg · kg−1 · d−1) that did not attenuate ROCK activity also had no effect on somatic growth, coupled with the similarity in effects on growth between two structurally dissimilar ROCK inhibitors, strongly suggests that growth restriction was related to systemic inhibition of ROCK, rather than through an off-target effect. Whether growth restriction and mortality arose from the same downstream effect of ROCK inhibition is uncertain, as mortality affected both air- and hypoxia-exposed pups, whereas growth restriction was only seen in those chronically exposed to hypoxia. Systemic hypoperfusion, because of parallel dilating effects of ROCK inhibitors on the systemic vasculature (32) could contribute to both phenomena. Alternatively, ROCK is known to be expressed in both vascular and nonvascular cell types in many tissues (18,19); therefore, it is likely that ROCK modulates proliferation in many cell types and that its role is amplified under hypoxic conditions. Regardless of mechanism, given the apparent increased sensitivity of newborn animals to the systemic effects of ROCK inhibitors and the narrow therapeutic-toxic dose range, our results suggest that systemic treatment with this class of agents should only be undertaken in neonates with caution. A potentially safer and equally efficacious approach may be through delivery of smaller doses directly to the lung, either by intratracheal instillation (similar to exogenous surfactant) or by nebulization, which has been shown in adult animals to limit associated effects on the systemic vasculature (32).
ROCK signaling has been demonstrated to be critical for cardiac morphogenesis (33); however, its role in postnatal lung development has received limited attention. McMurtry et al. (34) reported that chronic PHT was attenuated by enteral (via mother's milk) fasudil over the first 8 wk of life in fawn-hooded rats at Denver altitude. It was further suggested that fasudil enhanced alveolar development, although morphometric analyses were not performed (34). Our observations differ in that neither Y-27632 nor fasudil had any impact on hypoxia-induced septal thinning or alveolarization, as assessed by secondary crest counts. Just as importantly, lung morphology in air-exposed animals was unaffected by either treatment, suggesting that ROCK is not critical to normal postnatal alveolarization. These observations provide a measure of reassurance regarding potential safety of ROCK inhibitors for the treatment of refractory PHT in neonates, should direct delivery to the lung prove efficacious in future studies.
Abbreviations
- BrdU:
-
5-bromo-2′-deoxyuridine
- GAPDH:
-
glyceraldehyde-3-phosphate dehydrogenase
- MLC20:
-
myosin regulatory light chain
- %MWT:
-
percentage arterial medial wall thickness
- PAAT:
-
pulmonary arterial acceleration time
- PHT:
-
pulmonary hypertension
- PVR:
-
pulmonary vascular resistance
- ROCK:
-
Rho-kinase
- RVET:
-
right ventricular ejection time
- RVH:
-
right ventricular hypertrophy
- SMC:
-
smooth muscle cell
References
Miniati D 2007 Pulmonary vascular remodeling. Semin Pediatr Surg 16: 80–87
Kantores C, McNamara PJ, Teixeira L, Engelberts D, Murthy P, Kavanagh BP, Jankov RP 2006 Therapeutic hypercapnia prevents chronic hypoxia-induced pulmonary hypertension in the newborn rat. Am J Physiol Lung Cell Mol Physiol 291: L912–L922
Geggel RL, Reid LM 1984 The structural basis of PPHN. Clin Perinatol 11: 525–549
Thibeault DW, Truog WE, Ekekezie II 2003 Acinar arterial changes with chronic lung disease of prematurity in the surfactant era. Pediatr Pulmonol 36: 482–489
Oka M, Fagan KA, Jones PL, McMurtry IF 2008 Therapeutic potential of RhoA/Rho kinase inhibitors in pulmonary hypertension. Br J Pharmacol 155: 444–454
