Abstract
We have previously shown that milk sensitization aggravates intestinal dysfunction in the malnourished guinea pigs, suggesting that it may also impair the recovery from malnutrition. To test this hypothesis, the growing guinea pigs were malnourished by feeding only maize for 7 d and then were refed for 21 d with a balanced diet containing either intact or hydrolyzed cow's milk proteins. The control animals received the hydrolyzed milk protein diet for 28 d. After an initial period of total inhibition of growth owing to maize, guinea pigs gained weight regularly, with both balanced diets, and there was no evidence of mucosal damage at the end of the refeeding period. However, refeeding with intact milk proteins induced milk sensitization, which was demonstrated on the systemic level by the presence of anti-β-lactoglubulin IgG1 antibodies, and on the local level by the intestinal anaphylaxis measured by the increase in short circuit current induced by β-lactoglobulin (16.4 ± 2.6 µA/cm2) in jejunal segments mounted in Ussing chambers. Such an immune sensitization was associated with impaired intestinal permeability, as both the ionic conductance (21.0 ± 1.6 versus 14.6 ± 0.7 mS/cm2) and the transepithelial fluxes of horseradish peroxidase (537 ± 203 versus 152 ± 28 ng/h·cm2) were significantly increased in guinea pigs refed with the intact milk proteins compared with controls. In contrast, there was no difference in intestinal permeability between controls and guinea pigs refed with the hydrolyzed milk protein diet. These data show that sensitization to cow's milk proteins can develop in guinea pigs recovering from severe malnutrition and may impair full intestinal repair.
Similar content being viewed by others
Main
In children with cow's milk allergy, gastrointestinal symptoms are often associated with failure to thrive (1). On the other hand, malnutrition may trigger immune sensitization to dietary proteins by altering protein hydrolysis (2), by inducing a deficiency in the mucosal secretory IgA (3), and by enhancing the permeability to macromolecules (4). This increased antigenic load could stimulate the mucosal immune system and increase the risk of persistent diarrhea in malnourished children. Although the hypothesis of a positive link between malnutrition and food allergy has frequently been raised, the conclusive clinical and experimental evidence is still lacking (5,6).
The incidence of cow's milk allergy in infancy, estimated to 2-3% in Western industrialized countries (7), is unknown in poorer areas in the world. Clinical reports have suggested that atopic cutaneous manifestations of food allergy are infrequent in malnourished children (8,9), but, on the other hand, cow's milk sensitive enteropathy has been described in the countries where child malnutrition is prevalent (10–13). Two major immune mechanisms are involved in cow's milk allergy with gastrointestinal symptoms: an IgE-dependent mechanism leading to the immediate symptoms and the intestinal anaphylaxis, and a T cell-dependent mechanism with delayed reactions leading to enteropathy (14). Both mechanisms are likely to appear in malnourished children since an IgE-dependent mechanism has been described in children infected with the parasite Trichuris trichiura (15), and T cell-mediated damage has been reported in children suffering from persistent diarrhea (16). It is conceivable that malnutrition is compatible with gastrointestinal, but not cutaneous, manifestations of food allergy.
Cow's milk-based diets are now widely used in the treatment of severe malnutrition (17,18). Therefore, the possibility of developing milk sensitization during refeeding with milk deserves attention. In fact, a multicenter study has recently shown that up to 40% of malnourished children with persistent diarrhea do not respond favorably to the milk-based diets (19). The pathophysiologic events underlying such treatment failures are unknown, but they may involve cow's milk protein allergy. Indeed, we previously reported that malnutrition in guinea pigs was compatible with the sensitization to milk proteins (20). In the present study, by using the guinea pig model of the immediate intestinal hypersensitivity to cow's milk proteins (21) combined with a model of malnutrition induced by a cereal-based diet, we have tested the hypothesis that cow's milk allergy can develop during the recovery from severe malnutrition and can interfere with intestinal repair.
METHODS
Animals and Diets
Young male Dunkin-Hartley guinea pigs weighing 200-250 g (Charles River, Saint-Aubin les Elboeuf, France) were submitted to different dietary protocols (Fig. 1). All experimental diets (two balanced diets and three deficient diets) were purchased from INRA/APAE (Jouy en Josas, France) and given ad libitum. Table 1 gives the composition of these diets based on maize as a source of digestible carbohydrates. In the two balanced diets, to fulfill the known nutritional requirements of the guinea pig (22), maize was supplemented with proteins of high nutritional value (20% cow's milk proteins, CMP), fibers (10%), lipids (2.5%), minerals (6.5%), and vitamins (1%). The first balanced diet contained 20% hydrolyzed CMP consisting of casein hydrolysate. The second one contained 16% hydrolyzed CMP and 4% intact CMP composed of whey proteins naturally rich in β-lactoglobulin (β-Lg). The three deficient diets contained one of the following: 100% maize or 96% maize plus 4% intact CMP, or 96% maize plus 4% hydrolyzed CMP. During the first week of the study, the animals were assigned to one of two dietary regimens: the balanced diet containing 20% hydrolyzed CMP to obtain well nourished controls or the deficient diet containing 100% maize to induce malnutrition. During the next 3 wk, the animals were divided into six dietary groups. The well nourished guinea pigs were divided into two control groups: the first group received the balanced diet containing hydrolyzed CMP (group CH, n = 8), and the second group received the balanced diet containing intact CMP (group CI, n = 7). The malnourished guinea pigs were divided into four dietary groups: two groups remained malnourished on a deficient diet containing intact CMP (group MI, n = 14) or casein hydrolysate (group MH, n = 17), and the last two groups were refed with a balanced diet containing intact CMP (group RI, n = 9) or casein hydrolysate (group RH, n = 9).
