Abstract
Previous studies have shown altered brain metabolism after cerebral hypoxia-ischemia, using magnetic resonance spectroscopy with echo times (TE) of 272 and 136 ms, based on peak-area or peak-height ratios. The present study examined the additional value of proton magnetic resonance spectroscopy with a short TE (31 ms) to predict a poor outcome in neonates with brain hypoxia-ischemia. Studies were performed in 21 full-term neonates with perinatal asphyxia in a 1.5 tesla magnetic field. Proton magnetic resonance spectroscopy was performed in a single volume of interest including the basal ganglia. TE of 272, 136 and 31 ms were used. After curve-fitting procedures, peak-areas as well as peak-height ratios of different brain metabolites were calculated, comparing patients with a poor versus a good outcome. Seven neonates out of 21 had a poor outcome. Neonates with a poor outcome showed a significantly lower N-acetylaspartate/choline (NAA/Cho) and a significantly raised lactate/NAA (Lac/NAA) ratio using TE of 272 and 136 ms. Using a TE of 31 ms, no differences were found in glutamate/NAA (Glx/NAA), Glx/Cho, myo-inositol/NAA (mI/NAA), and mI/Cho ratios between neonates with a good and those with a poor outcome. Highest predictive values could be achieved for NAA/Cho with a TE of 136 ms. We conclude that low NAA/Cho and high Lac/NAA ratios predict a poor outcome in neonates with cerebral hypoxia-ischemia. TE of 272 and 136 ms have a better predictive value than a TE of 31 ms.
Similar content being viewed by others
Main
Previous studies have shown changes in the cerebral metabolism of human neonates and of animals following hypoxia-ischemia (1–5). Using 1H-MRS, decreases in NAA/Cho and NAA/Cr ratios were noted to predict poor neurodevelopment (1). An increased brain Lac, which, under normal circumstances, is present in only very small amounts in the neonatal brain and is hardly detectable by 1H-MRS at term age, also predicts a poor outcome (3, 6). These studies used TE of 272 or 136 ms (1, 2, 4, 6). Using a TE of 272 ms, the peak at 1.33 ppm represents Lac. Using a TE of 136 ms, the Lac peak will be inverted, thereby distinguishing between Lac and lipids or macromolecules. Due to coupling effects, the amplitude of the Lac peak is expected to be smaller at TE 136 ms compared with TE 272 ms (7). Secondly, T2 values for NAA, Cho, and Cr differ (8, 9), and thereby differences in NAA/Cho or NAA/Cr ratios between good outcome and poor outcome groups might be more prominent at certain TE. In addition, T2 values may change following cerebral hypoxia-ischemia (10). Therefore, differences in metabolite ratios might be more prominent at longer TE. In fact, a recent study demonstrated a better predictive value for a long TE (270 ms) versus a short TE (20 ms) in occipital gray matter of young children (11).
With shorter TE, e.g. 30 ms, lipids and macromolecules can be identified. Especially in ischemic brain areas, these metabolites with resonances of 0.9–1.3 ppm will be elevated massively, thereby complicating the detection of lactate at 1.33 ppm (12). Elevated lipid signal in adults with stroke may result from myelin breakdown. Its importance in the far less myelinated brain of the neonate is uncertain.
Animal experiments have emphasized the role of the excitotoxic amino acid Glx in causing progression of neurologic damage following brain hypoxia-ischemia (13, 14). Levels of Glx were also raised in the cerebrospinal fluid of asphyxiated human neonates, and correlated with the severity of hypoxic-ischemic encephalopathy (15). At short TE, e.g. 31 ms, Glx can be detected in vivo in cerebral tissue with 1H-MRS (16, 17), but cannot be discriminated from glutamine and gamma-amino-butyric acid, which have similar resonances. A recent paper by Pu et al.(18) suggested that 1H-MRS detectable levels of Glx were elevated in neonates with severe hypoxic-ischemic encephalopathy.
mI is a very prominent compound of neonatal spectroscopy. This molecule is thought to play a role in osmoregulation, cell nutrition, detoxification, and surfactant production and as a second messenger (8). mI is thought to be a glial cell marker (19), although this has been debated in a recent abstract (20). Brain mI levels are decreased during hepatic encephalopathy and hypo-osmolarity (21). As cerebral water shifts take place in the acute phases of brain hypoxia-ischemia (22, 23), mI levels may be changed during the acute phase of brain hypoxia-ischemia. Elevated levels of mI/Cr ratios have been found in neonates with cerebral hypoxia during the first week of life (24). No changes in mI have been seen in children with chronic cerebral ischemia, suggesting relative resistance of glial cells to ischemia (25).
