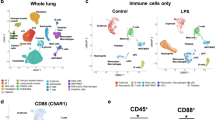
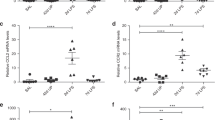
Abstract
The meconium aspiration syndrome is an important cause of respiratory distress in newborn infants. Alveolar macrophages (AMs) provide a first line of defense in the lower respiratory tract against inhaled pathogens and particles such as meconium. In this study, we examined the effect of meconium on two primary macrophage functions: phagocytosis and respiratory burst. Short-term exposure of rat NR8383 AMs to sterile meconium from human or equine neonates (1.2–24 mg/mL) produced a dose-dependent decrease in phagocytosis of fluorescent latex beads. This effect was not due to decreased cell viability or to an elevation of intracellular cAMP. The effect of short-term exposure to meconium on the respiratory burst response in AMs was quantified using flow cytometry to measure oxidation of dichlorofluorescin diacetate. A robust respiratory burst was triggered when AMs were exposed to 12 or 24 mg/mL meconium. This effect was attenuated but not eliminated by filtration of the meconium. However, subsequent to meconium exposure, AMs had a reduced respiratory burst in response to stimulation with phorbol myristate acetate. In addition, AMs that were exposed to meconium for an extended period (24 h) showed DNA fragmentation indicative of apoptosis. Meconium therefore may interfere with AM function by inducing oxidative stress and apoptosis. Tissue injury from release of reactive oxygen species by AMs may be important in the pathophysiology of the meconium aspiration syndrome.
Similar content being viewed by others
Main
Meconium aspiration syndrome (MAS) is an important cause of respiratory distress in newborn infants (1). Approximately 12–15% of human infants are born through meconium-contaminated amniotic fluid (2), and these infants are much more likely to develop respiratory distress and require respiratory support (3). When meconium is present in the amniotic fluid, ∼5% of neonates will develop MAS, and ∼5% or more of these infants will die (2).
The pathophysiology of MAS is complex and involves airway obstruction, surfactant dysfunction, and pulmonary inflammation (4). Alveolar macrophages (AMs) are important in defending the alveolar space against inhaled pathogens and particles. Because the phagocytic activity of AMs is a crucial component of host defense, it is important to know the effect of meconium on phagocytosis. Meconium has been shown to decrease phagocytosis by neutrophils in vitro (5), so it is reasonable to postulate that AM phagocytic activity may also be adversely affected.
Once phagocytosis has occurred, macrophages undergo an oxidative metabolic process called respiratory burst, generating reactive oxygen species (ROS) with activity against a wide range of invading organisms. Although production of antimicrobial molecules is essential in host defense, excessive ROS production can also cause injury to surrounding tissue (6,7). For example, ROS generated through respiratory burst activity plays a role in inducing pulmonary injury in diseases such as acute respiratory distress syndrome (8) and may also contribute to the pathophysiology of MAS. The purpose of this study was to investigate the effect of meconium on the phagocytic activity and respiratory burst response of AMs.
METHODS
Cells.
A continuous rat AM cell line, NR8383 (9), was obtained from American Type Culture Collection (Manassas, VA) and used in all experiments. Although considerable differences are seen in phagocytic and respiratory burst activity of AMs depending on the cell source and experimental conditions (10–12), the NR8383 AM line has been shown to be a good model for various AM functions and to produce levels of activity similar to that of freshly derived rat AMs (10,13). NR8383 cells were cultured in Ham's F12 nutrient mixture with glutamine, supplemented with 15% heat-inactivated FCS, 100 U/mL penicillin, and 100 μg/mL streptomycin (Sigma Chemical Co.-Aldrich, St. Louis, MO). Cultures were maintained at 37°C in a humidified, 5% CO2 atmosphere.
Meconium.
Human meconium samples were collected from soiled diapers of five healthy, full-term newborns within 8 h of delivery. Collection of these samples was approved by the Research Ethics Board (IWK Grace Health Centre, Halifax, NS, Canada), and informed consent was obtained from parents. The samples were cultured (Diagnostic Services, Atlantic Veterinary College, Charlottetown, PEI, Canada) to determine sterility, then pooled and diluted with supplemented Ham's medium to make a 20% solution. Aliquots were frozen at −70°C. After desiccation, the dry matter of the 20% meconium was determined to be 47.5 mg/mL.
Equine meconium was collected aseptically from the distal colon of a newborn foal submitted for necropsy at the Atlantic Veterinary College. A portion of equine meconium was cultured and examined microscopically to confirm absence of bacterial growth. The equine meconium was lyophilized for storage at −70°C, then solubilized in complete Ham's medium at a concentration of 50 mg/mL. For some experiments, filtered meconium was obtained by centrifuging the meconium at 360 × g for 10 min to remove large suspended particles and then by passing the supernatant through a 0.2-μm filter.