General dietary protocol; the different diets are detailed in Table 1. During the first week of the study, the animals were assigned to one of two dietary regimens: the balanced diet containing 20% hydrolyzed CMP to obtain well nourished controls or the deficient diet containing 100% maize to induce malnutrition. Then, the animals were divided into six dietary groups during the next 3 wk. The well nourished guinea pigs were divided into two control groups: the first group received the balanced diet containing hydrolyzed CMP (control/hydrolyzed CMP, group CH), and the second group received the balanced diet containing intact CMP (control/intact CMP, group CI). The malnourished guinea pigs were divided into four dietary groups: two groups remained malnourished with a deficient diet containing either intact CMP (malnourished/intact CMP, group MI) or casein hydrolysate (malnourished/hydrolyzed CMP, group MH), and the last two groups were refed with a balanced diet containing either intact CMP (refed/intact CMP, group RI) or casein hydrolysate (refed/hydrolyzed CMP, group RH).
Experimental Design
Three days before sacrifice, the animals were shifted to the casein hydrolysate-based diet to keep the intestine free of allergic reactions until the anaphylactic responses were tested in vitro. After the 28-d dietary protocol, the guinea pigs were anaesthetized i.p. with 90 mg/kg sodium pentobarbital. The blood was obtained by cardiac puncture, and the plasma samples were stored at -80°C. The entire small intestine was removed up to the caecum, starting 30 cm from the pylorus and, to remove the intestinal content, was carefully rinsed with cold Ringer's solution containing 140 mM Na+, 5.2 mM K+, 120 mM Cl-, 25 mM HCO3-, 1.2 mM Ca2+, 2.4 mM HPO42-, 0.4 mM H2PO4-, 1.2 mM Mg2+, and 2 mM glutamine. Twenty cm of jejunum were stripped of the outer muscular layer and mounted in Ussing chambers. Unstripped segments were used for histologic examination.
Immune Sensitization to β-Lg
Systemic antibody response to β-Lg. In guinea pigs, anaphylactic antibodies essentially belong to the IgG1 subclass. Therefore, milk sensitization was assessed at the systemic level by measuring plasma anti-β-Lg IgG1 antibodies. We used a modified ELISA originally described by Kawabata et al, (23). Briefly, 100-µL plasma samples were serially diluted (1:4 to 1:65536) in PBS-Tween (0.05% Tween 20 in 0.01 M PBS) and kept for 90 min at room temperature in the microtiter plates (Maxisorp, Nunc) previously coated overnight at 4°C with β-Lg (100 µL of 0.1 mg/mL β-Lg in 0.01 M PBS, pH 7.2). Then, they were saturated with gelatin at 37°C for 90 min (1% in 0.01 M PBS). Finally, the IgG1 were detected with a goat anti-guinea pig IgG1 peroxidase conjugate (1:7500; Tebu) revealed by H2O2 and orthophenylene diamine. Between each step, except after gelatine, plates were washed four times with PBS-Tween. Positive titers were denoted as the last dilution giving an OD at least two times higher than that of the background.
Intestinal anaphylaxis. The local intestinal immune response was assessed in vitro in the jejunal segments mounted in Ussing chambers by recording the maximal rise in short circuit current (Isc) induced by serosal or mucosal addition of 0.4 mg/mL β-Lg:ΔIscβ-Lg. Intestinal tissues from the milk-sensitized guinea pigs generally respond to antigen challenge by a type I hypersensitivity reaction termed intestinal anaphylaxis. The latter is associated with fluid secretion and is characterized by a rapid rise in Isc owing to the net chloride secretion in the colon (21). Data from various experimental models of intestinal anaphylaxis, including the present one (24), indicate that such an electrogenic activity (rise in Isc) is induced by the degranulation of mucosal mast cells leading to the subsequent release of inflammatory mediators capable of stimulating chloride secretion (25).
Morphologic Analysis of Intestinal Mucosa
One-cm jejunal segment from each animal was fixed in 10% formaldehyde, dehydrated, embedded in paraffin, cut in 4-µm sections, and stained with hematoxylin, eosin, and safranin for morphologic analysis and with Giemsa for mast cells counting. Coded sections were evaluated in a blind manner by one observer, and two separate measurements were performed for each sample. A micrometer was used to measure the total mucosal height and crypt depth/villus height ratio (C/V ratio). Mucosal mast cells were counted on a defined mucosal length. In a first series of measurements, all metachromatic cells were counted to obtain the total number of mast cells. Mast cell counts were expressed per millimeter of muscularis mucosae, as this parameter is not highly affected by malnutrition (26). In a second series of measurements, only intensively stained mast cells were counted and considered as granulated mast cells. The percentage of degranulated mast cells was then calculated.
