Abstract
The acquired or perinatal form of biliary atresia is a Th1 fibro-inflammatory disease affecting both the extrahepatic and intrahepatic bile ducts. Osteopontin (OPN) is a Th1 cytokine implicated in several fibro-inflammatory and autoimmune diseases. We examined the expression of OPN in acquired biliary atresia in comparison to normal liver and several pediatric cholestatic liver diseases. We also assessed OPN expression by cultured human bile duct epithelial cells. We found that liver OPN mRNA and protein expression were significantly increased in biliary atresia versus normal and other cholestatic diseases. OPN expression in biliary atresia was localized to epithelium of proliferating biliary structures (ductules and/or ducts) and bile plugs contained therein. No portal biliary OPN expression could be demonstrated in normal liver, syndromic biliary atresia, biliary obstruction not due to biliary atresia, and idiopathic neonatal hepatitis. OPN expression by human bile duct epithelial cells in culture was responsive to IL-2 and TNF-α. Our results demonstrate an up-regulation of OPN expression by interlobular biliary epithelium in biliary atresia, which correlates with biliary proliferation and portal fibrosis. These findings suggest a role for OPN in the pathogenesis of biliary atresia.
Similar content being viewed by others
Main
Biliary atresia is the most common liver disease of infancy that leads to cirrhosis, end-stage liver disease and the need for liver transplantation (1). A small proportion of cases are thought to be congenital in that they are associated with other developmental anomalies, whereas most cases are diagnosed at 4–8 wk of age and appear to represent a disease acquired in perinatal or neonatal life. The etiology and pathogenesis of biliary atresia remain unknown. A current working unifying hypothesis that can explain the clinical and pathologic features of the acquired form of biliary atresia is that some injury to the bile ducts, likely a perinatal viral infection, leads to an autonomous immune response that results in progressive bile duct injury and fibrosis (2). This progressive, inflammatory cholangiopathy results in extrahepatic bile duct obstruction (1,3). The extrahepatic bile duct is partially or entirely obliterated by fibrosis in association with inflammation within the fibrous remnant. The intrahepatic biliary system also appears to be affected by the primary disease process. Portal areas are expanded with fibrosis and exhibit marked proliferation of biliary elements (ductules and/or ducts) (4–8). These duct structures often contain bile plugs. Biliary proliferation may still be a feature of the disease even at end-stage, but in some cases all duct structures disappear.
Previous studies have shown that the mononuclear inflammatory infiltrate in the portal tracts comprises macrophages, CD4+ T-cells and NK cells (9–13). We have shown that the inflammation is typically Th1 in character, in that it consists mainly of macrophages, CD4+ T-cells and CD8+ T-cells with production of IL-2, IFN-γ, TNF-α and IL-12 (14). The inciting agent leading to this inflammation and the processes leading to bile duct destruction remain unknown.
Osteopontin (OPN) is a phosphorylated glycoprotein that is synthesized and secreted by a variety of cell types, including chondrocytes, several types of immune cells, smooth muscle cells, vascular endothelium, and some epithelia (15–17). It has many functions in both physiologic and pathologic processes (16–18). It is involved in macrophage recruitment during inflammation, acts as a survival or mitogenic factor for epithelial and vascular cells, and is associated with extracellular matrix synthesis and fibrosis (17,19–24). It is involved in the pathogenesis of a variety of inflammatory and fibrotic diseases including renal tubulointerstitial injury and atherosclerosis (23–32). Most germane to this work is its role as a Th1 cytokine (33,34). OPN stimulates T-cell proliferation and induces T-cells and macrophages to express other Th1 cytokines (33,35). Recent studies have shown an important proinflammatory role for OPN in autoimmune diseases including rheumatoid arthritis (36–38), multiple sclerosis (15,39,40) and autoimmune myocarditis (41). It is also a key cytokine in granulomatous inflammation (42,43).
Little is known about OPN in liver disease. Carbon tetrachloride intoxication in the rat has been shown to increase liver OPN expression that was localized mainly to Kupffer cells, macrophages and stellate cells (44). Human recombinant OPN had a positive effect on rat hepatic macrophage migration in vitro (44). These data suggest that OPN could play an important role in recruiting inflammation to the liver and promoting fibrosis in parenchymal liver diseases. In addition, marked expression of OPN has been observed in hepatocellular carcinoma (45–47). We recently found that increased hepatic expression of OPN is involved in the development of liver injury and fibrosis in dietary murine models of nonalcoholic steatohepatitis (NASH) (48,49). We have demonstrated that OPN is synthesized and secreted by cultured hepatocytes; synthesis is up-regulated by TNF-α, TGF-α, and leptin. In the experimental animal model, increased hepatocyte OPN expression preceded the development of hepatitis and fibrosis and was associated with increases in collagen 1 mRNA expression. OPN-null mice exposed to the same experimental conditions had marked reduction in serum ALT compared with wild-type littermates and did not develop hepatic fibrosis. We concluded from these studies that OPN is involved in the progression of hepatic fibrosis in this experimental model of NASH. There are few data regarding OPN in biliary tract diseases. Hepatic OPN expression is increased in primary biliary cirrhosis (50,51). A gene chip array analysis showed that OPN was the most highly over expressed gene in biliary atresia relative to cholestatic control livers (52). This finding suggests a potential importance for OPN in the Th1 mediated fibro-inflammatory process that characterizes biliary atresia.
In the present study, we sought to determine the expression of OPN in biliary atresia. We used quantitative methods to measure OPN mRNA and protein expression in liver samples and examined its localization by immunohistochemistry. We also determined if the pattern of OPN expression is specific to biliary atresia by examining it in other childhood cholestatic diseases. To verify our findings regarding biliary OPN expression, we examined whether cultured human bile duct epithelial cells synthesize OPN.