Phagocytic assay.
Phagocytic activity of AMs that were incubated with meconium was assessed and compared with control macrophages by quantifying the uptake of fluorescent latex beads using flow cytometry (14,15). For these assays, NR8383 cells were suspended in Ham's medium at a concentration of 2 × 106 cells/mL, and 500-μL aliquots were placed in 5-mL round-bottom polystyrene tubes along with the desired concentrations of meconium in a 500-μL volume. Controls consisted of macrophages plus medium. As an additional control, some cells were incubated with nonfluorescent latex particles (average diameter 1 μm; Sigma-Aldrich Chemical Co.) instead of meconium, at a ratio of 1 × 106 particles per cell, which approximated the OD of meconium at 24 mg/mL (OD600 3 ± 1). Fifteen minutes after the addition of meconium, carboxylated fluorescent latex beads (Sigma-Aldrich Chemical Co.) with an average diameter of 2 μm were added at a ratio of 50 beads/cell to half of the tubes. The beads were thoroughly vortexed before use, and flow cytometer analysis showed that <7% of beads existed as doublets or larger aggregates. An equal volume (10 μL) of sterile PBS was added to the remaining tubes. The tubes then were capped, vortexed briefly, placed in an opaque container to protect them from light, and incubated for 90 min in a shaking incubator at 37°C. After incubation, 2 mL of ice-cold PBS was added to stop phagocytosis. The cells were centrifuged at 360 × g for 5 min, washed with 1 mL of PBS, and centrifuged again. The pellet was resuspended in 400 μL of PBS, and the cells were kept on ice for a maximum of 1 h before flow cytometric analysis.
Respiratory burst assay.
Respiratory burst activity of meconium-exposed AMs was assessed and compared with control macrophages using flow cytometry as previously described (16). For these assays, NR8383 cells were suspended in Ham's complete medium at a concentration of 2 × 106 cells/mL. Aliquots of 500 μL were placed in 5-mL round-bottom polystyrene tubes. NR8383 cells were loaded with dichlorofluorescin diacetate (DCFH-DA) by incubation with 20 μM of DCFH-DA for 20 min at 37°C in the dark on a shaker platform. In the presence of ROS, DCFH-DA is oxidized to dichlorofluorescein (DCF), which can be detected by flow cytometry and provides a quantitative assessment of the respiratory burst in individual cells.
After loading with DCFH-DA, various concentrations of meconium were added to experimental samples, and the cells were incubated further for 1 h. Control samples contained macrophages plus additional medium or were stimulated with phorbol myristate acetate (PMA; 100 ng/mL) before the final incubation. As an additional control, some cells were incubated with latex particles instead of meconium, as described above. After incubation, ice-cold PBS was added to stop the reaction, and the cells were washed twice and resuspended in 400 μL of cold PBS for analysis by flow cytometry, which was performed within 30 min.
For investigating the duration of the effect of meconium on AMs, some macrophages were incubated with meconium or latex particles for 2 h, then washed and incubated in supplemented Ham's medium overnight. After 24 h, DCFH-DA was loaded as described above. In half of the samples, cells were stimulated with 100 ng/mL PMA before flow cytometric analysis.
Flow cytometry.
The fluorescent intensity of 10,000 cells from each sample was measured using a Becton Dickinson FACSCalibur flow cytometer, equipped with an argon ion laser operating at 350 mW, 488 nm. Data were acquired in list mode using CellQuest software (Becton Dickinson, San Jose, CA) and analyzed for red and green fluorescence using FCS Express software (De Novo Software). Electronic gating based on forward- and side-scatter distribution profiles was used to eliminate meconium debris and free latex beads from analysis. As an additional control, some of the meconium was passed through a 5.0-μm filter to remove any aggregates of meconium that could be confused with cells during flow cytometry. For the phagocytosis experiments, propidium iodide (PI; 3 μL; Sigma-Aldrich Chemical Co.) was added to each tube just before analysis. Electronic gating was used to eliminate from analysis the nonviable cells that had taken up PI and consequently had elevated red fluorescence. Fluorescence data were collected on log scale. Green fluorescence from the FITC-labeled beads was measured at 530 ± 30 nm, and red fluorescence from the PI was measured at 585 ± 42 nm. Electronic compensation was used to minimize spectral overlap between the two fluorochromes.