Intestinal Function in Ussing Chambers
Eight adjacent jejunal segments from each animal were placed on 8-µm filters and mounted as flat sheets in Ussing chambers with an exposed area of 0.5 cm2. The filters, as well as the mucosal and serosal compartments, were previously coated for 1 h with gelatin (1% in 0.9% NaCl) to prevent adsorption. Intestinal segments were bathed on both sides with 12 mL of Ringer's solution, which was continuously thermostated, circulated, oxygenated, and maintained at pH 7.4 with carbogen (5% CO2, 95% O2). The mucosal and serosal bathing solutions were connected via agar bridges to the calomel electrodes for measurement of the transepithelial potential difference and to the Ag-AgCl electrodes for applying the current. The tissue was kept under short circuit conditions by an automatic clamping device (World Precision Instruments, Aston, England) that canceled out the fluid resistance. The short circuit current (Isc) was constantly recorded, and the tissue was pulsed at 0.5 mV every 30 s. The Isc deflection was used to calculate the ionic conductance (G) according to Ohm's law.
Absorption and secretion. In the intestine, water movements often follow ionic movements, i.e. Na+ absorption and Cl- secretion. Intestinal absorption was assessed by the cotransport glucose-Na+ measured by the increase in Isc induced by glucose (10 mM, serosal and mucosal). Intestinal secretion was assessed by the increase in Isc induced by the mast cell mediator, 5-hydroxytryptamine (5-HT, 100 µM, serosal). This secretagogue was chosen because, among the inflammatory mediators that are involved in intestinal anaphylaxis, 5-HT is believed to play a major role in the β-Lg-induced electrogenic response in the small intestine of the milk-sensitized guinea pigs (27).
Intestinal permeability. Potential difference (PD), Isc, and G, an index of paracellular permeability, were measured 30 min after tissue equilibration. Transepithelial permeability to macromolecules (endocytotic transport) was assessed by measuring the mucosal to serosal fluxes of horseradish peroxidase (HRP) in the jejunal segments mounted in Ussing chambers. After 30 min of equilibration, HRP (type II, Sigma) was added on the mucosal side at the final concentration of 0.4 mg/mL. Its appearance on the serosal side was monitored by sampling aliquots at 10, 50, 90, and 130 min with buffer replacement and measuring the enzymatic activity of peroxidase in 200-µL serosal samples, as previously described (28). HRP fluxes (ng/h·cm2) are given at steady state as the mean of the fluxes at 90 and 130 min.
Statistical Analysis
Data were analyzed using the SAS package (SAS Institute, Cary, NC). Analysis of variance was performed according to the general linear model procedure and was used to compare means and ranges. Results are means ± SE, with n as the number of animals. Mortality data were analyzed by the Chisquare test.
RESULTS
Clinical and Nutritional Data
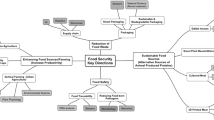
Figure 2 shows the body weight of guinea pigs during the feeding protocol in the six dietary groups. The control guinea pigs (CH and CI) gained weight regularly throughout the study. Their mean body weight was significantly greater than that of malnourished or refed guinea pigs in every study period.
Evolution of the body weight in guinea pigs of the six dietary groups. Each point represents mean ± SE, n = 7-9 guinea pigs. The arrow indicates that guinea pigs were divided into six groups (see Fig. 1). Comparison before day 7: *, significantly different from the well nourished animals (p < 0.01). Comparison after day 7: **, significantly different from the control groups CH or CI (p < 0.01); †, significantly different from the refed groups RH or RI (p < 0.01).
There was a high degree of mortality among the guinea pigs receiving a deficient diet for 28 d. In fact, 10 of 17 animals in the MH group and seven of 14 animals in the MI group died during the feeding protocol. Those animals were not included in analysis. Mortality was not significantly different between these two groups of malnourished guinea pigs but was significantly higher (p < 0.01) than that observed in the four other groups, where no death occurred. The malnourished guinea pigs experienced a severe weight loss. At the end of the study, their body weight was below their initial weight and 2.5 times lower than that of the controls. Most of the guinea pigs from the MH group and all the guinea pigs from the MI group had a liquid yellowish small intestinal content, suggestive of bile acid malabsorption, and developed irritation of the perianal skin and diarrhea often associated with blood loss.
In the two groups of refed guinea pigs (RH and RI), refeeding allowed the recovery of weight gain after a period of latency of 3-4 d. After 10 d of refeeding, their mean body weight became significantly greater than that of the malnourished guinea pigs but up to the end of the study remained significantly lower than that of controls. These differences in body weight between the control, malnourished, and refed guinea pigs were not associated with differences in plasma protein level, which was similar in the six dietary groups (data not shown). Similarly, no significant difference in body weight was noticed between CH and CI, MH and MI, or RH and RI groups, suggesting that the nature of the CMP in the diet, i.e. intact or hydrolyzed, had no impact on growth.
