Abstract
Medulloblastoma is the most common malignant brain tumor of childhood. Surgery, radiation therapy, and chemotherapy successfully cure many patients, but survivors can suffer long-term toxicities affecting their neurocognitive and growth potential; furthermore, there is no curative therapy in up to 30% of cases, mainly because of our incomplete understanding of many of the underlying molecular and cellular processes. Angiogenesis is a hallmark of the progression of medulloblastoma and, over the last years, investigators have sought to develop effective and less toxic antiangiogenic strategies, including the inhibition or destruction of abnormal blood vessels using either antiangiogenic or vascular disrupting agents. However, the results are conflicting principally because of the complex biology of tumor vasculature and the irregular geometry of the vascular system in real space. In addition, current targets of antiangiogenic therapy, such as vascular endothelial growth factor (VEGF), are thought to be critical for both physiologic and pathologic angiogenesis, and clinical side effects of anti-VEGF therapy are beginning to emerge. We here review the state-of-the-art concerning antiangiogenic targets for medulloblastoma treatment, and discuss the complexity of the vascular system that intrinsically limits the efficacy of current strategies.
Similar content being viewed by others
Main
Cancer is the second leading cause of death among children between ages 1 and 14 y in the United States (1). The most common cancers in children include leukemia, brain and other nervous system cancers, soft tissue sarcomas, non-Hodgkin lymphoma, and renal tumors (1).
Medulloblastoma is an aggressive brain tumor that occurs in the cerebellum of children and young adults (2,3). The term “medulloblastoma” was originally introduced in 1910 by the American pathologist James Homer Wright (4). Bailey and Cushing (2,5) in 1925 hypothesized that medulloblastoma arises from an embryonic neuron-epithelial precursor cell, called “medulloblast.” However, this cell has still not been isolated, leading Rorke (2) to include medulloblastoma in a family of primitive central nervous system (CNS) neoplasia, called neuroectodermal tumors. It has been estimated that medulloblastoma has an incidence of two to five cases per 10,000 persons for year, resulting in about 240 new cases per year in the United States (6).
Medulloblastomas predominantly arise in the roof of the fourth ventricle. They grow to invade through the ependyma in the floor of the ventricle to enter the brain stem. It has been shown that its consistent tendency is to invade the leptomeninges and to spread widely within the CNS via the cerebrospinal fluid (7).
Five histologic subtypes of medulloblastoma have been described (8). In the classic variant, the cells are arranged in sheets, occasionally displaying features of neuroblastic differentiation (8). Desmoplastic medulloblastomas contain nodules of tumor cells that commonly show neurocytic differentiation and are surrounded by collagen rich tissue. A third variant of medulloblastoma has been described that contains large neoplastic cells with pleiomorphic nuclei, prominent nucleoli, and abundant cytoplasm. These tumors, which are also characterized by anaplasia, are named large-cell anaplastic medulloblastomas and are associated with an especially poor prognosis (9). The melanotic and medullomyoblastoma are rare subtypes of medulloblastoma.
Despite the advances in the molecular and cellular biology of medulloblastoma, the genetic alterations involved in the majority of these neoplasia cases are poorly understood (3,10). However, it is now recognized that medulloblastoma represents a valid prototype of how deregulated developmental mechanisms can lead to tumor development and progression (11).
The most observed (in 30–50% of cases) chromosomal abnormality in medulloblastomas is iso-chromosome 17q, in which most of the short arm is lost from two chromosomes 17 and they are then fused head-to-head producing a chromosome with two centromers, little 17p and two 17q arms (12–17). A number of other chromosomal aberrations have been identified including loss of 10q (18,19).
It is indubitable that a predominant contribution to our understanding of medulloblastoma has come from the identification of two genetic syndromes exhibiting a predisposition to medulloblastoma development. Gorlin syndrome (hereditary nevoid basal cell carcinoma syndrome) and familial adenomatous polyposis syndrome arise from mutations in the human patched (PTCH) and APC genes, respectively, and both are associated with medulloblastoma formation (12). It is now well known that the gene products of these two genes take part in interrelated pathways that are fundamental to neural development and cell turnover.
Other genes including Smoothened (SMOH) (20) and Suppressor of fused (SUFU) (21) have been investigated; several genes currently being explored for their potential role in medulloblastoma include the myc family (22,23) and the platelet-derived growth factor (PDGF) receptors and ligands (24,25).
It has been show that normal cells and cancer cells share a variable number of morphologic and behavioral properties (26). Normal embryogenesis and carcinogenesis involve changes in the proliferation, differentiation, motility and death of cells, in addition to neo-vascularization and lymphangiogenesis. Medulloblastoma originates from granule-cell progenitors that are located in the external granular layer of the cerebellum (27). This is a germinal zone harboring actively proliferating progenitor cells originating from the rhombic lip during embryonic development (10). Recent advances in understanding the molecular mechanisms involved in the control of proliferation and differentiation of these precursor cells have shed new light on the molecular pathogenesis of these cancers (10,11).
It is now widely accepted that the Sonic Hedgehog (SHH)–PTCH signaling pathway is a major mitogenic regulator of external granular layer precursor cells (10,28). In brief, Purkinje cells are the main source of the glycoprotein SHH during cerebellum development. Secreted SHH binds to the receptor PTCH, which is mainly expressed on external granular layer precursor cells and activates the pathway by relieving the inhibition of SMOH (10). This results in the activation of target genes, such as PTCH itself and the Gli family of transcription factors. It has been demonstrated that the crucial role of SHH in granule-cell precursor proliferation has recently been linked to cell-cycle control by the demonstration that SHH induces CyclinD1 and CyclinD2 expression during development through N-Myc (10). Progression through the G1 phase of the cell cycle in SHH-treated cerebellar granule neurons is achieved through the activation of D-Cyclins, hyperphosphorylation of Retinoblastoma protein, and activation of E2F transcription factors. It has been shown that mutations to the key mediators of the SHH–PTCH pathway (PTCH, SUFU, and SMOH) occur in 25% of sporadic human medulloblastomas (29), and germline mutations of PTCH cause a familial cancer syndrome that is characterized by medulloblastomas, basal-cell carcinomas, and rhabdomyosarcomas (10,30).
