Abstract
The renin-angiotensin system plays an important role in renal growth and development: exposure of the fetus or neonate to angiotensin-converting enzyme (ACE) inhibitors increases mortality and results in growth retardation and abnormal renal development. This study was designed to investigate the effects of ACE inhibition in the neonatal rat on the expression of genes known to modulate renal cellular proliferation, cell interactions, and extracellular matrix. Newborn rat pups were treated with enalapril (30 mg/kg/d) or vehicle for 14 d, and kidneys were removed for Northern analysis of mRNA for transforming growth factor-β1 (TGF-β1), prepro epidermal growth factor (EGF), clusterin, and renin. Distribution of TGF-β1, EGF, and clusterin was also determined by immunohistochemistry. Enalapril treatment resulted in 40% mortality by d 14, reduced body and kidney weight, decreased glomerular area, and caused tubular dilatation (p < 0.05 versus vehicle group). Enalapril decreased renal TGF-β1 and EGF mRNA expression, and increased renal clusterin and renin expression (p < 0.05). Renal tubular immunoreactive EGF was decreased, and clusterin was increased by enalapril treatment. These results indicate that ACE inhibition in the developing kidney reduces the renal expression of critical growth factors, which may account for renal growth impairment. Clusterin expression may increase either due to blockade of tonic angiotensin-mediated inhibition, or as an adaptive response to renal ischemia.
Similar content being viewed by others
Main
The renin-angiotensin system plays a central role in the regulation of vascular tone and fluid homeostasis. In addition, ANG II has been shown to stimulate growth in a variety of tissues, including the kidney(1). Compared with that in the adult, the activity of the renal renin-angiotensin system is markedly activated in early development(2). Blocking ANG II by ACE inhibition or ANG AT1 receptor inhibition in fetal life causes hypotension, growth impairment, and abnormal renal development(3, 4). These reports suggest that ANG is necessary for normal renal development.
The cellular mechanisms underlying ANG-dependent stimulation of renal development have not been elucidated. The present study was therefore designed to investigate the role of endogenous ANG II in the regulation of autocrine and paracrine compounds known to mediate cell proliferation, extracellular matrix deposition, and cell-cell and cell-matrix interactions. ANG II has been shown to induce proximal tubular cell hypertrophy through stimulation of TGF-β1(5). Alternatively, the growth response to ANG II may be mediated by conversion of TGF-β1 to its active form(6). In addition, TGF-β1 inhibits tubular cell migration(7) and stimulates deposition of extracellular matrix, although inhibiting its degradation(8). In contrast to TGF-β1, EGF stimulates renal differentiation(9). ANG II potentates the mitogenic action of EGF on proximal tubular cells(10), and inhibition of AT1 receptors decreases the renal expression of EGF in the neonatal rat(11).
Clusterin (sulfated glycoprotein-2) is a glycoprotein produced by mesenchymal cells in renal embryogenesis and by renal tubular cells in response to tubular injury(12). It appears to play a major role in promoting epithelial cell aggregation(13). Inhibition of AT1 receptors increases the renal expression of clusterin in the neonatal rat, suggesting that clusterin expression is normally suppressed by ANG II(11).
The present study was designed to determine whether inhibition of endogenous ANG II production during renal development modulates steady state levels of renal mRNA for TGF-β1, prepro EGF, and clusterin. The postnatal rat was chosen for investigation because only 10% of nephrons are present at birth in this species, with the remainder being formed by 14 d of age(14). Thus, the early postnatal period in the rat is analogous to the midgestational period in the human. In a recent report, all of the components of the renin-angiotensin system have been demonstrated in the human fetal kidney(15).
METHODS
Studies were performed on 28 neonatal Sprague-Dawley rats. Each pregnant rat was put into a separate cage and was allowed free access to regular rat chow and tap water. At birth, neonatal rats were allocated to eight individuals per litter, and the mothers suckled their newborns up to harvest. The experimental protocol was approved by the Animal Care Committee of the University of Virginia.
