Abstract
Dexamethasone is commonly administered to ventilator-dependent preterm infants with chronic lung disease. Infants receiving dexamethasone therapy frequency exhibit decreased rates of weight gain. The purpose of this investigation was to determine whether decreased growth in infants receiving dexamethasone therapy is caused by increased energy expenditure. Twelve infants were studied: 6 received dexamethasone treatment at 2 wk of age and crossed over to receive placebo treatment at 4 wk; the treatment order was reversed in the other 6 infants. The doubly labeled water method was used to determine energy expenditure for a 1-wk period during each treatment phase. The rate of weight gain during dexamethasone treatment was 6.5 ± 10.6 and 20.0 ± 5.7 g/kg/d during placebo treatment. Energy expenditure was 93.1 ± 34.6 kcal/kg/d during dexamethasone treatment and 88.3 ± 37.1 kcal/kg/d during placebo treatment. Energy intake was 119.2 ± 29.0 kcal/kg/d during dexamethasone treatment and 113.8 ± 23.7 kcal/kg/d during placebo treatment. The difference between intake and expenditure, or the energy available for growth, was 26.2 ± 36.8 kcal/kg/d during dexamethasone treatment and 25.5 ± 37.4 kcal/kg/d during placebo treatment. No significant differences were found in energy expenditure or energy intake between the treatment phases. The reduced growth seen in infants receiving dexamethasone treatment cannot be explained by increased energy expenditure or decreased energy intake, but may be due to differences in the composition of newly accreted tissue.
Similar content being viewed by others
Main
DEX is a glucocorticoid commonly used to treat chronic lung disease in ventilator-dependent preterm infants(1–3). DEX therapy has been shown to improve lung compliance and shorten time to extubation. However, it also causes changes in protein, carbohydrate, and lipid metabolism(4,5), which may lead to reduced growth, glucose intolerance, and decreased bone mineralization in these infants(4,6–9). Numerous studies have reported decreased weight gain in preterm infants receiving DEX(4,8–12). Although the mechanisms for this decreased growth rate are not clear, it may be caused by changes in energy balance brought about by DEX therapy.
Corticosteroids have been shown to increase energy expenditure in adults(5,13–15). In addition, corticosteroids have been shown to increase protein turnover(16) which, as an energy expensive metabolic process, contributes to increased energy expenditure. No measurements of energy expenditure in infants receiving corticosteroid therapy have been reported. However, corticosteroid administration has been shown to increase protein turnover in preterm infants(9–11), which suggests the possibility of increased energy expenditure in this population.
The purpose of this study was to test the hypothesis that DEX alters growth rate by increasing energy expenditure in ventilator dependent preterm infants. In this blinded, placebo-controlled study, infants received either DEX or placebo treatment at 2 wk of age and crossed over to receive the opposite treatment at 4 wk of age. The doubly labeled water method was used to measure energy expenditure for a 1-wk period during each of the treatment phases.
METHODS
Subjects. The study population consisted of 12 ventilator dependent very low birth weight infants with chronic lung disease. Patient characteristics at birth are shown in Table 1. These infants were a subset of infants enrolled in a multicenter, randomized, masked, placebo-controlled clinical trial of the optimal timing of DEX therapy in this population(3). Infants were eligible for inclusion in the study at 11-13 d of age if they had birth weights between 501-1500 g, required intermittent mandatory ventilation, and had RIS ≥ 2.4. RIS is defined as mean airway pressure times fraction of inspired oxygen. Infants were excluded from the study if they had received prior postnatal DEX therapy, if congenital cardiovascular, pulmonary, or central nervous system anomalies were present, or if there was clinical evidence of sepsis. The study was approved by the Institutional Review Board of Indiana University-Purdue University at Indianapolis and Informed Consent was obtained from the infants' parents or guardians before initiation of the study.
Infants were randomly assigned to one of the following: group 1 infants received a 14-day course of DEX followed by a 14-day course of placebo (normal saline); group 2 infants received a 14-day course of placebo followed by a 14-day course of DEX or a 14-day course of placebo. DEX was administered as a tapering 14-day course in twice a day doses consisting of 0.25 mg/kg/dose for 5 d, then 0.15, 0.07, and 0.03 mg/kg/dose for 3 d each. Infants were screened at the conclusion of the 14-d course of medication, and started on a tapering 14-d course of DEX if the RIS was ≥ 2.4, or a 14-d course of placebo.
