Abstract
Inasmuch as smooth muscle contractile protein abnormalities may account for the maintenance of a high pulmonary vascular resistance, we evaluated the pulmonary arterial myosin light chain kinase (MLCK) and phosphatase (MLCP) in normal and pulmonary hypertensive (PH) fetal sheep. In addition, aorta and vena cava MLCP and MLCK activities were also measured. The MLCK activity(nanomoles/min/mg) was determined by the incorporation of[32P]PO4-3 to the 20-kD smooth muscle myosin light chains and the MLCP activity by assaying for the dephosphorylation of the 20-kD myosin light chain (MLCP-light chain) and heavy meromyosin (MLCP-HMM). The MLCP content was determined by Western blot analysis. PH was characterized by a significant increase in the right-to-left ventricular wall weight ratio from 0.99 ± 0.04 in the control to 1.52 ± 0.12 in the experimental group (p < 0.01). The pulmonary MLCP-light chain and MLCP-HMM activities in the experimental group were 2.0 ± 0.2 and 1.3 ± 0.2 and significantly lower than in the control group values (3.8 ± 0.5 and 2.5 ± 0.3; p < 0.01). The MLCK activity was 9.6± 1.2 in the control and 7.8 ± 0.7 in the experimental fetal pulmonary artery (p = NS). The activities of both enzymes in the aorta and vena cava samples were not altered by PH. The MLCP content in experimental animals (0.50 ± 0.09 OD × mm2) was significantly lower than that for the control pulmonary tissue (1.72 ± 0.42; p < 0.01), suggesting that PH down-regulates pulmonary vascular MLCP expression. In conclusion, the maintenance of a high pulmonary vascular resistance in PH may be secondary to abnormalities in tissue content and/or activity of MLCP.
Similar content being viewed by others
Main
PPHN is a condition associated with a maintenance of high pulmonary vascular resistance postnatally. Its etiology is unknown, but the pathogenesis of the syndrome is thought to be related to an increase in pulmonary vascular muscularization and extension of muscle to peripheral, not normally muscular, arteries, resulting in an increase in the vascular resistance postnatally to blood flow(1). Recently, nitric oxide inhalation has been introduced as part of the therapy in infants with this condition(2, 3). Although it is a potent vasodilator, not all infants with PPHN exhibit an improvement in blood oxygenation with nitric oxide(4), suggesting that factors other than pulmonary vasoconstriction may contribute to the failure of the vascular resistance to decrease after birth.
Closure of the ductus arteriosus prenatally in sheep either by indomethacin administration(5), or by mechanical constriction(6, 7) has been shown to induce lung histologic and central hemodynamic changes similar to those observed in infants with PPHN. Yet, the factors accounting for the maintenance of a high pulmonary vascular resistance postnatally in this sheep model of PPHN are unknown. We have previously reported significant abnormalities in the pulmonary vascular smooth muscle mechanical property in this animal model syndrome(8). In spite of the increased muscularization of these vessels, the pulmonary smooth muscle of the hypertensive animals exhibits a lower stress, similar shortening capacity, and significantly longer half-relaxation time(8).
Recent data indicate that abnormalities of pulmonary endothelial cell function and vascular smooth muscle may account for the hemodynamic changes in the fetal sheep. A decrease in nitric oxide(9) and endothelin receptor (ETB) activity(10) have been demonstrated after partial ligation of the ductus arteriosus. Abnormalities in the generation of cGMP by the pulmonary vascular smooth muscle have also been reported(11) and may account for the observed longer muscle relaxation.
Smooth muscle contraction and relaxation are primarily dependent on the rates of phosphorylation and dephosphorylation of the 20-kD light chains of myosin by MLCK and MLCP, respectively. These enzymes are two key smooth muscle regulatory proteins. Disease-related alteration in the content and/or activities of these enzymes may impair the muscle contractile apparatus and could play a role in the maintenance of high resistance to blood flow in a vascular bed. To our knowledge, the activities of these enzymes in neonatal or adult pulmonary hypertension have not been previously evaluated.
