Abstract
The cellular aspects of the immunologic development of the fetus during pregnancy have been studied mainly in populations living in economically well developed countries, and there is no data concerning variation of the neonatal cellular immune system in geographically distinct areas with different environments. Here, we report a comparative immunologic marker analysis of the circulating mononuclear cell subsets in unstimulated cord blood of newborns from Gabon and Austria, assessing the activation and maturation status of T and B lymphocytes as well as antigen-presenting cells. Cells and markers hypothesized to be modulated by frequent exposure to microorganisms and parasites such as regulatory T cells and the expression of toll-like receptor 2 on antigen-presenting cells were also studied. We found marked differences in terms of expression of immunologic markers between the two populations, pointing to a comparatively enhanced maturation status of the neonatal immune system in general in the African setting. The observations suggest that environmental factors, including differential exposure to pathogens as well as nutritional differences, may have substantial impact on the development of the fetal immune system.
Similar content being viewed by others
Main
Vaccination is a cost-effective measure for preventing infectious diseases in early life. In an immunologic context, an important issue, concerning more than 353,000 humans born daily (http://www.cia.gov/library/publications/the-world-factbook/index.html), is the development of the immune system during gestation. Available evidence suggests that, genetic predispositions aside, neonatal immune responses reflect the in utero exposure of the fetus to antigens and consequent immune priming (1–9). Clearly, the maternal “environment,” which includes metabolism-, nutrition- and pathogen-related factors, will play a role here. In fact, most investigations to date have focused on in utero exposure to allergens as reflected by altered cord blood mononuclear cell (CBMC) responses to distinct antigens. More general aspects of fetal cellular immunologic development have not been studied extensively, and the possible variation in neonatal cellular immune responses as a function of distinct geographical environmental exposure has not been investigated.
The study described here compared mononuclear blood cell phenotypes of neonates born to mothers living in two geographically distinct environments: a semiurban area in Central Africa and an urban area in Central Europe. The distribution of subsets of mononuclear blood cells and markers known to indicate exposure to antigens (10) or pathogen-associated molecular patterns (PAMPs) (11,12) were studied. Particular attention was given to the regulatory T cells thought to robustly develop in areas where environmental exposure to pathogens is intense (13).
SUBJECTS AND METHODS
Study population.
In the maternity departments of the Albert Schweitzer Hospital and the General Hospital of Lambaréné, Gabon, and the General Hospital in Vienna, Austria, umbilical cord blood was collected after delivery and before placental expulsion into heparin-containing tubes and processed within 8 h after delivery. Eligible women were those who gave vaginal delivery to a full-term singleton child and who met the following criteria 1) absence of signs of acute illness and 2) no history of chronic diseases such as AIDS, diabetes, asthma, or hepatitis. Lambaréné with approximately 20,000 inhabitants situated in a tropical rainforest area, where viral, bacterial, and parasitic infections are endemic (14). HIV was not routinely screened when the study took place, but the prevalence of HIV in childbearing women in Lambaréné was estimated to be <4% from data obtained in the mother-to-child HIV transmission clinic of the Albert Schweitzer Hospital in 2003 (Adegnika A.A., et al., unpublished data).
In Lambaréné and Vienna, the study was approved by the ethics committee of the International Foundation of the Albert Schweitzer Hospital and of the Medical University of Vienna, respectively. Informed consent has been obtained in both places.
Plasmodial parasite detection.
Parasites were detected microscopically in maternal peripheral, placental, or cord blood smears and quantified using a previously described method (15).
CBMC isolation and flow cytometric acquisition.