Beginning on d 1 of life, rats were weighed and gavage-fed a daily dose of enalapril (Sigma Chemical Co., St. Louis, MO) (30 mg/kg of body weight, dissolved in distilled water, n = 16), or vehicle (distilled water, n = 12). This dose of enalapril has been shown to block the pressor response to ANG I in rats(16). Rats were killed at 14 d of age. Kidneys were removed, decapsulated, weighed, and processed for RNA analysis.
Northern blots. Total renal RNA was extracted by a modified method of Chomczynski and Sacchi(17) using guanidium isothiocyanate. A 20-μg RNA sample was electrophoresed on denaturing 1.2% agarose-formaldehyde gel, transferred to a nylon membrane by capillary action, heated, and exposed to UV (254 nm). Northern blot membranes were hybridized, using the method of Church and Gilbert(18), with the use of a rat TGF-β1 cDNA (gift of Su Wen Qian, National Cancer Institute, Bethesda, MD), a mouse EGF cDNA (gift of Graeme I. Bell, Howard Huges Medical Institute, University of Chicago, Chicago, IL), a clusterin cDNA (gift of M. Tenniswood, University of Ottawa, Ottawa, Canada), and a rat renin cDNA (gift of Kevin Lynch, University of Virginia, Charlottesville, VA). cDNAs were labeled with 32P by random priming to specific activities equal to or higher than 1 × 108 cpm/μg. In addition, blots were hybridized with a housekeeping gene, a 780-bp cDNA fragment of human GAPDH (American Type Culture Collection, Rockville, MD), to control for equal loading. Hybridization signals were detected and quantitated by a PhosphorImager system (Molecular Dynamics, Sunnyvale, CA). The ratio of each mRNA to GAPDH mRNA was calculated for each group.
Morphometric and immunohistochemical study. Kidneys from six control and six enalapril-treated rats were fixed in Bouin's solution, embedded in paraffin, sectioned at 4 μm, and stained with periodic acid-Schiff. Paired kidneys from the same rats were fixed in 10% formalin, embedded in paraffin, and sectioned. Using periodic acid-Schiff-stained sections, the relative area of 25 glomeruli from each animal was measured using a digital imaging system (Mocha, Jandel Scientific, San Rafael, CA). Using methylene green-stained formalin-fixed sections, tubular intraluminal areas were measured in 10 non-overlapping fields viewed under 400× magnification.
For each antibody, kidneys from five to six rats were studied for each group. Immunoreactive TGF-β1, EGF, and clusterin were detected with the avidin-biotin immunoperoxidase method (Vectastain, Vector Labs, Burlingame, CA). Antibodies used included a 1:50 dilution of rabbit monoclonal antihuman TGF-β1 antibody (Promega, Madison, WI), 1:400 dilution of rabbit polyclonal anti-rat EGF antibody (Biomedical Technologies, Stoughton, MA), or 1:50 dilution of rabbit monoclonal anti-rat clusterin antibody (Upstate Biotechnology, Lake Placid, NY). As a negative control, the primary antiserum was replaced by nonimmune rabbit serum, and no staining occurred. Sections were counterstained with methylene green and examined in blinded fashion by light microscopy. The mean luminal area of clusterin-stained tubules was compared with that of nonstained tubules.
Statistical analysis. Data are presented as mean ± SEM. Comparisons between groups for each age were performed by one-way ANOVA, the Student-Newman-Keuls test, and t test. Statistical significance was defined as p < 0.05.
RESULTS
Mortality. A death rate of 40% was observed in the enalapril-treated group. There was no mortality in the vehicle-treated group.
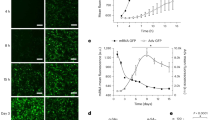
Body weight and kidney weight. On d 7, the body weight of pups receiving enalapril was significantly lower than that of the control group (Fig. 1A). This difference persisted to d 14 (Fig. 1A). By d 14, kidney weight was also significantly decreased in the enalapril group (Fig. 1B), but the kidney/body weight ratio was not different between the groups.
Glomerular and tubular luminal area. Compared with the control group, enalapril treatment reduced mean glomerular area by 27% (Fig. 1C). Despite the reduction in glomerular area, there was no glomerular sclerosis or infarction (Fig. 2C). Enalapril treatment doubled mean tubular luminal area (Figs. 1D and 2D).