The purpose of the present study was to evaluate the MLCK and MLCP activities in pulmonary, aortic, and vena cava tissues of normal and pulmonary hypertensive fetal sheep. We hypothesized that pulmonary MLCK and MLCP activity was reduced in pulmonary hypertension.
METHODS
Animal preparation. Pregnant ewes between 123 and 127 d of gestation (term, 145 d) were fasted for at least 24 h before surgery. The ewes were anesthetized with i.v. pentobarbital sodium (loading dose, 20 mg/kg; maintenance, 1 mg/kg every 30 min). Eight animals constituted the experimental group. The fetal heads and upper chests of these animals were delivered through a uterine incision under sterile conditions. A left fetal thoracotomy was performed, exposing the heart and great vessels. The ductus arteriosus was identified and ligated with 2-0 silk sutures. The chest was closed in layers. The fetus was carefully returned to the uterus, the wall of which was closed in layers. Particular care was taken to avoid any significant amniotic fluid loss. The ewe received penicillin (1 × 106 U) and gentamicin (50 mg) intramuscularly twice daily for 4 d. Thirteen noninstrumented fetuses, eight of which were twins of the experimental animals, served as controls.
Ten days post ductus arteriosus ligation in the experimental group or at 135 d of gestation in the controls, the ewes were subjected to a cesarean section under sodium pentobarbital anesthesia. The fetuses were removed and killed with an i.v. dose of potassium chloride, and the lungs were removed in block. Segments of the thoracic aorta and vena cava were excised, washed with normal saline solution (to eliminate any remainder pentobarbital or potassium chloride), weighed, and frozen for later analyses. Confirmation of the effective ligature of the ductus arteriosus in the experimental animals was always sought by probing the ductus arteriosus from the pulmonary artery side during postmortem examination. The second generation intralobar pulmonary artery segments were dissected, washed and cleaned within minutes after death, weighed, and immediately frozen at -80°C for later analysis. The right and left cardiac ventricular free wall and the septum were removed immediately after death and weighed for assessment of the degree of right ventricular hypertrophy. We have previously shown that right ventricular hypertrophy in this animal model is always associated with histologic evidence of pulmonary hypertension(12).
This protocol was approved by the University of Manitoba Committee on Animal Experimentation.
Preparation of tissue extracts. Because the vascular tissues collected for analysis were not of the same size and lengths, the tissues were extracted with the same ratios of tissue:volume of extraction buffer to result in extracts with comparable weight of tissue per unit volume of extraction buffer. The frozen tissue was ground and homogenized in four volumes of extraction buffer (0.5 mM NaCl, 50 mM Tris-HCl, pH 7.5, 10 mM MgCl2, 1 mM EDTA, 1 mM EGTA, 5 mM DTT) in the presence of protease inhibitors (0.1 mM phenylmethylsufonyl fluoride, 10 mg/L benzylarginylmethyl ester, 10 mg/L soy bean trypsin inhibitor, 1 mg/L leupeptin, 1 mg/L pepstatin, and 10 mg/L L-1-tosylamido-2-phenylethyl chloromethyl ketone) at 4°C for 1 h. The homogenate was centrifuged in a microcentifuge at 15 000 rpm for 15 min at 4°C, and the supernatant of the extract was assayed for enzyme activities. The protein concentration of the extract was determined by the method of Bradford(13).
MLCK activity assay. The MLCK activity was determined in a reaction mixture (100 μL) containing 50 mM Tris-HCl, pH 7.5, 1.6 mg/mL 20-kD turkey gizzard myosin light chains, 0.1 mM [32P]ATP, 0.2 mM CaCl2, 10 mM MgCl2, and 0.1 mM calmodulin at 24°C(14). The reaction was initiated by the addition of the extract. The time course of the reaction was determined by taking 20-μL aliquots of the reaction mixture at various times and spotting on strips of P81 phosphocellulose paper. The paper strips were washed with 75 mM H3PO4, dried, and counted in a liquid scintillation counter. The MLCK activity (nanomoles of [32P]PO4-3 incorporated/min/mg of extract) was calculated from the linear portion of the activity curve with respect to time. To correct for Ca2+-independent protein kinase activities in the extract, the kinase was assayed in the presence of EGTA. No significant activity was observed under this condition. To determine the contribution of multifunctional calmodulin-dependent protein kinase II to the measured MLCK activity, the assay was performed in the presence of KN-93 (Calbiochem), an inhibitor of calmodulin-dependent protein kinase, and KN-92 (Calbiochem), the negative control for KN-93. No difference in the MLCK activity was observed in the presence of 5 μM KN-92 and KN-93, suggesting that the extracts do not contain significant calmodulin-dependent protein kinase II activity.