It has also been found that 14% of mice heterozygous for PTCH develop medulloblastoma, probably through haploinsufficiency of the PTCH protein (31), and murine medulloblastoma arising in mice deficient for Parp-1 and p53 (32) over-express Gli1, which is indicative of pathway activation. Although medulloblastoma remains a complex disease with a high mortality, these findings all suggest that probably it may arise from a deregulation of SHH–PTCH signaling in granule-cell precursors. It should be underlined, however, that up until now none of the molecular prognostic markers have been validated for routine clinical use.
CURRENT TREATMENTS OF MEDULLOBLASTOMA
It is indubitable that the recognition of molecular pathways involved in medulloblastoma development and progression could improve the clinical management of this neoplasia, a more accurate prediction of the disease risk could be achieved and new targeted treatments explored (10,11,33). It is now known that the clinical outcome of children with medulloblastoma varies according to age, postoperative tumor residuum, and metastatic stage. This has led to the development of risk-adapted treatment for this neoplasia (8). Children with medulloblastoma are currently distinguished in two groups: a) patients with average risk medulloblastoma which are diagnosed after the age of 3 y with nonmetastatic, and totally or near totally, excise disease, and b) patients who do not meet these criteria as being classified as high risk (8).
Today, surgical removal of the tumor, and adjuvant radiation therapy and chemotherapy represent the treatment of choice for patients with medulloblastoma. The standard dose of radiation therapy is 54–56 Gy to the posterior fossa and 36 Gy to the whole neuroaxis (7,34). Radiation therapy has been shown to prolong survival and result in cures. Because the cancer cells have a high potentiality to reach the cerebrospinal fluid, additional quantities of radiations are usually given to the entire brain and spinal cord. The overwhelming effects on intellectual function, academic achievement, memory, attention, and processing speed caused by current treatments especially in children younger than 8 y have been however well-documented (35,36). It has been shown that younger the child is at the time of irradiation worse is the intellectual outcome. In addition, patients whose disease recurs after combined therapy have a poor chance of being cured. It should be underlined that although different studies have shown the efficacy of high dose chemotherapy, only children with isolated local relapse, chemo sensitive disease, and minimal residual disease at the time of high-dose chemotherapy benefit.
A number of evidences suggest, however, that the prognosis of medulloblastoma is still grim in a significant proportion of patients, and novel therapeutic strategies are needed. Recently, Raffaghello et al. have investigated the expression of HLA class I antigen processing machinery component expression and function in medulloblastoma lesions, to develop effective and less toxic immunotherapeutic strategies (37). They found that multiple defects in the expression of HLA class I-related antigen processing machinery components are present in pediatric medulloblastoma, but not in pediatric noninfiltrating astrocytoma, tested as a model of well-differentiated CNS neoplasia (37). Interestingly, Ahmed et al. have demonstrated that adoptive transfer of HER2-specific T cells may represent a promising immunotherapeutic approach for medulloblastoma (38). Taken together, these findings may pave the way to future development of T cell immunotherapy of medulloblastoma using autologous tumor-specific cytotoxic T lymphocytes.
ANTIANGIOGENESIS IN MEDULLOBLASTOMA: IS IT A HELPFUL APPROACH?
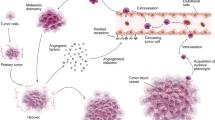
Angiogenesis is a dynamic process highly regulated by a balance of pro- and antiangiogenic molecules. It is now widely accepted that the “angiogenic switch” is “off” when the effects of pro-angiogenic molecules are balanced by that of antiangiogenic molecules, and “on” when the net balance is tipped in favor of angiogenesis (39,40). Pro- and antiangiogenic molecules can be secreted from cancer cells, endothelial cells, stromal cells, blood, and the extracellular matrix (41,42), the relative contributions of which are likely to change with tumor type and site, as well as with tumor growth, regression, and relapse (39).
Several clinical trials of antiangiogenic therapies are being conducted throughout the world, but investigators are still concerned about how to achieve the maximum benefit from them and how to monitor patient response.
Although there have been advances in tumor genetics, knowledge about the tumor microvasculature in medulloblastoma is limited. As the quantification of the microvascular network is important for a better understanding of tumor angiogenesis, Gilhuis et al. performed three-dimensional reconstruction as well as morphometrical analysis of three vascular parameters (number, area, perimeter) in the main histopathological subtypes of medulloblastomas under the hypothesis that the histopathological subtype is reflected by the microvascular architecture (43).
It has been shown that the main feature of the newly generated vasculature is the structural diversity of the vessel sizes, shapes, and connecting patterns (43). Gilhuis et al. found a spectrum of patterns in the microvascular network in medulloblastoma subtypes, ranging from intensely to sparsely vascularized (43). This study clearly shows the disorganized and tortuous nature of the vasculature of some medulloblastoma subtypes (43).
