Abstract
Studies were conducted to assess the efficacy and safety of a synthetic peptide-containing surfactant in the treatment of respiratory distress syndrome (RDS) in preterm (approximately 80% of normal gestation) infant rhesus monkeys. Surfactant was prepared consisting of the phospholipids dipalmitoylphosphatidyl choline and palmitoyl-oleoyl phosphatidyl glycerol and a synthetic peptide modeled after surfactant protein B (SP-B),“KL4-Surfactant” contained a peptide having the sequence KLLLLKLLLLKLLLLKLLLLK, where “K” is lysine and “L” is leucine. The peptide was selected because it mimics the repeating stretches of hydrophobic residues with intermittent basic hydrophilic residues seen in SP-B. KL4-Surfactant was shown to have biophysical activity assessed as the ability to lower surface tension at an air-liquid interface in a pulsating bubble surfactometer. Thirty premature rhesus monkeys were treated shortly after birth with one dose of KL4-Surfactant. The arterial to alveolar oxygen partial pressure ratio (a/A) was found to rise from a pretreatment level of 0.11 ± 0.01 (mean ± SEM), indicative of severe RDS, to 0.40 ± 0.02 at 12-13 h post-treatment. The improvement in oxygenation persisted throughout the study period, with a mean a/A at 22-23 h of 0.45± 0.07. Chest radiographs and gross and microscopic examination of the lungs all confirmed the reversal of the atelectasis seen before treatment. Animals treated with a dose of 200 mg/kg showed a faster, more consistent, and greater response than did a group treated with an average dose of 127 mg/kg. There was no evidence of toxicity after treatment with the higher dose as demonstrated by physiologic, hematologic, biochemical, and pathologic data. The importance of the peptide in the synthetic surfactant was apparent from the results obtained with a control group of nine premature monkeys treated with a non-peptide-containing surfactant; the a/A of this group was 0.15± 0.03 at nine hours of age as compared with a value of 0.38 ± 0.02 for 30 comparable animals receiving KL4-Surfactant.
Similar content being viewed by others
Main
The major constituents of pulmonary surfactant are phospholipids and proteins. Four proteins have been detected, SP-A, -B, -C. and -D, two of which(SP-B and C) are strongly hydrophobic. Of the four proteins, SP-B, when combined with phospholipids, exhibits the strongest capacity to reduce surface tension and induce pulmonary expansion in 27-d gestation premature rabbits(1–4). In addition, human infants born with an absence of SP-B, but with abundant SP-A and SP-C, exhibit respiratory distress(5); and antibodies to SP-B cause respiratory failure in mice(6) and rabbits(7, 8).
SP-B is a markedly hydrophobic protein of 79-81 residues(2, 9–15), the amino acid sequence of which was predicted from the cDNA(2, 11, 16, 17). Insight into the mechanism by which dispersions of SP-B and phospholipids lower surface tension and expand pulmonary alveoli was provided by studies using peptides synthesized in accordance with the SP-B sequence. Fifteen-residue peptides made over the entire sequence, when incorporated individually into DPPC and PG, all conferred properties of lowering surface tension(18). Synthetic peptides corresponding to residues 1-25 and 46-66 of SP-B(19) and peptides with helical form, bearing hydrophilic and hydrophobic regions unrelated to SP-B(20, 21), were also active. The data suggested that, rather than a specific submolecular domain being responsible for the function of SP-B, a pattern throughout the structure had to be considered. Attention was focused on the repeating pattern of hydrophobic stretches with intermittent basic hydrophilic residues found in SP-B. Peptides of 20-23 residues consisting of only leucine (L) and arginine (R) or lysine (K), synthesized to contain stretches of 2-8 hydrophobic L residues with intermittent K or R basic hydrophilic residues (simplified peptides), exhibited activity equal to that of peptides derived from the native sequence(22, 23). One example of such peptides is KLLLLKLLLLKLLLLKLLLLK (KL4-).