Screening RIS values for the infants in this study are shown in Table 2. No significant differences existed between groups on d 13 of life. However, group 1 infants had significantly lower (p ≤ 0.03) RIS values at the start of phase 2 than at the start of phase 1. Group 2 infants had significantly higher (p ≤ 0.02) RIS values at the start of phase 2 than group 1 infants.
Energy expenditure. Total daily energy expenditure was measured using the DLW method over a 7-day period during each of the two treatment phases. This method is based on the premise that oxygen exists the body as water and CO2 although hydrogen exists solely as water. Therefore, if both oxygen and hydrogen elimination rates are known, the CO2 production rate can be determined by difference. This is accomplished by administration of an oral dose of water labeled with the stable isotopes 18O and deuterium (2H) and subsequent measurement of 18O and deuterium levels in urine over a period of several days. TBW is determined from the dilution of the isotopes in the body water pool. Once the TBW pool size and respiratory or food quotient are known, energy expenditure can be calculated.
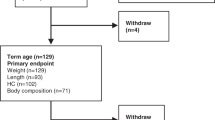
The study timeline is shown in Figure 1. On d 3 of each treatment phase, a baseline urine sample was collected, and an oral dose of DLW (2H- and 18O-labeled water) was administered (2.0 g H2 18O/kg, 10.0 atom % excess, Cambridge Isotope Laboratories, Inc., Andover, MA, and 0.08 g 2H2O/kg, 99.8 atom % excess, Isotec, Inc., Miamisburg, OH). Serial urine samples were obtained over the next 24 h to measure the TBW pool size. Daily urine samples were collected over the next 7 d to measure elimination rates of 2H and 18O. On the last day of each DLW period, a second dose of DLW (1.25 g H2 18O/kg TBW and 0.05 g 2H2O/kg TBW) was given, and serial urine samples were again collected over the next 24 h to measure any changes in TBW. All urine samples were obtained from cotton balls placed in the infant's diaper, and the date and time of collection recorded. Samples were prepared for isotopic analysis using standard vacuum techniques and isotopic enrichment measured by isotope ratio mass spectrometry (Finnegan MAT 252, San Jose, CA).
To examine the magnitude of changes in isotopic baseline due to influx of unlabeled water from dietary sources or labeled water from re-breathing, urine samples were collected from two infants meeting inclusion criteria for the study who did not receive DLW. Daily urine samples were collected. Fluctuations in 18O enrichment produced a SD of 0.6 per mil around the mean enrichment for the week; the estimated analytical SD is 1.4 per mil. Fluctuations in 2H enrichment produced a SD of 7.9 per mil; the estimated analytical SD is 3.5 per mil. Doses of the isotopes were chosen so that these observed isotopic fluctuations would produce <1% error in maximum isotopic enrichments. Differences of this magnitude in maximum isotopic enrichment would produce approximately a 1.5% error in energy expenditure.
Weights and caloric intakes (enteral and parenteral) of the infants were recorded daily. Respiratory status, ventilator setting, and medications were also recorded throughout the study.
Anthropometry. Anthropometric measurements were recorded at birth and at the beginning and end of each phase of the study. Weight was measured to the nearest g. Crown-heel length and OFC were measured to the nearest mm using a nonstretchable plastic measuring tape (1 cm wide). All measurements were taken by to observers and each observer took three measurements. Mean values were then used.
Calculations. Isotopic dilution space was determined from the amount of isotope given to each infant and from the baseline and peak concentrations of the isotope in the urine. The TBW was determined from the dilution space of both isotopes(17). No difference in TBW results using 18O or deuterium was found; mean values were used in further calculations. The deuterium and 18O elimination rates were then calculated from the isotope enrichments in the samples over each 7 d period. The isotopic elimination rates were used to calculate the rate of CO2 production in mol/day(18). CO2 production was converted to total daily energy expenditure in kcal/kg/day using the modified Weir formula(18,19). TEE was calculated using an RQ of 0.91 as suggested for infants in this age group(20–22).