Although still in the very early stages of clinical development, the combination of antiangiogenics with contemporary chemo-radiotherapy regimens has emerged as a feasible and promising approach to many human cancers, including medulloblastoma. It is indubitable that targeting tumor blood vessels has become an attractive anticancer strategy. Unluckily, a large number of phase III trials using nonspecific inhibitors of angiogenesis failed to show a survival advantage (44).
Malignant brain tumors are among the most angiogenic of all human solid tumors. The principal angiogenic factors produced by medulloblastomas are vascular endothelial growth factor (VEGF) and basic fibroblast growth factor (bFGF) (45). It has been shown that VEGF expression and microvessel density (MVD) correlate directly with the degree of malignant characteristics and the overall outcome of tumors (45). One described mechanism by which VEGF and bFGF promote angiogenesis is by stimulating the activity of integrins [alpha]v[beta]3 and [alpha]v[beta]5 on endothelial cells (45–47). Integrin activation and ligand binding result in the propagation of intracellular signals, which maintain endothelial cell survival and enhance proliferation, motility, and capillary sprouting (48,49). As a consequence, targeted antagonism of [alpha]v[beta]3 and [alpha]v[beta]5 integrins inhibit brain tumorgenesis in vivo and may represent an important novel adjuvant therapeutic approach to brain tumors (45).
Huber et al. found that medulloblastomas produce a wide range of angiogenic factors that are, individually or together, likely to play a direct role in tumor growth (50). In 93% of the primary medulloblastoma, more than four different angiogenic factors were detected (50). In particular, VEGF165 and PDGF-A were expressed in 100%, followed by VEGF121 (89%), Ang-1 (86%), Ang-2 (79%), VEGF-C (79%), TGF-α (75%), VEGF189 (75%), and VEGF-B (57%) (50). In addition, bFGF and VEGF-C were also abundantly expressed in primary medulloblastomas (50). These findings suggest that many angiogenic peptides act in concert in the regulation of neovascularization in medulloblastoma. The ubiquitous expression of several angiogenesis stimulators in medulloblastoma indicates that antiangiogenesis therapy may provide a novel strategy that may be particularly useful for highly vascularized tumors. However, it also indicates that antiangiogenesis therapeutic strategies targeting VEGF alone may be insufficient.
Recently, a specific inhibitor of the VEGF receptor family of molecules called AZD2171 has been developed (51). Wedge et al. have shown broad-spectrum activity against a variety of adult human malignancies in preclinical xenograft models through an antiangiogenic mechanism (52). AZD2171 is being studied in a phase 1 trial by the Pediatric Brain Tumor Consortium, and other agents (i.e., bevacizumab, sunitinib, and sorafenib) are in early phase clinical trials for children with cancer (51).
Application of antiangiogenic strategies to pediatric cancers presents special challenges, as the chronic administration strategies envisioned for maintaining tumor dormancy in epithelial cancers are not appropriate in growing children because of the effects on growth plates and possibly on other tissues (51,53,54).
The failure of several targeted agents, however, sent many researchers back to the bench in an attempt to clarify the discrepancy between clinical and preclinical results (43). It has been shown that angiogenesis is a hallmark of the progression of medulloblastoma and, over the last years, investigators have sought to develop effective and less toxic antiangiogenic strategies, including the inhibition or destruction of abnormal blood vessels using either antiangiogenic or vascular disrupting agents. However, the results are conflicting, principally because of the complex biology of tumor vasculature and the irregular geometry of the vascular system in real space (55–58). In addition, current targets of antiangiogenic therapy, such as VEGF, are thought to be critical for both physiologic and pathologic angiogenesis, and clinical side effects of anti-VEGF therapy are beginning to emerge (59).
Tumor vessels are structurally and functionally abnormal (39,40): unlike normal vessels, they are highly disorganized, tortuous, and dilated, and have uneven diameters and excessive branching and shunts. This may be mainly due to the heterogeneous distribution of angiogenic regulators, such as VEGF, bFGF, and angiopoietin (42,60), leading to chaotic tumor blood flow, and hypoxic, and acidic tumoral regions (42,61–63). Moreover, although it is commonly believed that the endothelial cells making-up tumor vessels are genetically stable diploid cells (and thus different from genetically unstable neoplastic cells), tumor vasculature seems to be much more unpredictable (64).
Currently, there are no markers of the net angiogenic activity of a tumor that can help investigators to design specific antiangiogenic treatment strategies (42,65), but it is reasonable to resume that the quantification of various aspects of tumor vasculature may provide an indication of angiogenic activity (55–58).
One often-quantified element of tumor vasculature is MVD, which is used to allow a histologic assessment of tumor angiogenesis (65). The results of studies carried out over the last decade have suggested the value of using tumor MVD as a prognostic index in a wide variety of solid cancers, and it has recently been assumed that MVD may reveal the degree of angiogenic activity in a tumor (50,66–70). However, MVD has a number of substantial limitations, mainly due to the complex biology characterizing tumor vasculature (64) and the highly irregular geometry that the vascular system assumes in real space (55–58), which cannot be measured using the principles of Euclidean geometry because it is only capable of interpreting regular and smooth objects that are almost impossible to find in nature.
THE PHYSICS OF ANGIOGENESIS
Although considerable advances have been made in our molecular and cellular knowledge of the promotion (i.e., the activation of the cell cycle, and deterioration of intercellular communications), progression (i.e., the loss of any brake on cell division and the lack of responsiveness to external control signals), mediation and inhibition of angiogenesis, very little is known about its underlying complex dynamics. It is today recognized that vasculature and more generally tubular organs develop in a wide variety of ways involving many cell processes (71–73).
In mathematical terms, angiogenesis is a nonlinear dynamic system that is discontinuous in space and time, but advances through qualitatively different states. The word state defines the configuration pattern of the system at any given moment, and a dynamic system can be represented as a set of different states and a number of transitions from one state to another over a certain time interval (56).
