Abstract
The glucocorticoid dexamethasone (Dex) is widely used in preterm infants for the prevention of chronic lung disease. However, major concern has arisen about the long-term sequelae of this therapy. Here we report that neonatal treatment with dexamethasone significantly shortens the lifespan by 25% of male rats (28.6 ± 1.1 to 21.3 ± 0.8 mo) and by 18% of female rats (26.9 ± 1.8 to 22.0 ± 0.7 mo). Histopathological examination indicated end-stage cardiac and renal failure as the cause of premature death. Furthermore, Dex- treated rats showed symptoms of hypertension at young adult age, which worsened with increasing age. Thus, a brief period of glucocorticoid treatment during early life results in untimely death presumably due to cardiovascular and renal disease later in life. These serious, adverse long-term consequences call for prudence with glucocorticoid treatment of human preterm infants and careful follow-up of young adults with a history of neonatal glucocorticoid treatment.
Similar content being viewed by others
Main
Severe respiratory distress syndrome with concomitant chronic lung disease carries a high incidence of morbidity and mortality (1,2). Inflammation is thought to be an important factor in its pathogenesis. Therefore, treatment with glucocorticoids (GCs), particularly dexamethasone (Dex), was introduced in the eighties resulting in a reduction in chronic lung disease (3–5).
Because of these potential benefits in relation to short-term effects on lung function and mechanics (3–5), neonatal Dex became common practice in many centers around the world despite the fact that there had been previous animal studies that showed potential adverse CNS effects of this treatment (6,7). More recently, animal studies indicated that neonatal treatment with GCs affects neurodevelopment and has long lasting adverse effects on cognition and behavior (8,9). In 2000, two papers were published that cautioned the use of Dex during the neonatal period in humans (10,11). Since then, more adverse effects of neonatal GC have been shown in rodents on the immune (12) and neuroendocrine systems (13), on the NMDA receptor (14) and in human follow-up studies of prematurely born children treated with Dex during the neonatal period (15,16).
Although the available data leave no doubt that neonatal GC treatment can have long-term adverse effects on a wide variety of brain and bodily functions in animals, it remains unclear whether or not this treatment results in higher rates of mortality and cardiovascular morbidity in the long run. In rat pups we have found that neonatal Dex suppresses proliferation of cardiomyocytes leading to a lower number of cardiomyocytes (17). This reduced cardiomyocyte number was associated with a substantial cardiomyocyte hypertrophy and increased fibrosis at adult age (18). Furthermore, Le Cras et al. (19) described that GC treatment of neonatal rats causes lung hypoplasia and increased pulmonary arterial pressures. We hypothesized that the myocardial changes previously found in rats induced by neonatal Dex treatment, whether or not in combination with hemodynamic instability, may have implications for the life expectancy. To test this hypothesis, we compared the survival of rats neonatally treated with Dex with that of saline (Sal) controls. Subsequently, we investigated if the observed effects on mortality were associated with hypertension and/or histopathological alterations in organ tissues.
MATERIALS AND METHODS
Animals.
Ten days pregnant Wistar rats (250–280 g, Central Animal Laboratory, University Medical Center Utrecht, The Netherlands) were housed individually. For the experiments described in this manuscript animals from 22 litters were used. Pups were born on day 22–23 of gestation. On the day of birth (day 0) the pups were removed from their nest and 8 pups (4 females and 4 males) were randomly placed back with each dam. Pups were weaned at day 21 of age and then group-housed with same-sex littermates until experimentation. At weaning animals were randomly assigned to the various experimental conditions. Rats had ad libitum access to food and water. Light/dark cycle (dark phase 1900–0700 h), temperature (21°C) and humidity (60%) were kept constant. All experimental procedures were approved by the Committee for Animal Experimentation of the University Medical Center Utrecht.
Glucocorticoid treatment design.