METHODS
We examined surgical biopsies of 13 infants with typical biliary atresia obtained at the time of diagnosis when the infants were undergoing portoenterostomy and hepatic explants of nine patients with advanced biliary atresia (Table 1). None of these patients had other developmental anomalies and were considered to have the acquired form of the disease. We also examined surgical biopsies of four infants with syndromic biliary atresia obtained when the infants were undergoing portoenterostomy. These infants had anatomic anomalies of abdominal situs typical for the condition. For comparison to biliary atresia at the time of diagnosis, we examined biopsy samples obtained during diagnostic evaluation from ten infants with idiopathic neonatal hepatitis and during surgery from six infants with bile duct obstruction not due to biliary atresia. We also examined hepatic explants from five patients with Alagille syndrome. Finally, we examined liver from two groups of “normal” children: one group comprised of nine deceased liver donors, and the other comprised of four children with extrahepatic portal vein thrombosis and completely normal hepatic histopathology undergoing mesenteric to left portal vein bypass (53). We reviewed our pathology archives of hilar remnants obtained from infants with biliary atresia undergoing portoenterostomy and identified two samples that contained biliary epithelium. We identified one example of normal infant extrahepatic bile duct (a 5-wk old deceased donor) for comparison.
Liver samples were collected from infants with biliary atresia during portoenterostomy and from children with extrahepatic portal vein thrombosis during mesenteric to left portal vein bypass surgery. Surgical biopsy samples were wrapped in tinfoil, immediately snap-frozen in liquid nitrogen and stored at -80° C until analysis. Liver samples from child-aged deceased liver donors, advanced biliary atresia and Alagille syndrome were obtained during transplantation procedures. The liver was immediately cubed, snap-frozen in liquid nitrogen and stored at -80° C until analysis. Formalin-fixed and paraffin-imbedded specimens for histology and immunostaining were obtained from our pathology archives. These studies were approved by the Institutional Review Board at Children's Memorial Hospital. Informed consent was obtained from parents to perform this study.
Histology and Immunohistochemistry.
Formalin-fixed liver tissue was processed and 5 μm thick paraffin sections were stained with hematoxylin and eosin (H & E) and Masson's trichrome stain for histologic analysis. A hepatopathologist (HMA) scored the portal findings of all sections according to the following scales. Fibrosis and inflammation were graded on 4-point scales as follows. Portal fibrosis: 1 = none, 2 = increased without bridging, 3 = bridging, 4 = cirrhosis. Inflammation: 1 = minimal or normal, 2 = mildly increased, 3 = moderately increased, 4 = severe inflammation. The number of duct or ductular contours in all portal areas contained in the section was counted and averaged. The number of portal areas sampled varied according to the source of the material examined. For percutaneous biopsy samples from neonatal hepatitis the number of portal areas ranged from 4–11 (median 7), whereas for all other samples, the number exceeded 20. Paucity/proliferation was graded as: 1 = complete absence of ducts, 2 = paucity of ducts (>0 < 0.5 ducts per portal area), 3 = normal (0.5 – 2 ducts per portal area), 4 = duct or ductular proliferation (>2 profiles per portal area).
Osteopontin immunostaining was performed using a Vectastain Elite ABC kit and 3,3′-diaminobenzidine (DAB) (Vector laboratories, Burlingame, CA). Briefly, sections were deparaffinized, washed, and preincubated in blocking solution followed by incubation with a monoclonal anti-human OPN antibody (Assay Design, Ann Arbor, MI). Sections were then incubated with biotinylated secondary antibody, washed, covered with DAB, and counterstained with hematoxylin. Sections treated with nonspecific IgG were used as negative controls. The walls of blood vessels stain positively for OPN in some samples, which provides an internal positive control. In addition, mouse kidney samples were used as a positive control for OPN in each batch of immunostains for quality control purposes.
Real-Time PCR Analysis.
The mRNA expression of OPN was assessed by real-time PCR. Total RNA was isolated from liver samples using TRIzol reagent (GIBCO-BRL, Grand Island, NY). One μg of total RNA was reverse-transcribed using 50 U of SuperScript II RNaseH- reverse transcriptase and 50 ng of random hexamers (Invitrogen, Carlsbad, CA). Real-time PCR was performed using 4 μL of the total cDNA in a 50 μL reaction volume containing QuantiTect SYBR Green PCR Master Mix (Qiagen, Valencia, CA) with the specific primers for human OPN and the housekeeping gene GAPDH (Integrated DNA Technologies, Coralville, IA). The primer sequences used are: OPN- forward 5′-GCC GAG GTG ATA GTG TGG TT- 3′; reverse 5′- ATT CAA CTC CTC GCT TTC CAT- 3′ and GAPDH-forward 5′-GTC GTG GAT CTG ACG TGC C-3′; reverse 5′-TGC CTG CTT CAC CAC CTT C-3′. Amplification was performed in duplicate for each sample in an ABI Prism 5700 Sequence Detector (PE Applied Biosystems, Foster City, CA) with denaturation for 15 min at 95°C followed by 40 PCR cycles of denaturation at 94°C for 15 s, annealing at 60°C for 30 s and extension at 72°C for 30 s. The amount of mRNA was calculated using GAPDH as the endogenous control.
Enzyme Linked Immunosorbent Assay (ELISA) and Western Blotting.
OPN protein expression was assessed in liver samples by ELISA using a kit procedure (Assay Designs, Ann Arbor, MI). Some samples were also analyzed by western blotting. Liver samples were homogenized in a lysis buffer (50 mM Tris-HCl, pH 7.4 containing 150 mM NaCl, 25 mM EDTA, 5 mM EGTA, 0.25% sodium deoxycholate, 1% Nonidet P40, and 1 mM DTT) containing protease inhibitor cocktail (Calbiochem, La Jolla, CA). Homogenates were centrifuged at 12,000 × g for 5 min at 4°C. Samples containing 300 μg – 1 mg protein were analyzed by ELISA as per kit instructions. Results are expressed as ng OPN per μg total protein.
For western blotting, liver homogenates were mixed with 5× reducing electrophoresis sample buffer (50 mM Tris-HCl, pH 6.8 containing 10% glycerol, 2% SDS, 1% β-mercaptoethanol, and 0.02% bromophenol blue) and heated for 5 min at 95°C. Samples containing 25 μg protein were resolved by 10% SDS PAGE and then transferred overnight onto nitrocellulose membranes by electrophoresis. OPN protein was detected using a monoclonal anti-OPN antibody MPIIIB10 (1:10 dilution) (Development Studies Hybridoma Bank, University of Iowa, Iowa City, Iowa) with overnight incubation at 4°C. The bound primary antibodies were detected with a horseradish peroxidase-conjugated secondary antibody (1:1000 dilution, Amersham, Arlington Heights, IL) and visualized with an enhanced chemiluminescence method. Quantitation of protein levels was performed by densitometric analysis using an Eagle Eye II video system (Strategene, La Jolla, CA).