CBMC were isolated by centrifugation over Ficoll-Hypaque (Apotheek AZL, The Netherlands). Cells were fixed in 3.7% formaldehyde (Sigma Chemical Co.), cryopreserved in 10% DMSO (DMSO, Fluka Chemie, Swiss)-containing medium and stored at −80°C until analysis. This method preserves the exact ex vivo status of the cells. For analyses, cryopreserved CBMC were thawed, washed twice with RPMI medium (Invitrogen, Breda, The Netherlands), and diluted in fluorescent-activated cell sorting (FACS) buffer (PBS containing 5% BSA, 1% human serum, and 5% FCS) to a concentration of 1 × 106 cells/mL. For staining, cells were incubated with 20 μL (diluted 1:2 up to 1:200) specific monoclonal antibodies (mAb) for 30 min in the dark on ice. Then cells were washed twice with FACS buffer for extracellular staining or with permeabilization buffer (eBioscience, ITK Diagnostics BV, The Netherlands) for intracellular staining. mAb were added to each incubation step in optimal dilutions. Finally, the cells were resuspended in 150 μL FACS buffer, and stored in the dark at 4°C until analysis.
The mAb (all Becton Dickinson, San Jose, CA) used in this study were specific for cluster differentiation (CD) and were conjugated to fluorescein isothiocyanate for CD3, CD4, CD19, CD25, CD27, CD38, lin (lineage marker-negative) 1-, Forkhead box P (Foxp) 3; phycoerythrin for CD3, CD8, CD28, CD69, CD152, T2.5, blood dendritic cell antibody (BDCA)-4; peridinin chlorophyll a protein for CD4, CD8, CD14; or allophycocyanin for BDCA1, CD3, CD5, CD25. mAb were purchased from eBioscience, Inc., San Diego, CA and from Miltenyi Biotec, Bergisch Gladbach, Germany to identify the different cell subsets. mAb were diluted to an optimal concentration in FACS buffer (for extracellular stainings) or in eBioscience permeabilization buffer for intracellular staining. A minimum of 50,000 events for each cell preparation was acquired using a FACSCalibur flow cytometer (Becton Dickinson, San Jose, CA) equipped with a 488-nm Argon and a 635-nm diode laser, allowing four-color fluorescence data acquisition.
Analysis of flow cytometric data.
T cell subsets were defined as cells expressing CD4+ (T helper cells) and CD4+ and CD25++ (regulatory T cells). Additional markers to define regulatory T cells included cytotoxic Tlymphocyte a ntigen (CTLA)-4 (CD152) and Foxp3. CD4+ cells were further characterized using antibodies to CD38, CD27, and CD28. B cells were identified as those expressing CD19, and B cell subsets additionally on CD5 expression. Furthermore, monocyte subsets were characterized by the expression of CD14. Expression of toll-like receptor 2 (TLR 2), mainly expressed on dendritic cells (DC), monocytes, and B cells, was also assessed. A lineage marker antibody cocktail (CD3, CD14, CD16, CD19, CD20, CD56) was used to exclude non-DC (lin−) cell populations. Myeloid (mDC) and plasmacytoid (pDC) subtypes were identified, respectively, as BDCA-1+ and BDCA-4+ cells within the lin− cells. Results were expressed as the percentage of positive cells within the selected gate or as geometric mean fluorescence intensity index (GMFI) as for a measure of the expression level per cell. However, when all cells in a given gate expressed a given marker, only the GMFI could be presented, and conversely, when a distinct subpopulation of cells could be identified, no GMFI measurements were determined.
Statistical analysis.
The statistical analyses were performed with the SPSS software package version 14 (SPSS Inc., Chicago, IL). For normally distributed data, t-test was used for comparison of continuous variables and Pearson's χ2 test for comparison of proportions. For variables that were not normally distributed data, the nonparametric Mann-Whitney U-test was used to determine the differences between variables and Spearman's test for correlations. Differences were considered statistically significant at the level of p < 0.05.
RESULTS
Description of study population.
The study population comprised of 51 Gabonese and 26 Austrian women and their offspring. The population characteristics are listed in Table 1. The groups were comparable for parity as well as newborn's gender but not for maternal age and newborn weight at birth. Because of, at times, technical insufficiencies, not all 51 Gabonese samples could be used in every staining. Plasmodium falciparum infection at delivery was found in 15 of the Gabonese women (29%).
Composition of cord blood cell populations.
