Abstract
Prepubertal years of insulin-dependent diabetes mellitus are protected from the nephropathic effects of this disease, yet this effect of immaturity has not been investigated in an animal model. Male Munich-Wistar rats were made diabetic with streptozocin at two ages: weanling (≈4 wk) and pubescent(≈10 wk). After 5 wk of untreated diabetes, weanling diabetic animals showed relatively greater growth of the medulla, whereas relative proportions of these areas were constant in the older animals. Glomerular volume increased by ≈35% in older diabetic animals, but no glomerular enlargement was demonstrated in weanling rats with diabetes. Glomerular ultrastructure was not significantly altered during the short course of this study. The renal structural response to diabetes is age-dependent in the rat, with prepubertal animals protected from glomerular hypertrophy. Longer studies are needed to see if these differences will eventually parallel those demonstrated in patients with onset of diabetes before and after puberty. This model may ultimately prove to be valuable in determining the mechanism via which prepubertal kidneys are protected from the nephropathic effects of insulin-dependent diabetes mellitus.
Similar content being viewed by others
Main
Diabetes mellitus is the most important cause of end-stage renal disease in the United States(1). Between 30 and 40% of patients with IDDM will develop diabetic nephropathy(2). Strict glycemic control can retard or prevent development of microalbuminuria, the earliest clinical indicator of diabetic kidney disease(3); however, it is unlikely that sufficient metabolic control can be achieved throughout the population to eliminate IDDM nephropathy. It has been suggested that current levels of care may be reducing the incidence of nephropathy, although this is not a universal finding(4, 5). Better understanding of the nephropathic effects of the diabetic state is thus still of importance, even after the Diabetes Control and Complications Trial(3).
Understanding a state that is protected from the adverse consequences of IDDM could further our understanding of its pathogenesis. The period of IDDM before puberty may be a naturally protected state(6, 7). Structural studies of kidney biopsies from young diabetic patients suggest that, although glomerulopathy is developing during this period, its consequences on renal structure and function are blunted(8–10). Other complications may be affected by the age of onset of diabetes. Peripheral nerve structure and function in the rat are altered by diabetes in an age-dependent manner(11). The renoprotective nature of the prepubescent period has not been thoroughly addressed in animal models of diabetes. The following study demonstrated that the short-term renal structural response to the diabetic state induced by STZ is also age-dependent in the rat.
METHODS
Animals. Male Munich-Wistar rats were used for these experiments. Weanling rats were approximately 4 wk of age at the beginning of these studies and weighed 86 ± 7 g (mean ± SD). Older animals were 10 wk of age and weighed 256 ± 14 g.
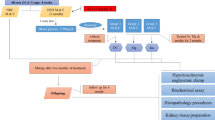
On the first day of these studies, diabetic animals received an intraperitoneal injection of STZ, 65 mg per kg of body weight. Control animals in each age group received an equivalent volume of normal saline. The onset of diabetes was confirmed by the presence of glycosuria 2 d after injection. If glycosuria had not developed, the animal was killed and excluded from further study.
All animals had free access to standard chow and tap water throughout these studies. Diabetic animals were not treated with insulin. During the final week of the experiment, a drop of blood was drawn from a tail vein for determination of glucose using a blood glucose meter (Glucometer 3, Miles Inc., Elkhart, IN). After 5 wk of STZ diabetes, the animals were killed in a CO2 chamber. This time course was chosen so that the older groups would have reached sexual maturity, yet the younger groups would not have completed puberty.
Morphometric studies. At the conclusion of these experiments, the kidneys were rapidly excised, weighed, and immersion-fixed in Karnovsky's solution (glutaraldehyde-paraformaldehyde). After 24 h in fixative, one kidney was sectioned transversely at 4-mm thickness, and one of these transverse slices was then processed in methacrylate, sectioned at 2 μm, and silver-stained. A smaller portion of an adjacent kidney slice was processed for electron microscopy. All morphometric studies were performed by a single observer masked to the identity of the tissue using standard techniques that have been described in detail elsewhere(12).
The relative proportions of the kidney composed of cortex and medulla were determined via point counting on a single slide at a final magnification of 60 using a 2-cm lattice grid. The relative proportions of the cortex composed of tubules and interstitium were estimated in a similar manner at a magnification of 150. Mean glomerular volume (VG) was calculated from the mean profile area for 50 glomeruli on a single section(13). Electron microscopic studies were performed on three or more glomeruli per animal. The width of the GBM was estimated using the orthogonal intercept method on electron micrographs with a final magnification of 18 000(13, 14). These same micrographs were studied with a 1-cm lattice grid to estimate the relative proportions of the mesangium composed of cells and matrix. A montage of the glomerulus was assembled from micrographs of 6000 magnification. Using standard techniques, the relative volume of the glomerulus composed of mesangium (Vvmes/G) and the surface density of peripheral GBM per unit volume of glomerulus (SvPGBM/G) were determined. These volume fractions or proportions were multiplied by VG, the appropriate reference volume, to generate absolute quantities of the parameter of interest.