Studies employing tryptophan fluorescence(19, 23), infrared spectroscopy(24), vibrational Raman spectroscopy(25), fluorescence anisotropy(26), and 31P nuclear magnetic resonance and circular dichroism studies (Ouyang C, Wong K, Glavinos P, Revak SD, Cochrane CG, Madden TD, manuscript in preparation), in addition to studies of direct substitution of the hydrophilic residues(22, 23, 27) all indicate that SP-B and its derivative peptides increase lateral stability of the phospholipid layer. Such lateral stability may well account for the functional capacity of pulmonary surfactant to lower surface tension at an air-water interface and to induce and maintain expansion of pulmonary alveoli.
Additionally, synthetic peptides, modeled from the structure of SP-B, and simple peptides mimicking SP-B have been shown to behave similarly to SP-B in conferring surface tension lowering properties to dispersions of DPPC and PG and in inducing expansion of alveoli of premature infant rabbits(18, 23) and saline-lavaged rats(19), models having a demonstrated deficiency in pulmonary surfactant. As those in vivo studies were of short duration, and were restricted to rabbits and rats, it was important to determine whether synthetic peptides resembling SP-B in dispersions of DPPC and POPG could induce expansion of pulmonary alveoli in surfactant-deficient premature primates and if the effect would persist through a period of 24 h. The peptides selected consisted of stretches of hydrophobic leucines with intermittent arginines or lysines. These are referred to as “KL4 peptide,” having a sequence of KLLLLKLLLLKLLLLKLLLLK, where“K” is lysine and “L” is leucine, and“RL4 peptide,” with a sequence of RLLLLRLLLLRLLLLRLLLLR, where “R” is arginine. When mixed with the phospholipids DPPC and POPG and the fatty acid palmitic acid, the resulting surfactants are called“KL4-Surfactant” and “RL4-Surfactant.” The inclusion of free palmitic acid, as well as the unsaturated acyl chain in POPG, allows for a more rapid conversion from vesicle bilayer to surface monolayer in the alveoli, resulting in increased activity both in vitro and in vivo(28). The current report presents information on the capacity of these synthetic peptide surfactants to expand the lungs of premature infant rhesus monkeys over a 24-h period. The studies have the additional advantages that they allow monitoring of the animals' clinical condition, including lung function, through blood gas analyses, as well as assessment of the degree of lung expansion by frequent radiographic examination. Additionally, pathologic examination of the lungs at necropsy provides information on the precise status of the lung parenchyma. Data were also collected which would show potential toxicity over the 24-h period, if it occurred. Reported separately, the capacity of KL4-Surfactant to induce alveolar expansion and implement normal function in human premature infants with RDS is presented(29).
METHODS
Surfactants. Synthetic peptide-containing surfactants were prepared by mixing the phospholipids DPPC and POPG in a 3:1 ratio by weight with palmitic acid, 15% by weight compared with the phospholipids in an organic solvent. DPPC, POPG, and palmitic acid were all from Avanti Polar Lipids (Birmingham, AL). The peptide was likewise dissolved in organic solvent and added to the lipid mixture. The two peptides used in the studies reported here were KL4 peptide and RL4 peptide, both 21-residue synthetic peptides (see above). Peptides were supplied by the R. W. Johnson Pharmaceutical Research Institute (La Jolla, CA) and were 3% by weight compared with phospholipid concentration. Organic solvents were removed from the lipid/peptide mixture by evaporation under nitrogen or vacuum or by dialysis. A Tris buffer solution was added to form liposomes of the peptide-containing surfactant. The final product had a pH of 7.2-7.4 and was between 250 and 350 mosmol/kg. The similar positive charge of arginine and lysine as well as previous studies(23) suggest that RL4- and KL4-Surfactants would function similarly. A phospholipid alone control liposome preparation for use in in vitro tests, was prepared identically with the omission of the peptide.