The comparison of the different cell populations in the two groups indicated significant differences in mononuclear cell subsets (Table 2). There was no difference between the proportions of CD3+ cells, but the percentage of CD8+ cells was higher in Gabonese CBMC samples, whereas the percentage of CD4+ cells was significantly higher in Austrian CBMC (Table 2). There were no differences in percentages of B lymphocytes (CD19+ cells), but Gabonese had significantly higher percentage of monocytes (CD14+ cells). Lastly, we found a significantly higher percentage of mDC (lin−, BDCA1+ cells) in Gabonese CBMC but a significantly lower proportion of pDC (lin−, BDCA4+ cells) in the same samples compared with Austrian CBMC (Table 2).
Maturation status of lymphocytes in cord blood.
A panel of markers for T cells (CD27, CD28, CD38, CD69) and B cells (CD5) was used to assess their relative maturation status. In Gabon cord, CD4+ cells' expression of CD38 was significantly lower than in Austria, as was the expression of the two activation markers, CD27 (Fig. 1) and CD28 (11% versus 43%, p < 0.001). The proportion of CD4+ cells expressing CD69, a marker for recently activated cells, however, did not differ between the two populations. The loss of expression of CD5 on CD19+ cells indicates antigen exposure. In Gabon CBMC contained a significantly higher percentage of CD5− B cells than in Austria (Fig. 1).
Markers for regulatory T cells subset in cord blood.
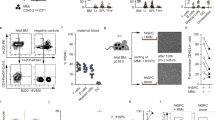
The characterization of CD4+ T cells with a regulatory phenotypic profile relied on the use of antibodies with specificity for cell surface (CD25, CD152) and intranuclear (Foxp3) markers. The percentage of CD4+ cells expressing high levels of CD25 (CD25++) was significantly lower in CBMC from Gabonese compared with Austrians (0.04% versus 0.08%, p = 0.004) and, as shown in Figure 2, the same pattern applied to the expression of both CD152 (CLTA-4) and Foxp3 in the subpopulation of CD4+CD25++ cells. Of note, the expression of CD152 (CTLA-4) and Foxp3 by CD4+CD25++ cells was markedly higher than that of CD4+CD25+ cells in CBMC of both Gabonese and Austrians (Fig. 3), suggesting that, although not specifically determined here, CD4+CD25++ cells are indeed likely to display regulatory function. We noted a significant correlation between %CD25++ and %CD69+ positive CD4 cells (r = 0.521, p = 0.001, Spearman correlation) suggesting that most CD25++ cells are recently activated cells; however, as we did not have staining data for CD69 and CD25 on the same cells, we do not know whether the regulatory T cells are recently activated or not.
The percentage of CD152 (CLTA-4) and Foxp3 expression by the subpopulation of CD4+CD25++ cells in Austrian and Gabonese CBMC. The top, bottom and line through the middle of the box correspond to the 75th, 25th, and 50th percentile, respectively. The whiskers correspond to 10th and 90th percentile. **p < 0.001.
The expression of CD152 (CTLA-4) (A) and Foxp3 (B) by CD4+ cells in Austrian and Gabonese CBMC. The top, bottom and line through the middle of the box correspond to the 75th, 25th, and 50th percentile, respectively. The whiskers correspond to 10th and 90th percentile. p values are indicated. **p < 0.001, †p = 0.004.
Expression of toll-like receptor 2 on B cells, monocytes, and dendritic cells.
We assessed the expression of TLR 2 because i) it is known to recognize the broadest array of PAMPs and ii) a well-characterized and directly labeled anti-TLR 2 antibody is commercially available. The percentage of cells expressing TLR 2 and the mean level of TLR 2 expression per cell are given in Fig. 4. In Gabon CBMC, monocytes showed a significantly lower level of TLR 2 expression, whereas the percentage of TLR 2+ B cells was significantly higher than in Austria, but the percentage of TLR 2+ mDCs was significantly lower in Gabonese compared with Austrians.
The percentage of cells expressing TLR 2 on myeolide dendritic cells (BDCA1+cells) (A) and on CD19+ B cells (B) and the level (geometric mean) of TLR 2 expression per cell on CD14+ monocytes (A) is shown. The top, bottom and line through the middle of the box correspond to the 75th, 25th, and 50th percentile, respectively. The whiskers correspond to 10th and 90th percentile. p values are indicated. **p < 0.001, †p = 0.005.