Rat pups were injected intraperitoneally with dex 21-phosphate (Dex; Organon International B.V., Oss, The Netherlands) on neonatal day 1 (0.5 mg/kg body weight), day 2 (0.3 mg/kg) and day 3 (0.1 mg/kg) or with equal volumes (10 mL/kg) of sterile pyrogen free saline (Sal) for a total of 3 d. All pups in a nest received the same treatment, i.e., either Dex or Sal. The dose and duration of the treatment was based on a 21-d tapering course of Dex (starting dose, 0.5 mg/kg) to prevent or reduce chronic lung disease in preterm infants. The separate experiments were performed using different groups of male and female offspring.
Lifespan determination.
Groups of male rats (Dex n = 17; Sal n = 18) were allowed to reach senescence. The age of natural death was recorded for each individual. To reveal if long-term consequences of neonatal Dex treatment on mortality was gender-specific, the same experiment was performed with female rats (Dex n = 13; Sal n = 12).
Histopathology.
To obtain an indication of the possible cause of death, groups of Dex (n = 5) and Sal (n = 6) male rats were kept under similar conditions and treated following the same protocol as in the lifespan experiment. Rats were killed at 15 mo of age for histopathological examination using 5-μm sections of formalin perfused, formalin postfixed and paraffin embedded parts of brain, lung, liver, spleen, and adrenal routinely stained with hematoxylin and eosin for conventional histopathological analysis. Histopathological sections (5-μm) from the hearts, in a plane parallel to the equator, were routinely stained with hematoxylin and eosin for conventional histopathological analysis. Staining with a modification of the AZAN technique was used to highlight cardiomyocyte profiles including intercalated discs. The kidneys were sliced in 5-μm sections and stained with hematoxylin and eosin.
Telemetry.
Two cohorts of Dex and Sal rats were kept under similar conditions and treated following the same protocol as in the life-span experiment. Groups of male rats were equipped with implanted telemetric transmitters at 3 mo of age (Dex n = 16; Sal n = 14) or at 11 mo of age (Dex n = 4; Sal n = 5) to enable continuous recording of heart rate, blood pressure and somatomotor activity under freely moving conditions in their home cages. Surgery was performed in a sterile laminar flow cabinet to minimize the risk of infection. Telemetric transmitters were implanted in the abdominal cavity according to the procedure described previously (20). Briefly, a small longitudinal incision was made on the linea alba at the anterior of the abdomen. Two electrodes originate from the top of the transmitter, one of which was fixed to the dorsal surface of the xiphoid and the other guided under the sternohyoideus muscle and then along the trachea into the anterior mediastinum. Postoperatively, the animals received the long-acting opiate analgesic Buprenorfine hydrochloride (Temgesicâ, Reckitt and Colman, Kingston-upon-Hull, UK; 0.1 mL sc). After surgery, animals were housed individually in Plexiglas cages (25 × 25 × 35 cm) and allowed to recover for 14 d. The telemetry system consisted of small wireless transmitters model TA11CTA-F40 and receivers model RLA1020 (Data Sciences, St. Paul, MN, USA). As described previously (20) for every rat, digital data and electrocardiograms were transmitted every 10 min for 3 successive days, collected by the receiver, and led to a DataQuest 4 system (Data Sciences), after which the mean heart rate, blood pressure and somatomotor activity of those 3 d was computed.
Statistical analysis.
Data are presented as mean ± SEM. Survival data were analyzed using a Kaplan-Meier test. Telemetric data were analysed by Analysis of Variance for repeated measurements, with one between-subjects factor (treatment) and one repeated within-subjects factor (time). All other group differences were analyzed by t test. P < 0.05 considered statistically significant.
RESULTS
Neonatal dex treatment reduces lifespan.
Fig. 1 shows the survival curve of male rats neonatally treated with Dex (n = 17) or Sal (n = 18). Dex-treated rats died at considerably younger age than Sal-treated rats (p < 0.0001). While Sal-treated rats on average reached an age of 28.6 ± 1.1 mo, Dex-treated rats reached an age of 21.3 ± 0.8 mo. Thus, neonatal treatment with Dex shortened the average lifespan by approximately 25% (p < 0.0001). The last Dex-treated male rat died at 27 mo of age. At that age, 50% of the Sal (control) male rats were still alive. The last Sal-treated rat died at 36 mo.