The present study examined the predictive value of 1H-MRS with different TE in neonates with cerebral hypoxia-ischemia. Secondly, the hypothesis was tested whether Glx and mI were increased in neonates with cerebral hypoxia-ischemia and a poor neurodevelopment.
PATIENTS AND METHODS
Patients
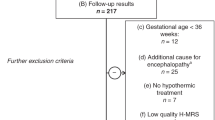
Studies were performed in 21 full-term neonates (mean gestational age 40.5 wk) with perinatal asphyxia. Patients were diagnosed as having perinatal asphyxia when at least three of the following criteria were met: abnormal fetal heart rate patterns, need for resuscitation at birth with Apgar scores <5 at 5 min, meconium stained amniotic fluid, and pH of the umbilical artery <7.10. All infants were admitted to the Neonatal Intensive Care Unit of the Wilhelmina Children's Hospital between 1995 and 1997. Cranial ultrasound was performed as soon as possible after admission and at least once a week until discharge. Patient characteristics are shown in Table 1.
MRI and 1H-MRS studies were performed at a mean age of 8 d after birth, i.e. after the hypoxic-ischemic insult. MRI examinations were performed for clinical reasons, and 1H-MRS was added to the scan protocol following informed parental consent. The study was approved by the Medical Ethical Committee of the Wilhelmina Children's Hospital/University Medical Center Utrecht.
The patients were transferred from the Neonatology Intensive Care Unit to the MR unit in a transport incubator. If considered necessary, the infants were sedated for the examination with a combination of i.m. pethidine (2 mg/kg body weight), chlorpromazine (0.5 mg/kg body weight), and promethazine (0.5 mg/kg body weight). Previously, we have demonstrated this to be safe and effective (1). During the MR studies, heart rate and transcutaneous oxygen saturation were monitored using standard equipment (Nonin, Minneapolis, MN, U.S.A.) as well as respiratory rate (Philips ACS-NT, Best, The Netherlands).
The 18 surviving infants were seen in the follow-up clinic at 3, 9, 18, and 24 mo of age. Assessment of neuromotor outcome was made using items from Amiel-Tison, and Grenier and Touwen during the first year of life, and applying the Griffiths Mental Developmental Scale during the second year of life (26–28). Cerebral palsy was classified according to the criteria of Hagberg et al.(29). A DQ below 85 on the Griffiths scale was considered abnormal.
Methods
MRI and 1H-MRS.
Studies were performed in a 1.5 tesla Philips ACS-NT system (Best, Netherlands). MRI included spin echo sagittal T1 (TR/TE: 450/30 ms), and axial T2 (TR/TE: 3000/50,150 ms) and IR weighted (TR/TI/TE: 2500/800/30 ms) scans. Thereafter, one volume of interest was selected using a PRESS sequence, including the left basal ganglia. The size of the volume was dependent on the size of the basal ganglia, but was mostly 20 × 20 × 20 mm3 (anteroposterior, left-to-right, and feet-to-head directions). Contact with the periventricular white matter and the lateral ventricle was avoided. For 1H-MRS, 64 signals were averaged, 512 data points, and a bandwidth of 1000 Hz were used. TR/TE were 2000/31,136,272 ms. The data were processed by applying Lorenz-Gaussian windowing in the time domain (Gaussian broadening 6 Hz, exponential narrowing 4 Hz) for noise reduction and spectral resolution enhancement, followed by zero-filling to 4096 data points.
Curve fitting was performed using MRUI software, including VARPRO/AMARES (EC Human Capital & Mobility/Networks program, Universitat Autonoma, Barcelona, Spain). Peaks were identified by the operator. Time-domain-algorithm ratios of peak areas were calculated and included NAA/Cho, NAA/Cr, and Cho/Cr, Lac/NAA (TE 272,136 ms) and Glx/NAA, Glx/Cho, Glx/Cr, mI/NAA, mI/Cho, and mI/Cr (TE 31 ms). In case of coupled resonances (Lac) the combined area under both peaks was used for calculations. (See Figure 1).
Statistical analysis.