MLCP activity assay. MLCP activity was monitored by the release of [32P]PO4-3 from the substrate(15). The two substrates used were[32P]PO4-3-labeled 20-kD myosin light chain and myosin HMM, which were prepared from turkey gizzards and phosphorylated by MLCK. HMM is a chymotryptic fragment of myosin that retains the structure of the head region and its actin-activated MgATPase activity, but could not polymerize due to the loss of a part of its tail region. As a consequence, HMM is soluble at high concentration in low ionic strength solutions. Under these conditions, myosin precipitates out. Therefore, we preferentially used HMM to myosin in our study. The dephosphorylation reaction was initiated by addition of tissue extract to a reaction mixture (total volume of 200 μL) containing 50 mM Tris-HCl, pH 7.4, 2 μM myosin light chains, or 0.5 mM myosin HMM and 1 mM DTT at 30°C. The time course of the reaction was determined by taking a 40-μL aliquot of the reaction mixture at various times and pipetting it into 100 μL of 17.5% trichloroacetic acid to terminate the reaction. After the addition of 100 μL of 6 mg/mL BSA, the resulting mixture was chilled and centrifuged at 15 000 rpm for 1 min in a microcentrifuge. A 200-μL aliquot of the supernatant was taken, added to 4 mL of scintillation fluid, and counted in a scintillation counter. The activity of the enzyme was calculated from the linear portion of the enzyme activity curve with respect to time and expressed as nanomoles of substrate dephosphorylated/min/mg of extract.
Western blot analyses. The extracts (16 μg) were applied to 12.5% SDS-polyacrylamide gels and electroblotted to nitrocellulose paper according to a modified method of Towbin et al.(16). To facilitate the transfer of the proteins to the nitrocellulose paper, 0.1% SDS was included in the transfer buffer. The efficiency of transfer was verified by staining the gel with Coomassie Blue after the transfer. The blot was blocked overnight with 5% nonfat dry milk in TTBS (20 mM Tris-HCl, pH 7.5, 500 mM NaCl, 0.05% Tween-20). The blots were incubated with the primary antibodies in TTBS with 1% nonfat milk and then with horseradish peroxidase-conjugated secondary antibodies in TTBS containing 2.5% nonfat milk. All washes were carried out with TTBS containing 2.5% nonfat milk. The cross-reactivity of the antibodies was detected by chemiluminescence using a mixture of equal volumes of enhanced luminol reagent and oxidizing reagent. The primary antibodies used for detection of PP1 was MAb against the catalytic subunit of PP1 from rabbit skeletal muscle (gift of Dr. Jackie Vandenheede, Leuven University, Belgium). The crossreactivity was quantitated by two-dimensional scanning of the autoradiograms of the blots with a high resolution scanner (ImageMaster Analyser, Pharmacia). The control and experimental lanes were loaded with equal amounts of tissue extract (16 μg of protein), and the intensity of the 43-kD bands served as an internal control of the amount of samples applied to the lanes. The content was expressed as OD per band area (OD × mm2).
Statistical analysis. Data were processed by ANOVA. All data are reported as mean ± SEM, and p < 0.05 was considered significant.
RESULTS
Eight experimental and 13 control fetuses were studied. The experimental fetuses had a gestational age of 132 ± 1 d and weight of 3.5 ± 0.1 kg, compared with 134 ± 1 d and 3.6 ± 0.2 kg in the experimental group. The average duration of ductus arteriosus ligation in the experimental group was 10 ± 2 d.