Figure 2 shows the survival of female rats neonatally treated with Dex (n = 13) or Sal (n = 12). As was the case with Dex-treated males, female Dex-treated rats too died at considerably younger age than their Sal-treated controls (p < 0.005). Dex-treated female rats reached an average age of 22.0 ± 0.7 mo, whereas Sal-treated female rats reached an average age of 26.9 ± 1.8 mo. Thus, neonatal treatment with Dex shortened the average lifespan of female rats with approximately 18% (p < 0.005). The last Dex- and Sal-treated female rats died at 25 mo and 35 mo of age respectively.
Dex leads to hypertrophic cardiomyopathy and early severe nephropathy.
The lifespan experiment showed that the first Dex-treated male rat died at 15 mo of age. To reveal if the observed effect on mortality was associated with changes in vital organs, groups of male Dex- and Sal-treated rats were killed at 15 mo of age for histopathological examination (Dex n = 5; Sal n = 6). The heart and kidneys of Dex-treated rats showed gross abnormalities compared with those of Sal-treated controls (Figs. 3 and 4). The heart of Dex-treated rats was hypertrophic, with thickening of the left ventricular wall. Compared with Sal-treated rats (Fig. 3A, C) cardiomyocytes were elongated and increased in diameter (Fig. 3B, D) with pronounced interstitial fibrosis, comparable with histopathological hallmarks of end-stage cardiac failure. The kidneys of Dex-treated rats showed signs of chronic progressive glomerulonephritis with extensive scarring and glomerulosclerosis, and dilatation, atrophy and some regeneration of the tubular system (Fig. 4B). A high proportion of the tubuli contained large quantities of protein. Interstitial fibrosis with irregular accumulation of lymphocytes and macrophages indicated chronic inflammation. These findings are compatible with early and very severe old rat nephropathy. No histopathological abnormalities were observed in the other organs examined (lungs, liver, brain, adrenals and spleen). No data are presented here of female rats.
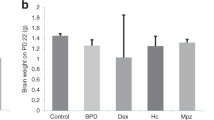
As shown in Table 1, the 15-mo-old Dex-treated male rats had a lower body weight than their Sal-treated male controls. When corrected for body weight, the weight of the heart, kidney and lungs was increased (p < 0.05) in Dex compared with Sal-treated rats, which is often observed in end-stage cardiomyopathy (21,22) and nephropathy (23,24). Together, these data point to heart and end-stage kidney failure as being the most likely cause of the premature death of Dex-treated rats.
Neonatal dex treatment leads to hypertension. Since hypertension is one of the most frequent sequelae of kidney failure and may cause hypertrophic cardiomyopathy with heart failure, blood pressure and heart rate were continuously telemetrically monitored over 3 complete diurnal cycles in freely moving, young adult male Dex- and Sal-treated rats of 3 mo of age (Dex n = 16; Sal n = 14). The systolic blood pressure of Dex-treated rats appeared to be consistently increased compared with that of Sal rats throughout the dark phase of the diurnal cycle when rats are active (Dex: 127.1 ± 2.1; Sal: 120.0 ± 2.2 mm Hg; p < 0.05), as well as during the light phase when rats are inactive (Dex: 123.9 ± 2.2; Sal: 116.5 ± 2.3 mm Hg; p < 0.05)(Fig. 5B). No significant differences in heart rate, diastolic blood pressure or mean arterial blood pressure were observed (Fig. 5A, C, D).
Effect of neonatal dexamethasone ( n = 16) or saline (• n = 14) treatment on heart rate (A), systolic blood pressure (B), diastolic blood pressure (C) and mean arterial pressure (D) assessed over the complete diurnal cycle in freely moving 3-mo-old rats (* p < 0.05). The light phase was from 700–1900 h. The horizontal axis values are the same for all four parameters.
n = 16) or saline (• n = 14) treatment on heart rate (A), systolic blood pressure (B), diastolic blood pressure (C) and mean arterial pressure (D) assessed over the complete diurnal cycle in freely moving 3-mo-old rats (* p < 0.05). The light phase was from 700–1900 h. The horizontal axis values are the same for all four parameters.