At least seven critical steps have so far been identified in the sequence of angiogenic events on the basis of sprout formation: a) endothelial cells are activated by an angiogenic stimulus; b) the endothelial cells secrete proteases to degrade the basement membrane and extracellular matrix; c) a capillary sprout is formed as a result of directed endothelial cell migration; d) grows by means of cell mitoses and migration; e) forms a lumen and a new basement membrane; f) two sprouts come together to form a capillary loop; and g) second-generation capillary sprouts begin to form (56). The advancement of these different events generates a complex ramified structure that irregularly fills the surrounding environment.
The human vascular system can be geometrically represented as a fractal network of vessels that irregularly branch with a systematic reduction in their length and diameter (55–58).
Fractal objects are mainly characterized by four properties: a) the irregularity of their shape; b) the self-similarity of their structure; c) their noninteger or fractal dimension; and d) scaling, which means that the measured properties depends on the scale at which they are measured (55–58).
One particular feature of fractal objects is that the schemas defining them are continuously repeated at decreasing orders of magnitude, and so the form of their component parts is similar to that of the whole (58): this property is called self-similarity. Unlike geometrical self-similarity, which only concerns mathematical fractal objects in which every smaller piece is an exact duplicate of the whole, statistical self-similarity concerns all complex anatomical systems, including tumor vasculature. The smaller pieces constituting anatomical entities are rarely identical copies of the whole, but more frequently “similar” to it and, in such systems, the statistical properties of the pieces are proportional to the statistical properties of the whole (55–58).
Dimension is a numerical attribute of an object that does not depend on its process of generation, and has been defined in two ways. The first is the topological or Euclidean dimension, which assigns an integer to every point or set of points in Euclidean space (E): 0 to a point (defined as that which has no part); 1 to a straight line (defined as a length without thickness), 2 to a plane surface (defined as having length and thickness, but no depth); and 3 to three-dimensional figures (a volume defined by length, thickness, and depth). The second was introduced by the mathematicians, Felix Hausdorff and Abram S. Besicovitch, who attributed a real number to every natural object in E lying between the topological dimensions 0 and 3.
Benoit Mandelbrot uses the symbol Dγ to indicates the topological dimension, and the symbol D to indicate that of Hausdorff-Besicovitch (also called the fractal dimension) (55,56). The Dγ and D of all Euclidean figures are coincident (Dγ = D), but this is not true of fractal objects in which D is always >Dγ.
As no anatomical entity corresponds to a regular Euclidean figure, their dimension is always expressed by a noninteger number falling between two integer topological dimensions. In our case, the vascular network has a dimension lying between 2 (plane surface) and 3 (volume), and any two-dimensional section of a vascular system (as in the case of a histologic section) has a dimension lying between 0 (the dimension of a single isolated point) and 2 when the sectioned vessels entirely fill a plane surface (55–58).
Anatomical structures are also hierarchical systems that operate at different spatial and temporal scales, and different patterns can change, appear, or disappear depending on the scale of magnification. A fundamental characteristic is that the process operating at a given scale cannot be important at higher or lower scales.
The irregularity and self-similarity underlying scale changes are the main attributes of the architectural complexity of both normal and pathologic biologic entities. In other words, the shape of a self-similar object does not change when the scale of measure changes because every part of it is similar to the original object; however, the magnitude and other geometrical parameters of an irregular object differ when inspected at increasing resolutions that reveal an increasing number of details. Experimental evidence has shown that the fractal patterns or self-similar structures of biologic tissues can only be observed within the scaling window of an experimentally established measure of length ε1-ε2, within which experimental data sets follow a straight line with a slope (1-D): i.e., the fractal dimension remains invariant at different magnifications (56).
CONCLUDING KEY POINTS
Medulloblastoma is still today a complex disease that affects a high proportion of young people throughout the world (1,2). Although there is a general consensus that a better understanding of disease biology will allow us to develop more effective and less damaging treatments of medulloblastoma, none of the candidate molecular prognostic markers and therapeutic targets have been validated for routine clinical use (33).
This has been mainly attributed to three reasons (33):
-
a
The experimental design. Historically, molecular alterations in medulloblastoma have been identified by isolated research groups studying small number of locally and retrospectively collected tumors.
-
b
The experimental technology. Limitations in experimental technology have slowed our progress toward the identification of the molecular alterations that cause medulloblastoma. In addition, all of the identified markers have not fully validated in larger independent studies, and the relationship of these to other molecular alterations remains unknown.
-
c
Clinical trials structure. The current “three-phase” clinical trials system was designed to assess the toxicity and efficacy of combinations of cytotoxic anticancer treatments. Because the action of these agents was viewed largely as “nonspecific” then, very few resources were invested to collect tumor material for studies of tumor biology and pharmacodynamics.
Current treatment for medulloblastoma includes maximum surgical resection, whole neuroaxis radiation, and chemotherapy. Despite this aggressive treatment, only 60% of children with medulloblastoma will be cured, and most of these will suffer long-term side effects (36).
Although a large number of clinical trials of antiangiogenic therapies are being conducted throughout the world, investigators are still concerned about how to achieve the maximum benefit from them and how to monitor patient response (74).
It has been demonstrated that blood vessels play a primary role in tumor growth and metastasis, but it is now acknowledged that the structure and function of the vasculature is abnormal: the system lacks arterioles, venules, and capillaries, and the interconnections of the vessels are sometimes incomplete. Furthermore, the vessels themselves are irregularly shaped with areas of dilation and constriction, and there is no doubt that these features of the vascular system cannot be geometrically translated into Euclidean terms (55–58).