The addition of meconium to experimental solutions caused a directly proportional increase in fluorescent intensity, even when no fluorescent beads or DCFH-DA was added. This meant that the fluorescence as a result of phagocytosis or respiratory burst could not be compared directly between control and meconium-exposed cells. This problem was overcome by including, for each concentration of meconium used, a control sample of cells that were incubated with meconium but not exposed to fluorescent beads or DCFH-DA. These control samples provided a value for background fluorescence. Measurement of phagocytosis and respiratory burst included assessment of two parameters: the percentage of positive cells and the net median fluorescent intensity (MFI) of the sample population. The percentage of positive cells was determined by comparison of the fluorescent profile of cells that were exposed to either latex beads or DCFH-DA to the background fluorescence of cells not thus exposed, using Overton histogram subtraction (17). The cells with a fluorescent intensity greater than background were considered positive, meaning that they were actively phagocytic and associated with one or more fluorescent beads or, in the case of the respiratory burst assays, that respiratory burst had occurred. The net MFI was calculated by subtracting the background MFI from the MFI of the sample population after exposure to latex beads or DCFH-DA. For the phagocytosis assays, the fluorescent intensity of each cell is directly proportional to the number of internalized and bound fluorescent beads (15); therefore, the net MFI is directly related to the average number of beads associated with each cell. For the respiratory burst assays, the fluorescent intensity of each cell is directly proportional to the amount of DCFH-DA oxidized and therefore directly related to the magnitude of the respiratory burst response. For the experiments in which AMs were incubated overnight after exposure to meconium, the net MFI was calculated by subtracting the MFI of unstimulated cells from that of cells that were stimulated with PMA.
cAMP ELISA.
Intracellular cAMP levels in meconium-treated AMs were measured using an ELISA kit (Amersham Pharmacia Biotech Inc., Piscataway, NJ). NR8383 cells (1 × 106 cells/mL) were incubated for 2 h with various concentrations of equine meconium or filtered equine meconium and washed, and cell lysates were obtained for analysis by competitive binding assay performed according to the manufacturer's instructions. A standard curve was generated using serial dilutions of a known concentration of cAMP provided in the kit. The concentration of cAMP in fmol/well was determined for the experimental samples by comparison with this standard curve. The assays were performed in quadruplicate for all unknowns, and results are presented as means ± SD.
Cell membrane integrity assay.
NR8383 AMs were incubated at 2 × 106 cells/mL in Ham's medium with various concentrations of meconium at 37°C for either 6 h in total or 2 h followed by washing and 24 h of incubation without meconium. The membrane integrity of NR8383 cells after exposure to meconium was assessed by trypan blue exclusion.
JAM assay.
DNA fragmentation, which is indicative of apoptosis (18), was measured using a JAM assay as previously described (19). Briefly, NR8383 cells were incubated for 4 h with 5 μCi/mL [3H]thymidine at 37°C in a humidified atmosphere that contained 5% CO2, then washed three times. Cells were resuspended in Ham's medium, incubated for 2 h with or without various concentrations of meconium or latex particles, then washed three times and incubated for 24 h in 96-well culture plates with 50,000 cells/well in a total volume of 200 μL. For some experiments, NR8383 cells were incubated directly in the culture plates for 24 h with or without various concentrations of meconium or latex particles. Parallel cultures were incubated with 10 mM of the antioxidant N-acetyl-l-cysteine (NAC). DNA was harvested onto glass fiber filter mats, and radioactivity was measured by liquid scintillation counting. Percentage of DNA fragmentation was calculated as [(Ccpm − Ecpm)/(Ccpm)] × 100, where Ccpm and Ecpm were the retained DNA in the control and experimental conditions, respectively.
Data analysis.
Statistical analysis was performed using InStat2 software (GraphPad Software Inc., San Diego, CA). Results are reported as means ± SEM unless otherwise stated. Student's t test or one-way ANOVA followed by Dunnett's multiple comparison test were used to compare control values with various concentrations of meconium. Differences were considered significant at p < 0.05.
RESULTS
Meconium inhibited the phagocytic activity of NR8383 AMs in a dose-dependent manner. Exposure to human meconium at a concentration of 24 mg/mL caused a 41% decrease (p < 0.05) in the net MFI of AM phagocytosing latex beads (Fig. 1A), suggesting an inhibitory effect on the phagocytic ability of individual cells. There was also a dose-dependent decrease in the percentage of AMs that actively phagocytosed latex beads, which was significant at meconium concentrations of 5 mg/mL (p < 0.05) and 24 mg/mL (p < 0.01; Fig. 1B). A mean of 90% of the control cells were actively phagocytic, whereas only 44% of the cells that were exposed to the highest meconium concentration phagocytosed one or more fluorescent beads, representing a 51% reduction in phagocytic activity. Exposure to equine meconium (25 mg/mL) had a similar inhibitory effect (70% reduction) on the phagocytic activity of AMs (data not shown). In contrast, AMs that were incubated with latex particles did not show decreased phagocytosis of fluorescent latex beads. Rather, the phagocytic activity of AMs that were incubated with latex particles was increased by 14% (p < 0.05) compared with that of control cells (data not shown), suggesting that phagocytic receptors had been up-regulated.