A Mann-Whitney U test was used to compare metabolite ratios of patients with a normal versus an abnormal outcome. The correlation between peak height versus time-domain-algorithm peak area ratios was analyzed. Analysis was done using SPSS version 8.0 for Windows software. A p value of <0.05 was considered statistically significant.
Receiver operator characteristics (ROC) curves were calculated using MedCalc software (MedCalc Software, v4.16A, Mariakerke, Belgium) and the areas under the ROC curve were used to determine the optimum test parameters. This optimum test parameter was used as a cutoff level. PPV and NPV were calculated, based on the NAA/Cho and Lac/NAA ratio with optimum sensitivity and positivity.
RESULTS
MRI
Results of MRI and follow-up are listed in Table 2. Twelve infants showed normal development (DQ >85). Two of these infants however had an Erb's paresis. Seven newborns had a poor outcome, three of whom died. Six of these seven infants showed severe lesions of the basal ganglia. One infant with a normal MRI had a DQ <85, but no motor impairment. This child had also dysmorphic features, but no syndrome has been found so far.
In the 12 neonates with a normal development, MRI showed minor lesions in six infants. Both children with the Erb's paresis had normal MRI and a normal developmental quotient.
1H-MRS
Figures 1A and B are an example of 1H-MRS of an individual patient. Table 3 shows NAA/Cho, NAA/Cr, Cho/Cr, and Lac/NAA ratios using a TE of 272 ms. In Table 4, the same ratios are listed as in Table 3, but here a TE of 136 ms was used. In Figures 2 and 3, individual data of NAA/Cho and Lac/NAA ratios with TE 136 ms are presented versus postnatal age. NAA/Cho was significantly lower in neonates with a poor outcome compared with the patients with a good outcome. NAA/Cr was also decreased, but not significantly. Lac/NAA ratios were significantly higher in children with a poor outcome. Using a TE of 31 ms, NAA/Cho and Lac/NAA ratios did not differ significantly between the groups with a good or a poor outcome.
(A) Proton MR spectra from the brain of a neonate following severe asphyxia (case 18). Using TE of 136 and 272 ms, a prominent Lac doublet is demonstrated at 1.33 ppm. Using a TE of 31 ms, Glx is shown at 2.0–2.3 ppm and mI at 3.5–3.6 ppm. (B) Proton MR spectra from case 13, using a TE of 31 ms (top). Using curve fitting, five peaks were identified for further calculations (bottom). 1 : mI;2 : Cho;3 : Cr;4 : Glx;5 : NAA. Resonances at 0.8–1.3 ppm were not fitted deliberately, as they contained a major contribution from mobile lipids and macromolecules.
Glx and mI ratios are listed in Table 5, using a TE of 31 ms. Individual data versus postnatal age are presented in Figures 4 and 5. Glx ratios of 11 infants with normal follow-up were compared with 6 newborns with abnormal follow-up. Glx ratios appeared to be higher in children who died or had a poor neurodevelopment, but none of these ratios were significantly higher in these patients. Increased ratios of mI/NAA and mI/Cho were found, but none of these differed significantly.
Table 6 shows the areas under the ROC curves and predictive values for TE 272 and 136 ms. The areas under the ROC curves of both TE did not differ significantly. Using a TE of 272 ms, the PPV of NAA/Cho was higher than using a TE of 136 ms, using a cutoff value of 0.79 for a TE of 272 ms and 0.62 for a TE of 136 ms. The PPV for Lac/NAA was equal for both TE, using cutoff values of 0.44 for a TE of 272 ms and 0.09 for a TE of 136 ms. The NPV of NAA/Cho was higher using a TE of 136 ms, and almost equal for Lac/NAA.
PPV and NPV of Glx and mI ratios were not calculated because no significant differences were found between patients with a poor versus a good outcome.
DISCUSSION
The aim of our study was to examine the prognostic value of an adverse outcome of different TE in neonates with cerebral hypoxia-ischemia. In children with a good versus a poor outcome, the NAA/Cho, NAA/Cr, Lac/NAA, Glx/NAA, and mI/NAA ratios were compared using TE of 272, 136, and 31 ms. Our results showed that for TE of 272 and 136, NAA/Cho was significantly decreased in children with a poor outcome compared with patients with a normal neurodevelopment. NAA/Cho and NAA/Cr ratios obtained at a TE of 31 ms showed too wide a range to be used for prediction. Recently, this has also been observed by others (11). Lac/NAA was raised in children with a poor outcome at TE of 272 ms and 136 ms. Glx and mI ratios were not altered. The predictive value of TE 136 ms was slightly better than using a TE of 272 ms. Differences in T2 values of metabolites and the effects of brain hypoxia-ischemia on these T2 values might change metabolite ratios (9, 10). Therefore, differences in ratios between neonates with a good or a poor outcome may be more prominent at certain TE.