Bile Duct Epithelial Cell Culture.
An epithelial cell line derived from a human gallbladder carcinoma was kindly provided by Greg Fitz, University of Colorado, Denver. These cells exhibit a differentiated bile duct epithelial phenotype and have been previously used in studies of bile duct injury (54). Cultures were grown in CMRL-1060 medium supplemented with 10% fetal bovine serum and 200 mM glutamine. Cultures were maintained in 75 cm3 flasks in their growth medium in 5% CO2/95% air at 37°C. To assess the effect of IL-2 and TNF-α on OPN expression, cells were subcultured in 100 mm dishes in growth medium until the cultures reached 70–80% confluence. At this time cells were made quiescent by incubation for 24 h in serum-free CMRL-1060 medium. Quiescent cultures were exposed to IL-2 (100 ng/mL) or TNF-α (100 ng/mL) for 18 h. At the end of the incubation, conditioned medium was removed and analyzed for OPN protein expression by western blotting and ELISA. Cells were harvested, RNA extracted as above and mRNA expression measured by real time PCR.
Statistical Analysis.
Comparison between groups was performed using t test for unpaired samples. A p-value of <0.05 was considered statistically significant.
RESULTS
Histology and OPN expression by immunohistochemistry: Table 1 shows the portal histopathologic findings in the liver samples examined. Both groups of “normal” children had completely normal portal histology (Table 1 and Fig. 1A). Acquired biliary atresia at the time of diagnosis was notable for extensive portal fibrosis, moderate inflammation and severe proliferation of biliary structures (Fig. 1C and Table 1). Syndromic biliary atresia at the time of diagnosis also showed extensive portal fibrosis and severe proliferation of biliary structures (Fig. 1E and Table 1). Idiopathic neonatal hepatitis demonstrated minimal or no portal fibrosis, mild to moderate inflammation, and normal numbers of interlobular bile ducts (Fig. 1G and Table 1). Samples obtained from infants with biliary obstruction not due to biliary atresia had lower scores than biliary atresia for fibrosis and inflammation and similarly high scores for proliferation of biliary structures (Fig. 1I and Table 1). Samples obtained from biliary atresia at the time of transplant all showed biliary cirrhosis with expansive portal fibrosis and minimal inflammation (Table 1). They were clearly divided into two groups with regard to biliary findings. One group comprising six samples exhibited proliferation of biliary structures (Fig. 2A), while no biliary structures could be identified in the remaining three samples (Fig. 2C). The samples from Alagille syndrome patients showed duct paucity, whereas on average, portal fibrosis was mildly increased without bridging, and portal inflammation was mild consisting almost exclusively of histiocytes (Fig. 2E and Table 1).
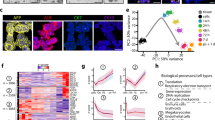
Portal histology and OPN expression in normal subjects and in patients with cholestatic disease in early infancy (<12 wk of age). (A,B) Infant deceased donor liver (age 5 wk). (A) Normal portal histology (H&E). (B) Immunostain shows no OPN expression in interlobular bile duct (arrow) and some expression in hepatocytes. (C,D) Biliary atresia at the time of diagnosis (age 6 wk). (C) Expanded portal area with fibrosis and mild inflammation containing proliferating bile duct structures (arrow) (H&E). (D) Immunostain shows marked OPN staining in biliary epithelium (arrows) and scattered mononuclear inflammatory cells. (E,F) Syndromic biliary atresia (age 4 wk). (E) Expanded portal area containing proliferating bile duct structures (arrow) (H&E). (F) Biliary epithelium shows no OPN expression by immunostain (arrows). (G,H) Idiopathic neonatal hepatitis (age 5 wk). (G) A small portal area in the center of the field contains a normal bile duct (arrow) (H&E). (H) No OPN expression is seen in bile duct epithelium (arrow) by immunostain while scattered mononuclear inflammatory cells stain positively. (I,J) Bile duct obstruction due to gallstone (age 7 wk). (I) Portal area is mildly expanded and contains mild inflammation nd increased numbers of biliary structures (arrows) (H&E). (J) Immunostain demonstrates no OPN expression in biliary epithelium (arrows) (all images at original 200× magnification; line bar length = 0.1 mm).
(A-F) Portal histology and OPN expression in pediatric cholestatic disease at time of transplantation. (G-H) Extrahepatic biliary OPN expression. (A,B) Biliary atresia and cirrhosis (age 7 mo). (A) Proliferating biliary structures containing bile plugs are seen in an expanded portal area (H&E). (B) Immunostain of same portal area shows OPN in biliary epithelium and bile plugs. The insert shows the next serial section treated with nonspecific IgG demonstrating no staining of OPN in bile or biliary epithelium. (C,D) Biliary atresia and cirrhosis (age 13 mo). (C) Bile ducts are completely absent in the sample as demonstrated by this view of an expanded fibrotic portal area that contains several arteries (H&E). (D) Immunostain of same portal area shows no OPN expression except in arteries (arrow). (E,F) Alagille syndrome (age 4 y). (E) The hepatic architecture is relatively preserved, with a mildly expanded portal area that lacks a bile duct (H&E). (F) Immunostain shows OPN expression in arteries (arrow) and hepatocytes. (G) Immunostain of normal extrahepatic bile duct obtained from a 5-wk-old deceased donor shows OPN expression in biliary epithelium (arrows), which is localized in both the apical and basal poles of epithelial cells. (H) Immunostain of extrahepatic bile duct in a hilar remnant obtained from a 7-wk-old biliary atresia subject at the time of portoenterostomy shows OPN expression in biliary epithelium (single arrow) and in the fibrous matrix surrounding the duct (double arrows). (all images at original 200× magnification; line bar length = 0.1 mm)
Table 2 shows the OPN expression on immunohistochemistry of the various samples examined. Both groups of “normal” children showed some expression of OPN in hepatocytes, but none in interlobular bile ducts (Fig. 1B). The expression of OPN and its tissue location were distinctly different in biliary atresia from other cholestatic diseases examined. Biliary atresia at the time of diagnosis showed marked OPN staining in portal areas predominantly in biliary epithelium (Fig. 1D). Some OPN expression was also observed in the inflammatory cells (Fig. 1D). In contrast, syndromic biliary atresia showed no OPN expression in biliary epithelium (Fig. 1F), whereas there was apparent increased expression in hepatocytes. Idiopathic neonatal hepatitis typically demonstrated OPN staining in portal inflammatory cells but not in interlobular bile ducts (Fig. 1H). Biopsies from infants with biliary obstruction not due to biliary atresia showed no OPN staining in epithelium of interlobular biliary structures (Figs. 1J), whereas inflammatory cells in these samples showed positive staining.