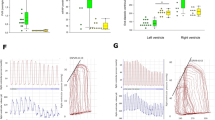
The right-to-left ventricular wall weight ratio was 0.99 ± 0.04 in the control and 1.52 ± 0.35 in the experimental (p < 0.01) animals. The control group right ventricular/left ventricular + septum weight ratio was 0.55 ± 0.02 and significantly greater in the experimental group (0.76 ± 0.04; p < 0.01).
The pulmonary artery extracts prepared from both normal and experimental animals were assayed for protein concentration and MLCK and MLCP enzymatic activities. The pulmonary vascular protein concentration of the control extracts was 4.7 ± 0.6 mg/mL and significantly higher than those of the experimental fetuses (7.2 ± 1.0 mg/mL; p < 0.01). Comparison of the MLCP activity toward the substrates, 20-kD myosin light chains, and HMM (Fig. 1), showed that the phosphatase activity is reduced by about 50% in the ductus arteriosusligated animals(p < 0.01). On the other hand, the pulmonary MLCK activity of the experimental animals was slightly lower but not significantly different from that of the control (Fig. 2).
In contrast to the pulmonary arteries, no significant difference was observed in the MLCP activity with either substrate (Fig. 1) of the aorta and vena cava tissues of the experimental and control animals. The MLCK activity of the aorta and vena cava was also similar for both groups (Fig. 2).
To evaluate whether the decrease in the MLCP activity in the experimental pulmonary arteries was due to a reduced enzymatic tissue content or function, Western blot analysis with MAb to the catalytic subunit of PP1 was carried out in six experimental and control animals' tissue extracts.Figure 3 depicts representative samples of the results of the Western blots of the pulmonary tissue. The MLCP content in experimental animals (0.50 ± 0.09 OD × mm2) was significantly lower than that for the control pulmonary tissue (1.72 ± 0.42; p< 0.01).
DISCUSSION
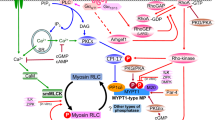
The smooth muscle contractile apparatus consists of the contractile proteins actin and myosin, as well as other associated regulatory proteins, such as tropomyosin, calmodulin, calponin, MLCK, and MLCP. The activities of MLCK and MLCP determine the state of phosphorylation and dephosphorylation of the myosin light chains, which is the prime factor regulating smooth muscle contraction and relaxation(17). The phosphorylation of Ser19 of the two 20-kD light chains of myosin by MLCK, a Ca2+ - and calmodulin-dependent kinase, is a fundamental step for activation of myosin and the formation of actin-myosin cross-bridges necessary for muscle contraction. Dephosphorylation of myosin by MLCP is required for muscle relaxation. Thus, MLCK and MLCP play important roles in the contractile activity of smooth muscle.
We have previously reported that both PP1 and PP2 are present in smooth muscles. SMP-I (PP2A), -II (PP2C), -III (PP1), and -IV (PP1) have been purified from turkey gizzards(18) and rabbit uterine muscle(19). SMP-III is composed of regulatory subunits, 130 and 20 kD, and catalytic subunit, 38 kD, and is the same as the myosin protein phosphatase, PP1M, reported by other investigators(20). SMP-IV is composed of 58- and 38-kD subunits and is a derivative of SMP-III. The 55-kD subunit was demonstrated to be a proteolytic product of the 130-kD subunit of SMP-III(21). All these enzymes rapidly dephosphorylate the isolated myosin light chains but only PP1s, SMP-III and IV, dephosphorylate the intact myosin and HMM, although the phosphorylated amino acid in both substrates are the same. Thus, the activity of the extracts toward myosin light chains reflects the activities of both PP1 and PP2, whereas the activity toward myosin HMM represents the activity of PP1, the enzyme which appears to be directly involved in smooth muscle relaxation.