Although NAA appears to be present in precursors of oligodendrocytes (30, 31), NAA is still considered a neuronal marker, whereas Cho and Cr are present in all types of cells (30). In accordance with previous studies (1, 4, 32–34), we found decreased NAA/Cho ratios for TE of 272 and 136 ms, indicating a more severe neuronal loss in the children with an abnormal follow-up. In newborns with a poor outcome, the NAA/Cr tended to be decreased, but differences were not significant. Although others have described a decrease in Cr simultaneous with the decrease in NAA (35), this is unlikely in our study, as Cho/Cr ranges did not change at all. Others have described persisting decreases of NAA/Cr in neonates following perinatal brain hypoxia-ischemia (36). Lac is produced in the acute stage as an end product of the anaerobic glycolysis. Following resuscitation, it decreases, but due to the secondary energy failure it increases again after 24 h (5, 37). Elevated Lac levels have been shown until months after the hypoxia-ischemia, probably due to an influx of Lac-producing macrophages in the damaged tissue or an altered redox state (36, 38, 39). Lac/NAA was significantly elevated in the group with abnormal outcome, as in previous reports (1, 6, 32, 40, 41). Only three neonates were examined during the first day of life, so most of the Lac found is probably due to secondary energy failure and influx of macrophages (42).
Amplitude of the area under the Lac peak was higher at TE 272 ms compared with TE 136 ms. This may be caused by coupling effects at TE 136 ms (7), causing signal loss at TE 136 ms. Introduction of a correction factor would be justified on a theoretical basis. However, we did not do so because it would affect Lac/NAA ratios similarly in both good and poor outcome groups, and therefore would not influence further statistical analysis. Although the ROC curve for Lac/NAA had a larger area under the curve at TE 272 ms than at TE 136 ms, the PPV and NPV were not affected by this loss of signal.
Glx is an important neurotransmitter in the cascade leading to neuronal cell damage following hypoxia-ischemia (43). It activates postsynaptic receptors resulting in opening of the Ca2+ channels (44, 45). Calcium plays a crucial role in the formation of oxygen free radicals and neuronal damage (46, 47). Ischemia decreases the availability of glucose. During ischemia, glutamine is also used as an alternative substrate to glucose for neuronal cells, and Glx and GABA for the glial compartment (48). In our study, Glx ratios tended to be elevated in patients with a poor neurodevelopment, but were not significantly higher when compared with patients with a normal follow-up. Also, in cerebral fluid of newborn infants with hypoxic-ischemic encephalopathy, Glx levels were only elevated during the first two days of life (15). This is also the period when patients with hypoxic-ischemic encephalopathy may show severe seizures. Our patients were examined at a mean postnatal age of 8 d (range 1–30 d), which may be too late to detect a significantly raised amount of Glx. It is possible that Glx levels had decreased due to normalization of Glx uptake and synthesis after a period of hypoxia. Another explanation may be that it is used as alternative fuel for neuronal and glial cells during the ischemia. Thirdly, Glx is excreted outside the cell so Glx levels are raised in the extracellular space (49), whereas MRS detects mainly intracellular metabolites. Pu et al.(18) reported raised peaks of α-glutamate at 3.75 ppm, using a TE of 135 ms. However, these α-Glx resonances in their publication are very small. In our experience, the α-Glx peak at a TE of 136 ms was too small for reliable curve fitting.
mI levels are high after birth, followed by a rapid fall during the first year of life (8). It is a precursor of the inositol phosphates, which are active in releasing Ca2+(50). They also act as osmoregulators in astrocytes (19, 51), and in addition, they may act as a storage pool for glucose (50). During recovery of hypoxia-ischemia it is raised (52).
Levels of mI/NAA, mI/Cho, and mI/Cr were not significantly different between the good and poor outcome groups. This may be due to the fact that most of our patients were examined a few days after the acute period of hypoxia-ischemia. At that time, initial changes in brain osmolarity and thereby changes in levels of mI may have subsided at the time of MRS.