OPN staining in samples obtained from biliary atresia at the time of transplant fell into two groups, consonant with the presence of proliferation of biliary structures or their absence. In samples with biliary proliferation, marked OPN expression was seen in biliary epithelium and in bile within the duct structures (Fig. 2B), whereas samples with absent duct structures showed minimal OPN staining in portal areas, exclusively in blood vessels (Fig. 2D). Samples from Alagille syndrome showed minimal portal OPN staining (Fig. 2F). Blood vessels and hepatocytes stained, but histiocytic inflammatory infiltrates did not.
Extrahepatic bile ducts from a limited number of samples, one infant deceased donor and two infants with biliary atresia, were examined for OPN staining. Normal infant extrahepatic bile duct showed OPN staining localized to bile duct epithelium (Fig. 2G). These findings suggest a differential location of normal constitutive OPN expression to larger bile ducts (see Fig. 1B for comparison). Biliary atresia samples showed a similar degree of OPN expression in intact biliary epithelium and significant staining within the fibrous matrix surrounding the bile duct (Fig. 2H).
OPN mRNA and protein expression.
The quantitative expression of OPN mRNA and protein in liver did not differ between the two groups of “normal” children and are combined in these analyses. It should be noted that we only had formalin-fixed tissue from the 5-wk old deceased donor, which could not be included in this analysis. Figure 3A shows the expression of OPN mRNA in tissue samples from biliary atresia and Alagille syndrome relative to normal liver. OPN mRNA was increased 4 –5-fold over normal in biliary atresia at the time of diagnosis. This was further increased to 10 – 11-fold over normal in samples from biliary atresia at the time of transplantation in which biliary proliferation was evident. In contrast, samples from biliary atresia at the time of transplantation in which duct structures were absent and samples from Alagille syndrome, all of which had paucity of ducts and no ductular proliferation, showed OPN mRNA expression that was not different from normal.
(A) OPN mRNA expression in liver as assessed by real-time PCR normalized to GAPDH and expressed as fold increase vs normal. Expression was significantly increased in tissue from biliary atresia at time of diagnosis and in hepatic explants of biliary atresia that contained proliferating bile duct structures (p < 0.01). It was not significantly increased in explants of biliary atresia that showed absence of bile ducts or in Alagille syndrome. (B) Expression of OPN protein in liver as assessed by ELISA. Expression was significantly increased in tissue in hepatic explants of biliary atresia that contained proliferating bile duct structures (p < 0.01). In comparison, it was much less increased in explants of biliary atresia with absent bile ducts and in Alagille syndrome samples that had bile duct paucity (p < 0.05). Inadequate samples were available from biliary atresia at time of diagnosis to perform the analysis. n = 13 for normal subjects; 13 for BA at diagnosis; 6 for BA at Tx with bile ducts; 3 for BA at Tx without bile ducts; 5 for Alagille syndrome.
Figure 3B shows the expression of OPN protein as measured by ELISA in tissue samples from biliary atresia and Alagille syndrome relative to a normal liver. OPN protein concentration in the normal liver samples was 11 ± 3 ng/μg total protein. There was inadequate tissue in the limited samples available for biliary atresia at diagnosis to perform this analysis. Expression in samples from biliary atresia at the time of transplantation in which biliary proliferation was evident was increased to 54 ± 5 ng/μg total protein. Samples from biliary atresia with absent duct structures and samples from Alagille syndrome showed much lower OPN protein concentrations, 23 ± 2 and 20 ± 4 ng/μg total protein, respectively. Figure 4 shows a western blot of OPN protein in biliary atresia at the time of transplantation. Marked increases in 66 kD OPN and smaller isoforms (40 kD, 32 kD and 20 kD) were observed in samples in which there was biliary proliferation when compared with their expression in normal liver. In contrast, OPN expression was only slightly increased in biliary atresia samples with absent bile duct structures compared with normal liver.
Western blot for OPN of liver from normal infant deceased liver donor (lane 1) and two from biliary atresia at the time of transplantation, which were similar in the severity of cirrhosis but dissimilar with regard to the presence of biliary proliferation. The sample in lane 2 (BA 1) is representative of the six samples in which histology showed ongoing extensive biliary proliferation (histology of BA 1 shown in Fig. 2A). It shows marked increased expression of the secretory forms of OPN, from 66 kD extending down to 20 kD. This sample and the normal liver also show the 78 kD constitutive OPN. The sample in lane 3 (BA 2) is representative of the three samples in which ducts could not be identified by histology (histology of BA 2 shown in Fig. 2C). It shows markedly less expression of secretory OPN and only a faint expression of constitutive OPN.
Synthesis of OPN by human bile duct epithelial cells.
These cells, which are derived from a gallbladder carcinoma, in culture showed considerable constitutive levels of OPN mRNA (Fig. 5A) and protein expression (Fig. 5B) as assessed by real-time PCR and western blotting, respectively. Treatment of cells with TNF-α significantly reduced both the mRNA and protein expression of OPN. Incubation with IL-2 resulted in increased expression of OPN protein, whereas the OPN mRNA levels remained unchanged.
(A,B) Effect of IL-2 and TNF-α on OPN expression in cultured bile duct epithelial cells. Quiescent cells were exposed in a serum-free medium either to IL-2 or TNF-α at concentrations of 100 ng/mL for 18 h. At the end of respective incubations, mRNA expression was determined in cells (panel A), and conditioned medium was analyzed for OPN protein expression by western blotting (panel B). TNF-α inhibited both OPN mRNA and protein expression, whereas IL-2 increased OPN protein expression but had no effect on mRNA levels. Each value is mean ± SE of 5 separate determinations.