A non-peptide-containing surfactant, Exosurf Neonatal (Burroughs Wellcome Co., Research Triangle Park, NC), was reconstituted and used according to the manufacturer's directions. Each milliliter of the reconstituted surfactant contained 13.5 mg of DPPC, 1.5 mg of cetyl alcohol, and 1.0 mg of tyloxapol in 0.1 N NaCl. It was used at the recommended dosage of 5 mL/kg in the primate studies.
Natural human surfactant was isolated from term amniotic fluid as described previously(30) and used in in vitro tests.
Surface tension-lowering assay. The ability of the surfactants to lower surface tension at an air-liquid interface was measured using a pulsating bubble surfactometer as described previously(31). All samples were diluted to 10 mg/mL before assay.
Fetal monkey model. Rhesus monkeys (Macaca mulatta), delivered by cesarean section at 127-131 d of gestation (full term = 160 d), have been shown to be deficient in pulmonary surfactant(32) and thus provide a useful model for assessing the biologic activity of synthetic surfactants. All studies reported here were conducted at the California Regional Primate Research Center in Davis, CA, and were approved by the Animal Use and Care Committee at the University of California at Davis. Activities related to animal care, surgery, and necropsy were performed according to standard Primate Center operating procedures and conform to the requirements of the Animal Welfare Act and National Institutes of Health guidelines.
Pregnancies were monitored for normal fetal growth by ultrasonographic analyses until elective cesarean section at 127-131 d of gestation. At the time of delivery, the dam received ketamine as a neuroleptic agent, was intubated, and given general anesthesia using oxygen and isofluorane. The cesarean section was performed using a midline uterotomy for exposure of the fetal head and neck. The fetal trachea was exposed, and a tracheostomy performed with placement of a 2.0 inside diameter endotracheal tube with the distal tip being at the level of the mid-trachea (approximately 0.5 cm above the carina). The endotracheal tube was secured by ligature. The monkey was fully delivered after placement of the endotracheal tube, and the umbilical cord was doubly clamped and cut. The infant was taken immediately to the Primate Intensive Care Nursery, weighed, dried, and placed under a radiant warmer. Mechanical ventilation was initiated at a peak inspiratory pressure of 30-35 cm H2O, positive end expiratory pressure of 4 cm H2O, a rate of 40 breaths/min, an inspiratory time of 0.4 s, and an Fio2 of 1.0. Electrocardiographic leads and oxygen saturation probes were placed on the newborn, and the radiant warmer servo-thermal probe was placed rectally. After neuromuscular blockade with vecuronium bromide, a 3.5 Fr umbilical artery catheter was placed into the aorta. The infant was infused with 5% dextrose in water with 0.5 U/mL heparin at 120-200 mL/kg/24 h. Continuous measurements of heart rate, arterial blood pressure, oxygen saturation, and temperature were maintained throughout the experiment. Arterial blood samples were obtained at intervals of 20-60 min for blood gas analysis and pH. Mechanical ventilation and oxygen administration were adjusted to maintain a Po2 between 6.7 and 9.3 kPa (50-70 mm Hg), Pco2 between 5.3 and 6.7 kPa (40-50 mm Hg), and pH > 7.25, with infusions of sodium bicarbonate permitted for metabolic acidosis. Boluses of normal saline or heparinized fetoplacental blood or maternal blood were used for volume replacement. Chest radiographs were obtained generally within 1 h after birth and periodically thereafter during the course of the experiment. In some studies, blood samples were drawn within the 1st h and just before sacrifice for serum chemistry and blood hematology analyses. Paralysis was maintained throughout the period of the study with subsequent doses of vecuronium bromide when needed; generally two doses maintained the paralysis for 24 h.
Once RDS was established by meeting clinical and radiographic criteria (an a/A of <0.22 and diffuse, granular pulmonary radiopacity on chest radiograph), the infant monkey was dosed intratracheally with the appropriate surfactant. All doses were administered through a 3.5 Fr umbilical catheter cut to the length of the endotracheal tube and advanced through the endotracheal tube so the tip was just distal to the end of the tube. One half of the dose was administered with the animal in the right lateral decubitus position and half in the left lateral decubitus position. Ventilation was transiently paused during the 10-30 s of dose instillation. The volume of peptide surfactant was generally 5.0-5.7 mL/kg depending on the concentration of the sample and the desired dosage. Non-peptide-containing surfactant was administered at the manufacturer's suggested dose of 5.0 mL/kg.