It would be preferable for all metabolites to use absolute concentrations instead of metabolite ratios. However, this would include T1 and T2 measurements in all individual patients. As measuring time is limited in these neonates to approximately 1 h, absolute concentrations could not be measured.
Predictive values of 1H-MRS using a TE of 136 ms are good and comparable with those of cerebral function monitor (CFM) (PPV 86%, NPV 91%) (53) and somatosensory evoked potentials (PPV 82%, NPV 92%) at an age of 6 h (54). At the end of the first week, CFM and evoked potentials normalize in most asphyxiated patients, even if they will develop a neurodevelopmental delay. This is in contrast with 1H-MRS, which is predictive at an early time point after perinatal asphyxia (55), and retains its prognostic value throughout the first month after hypoxia-ischemia.
Peak-height ratios and time-domain algorithms producing peak-area ratios correlated well (Pearson correlation 0.915, p < 0.001, data not shown). Both peak-height as well as time- domain algorithms can therefore be used for prognostic ends (1). As reference values are dependent on the hardware and software used, local reference values need to be acquired for prognostic purposes.
We conclude that low NAA/Cho and elevated Lac/NAA ratios during the first month of life predict a poor outcome after perinatal hypoxia-ischemia. Predictive values of 1H-MRS are comparable with neurophysiological examinations, but 1H-MRS can be performed at a later time point after the hypoxic-ischemic moment without a decrease of its predictive values. Glx/NAA and mI/NAA ratios do not significantly differ between children with a good or poor outcome and therefore a TE of 31 ms has no additional predictive value in neonates tested at a mean posthypoxia age of 8 d. For prognostic purposes, 1H-MRS with a TE of 136 ms has slight advantages over a TE of 272 ms.
Abbreviations
- Cho:
-
total choline
- Cr:
-
phosphocreatine and creatine
- DQ:
-
developmental quotient
- Glx:
-
glutamate, glutamine and GABA
- 1H-MRS:
-
proton magnetic resonance spectroscopy
- IR:
-
inversion recovery
- Lac:
-
lactate
- mI:
-
myo-inositol
- MRI:
-
magnetic resonance imaging
- NAA:
-
N-acetylaspartate
- NPV:
-
negative predictive value
- PPV:
-
positive predictive value
- PRESS:
-
point-resolved spectroscopy
- TE:
-
echo time
- TI:
-
time to inversion
- TR:
-
repetition time
References
Groenendaal F, Veenhoven RH, Van der Grond J, Jansen GH, Witkamp TD, De Vries LS 1994 Cerebral lactate and N-acetyl-aspartate/choline ratios in asphyxiated full-term neonates demonstrated in vivo using proton magnetic resonance spectroscopy. Pediatr Res 35: 148–151
Hanrahan JD, Cox IJ, Edwards AD, Cowan FM, Sargentoni J, Bell JD, Bryant DJ, Rutherford MA, Azzopardi D 1998 Persistent increases in cerebral lactate concentration after birth asphyxia. Pediatr Res 44: 304–311
Hope PL, Cady EB, Chu A, Delpy DT, Gardiner RM, Reynolds EOR 1987 Brain metabolism and intracellular pH during ischaemia and hypoxia: an in vivo 31P and 1H nuclear magnetic resonance study in the lamb. J Neurochem 49: 75–82
Peden CJ, Cowan FM, Bryant DJ, Sargentoni J, Cox J, Menon DK, Gadian DG, Bell JD, Dubowitz LM 1990 Proton MR spectroscopy of the brain in infants. J Comput Assist Tomogr 14: 886–894
Penrice J, Lorek A, Cady EB, Amess PN, Wylezinska M, Cooper CE, D'Souza P, Brown GC, Kirkbride V, Edwards AD, Wyatt JS, Reynolds EOR 1997 Proton magnetic resonance spectroscopy of the brain during acute hypoxia-ischemia and delayed cerebral energy failure in the newborn piglet. Pediatr Res 41: 795–802
Leth H, Toft PB, Peitersen B, Lou HC, Henriksen O 1996 Use of brain lactate levels to predict outcome after perinatal asphyxia. Acta Paediatr 85: 859–864