To reveal if this early symptom of hypertension in adult rats induced by neonatal Dex treatment amplifies with age, hemodynamics were determined in 11-mo-old male Dex- and Sal-treated rats (Dex n = 4; Sal n = 5) (see Fig. 6). In Dex-treated rats, systolic blood pressure (p < 0.01), diastolic blood pressure (p < 0.01) and mean arterial blood pressure (p < 0.01) appeared to be consistently increased compared with those of Sal-treated rats. The increase in heart rate was not significant, but only reached a tendency (p = 0.08).
Effect of neonatal dexamethasone ( n = 4) or saline (• n = 5) treatment on heart rate (A), systolic blood pressure (B), diastolic blood pressure (C) and mean arterial pressure (D) assessed over the complete diurnal cycle in freely moving 11-mo-old rats (* p < 0.05). The light phase was from 700–1900 h. The horizontal axis values are the same for all four parameters.
n = 4) or saline (• n = 5) treatment on heart rate (A), systolic blood pressure (B), diastolic blood pressure (C) and mean arterial pressure (D) assessed over the complete diurnal cycle in freely moving 11-mo-old rats (* p < 0.05). The light phase was from 700–1900 h. The horizontal axis values are the same for all four parameters.
Thus, the hemodynamic changes in 11-mo-old Dex-treated male rats were considerably more pronounced than those found in 3-mo-old Dex-treated rats. The systolic blood pressure during the dark phase of the diurnal cycle was 144.8 ± 1.2 mm Hg in Dex-treated rats and 130.1 ± 1.1 mm Hg in Sal-treated rats (p < 0.05). During the light phase, when rats are inactive, systolic blood pressure amounted to 141.2 ± 1.2 mm Hg in Dex-treated rats and 128.2 ± 1.0 mm Hg in Sal-treated rats (p < 0.05)(Fig. 6B).
DISCUSSION
The present study shows that neonatal treatment with clinically relevant dosages of Dex substantially reduces lifespan of rats. This appeared to be true for male as well as for female rats. The reduced lifespan likely is the functional implication of the hypertension and the histopathological findings, as reported in the present study, which showed gross abnormalities fitting with end-stage nephropathy and a progressive hypertrophic cardiomyopathy as reported earlier by our group (18).
Early, short-term effects of Dex on the neonatal cardiovascular system such as myocardial hypertrophy and hypertension have been previously reported in experimental animal and human studies. These effects were mostly considered to be transient (25–27). Although long-term effects of antenatal glucocorticoid exposure on the cardiovascular system have been observed in animals and humans (28,29), less is known about the long-term effects of neonatal Dex treatment on the heart and kidneys. Rudolph et al. reported earlier that perinatal Dex treatment inhibits or even halts physiologic myocardial hyperplasia, leaving hypertrophy as the only possibility for the still undeveloped heart to grow (30). We indeed found myocardial hypertrophy and myocardial fibrosis in the neonatally Dex-treated adult rat at 11 mo of age together with a decreased number of cardiomyocytes (18), which originated from a direct effect of neonatal Dex administration (17). In a recent study of our group we studied the hearts of rats at 4, 8 and 50 wk of age after neonatal Dex treatment. We found a significant increase in cardiomyocyte length of the Dex-treated rats compared with controls in all three age groups. This was accompanied by a significant increase in cardiomyocyte width in the 50-wk-old rats. This all resulted in significantly increased cardiomyocyte volume at 8 and 50 wk indicating cellular hypertrophy (article submitted).These above mentioned changes in neonatally Dex-treated rats may indicate early myocardial degeneration, leading to untimely ageing of the myocardium and ultimately to premature death. This process may be further complicated and deteriorated by the hypertension that started to develop already at an age of 3 mo. This corroborates observations of Le Cras et al., who found an increased risk of developing pulmonary hypertension in rats treated with Dex in neonatal life (19). To our knowledge, renal abnormalities, such as signs of chronic glomerulonephritis and atrophy of the tubular system have not been reported earlier in adult rats, neonatally treated with Dex. These abnormalities may be the result of ongoing and increasing hypertension. On the other hand, however, they may have resulted from a direct effect of Dex on the developing kidney and contributed to the hypertension. Indeed, several investigators have reported that antenatal glucocorticoid treatment causes permanent changes in the kidney morphology and renal function with hypertension in the offspring (31–33).