Immune Responses to β-Lactoglobulin
Systemic sensitization. As shown in Figure 3, anti-β-Lg IgG1 antibodies developed in all the animals receiving intact CMP (CI, MI, and RI groups). Such an immune sensitization was not affected by malnutrition (no difference in anti-β-Lg IgG1 titers between MI and CI was found) and was diminished by refeeding (significantly lower titers in RI than in CI). In contrast, no positive titers were detected in guinea pigs from CH, MH, and RH groups (data not shown), indicating that guinea pigs fed hydrolyzed CMP did not developed immune sensitization. This confirms the hypoallergenic properties of these hydrolysates in the guinea pig (29).
Intestinal anaphylaxis. In the guinea pigs fed intact CMP, milk sensitization was demonstrated at the intestinal level by the in vitro response to β-Lg, i.e. an increase in Isc (ΔIsc) after addition of β-Lg on jejunal segments mounted in Ussing chambers. As shown in Figure 3, the response was lower when β-Lg was added in the mucosal (ΔIscβ-Lgm) than in the serosal (ΔIscβ-Lg) side of the jejunal segment, although the protein concentration was the same. This can be explained by the fact that only a minute quantity of the mucosal antigen is transported across the epithelial layer and can activate the mucosal mast cells. As in systemic sensitization, intestinal anaphylaxis was not affected by malnutrition (no difference in ΔIscβ-Lgm or ΔIscβ-Lgs between MI and CI) but was decreased by refeeding (ΔIscβ-Lgm and ΔIscβ-Lgs significantly lower in RI than in CI).
Histologic Examination of the Intestinal Mucosa
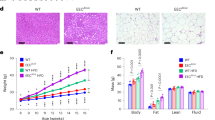
Mucosal morphology. The histologic analysis failed to reveal any important difference between the jejunal fragments from the four groups of control or refed guinea pigs (CH, CI, RH, and RI). In particular, there was no difference in intestinal morphometry (Fig. 4) or in lamina propria cellularity, between the sensitized (CI) and nonsensitized (CH) controls, confirming that milk sensitization does not induce important mucosal damage in the present animal model (30). However, minor alterations were sometimes observed in sensitized animals, such as subnuclear vacuolization and edema, leading to the separation of the epithelial cell layer from the basal membrane, as previously shown in rats sensitized to ovalbumin (31). The jejunum from the malnourished (MH and MI) animals showed a significant decrease in the total mucosal height and an increase in crypt-villus ratio compared with those of control guinea pigs (CH or CI) (Fig. 4). This mucosal damage was characterized by a villus atrophy without crypt hyperplasia and was often associated with an inflammatory infiltrate. In the MH group, some specimens (four of seven) showed an almost normal cellularity in the lamina propria, whereas a dense infiltration of lymphocytes, plasmocytes, polymorphonuclear neutrophils, and histiocytes was observed in the lamina propria of the three other specimens. In the MI group, all the specimens (n = 10) showed such a dense intersticial population, typical of mucosal inflammation. Thus, mucosal inflammation was of variable severity in malnourished guinea pigs fed hydrolysates (MH) but was systematically observed in malnourished guinea pigs fed intact milk proteins (MI).
Mast cell counts. As shown in Table 2, the number of mast cells was similar in the control guinea pigs fed hydrolyzed (CH) or intact (CI) CMP, suggesting that milk sensitization had no influence on this parameter. This was further confirmed in the malnourished (MI versus MH) and refed (RI versus RH) groups. This lack of impact of immune sensitization on mucosal mast cell number in the basal state is in accordance with the previous data obtained in rats sensitized to ovalbumin (32). We did not observe any significant difference in the percentage of degranulated mast cells between sensitized and nonsensitized guinea pigs. This is concordant with other experimental models of intestinal anaphylaxis, where a decrease in the number of granulated mucosal mast cells in found only after antigen challenge (31). Interestingly, a lower mast cell count was found in the jejunum of the malnourished than of the control guinea pigs, suggesting that malnutrition was responsible for a decrease in total mucosal mast cell. In both groups of refed guinea pigs, the total number of mucosal mast cells was also decreased.
Intestinal Function
Absorption and secretion. There was no significant difference in basal PD or Isc between the six dietary groups. Figure 5 shows that chloride secretion in response to 5-HT and sodium absorption after addition of glucose were similar in both control groups, sensitized or not, suggesting that milk sensitization by itself had no impact on ionic transport. In contrast, stimulated absorption and secretion were significantly increased in both groups of malnourished guinea pigs compared with controls. In addition, the malnutrition-induced increase in Na+-glucose cotransport was further increased when malnutrition was combined with milk sensitization (p = 0.03), but the pathophysiologic significance of this finding is unknown. In refed guinea pigs, ionic absorption and secretion were not different from the control values.
Intestinal permeability. Figure 6 shows the basal ionic conductance G and HRP fluxes in the six dietary groups. G was similar in both control groups (CH and CI), suggesting that milk sensitization by itself had no impact on the paracellular permeability. In contrast, G was significantly increased in both groups of malnourished guinea pigs (MH and MI), suggesting that malnutrition per se induced a defect in the paracellular barrier function. This increase in G was also observed in the guinea pigs refed with intact CMP (RI) but not in the guinea pigs refed with hydrolyzed CMP (RH). The HRP fluxes were similar in CH, MH, and RH guinea pigs, showing that neither malnutrition by itself (MH) nor refeeding (RH) was responsible for alteration of the intestinal barrier to macromolecules. In contrast, the HRP fluxes were high in all the groups of guinea pigs consuming intact CMP irrespective of their nutritional status, the difference between the control groups (CH versus CI) reaching statistical significance. Moreover, when the guinea pigs consuming intact CMP were globally compared with those consuming hydrolysates, a significant difference was found in the HRP fluxes (p = 0.011), suggesting that the increase in the macromolecular permeability is a direct consequence of milk sensitization.