Ernst T, Hennig J 1991 Coupling effects in volume selective 1H spectroscopy of major brain metabolites. Magn Reson Med 21: 82–96
Kreis R, Ernst T, Ross BD 1993 Development of the human brain: in vivo quantification of metabolite and water content with proton magnetic resonance spectroscopy. Magn Reson Med 30: 424–437
Toft PB, Christiansen P, Pryds O, Lou HC, Henriksen O 1994 T1, T2, and concentrations of brain metabolites in neonates and adolescents estimated with H-1 MR spectroscopy. J Magn Reson Imaging 4: 1–5
Cady EB, Lorek A, Penrice J, Wylezinska M, Cooper CE, Brown GC, Owen-Reece H, Kirkbride V, Wyatt JS, Osmund E 1994 Brain-metabolite transverse relaxation times in magnetic resonance spectroscopy increase as adenosine triphosphate depletes during secondary energy failure following acute hypoxia-ischaemia in the newborn piglet. Neurosci Lett 182: 201–204
Holshouser BA, Ashwal S, Shu S, Hinshaw DB 2000 Proton MR spectroscopy in children with acute brain injury: comparison of short and long echo time acquisitions. J Magn Reson Imaging 11: 9–19
Saunders DE, Howe FA, van den Boogaart A, Griffiths JR, Brown MM 1997 Discrimination of metabolite from lipid and macromolecule resonances in cerebral infarction in humans using short echo proton spectroscopy. J Magn Reson Imaging 7: 1116–1121
Ueda Y, Obrenovitch TP, Lok SY, Sarna GS, Symon L 1992 Efflux of glutamate produced by short ischemia of varied severity in rat striatum. Stroke 23: 253–259
Velasco I, Tapia R, Massieu L 1996 Inhibition of glutamate uptake induces progressive accumulation of extracellular glutamate and neuronal damage in rat cortical cultures. J Neurosci Res 44: 551–561
Hagberg H, Thornberg E, Blennow M, Kjellmer I, Lagercrantz H, Thiringer K, Hamberger A, Sandberg M 1993 Excitatory amino acids in the cerebrospinal fluid of asphyxiated infants: relationship to hypoxic-ischemic encephalopathy. Acta Pediatr 82: 925–929
Mason GF, Pan JW, Ponder SL, Twieg DB, Pohost GM, Hetherington HP 1994 Detection of brain glutamate and glutamine in spectroscopic images at 4.1 T. Magn Reson Med 32: 142–145
Prost RW, Mark L, Mewissen M, Li SJ 1997 Detection of glutamate/glutamine resonances by 1H-magnetic resonance spectroscopy at 0.5 tesla. Magn Reson Med 37: 615–618
Pu Y, Li QF, Zeng CM, Gao J, Qi J, Luo DX, Mahankali S, Fox PT, Gao JH 2000 Increased detectability of alpha brain glutamate/glutamine in neonatal hypoxic-ischemic encephalopathy. AJNR Am J Neuroradiol 21: 203–212
Brand A, Richter-Landsberg C, Leibfritz D 1993 Multinuclear NMR studies on the energy metabolism of glial and neuronal cells. Dev Neurosci 15: 289–298
Moore GJ, Koch S, Chen G, Santalucia J Jr, Manji HK 1999 Myo-inositol is not exclusively glial in the human CNS. Proceedings of the 7th scientific meeting and exhibition of the International Society for Magnetic Resonance in Medicine, Philadelphia, PA, page 6, abstract 33
Haussinger D, Laubenberger J, vom Dahl S, Ernst T, Bayer S, Langer M, Gerok W, Hennig J 1994 Proton magnetic resonance spectroscopy studies on human brain myo-inositol in hypo-osmolarity and hepatic encephalopathy. Gastroenterology 107: 1475–1480
Van der Toorn A, Verheul HB, van der Sprenkel JW, Tulleken CA, Nicolay K 1994 Changes in metabolites and tissue water status after focal ischemia in cat brain assessed with localized proton MR spectroscopy. Magn Reson Med 32: 685–691
Cowan FM, Pennock JM, Hanrahan JD, Manji KP, Edwards AD 1994 Early detection of cerebral infarction and hypoxic ischemic encephalopathy in neonates using diffusion-weighted magnetic resonance imaging. Neuropediatrics 25: 172–175
Lewis RH, Kuint J, Rutherford MA, Coutts GA, Allsop J, Cox IJ, Edwards AD, Robertson NJ 1999 Cerebral myo-inositol in infants following perinatal hypoxia-ischaemia. Early Hum Dev 56: 241–242( abstr)