We have recently pointed out that the fractal geometry of tumor vasculature and its well-known biologic properties mean that it cannot be measured on the basis of MVD estimates alone (55–58). Our observations also support the findings of various authors who have shown the uselessness of MVD as a predictor of the efficacy of antiangiogenic treatment or as a means of stratifying patients in therapeutic trials. It has also been indicated that MVD evaluation is difficult to standardize, MVD of a biopsy does not correlate with the MVD of an entire lesion, and that changes in MVD are not necessarily induced with antiangiogenic drugs (74).
The applicability of quantitative fractal indices makes it possible to explore the range of the morphologic variability of the vasculatures that can be produced in nature, thus increasing the diagnostic importance of such variability in cancer research.
In conclusion, it can be said that:
-
a
Angiogenesis is a process whose large number of molecular players make it complex in time and space.
-
b
Analysis of the angiogenic process allows the identification of a number of different states during a certain time interval, and transitions between two successive states. However, it must be emphasized that the parameter time depends on a large number of variables that are nonlinearly interconnected in a multitude of ways, thus making it extremely difficult to predict the exact time between two states.
-
c
There is an increasing interest in the tumor vasculature as a potential target for antitumor therapy.
-
d
In medulloblastoma, clinical development of antiangiogenics alone or in combination with chemo-radiotherapy is still in its early stages.
-
e
A number of “molecularly targeted” antiangiogenic drugs are available, but their clinical use suffers from several relevant limitations.
-
f
Surrogate biomarkers of angiogenesis are needed to design preclinical studies and clinical trials involving antiangiogenic drugs, alone or in association with other therapies.
-
g
The spatial nonlinear advancement of the states of the promotion, progression, mediation, and inhibition of angiogenesis generates a complex ramified structure, which, in geometrical terms, irregularly fills the surrounding environment.
-
h
The resulting structure and function of the vasculature can be considered abnormal: it lacks an organized structure, with the absence of arterioles, venules, and capillaries; the interconnections of the vessels are sometimes incomplete; and vessels themselves are irregular in shape, with many dilated or constricted areas.
-
i
It is now demonstrated that the heterogeneous distribution of a large number of angiogenic regulators, such as VEGF and bFGF, lead to a chaotic tumor blood flow, and hypoxic and acidic tumoral regions.
-
j
The endothelial cell is a preferential target for therapy because it is common to all solid tumors. However, it should be underlined that endothelial cell phenotypes are differentially regulated in space and time, giving rise to the phenomenon of “endothelial cell heterogeneity” (59,75,76).
-
k
The microenvironment is critical to tumor behavior and in determining its responsiveness to such biologically directed therapies. Identifying which micro-environmental cues are responsible for coordinating these biologic outcomes is critical for our future understanding and development of antiangiogenesis strategies. Tumor angiogenesis involves the tight interplay of tumor cells, endothelial cells, phagocytes, and their secreted factors.
It has been widely shown that these conditions reduce the effectiveness of treatments, modulate the production of pro- and antiangiogenic molecules, and select a subset of more aggressive cancer cells with greater metastatic potential. There is also no doubt that these aspects and its irregular geometry make the new vasculature development and growth one of the most complex structures in biology. It is now recognized that its irregular geometry is a primary cause of the errors in visual interpretation and discordant results concerning the same tumor from different laboratories.
However, the human vascular system can be seen as a natural fractal network of vessels whose irregular branches are systematically shorter and smaller in diameter. The application of Fractal geometry to the quantification of neovascularity may therefore be more suitable to its non-Euclidean nature because irregularly tortuous contours and branching structures, such as those seen in tumoral micro-vessels, can be quantitatively characterized by their fractal dimension.
The use of fractal models of the architecture of tumor vasculature has demonstrated important implications for treatment delivery.
The careful application of fractals may have a significant impact on our understanding of the challenges of cancer treatment delivery. Quantifying the irregular structures present in tumors might help to clarify why treatment is so exasperatingly difficult, a disappointing but important finding; furthermore, we can improve our understanding of the formation of tumoral vasculature and how it differs from that of natural tissue, and thus develop more effective and directed therapies against cancer.