Meconium inhibits phagocytosis by AMs. NR8383 rat AMs were incubated for 15 min with the indicated concentrations of human meconium, and the net MFI (A) and percentage of actively phagocytosing cells (B) were determined after an additional 90-min exposure to fluorescent latex beads. Results are shown as means ± SEM (n = 5; *p < 0.05; **p < 0.01).
Exposure of AMs to human meconium stimulated a dose-dependent increase in respiratory burst activity, as measured by DCFH-DA conversion to DCF. Figure 2A shows that human meconium at a concentration of 24 mg/mL produced a net MFI that was >70-fold greater than that of control cells (p < 0.01). In contrast, PMA, a commonly used stimulant of respiratory burst, produced a net MFI that was only 4-fold greater than control. The percentage of AMs that produced an oxidative response was also significantly increased by human meconium (Fig. 2B). In comparison with control cells, 62% of which produced a respiratory burst, 86% of AMs that were incubated with 24 mg/mL meconium exhibited respiratory burst (p < 0.01). In contrast, incubation of AMs with inert latex particles did not trigger a significant respiratory burst (data not shown). To confirm that these results were not unique to human meconium, we repeated the experiment with similar results using equine meconium. The net MFI for AMs that were exposed to 25 mg/mL equine meconium was 181, whereas that of control cells was 13 (p < 0.01). The percentage of responding AMs increased from 70% in controls to 86% in cultures that were stimulated with 25 mg/mL equine meconium (p < 0.01).
Meconium stimulates a respiratory burst response in AMs. NR8383 rat AMs were incubated for 1 h with the indicated concentrations of unfiltered human meconium (A and B), 0.2-μm-filtered human meconium (C and D), or 100 ng/mL PMA (A and B), and the respiratory burst response was compared with that of control macrophages. The net MFI (A and C) and the percentage of positive cells (B and D) were determined by measuring fluorescence as a result of intracellular oxidation of DCFH-DA to DCF. Results are shown as means ± SEM (n = 5 for A and B; n = 3 for C and D). Statistical comparison between meconium-treated and control macrophages was made using ANOVA. PMA-stimulated cells were compared with control macrophages using an unpaired, two-tailed t test (*p < 0.05; **p < 0.01).
To determine whether the stimulatory effect of meconium on respiratory burst was associated with phagocytosis of the particulate component of the meconium, we repeated the experiments using human meconium that had been passed through a 0.2-μm filter. Even after filtration, meconium (24 mg/mL) caused an 18-fold increase (p < 0.01) in net MFI (Fig. 2C), indicating an increase in respiratory burst. In addition, the percentage of AMs that showed a respiratory burst response was significantly increased at both the 12- and 24-mg/mL meconium concentration levels (Fig. 2D).
To investigate whether the respiratory burst response would persist after meconium stimulation, we exposed macrophages to human meconium for 2 h, then washed and incubated them overnight. The next day, AMs were loaded with DCFH-DA and stimulated with PMA. After overnight incubation, AMs that were exposed to meconium showed virtually no respiratory burst in response to PMA stimulation (Fig. 3A). The percentage of AMs that showed a respiratory burst response was also dramatically decreased (Fig. 3B), from 96% in the control cells to 35 and 24% in the cells that were exposed to 10 or 24 mg/mL meconium, respectively (p < 0.01). Although respiratory burst was also decreased 24 h after incubation with latex particles, the effect was comparatively modest (89% in the control cells versus 60% in the particle-incubated cells).