Associations between dendritic cells, T cell activation markers, and T regulatory cells.
Because DCs are considered to play an essential role in the activation of naive T cells, we determined their relationship with the different T cell phenotypes examined. Significant associations were found only in CBMC from Gabonese, in which BDCA4+ (pDCs) but not BDCA1+ (mDCs) cell percentages were correlated with the level of expression of CD27 on CD4+ cells (p < 0.001, r = 0.66). With respect to regulatory T cell phenotypes, the percentages of both BDCA1+ and BDCA4+ cells were correlated with the level of expression of Foxp3 in CD4+CD25++ cells (BDCA1: r = 0.56, p = 0.011, BDCA4: r = 0.48, p = 0.033).
DISCUSSION
Cord blood cells from African and European neonates showed remarkable differences in terms of activation and maturation of the B and T cell compartment and in distribution of cell subsets and the expression of pattern recognition receptors. The data obtained from the Austrian group were in agreement with data from a study on cord blood of Italian newborns (16). In our study, Gabonese neonates showed a lower expression of costimulatory markers, CD27 and CD28, within the CD4 compartment compared with Austrians. As these markers have been shown to be down-regulated on antigen-experienced cells (17), the results suggest that neonatal T cells from Gabonese are highly differentiated from a naive phenotype. Additionally, the expression of CD38, a multifunctional protein, known to be highly expressed on thymic and unprimed cord blood CD4+ T cells (18,19), was also lower in Gabonese. However, CD69 expression, an early activation marker on T cells (20,21), was similar in the two populations, suggesting that stimulations leading to the maturity of the cells might be of a chronic nature.
Not only the CD4+ T cells but also CD19+ B cells were found to be in a mature and adult-like state. B cells carrying the CD5 surface marker (B-1 cells) are considered immature, functionally “naïve,” and constitute a minority subset in adults compared with newborns (22,23). Thus, finding a lower expression of CD5 on B cells within the Gabonese samples might be additional evidence for a further maturation of the fetal immune system in Gabon.
The CD4+ T cells were further analyzed in terms of markers associated with T regulatory cells. One of the best-characterized regulatory T cell subsets are the CD4+ cells expressing high levels of CD25 (CD4 +CD25++) cells, which suppress activated T cells (24–28). The function of CD4+CD25++ T cells is dependent on signaling via the cytotoxic T lymphocyte-associated antigen (CTLA)-4 (CD152), which is constitutively expressed by these regulatory T cells (29,30). In addition, regulatory T cells express Foxp3, which is a key transcription factor in their development and function (20). We showed a decreased expression of the percentage of CD4+CD25++ cells and of the intracellular expression of Foxp3 and CD152 within these cells in Gabonese compared with Austrians. In cord blood samples, both from Gabon and Austria, the highest expression of Foxp3 and CD152 was within the CD4+CD25++ group compared with the CD4+CD25+ group suggesting that T regulatory cells may occur particularly in the group of CD4+CD25++ cells. Therefore, our data indicate that regulatory T cells might be less abundant in Gabonese neonates. Interestingly, CD69 expression was correlated with CD25 suggesting that in cords with recently activated CD4+ cells, the regulatory T cell numbers are higher.
In the antigen-presenting compartment, a 2-fold higher percentage of monocytes in the Gabonese was found compared with Austrians. Increased percentages of monocytes have been reported in adults compared with cord samples (31), indicating that higher percentages of monocytes in Gabonese neonates might be a reflection of an “adult-like” immune system. Moreover, the percentage of myeloid DCs was significantly higher in Gabonese compared with Austrian neonates. Recently, a high percentage of mDCs in cord blood of neonates born to mothers with malarial infection has been reported (32). The higher ratio of mDCs to pDCs is also seen in adults experiencing P. falciparum infection that leads to a lower percentage of pDCs (33). Therefore, the higher exposure to pathogens in Gabon, such as P. falciparum, might be leading to an increased percentage of mDCs and lower percentage of pDCs in Gabonese neonates. Here, we found no significant differences in the ratio of mDCs/pDcs in cord of neonates born to plasmodia infected and noninfected mothers; however, we expect that a larger sample size is needed to show a significant effect of malarial infection on the immune system.