Abbreviations
- bFGF:
-
basic fibroblast growth factor
- D :
-
fractal dimension
- D γ :
-
Euclidean dimension
- MVD:
-
micro-vessel density
- PTCH:
-
human patched gene
- SHH:
-
Sonic Hedgehog signaling pathway
- SMOH:
-
Smoothened gene
References
Jemal A, Siegel R, Ward E, Murray T, Xu J, Thun MJ 2007 Cancer statistics, 2007. CA Cancer J Clin 57: 43–66
Raffel C 2004 Medulloblastoma: molecular genetics and animal models. Neoplasia 6: 310–322
Polkinghorn WR, Tarbell NJ 2007 Medulloblastoma: tumorigenesis, current clinical paradigm, and efforts to improve risk stratification. Nat Clin Pract Oncol 4: 295–304
Wright JH 1910 Neurocytoma or neuroblastoma, a kind of tumor not generally recognized. J Exp Med 12: 556–561
Read TA, Hegedus B, Wechsler-Reya R, Gutmann DH 2006 The neurobiology of neurooncology. Ann Neurol 60: 3–11
Humphreys RP 1983 Posterior cranial fossa brain tumors in children. In: Youmans JR (ed) Neurological Surgery. Saunders, Philadelphia, pp 2733–2752
Matsutani M 2004 Chemoradiotherapy for brain tumors: current status and perspectives. Int J Clin Oncol 9: 471–474
Gilbertson RJ 2004 Medulloblastoma: signaling a change in treatment. Lancet Oncol 5: 209–218
Eberhart CG, Kepner JL, Goldthwaite PT, Kun LE, Duffner PK, Friedman HS, Strother DR, Burger PC 2002 Histopathologic grading of medulloblastomas: a Pediatric Oncology Group study. Cancer 94: 552–560
Marino S 2005 Medulloblastoma: developmental mechanisms out of control. Trends Mol Med 11: 17–22
Grimmer MR, Weiss WA 2006 Childhood tumors of the nervous system as disorders of normal development. Curr Opin Pediatr 18: 634–638
Collins VP 2004 Brain tumours: classification and genes. J Neurol Neurosurg Psychiatry 75: ii2–ii11
Bigner SH, McLendon RE, Fuchs H, McKeever PE, Friedman HS 1997 Chromosomal characteristics of childhood brain tumors. Cancer Genet Cytogenet 97: 125–134
Bigner SH, Mark J, Friedman HS, Biegel JA, Bigner DD 1988 Structural chromosomal abnormalities in human medulloblastoma. Cancer Genet Cytogenet 30: 91–101
Biegel JA, Burk CD, Barr FG, Emanuel BS 1992 Evidence for a 17p tumor related locus distinct from p53 in pediatric primitive neuroectodermal tumors. Cancer Res 52: 3391–3395
Reardon DA, Michalkiewicz E, Boyett JM, Sublett JE, Entrekin RE, Ragsdale ST, Valentine MB, Behm FG, Li H, Heideman RL, Kun LE, Shapiro DN, Look AT 1997 Extensive genomic abnormalities in childhood medulloblastoma by comparative genomic hybridization. Cancer Res 57: 4042–4047
James CD, He J, Carlbom E, Mikkelsen T, Ridderheim PA, Cavenee WK, Collins VP 1990 Loss of genetic information in central nervous system tumors common to children and young adults. Genes Chromosomes Cancer 2: 94–102
Bayani J, Zielenska M, Marrano P, Kwan Ng Y, Taylor MD, Jay V, Rutka JT, Squire JA 2000 Molecular cytogenetic analysis of medulloblastomas and supratentorial primitive neuroectodermal tumors by using conventional banding, comparative genomic hybridization, and spectral karyotyping. J Neurosurg 93: 437–448
Michiels EM, Weiss MM, Hoovers JM, Baak JP, Voute PA, Baas F, Hermsen MA 2002 Genetic alterations in childhood medulloblastoma analyzed by comparative genomic hybridization. J Pediatr Hematol Oncol 24: 205–210
Reifenberger J, Wolter M, Weber RG, Megahed M, Ruzicka T, Lichter P, Reifenberger G 1998 Missense mutations in SMOH in sporadic basal cell carcinomas of the skin and primitive neuroectodermal tumors of the central nervous system. Cancer Res 58: 1798–1803
Taylor MD, Liu L, Raffel C, Hui CC, Mainprize TG, Zhang X, Agatep R, Chiappa S, Gao L, Lowrance A, Hao A, Goldstein AM, Stavrou T, Scherer SW, Dura WT, Wainwright B, Squire JA, Rutka JT, Hogg D 2002 Mutations in SUFU predispose to medulloblastoma. Nat Genet 31: 306–310
Herms J, Neidt I, Luscher B, Sommer A, Schurmann P, Schroder T, Bergmann M, Wilken B, Probst-Cousin S, Hernaiz-Driever P, Behnke J, Hanefeld F, Pietsch T, Kretzschmar HA 2000 C-MYC expression in medulloblastoma and its prognostic value. Int J Cancer 89: 395–402
Grotzer MA, Hogarty MD, Janss AJ, Liu X, Zhao H, Eggert A, Sutton LN, Rorke LB, Brodeur GM, Phillips PC 2001 MYC messenger RNA expression predicts survival outcome in childhood primitive neuroectodermal tumor/medulloblastoma. Clin Cancer Res 7: 2425–2433
MacDonald TJ, Brown KM, LaFleur B, Peterson K, Lawlor C, Chen Y, Packer RJ, Cogen P, Stephan DA 2001 Expression profiling of medulloblastoma: PDGFRA and the RAS/MAPK pathway as therapeutic targets for metastatic disease. Nat Genet 29: 143–152
Gilbertson RJ, Clifford SC 2003 PDGFRB is overexpressed in metastatic medulloblastoma. Nat Genet 35: 197–198
Grizzi F, Di Ieva A, Russo C, Frezza EE, Cobos E, Muzzio PC, Chiriva-Internati M 2006 Cancer initiation and progression: an unsimplifiable complexity. Theor Biol Med Model 3: 37