Previous exposure to meconium inhibits the PMA-induced respiratory burst response in AMs. NR8383 rat AMs were exposed to human meconium for 2 h, then washed and incubated for 24 h. Net MFI (A) and percentage of positive cells (B) were determined by measuring DCF fluorescence in unstimulated and PMA-stimulated cells. Results are shown as means ± SEM (n = 3; *p < 0.05; **p < 0.01). □ Unstimulated cells; ▪ PMA stimulated cells.
cAMP has previously been shown to down-regulate the phagocytic function of macrophages (20). However, the intracellular production of cAMP within AMs was not significantly altered by culture in the presence of equine meconium (39 ± 23 fmol/well for control AMs versus 33 ± 12 fmol/well for AMs that were incubated with 25 mg/mL meconium), suggesting that the inhibitory effect of meconium was not mediated by cAMP. Furthermore, the trypan blue dye exclusion test and the JAM assay did not show any change in cell membrane integrity or increase in DNA fragmentation when AMs were cultured for 2 h in the presence of 24 mg/mL human or equine meconium, then washed and incubated 24 h in medium (data not shown). However, AMs that were cultured for 24 h in the presence of meconium showed a dose-related increase in DNA fragmentation, suggesting induction of apoptosis (Fig. 4). The apoptotic response was unique to meconium because latex particles did not have a similar effect. The addition of the antioxidant NAC to the meconium-containing culture medium reduced the amount of DNA fragmentation in AMs, suggesting that meconium-induced apoptosis was a consequence of ROS production by AMs.
Meconium induces ROS-dependent DNA fragmentation in AMs. NR8383 rat AMs were labeled with tritiated thymidine, then incubated for 24 h with or without 10 mM NAC in the presence of the indicated concentrations of meconium or latex particles. DNA was harvested onto glass fiber filter mats, and radioactivity was determined by liquid scintillation counting. Percentage of DNA fragmentation was calculated as [(Ccpm − Ecpm)/(Ccpm)] × 100, where Ccpm and Ecpm were retained DNA in the control and experimental conditions, respectively. Data are expressed as the means of quadruplicate cultures ± SEM. □ without NAC; ▪ with NAC.
DISCUSSION
AMs play a crucial role in clearing inhaled particles and protecting the host against inhaled pathogens. Although the primary function of AMs is usually considered to be phagocytosis, AMs also play an essential role in the generation and orchestration of immune responses in the lung, through production of numerous pro- and anti-inflammatory molecules (7). The response of AMs to inhaled particles is variable and can range from simple ingestion and clearance to release of abundant inflammatory mediators (21–23). A marked inflammatory response is characteristic of MAS, and elevated levels of inflammatory mediators such as nitric oxide and thromboxane A2 have been identified in association with MAS (24,25). Oxidative injury resulting from AM stimulation is a component of the pathophysiology of several respiratory diseases (6,7) and may also be important in MAS. Exposure of AMs to various types of particulates, including bacteria such as Staphylococcus aureus (26) and Pneumocystis carinii (27), and other particles, including zymosan (28), asbestos fibers (29), and various environmental air pollution particles (30), have been shown to stimulate a respiratory burst response and production of ROS. However, the magnitude and the duration of the oxidative response after ingestion of particles is variable and may in part depend on the specific receptors that are ligated. Some particles, particularly Fc-opsonized particles, consistently trigger a strong oxidative response (21). However, particles that are phagocytosed via other receptors may not always trigger respiratory burst (31,32).
We have shown here that meconium decreased the phagocytic activity of AMs in a dose-dependent manner. This effect was not merely due to saturation, because incubation with a comparable concentration of latex particles did not decrease the phagocytic activity of AMs. Exposure of AMs to meconium also triggered a robust respiratory burst, whereas exposure to latex particles did not. Previous studies have examined the effect of meconium on phagocyte oxidative burst with contradictory results. In human neutrophils, Clark and Duff (5) reported a decrease in respiratory burst after meconium exposure, whereas Soukka et al. (33) reported that meconium stimulates oxidative burst in neutrophils. Kojima et al. (34) reported that meconium failed to stimulate a spontaneous respiratory burst in rabbit bronchoalveolar lavage macrophages, although an enhanced response to subsequent PMA stimulation was measured. In our hands, both human and equine meconium stimulated spontaneous respiratory burst in AMs. Discrepancies between our findings and those of other investigators could be due to the use of different cell types, differences in the activation state of the cells, and/or the relative sensitivity of flow cytometry versus chemiluminescence for the evaluation of respiratory burst response. In addition, the concentration of meconium used by Clark and Duff (0.5 and 1 mg/mL) was considerably less than that used in the present study, which might account for their failure to observe a stimulation of respiratory burst in response to meconium (5).
Filtration to remove particles >0.2 μm in diameter attenuated but did not eliminate the stimulatory effect of meconium on the respiratory burst response of AMs. This suggests that either soluble factors or ultrafine particles that remained in the meconium samples contributed to the inhibitory effect. Recently, there has been considerable interest in the effect of ultrafine particles (<0.1 μm) on AM function (35–38). Pulmonary injury from inhalation of ultrafine particles in polluted urban air is thought to be related to oxidative stress (36), and some studies have shown that these particles can induce inflammation and ROS production by AMs (39). However, other investigators have found no increase in respiratory burst activity in macrophages after exposure to ultrafine particles (40). Because meconium is a complex substance, it will be important in future studies to separate and analyze the various components of meconium to elucidate the factors that are responsible for stimulating respiratory burst.