Taken together, the mDCs, monocytes, and the activation markers on CD4 cells and results with lower frequency of the regulatory T phenotype in Gabonese support the notion, that the neonatal immune system in Gabon has a more activated/stimulated phenotype compared with the Austrian situation.
Recently, it has been shown that maturing pDCs have an intrinsic ability to inhibit immune responses by inducing IL-10-producing T regulatory cells (34). Although there are no data on cord cells, the lower percentage of pDCs may be one reason for the reduced percentage of regulatory T cells in Gabonese neonates. Whereas there was no correlation for the mDCs, the percentage of pDCs was correlated with the expression of CD27 on CD4+ cells in Gabonese. As the presence of CD27 is thought to indicate a less differentiated CD4 cell, pDCs and not mDCs seems to be associated with markers indicative of lower activation.
TLRs are part of the innate immune system and abundantly expressed by monocytes, DCs as well as B cells. They detect conserved PAMPs of bacteria, parasites, fungi, or viruses (35). For DCs, they play a key role in the initiation of an adaptive immune response by inducing the maturation and cytokine production of DCs (36). Whereas the TLR 2 expression level on monocytes found in Austrians is similar to published expression levels for cord blood monocytes in European neonates (37), we found a lower TLR 2 expression on mDCs and monocytes in Gabonese. This could be the result of TLR 2 down-regulation as activated TLR 2-receptors on monocytes have been shown to be internalized (38). The observation that TLR 2 expression is higher in B cells might be taken as contradicting the findings in monocytes and mDCs; however, it is known that in B cells that have been stimulated via B cell receptors, TLR expression is up-regulated (39–42). The higher percentage of CD5− B cells in Gabonese neonates vouches for a higher degree of B cell receptor engagement and explains the higher expression of TLR 2 on these cells. Regarding TLR expression, a study conducted in children of traditional farmers in Switzerland reported a higher TLR 2 mRNA expression in blood cells of children suggesting that higher exposure to microorganisms in that environment might drive the up-regulation of the TLR 2 expression (43). It is not possible to directly compare our results with that of Lauener et al. because of different measurements used; in our studies, we have analyzed protein expression on cell subsets, whereas they measured mRNA expression levels on total cells in peripheral blood. Moreover, the microorganisms in the farming environment might be very distinct to what is encountered in Gabon, and thus, the effect on TLR expression may also be different. The exact relation of TLR expression and exposure to pathogens is not clear and needs to be clarified by using experimental approaches that examines cells after stimulation with specific ligands derived from different pathogens. With respect to this, when samples originating from Plasmodium-infected subjects were left out of the analysis, the differences in the immunologic profiles between Gabonese and Austrians were still present (a selection of markers is shown in Table 3) indicating that indeed many additional pathogens may contribute to the alteration in the immune system of Gabonese neonates.
The data suggest that Gabonese cells exposed to microbial and parasitic products during fetal life have a more activated immune system. At this stage, there are little regulatory T cells, but later in life (in early childhood), this could lead to increased number of regulatory T cells to keep overt immune activation under control. However, it has to be noted that we only measured phenotype, and functional assays need to be performed in future studies.
In conclusion, the morphologic data we presented need validation by functional data to gain a better insight of the discussed mechanisms. However, the differences found are substantial and suggest that Gabonese neonates have an antigen experienced and mature phenotype as a result of exposure to products from microorganisms and/or parasites highly prevalent in the area. It cannot be excluded that the genetic make up of the two populations or different nutritional intakes during pregnancy may also contribute to the shaping of the neonatal immune system. Larger studies need to be undertaken to allow full understanding of, at mechanistic level, the consequences that an altered immune system of a newborn neonate has on a child's health in early life.