DISCUSSION
The aim of the present study was to carefully examine the expression of OPN in biliary atresia. The over-expression of OPN mRNA in biliary atresia relative to other pediatric cholestatic diseases has been reported (52). However, the cell type contributing to that over-expression has not been examined, and the specificity of OPN expression for biliary atresia has not been determined. The focus of the current study was to determine whether OPN contributes to the unique pathophysiology of biliary atresia. Our cell culture studies show that OPN is synthesized by bile duct epithelium. Synthesis and secretion can be modulated by IL-2 and TNF-α, Th1 cytokines that have also been implicated in biliary atresia (14). We demonstrated expression of OPN in biliary epithelium of normal infant extrahepatic bile duct, but not in normal interlobular bile duct epithelium. We also demonstrated that OPN is greatly over-expressed in proliferating interlobular biliary structures and bile retained within them in biliary atresia. In contrast, interlobular biliary structures in syndromic biliary atresia and biliary obstruction not due to biliary atresia showed no such OPN expression. The findings in biliary atresia suggest a change in OPN expression by interlobular bile duct structures potentially resulting from a specific biliary injury.
Biliary atresia is accompanied by aggressive and severe portal fibrosis in most cases (4), as was demonstrated in the samples we examined. Hepatic fibrosis is thought to be the product of activated stellate cells in response to injury, and portal fibrosis is thought to be the product other fibroblastic cells infiltrating the portal areas, for which cytokine signaling is necessary (55,56). OPN has been shown to be critical in the development of fibrosis in models of renal tubulo-interstitial disease (20,24,57,58). In these studies, OPN-knockout mice were shown to have marked reductions in collagen synthesis and deposition relative to wild type mice exposed to the same experimental injury. Our recent studies involving a dietary murine model of nonalcoholic steatohepatitis demonstrate an important role for hepatocyte derived OPN in the development of hepatic fibrosis (48). OPN-null mice showed much less collagen I mRNA expression and minimal hepatic fibrosis compared with wild type littermates exposed to the same experimental conditions (48). In the current study, we showed that OPN mRNA is substantially over-expressed in whole liver samples from biliary atresia obtained at the time of diagnosis, which is consistent with published findings (52). OPN protein is located mainly in the epithelium of proliferating biliary structures by immunohistochemistry suggesting that biliary epithelium is the source of much of the OPN over-expressed in whole liver at this time. It has been shown that recombinant OPN can act as a cytokine for Kupffer cell migration and macrophage activation (17,44). In turn, local accumulation of Kupffer cells and macrophages is considered to be important in the cascade of stellate cell activation and fibrosis in hepatobiliary disease (59,60). This suggests that bile duct derived OPN could play a role in the progression of biliary atresia.
Biliary atresia is also noted for extensive proliferation of interlobular biliary epithelium. OPN has been shown to exert a mitogenic effect on renal tubular epithelial cells (27) and is strongly anti-apoptotic in several tissues (61,62). In contrast, TNF-α has been shown to be pro-apoptotic to bile duct epithelial cells (63). It is possible that OPN synthesized by biliary epithelium in biliary atresia is acting in an autocrine fashion to maintain proliferation and/or reduce apoptosis in opposition to TNF-α produced by local inflammation. Consistent with this notion, OPN has been shown to mediate the proliferation of cultured mesangial and vascular smooth muscle cells (23,24,27). There is reasonable evidence to suggest that OPN and TNF-α may have somewhat oppositional effects in the Th1 inflammatory process. We demonstrated that TNF-α has an inhibitory effect on bile duct epithelial cell expression of OPN, and yet OPN induces macrophages to produce TNF-α (64). The loss of interlobular bile duct structures in some cases of biliary atresia may represent an imbalance of cytokine signals.
The stimulus for increased expression of OPN by proximal bile duct epithelium in biliary atresia could be a primary injury or the result of distal obstruction. It is of interest that proliferating interlobular bile ducts in cases of biliary obstruction not due to biliary atresia do not express OPN. Moreover, proliferating interlobular biliary epithelium in syndromic biliary atresia does not stain for OPN. This finding is consistent with a recent gene expression analysis that failed to show over-expression of OPN in syndromic biliary atresia (65). These findings suggest that the pathogenesis of interlobular biliary proliferation in distal obstruction, including that due to syndromic biliary atresia, may involve different signaling mechanisms.
Cholestasis itself might be a stimulus for increased hepatic expression of OPN. To address this question, we compared the expression of OPN in cases of idiopathic neonatal hepatitis, which were relatively age-matched for biliary atresia at diagnosis, and Alagille syndrome, which were similar in age to biliary atresia at transplantation. Immunohistochemistry demonstrated no expression of OPN in interlobular bile ducts in cases of idiopathic neonatal hepatitis. The whole liver samples from Alagille syndrome showed no increase in OPN mRNA, whereas OPN protein expression was increased above normal. This correlated with increased hepatocyte OPN staining, which is consistent with posttranscriptional regulation of hepatocyte OPN synthesis as we have previously demonstrated (48). Samples of biliary atresia obtained at transplantation that had extreme duct paucity showed similar OPN protein expression to Alagille syndrome, about 2-fold greater than normal. In contrast to Alagille syndrome, we could not demonstrate increased hepatocyte OPN immunostaining in these samples. However, they did contain increased numbers of arteries that stained for OPN (Fig. 2D) and expansive fibrosis that could diffusely contain OPN protein, which could not be demonstrated by immunostains. Focal accumulation of OPN was demonstrated in the fibrous matrix of the hilar remnant in biliary atresia (Fig. 2H), which shows that this secretory protein can be sequestered in areas of fibrosis. Taken together, these findings suggest that cholestasis itself does not lead to OPN over-expression by bile ducts in pediatric liver disease, but may lead to increased expression by other elements of the liver.