After the initial oxidative response, AMs that were exposed to meconium exhibited a significantly reduced respiratory burst response to subsequent stimulation with PMA. Unlike neutrophils, monocytes produce a constitutive respiratory burst response that can be enhanced further by phagocytosis (41). The AMs used in our experiments also exhibited a robust constitutive respiratory burst that was only slightly increased upon stimulation with PMA. It is interesting that short-term treatment of AMs with meconium decreased spontaneous respiratory burst measured after 24h, and also resulted in the failure of these AMs to respond to subsequent PMA stimulation. Elevation of cellular cAMP levels and subsequent activation of protein kinase A is a known inhibitory pathway for various macrophage functions, including phagocytosis and respiratory burst (20,42). However, we did not find a significant increase in intracellular cAMP levels in AMs after incubation with meconium. An alternative explanation for the meconium-induced inhibition of AM function is that ROS that are produced in response to meconium lead to the induction of apoptosis. AM membrane integrity, as determined by trypan blue exclusion, was not adversely affected by the presence of meconium. Furthermore, no increase in DNA fragmentation was seen in AMs 24 h after a 2-h exposure to meconium, indicating that short-term exposure to meconium was not sufficient to trigger apoptosis. However, after 24 h of culture in the presence of 24 mg/mL meconium, AMs showed a 70% increase in DNA fragmentation, which is indicative of apoptosis. The apoptotic effect on AMs was specific to meconium because exposure to latex particles for the same period did not cause apoptosis. Moreover, the antioxidant NAC was able to protect AMs from meconium-induced apoptosis, particularly at lower concentrations of meconium. This finding is consistent with the observation that phagocytosis of diesel exhaust particles induces apoptosis in primary AMs and macrophage cell lines through a ROS-dependent mechanism (43). Macrophages are normally protected from the damaging effects of their own respiratory burst activity (43), but excessive production of ROS can overwhelm antioxidant defenses and also damage neighboring cells when ROS are liberated into the environment (44). Whereas exposure to high levels of ROS can induce apoptosis, exposure to lower levels of ROS may be sufficient to induce sublethal oxidative stress. For example, in T cells, a low level of oxidative stress induces a state of unresponsiveness that is not associated with apoptosis (45). It therefore is possible that short-term (2 h) exposure of AMs to meconium caused sufficient oxidative stress to inhibit the respiratory burst response, even though ROS levels did not reach the apoptosis-inducing threshold.
The findings reported in this study suggest that oxidative injury may be an important contributor to the pathophysiology of MAS, because the initial response of AMs to meconium exposure is phagocytosis of meconium particles and a robust respiratory burst response. Depending on the duration of exposure and the amount of meconium aspirated, the ROS that are generated through this respiratory burst response likely induce oxidative damage to surrounding tissue and contribute directly to the pathophysiology of MAS. Meconium-exposed AMs may also undergo oxidative stress and apoptosis, leading to an overall reduction in phagocytic activity and respiratory burst response. However, this effect is likely to be less significant than the initial oxidative response because there is a continuous turnover of AMs in the lung (46). Nevertheless, meconium-induced inhibition of phagocytic activity and respiratory burst response by AMs may render infants with MAS more susceptible to pulmonary infections and further lung damage, because AMs are crucial in defending against inhaled pathogens and particles that can damage more sensitive pulmonary cells.