Photomicrographs of representative rat kidneys obtained at the end of the study period. (A) Immunostaining (brown) EGF in control group. EGF is widely distributed in distal tubules. (B) Immunostaining EGF in enalapril-treated group. There is widespread tubular dilatation and markedly reduced EGF immunoreactivity. Glomeruli appear normal. (C) Immunostaining clusterin in control group. There is no identifiable staining. (D) Immunostaining clusterin in enalapril-treated group. Scattered dilated tubules contain immunoreactive clusterin (arrowhead).
TGF- β 1 immunoreactivity. Immunoreactive TGF-β1 was diffusely distributed along the luminal border of tubular epithelial cells, with no detectable difference in distribution or intensity between groups (not shown).
EGF immunoreactivity. Immunoreactive EGF was localized to the cytoplasm of control distal tubules as shown in Fig. 2A. Enalapril treatment markedly suppressed tubular EGF immunostaining (Fig. 2B).
Clusterin immunoreactivity. Immunoreactive clusterin was not detectable in control kidneys (Fig. 2C), but was localized to scattered dilated tubules in kidneys from enalapril-treated rats (Fig. 2D). The median luminal area of clusterin-staining tubules was 4-fold greater than that of nonstaining tubules (p < 0.05, ANOVA on rank sum).
TGF-β1 mRNA expression. Treatment for 14 d with enalapril reduced steady state renal TGF-β1 mRNA expression by nearly 50% (Figs. 3 and 4A).
EGF mRNA expression. Enalapril treatment decreased renal EGF mRNA expression by 81% (Figs. 3 and 4B).
Clusterin mRNA expression. In contrast, enalapril treatment increased renal clusterin mRNA expression over 3-fold that of the control group (Figs. 3 and 4C).
Renin mRNA expression. Enalapril nearly doubled renal renin mRNA expression (Figs. 3 and 4D).
DISCUSSION
The present study demonstrates that ACE inhibition by enalapril impairs somatic and renal growth in the neonatal rat. Moreover, renal development is impaired as evidenced by reduced glomerular volume and tubular dilatation. The increase in renal renin expression is the expected consequence of recruitment of renin-secreting cells resulting from ANG II inhibition(16). The results are consistent with reports of intrauterine growth retardation, renal tubular dysplasia, and neonatal death resulting from the maternal use of ACE inhibitors during pregnancy in humans, primates, sheep, and rabbits(3, 19–21). The long-term consequences of ACE inhibition or ANG II antagonism in the neonatal rat include papillary atrophy and impaired urine concentrating ability in adulthood(22). Mice homozygous for a null mutation in the angiotensinogen gene show delayed glomerular maturation, abnormal renal vascular development, and renal papillary hypoplasia(23). It should be noted that, in these mice, the abnormalities present in the kidneys are not present in the heart, liver, or major vessels. Although the effects of enalapril in neonatal rats demonstrated in the present study may not be limited to the kidney, the studies of angiotensinogen-deficient mice suggest that this organ is the most severely affected by ACE inhibition. Interference with normal renal maturation by ACE inhibitors has been reported even for amphibians: tadpoles exposed to water containing enalapril develop dysplastic changes in the mesonephros(4).
Administration of losartan (an AT1 receptor antagonist) to neonatal rats also impairs somatic and renal growth, by interfering with renal vascular and glomerular development(4). This effect was not obtained with administration of an AT2 receptor inhibitor, suggesting that the primary effect of ACE inhibitors on renal growth is mediated by AT1 receptors(4). Although the fetal consequences of maternal ACE inhibition have been ascribed to fetal hypotension and renal ischemia(3), administration of hydralazine to neonatal rat pups does not impair renal growth or result in renal dysgenesis(4, 24). Enalapril (but not hydralazine) causes growth retardation in maturing glomeruli in the rat(25). This suggests that the changes observed in the present study are the result of inhibition of ANG II formation rather than being a response to hypotension. We have also recently reported that administration of losartan to neonatal rats impairs growth of the normal kidney, but does not further decrease growth of the kidney subjected to chronic ureteral obstruction(11). ANG II induces cellular hypertrophy in cultured proximal tubular cells(10), whereas administration of exogenous ANG II to neonatal rats stimulates renal growth and glomerular maturation(26). These results suggest a dominant role for ANG in the overall regulation of renal growth during the period of nephrogenesis.