In summary, our data show that hepatic OPN expression is markedly increased in biliary atresia relative to other pediatric cholestatic diseases. OPN appears to be localized predominantly in interlobular biliary epithelium and bile within duct structures. Its increased expression in biliary atresia coincides with proliferation of biliary structures and fibrosis. Together, these findings suggest that OPN may participate in the Th1 signaling involved in the pathogenesis of biliary atresia.
Abbreviations
- IFN:
-
interferon
- IL:
-
interleukin
- OPN:
-
osteopontin
- TNF:
-
tumor necrosis factor
References
Balistreri WF, Bove KE, Ryckman FC 2001 Biliary atresia and other disorders of the extrahepatic bile ducts In: Suchy FJ, Sokol RJ, Balistreri WF (eds) Liver Disease in Children. Lippincott, Williams and Wilkins, Philadelphia, pp 253–274
Sokol RJ, Mack C 2001 Etiopathogenesis of biliary atresia. Semin Liver Dis 21: 517–524
Landing BH 1974 Considerations of the pathogenesis of neonatal hepatitis, biliary atresia and choledochal cyst the concept of infantile obstructive cholangiopathy. Prog Pediatr Surg 6: 113–139
Ishak KG, Sharp HL 2002 Developmental abnormalities and liver disease in childhood. In: MacSween RNM, Burt AD, Portmann BC, Ishak KG, Scheuer PJ, Anthony PP (eds) Pathology of the liver. Churchill-Livingstone, London, pp 107–154
Ohya T, Fujimoto T, Shimomura H, Miyano T 1995 Degeneration of intrahepatic bile duct with lymphocyte infiltration into biliary epithelial cells in biliary atresia. J Pediatr Surg 30: 515–518
Haas JE 1978 Bile duct and liver pathology in biliary atresia. World J Surg 2: 561–569
Bill AH, Haas JE, Foster GL 1977 Biliary Atresia: histopathologic observations and reflections upon its natural history. J Pediatr Surg 12: 977–982
Kinugasa Y, Nakashima Y, Matsuo S, Shono K, Suita S, Sueishi K 1999 Bile ductular proliferation as a prognostic factor in biliary atresia: an immunohistochemical assessment. J Pediatr Surg 34: 1715–1720
Kobayashi H, Puri P, O'Briain DS, Surana R, Miyano T 1997 Hepatic overexpression of MHC class II antigens and macrophage-associated antigens (CD68) in patients with biliary atresia of poor prognosis. J Pediatr Surg 32: 590–593
Urushihara N, Iwagaki H, Yagi T, Kohka H, Kobashi K, Morimoto Y, Yoshino T, Tanimoto T, Kurimoto M, Tanaka N 2000 Elevation of serum interleukin-18 levels and activation of Kupffer cells in biliary atresia. J Pediatr Surg 35: 446–449
Tracy TF Jr, Dillon P, Fox ES, Minnick K, Vogler C 1996 The inflammatory response in pediatric biliary disease: macrophage phenotype and distribution. J Pediatr Surg 31: 121–125
Broome U, Nemeth A, Hultcrantz R, Scheynius A 1997 Different expression of HLA-DR and ICAM-1 in livers from patients with biliary atresia and Byler's disease. J Hepatol 26: 857–862
Davenport M, Gonde C, Redkar R, Koukoulis G, Tredger M, Mieli-Vergani G, Portmann B, Howard ER 2001 Immunohistochemistry of the liver and biliary tree in extrahepatic biliary atresia. J Pediatr Surg 36: 1017–1025
Mack CL, Tucker RM, Sokol RJ, Kotzin BL, Whitington PF, Miller SD 2004 Biliary atresia is associated with CD4+ Th1 cell mediated inflammation within portal tracts. Pediatr Res 56: 79–87
Chabas D, Baranzini SE, Mitchell D, Bernard CC, Rittling SR, Denhardt DT, Sobel RA, Lock C, Karpuj M, Pedotti R, Heller R, Oksenberg JR, Steinman L 2001 The influence of the proinflammatory cytokine, osteopontin, on autoimmune demyelinating disease. Science 294: 1731–1735
Denhardt DT, Noda M, O'Regan AW, Pavlin D, Berman JS 2001 Osteopontin as a means to cope with environmental insults: regulation of inflammation, tissue remodeling, and cell survival. J Clin Invest 107: 1055–1061
Mazzali M, Kipari T, Ophascharoensuk V, Wesson JA, Johnson R, Hughes J 2002 Osteopontin–a molecule for all seasons. QJM 95: 3–13
Johnson GA, Burghardt RC, Bazer FW, Spencer TE 2003 Osteopontin: roles in implantation and placentation. Biol Reprod 69: 1458–1471
Philip S, Kundu GC 2003 Osteopontin induces nuclear factor kappa B-mediated promatrix metalloproteinase-2 activation through I kappa B alpha /IKK signaling pathways, and curcumin (diferulolylmethane) down-regulates these pathways. J Biol Chem 278: 14487–14497
Ophascharoensuk V, Giachelli CM, Gordon K, Hughes J, Pichler R, Brown P, Liaw L, Schmidt R, Shankland SJ, Alpers CE, Couser WG, Johnson RJ 1999 Obstructive uropathy in the mouse: role of osteopontin in interstitial fibrosis and apoptosis. Kidney Int 56: 571–580
Lin YH, Yang-Yen HF 2001 The osteopontin-CD44 survival signal involves activation of the phosphatidylinositol 3-kinase/Akt signaling pathway. J Biol Chem 276: 46024–46030
Malyankar UM, Scatena M, Suchland KL, Yun TJ, Clark EA, Giachelli CM 2000 Osteoprotegerin is an alpha vbeta 3-induced, NF-kappa B-dependent survival factor for endothelial cells. J Biol Chem 275: 20959–20962
Sodhi CP, Phadke SA, Batlle D, Sahai A 2001 Hypoxia stimulates osteopontin expression and proliferation of cultured vascular smooth muscle cells: potentiation by high glucose. Diabetes 50: 1482–1490