Abbreviations
- AM:
-
alveolar macrophage
- DCF:
-
dichlorofluorescein
- DCFH-DA:
-
dichlorofluorescin diacetate
- MAS:
-
meconium aspiration syndrome
- MFI:
-
median fluorescent intensity
- NAC:
-
N-acetyl-l-cysteine
- PI:
-
propidium iodide
- PMA:
-
phorbol myristate acetate
- ROS:
-
reactive oxygen species
References
Srinivasan HB, Vidyasagar D 1999 Meconium aspiration syndrome: current concepts and management. Compr Ther 25: 82–89
Wiswell TE 2001 Handling the meconium-stained infant. Semin Neonatol 6: 225–231
Ziadeh SM, Sunna E 2000 Obstetric and perinatal outcome of pregnancies with term labour and meconium-stained amniotic fluid. Arch Gynecol Obstet 264: 84–87
Cleary GM, Wiswell TE 1998 Meconium-stained amniotic fluid and the meconium aspiration syndrome. An update. Pediatr Clin North Am 45: 511–529
Clark P, Duff P 1995 Inhibition of neutrophil oxidative burst and phagocytosis by meconium. Am J Obstet Gynecol 173: 1301–1305
Ricevuti G 1997 Host tissue damage by phagocytes. Ann NY Acad Sci 832: 426–448
Ward PA 1997 Phagocytes and the lung. Ann NY Acad Sci 832: 304–310
Bellingan G 1999 Inflammatory cell activation in sepsis. Br Med Bull 55: 12–29
Helmke RJ, Boyd RL, German VF, Mangos JA 1987 From growth factor dependence to growth factor responsiveness: the genesis of an alveolar macrophage cell line. In Vitro Cell Dev Biol 23: 567–574
Helmke RJ, German VF, Mangos JA 1989 A continuous alveolar macrophage cell line: comparisons with freshly derived alveolar macrophages. In Vitro Cell Dev Biol 25: 44–48
Nguyen BY, Peterson PK, Verbrugh HA, Quie PG, Hoidal JR 1982 Differences in phagocytosis and killing by alveolar macrophages from humans, rabbits, rats, and hamsters. Infect Immun 36: 504–509
Hoidal JR, Beall GD, Rasp FL Jr, Holmes B, White JG, Repine JE 1978 Comparison of the metabolism of alveolar macrophages from humans, rats, and rabbits: phorbol myristate acetate. J Lab Clin Med 92: 787–794
Jones BG, Dickinson PA, Gumbleton M, Kellaway IW 2002 The inhibition of phagocytosis of respirable microspheres by alveolar and peritoneal macrophages. Int J Pharm 236: 65–79
Dunn PA, Tyrer HW 1981 Quantitation of neutrophil phagocytosis, using fluorescent latex beads. Correlation of microscopy and flow cytometry. J Lab Clin Med 98: 374–381
Parod RJ, Brain JD 1983 Uptake of latex particles by macrophages: characterization using flow cytometry. Am J Physiol 245: C220–C226
Bass DA, Parce JW, Dechatelet LR, Szejda P, Seeds MC, Thomas M 1983 Flow cytometric studies of oxidative product formation by neutrophils: a graded response to membrane stimulation. J Immunol 130: 1910–1917
Overton WR 1988 Modified histogram subtraction technique for analysis of flow cytometry data. Cytometry 9: 619–626
Bohm I, Schild H 2003 Apoptosis: the complex scenario for a silent cell death. Mol Imaging Biol 5: 2–14
Matzinger P 1991 The JAM test. A simple assay for DNA fragmentation and cell death. J Immunol Methods 145: 185–192
Rossi AG, McCutcheon JC, Roy N, Chilvers ER, Haslett C, Dransfield I 1998 Regulation of macrophage phagocytosis of apoptotic cells by cAMP. J Immunol 160: 3562–3568
Kobzik L, Godleski JJ, Brain JD 1990 Selective down-regulation of alveolar macrophage oxidative response to opsonin-independent phagocytosis. J Immunol 144: 4312–4319
Kobzik L, Huang S, Paulauskis JD, Godleski JJ 1993 Particle opsonization and lung macrophage cytokine response. In vitro and in vivo analysis. J Immunol 151: 2753–2759
Zhang Y, Lee TC, Guillemin B, Yu MC, Rom WN 1993 Enhanced IL-1 beta and tumor necrosis factor-alpha release and messenger RNA expression in macrophages from idiopathic pulmonary fibrosis or after asbestos exposure. J Immunol 150: 4188–4196
Soukka H, Viinikka L, Kaapa P 1998 Involvement of thromboxane A2 and prostacyclin in the early pulmonary hypertension after porcine meconium aspiration. Pediatr Res 44: 838–842
Li YH, Yan ZQ, Brauner A, Tullus K 2001 Meconium induces expression of inducible NO synthase and activation of NF-κB in rat alveolar macrophages. Pediatr Res 49: 820–825
Kobzik L, Godleski JJ, Brain JD 1990 Oxidative metabolism in the alveolar macrophage: analysis by flow cytometry. J Leukoc Biol 47: 295–303
Koziel H, Li X, Armstrong MY, Richards FF, Rose RM 2000 Alveolar macrophages from human immunodeficiency virus-infected persons demonstrate impaired oxidative burst response to Pneumocystis carinii in vitro. Am J Respir Cell Mol Biol 23: 452–459