Abbreviations
- BDCA:
-
blood dendritic cell antibody
- CBMC:
-
cord blood mononuclear cells
- CD:
-
cluster of differentiation
- CTLA:
-
cytotoxic T lymphocyte antigen
- FACS:
-
fluorescent-activated cell sorting
- GMFI:
-
geometric mean fluorescence intensity index
- TLR:
-
toll-like receptor
References
Szepfalusi Z, Pichler J, Elsasser S, van Duren K, Ebner C, Bernaschek G, Urbanek R 2000 Transplacental priming of the human immune system with environmental allergens can occur early in gestation. J Allergy Clin Immunol 106: 530–536
Szepfalusi Z, Nentwich I, Gerstmayr M, Jost E, Todoran L, Gratzl R, Herkner K, Urbanek R 1997 Prenatal allergen contact with milk proteins. Clin Exp Allergy 27: 28–35
Prescott SL, Macaubas C, Holt BJ, Smallacombe TB, Loh R, Sly PD, Holt PG 1998 Transplacental priming of the human immune system to environmental allergens: universal skewing of initial T cell responses toward the Th2 cytokine profile. J Immunol 160: 4730–4737
Jones AC, Miles EA, Warner JO, Colwell BM, Bryant TN, Warner JA 1996 Fetal peripheral blood mononuclear cell proliferative responses to mitogenic and allergenic stimuli during gestation. Pediatr Allergy Immunol 7: 109–116
Soboslay PT, Geiger SM, Drabner B, Banla M, Batchassi E, Kowu LA, Stadler A, Schulz Key H 1999 Prenatal immune priming in onchocerciasis-onchocerca volvulus-specific cellular responsiveness and cytokine production in newborns from infected mothers. Clin Exp Immunol 117: 130–137
Pit DS, Polderman AM, Schulz-Key H, Soboslay PT 2000 Prenatal immune priming with helminth infections: parasite-specific cellular reactivity and Th1 and Th2 cytokine responses in neonates. Allergy 55: 732–739
Malhotra I, Mungai P, Muchiri E, Ouma J, Sharma S, Kazura JW, King CL 2005 Distinct Th1- and Th2-Type prenatal cytokine responses to Plasmodium falciparum erythrocyte invasion ligands. Infect Immun 73: 3462–3470
Broen K, Brustoski K, Engelmann I, Luty AJ 2007 Placental Plasmodium falciparum infection: causes and consequences of in utero sensitization to parasite antigens. Mol Biochem Parasitol 151: 1–8
Adkins B, Leclerc C, Marshall-Clarke S 2004 Neonatal adaptive immunity comes of age. Nat Rev Immunol 4: 553–564
Hintzen RQ, de Jong R, Lens SM, Brouwer M, Baars P, van Lier RA 1993 Regulation of CD27 expression on subsets of mature T-lymphocytes. J Immunol 151: 2426–2435
Prabha C, Rajashree P, Sulochana DD 2008 TLR 2 and TLR 4 expression on the immune cells of tuberculous pleural fluid. Immunol Lett 117: 26–34
Hartgers FC, Obeng BB, Kruize YC, Duijvestein M, de Breij A, Amoah A, Larbi IA, van Ree R, Wilson MD, Rodrigues LC, Boakye DA, Yazdanbakhsh M 2008 Lower expression of TLR 2 and SOCS-3 is associated with Schistosoma haematobium infection and with lower risk for allergic reactivity in children living in a rural area in Ghana. PLoS Negl Trop Dis 2: e227
Yazdanbakhsh M, Kremsner PG, van Ree R 2002 Allergy, parasites, and the hygiene hypothesis. Science 296: 490–494
Adegnika AA, Agnandji ST, Chai SK, Ramharter M, Breitling L, Kendjo E, Issifou S, Yazdanbakhsh M, Kombila M, Kremsner PG 2007 Increased prevalence of intestinal helminth infection during pregnancy in a Sub-Saharan African community. Wien Klin Wochenschr 119: 712–716
Planche T, Krishna S, Kombila M, Engel K, Faucher JF, Ngou-Milama E, Kremsner PG 2001 Comparison of methods for the rapid laboratory assessment of children with malaria. Am J Trop Med Hyg 65: 599–602