Statistics. Results were compared using paired t tests, analysis of variance and analysis of covariance. Data are expressed as mean ± SD.
RESULTS
Infant characteristics at the start of each phase of the DLW study are shown in Table 3. No significant differences existed between the two groups in age, weight, length, or OFC at the start of the either phase of the study. Group 1 infants had significantly (p ≤ 0.005) lower RIS values at the start of the DLW period during DEX treatment than group 2 infants receiving placebo. Group 2 infants had significantly (p ≤ 0.005) higher RIS values at the start of the DLW period during placebo treatment than during DEX treatment.
Table 4 shows the growth rates of the infants during each treatment. Infants showed significantly lower rates of change in weight (p ≤ 0.01) and OFC (p ≤ 0.01) during DEX treatment than when receiving placebo. Linear growth rate was also slower during DEX treatment. There were no significant changes in the % TWB over the entire study period, regardless of treatment. During DEX treatment, % TBW was 82.2 ± 9.0%; during placebo treatment, % TBW was 81.8 ± 7.7%.
Energy expenditures, energy intakes and weight gains during the two treatment phases are compared in Figure 2. No statistically significant correlation was found between energy expenditure and birth weight, age, or treatment. Total energy expenditure was 93.1 ± 34.6 kcal/kg/d (range 51.7-158.8 kcal/kg/d) during DEX treatment and 88.3 ± 37.1 kcal/kg/d (range 51.7-168.6 kcal/kg/d) during placebo treatment. Energy intake was 119.2 ± 29.0 kcal/kg/d (range 63.0-162.0 kcal/kg/d) during DEX treatment and 113.8 ± 23.7 kcal/kg/d (range 74.5-142.0 kcal/kg/d) during placebo treatment. Enteral and parenteral feeds provided 84.9 and 15.1% of total calories respectively during DEX treatment and 86.0 and 14.0%, respectively, during placebo treatment. Energy intake was significantly (p ≤ 0.05) correlated with age. The difference between energy intake and energy expenditure largely reflects the energy stored in newly accreted tissue. This difference was 26.2 ± 36.8 kcal/kg/d (range -34.8-70.0 kcal/kg/d) during DEX treatment and 25.5 ± 37.4 kcal/kg/d (range -40.3-73.2 kcal/kg/d) while receiving the placebo. Two infants had differences between intake and expenditure <0 during the DEK phase and two infants had differences <0 during the placebo phase. One infant had differences <0 during both treatment phases.
DISCUSSION
We have examined energy balance and growth using the doubly labeled water method in a group of ventilator-dependent preterm infants with chronic lung disease. No differences were found in energy expenditure or energy intake between the treatment phases. Although the energy balance was identical during the two treatment phases, the rate of weight gain during DEX treatment was approximately one-third of that during placebo treatment. Infants also displayed slower rates of increase in length and OFC during DEX treatment.
The DLW method for measuring energy expenditure has been validated in both preterm(20–22) and term infants(18,23–25). The method is potentially more sensitive to errors in preterm infants than in other populations due to their rapid growth rates, high % TBW, and rapid H2O turnover relative to the rate of CO2 production. We attempted to minimize potential errors in the method by measuring TBW at the beginning and end of each phase of the study and by choosing high enough doses of the isotopes to avoid analytical difficulties due to high turnover rates. Because infants from both treatment groups were studied under identical conditions, any remaining methodological errors would affect each group equally.
Contrary to our hypothesis, no increase in total energy expenditure was found during DEX treatment. In addition, no effect of age or treatment order on energy expenditure was found. This finding differs from the results found in adults. Both Brillon et al.(13) and Tataranni et al.(5) measured 10-15% increases in resting energy expenditure after the acute administration of corticosteroids in adults. In addition, Tatarrani et al.(5) also measured significantly elevated 24-h energy expenditure after 4 d of steroids. Horber et al.(14) demonstrated significant increases in resting energy expenditure after 7 d of prednisone therapy in the fed state but not in the fasted state. Similarly, Chong et al.(15) also showed no change in resting energy expenditure after 7 d of steroid therapy, but determined a significant 26% increase in total energy expenditure using the doubly labeled water method.