Indexes of the intestinal barrier capacity (ionic conductance and mucosal to serosal fluxes of horseradish peroxidase) measured in jejunal segments of guinea pigs from the six dietary groups. Results are means ± SE, n = 7-9 animals. *, significantly different from the CH group (p < 0.05).†, significantly different from the RH group (p < 0.01).
DISCUSSION
The present results confirm that malnourished guinea pigs can be orally sensitized to cow's milk proteins (CMP) (20) and indicate that such an immune sensitization can also develop during the phase of recovery from malnutrition, although it was diminished in refed compared with well nourished controls. Furthermore, they demonstrate that the malnourished guinea pigs refed with intact, but not with hydrolyzed, CMP present a persistent alteration of the intestinal epithelial barrier. This indicates that the development of milk sensitization during refeeding may impair full intestinal repair.
It is now recognized that malnutrition in children cannot be considered solely a deficiency in proteins and/or in energy. In fact, it also involves the multiple mineral and vitamin deficiencies owing to the consumption of cereal-based diets (18,33). The low dietary quality, particularly the suboptimal micronutrient density, of the cereal-based diets currently used as weaning diets in poor areas of the world may explain the high prevalence of child malnutrition in those areas (33). To simulate this situation, we induced malnutrition in guinea pigs by feeding them maize (100% maize for 1 wk then 96% maize + 4% CMP for 3 wk). As expected, maize induced a severe malnutrition with a total growth inhibition. This was not the result of the maize toxicity per se, as the balanced diets used in the present study induced an optimal growth despite their high maize content (60%). Interestingly, the addition, after 7 d of malnutrition, of 4% CMP, considered proteins of high biologic value, did not allow the weight gain, indicating that the impairment of growth rate owing to maize involves not only the poor quality and quantity of proteins but also deficiencies in essential micronutrients, such as calcium, vitamin A, iron, and zinc. In this study, although the small intestinal mucosa of the maize-fed guinea pigs was generally well preserved, it was thinner than that of the controls. This finding is in accordance with the morphologic alterations described in animals fed a low protein diet (26,34) or submitted to food restriction (35), as well as in marasmic children (36). As it has been described in other models of experimental malnutrition, we have confirmed that malnutrition is accompanied by intestinal dysfunction, attested by the increase in the Na+-glucose cotransport (37,38) and in the intestinal ionic conductance (39,40) and the exacerbation of chloride secretion in response to inflammatory mediators (41). However, in our model, the impact of malnutrition on the clinical state of the animals was more severe than in other experimental models of malnutrition. In fact, in contrast to the reports of protein deprivation (34) or dietary restriction (35), but in accordance with the reports of child malnutrition (42), the present polydeficient malnutrition induced a high mortality and diarrhea often associated with mucosal inflammation and blood loss.
Our previous finding that intestinal anaphylaxis to CMP was increased by malnutrition in guinea pigs supported the hypothesis of a positive link between malnutrition, intestinal dysfunction, and protein sensitization (20). In this previous study, the guinea pigs received a protein-deficient diet containing intact CMP, which induced simultaneously malnutrition and sensitization. This implied that their nutritional and immune status was intact at the first contact with antigen and that nutrients which play a crucial role in immunity, such as minerals, vitamins, and essential fatty acids, were provided to guinea pigs in an adequate amount during the whole experiment. This might explain their capacity to develop sensitization during malnutrition. Indeed, earlier analysis suggested that the immune status of malnourished children was not compatible with the development of food allergy (8,9). The present results confirm that sensitization to intact CMP is possible during malnutrition, even when animals are deprived of essential micronutrients before and during the sensitization process, because both reaginic IgG1 and anaphylactic intestinal responses are obtained in maize-fed (MI) guinea pigs, although to a lower extent than in well nourished controls. Indeed, in contrast with our previous results obtained with the protein-deficient guinea pigs (20), in the present study using the maize-fed guinea pigs, the milk protein sensitization was lower in the malnourished compared with the control animals. In fact, the total mucosal mast count was lower in malnourished maize-fed guinea pigs, which is in agreement with the data reported in protein-deficient rats (26) and gerbils (43). Despite a lower count of mast cells in malnourished (MI) than in control guinea pigs, the intestinal anaphylaxis was similar in both groups, suggesting that the increase in the secretory response observed in malnutrition had counterbalanced the decrease in the mast cell number.
It is noticeable that intestinal inflammation was more frequent and more pronounced in the malnourished animals receiving intact milk proteins than in those receiving hydrolysates. Moreover, in the malnourished guinea pigs receiving intact milk proteins (MI), both paracellular permeability (G) and the permeability to HRP were increased, whereas only G was increased in the malnourished animals receiving hydrolysates (MH). These results confirm that it is not malnutrition per se that increases the macromolecular permeability (20,44). They rather suggest that this effect is the result of the sensitization and the activation of mucosal immune cells. Indeed, human malnutrition is frequently complicated with enteral infections activating the mucosal immune system and is often associated with intestinal inflammation (16,36), which might be the factor responsible for the increased intestinal permeability to proteins we (4) and others (45) previously found in malnourished patients. The present data suggest that during malnutrition, food protein sensitization could be, like infection, an activating factor of the mucosal immune system, worsening intestinal dysfunction.