The present study reveals that ACE inhibition significantly reduced the expression of TGF-β1 in the maturing kidney. Because the renin-angiotensin system is activated in early development, this is consistent with the increased expression of TGF-β1 by renal proximal tubular cells undergoing hypertrophy after exposure to ANG(5). TGF-β1 enhances the extent of gap junction-mediated intercellular communication between normal rat kidney cells(27). TGF-β1 also regulates the glomerular and renal interstitial production of numerous extracellular matrix molecules, as well as the integrins that are the receptors for these molecules(28). In this regard, enalapril reduces renal TGF-β1 expression and interstitial fibrosis which are stimulated by ureteral obstruction(29). We found that whereas losartan reduced the augmented TGF-β1 expression by the obstructed neonatal rat kidney, there was no effect on TGF-β1 expression by the normal kidney(11). The reasons for these differences may relate to incomplete inhibition of the AT1 receptor by losartan (although a large dose was used), or decreased degradation of bradykinin resulting from ACE inhibition in the present study. The latter is unlikely, because TGF-β1 expression by cultured mesangial cells is unaffected by bradykinin, which stimulates (rather than inhibiting) mesangial proliferation(30). An alternative explanation is the regulation of TGF-β1 expression by ANG receptors other than the AT1 receptor. Thus, whereas losartan increases ANG II levels, ACE inhibition by enalapril reduces ANG II levels. Renal TGF-β1 is localized to cortical distal tubular cells, and expression decreases during early postnatal development in the rat(31). It is likely that TGF-β1 plays a role in controlling interactions between epithelia and surrounding mesenchyme in the developing kidney(32), and ACE inhibition may impair renal growth in part by this mechanism.
Inhibition of renal EGF expression by enalapril in the neonatal rat as found in the present study is similar to the response to losartan(11). EGF is a potent growth promoter for renal proximal tubular cells(33) and regulates tubulogenesis(9, 34). ANG II and EGF are synergistic in stimulating cellular proliferation, by complementary actions at sequential cell cycle loci(35). Renal EGF expression increases progressively in the maturing rat and mouse, after first appearing in distal tubules several days after birth(36, 37). In addition, renal EGF receptors are induced and activated in late gestation in the rat, which suggests their participation in renal growth and development(38). Expression of EGF is also reduced in polycystic kidney disease of mice(39), and administration of exogenous EGF reduces tubular dilatation and improves renal function in this model(40). Moreover, chronic administration of ANG II in the rat increases aortic expression of EGF receptor mRNA(41). Inhibition of ANG II formation by enalapril in the present study may therefore also contribute to impaired renal growth and development by interfering with production of EGF and its receptor.
Clusterin is a glycoprotein expressed by a variety of tissues, that promotes aggregation and adhesion of renal epithelial cells(13). Clusterin expression is increased in the developing glomeruli during epithelial polarization, and may play a significant role in this process(42). In addition, renal clusterin expression is activated in response to injury, including ureteral obstruction, renal ablation, and renal ischemia(12). In the present study, enalapril markedly increased renal clusterin expression in the neonatal kidney, a response similar to that resulting from losartan administration(11). Clusterin was localized to dilated tubules, a pattern similar to that resulting from ureteral obstruction and cystic kidney disease(43, 44). This suggests that clusterin expression is chronically suppressed by ANG II AT1 receptors. However, in a preliminary study, we demonstrated a marked increase in renal clusterin expression after ANG II administration in 3-d-old rats subjected to ureteral obstruction(26). Because this response can be blocked by an AT2 receptor inhibitor, but not by losartan(45), clusterin expression may be stimulated by AT2 receptors, which are more abundant in early life, and inhibited by AT1 receptors, which predominate in the mature kidney(46).