Infants may simply respond to DEX treatment differently than adults, and may not increase their energy expenditure in response to DEX. However, we cannot rule out the possibility that energy expenditure was in fact somewhat elevated in these infants by the use of DEX, but that this increase was offset by decreases in energy expenditure elsewhere. It has been suggested that improvements in pulmonary mechanics in preterm infants resulting from DEK therapy(26) could cause a decrease in energy expenditure in these infants(8). In addition, Bos et al.(27) studied general movements of preterm infants receiving DEX and noted that both the amount and intensity of movement decreased in response to DEX administration, suggesting that the energy expended in physical activity may be decreased in these infants. However, Thureen et al.(28) performed direct measurements of the energy expended in physical activity in a group of preterm infants and found that it comprised only ∼3.5% of total energy expenditure. Therefore, possible changes in the physical activity levels of infants on DEX would likely have a minimal impact on total energy expenditure.
No differences were found in energy intake between the two treatment phases. Although we cannot completely rule out the possibility of differences in nutrient absorption during the two treatment phases, we have found no reports of malabsorption due to corticosteroid treatment. Therefore, because neither energy intake nor energy expenditure differed between treatment groups, there was no difference in energy balance (intake minus expenditure) between groups.
Despite identical energy balance between the two treatments, regardless of order, we found substantially decreased rates of weight, length, and OFC gain in infants receiving DEX. Decreased rates of weight gain in preterm infants in response to DEX therapy for chronic lung disease has been noted previously(3,4,8–12). Weiler et al.(7) also reported significantly decreased linear growth in DEX-treated preterm infants despite similar caloric intakes between the DEX-treated infants and controls. Both Weiler et al.(7) and Papile et al.(3) reported decreased rates of change in OFC in infants receiving DEX. Our results strongly suggest that this decreased growth is not due to changes in energy balance caused by DEX treatment.
Because changes in energy balance resulting from DEX therapy cannot account for the growth reductions seen in these infants, the effect of DEX on body composition and the composition of newly accreted tissue must be examined. Corticosteroids have been shown to increase protein catabolism in animals(29–31) adults(5,32) and preterm infants(9–11). In premature infants, it is clear that DEX-induced increases in protein catabolism result in a substantial reduction in protein accretion(9). Corticosteroids have also been shown to alter lipid metabolism by increasing the activity of lipoprotein lipase(33) and promoting the maturation of adipocytes(34,35), leading to increases in fat mass. In piglets receiving DEX at doses similar to those used in preterm infants, reduced growth rates were accompanied by significant increases in fat mass and decreases in lean tissue(31).
Our results support the concept that DEX reduces growth rate primarily by altering the composition of weight gain. The estimated energy content of new tissue (energy balance/weight gain) is 3-fold higher during DEX therapy, suggesting accretion of more fat and less protein. It must be noted that relatively small absolute changes in fat and protein accretion can produce substantial changes in the rate of weight gain. The composition of weight gain can be estimated assuming a 12% protein content in lean tissue of premature infants(36), and caloric value of tissue protein (5.65 kcal/g) and fat (9.25 kcal/g). Using these assumptions, accretion rates of ∼1.5 g/kg/d of fat and ∼1.8 g/kg/d of protein can account for the energy balance and rate of weight gain observed during the placebo period. During DEX therapy, an increase in fat accretion of ∼2.4 g/kg/d and a decrease in protein accretion to ∼0.6 g/kg/d can account for the reduced rate of weight gain and similar energy balance observed in this period. These changes in the composition of weight gain will only minimally alter overall body composition in a 1-wk period, and are too small to be detected by the techniques used in our study.
In conclusion, we have demonstrated that the reduced rates of growth observed in preterm infants receiving DEX therapy for chronic lung disease cannot be explained by increased energy expenditure or reduced energy intake. Lower growth rates in the face of unchanged energy expenditure or intake strongly suggest that DEX alters the composition of newly accreted tissue toward fat and away from protein. These findings suggest that a strategy simply directed at increasing caloric intake in infants receiving DEX is unlikely to be successful in achieving normal growth. Future strategies designed to ameliorate the nutritional effects of DEX will need to include precise measures of overall body composition and the composition of weight gain.