D'Arena G, Musto P, Cascavilla N, Di Giorgio G, Fusilli S, Zendoli F, Carotenuto M 1998 Flow cytometric characterization of human umbilical cord blood lymphocytes: immunophenotypic features. Haematologica 83: 197–203
Appay V, Rowland-Jones SL 2002 Premature ageing of the immune system: the cause of AIDS?. Trends Immunol 23: 580–585
Imanishi K, Kato H, Fujii H, Uchiyama T 2003 Maturation of adult peripheral blood CD38(+)CD4(+) T cells demonstrated by cytokine production in response to a superantigen, TSST-1. Cell Immunol 222: 89–96
de Vries E, de Bruin-Versteeg S, Comans-Bitter WM, de Groot R, Hop WC, Boerma GJ, Lotgering FK, van Dongen JJ 2000 Longitudinal survey of lymphocyte subpopulations in the first year of life. Pediatr Res 47: 528–537
Bogunia-Kubik K, Natarajan P, Madrigal JA, Cohen SB 2002 The effect of cord blood sera on CD69 expression. Immunol Lett 84: 77–80
López-Cabrera M, Santis AG, Fernández-Ruiz E, Blacher R, Esch F, Sánchez-Mateos P, Sánchez-Madrid F 1993 Molecular cloning, expression, and chromosomal localization of the human earliest lymphocyte activation antigen AIM/CD69, a new member of the C-type animal lectin superfamily of signal-transmitting receptors. J Exp Med 178: 537–547
Bhat NM, Kantor AB, Bieber MM, Stall AM, Herzenberg LA, Teng NN 1992 The ontogeny and functional characteristics of human B-1 (CD5+B) cells. Int Immunol 4: 243–252
Kotiranta-Ainamo A, Apajasalo M, Pohjavuori M, Rautonen N, Rautonen J 1999 Mononuclear cell subpopulations in preterm and full-term neonates: independent effects of gestational age, neonatal infection, maternal pre-eclampsia, maternal betamethason therapy, and mode of delivery. Clin Exp Immunol 115: 309–314
Sakaguchi S 2005 Naturally arising Foxp3-expressing CD25+CD4+ regulatory T cells in immunological tolerance to self and non-self. Nat Immunol 6: 345–352
Sakaguchi S, Sakaguchi N, Asano M, Itoh M, Toda M 1995 Immunologic self-tolerance maintained by activated T cells expressing IL-2 receptor alpha-chains (CD25). Breakdown of a single mechanism of self-tolerance causes various autoimmune diseases. J Immunol 155: 1151–1164
Stephens LA, Mottet C, Mason D, Powrie F 2001 Human CD4(+)CD25(+) thymocytes and peripheral T cells have immune suppressive activity in vitro. Eur J Immunol 31: 1247–1254
Levings MK, Sangregorio R, Roncarolo MG 2001 Human cd25(+)cd4(+) t regulatory cells suppress naive and memory T cell proliferation and can be expanded in vitro without loss of function. J Exp Med 193: 1295–1302
Wing K, Larsson P, Sandström K, Lundin SB, Suri-Payer E, Rudin A 2005 CD4+ CD25+ FOXP3+ regulatory T cells from human thymus and cord blood suppress antigen-specific T cell responses. Immunology 115: 516–525
Shevach EM 2001 Certified professionals: CD4(+)CD25(+) suppressor T cells. J Exp Med 193: F41–F46
Birebent B, Lorho R, Lechartier H, de Guibert S, Alizadeh M, Vu N, Beauplet A, Robillard N, Semana G 2004 Suppressive properties of human CD4+CD25+ regulatory T cells are dependent on CTLA-4 expression. Eur J Immunol 34: 3485–3496
Liu E, Tu W, Law HK, Lau YL 2001 Changes of CD14 and CD1a expression in response to IL-4 and granulocyte-macrophage colony-stimulating factor are different in cord blood and adult blood monocytes. Pediatr Res 50: 184–189
Breitling LP, Fendel R, Mordmueller B, Adegnika AA, Kremsner PG, Luty AJ 2006 Cord blood dendritic cell subsets in African newborns exposed to Plasmodium falciparum in utero. Infect Immun 74: 5725–5729