After dosing, all animals were maintained and monitored as described above for the 8-28 h of the experiment. Euthanasia was by intravascular administration of pentobarbital. An immediate postmortem evaluation was performed with particular attention to the gross and microscopic examination of the lungs.
Treatment groups. Thirty monkeys received KL4-Surfactant. Of the 30, 24 received a “high dose” of 200 mg/kg and six received a “low dose” of 99 (n = 1) or 133(n = 5) mg/kg. Nine monkeys received 5 mL/kg of a non-peptide-containing surfactant (Exosurf Neonatal). A single monkey was treated at 28 h of age with 119 mg/kg RL4-Surfactant; data from this animal is discussed separately (see “Confirmation of fetal primate model for analysis of surfactant efficacy”).
Lung radiographic scoring of severity of RDS. Chest radiographs were scored for severity of RDS without knowledge of the time or nature of surfactant administered. The scoring system used was similar to that described by Edwards et al.(33), where a score of“1” reflects no, or very mild RDS, and a score of “5” signifies severe RDS with significant opacification of the lungs.
Lung morphometry analyses. Quantitative morphometric measurements were performed on fixed lung sections using an automated image analysis system (Microtech model 100, Analytic Imaging Concepts, Irvine, CA) using a method similar to that previously described(34). Twelve to twenty-nine areas were measured from the lungs of each of the eight animals analyzed. Fixation was in formalin under ambient air pressure.
Statistical analyses. Groups were compared using a two-group unpaired t test. Statistical difference was taken as p< 0.05.
RESULTS
In vitro biophysical activity. An initial assessment of biophysical activity was made using a bubble surfactometer to measure the ability of the peptide-containing surfactants of lower surface tension at an air/liquid interface. Table 1 shows this activity at minimal and maximal bubble radii for synthetic surfactants containing KL4- and RL4 peptides as compared with the same phospholipid mixture in the absence of the peptides. The activity of a commercial non-peptide-containing surfactant and that of natural human surfactant are also shown for comparison. It can be seen that the ability to lower surface tension, at both minimal and maximal bubble radii, of the KL4-Surfactant and the RL4-Surfactant are comparable to that of natural human surfactant and far better than that obtained with the two samples lacking protein or peptides.
Confirmation of fetal primate model for analysis of surfactant efficacy. Rhesus monkeys delivered prematurely at 127-131 d of gestation, as in the current studies, are known to lack endogenous pulmonary surfactant(32) but can often be kept alive for over 24 h with aggressive positive pressure ventilatory support(35). Their lung function, however, remains poor during the first 24-36 h of life, with mean a/A of approximately 0.12 at 24 h and approximately 0.18 at 36 h for a group of five placebo-treated monkeys being reported(35). We confirmed these historical data with a rhesus monkey of 127-131 d of gestation delivered by cesarean section and maintained on positive pressure intermittent mandatory ventilation for 28 h. During this time, blood oxygenation was monitored, and mechanical ventilation and oxygen administration were adjusted to maintain a Po2 between 6.7 and 9.3 kPa(50-70 mm Hg), Pco2 between 5.3 and 6.7 kPa (40-50 mm Hg), and pH > 7.25. The a/A was calculated at approximately 1-h intervals over this time period and found to be generally between 0.10 and 0.20 (Fig. 1). At 28.7 h of age, with an oxygen requirement of 0.81 (Fio2), the monkey received an intratracheal instillation of RL4-Surfactant at a dose of 119 mg/kg. Within 1.7 h of dosing, the a/A was noted to rise from a predosing value of 0.12 to 0.24. Lung function continued to improve over the next 6 h, and when the animal was killed at 36 h of age (7.7 h after surfactant treatment), the a/A was 0.52 and the animal was stable on room air. This experiment served to confirm that monkeys of this gestational age do not spontaneously improve their lung function during the first 24 h of life, thereby establishing this primate model as one ideal for studying the efficacy of exogenous synthetic surfactants.