Whatever the type of CMP-intact or hydrolyzed-used in the refeeding diet, a rapid recovery in weight gain was observed in the maize-fed guinea pigs. However, a complete catch-up growth was not obtained after 3 wk of refeeding. There was no difference in the mucosal morphometry between control (CH or CI) and refed (RH or RI) guinea pigs, suggesting that 3 wk of refeeding were sufficient to normalize most of the morphologic alterations induced by malnutrition. An important finding of the present study is that severely malnourished animals refed with intact CMP developed cow's milk sensitization. However, the reaginic IgG1 titers and the anaphylaxic response in this group were lower than in the control or malnourished guinea pigs. The lower sensitization to CMP in refed animals could be related to the fact that refeeding can counteract the malnutrition-induced hypersecretion in response to 5-HT but cannot restore the mucosal mast cell number, the latter remaining low after refeeding. Sensitization to CMP was not responsible per se for growth retardation, as the weight gain was similar in RH and RI guinea pigs, and did not alter the normalization of glucose-Na+ cotransport and the 5-HT-stimulated Cl- secretion. Nevertheless, the present study shows that the intestinal epithelial barrier cannot be fully repaired when intact CMP are present in the refeeding diet. This is in agreement with a previous report of Boza et al. (46) in starved rats. In the present study, the ionic conductance and the HRP fluxes were as high in the guinea pigs refed with intact CMP (RI) as in the sensitized guinea pigs that had been malnourished for 4 wk (MI). Considering that the increase in HRP permeability is the result of sensitization (47–49) and that the increase in ionic conductance G is because of malnutrition (20,39,40), we suggest that the development of milk sensitization during refeeding has a double impact on intestinal permeability: it increases the macromolecular permeability and inhibits the normalization of the paracellular permeability. Thus, in this model of allergic-prone guinea pigs, refeeding with hydrolyzed CMP has a double advantage: first, it allows a total restoration of the paracellular barrier capacity; second, it avoids an increase in the macromolecular permeability owing to the sensitization to CMP.
The relevance of the present findings to child malnutrition and refeeding is unknown. The impact of milk sensitization on the repair of the intestinal barrier in the malnourished guinea pigs is reminiscent of the difficulty to improve the epithelial barrier in children recovering from severe malnutrition and diarrhea (4,50). This may have an impact on the long-term efficacy of dietary treatments as a defect in intestinal barrier may be predictive of poor growth performance (51). The present experimental results indicate that refeeding of the individuals susceptible to milk sensitization with intact CMP may impair the recovery from malnutrition by inhibiting full restoration of the intestinal barrier. This might explain why some malnourished children are unable to recover from malnutrition while kept on cow's milk-based diets and must be treated by the empirical removal of cow's milk proteins (19,52). The present results suggest, therefore, that immune sensitization to CMP might be involved in some of the treatment failures observed with cow's milk-based diets and that the use of milk hydrolysates may present some advantages in such cases.
Abbreviations
- β-Lg:
-
β-lactoglobulin
- CH:
-
well nourished controls receiving hydrolyzed cow's milk proteins
- CI:
-
well nourished controls receiving intact cow's milk proteins
- CMP:
-
cow's milk proteins
- G:
-
ionic conductance
- HRP:
-
horseradish peroxidase
- Isc:
-
short circuit current
- MH:
-
malnourished receiving hydrolyzed cow's milk proteins
- MI:
-
malnourished receiving intact cow's milk proteins
- RH:
-
malnourished refed with a balanced diet containing hydrolyzed cow's milk proteins
- RI:
-
malnourished refed with a balanced diet containing intact cow's milk proteins
- 5-HT:
-
5-hydroxytryptamine
References
Savilahti E, Verkasalo M 1984 Intestinal cow's milk allergy: pathogenesis and clinical presentation. Clin Rev Allergy 2: 7–23
Barbezat GO, Hansen JDL 1968 The exocrine pancreas and calorie-protein malnutrition. Pediatrics 42: 77–92
Green F, Heyworth B 1980 Immunoglobulin-containing cells in jejunal mucosa of children with protein-energy malnutrition and gastroenterits. Arch Dis Child 55: 380–383
Heyman M, Boudraa G, Sarrut S, Giraud M, Evans L, Touhami M, Desjeux JF 1984 Macromolecular transport in jejunal mucosa of children with severe malnutrition: a quantitative study. J Pediatr Gastroenterol Nutr 3: 357–363