Sodhi CP, Phadke SA, Batlle D, Sahai A 2001 Hypoxia and high glucose cause exaggerated mesangial cell growth and collagen synthesis: role of osteopontin. Am J Physiol Renal Physiol 280: F667–674
Mazzali M, Jefferson JA, Ni Z, Vaziri ND, Johnson RJ 2003 Microvascular and tubulointerstitial injury associated with chronic hypoxia-induced hypertension. Kidney Int 63: 2088–2093
Hampel DJ, Sansome C, Romanov VI, Kowalski AJ, Denhardt DT, Goligorsky MS 2003 Osteopontin traffic in hypoxic renal epithelial cells. Nephron Exp Nephrol 94: e66–76
Sodhi CP, Batlle D, Sahai A 2000 Osteopontin mediates hypoxia-induced proliferation of cultured mesangial cells: role of PKC and p38 MAPK. Kidney Int 58: 691–700
Matsui Y, Rittling SR, Okamoto H, Inobe M, Jia N, Shimizu T, Akino M, Sugawara T, Morimoto J, Kimura C, Kon S, Denhardt D, Kitabatake A, Uede T 2003 Osteopontin deficiency attenuates atherosclerosis in female apolipoprotein e-deficient mice. Arterioscler Thromb Vasc Biol 23: 1029–1034
Bruemmer D, Collins AR, Noh G, Wang W, Territo M, Arias-Magallona S, Fishbein MC, Blaschke F, Kintscher U, Graf K, Law RE, Hsueh WA 2003 Angiotensin II-accelerated atherosclerosis and aneurysm formation is attenuated in osteopontin-deficient mice. J Clin Invest 112: 1318–1331
Isoda K, Kamezawa Y, Ayaori M, Kusuhara M, Tada N, Ohsuzu F 2003 Osteopontin transgenic mice fed a high-cholesterol diet develop early fatty-streak lesions. Circulation 107: 679–681
Isoda K, Nishikawa K, Kamezawa Y, Yoshida M, Kusuhara M, Moroi M, Tada N, Ohsuzu F 2002 Osteopontin plays an important role in the development of medial thickening and neointimal formation. Circ Res 91: 77–82
Chiba S, Okamoto H, Kon S, Kimura C, Murakami M, Inobe M, Matsui Y, Sugawara T, Shimizu T, Uede T, Kitabatake A 2002 Development of atherosclerosis in osteopontin transgenic mice. Heart Vessels 16: 111–117
Ashkar S, Weber GF, Panoutsakopoulou V, Sanchirico ME, Jansson M, Zawaideh S, Rittling SR, Denhardt DT, Glimcher MJ, Cantor H 2000 Eta-1 (osteopontin): an early component of type-1 (cell-mediated) immunity. Science 287: 860–864
Gravallese EM 2003 Osteopontin: a bridge between bone and the immune system. J Clin Invest 112: 147–149
O'Regan AW, Chupp GL, Lowry JA, Goetschkes M, Mulligan N, Berman JS 1999 Osteopontin is associated with T-cells in sarcoid granulomas and has T-cell adhesive and cytokine-like properties in vitro. J Immunol 162: 1024–1031
Yamamoto N, Sakai F, Kon S, Morimoto J, Kimura C, Yamazaki H, Okazaki I, Seki N, Fujii T, Uede T 2003 Essential role of the cryptic epitope SLAYGLR within osteopontin in a murine model of rheumatoid arthritis. J Clin Invest 112: 181–188
Ohshima S, Yamaguchi N, Nishioka K, Mima T, Ishii T, Umeshita-Sasai M, Kobayashi H, Shimizu M, Katada Y, Wakitani S, Murata N, Nomura S, Matsuno H, Katayama R, Kon S, Inobe M, Uede T, Kawase I, Saeki Y 2002 Enhanced local production of osteopontin in rheumatoid joints. J Rheumatol 29: 2061–2067
Yumoto K, Ishijima M, Rittling SR, Tsuji K, Tsuchiya Y, Kon S, Nifuji A, Uede T, Denhardt DT, Noda M 2002 Osteopontin deficiency protects joints against destruction in anti-type II collagen antibody-induced arthritis in mice. Proc Natl Acad Sci U S A 99: 4556–4561
Caillier S, Barcellos LF, Baranzini SE, Swerdlin A, Lincoln RR, Steinman L, Martin E, Haines JL, Pericak-Vance M, Hauser SL, Oksenberg JR 2003 Osteopontin polymorphisms and disease course in multiple sclerosis. Genes Immun 4: 312–315
Jansson M, Panoutsakopoulou V, Baker J, Klein L, Cantor H 2002 Cutting edge: Attenuated experimental autoimmune encephalomyelitis in eta-1/osteopontin-deficient mice. J Immunol 168: 2096–2099
Hanawa H, Abe S, Hayashi M, Yoshida T, Yoshida K, Shiono T, Fuse K, Ito M, Tachikawa H, Kashimura T, Okura Y, Kato K, Kodama M, Maruyama S, Yamamoto T, Aizawa Y 2002 Time course of gene expression in rat experimental autoimmune myocarditis. Clin Sci (Lond) 103: 623–632
O'Regan A, Berman JS 2000 Osteopontin: a key cytokine in cell-mediated and granulomatous inflammation. Int J Exp Pathol 81: 373–390
O'Regan AW, Hayden JM, Body S, Liaw L, Mulligan N, Goetschkes M, Berman JS 2001 Abnormal pulmonary granuloma formation in osteopontin-deficient mice. Am J Respir Crit Care Med 164: 2243–2247
Kawashima R, Mochida S, Matsui A, YouLuTu ZY, Ishikawa K, Toshima K, Yamanobe F, Inao M, Ikeda H, Ohno A, Nagoshi S, Uede T, Fujiwara K 1999 Expression of osteopontin in Kupffer cells and hepatic macrophages and Stellate cells in rat liver after carbon tetrachloride intoxication: a possible factor for macrophage migration into hepatic necrotic areas. Biochem Biophys Res Commun 256: 527–531
Gotoh M, Sakamoto M, Kanetaka K, Chuuma M, Hirohashi S 2002 Overexpression of osteopontin in hepatocellular carcinoma. Pathol Int 52: 19–24
Pan HW, Ou YH, Peng SY, Liu SH, Lai PL, Lee PH, Sheu JC, Chen CL, Hsu HC 2003 Overexpression of osteopontin is associated with intrahepatic metastasis, early recurrence, and poorer prognosis of surgically resected hepatocellular carcinoma. Cancer 98: 119–127
Medico E, Gentile A, Lo Celso C, Williams TA, Gambarotta G, Trusolino L, Comoglio PM 2001 Osteopontin is an autocrine mediator of hepatocyte growth factor-induced invasive growth. Cancer Res 61: 5861–5868