The present study was not designed to unravel the exact mechanism(s) underlying the premature death, but merely to test the hypothesis that neonatally Dex-induced alterations in vital organ systems such as the heart and kidneys are associated with the premature death of these treated rats. The results clearly confirm our hypothesis for the male rat. In previous studies, we found no indications for the existence of gross differences between male and female rats regarding the effects of neonatal Dex treatment, for example on the HPA-axis (13). It is therefore likely, that the cause of premature death in females is the same as in males.
Evidently, it is hazardous to directly extrapolate the present findings in the rat to the human situation. There are, however, human follow-up studies covering follow-up data up to 12 y of age, and these show some similarities with our present and previous results in the rat both with respect to short-term and long-term adverse effects due to GC treatment. In particular, these similarities concern transient effects such as myocardial hypertrophy (25,27,34) and cessation of body and skull growth during neonatal Dex treatment, and long-term adverse effects on neurologic and motor development (16,35,36), cognitive performance and social behavior (14,15,37). On the other hand, the developing myocardium in the neonatal rat differs from that of the human fetus and premature neonate. In rat neonates there is still a considerable cardiomyocyte proliferation (38) while this is less obvious in the human neonatal heart, at least in term neonates as investigated by Huttenbach et al. and by Mayhew et al. (39,40). The same investigators, however, reported still cardiomyocyte proliferative activity in myocardial tissue during the preterm period in humans. Thus, although the development of the heart of neonatal rats may not be fully comparable to that of human infants, the fact remains that cardiomyocyte proliferation may exist in the preterm infant. Therefore the present results should be taken seriously. Moreover, this study in the rat will hopefully urge researchers to investigate possible long-term adverse effects on the heart (and kidneys) of prematurely born babies treated with GCs in this vulnerable period of life.
In conclusion, the present study showed that neonatal Dex treatment in the rat leads to long-term cardiovascular and renal morbidity and to a reduced lifespan, presumably because of the longstanding cardiomyocyte hypertrophy, hypertension and end-stage nephropathy.
Abbreviations
- Dex:
-
dexamethasone
- GCs:
-
glucocorticoids
- Sal:
-
saline
References
Bancalari E, Claure N, Sosenko IR 2003 Bronchopulmonary dysplasia: changes in pathogenesis, epidemiology and definition. Semin Neonatol 8: 63–71
Kinsella JP, Greenough A, Abman SH 2006 Bronchopulmonary dysplasia. Lancet 367: 1421–1431
Mammel MC, Green TP, Johnson DE, Thompson TR 1983 Controlled trial of dexamethasone therapy in infants with bronchopulmonary dysplasia. Lancet 1: 1356–1358
Avery GB, Fletcher AB, Kaplan M, Brudno DS 1985 Controlled trial of dexamethasone in respirator-dependent infants with bronchopulmonary dysplasia. Pediatrics 75: 106–111
Cummings JJ, D'Eugenio DB, Gross SJ 1989 A controlled trial of dexamethasone in preterm infants at high risk for bronchopulmonary dysplasia. N Engl J Med 320: 1505–1510
Turner BB, Katz RJ, Carroll BJ 1979 Neonatal corticosteroid permanently alters brain activity of epinephrine-synthesizing enzyme in stressed rats. Brain Res 166: 426–430