Statistics. All values are reported as mean ± SD. Values for the four groups were first compared with analysis of variance. Post hoc comparisons for diabetic versus control weanlings and diabetic versus control older animals were performed with Fisher's protected least significant difference method. p < 0.05 was considered significant. Comparisons between continuous parameters were examined with linear regression analysis. All computations were performed with Statview 4.5 software (Abacus Concepts, Inc., Berkeley, CA).
RESULTS
Twenty-six animals completed these experiments, including nine DW, five CW, seven DO, and five CO. Body weight at the initiation of these experiments were similar in DW and CW animals (84 ± 7 and 88 ± 8 g) and in DO and CO animals (264 ± 14 and 248 ± 14 g). Body weight after 5 wk of diabetes was lower for DW animals (217 ± 40 for DW and 267 ± 50 for the CW), but was not statistically different in the two older groups (275± 20 for DO and 313 ± 36 for CO). There was a trend toward less weight gain in the diabetic groups of both ages (214 ± 73% of initial body weight for CW and 159 ± 52% for DW; p < 0.05; 26± 7% for CO and 4 ± 4% for DO; p = 0.4). All diabetic animals had blood glucose values that exceeded the upper limit of the monitor(>27.8 mmol/L or >500 mg/dL), whereas control animals had detectable levels less than 8.3 mmol/L (<150 mg/dL).
Kidney weight was not significantly altered by STZ diabetes, although there was a trend toward increased weight in both diabetic groups(Table 1). Kidney growth in the weanling animals included a disproportionate increase in the fraction of the kidney composed of medulla(Table 1). Normal proportions of cortex and medulla were maintained in older animals. Cortical tubular volume fraction tended to be higher in DO than CO animals, whereas no difference was seen in weanlings(Table 1). Vvinterstitium/cortex was decreased in the DO group compared with the CO group (Table 1).
VG was significantly increased in older diabetic animals, but STZ diabetes did not increase glomerular size in the weanling animals (Fig. 1). GBM width did not differ significantly among these groups (Table 2). Mean peripheral GBM surface area per glomerulus (SvPGBM/G × VG) was similar for weanling animals with and without diabetes, but was greater in adult diabetic animals than in controls (Table 2). This difference was due solely to enlargement of VG rather than changes in SvPGBM/G (0.241 ± 0.026 for DW, 0.258± 0.035 for CW, 0.260 ± 0.055 for DO, and 0.264 ± 0.047μm2/μm3 for CO). The proportion of the glomerulus composed of mesangium (Vvmes/G) was similar for all the groups, as was the absolute volume of mesangium per glomerulus (Table 2). The volume fractions of mesangial cells and matrix per glomerulus were also similar in these four groups (Table 2). Although not statistically different, the volume of mesangial matrix per glomerulus in DO animals was approximately 50% greater than CO animals.
DISCUSSION
As expected, the older diabetic animals showed glomerular enlargement, with≈35% increase in VG(15). Similar to the results of Ellis et al.(16) weanling animals with STZ diabetes did not demonstrate an increase in glomerular size, nor did these animals demonstrate ultrastructural changes. This age group did develop medullary enlargement, a finding not previously reported. The blood glucose determinations did not allow comparison of the exact level of hyperglycemia in weanling and older diabetic animals, so subtle differences in glycemic control could have contributed to these findings. However, all animals had severe hyperglycemia, and these results confirm those of Ellis et al.(16), so an age-mediated effect seems likely. Differences in hyperglycemia or accumulation of advanced glycosylation end products cannot be excluded as a cause of the differences demonstrated in the present study.
Previous studies of the kidney after 6-7 wk of STZ diabetes have demonstrated a degree of glomerular enlargement similar to the present study with GBM thickening and accumulation of extracellular matrix material(17). However, animals studied by Østerby and Gundersen(17) were 5-8 mo of age and 240-270 g in body weight and were considerably older than all ages presented here.“Older” animals in the present study were in mid-puberty at the onset and had completed sexual maturation by the conclusion of these experiments. In male rats, plasma testosterone begins to increase by 5 wk of age, reaching adult levels by 10 wk(18). The pubertal plasma surge of IGF-I begins during the 6th wk of life and plateaus by 11 wk of age(19). Spermatogenesis occurs by 8 wk of age with onset of breeding at 13 wk(18).