Pichyangkul S, Yongvanitchit K, Kum-arb U, Hemmi H, Akira S, Krieg AM, Heppner DG, Stewart VA, Hasegawa H, Looareesuwan S, Shanks GD, Miller RS 2004 Malaria blood stage parasites activate human plasmacytoid dendritic cells and murine dendritic cells through a Toll-like receptor 9-dependent pathway. J Immunol 172: 4926–4933
Ito T, Yang M, Wang YH, Lande R, Gregorio J, Perng OA, Qin XF, Liu YJ, Gilliet M 2007 Plasmacytoid dendritic cells prime IL-10-producing T regulatory cells by inducible costimulator ligand. J Exp Med 204: 105–115
Akira S, Uematsu S, Takeuchi O 2006 Pathogen recognition and innate immunity. Cell 124: 783–801
Iwasaki A, Medzhitov R 2004 Toll-like receptor control of the adaptive immune responses. Nat Immunol 5: 987–995
Sadeghi K, Berger A, Langgartner M, Prusa AR, Hayde M, Herkner K, Pollak A, Spittler A, Forster-Waldl E 2007 Immaturity of infection control in preterm and term newborns is associated with impaired toll-like receptor signaling. J Infect Dis 195: 296–302
Triantafilou M, Gamper FG, Haston RM, Mouratis MA, Morath S, Hartung T, Triantafilou K 2006 Membrane sorting of toll-like receptor (TLR)-2/6 and TLR 2/1 heterodimers at the cell surface determines heterotypic associations with CD36 and intracellular targeting. J Biol Chem 281: 31002–31011
Bernasconi NL, Traggiai E, Lanzavecchia A 2002 Maintenance of serological memory by polyclonal activation of human memory B cells. Science 298: 2199–2202
Bernasconi NL, Onai N, Lanzavecchia A 2003 A role for Toll-like receptors in acquired immunity: up-regulation of TLR 9 by BCR triggering in naive B cells and constitutive expression in memory B cells. Blood 101: 4500–4504
Bourke E, Bosisio D, Golay J, Polentarutti N, Mantovani A 2003 The toll-like receptor repertoire of human B lymphocytes: inducible and selective expression of TLR 9 and TLR 10 in normal and transformed cells. Blood 102: 956–963
Lanzavecchia A, Sallusto F 2007 Toll-like receptors and innate immunity in B-cell activation and antibody responses. Curr Opin Immunol 19: 268–274
Lauener RP, Birchler T, Adamski J, Braun-Fahrländer C, Bufe A, Herz U, von Mutius E, Nowak D, Riedler J, Waser M, Sennhauser FH 2002 ALEX study group expression of CD14 and toll-like receptor 2 in farmers' and non-farmers' children. Lancet 360: 465–466
Acknowledgements
The authors thank first and foremost all parents and children for their exceptional devotion to the study. They are grateful to Ms Yvonne Kruize, Ms Yvonne Fillié, and Dr. Franca Hartgers for technical assistance. The authors are indebted to the nurses and midwives in Lambaréné and at General Hospital of Vienna for their assistance in the conduct of this study.
Author information
Authors and Affiliations
Corresponding author
Additional information
Supported by Netherlands Foundation for the Advancement of Tropical Research Grant W93-385 20077; EU-Project GLOFAL “Global View of Food Allergy: opportunities to study the influence of microbial exposure” FP6–2003-Food-2B.
Rights and permissions
About this article
Cite this article
Köhler, C., Adegnika, A., Linden, R. et al. Comparison of Immunological Status of African and European Cord Blood Mononuclear Cells. Pediatr Res 64, 631–636 (2008). https://doi.org/10.1203/PDR.0b013e31818718ba
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/PDR.0b013e31818718ba