Davies SP, Reddy H, Caivano M, Cohen P 2000 Specificity and mechanism of action of some commonly used protein kinase inhibitors. Biochem J 351: 95–105
Broughton BR, Walker BR, Resta TC 2008 Chronic hypoxia induces Rho kinase-dependent myogenic tone in small pulmonary arteries. Am J Physiol Lung Cell Mol Physiol 294: L797–L806
Tourneux P, Chester M, Grover T, Abman SH 2008 Fasudil inhibits the myogenic response in the fetal pulmonary circulation. Am J Physiol Heart Circ Physiol 295: H1505–H1513
Fagan KA, Oka M, Bauer NR, Gebb SA, Ivy DD, Morris KG, McMurtry IF 2004 Attenuation of acute hypoxic pulmonary vasoconstriction and hypoxic pulmonary hypertension in mice by inhibition of Rho-kinase. Am J Physiol Lung Cell Mol Physiol 287: L656–L664
McNamara PJ, Murthy P, Kantores C, Teixeira L, Engelberts D, van Vliet T, Kavanagh BP, Jankov RP 2008 Acute vasodilator effects of Rho-kinase inhibitors in neonatal rats with pulmonary hypertension unresponsive to nitric oxide. Am J Physiol Lung Cell Mol Physiol 294: L205–L213
Weigand L, Sylvester JT, Shimoda LA 2006 Mechanisms of endothelin-1-induced contraction in pulmonary arteries from chronically hypoxic rats. Am J Physiol Lung Cell Mol Physiol 290: L284–L290
Abe K, Shimokawa H, Morikawa K, Uwatoku T, Oi K, Matsumoto Y, Hattori T, Nakashima Y, Kaibuchi K, Sueishi K, Takeshit A 2004 Long-term treatment with a Rho-kinase inhibitor improves monocrotaline-induced fatal pulmonary hypertension in rats. Circ Res 94: 385–393
Ishikura K, Yamada N, Ito M, Ota S, Nakamura M, Isaka N, Nakano T 2006 Beneficial acute effects of Rho-kinase inhibitor in patients with pulmonary arterial hypertension. Circ J 70: 174–178
Li F, Xia W, Yuan S, Sun R 2009 Acute inhibition of Rho-kinase attenuates pulmonary hypertension in patients with congenital heart disease. Pediatr Cardiol 30: 363–366
Balasubramaniam V, Le Cras TD, Ivy DD, Grover TR, Kinsella JP, Abman SH 2003 Role of platelet-derived growth factor in vascular remodeling during pulmonary hypertension in the ovine fetus. Am J Physiol Lung Cell Mol Physiol 284: L826–L833
Jankov RP, Kantores C, Belcastro R, Yi S, Ridsdale RA, Post M, Tanswell AK 2005 A role for platelet-derived growth factor β-receptor in a newborn rat model of endothelin-mediated pulmonary vascular remodeling. Am J Physiol Lung Cell Mol Physiol 288: L1162–L1170
Perros F, Montani D, Dorfmuller P, Durand-Gasselin I, Tcherakian C, Le Pavec J, Mazmanian M, Fadel E, Mussot S, Mercier O, Herve P, Emilie D, Eddahibi S, Simonneau G, Souza R, Humbert M 2008 Platelet-derived growth factor expression and function in idiopathic pulmonary arterial hypertension. Am J Respir Crit Care Med 178: 81–88
Matsui T, Amano M, Yamamoto T, Chihara K, Nakafuku M, Ito M, Nakano T, Okawa K, Iwamatsu A, Kaibuchi K 1996 Rho-associated kinase, a novel serine/threonine kinase, as a putative target for small GTP binding protein Rho. EMBO J 15: 2208–2216
Amano M, Chihara K, Kimura K, Fukata Y, Nakamura N, Matsuura Y, Kaibuchi K 1997 Formation of actin stress fibers and focal adhesions enhanced by Rho-kinase. Science 275: 1308–1311
Jankov RP, Luo X, Cabacungan J, Belcastro R, Frndova H, Lye SJ, Tanswell AK 2000 Endothelin-1 and O2-mediated pulmonary hypertension in neonatal rats: a role for products of lipid peroxidation. Pediatr Res 48: 289–298
Padela S, Cabacungan J, Shek S, Belcastro R, Yi M, Jankov RP, Tanswell AK 2005 Hepatocyte growth factor is required for alveologenesis in the neonatal rat. Am J Respir Crit Care Med 172: 907–914
Sebbagh M, Renvoize C, Hamelin J, Riche N, Bertoglio J, Breard J 2001 Caspase-3-mediated cleavage of ROCK I induces MLC phosphorylation and apoptotic membrane blebbing. Nat Cell Biol 3: 346–352