In summary, chronic inhibition of endogenous ANG II in neonatal rats impaired somatic and renal growth, and increased renal renin expression. This was associated with suppression of TGF-β1 and EGF gene expression. These growth factors have well established effects in the kidney, to promote cellular growth and differentiation. The findings are consistent with the hypothesis that ACE inhibitor “fetopathy”(3) is a consequence of impaired expression of growth factors under the regulation of ANG II. Stimulation of the renal expression of clusterin after ACE inhibition may result from inhibition of AT1 receptors.
Abbreviations
- ACE:
-
angiotensin converting enzyme
- ANG II:
-
angiotensin II
- EGF:
-
epidermal growth factor
- GAPDH:
-
glyceraldehyde-3-phosphate dehydrogenase
- TGF-β1:
-
transforming growth factor-β1
References
Wolf G 1995 Angiotensin as a renal growth promoting factor. Adv Exp Med Biol 377: 225–236.
Gomez RA, Lynch KR, Sturgill BC, Elwood JP, Chevalier RL, Carey RM, Peach MJ 1989 Distribution of renin mRNA and its protein in the developing kidney. Am J Physiol 257:F850–F858.
Pryde PG, Sedman AB, Nugent CE, Barr M 1993 Angiotensin-converting enzyme inhibitor fetopathy. J Am Soc Nephrol 3: 1575–1582.
Tufro-McReddie A, Romano LM, Harris JM, Ferder L, Gomez RA 1995 Angiotensin II regulates nephrogenesis and renal vascular development. Am J Physiol 269:F110–F115.
Wolf G, Mueller E, Stahl RAK, Ziyadeh FN 1993 Angiotensin II-induced hypertrophy of cultured murine proximal tubular cells is mediated by endogenous transforming growth factor-β. J Clin Invest 92: 1366–1372.
Gibbons GH, Pratt RE, Dzau VJ 1992 Vascular smooth muscle cell hypertrophy vs. hyperplasia. Autocrine transforming growth factor-β1 expression determines growth response to angiotensin II. J Clin Invest 90: 456–461.
Sponsel HT, Breckon R, Hammond W, Anderson RJ 1994 Mechanisms of recovery from mechanical injury of renal tubular epithelial cells. Am J Physiol 267:F257–F264.
Roberts AB, McCune BK, Sporn MB 1992 TGF-β: regulation of extracellular matrix. Kidney Int 41: 557–559.
Taub M, Wang Y, Szczesny TM, Kleinman HK 1990 Epidermal growth factor or transforming growth factor a is required for kidney tubulogenesis in matrigel cultures in serum-free medium. Proc Natl Acad Sci USA 87: 4002–4006.
Wolf G, Neilson EG 1990 Angiotensin II induces cellular hypertrophy in cultured murine proximal tubular cells. Am J Physiol 259:F768–F777.
Chung KH, Gomez RA, Chevalier RL 1995 Regulation of renal growth factors and clusterin by angiotensin AT1 receptors during neonatal ureteral obstruction. Am J Physiol 268:F1117–F1123.
Rosenberg ME, Silkensen J 1995 Clusterin and the kidney. Exp Nephrol 3: 9–14.
Silkensen JR, Skubitz KM, Skubitz APN, Chmielewski DH, Manivel JC, Dvergsten JA, Rosenberg ME 1995 Clusterin promotes the aggregation and adhesion of renal porcine epithelial cells. J Clin Invest 96: 2646–2653.
Merlet-Benichou C, Gilbert T, Muffat-Joly M, Lelievre-Pegorier M, Leroy B 1994 Intrauterine growth retardation leads to a permanent nephron deficit in the rat. Pediatr Nephrol 8: 175–180.
Schuetz S, Le Moullec JM, Corvol P, Gasc JM 1996 Early expression of all the components of the renin-angiotensin-system in human development. Am J Pathol 149: 2067–2079.
Gomez RA, Lynch KR, Chevalier RL, Everett AD, Johns DW, Wilfong N, Peach MJ, Carey RM 1988 Renin and angiotensinogen gene expression and intrarenal renin distribution during ACE inhibition. Am J Physiol 254:F900–F906.