Reddy AT, Packer RJ 1999 Medulloblastoma. Curr Opin Neurol 12: 681–685
Wechsler-Reya R, Scott MP 2001 The developmental biology of brain tumors. Annu Rev Neurosci 24: 385–428
Zurawel RH, Allen C, Chiappa S, Cato W, Biegel J, Cogen P, de Sauvage F, Raffel C 2000 Analysis of PTCH/SMO/SHH pathway genes in medulloblastoma. Genes Chromosomes Cancer 27: 44–51
Unden AB, Holmberg E, Lundh-Rozell B, Stähle-Bäckdahl M, Zaphiropoulos PG, Toftgård R, Vorechovsky I 1996 Mutations in the human homologue of Drosophila patched (PTCH) in basal cell carcinomas and the Gorlin syndrome: different in vivo mechanisms of PTCH inactivation. Cancer Res 56: 4562–4565
Wetmore C, Eberhart DE, Curran T 2000 The normal patched allele is expressed in medulloblastomas from mice with heterozygous germ-line mutation of patched. Cancer Res 60: 2239–2246
Tong WM, Ohgaki H, Huang H, Granier C, Kleihues P, Wang ZQ 2003 Null mutation of DNA strand break-binding molecule poly(ADP-ribose) polymerase causes medulloblastomas in p53(−/−) mice. Am J Pathol 162: 343–352
Gilbertson RJ, Gajjar A 2005 Molecular biology of medulloblastoma: will it ever make a difference to clinical management?. J Neurooncol 75: 273–278
Verlooy J, Mosseri V, Bracard S, Tubiana AL, Kalifa C, Pichon F, Frappaz D, Chastagner P, Pagnier A, Bertozzi AI, Gentet JC, Sariban E, Rialland X, Edan C, Bours D, Zerah M, Le Gales C, Alapetite C, Doz F 2006 Treatment of high risk medulloblastomas in children above the age of 3 years: a SFOP study. Eur J Cancer 42: 3004–3014
Palmer SL, Reddick WE, Gajjar A 2007 Understanding the cognitive impact on children who are treated for medulloblastoma. J Pediatr Psychol 32: 1040–1049
Gajjar A, Hernan R, Kocak M, Fuller C, Lee Y, McKinnon PJ, Wallace D, Lau C, Chintagumpala M, Ashley DM, Kellie SJ, Kun L, Gilbertson RJ 2004 Clinical, histopathologic, and molecular markers of prognosis: toward a new disease risk stratification system for medulloblastoma. J Clin Oncol 22: 984–993
Raffaghello L, Nozza P, Morandi F, Camoriano M, Wang X, Garre ML, Cama A, Basso G, Ferrone S, Gambini C, Pistoia V 2007 Expression and functional analysis of human leukocyte antigen class I antigen-processing machinery in medulloblastoma. Cancer Res 67: 5471–5478
Ahmed N, Ratnayake M, Savoldo B, Perlaky L, Dotti G, Wels WS, Bhattacharjee MB, Gilbertson RJ, Shine HD, Weiss HL, Rooney CM, Heslop HE, Gottschalk S 2007 Regression of experimental medulloblastoma following transfer of HER2-specific T cells. Cancer Res 67: 5957–5964
Carmeliet P 2005 Angiogenesis in life, disease and medicine. Nature 438: 932–936
Fidler IJ, Ellis LM 2004 Neoplastic angiogenesis—not all blood vessels are created equal. N Engl J Med 351: 215–216
Fukumura D, Xavier R, Sugiura T, Chen Y, Park EC, Lu N, Selig M, Nielsen G, Taksir T, Jain RK, Seed B 1998 Tumor induction of VEGF promoter activity in stromal cells. Cell 94: 715–725
Tandle A, Blazer DG III, Libutti SK 2004 Antiangiogenic gene therapy of cancer: recent developments. J Transl Med 2: 22
Gilhuis HJ, van der Laak JA, Pomp J, Kappelle AC, Gijtenbeek JM, Wesseling P 2006 Three-dimensional (3D) reconstruction and quantitative analysis of the microvasculature in medulloblastoma and ependymoma subtypes. Angiogenesis 9: 201–208
Jain RK, di Tomaso E, Duda DG, Loeffler JS, Sorensen AG, Batchelor TT 2007 Angiogenesis in brain tumours. Nat Rev Neurosci 8: 610–622
MacDonald TJ, Taga T, Shimada H, Tabrizi P, Zlokovic BV, Cheresh DA, Laug WE 2001 Preferential susceptibility of brain tumors to the anti-angiogenic effects of an alpha(v) integrin antagonist. Neurosurgery 48: 151–157
Brooks PC, Clark RA, Cheresh DA 1994 Requirement of vascular integrin alpha v beta 3 for angiogenesis. Science 264: 569–571
Hynes RO 1987 Integrins: a family of cell surface receptors. Cell 48: 549–554
Howe A, Aplin AE, Alahari SK, Juliano RL 1998 Integrin signaling and cell growth control. Curr Opin Cell Biol 10: 220–231
Longhurst CM, Jennings LK 1998 Integrin-mediated signal transduction. Cell Mol Life Sci 54: 514–526
Huber H, Eggert A, Janss AJ, Wiewrodt R, Zhao H, Sutton LN, Rorke LB, Phillips PC, Grotzer MA 2001 Angiogenic profile of childhood primitive neuroectodermal brain tumours/medulloblastomas. Eur J Cancer 37: 2064–2072
Maris JM, Courtright J, Houghton PJ, Morton CL, Gorlick R, Kolb EA, Lock R, Tajbakhsh M, Reynolds CP, Keir ST, Wu J, Smith MA 2008 Initial testing of the VEGFR inhibitor AZD2171 by the pediatric preclinical testing program. Pediatr Blood Cancer 50: 581–587
Wedge SR, Kendrew J, Hennequin LF, Valentine PJ, Barry ST, Brave SR, Smith NR, James NH, Dukes M, Curwen JO, Chester R, Jackson JA, Boffey SJ, Kilburn LL, Barnett S, Richmond GH, Wadsworth PF, Walker M, Bigley AL, Taylor ST, Cooper L, Beck S, Jurgensmeier JM, Ogilvie DJ 2005 AZD2171: a highly potent, orally bioavailable, vascular endothelial growth factor receptor-2 tyrosine kinase inhibitor for the treatment of cancer. Cancer Res 65: 4389–4400