In the present study, we documented a significant reduction in the MLCP activity in the pulmonary vascular arterial tissue of ductus arteriosus-ligated fetal sheep. This change in MLCP activity was not observed in other tissues assayed (aorta and vena cava). The pulmonary vascular MLCP content was also reduced. Given our previous finding that in the fetal sheep model of pulmonary hypertension the DNA content per tissue weight of the second generation pulmonary artery is unchanged(12), the present data indicate a decrease in the pulmonary vasculature cellular phosphatase content. Thus, the changes associated with pulmonary hypertension in this model are accompanied by synthesis down-regulation of the key enzyme responsible for muscle relaxation in the pulmonary arterial vasculature.
In the ductus arteriosus-ligated fetal sheep model of PPHN we have previously reported major smooth muscle biochemical and mechanical property abnormalities(8). In these fetuses, the myosin heavy chain content of the second through fifth generation pulmonary vessels was increased with an abnormal stoichiometric distribution, characterized by a greater proportion of the nonmuscle myosin isoform and an increased ratio of the high and low MHC isoforms. In addition, both decreased actin:myosin ratio and myofibrillar ATPase activity were observed in the ductus-ligated pulmonary vascular tissue, suggesting a lower potential for cross-bridge cycling and myosin light chain phosphorylation. These changes were associated with evidence that the pulmonary vascular muscle in the pulmonary hypertensive animals developed less response to electrical and high potassium stimulation and showed prolonged isotonic relaxation.
SMP-III and -IV, which are also generally referred to as PP1M, has previously been implicated as the enzyme which dephosphorylates myosin in vivo and elicits relaxation in smooth muscles(18, 20). Indeed, incubation of precontracted permeabilized smooth muscle fibers with SMP-IV resulted in the dephosphorylation of the myosin light chains and relaxation of the muscle fibers(22, 23). The rate of smooth muscle relaxation has been previously shown to directly related to the MLCP activity in nonvascular(24, 25) and vascular tissue(26). Finally, the observation that the rate of relaxation is inhibited partially by spermine and completely by microcystin, a potent phosphatase inhibitor, provides further evidence for the role of SMP-IV or PP1M in smooth muscle relaxation(23).
The present data suggest that the previously reported longer pulmonary muscle relaxation time exhibited by these fetal sheep(8) is due to hypertension-induced changes in the key smooth muscle regulatory enzyme responsible for muscle relaxation. That the enzyme involved in this process is type 1 protein phosphatase is supported by the observed decrease in the MLCP activity toward heavy chain meromyosin and lowered content of the catalytic subunit of PP1, as indicated by Western blot analysis. The changes observed in this study are consistent with the significant reduction in the rate of myosin dephosphorylation after mechanical strain previously reported in the airway smooth muscle cells(27). Finally, the observed higher pulmonary vascular protein content of the experimental animals is consistent with our previous reported increased pulmonary arterial myosin content in the fetal sheep with pulmonary hypertension(8).
No significant changes in the MLCK activity of any of the studied vessels was observed in our study. In the spontaneously hypertensive rat, Vescovo et al.(28) have observed downregulation of the expression of this smooth muscle enzyme in the renal arteries. The authors suggested that vascular smooth muscle hypertrophy associated with systemic hypertension induces intracellular changes in the expression of major smooth muscle enzymes as part of the remodeling process. In the fetal sheep model of pulmonary hypertension there was a tendency for a lower MLCK activity that did not reach statistical significance.
In the present study, we evaluated the MLCK and MLCP activities of only second generation pulmonary arteries. Although resistance to blood flow in the lung is observed at the level of smaller arteries, our measurements were limited to the second generation pulmonary arteries because we previously observed and documented abnormalities in the smooth muscle mechanical properties of this tissue(8).
Factors other than alterations in the MLCK and MLCP activity might also account for the maintenance of a higher pulmonary vascular resistance postnatally in the this animal model of PPHN. Abnormalities in endothelial cell function have been reported in this animal model. These include a decreased nitric oxide(9) and endothelin ETB receptor activity(10). In addition, cGMP abnormalities, the factor modulating nitric oxide-induced smooth muscle relaxation, have also been reported in the pulmonary hypertensive fetal sheep(11).