Wilichowski E, Pouwels PJ, Frahm J, Hanefeld F 1999 Quantitative proton magnetic resonance spectroscopy of cerebral metabolic disturbances in patients with MELAS. Neuropediatrics 30: 256–263
Sarnat HB, Sarnat MS 1976 Neonatal encephalopathy following fetal distress. A clinical and electroencephalographic study. Arch Neurol 33: 696–705
Amiel-Tison C, Grenier A 1980 Evaluation neuroligique du nouveau-né et du nourisson. Masson, Paris, pp 180–194
Touwen BLC 1979 Examination of the Child with Minor Neurological Dysfunction. In: Clinics in Developmental Medicine, No 71:SIMP. Heinemann, London
Griffiths R 1976 The Abilities of Babies: A Study in Mental Measurement. Association for Research in Infant and Child Development, Amersham, Bucks, U.K., pp 139–218
Hagberg B, Hagberg G, Olow I 1975 The changing panorama of cerebral palsy in Sweden 1954–1970. II. Analysis of various syndromes. Acta Paediatr Scand 64: 193–200
Urenjak J, Williams SR, Gadian DG, Noble M 1993 Proton nuclear magnetic resonance spectroscopy unambiguously identifies different neural cell types. J Neurosci 13: 981–989
Bhakoo KK, Pearce D 2000 In vitro expression of N-acetyl aspartate by oligodendrocytes: implications for proton magnetic resonance spectroscopy signal in vivo. J Neurochem 74: 254–262
Groenendaal F, Van der Grond J, Witkamp TD, De Vries LS 1995 Proton magnetic resonance spectroscopic imaging in neonatal stroke. Neuropediatrics 26: 243–248
Ford CC, Griffey RH, Matwiyoff NA, Rosenberg GA 1992 Multivoxel 1H-MRS of stroke. Neurology 42: 1408–1412
Graham SH, Meyerhoff DJ, Bayne L, Sharp FR, Weiner MW 1994 Magnetic resonance spectroscopy of N-acetylaspartate in hypoxic-ischemic encephalopathy. Ann Neurol 35: 490–494
Gideon P, Henriksen O, Sperling B, Christiansen P, Olsen TS, Jørgensen HS, Arlien-Søborg P 1992 Early time course of N-acetylaspartate, creatine and phosphocreatine and compounds containing choline in the brain after acute stroke; a proton magnetic resonance spectroscopy study. Stroke 23: 1566–1572
Robertson NJ, Cox IJ, Cowan FM, Counsell SJ, Azzopardi D, Edwards AD 1999 Cerebral intracellular lactic alkalosis persisting months after neonatal encephalopathy measured by magnetic resonance spectroscopy. Pediatr Res 46: 287–296
Lorek A, Takei Y, Cady EB, Wyatt JS, Penrice J, Edwards AD, Peebles D, Wylezinska M, Owen-Reece H, Kirkbride V, Cooper CE, Aldridge RF, Roth SC, Brown G, Delpy DT, Reynolds EOR 1994 Delayed (“secondary”) cerebral energy failure after acute hypoxia-ischemia in the newborn piglet: continuous 48-hour studies by phosphorus magnetic resonance spectroscopy. Pediatr Res 36: 699–706
Lopez-Villegas D, Lenkinski RE, Wehrli SL, Ho WZ, Douglas SD 1995 Lactate production by human monocytes/macrophages determined by proton MR spectroscopy. Magn Reson Med 34: 32–38
Petroff OAC, Graham GD, Blamire AM, Al-Rayess M, Rothman DL, Fayad PB, Brass LM, Shulman RG, Prichard JW 1992 Spectroscopic imaging of stroke in humans: histopathology correlates of spectral changes. Neurology 42: 1349–1354
Hanrahan JD, Sargentoni J, Azzopardi D, Manji K, Cowan FM, Rutherford MA, Cox IJ, Bell JD, Bryant DJ, Edwards AD 1996 Cerebral metabolism within 18 hours of birth asphyxia: a proton magnetic resonance spectroscopy study. Pediatr Res 39: 584–590
Penrice J, Cady EB, Lorek A, Wylezinska M, Amess PN, Aldridge RF, Stewart A, Wyatt JS, Reynolds EOR 1996 Proton magnetic resonance spectroscopy of the brain in normal preterm and term infants, and early changes after perinatal hypoxia-ischemia. Pediatr Res 40: 6–14
Graham GD, Blamire AM, Howseman AM, Rothman DL, Fayad PB, Brass LM, Petroff OAC, Shulman RG, Prichard JW 1992 Proton magnetic resonance spectroscopy of cerebral lactate and other metabolites in stroke patients. Stroke 23: 333–340