Krolewski et al.(6) suggested that the prepubertal years were somewhat protected from the adverse effects of diabetes mellitus. Data regarding the duration of diabetes at the onset of proteinuria were stratified by age of onset of diabetes. Those patients with onset in the first decade of life had a greater average duration of diabetes to onset of proteinuria, whereas patients with onset of IDDM in the third decade of life had the shortest duration. The overall incidence of proteinuria was the same, regardless of age of onset(6). Subsequent studies have confirmed that puberty may accelerate or induce diabetic nephropathy, especially microalbuminuria and renal hypertrophy(7, 20, 21).
These age-dependent findings may be due to different structural responses of the kidney to the diabetic state, as suggested by Drummond et al.(8). Patients with onset of IDDM before 15 y of age were matched for Vvmes/G with patients with the same duration of IDDM but onset after 15 y of age. Despite having similar degrees of mesangial expansion, patients with younger age of onset had increased peripheral GBM surface when compared with both normal adults and the matched older-onset IDDM patients. This is in contrast to multiple studies of peripheral GBM surface in adults with IDDM where increased Vvmes/G correlates inversely with surface area(22, 23). Others have confirmed that diabetic glomerulopathy, as well as tubulointerstitial lesions, occur in young diabetic patients but do not result in renal dysfunction as they do in older patients(9, 10).
The STZ rat is one of the most widely studied models of IDDM, yet few studies have documented the renal structural effects of induction of IDDM with this agent early in life. Bach and Jerums(24) found that renal hypertrophy was decreased in 5-wk-old animals given STZ when compared with the renal hypertrophy in 13-wk-old animals. Younger animals did not develop significant increases in renal weight until 7 d of STZ diabetes, whereas renal weight was significantly increased by 2 d in the postpubertal rats. Histologic studies were not performed in these experiments(24). Using morphometric techniques, Ellis et al.(16) found that juvenile rats did not develop glomerular hypertrophy after 3-5 mo of diabetes. Kidney size and glomerular volume were similar to weight-matched control animals, suggesting that the growth retardation associated with the diabetic state might be responsible. Older-onset animals with STZ diabetes were not included in the study of Ellis et al.(16), so duration-matched groups could not be compared directly. Malone et al.(11) have recently reported that peripheral nerve structure and function are affected by hyperglycemia in an age-dependent manner. However, the younger animal appears to be more affected by the diabetic state when peripheral nerves are studied, in contrast to the protection of the kidney during the early years of IDDM. This may reflect different pathogenic mechanisms for nephropathy and neuropathy in IDDM.
In summary, 5 wk of untreated STZ diabetes resulted in differing renal structural changes in the rat, dependent on the age of onset. Older animals, as previously described(15, 17), developed glomerular enlargement, whereas weanlings were spared alterations in glomerular size or structure. Further study is needed to see if these changes will eventually parallel the differences seen in patients with onset of IDDM before and after puberty, as well as to delineate the mechanism of these differences with special attention to the effect of age of onset on the degree of hyperglycemia and accumulation of advanced glycosylation end products(8). Early onset STZ diabetes may provide an excellent model for the study of a natural mechanism of protection from the nephropathic effects of the diabetic state.
Abbreviations
- IDDM:
-
insulin-dependent diabetes mellitus
- STZ:
-
streptozocin
- Vv X/Y :
-
volume fraction of Y (reference volume) composed of structure X;
- V G :
-
mean glomerular volume
- GBM:
-
glomerular basement membrane
- DW:
-
diabetic weanling animals
- CW:
-
control weanling animals
- DO:
-
diabetic older animals
- CO:
-
control older animals
References
1994 Excerpts from United States Renal Data System 1994 Annual Data Report. IV. Incidence and causes of treated ESRD. Am J Kidney Dis 24( Suppl 2): S48–S56.
Andersen AR, Christiansen JS, Andersen JK, Kreiner S, Deckert T 1983 Diabetic nephropathy in type 1 (insulin-dependent) diabetes: an epidemiological study. Diabetologia 25: 496–501.
The Diabetes Control and Complications Trial Research Group 1993 The effect of intensive treatment of diabetes on the development and progression of long-term complications in insulin-dependent diabetes mellitus. N Engl J Med 329: 977–986.
Bojestig M, Arnqvist J, Hermansson G, Karlberg B, Ludvigsson J 1994 Declining incidence of nephropathy in insulin-dependent diabetes mellitus. N Engl J Med 330: 15–18.
Rossing P, Rossing K, Jacobsen P, Parving H-H 1995 Unchanged incidence of diabetic nephropathy in IDDM patients. Diabetes 44: 739–743.