Brewster DR, Manary MJ, Menzies IS, Henry RL, O'Loughlin EV 1997 Comparison of milk and maize based diets in kwashiorkor. Arch Dis Child 76: 242–248
Snyder JD 1992 Dietary protein sensitivity: is it an important risk factor for persistent diarrhea? Acta Paediatr Suppl 381: 78–81
Host A, Jacobsen HP, Halken S, Holmenlund D 1995 The natural history of cow's milk protein allergy/intolerance. Eur J Clin Nutr 49( suppl 1): S13–S18
Abbassy AS, el-Din MK, Hassan AI, Aref GH, Hammad SA, el-Araby II, el-Din AA 1974 Studies of cell-mediated immunity and allergy in protein energy malnutrition: II. immediate hypersensitivity. J Trop Med Hyg 77: 18–21
Chandra RK 1975 Food antibodies in malnutrition. Arch Dis Child 50: 532–534
Rezzonico CA, Passera ML, Bertorello HN, Kohn IJ, Torres V, Ortiz A, Polacov P 1982 Sindromes clinicos digestivos associados con alergia alimentaria, particularmente con las proteinas de la leche. Arch Arg Ped 80: 326–341
Iyngkaran N, Robinson MJ, Sumithran E, Lam SK, Puthucheary SD, Yadav M 1978 Cow's milk protein-sensitive enteropathy: an important factor in prolonging diarrhoea of acute infective enteritis in early infancy. Arch Dis Child 53: 150–153
Manuel PD, Walker-Smith JA, Soeparto P 1980 Cow's milk sensitive enteropathy in Indonesian infants letter. Lancet 2: 1365–1366
Saïdi D, Heyman M, Kheroua O, Boudraa G, Bylsma P, Kerroucha R, Chekroun A, Maragi JA, Touhami M, Desjeux JF 1995 Jejunal response to β-lactoglobulin in infants with cow's milk allergy. CR Acad Sci Paris 318: 683–689
MacDonald TT, Path MRC 1991 Pathogenesis of intestinal inflammation. In: Walker WA, Durie PR, Hamilton JR, Walker-Smith JA, Watkins JB (eds) Pediatric Gastrointestinal Disease. BC Becker Inc., Philadelphia, 574–592.
Cooper ES, Spencer J, Whyte-Alleng CA, Cromwell O, Whitney P, Venugopal S 1991 Immediate hypersensitivity in colon of children with chronic Trichuris trichiura dysentery. Lancet 338: 1104–1107
Sullivan PB, Marsh MN, Mirakian R, Hill SM, Milla PJ, Neale G 1991 Chronic diarrhea and malnutrition: histology of the small intestinal lesion. J Pediatr Gastroenterol Nutr 12: 195–203
Briend A, Golden MH 1993 Treatment of severe child malnutrition in refugee camps. Eur J Clin Nutr 47: 750–754
Golden MHN 1995 Severe malnutrition. In: Weatherall DJ, Ledingham JGG, Warell DA (eds) The Oxford Textbook of Medicine. University Press, Oxford, 1278–1296.
International Working Group on Persistent Diarrhea 1996 Evaluation of an algorithm for the treatment of persistent diarrhea: a multicentre study. Bull WHO 75: 479–489
Darmon N, Heyman M, Candalh C, Blaton MA, Desjeux JF 1996 Anaphylactic intestinal response to milk proteins during malnutrition in guinea pigs. Am J Physiol 270: G442–G448
Cuthbert AW, McLaughlan P, Coombs RRA 1983 Immediate hypersensitivity reaction to β-lactoglobulin in the epithelium lining the colon of guinea pigs fed cow's milk. Int Arch Allergy Appl Immun 72: 34–40
Navia JM, Hunt CE 1976 Nutrition, nutritional diseases, and nutrition research applications. In: Wagner JE, Manning PJ (eds) The Biology of the Guinea Pig. Academic Press, New York, 235–267.
Kawabata TT, Babcock LS, Gauggel DL, Asquith TN, Fletcher ER, Horn PA, Ratajczak HV, Graziano FM 1995 Optimization and validation of an ELISA to measure specific guinea pig IgG1 antibody as an alternative to the in vivo passive cutaneous anaphylaxis assay. Fundam Appl Toxicol 24: 238–246
Theodorou V, Fioramonti J, Junien JL, Bueno L 1994 Anaphylactic colonic hypersecretion in cow's milk sensitized guinea pigs depends upon release of interleukin-1, prostaglandins and mast cell degranulation. Aliment Pharmacol Ther 8: 301–307
Castro GA, Powell DW 1994 The physiology of the mucosal immune system and immune-mediated responses in the gastrointestinal tract. In: Johnson LR, Alpers DH, Jacobson ED, Christensen J, Walsh JH (eds) Physiology of the Gastrointestinal Tract. Raven Press, New York, 709–750.
Cummins AG, Duncombe VM, Bolin TD, Davis AE, Yong J 1987 The response of the small intestine of the protein-deficient rat to infection with Nippostrongylus brasiliensis. Int J Parasitol 17: 1445–1450
Baird AW, Coombs RR, McLaughlan P, Cuthbert AW 1984 Immediate hypersensitivity reactions to cow milk proteins in isolated epithelium from ileum of milk-drinking guinea pigs: comparisons with colonic epithelia. Int Arch Allergy Appl Immun 75: 255–263
Maehly AC, Chance B 1954 The assay of catalases and peroxidases. In: Glick D (eds) Methods of Biochemical Analysis, Vol 1. Wiley Intersciences, New York, 357–398.