Sugar AM, Field KG 1988 Characterization of murine bronchoalveolar macrophage respiratory burst: comparison of soluble and particulate stimuli. J Leukoc Biol 44: 500–507
Lim Y, Kim SH, Kim KA, Oh MW, Lee KH 1997 Involvement of protein kinase C, phospholipase C, and protein tyrosine kinase pathways in oxygen radical generation by asbestos-stimulated alveolar macrophage. Environ Health Perspect 105( suppl 5): 1325–1327
Goldsmith CA, Frevert C, Imrich A, Sioutas C, Kobzik L 1997 Alveolar macrophage interaction with air pollution particulates. Environ Health Perspect 105( suppl 5): 1191–1195
Yamamoto K, Johnston RB Jr 1984 Dissociation of phagocytosis from stimulation of the oxidative metabolic burst in macrophages. J Exp Med 159: 405–416
Kobzik L 1995 Lung macrophage uptake of unopsonized environmental particulates. Role of scavenger-type receptors. J Immunol 155: 367–376
Soukka HR, Ahotupa M, Ruutu M, Kaapa PO 2002 Meconium stimulates neutrophil oxidative burst. Am J Perinatol 19: 279–284
Kojima T, Hattori K, Fujiwara T, Sasai-Takedatsu M, Kobayashi Y 1994 Meconium-induced lung injury mediated by activation of alveolar macrophages. Life Sci 54: 1559–1562
MacNee W, Donaldson K 2000 How can ultrafine particles be responsible for increased mortality?. Monaldi Arch Chest Dis 55: 135–139
Dick CA, Brown DM, Donaldson K, Stone V 2003 The role of free radicals in the toxic and inflammatory effects of four different ultrafine particle types. Inhal Toxicol 15: 39–52
Bunn HJ, Dinsdale D, Smith T, Grigg J 2001 Ultrafine particles in alveolar macrophages from normal children. Thorax 56: 932–934
Beck-Speier I, Dayal N, Karg E, Maier KL, Roth C, Ziesenis A, Heyder J 2001 Agglomerates of ultrafine particles of elemental carbon and TiO2 induce generation of lipid mediators in alveolar macrophages. Environ Health Perspect 109( suppl 4): 613–618
Moller W, Hofer T, Ziesenis A, Karg E, Heyder J 2002 Ultrafine particles cause cytoskeletal dysfunctions in macrophages. Toxicol Appl Pharmacol 182: 197–207
Lundborg M, Johansson A, Lastbom L, Camner P 1999 Ingested aggregates of ultrafine carbon particles and interferon-gamma impair rat alveolar macrophage function. Environ Res 81: 309–315
Bassoe CF, Smith I, Sornes S, Halstensen A, Lehmann AK 2000 Concurrent measurement of antigen- and antibody-dependent oxidative burst and phagocytosis in monocytes and neutrophils. Methods 21: 203–220
Geertsma MF, Zomerdijk TP, Nibbering PH, van Furth R 1994 Pulmonary surfactant inhibits monocyte bactericidal functions by altering activation of protein kinase A and C. Immunology 83: 133–139
Hiura TS, Kaszubowski MP, Li N, Nel AE 1999 Chemicals in diesel exhaust particles generate reactive oxygen radicals and induce apoptosis in macrophages. J Immunol 163: 5582–5591
Nel AE, Diaz-Sanchez D, Li N 2001 The role of particulate pollutants in pulmonary inflammation and asthma: evidence for the involvement of organic chemicals and oxidative stress. Curr Opin Pulm Med 7: 20–26
Malmberg KJ, Arulampalam V, Ichihara F, Petersson M, Seki K, Andersson T, Lenkei R, Masucci G, Pettersson S, Kiessling R 2001 Inhibition of activated/memory (CD45RO+) T cells by oxidative stress associated with block of NF-κB activation. J Immunol 167: 2595–2601
Holian A, Scheule RK 1990 Alveolar macrophage biology. Hosp Pract (Off Ed) 25: 53–62
Author information
Authors and Affiliations
Corresponding author
Additional information
This study was supported by the Atlantic Veterinary College Internal Research Fund.
Rights and permissions
About this article
Cite this article
Craig, S., Lopez, A., Hoskin, D. et al. Meconium Inhibits Phagocytosis and Stimulates Respiratory Burst in Alveolar Macrophages. Pediatr Res 57, 813–818 (2005). https://doi.org/10.1203/01.PDR.0000157724.02332.8B
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/01.PDR.0000157724.02332.8B
This article is cited by
-
A study of oxidative stress in neonates delivered through meconium-stained amniotic fluid
European Journal of Pediatrics (2017)
-
Role of prophylactic antibiotics in neonates born through meconium-stained amniotic fluid (MSAF)—a randomized controlled trial
European Journal of Pediatrics (2015)
-
Glucocorticoids in the treatment of neonatal meconium aspiration syndrome
European Journal of Pediatrics (2011)