To the extent that the fetal sheep model reflects the changes occurring in the PPHN syndrome in humans, the MLCP abnormalities observed in this study, in conjunction with our previous observation of reduced actin-activated myosin MgATPase, led us to speculate that vascular remodeling and abnormal muscle relaxation play greater roles than reactive vasoconstriction in the pathogenesis of this syndrome. The smooth muscle cells that comprised the excessive muscularization described on lung histology could have a defective contractile apparatus allowing some contraction albeit less than observed in normal pulmonary vascular smooth muscle. But its ability to relax is severely impaired on the basis of reduced activity and content of the MLCP, among other factors discussed above. Thus, the maintenance of a high pulmonary vascular resistance in infants with the PPHN syndrome would be the result of a reduced ability to vasorelax, rather than excessive vasoconstriction. In addition, the reduced potential for vasodilation of the pulmonary arterial circulation is rather intrinsic to the smooth muscle and related to abnormalities in the cross-bridge dephosphorylation and perhaps to a lesser extent the result of alterations in mediators of vasorelaxation.
In summary, we observed significant changes in the activity and concentration of the enzyme responsible for smooth muscle relaxation in pulmonary vascular tissue in the fetal sheep with ductus arteriosus-ligated pulmonary hypertension. This finding corroborates our previous report of significant relaxation abnormalities in the pulmonary vascular muscle of this model of PPHN, suggesting that the maintenance of a high pulmonary vascular resistance postnatally in the syndrome is related to impaired vasodilation.
Abbreviations
- PPHN:
-
persistent pulmonary hypertension syndrome of newborn
- MLCK:
-
myosin light chain kinase
- MLCP:
-
myosin light chain phosphatase
- HMM:
-
heavy meromyosin
- PP1:
-
PP2, protein phosphatase types 1 and 2
- PP1M:
-
myosin protein phosphatase
- SMP:
-
smooth muscle phosphatase
References
Walsh-Sukis MC 1993 Persistent pulmonary hypertension of the newborn. The black box revisited. Clin Perinatol 20: 127–143
Roberts JD, Polaner DM, Lang P, Zapol WM 1992 Inhaled nitric oxide in persistent pulmonary hypertension of the newborn. Lancet 340: 818–819
Kinsella JP, Neish SR, Ivy DD, Shaffer E, Abman SH 1993 Clinical responses to prolonged treatment of persistent pulmonary hypertension of the newborn with low dose of inhaled nitric oxide. J Pediatr 123: 103–108
Kinsella JP, Abman SH 1995 Recent developments in the pathophysiology and treatment of persistent pulmonary hypertension of the newborn. J Pediatr 126: 853–864
Levin DL, Mills LJ, Parkey M, Garriott J, Campbell W 1979 Constriction of the fetal ductus arteriosus after administration of indomethacin to the pregnant ewe. J Pediatr 94: 647–650
Abman SH, Shanley PF, Accurso FJ 1989 Failure of postnatal adaptation of the pulmonary circulation after chronic intrauterine pulmonary hypertension in fetal lambs. J Clin Invest 83: 1849–1858
Morin FC, Egan EA 1989 The effect of closing the ductus arteriosus on the pulmonary circulation of the fetal sheep. J Dev Physiol 11: 283–284
Belik J, Halayko AJ, Rao K, Stephen N 1993 Fetal ductus arteriosus ligation. Circ Res 72: 588–596
McQueston JA, Kinsella JP, Ivy DD, McMurtry IF, Abman SH 1995 Chronic pulmonary hypertension in utero impairs endothelium-dependent vasodilation. Am J Physiol 268:H288–H294
Ivy DD, Ziegler JW, Dubus MF, Fox JJ, Kinsella JP, Abman SH 1996 Chronic intrauterine pulmonary hypertension alters endothelin receptor activity in the ovine fetal lung. Pediatr Res 39: 435–442