Abbreviations
- DEX:
-
dexamethasone
- DLW:
-
doubly labeled water
- OFC:
-
occipitofrontal circumference
- RIS:
-
respiratory index score
- TBW:
-
total body water
References
Avery G, Fletcher A, Kaplan M, Brudno S 1985 Controlled trial of dexamethasone in respirator-dependent infants with bronchopulmonary dysplasia. Pediatrics 75: 106–111
Collaborative Dexamethasone Trial Group 1991 Dexamethasone therapy in neonatal chronic lung disease: an international placebo-controlled trial. Pediatrics 88: 421–427
Papile L, Tyson JE, Stoll BJ, Wright LL, Donovan EF, Bauer CR, Krause-Steinrauf H, Verter J, Korones SB, Lemons JA, Fanaroff AA, Stevenson DK, Ehrenkranz RA, Shankaran S 1998 Multi-center trial of two dexamethasone therapy regimens in ventilator-dependent premature infants. N Engl J Med 338: 1112–1118
Yeh T, Torre J, Rastogi A, Anyebuno M, Pildes R 1990 Early postnatal dexamethasone therapy in premature infants with severe respiratory distress syndrome: a double-blind, controlled study. J Pediatr 117: 273–282
Tataranni P, Larson D, Snitker S, Young J, Flatt J, Ravussin E 1996 Effects of glucocorticoids on energy metabolism and food intake in humans. Am J Physiol 271:E317–E325
Cummings JJ, D'Eugenio DB, Gross SJ 1989 A controlled trial of dexamethasone in preterm infants at high risk for bronchopulmonary dysplasia. N Engl J Med 320: 1505–1510
Weiler HA, Paes B, Shah JK, Atkinson SA 1997 A longitudinal assessment of growth and bone mineral accretion in prematurely born infants treated for chronic lung disease with dexamethasone. Early Hum Dev 47: 271–286
Gibson A, Pearse R, Wales J 1993 Growth retardation after dexamethasone administration: assessment by knemometry. Arch Dis Child 69: 505–509
Van Goudoever J, Wattimena J, Carnielli V, Sulkers E, Degenhart J, Sauer P 1994 Effect of dexamethasone on protein metabolism in infants with bronchopulmonary dysplasia. J Pediatr 124: 112–118
Brownlee K, Ng P, Henderson M, Smith M, Green J, Dear P 1992 Catabolic effect of dexamethasone in the preterm baby. Arch Dis Child 67: 1–4
Williams A, Jones M 1992 Dexamethasone increases plasma amino acid concentrations in bronchopulmonary dysplasia. Arch Dis Child 67: 5–9
Shrivastava A, Lyon A, McIntosh N 1995 The effect of dexamethasone on growth and bone mineralization in preterm infants with chronic lung disease. Early Hum Dev 43: 101
Brillon D, Zheng B, Campbell R, Matthews D 1995 Effect of cortisol on energy expenditure and amino acid metabolism in humans. Am J Physiol 268:E501–E513
Horber H, March M, Haymond MW 1991 Differential effects of prednisone and growth hormone on fuel metabolism and insulin antagonism in humans. Diabetes 40: 141–149
Chong P, Jung R, Scrimgeour C, Rennie M 1994 The effect of pharmacological dosages of glucocorticoids on free living total energy expenditure in man. Clin Endocrinol 40: 577–581
Daurman D, Matthews DE, Bier DM 1988 Physiological hypercortisolemia increases proteolysis, glutamine and alanine production. Am J Physiol 255:E366–E373
Schoeller D, van Santen E, Peterson D, Dietz W, Jaspan J, Klein P 1980 Total body water measurement in humans with 18O and 2H labeled water. Am J Clin Nutr 33: 2686–2693
Jones P, Winthrop A, Schoeller D, Swyer P, Smith J, Filler R, Heim T 1986 Validation of doubly labeled water for assessing energy expenditure in infants. Pediatr Res 21: 242–246
Weir J 1949 New methods for calculating metabolic rate with special reference to protein metabolism. J Physiol 109: 1–9
Roberts SB, Coward WA, Schlingenseipen K-H, Nohria V, A. L 1986 Comparison of the doubly labeled water (2H218O) method with indirect calorimetry and a nutrient-balance study for simultaneous determination of energy expenditure, water intake, and metabolizable energy intake in preterm infants. Am J Clin Nutr 44: 315–322