Chomczynski P, Sacchi N 1987 Single-step method of RNA isolation by acid guanidinium thiocyanate-phenol-chloroform extraction. Anal Biochem 162: 156–159.
Church GM, Gilbert W 1984 Genomic sequencing. Proc Natl Acad Sci USA 81: 1991–1995.
Shotan A, Widerhorn J, Hurst A, Elkayam U 1994 Risks of angiotensin-converting enzyme inhibition during pregnancy: Experimental and clinical evidence, potential mechanisms, and recommendations for use. Am J Med 96: 451–456.
Harewood WJ, Phippard AF, Duggin GG, Horvath JS, Tiller DJ 1994 Fetotoxicity of angiotensin-converting enzyme inhibition in primate pregnancy: a prospective, placebo-controlled study in baboons (Papio hamadryas). Am J Obstet Gynecol 171: 633–642.
Broughton-Pipkin F, Symonds EM, Turner SR 1982 The effect of captopril (SQ 14,225) upon mother and fetus in the chronically cannulated ewe and in the pregnant rabbit. J Physiol 323: 415–422.
Friberg P, Sundelin B, Bohman SO, Bobik A, Nilsson H, Wickman A, Gustafsson H, Petersen J, Adams MA 1994 Renin-angiotensin system in neonatal rats: induction of a renal abnormality in response to ACE inhibition or angiotensin II antagonism. Kidney Int 45: 485–492.
Niimura F, Labosky PA, Kakuchi J, Okubo S, Yoshida H, Oikawa T, Ichiki T, Naftilan AJ, Fogo A, Inagami T, Hogan BLM, Ichikawa I 1995 Gene targeting in mice reveals a requirement for angiotensin in the development and maintenance of kidney morphology and growth factor regulation. J Clin Invest 96: 2947–2954.
Charbit M, Dechaux M, Blazy I, Vargas R, Laouari D, Brocart D, Lacoste M, Gubler MC, Sachs C 1995 Deleterious effects of inhibition of the renin-angiotensin system in neonatal rats. Pediatr Nephrol 9: 303–308.
Fogo A, Yoshida Y, Yared A, Ichikawa I 1990 Importance of angiogenic action of angiotensin II in the glomerular growth of maturing kidneys. Kidney Int 38: 1068–1074.
Yoo KH, Krajewski S, Reed JC, Smith CD, Chevalier RL 1996 Angiotensin II promotes growth and inhibits apoptosis in the neonatal rat kidney with unilateral ureteral obstruction. Pediatr Res 39: 372A (abstr)
Van Zoelen EJJ, Tertoolen LGJ 1991 Transforming growth factor-β enhances the extent of intercellular communication between normal rat kidney cells. J Biol Chem 266: 12075–12081.
Sharma K, Ziyadeh FN 1994 The emerging role of transforming growth factor-β in kidney diseases. Am J Physiol 266:F829–F842.
Ishidoya S, Morrissey J, McCracken R, Klahr S 1996 Delayed treatment with enalapril halts tubulointerstitial fibrosis in rats with obstructive nephropathy. Kidney Int 49: 1110–1119.
El-Dahr SS, Dipp S, Cupp C, Yosipiv IV, Baricos WH 1995 Bradykinin stimulates AP-1/DNA binding activity and hyperplasia in cultured rat mesangial cells. J Am Soc Nephrol 6: 766 (abstr)
Coimbra TM, Da Silva CGA, Lachat JJ 1994 Renal transforming growth factor β1 production in neonate rats. Cell Prolif 27: 669–675.
Thompson NL, Flanders KC, Smith JM, Ellingsworth LR, Roberts AB, Sporn MB 1989 Expression of transforming growth factor-β1 in specific cells and tissues of adult and neonatal mice. J Cell Biol 108: 661–669.
Humes HD, Beals TF, Cieslinski DA, Sanchez IO, Page TP 1991 Effects of transforming growth factor-β, transforming growth factor-α, and other growth factors on renal proximal tubule cells. Lab Invest 64: 538–545.
Chailler P, Ferrari J, Briere N 1991 Fetal mouse kidney maturation in vitro: coordinated influences of epidermal growth factor, transferrin and hydrocortisone. Anat Embryol 184: 319–329.