Sahai A, Malladi P, Melin-Aldana H, Green RM, Whitington PF 2004 Upregulation of osteopontin expression is involved in the development of nonalcoholic steatohepatitis in a murine model. Am J Physiol Gastrointest Liver Physiol 287: G264–273
Sahai A, Malladi P, Pan X, Paul R, Melin-Aldana H, Green RM, Whitington PF 2004 Obese and diabetic db/db mice develop marked liver fibrosis in a model of nonalcoholic steatohepatitis: Role of short-form leptin receptors and osteopontin. Am J Physiol Gastrointest Liver Physiol G1035–G1043
Kikuchi K, Tanaka A, Miyakawa H, Kawashima Y, Kawaguchi N, Matsushita M, Gershwin ME 2003 Eta-1/osteopontin genetic polymorphism and primary biliary cirrhosis. Hepatol Res 26: 87–90
Harada K, Ozaki S, Sudo Y, Tsuneyama K, Ohta H, Nakanuma Y 2003 Osteopontin is involved in the formation of epithelioid granuloma and bile duct injury in primary biliary cirrhosis. Pathol Int 53: 8–17
Bezerra JA, Tiao G, Ryckman FC, Alonso M, Sabla GE, Shneider B, Sokol RJ, Aronow BJ 2002 Genetic induction of proinflammatory immunity in children with biliary atresia. Lancet 360: 1653–1659
Bambini DA, Superina R, Almond PS, Whitington PF, Alonso E 2000 Experience with the Rex shunt (mesenterico-left portal bypass) in children with extrahepatic portal hypertension. J Pediatr Surg 35: 13–18
Roman RM, Wang Y, Fitz JG 1996 Regulation of cell volume in a human biliary cell line: activation of K+ and Cl- currents. Am J Physiol 271: G239–248
Friedman SL 1999 Cytokines and fibrogenesis. Semin Liver Dis 19: 129–140
Kinnman N, Francoz C, Barbu V, Wendum D, Rey C, Hultcrantz R, Poupon R, Housset C 2003 The myofibroblastic conversion of peribiliary fibrogenic cells distinct from hepatic stellate cells is stimulated by platelet-derived growth factor during liver fibrogenesis. Lab Invest 83: 163–173
Mazzali M, Hughes J, Dantas M, Liaw L, Steitz S, Alpers CE, Pichler RH, Lan HY, Giachelli CM, Shankland SJ, Couser WG, Johnson RJ 2002 Effects of cyclosporine in osteopontin null mice. Kidney Int 62: 78–85
Persy VP, Verhulst A, Ysebaert DK, De Greef KE, De Broe ME 2003 Reduced postischemic macrophage infiltration and interstitial fibrosis in osteopontin knockout mice. Kidney Int 63: 543–553
Gressner AM 1995 Cytokines and cellular crosstalk involved in the activation of fat-storing cells. J Hepatol 22: 28–36
Mathew J, Hines JE, Toole K, Johnson SJ, James OF, Burt AD 1994 Quantitative analysis of macrophages and perisinusoidal cells in primary biliary cirrhosis. Histopathology 25: 65–70
Khan SA, Lopez-Chua CA, Zhang J, Fisher LW, Sorensen ES, Denhardt DT 2002 Soluble osteopontin inhibits apoptosis of adherent endothelial cells deprived of growth factors. J Cell Biochem 85: 728–736
Scatena M, Almeida M, Chaisson ML, Fausto N, Nicosia RF, Giachelli CM 1998 NF-kappaB mediates alphavbeta3 integrin-induced endothelial cell survival. J Cell Biol 141: 1083–1093
Utaisincharoen P, Ubol S, Tangthawornchaikul N, Chaisuriya P, Sirisinha S 1999 Binding of tumour necrosis factor-alpha (TNF-alpha) to TNF-RI induces caspase(s)-dependent apoptosis in human cholangiocarcinoma cell lines. Clin Exp Immunol 116: 41–47
Leali D, Dell'Era P, Stabile H, Sennino B, Chambers AF, Naldini A, Sozzani S, Nico B, Ribatti D, Presta M 2003 Osteopontin (Eta-1) and fibroblast growth factor-2 cross-talk in angiogenesis. J Immunol 171: 1085–1093
Zhang DY, Sabla G, Shivakumar P, Tiao G, Sokol RJ, Mack C, Shneider BL, Aronow B, Bezerra JA 2004 Coordinate expression of regulatory genes differentiates embryonic and perinatal forms of biliary atresia. Hepatology 39: 954–962
Author information
Authors and Affiliations
Corresponding author
Additional information
Supported by The Children's Memorial Research Center, Chicago, IL; The Children's Liver Research Fund of Children's Memorial Hospital, Chicago, IL; The Johnny Genna Foundation, Brookfield, IL; and The Liver Foundation for Kids, Lemont, IL
Rights and permissions
About this article
Cite this article
Whitington, P., Malladi, P., Melin-Aldana, H. et al. Expression of Osteopontin Correlates with Portal Biliary Proliferation and Fibrosis in Biliary Atresia. Pediatr Res 57, 837–844 (2005). https://doi.org/10.1203/01.PDR.0000161414.99181.61
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/01.PDR.0000161414.99181.61
This article is cited by
-
Elevated Serum Osteopontin Levels in Chronic Hepatitis C Virus Infection: Association with Autoimmune Rheumatologic Manifestations
Journal of Clinical Immunology (2012)
-
Modification of osteopontin and MMP-9 levels in patients with psoriasis on anti-TNF-α therapy
Archives of Dermatological Research (2012)
-
Association of circulating osteopontin levels with clinical outcomes in postoperative biliary atresia
Pediatric Surgery International (2011)
-
The role of osteopontin and tumor necrosis factor alpha receptor-1 in xenobiotic-induced cholangitis and biliary fibrosis in mice
Laboratory Investigation (2010)
-
Primary sclerosing cholangitis – The arteriosclerosis of the bile duct?
Lipids in Health and Disease (2007)