Westerterp KR, Lafeber HN, Sulkers EJ, Sauer PJJ 1991 Comparison of short term indirect calorimetry and doubly labeled water method for the assessment of energy expenditure in preterm infants. Biol Neonate 60: 75–82
Jensen CL, Butte NF, Wong WW, Moon JK 1992 Determining energy expenditure in preterm infants: comparison of 2H218O method and indirect calorimetry. Am J Physiol 263:R685–R692
Jones PJH, Winthrop AL, Schoeller DA, Filler RM, Swyer PR, Smith J, Heim T 1988 Evaluation of doubly labeled water for measuring energy expenditure during changing nutrition. Am J Clin Nutr 47: 799–804
Roberts SB, Coward WA, Ewing G, Savage J, Cole TJ, Lucas A 1988 Effect of weaning on accuracy of doubly labeled water method in infants. Am J Physiol 254:R622–R627
Bronstein M, Davies P, Hambidge K, Accurso F 1995 Normal energy expenditure in the infant with presymptomatic cystic fibrosis. J Pediatr 126: 28–33
Yoder MC, Chua R, Tepper R 1991 Effect of dexamethasone on pulmonary inflammation and pulmonary function of ventilator-dependent infants with bronchopulmonary dysplasia. Am Rev Respir Dis 143: 1044–1048
Bos AF, Martijn A, van Asperen RM, Hadders-Algra M, Okken A, Prechtl HFR 1968 Qualitative assessment of general movements in high-risk preterm infants with chronic lung disease requiring dexamethasone therapy. J Pediatr 132: 300–306
Thureen PJ, Phillips RE, Baron KA, DeMarie MP, Hay WW 1998 Direct measurement of the energy expenditure of physical activity in preterm infants. J Appl Physiol 85: 223–230
Tomas FM, Munroe HN, Young VR 1979 Effect of glucocorticoid administration on the rate of muscle protein breakdown in vivo in rats, as measured by urinary excretion of N-methylhistidine. Biochem J 178: 139–146
Rannels SR, Jefferson LS 1980 Effects of glucocorticoids on muscle protein turnover in perfused rat hemicorpus. Am J Physiol 238:E564–E572
Weiler HA, Wang Z, Atkinson SA 1997 Whole body lean mass is altered by dexamethasone treatment through reductions in protein and energy utilization in piglets. Biol Neonate 71: 53–59
Bennet WM 1992 Growth hormone and lean tissue catabolism during long-term glucocorticoid treatment. Clin Endocrinol 36: 161–164
Appel B, Fried S 1992 Effects of insulin and dexamethasone on lipoprotein in human adipose tissue. Am J Physiol 262:E695–E699
Gregoire F, Genart C, Hauser N, Remacle C 1991 Glucocorticoids induce a drastic inhibition of proliferation and stimulate differentiation of adult rat fat cell precursors. Exp Biol Res 196: 270–278
Hauner H, Schmid P, Pfeiffer EF 1987 Glucocorticoid and insulin promote the differentiation of human adipocyte precursors into fat cells. J Clin Endocrinol 64: 832–835
Ziegler E, O'Donnell A, Nelson S 1976 Body composition of the reference fetus. Growth 40: 329–341
Author information
Authors and Affiliations
Additional information
Supported by grants from the James Whitcomb Riley Memorial Association and the National Institutes of Health (S10-RR-07269, M01-RR-750, R01-HD-29153).
Rights and permissions
About this article
Cite this article
Leitch, C., Ahlrichs, J., Karn, C. et al. Energy Expenditure and Energy Intake During Dexamethasone Therapy for Chronic Lung Disease. Pediatr Res 46, 109–113 (1999). https://doi.org/10.1203/00006450-199907000-00018
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/00006450-199907000-00018
This article is cited by
-
A review and guide to nutritional care of the infant with established bronchopulmonary dysplasia
Journal of Perinatology (2023)