Granati B, Marioni L, Rubaltelli FF 1985 Evaluation in guinea pigs of the allergenic capacity of two infant formulae based on hydrolyzed milk proteins. Biol Neonate 48: 122–124
Baron DA, Baird AW, Cuthbert AW, Margolius HS 1988 Intestinal anaphylaxis: rapid changes in mucosal ion transport and morphology. Am J Physiol 254: G307–G314
Perdue MH, Chung M, Gall DG 1984 Effect of intestinal anaphylaxis on gut function in the rat. Gastroenterology 86: 391–397
Crowe SE, Soda K, Stanisz AM, Rantala I 1993 Intestinal permeability in allergic rats: nerve involvement in antigen-induced changes. Am J Physiol 264: G617–G623
Brown KH 1991 The importance of dietary quality versus quantity for weanlings in less developed countries: a framework of discussion. Food Nutr Bull 13: 86–92
Rodrigues MA, De Camargo JL, Coelho KI, Montenegro MR, Angeleli AY, Burini RC 1985 Morphometric study of the small intestinal mucosa in young, adult, and old rats submitted to protein deficiency and rehabilitation. Gut 26: 816–821
Butzner JD, Gall DG 1990 Impact of refeeding on intestinal development and function in infant rabbits subjected to protein-energy malnutrition. Pediatr Res 27: 245–251
Brunser O 1968 Jejunal mucosa in infant malnutrition. Am J Clin Nutr 21: 976–983
Lifshitz F, Hawkins RL, Diaz-Bensussen S, Wapnir RA 1972 Absorption of carbohydrates in malnourished rats. J Nutr 102: 1303–1310
Butzner JD, Brockway PD, Meddings JB 1990 Effects of malnutrition on microvillus membrane glucose transport and physical properties. Am J Physiol 259– G940–G946
Butzner JD, Gall DG 1988 Impact of protein-calorie malnutrition on the developing intestine. Biol Neonate 54: 151–159
Rodriguez P, Darmon N, Chappuis P, Candalh C, Blaton MA, Bouchaud C, Heyman M 1996 Intestinal paracellular permeability during malnutrition in guinea pigs: effect of high dietary zinc. Gut 39: 416–422
Young A, Levin RJ 1990 Diarrhoea of famine and malnutrition: investigations using a rat model. 1 Jejunal hypersecretion induced by starvation. Gut 31: 43–53
Bhan MK 1996 The gut in malnutrition. In: Walker WA, Durie PR, Hamilton JR, Walker-Smith JA, Watkins JB (eds) Pediatric Gastrointestinal Disease. Mosby, St. Louis, 867–878.
Leitch GJ, Udezulu IA, He Q, Visvesvara GS 1993 Effects of protein malnutrition on experimental giardiasis in the Mongolian gerbil. Scand J Gastroenterol 28: 885–893
Lamont AG, Gordon M, Ferguson A 1987 Oral tolerance in protein-deprived mice. II. evidence of normal "gut processing" of ovalbumin, but suppressor cell deficiency in deprived mice. Immunology 61: 339–343
Reynolds JV, O'Farrelly C, Feighery C, Murchan P, Leonard N, Fulton G, O'Morain C, Keane FB, Tanner WA 1996 Impaired gut barrier function in malnourished patients. Br J Surg 83: 1288–1291
Boza JJ, Jimenez J, Martinez O, Suarez MD, Gil A 1994 Nutritional value and antigenicity of two milk protein hydrolysates in rats and guinea pigs. J Nutr 124: 1978–1986
Heyman M, Andriantsoa M, Crain-Denoyelle AM, Desjeux JF 1990 Effect of oral or parenteral sensitization to cow's milk on mucosal permeability in guinea pigs. Int Arch Allergy Appl Immun 92: 242–246
Heyman M, Grasset E, Ducroc R, Desjeux JF 1988 Antigen absorption by the jejunal epithelium of children with cow's milk allergy. Pediatr Res 24: 197–202
Juvonen P, Jakobsson I, Lindberg T 1990 Macromolecular absorption and cow's milk allergy. Arch Dis Child 65: 300–303
Sullivan PB, Lunn PG, Northrop-Clewes C, Crowe PT, Marsh MN, Neale G 1992 Persistent diarrhea and malnutrition: the impact of treatment on small bowel structure and permeability. J Pediatr Gastroenterol Nutr 14: 208–215
Lunn PG, Northrop-Clewes CA, Downes RM 1991 Intestinal permeability, mucosal injury, and growth faltering in Gambian infants. Lancet 338: 907–910
Bhutta ZA, Hendricks KM 1996 Nutritional management of persistent diarrhea in childhood: a perspective from the developing word. J Pediatr Gastroenterol Nutr 22: 17–37
Author information
Authors and Affiliations
Additional information
Supported by Institut National de la Santé et de la Recherche Médicale.
Rights and permissions
About this article
Cite this article
Darmon, N., Abdoul, E., Roucayrol, AM. et al. Sensitization to Cow's Milk Proteins during Refeeding of Guinea Pigs Recovering from Polydeficient Malnutrition. Pediatr Res 44, 931–938 (1998). https://doi.org/10.1203/00006450-199812000-00018
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/00006450-199812000-00018