Kinoshita E, Kinoshita-Kikuta E, Takiyama K, Koike T 2006 Phosphate-binding tag, a new tool to visualize phosphorylated proteins. Mol Cell Proteomics 5: 749–757
Takeya K, Loutzenhiser K, Shiraishi M, Loutzenhiser R, Walsh MP 2008 A highly sensitive technique to measure myosin regulatory light chain phosphorylation: the first quantification in renal arterioles. Am J Physiol Renal Physiol 294: F1487–F1492
Massaro GD, Olivier J, Massaro D 1989 Short-term perinatal 10% O2 alters postnatal development of lung alveoli. Am J Physiol 257: L221–L225
Li Q, Muragaki Y, Ueno H, Ooshima A 1997 Stretch-induced proliferation of cultured vascular smooth muscle cells and a possible involvement of local renin-angiotensin system and platelet-derived growth factor (PDGF). Hypertens Res 20: 217–223
Yi SL, Kantores C, Belcastro R, Cabacungan J, Tanswell AK, Jankov RP 2006 8-Isoprostane-induced endothelin-1 production by infant rat pulmonary artery smooth muscle cells is mediated by Rho-kinase. Free Radic Biol Med 41: 942–949
Badejo AM Jr, Dhaliwal JS, Casey DB, Gallen TB, Greco AJ, Kadowitz PJ 2008 Analysis of pulmonary vasodilator responses to the Rho-kinase inhibitor fasudil in the anesthetized rat. Am J Physiol Lung Cell Mol Physiol 295: L828–L836
Guilluy C, Sauzeau V, Rolli-Derkinderen M, Guerin P, Sagan C, Pacaud P, Loirand G 2005 Inhibition of RhoA/Rho kinase pathway is involved in the beneficial effect of sildenafil on pulmonary hypertension. Br J Pharmacol 146: 1010–1018
Hyvelin JM, Howell K, Nichol A, Costello CM, Preston RJ, McLoughlin P 2005 Inhibition of Rho-kinase attenuates hypoxia-induced angiogenesis in the pulmonary circulation. Circ Res 97: 185–191
Abe K, Tawara S, Oi K, Hizume T, Uwatoku T, Fukumoto Y, Kaibuchi K, Shimokawa H 2006 Long-term inhibition of Rho-kinase ameliorates hypoxia-induced pulmonary hypertension in mice. J Cardiovasc Pharmacol 48: 280–285
Nagaoka T, Fagan KA, Gebb SA, Morris KG, Suzuki T, Shimokawa H, McMurtry IF, Oka M 2005 Inhaled Rho kinase inhibitors are potent and selective vasodilators in rat pulmonary hypertension. Am J Respir Crit Care Med 171: 494–499
Zhao Z, Rivkees SA 2003 Rho-associated kinases play an essential role in cardiac morphogenesis and cardiomyocyte proliferation. Dev Dyn 226: 24–32
McMurtry IF, Bauer NR, Fagan KA, Nagaoka T, Gebb SA, Oka M 2003 Hypoxia and Rho/Rho-kinase signaling. Lung development versus hypoxic pulmonary hypertension. Adv Exp Med Biol 543: 127–137
Author information
Authors and Affiliations
Corresponding author
Additional information
Supported by Canadian Institutes of Health Research [MOP-84290 (R.P.J.), MOP-15276 (A.K.T.), and MGC-25029 (A.K.T.)].
Rights and permissions
About this article
Cite this article
Ziino, A., Ivanovska, J., Belcastro, R. et al. Effects of Rho-Kinase Inhibition on Pulmonary Hypertension, Lung Growth, and Structure in Neonatal Rats Chronically Exposed to Hypoxia. Pediatr Res 67, 177–182 (2010). https://doi.org/10.1203/PDR.0b013e3181c6e5a7
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/PDR.0b013e3181c6e5a7
This article is cited by
-
Cardiovascular response and sequelae after minimally invasive surfactant therapy in growth-restricted preterm infants
Journal of Perinatology (2020)
-
Sildenafil therapy in bronchopulmonary dysplasia-associated pulmonary hypertension: a retrospective study of efficacy and safety
European Journal of Pediatrics (2015)
-
Rho-kinase inhibitor Y-27632 attenuates pulmonary hypertension in hyperoxia-exposed newborn rats
Acta Pharmacologica Sinica (2013)
-
Beneficial effect of dehydroepiandrosterone on pulmonary hypertension in a rodent model of pulmonary hypertension in infants
Pediatric Research (2013)