Slotkin TA, Barnes G, Lau C, Seidler FJ, Trepanier P, Weigel SJ, Whitmore WL 1982 Development of polyamine and biogenic amine systems in brains and hearts of neonatal rats given dexamethasone: role of biochemical alterations in cellular maturation for producing deficits in ontogeny of neurotransmitter levels, uptake, storage and turnover. J Pharmacol Exp Ther 221: 686–693
de Kloet ER, Rosenfeld P, Van Eekelen JA, Sutanto W, Levine S 1988 Stress, glucocorticoids and development. Prog Brain Res 73: 101–120
Felszeghy K, Gaspar E, Nyakas C 1996 Long-term selective down-regulation of brain glucocorticoid receptors after neonatal dexamethasone treatment in rats. J Neuroendocrinol 8: 493–499
Jobe AH 2000 Glucocorticoids in perinatal medicine: misguided rockets?. J Pediatr 137: 1–3
Finer NN, Craft A, Vaucher Y, Clark R, Sola A 2000 Postnatal steroids: Short-term gain, long-term pain?. J Pediatr 137: 9–13
Bakker JM, Kavelaars A, Kamphuis PJ, Cobelens PM, van Vugt HH, van Bel Heijnen CJ 2000 Neonatal dexamethasone treatment increases susceptibility to experimental autoimmune disease in adult rats. J Immunol 165: 5932–5937
Kamphuis PJ, Bakker JM, Broekhoven MH, Kunne C, Croiset G, Lentjes EG, Tilders FJ, van Bel F, Wiegant VM 2002 Enhanced glucocorticoid feedback inhibition of hypothalamo-pituitary-adrenal responses to stress in adult rats neonatally treated with dexamethasone. Neuroendocrinology 76: 158–169
Kamphuis PJ, Gardoni F, Kamal A, Croiset G, Bakker JM, Cattabeni F, Gispen WH, van Bel F, Di Luca M, Wiegant VM 2003 Long-lasting effects of neonatal dexamethasone treatment on spatial learning and hippocampal synaptic plasticity: involvement of the NMDA receptor complex. FASEB J 17: 911–913
Barrington KJ 2001 Postnatal steroids and neurodevelopmental outcomes: a problem in the making. Pediatrics 107: 1425–1426
Yeh TF, Lin YJ, Lin HC, Huang CC, Hsieh WS, Lin CH, Tsai CH 2004 Outcomes at school age after postnatal dexamethasone therapy for lung disease of prematurity. N Engl J Med 350: 1304–1313
de Vries WB, Bal MP, Homoet-van der Kraak P, Kamphuis PJ, van der Leij FR, Baan J, Steendijk P, de Weger RA, van Bel F, van Oosterhout MF 2006 Suppression of physiological cardiomyocyte proliferation in the rat pup after neonatal glucocorticosteroid treatment. Basic Res Cardiol 101: 36–42
de Vries WB, van der Leij FR, Bakker JM, Kamphuis PJ, van Oosterhout MF, Schipper ME, Smid GB, Bartelds B, van Bel F 2002 Alterations in adult rat heart after neonatal dexamethasone ther228 y. Pediatr Res 52: 900–906
Le Cras TD, Markham NE, Morris KG, Ahrens CR, McMurtry IF, Abman SH 2000 Neonatal dexamethasone treatment increases the risk for pulmonary hypertension in adult rats. Am J Physiol Lung Cell Mol Physiol 278: L822–L829
Bruijnzeel AW, Stam R, Croiset G, Wiegant VM 2001 Long-term sensitization of cardiovascular stress responses after a single stressful experience. Physiol Behav 73: 81–86
Olivetti G, Melissari M, Capasso JM, Anversa P 1991 Cardiomyopathy of the aging human heart. Myocyte loss and reactive cellular hypertrophy. Circ Res 68: 1560–1568
Lakatta EG, Levy D 2003 Arterial and Cardiac Aging: Major Shareholders in Cardiovascular Disease Enterprises: Part II: The Aging Heart in Health: Links to Heart Disease. Circulation 107: 346–354
Baylis C, Corman B 1998 The aging kidney: insights from experimental studies. J Am Soc Nephrol 9: 699–709
Epstein M 1996 Aging and the kidney. J Am Soc Nephrol 7: 1106–1122
Werner JC, Sicard RE, Hansen TW, Solomon E, Cowett RM, Oh W 1992 Hypertrophic cardiomyopathy associated with dexamethasone therapy for bronchopulmonary dysplasia. J Pediatr 120: 286–291