Hagberg H, Lehmann A, Sandberg M, Nyström B, Jacobson I, Hamberger A 1985 Ischemia-induced shift of inhibitory and excitatory amino acids form intra- to extracellular compartments. J Cereb Blood Flow Metab 5: 413–419
Choi DW 1990 Cerebral hypoxia: some new approaches and unanswered questions. J Neurosci 10: 2493–2501
Siesjö BK 1981 Cell damage in the brain: a speculative synthesis. J Cereb Blood Flow Metab 1: 155–185
Brooks KJ, Kauppinen RA 1993 Calcium-mediated damage following hypoxia in cerebral cortex ex vivo studied by NMR spectroscopy. Evidence for direct involvement of voltage-gated Ca2+-channels. Neurochem Int 23: 441–450
Budd SL 1998 Mechanisms of neuronal damage in brain hypoxia/ischemia: focus on the role of mitochondrial calcium accumulation. Pharmacol Ther 80: 203–229
Pascual JM, Carceller F, Roda JM, Cerdán S 1998 Glutamate, glutamine, and GABA as substrates for the neuronal and glial compartments after focal cerebral ischemia in rats. Stroke 29: 1048–1057
Hagberg H, Andersson P, Kjellmer I, Thiringer K, Thordstein M 1987 Extracellular overflow of glutamate, aspartate, GABA and taurine in the cortex and basal ganglia of fetal lambs during hypoxia-ischemia. Neurosci Lett 78: 311–317
Ross BD 1991 Biochemical considerations in H-spectroscopy. Glutamate and glutamine; myo-inositol and related metabolites. NMR Biomed 4: 59–63
Isaacks RE, Bender AS, Kim CY, Prieto NM, Norenberg MD 1994 Osmotic regulation of myo-inositol uptake in primary astrocyte cultures. Neurochem Res 19: 331–338
Salibi N, Brown MA 1998 Clinical MR Spectroscopy. First Principles. Wiley-Liss, New York, pp F19–F23
Toet MC, Hellström-Westas L, Groenendaal F, Eken P, De Vries LS 1999 Amplitude integrated EEG 3 and 6 hours after birth in full term neonates with hypoxic-ischaemic encephalopathy. Arch Dis Child 81: F19
Eken P, Toet MC, Groenendaal F, De Vries LS 1995 Predictive value of early neuroimaging, pulsed doppler and neurophysiology in full term infants with hypoxic-ischaemic encephalopathy. Arch Dis Child 73: F75
Hanrahan JD, Sargentoni J, Azzopardi D, Manji K, Cowan FM, Rutherford MA, Cox IJ, Bell JD, Bryant DJ, Edwards AD 1996 Cerebral metabolism within 18 hours of birth asphyxia: a proton magnetic resonance spectroscopy study. Pediatr Res 39: 584–590
Acknowledgements
The authors thank Marco Nijenhuis and all other technicians of the MR institute for their enthusiastic cooperation.
Author information
Authors and Affiliations
Additional information
Supported by a donation (Sterproject) of the University Medical Center Utrecht, the Netherlands [A.M.R.].
Rights and permissions
About this article
Cite this article
Roelants-Van Rijn, A., van der Grond, J., de Vries, L. et al. Value of 1H-MRS Using Different Echo Times in Neonates with Cerebral Hypoxia-Ischemia. Pediatr Res 49, 356–362 (2001). https://doi.org/10.1203/00006450-200103000-00009
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/00006450-200103000-00009
This article is cited by
-
Taurine supplementation improves hippocampal metabolism in immature rats with intrauterine growth restriction (IUGR) through protecting neurons and reducing gliosis
Metabolic Brain Disease (2022)
-
Feasibility study for applying the lower-order derivative fast Padé transform to measured time signals
Journal of Mathematical Chemistry (2020)
-
Automatic self-correcting in signal processing for magnetic resonance spectroscopy: noise reduction, resolution improvement and splitting overlapped peaks
Journal of Mathematical Chemistry (2019)
-
Iterative averaging of spectra as a powerful way of suppressing spurious resonances in signal processing
Journal of Mathematical Chemistry (2017)
-
Arterial spin-labelling perfusion MRI and outcome in neonates with hypoxic-ischemic encephalopathy
European Radiology (2015)