Krolewski AS, Warram JH, Christlieb AR, Busick EJ, Kahn CR 1985 The changing natural history of nephropathy in type I diabetes. Am J Med 78: 785–794.
Lawson ML, Sochett EB, Chait PG, Balfe JW, Daneman D 1996 Effect of puberty on markers of glomerular hypertrophy and hypertension in IDDM. Diabetes 45: 51–55.
Drummond K for the Diabetic Nephropathy Study Group 1990 Young kidneys respond differently than adult kidneys to insulin dependent diabetes mellitus. J Am Soc Nephrol 1: 307
Ellis E, Warady B, Wood E, Richardson W 1991 Glomerulopathy in early type I diabetes mellitus (DM). J Am Soc Nephrol 2: 288
Lane P, Warady B, Wood E, Ellis E 1993 Mesangial and interstitial expansion in young patients with insulin-dependent diabetes mellitus (IDDM). J Am Soc Nephrol 4: 304
Malone JI, Lowitt S, Korthals JK, Salem A, Miranda C 1996 The effect of hyperglycemia on nerve conduction and structure is age dependent. Diabetes 45: 209–215.
Lane PH 1995 Furosemide treatment, angiotensin II, and renal growth and development in the rat. Pediatr Res 37: 747–754.
Lane PH 1995 Determination of mean glomerular volume in nephrectomy specimens. Lab Invest 72: 765–770.
Jensen E, Gundersen H, Østerby R 1979 Determination of membrane thickness distribution from orthogonal intercepts. J Microsc 115: 19–33.
Seyer-Hansen K, Hansen J, Gundersen HJG 1980 Renal hypertrophy in experimental diabetes. Diabetologia 18: 501–505.
Ellis EN, Wiegmann TB, Savin VJ 1992 Diminished glomerular capillary hydraulic conductivity precedes morphologic changes in experimental diabetes mellitus in the rat. Diabetes 41: 1106–1112.
Østerby R, Gundersen H 1980 Fast accumulation of basement membrane material and the rate of morphological changes in acute experimental diabetic glomerular hypertrophy. Diabetologia 18: 493–500.
Knorr D, Vanha-Perttula T, Lipsett M 1970 Structure and function of rat testis through pubescence. Endocrinology 86: 1298–1304.
Handelsman D, Spaliviero J, Scott C, Baxter R 1987 Hormonal regulation of the peripubertal surge of insulin-like growth factor-I in the rat. Endocrinology 120: 491–496.
Kostraba JN, Dorman JS, Orchard TJ, Becker DJ, Ohki Y, Ellis D, Doft BH, Lobes LA, LaPorte RE, Drash AL 1989 Contribution of diabetes duration before puberty to development of microvascular complications in IDDM subjects. Diabetes Care 12: 686–693.
Salardi S, Cacciari E, Pascucci M, Giambiasi E, Tacconi M, Razzari R, Cicognani A, Boriani F, Publioli R, Mantovani W, Donati S 1990 Microalbuminuria in diabetic children and adolescents: relationship with puberty and growth hormone. Acta Paediatr Scand 79: 437–443.
Ellis EN, Steffes MW, Goetz FC, Sutherland DER, Mauer SM 1986 Glomerular filtration surface in type I diabetes mellitus. Kidney Int 29: 889–894.
Østerby R, Parving H-H Nyberg G, Jørgensen H, Løkkegaard H, Svalander C 1988 A strong correlation between glomerular filtration rate and filtration surface in diabetic nephropathy. Diabetologia 31: 265–270.
Bach LA, Jerums G 1990 Effect of puberty on initial kidney growth and rise in kidney IGF-I in diabetic rats. Diabetes 39: 557–562.
Acknowledgements
The author acknowledges the expert technical assistance of Colleen Seamatter in the care of these animals, and the assistance of the Electron Microscopy Center at Saint Louis University Health Sciences Center in the preparation of these tissues.
Author information
Authors and Affiliations
Additional information
This work was presented at the Annual Meeting of the Pediatric Academic Societies, May 7, 1996, and published in abstract in Pediatric Research 39:363A, 1996. Aspects of this work were also presented at the Annual Meeting of the American Diabetes Association, June 10, 1996, and published in abstract in Diabetes 45:204A, 1996.
Rights and permissions
About this article
Cite this article
Lane, P. Age of Onset of Streptozocin Diabetes Determines the Renal Structural Response in the Rat. Pediatr Res 41, 912–915 (1997). https://doi.org/10.1203/00006450-199706000-00019
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/00006450-199706000-00019
This article is cited by
-
Prepubertal onset of diabetes prevents expression of renal cortical connective tissue growth factor
Pediatric Nephrology (2008)
-
The Aging Kidney: A Review – Part I
International Urology and Nephrology (2005)