Bagby SP, Kirk EA, Mitchell LH, O'Reilly MM, Holden WE, Stenberg PE, Bakke AC 1993 Proliferative synergy of ANG II and EGF in porcine aortic vascular smooth muscle cells. Am J Physiol 265:F239–F249.
Chung KH, Chevalier RL 1996 Arrested development of the neonatal kidney following chronic ureteral obstruction. J Urol 155: 1139–1144.
Salido EC, Lakshmanan J, Shapiro LJ, Fisher DA, Barajas L 1990 Expression of epidermal growth factor in the kidney and submandibular gland during mouse postnatal development. An immunocytochemical and in situ hybridization study. Differentiation 45: 38–43.
Cybulsky AV, Goodyer PR, McTavish AJ 1994 Epidermal growth factor receptor activation in developing rat kidney. Am J Physiol 267:F428–F436.
Gattone VH, Andrews GK, Niu Fu-Wen, Chadwick LJ, Klein RM, Calvet JP 1990 Defective epidermal growth factor gene expression in mice with polycystic kidney disease. Dev Biol 138: 225–230.
Gattone VH, Lowden DA, Cowley BD Jr 1995 Epidermal growth factor ameliorates autosomal recessive polycystic kidney disease in mice. Dev Biol 169: 504–510.
Sambhi MP, Swaminathan N, Wang H, Rong H 1992 Increased EGF binding and EGFR mRNA expression in rat aorta with chronic administration of pressor angiotensin II. Biochem Med Metab Biol 48: 8–18.
French LE, Chonn A, Ducrest D, Baumann B, Belin D, Wohlwend A, Kiss JZ, Sappino A-P, Tschopp J, Schifferli JA 1993 Murine clusterin: molecular cloning and mRNA localization of a gene associated with epithelial differentiation processes during embryogenesis. J Cell Biol 122: 1119–1130.
Chevalier RL, Chung KH, Smith CD, Ficenec M, Gomez RA 1996 Renal apoptosis and clusterin following ureteral obstruction: the role of maturation. J Urol 156: 1474–1479.
Rosenberg ME, Manivel JC, Carone FA, Kanwar YS 1995 Genesis of renal cysts is associated with clusterin expression in experimental cystic disease. J Am Soc Nephrol 5: 1669–1674.
Yoo KH, Thornhill BA, Chevalier RL 1996 Angiotensin II stimulates transforming growth factor-β1 and clusterin gene expression in the neonatal rat kidney following unilateral ureteral obstruction. J Am Soc Nephrol 7: 1750–1751. (abstr)
Aguilera G, Kapur S, Feuillan P, Sunar-Akbasak B, Bathia AJ 1994 Developmental changes in angiotensin II receptor subtypes and AT1 receptor mRNA in rat kidney. Kidney Int 46: 973–979.
Author information
Authors and Affiliations
Additional information
Supported in part by National Institutes of Health Research Center of Excellence in Pediatric Nephrology and Urology, DK44756; National Institutes of Health O'Brien Center of Excellence in Nephrology and Urology, DK45179; and National Institutes of Health Child Health Research Center, HD 28810.
Rights and permissions
About this article
Cite this article
Yoo, K., Wolstenholme, J. & Chevalier, R. Angiotensin-Converting Enzyme Inhibition Decreases Growth Factor Expression in the Neonatal Rat Kidney. Pediatr Res 42, 588–592 (1997). https://doi.org/10.1203/00006450-199711000-00006
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/00006450-199711000-00006
This article is cited by
-
Angiotensin inhibition in the developing kidney; tubulointerstitial effect
Pediatric Research (2019)
-
Calcitriol reduces kidney development disorders in rats provoked by losartan administration during lactation
Scientific Reports (2017)
-
Early life obesity and chronic kidney disease in later life
Pediatric Nephrology (2015)
-
Cellular and RAS Changes in the Hearts of Young Obese Rats
Pediatric Cardiology (2011)
-
Renin–angiotensin system in ureteric bud branching morphogenesis: insights into the mechanisms
Pediatric Nephrology (2011)