Sicard RE, Werner JC 1992 Dexamethasone induces a transient relative cardiomegaly in neonatal rats. Pediatr Res 31: 359–363
La Mear NS, MacGilvray SS, Myers TF 1997 Dexamethasone-induced myocardial hypertrophy in neonatal rats. Biol Neonate 72: 175–180
Benediktsson R, Lindsay RS, Noble J, Seckl JR, Edwards CR 1993 Glucocorticoid exposure in utero: new model for adult hypertension. Lancet 341: 339–341
Dalziel SR, Walker NK, Parag V, Mantell C, Rea HH, Rodgers A, Harding JE 2005 Cardiovascular risk factors after antenatal exposure to betamethasone: 30-year follow-up of a randomised controlled trial. Lancet 365: 1856–1862
Rudolph AM 2000 Myocardial growth before and after birth: clinical implications. Acta Paediatr 89: 129–133
Celsi G, Kistner A, Aizman R, Eklof AC, Ceccatelli S, de Santiago A, Jacobson SH 1998 Prenatal dexamethasone causes oligonephronia, sodium retention, and higher blood pressure in the offspring. Pediatr Res 44: 317–322
Jahnukainen T, Chen M, Berg U, Celsi G 2001 Antenatal glucocorticoids and renal function after birth. Semin Neonatol 6: 351–355
Ortiz LA, Quan A, Weinberg A, Baum M 2001 Effect of prenatal dexamethasone on rat renal development. Kidney Int 59: 1663–1669
Bensky AS, Kothadia JM, Covitz W 1996 Cardiac effects of dexamethasone in very low birth weight infants. Pediatrics 97: 818–821
Halliday HL, Ehrenkranz RA, Doyle LW 2003 Early, moderately early and delayed postnatal corticosteroids for preventing chronic lung disease in preterm infants. Cochrane Database Syst Rev 1: CD001144–CD001146
Heide-Jalving M, Kamphuis PJ, van der Laan MJ, Bakker JM, Wiegant VM, Heijnen CJ, Veen S, van Bel F 2003 Short- and long-term effects of neonatal glucocorticoid therapy: is hydrocortisone an alternative to dexamethasone?. Acta Paediatr 92: 827–835
Kamphuis PJ, Croiset G, Bakker JM, van Bel F, Van Ree JM, Wiegant VM 2004 Neonatal dexamethasone treatment affects social behaviour of rats in later life. Neuropharmacology 47: 461–474
Li F, Wang X, Capasso JM, Gerdes AM 1996 Rapid transition of cardiac myocytes from hyperplasia to hypertrophy during postnatal development. J Mol Cell Cardiol 28: 1737–1746
Huttenbach Y, Ostrowski ML, Thaller D, Kim HS 2001 Cell proliferation in the growing human heart: MIB-1 immunostaining in preterm and term infants at autopsy. Cardiovasc Pathol 10: 119–123
Mayhew TM, Pharaoh A, Austin A, Fagan DG 1997 Stereological estimates of nuclear number in human ventricular cardiomyocytes before and after birth obtained using physical disectors. J Anat 191: 107–115
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kamphuis, P., de Vries, W., Bakker, J. et al. Reduced Life Expectancy in Rats After Neonatal Dexamethasone Treatment. Pediatr Res 61, 72–76 (2007). https://doi.org/10.1203/01.pdr.0000249980.95264.dd
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/01.pdr.0000249980.95264.dd
This article is cited by
-
Potential Adverse Effects of Dexamethasone Therapy on COVID-19 Patients: Review and Recommendations
Infectious Diseases and Therapy (2021)
-
Anticataleptic activity of nicotine in rats: involvement of the lateral entorhinal cortex
Psychopharmacology (2021)
-
Identification of functional corticosteroid response elements involved in regulation of Cacna1g expression in cardiac myocytes
Molecular and Cellular Biochemistry (2010)
-
Regulation of T-type Cav3.1 channels expression by synthetic glucocorticoid dexamethasone in neonatal cardiac myocytes
Molecular and Cellular Biochemistry (2009)