Steinhorn RH, Russell JA, Morin FC 3 1995 Disruption of cGMP production in pulmonary arteries isolated from fetal lambs with pulmonary hypertension. Am J Physiol 268:H1483–H1489
Belik J, Keeley FW, Baldwin F, Rabinovitch M 1994 Pulmonary hypertension and vascular remodelling in fetal sheep. Am J Physiol 266:H2303–H2309
Bradford M 1976 A rapid and sensitive method for the quantification of microgram quantities of protein utilizing the principles of dye bindings. Anal Biochem 72: 248–254
Pato MD, Lye SJ, Kerc E 1991 Purification and characterization of pregnant sheep myometrium myosin light chain kinase. Arch Biochem Biophys 287: 24–32
Tulloch AG, Pato MD 1991 Turkey gizzard SMP-III is a novel protein phosphatase. J Biol Chem 266: 20168–20174
Towbin HS, Gordon J 1979 Electrophoretic transfer of proteins from polyacrylamide gels to nitrocellulose sheets: procedure and some applications. Proc Natl Acad Sci USA 76: 4350–4354
Walsh MP 1994 Regulation of vascular smooth muscle tone. Can J Physiol Pharmacol 72: 919–936
Pato MD, Tulloch AG, Walsh MP, Kerc E 1994 Smooth muscle phosphatase: structure, regulation and function. Can J Physiol Pharmacol 72: 1427–1433
Pato MD, Kerc E 1990 Comparison of the properties of the protein phosphatases from avian and mammalian smooth muscles: purification and characterization of rabbit uterine smooth muscle phosphatases. Arch Biochem Biophys 276: 116–124
Alessi D, MacDougall LK, Sola MM, Ikebe M, Cohen P 1992 The control of protein phosphatase 1 by targeting subunit. The major myosin phosphatase in avian smooth muscle is a novel form of protein phosphatase 1. Eur J Biochem 210: 1023–1035
Okubo S, Ito M, Takashiba Y, Ichikawa Miyahara M, Shimuzu H, Konishi T, Shima H, Nagao M, Hartshorne D J, Nakano T 1994 A regulatory subunit of smooth muscle myosin bound phosphatase. Biochem Biophys Res Commun 200: 429–434
Hoar PE, Pato MD, Kerrick GL 1985 Myosin light chain phosphatase. Effect on the activation and relaxation of gizzard smooth muscle skinned fibers. J Biol Chem 260: 8760–8764
Sward K, Pato MD, Nilsson B, Nordstram I, Helstrand P 1995 Polyamines inhibit myosin phosphatase and increase LC20 phosphorylation and force in smooth muscle. Am J Physiol 269:C563–C571
Bialojan C, Merkel L, Ruegg JC, Gifford D, Di Salvo J 1985 Prolonged relaxation of detergent skinned smooth muscle involves decreased endogenous phosphatase activity. Proc Soc Exp Biol Med 178: 648–52
Haeberle JR, Hathaway DR, De Paoli-Roach AA 1985 Dephosphorylation of myosin by the catalytic subunit of a type 2 phosphatase produces relaxation of a chemically skinned uterine smooth muscle. J Biol Chem 260: 9965–9968
Bialojan C, Ruegg JC, Di Salvo J 1985 Phosphatase-mediated modulation of actinmyosin interaction in bovine aortic actomyosin and skinned porcine carotid artery. Proc Soc Exp Biol Med 178: 36–45
Smith PG, Tokui T, Ikebe M 1995 Mechanical strain increases contractile enzyme activity in cultured airway smooth muscle cells. Am J Physiol 268:L999–L1005
Vescovo G, Scannapieco G, Spano E, Calliari I, Leprotti C, Serafini F, Ambrosio GB, Dalla Libera L 1996 Myosin light chain kinase in vascular smooth muscle: an immunohistochemical study in normotensive and spontaneously hypertensive rats. Basic Appl Myol 6: 183–187
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Belik, J., Majumdar, R., Fabris, V. et al. Myosin Light Chain Phosphatase and Kinase Abnormalities in Fetal Sheep Pulmonary Hypertension. Pediatr Res 43, 57–61 (1998). https://doi.org/10.1203/00006450-199801000-00009
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/00006450-199801000-00009
This article is cited by
-
T18/S19 diphosphorylation of myosin regulatory light chain impairs pulmonary artery relaxation in monocrotaline-induced pulmonary hypertensive rats
Pflügers Archiv - European Journal of Physiology (2023)