Hahnfeldt P, Panigrahy D, Folkman J, Hlatky L 1999 Tumor development under angiogenic signaling: a dynamical theory of tumor growth, treatment response, and postvascular dormancy. Cancer Res 59: 4770–4775
O'Reilly MS, Holmgren L, Chen C, Folkman J 1996 Angiostatin induces and sustains dormancy of human primary tumors in mice. Nat Med 2: 689–692
Grizzi F, Colombo P, Taverna G, Chiriva-Internati M, Cobos E, Graziotti P, Muzzio PC, Dioguardi N 2007 Geometry of human vascular system: is it an obstacle for quantifying anti-angiogenic therapies?. Appl Immunohistochem Mol Morphol 15: 134–139
Grizzi F, Russo C, Colombo P, Franceschini B, Frezza EE, Cobos E, Chiriva-Internati M 2005 Quantitative evaluation and modeling of two-dimensional neovascular network complexity: the surface fractal dimension. BMC Cancer 5: 14
Grizzi F, Colombo P, Barbieri B, Franceschini B, Roncalli M, Chiriva-Internati M, Muzzio PC, Dioguardi N 2001 Correspondence re: E. Sabo et al., Microscopic analysis and significance of vascular architectural complexity in renal cell carcinoma. Clin Cancer Res 7: 553–537. Clin Cancer Res 7:3305–3307
Di Ieva A, Grizzi F, Ceva-Grimaldi G, Russo C, Gaetani P, Aimar E, Levi D, Pisano P, Tancioni F, Nicola G, Tschabitscher M, Dioguardi N, Baena RR 2007 Fractal dimension as a quantitator of the microvasculature of normal and adenomatous pituitary tissue. J Anat 211: 673–680
Seaman S, Stevens J, Yang MY, Logsdon D, Graff-Cherry C, St Croix B 2007 Genes that distinguish physiological and pathological angiogenesis. Cancer Cell 11: 539–554
Jain RK, Schlenger K, Hockel M, Yuan F 1997 Quantitative angiogenesis assays: progress and problems. Nat Med 3: 1203–1208
Harris AL 2002 Hypoxia—a key regulatory factor in tumor growth. Nat Rev Cancer 2: 38–47
Munn LL 2003 Aberrant vascular architecture in tumors and its importance in drug-based therapies. Drug Discov Today 8: 396–403
Stergiopulos N, Porret CA, De Brouwer S, Meister JJ 1998 Arterial vasomotion: effect of flow and evidence of nonlinear dynamics. Am J Physiol 274: H1858–H864
Streubel B, Chott A, Huber D, Exner M, Jager U, Wagner O, Schwarzinger I 2004 Lymphoma-specific genetic aberrations in microvascular endothelial cells in B-cell lymphomas. N Engl J Med 351: 250–259
Hlatky L, Hahnfeldt P, Folkman J 2002 Clinical application of anti-angiogenic therapy: microvessel density, what it does and doesn't tell us. J Natl Cancer Inst 94: 883–893
Grotzer MA, Wiewrodt R, Janss AJ, Zhao H, Cnaan A, Sutton LN, Rorke LB, Phillips PC 2001 High microvessel density in primitive neuroectodermal brain tumors of childhood. Neuropediatrics 32: 75–79
Miralbell R, Tolnay M, Bieri S, Probst A, Sappino AP, Berchtold W, Pepper MS, Pizzolato G 1999 Pediatric medulloblastoma: prognostic value of p53, bcl-2, Mib-1, and microvessel density. J Neurooncol 45: 103–110
Ozer E, Sarialioglu F, Cetingoz R, Yuceer N, Cakmakci H, Ozkal S, Olgun N, Uysal K, Corapcioglu F, Canda S 2004 Prognostic significance of anaplasia and angiogenesis in childhood medulloblastoma: a pediatric oncology group study. Pathol Res Pract 200: 501–509
Pavlakovic H, Von Schutz V, Rossler J, Koscielniak E, Havers W, Schweigerer L 2001 Quantification of angiogenesis stimulators in children with solid malignancies. Int J Cancer 92: 756–760
Folkerth RD 2000 Descriptive analysis and quantification of angiogenesis in human brain tumors. J Neurooncol 50: 165–172
Hogan BL, Kolodziej PA 2002 Organogenesis: molecular mechanisms of tubulogenesis. Nat Rev Genet 3: 513–523
Lubarsky B, Krasnow MA 2003 Tube morphogenesis: making and shaping biological tubes. Cell 112: 19–28
Parker LH, Schmidt M, Jin SW, Gray AM, Beis D, Pham T, Frantz G, Palmieri S, Hillan K, Stainier DY, De Sauvage FJ, Ye W 2004 The endothelial-cell-derived secreted factor Egfl7 regulates vascular tube formation. Nature 428: 754–758
Bertolini F, Mancuso P, Shaked Y, Kerbel RS 2007 Molecular and cellular biomarkers for angiogenesis in clinical oncology. Drug Discov Today 12: 806–812
Aird WC 2007 Phenotypic heterogeneity of the endothelium: I. Structure, function, and mechanisms. Circ Res 100: 158–173
Yano K, Gale D, Massberg S, Cheruvu PK, Monahan-Earley R, Morgan ES, Haig D, von Andrian UH, Dvorak AM, Aird WC 2007 Phenotypic heterogeneity is an evolutionarily conserved feature of the endothelium. Blood 109: 613–615
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Grizzi, F., Weber, C. & Di Ieva, A. Antiangiogenic Strategies in Medulloblastoma: Reality or Mystery. Pediatr Res 63, 584–590 (2008). https://doi.org/10.1203/01.pdr.0000305884.29279.6b
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/01.pdr.0000305884.29279.6b