The a/A for a single rhesus monkey treated at 28.7 h of age with one dose (119 mg/kg) of RL4-Surfactant. It should be noted that the a/A remained below 0.2 for most of the 28 h preceding treatment with the peptide-containing surfactant. After the bolus administration of the surfactant, the a/A rose rapidly.
Efficacy of KL4-Surfactant. Thirty fetal rhesus monkeys of 127-131 d of gestation were treated with one intratracheal bolus dose of KL4-Surfactant at an average age of 1.45 h at the time of dosing. The dose was divided equally between the right and left lungs. In all the animals, dosing was after RDS was established clinically and radiographically. The dose of KL4-Surfactant varied from 99 to 200 mg/kg, with a mean for the 30 animals of 185 mg/kg. Before and after treatment the monkeys were maintained on mechanical ventilation, with pressures, rates, and percent inspired oxygen(Fio2) varied to optimize oxygenation as dictated by the clinical condition of each animal.
All 30 monkeys receiving KL4-Surfactant improved over the 10-24-h period of the study, with the a/A partial pressure increasing from a mean value of 0.11 ± 0.01 (mean ± SEM) pretreatment to 0.40 ± 0.02 at 12-13 h posttreatment. Figure 2A shows the a/A as a function of time for the 30 animals. It should be noted that a/A values below 0.2 generally indicate the presence of severe RDS, values between 0.2 and 0.4 moderate RDS, and values ≥0.4 are considered to be in the normal range. Concomitant with the increase in a/A was a drop in the fraction of inspired oxygen (Fio2, Fig. 2B) as well as a drop in MAP (Fig. 2C). The improvement in oxygenation after the single dose of KL4-Surfactant persisted throughout the 10-24 h of the experimental time course. None of the animals, once responding, showed a deterioration of lung function; the a/A at 22-23 h was 0.45 ± 0.07. At the end of the experimental time course (10-24 h), 21/30 animals had an Fio2 of 0.21 (room air), the Pco2 averaged 4.93 kPa (37.0 mm Hg), and blood pH was within normal limits. There was no mortality in the group of 30 KL4-Surfactant-treated monkeys. At necropsy, the lungs were generally well expanded in all monkeys, often with a 1-2-mm rim of atelectasis involving pleural surface present along the lower rim of each lower lobe and, in several animals, mild scattered atelectasis was noted in the lung tissue. Microscopically, expansion of alveoli was diffuse in all KL4-Surfactant-treated animals, with small patches of atelectatic alveoli scattered in the lung fields. Figure 3 shows the microscopic appearance of a representative lung section from an animal treated with KL4-Surfactant; for comparison, a representative section of nonexpanded lung taken from a corresponding animal treated with a nonpeptide-containing surfactant (see below) is also shown. In lungs from the KL4-Surfactant-treated animals, hyaline material was present most prominently in areas of the lung not well expanded, although hyaline membranes were scattered through the lung fields. There were few to no leukocytes accumulated in the lung tissue.
The a/A (panel A), Fio2 (panel B), and the MAP (panel C), as a function of time, for 30 rhesus monkeys of 127-131 d of gestation treated with one dose of KL4-Surfactant at an average age of 1.45 h. The dose of KL4-Surfactant varied from 99 to 200 mg/kg, with a mean of 185 mg/kg. Data are expressed as the mean ± SEM.
Microscopic appearance of alveoli taken from the lungs of a rhesus monkey 5.9 h after the instillation of KL4-Surfactant(left panel). For comparison, the right-hand panel shows a comparable animal 5.9 h after receiving a non-peptide-containing surfactant. Both were fixed at ambient air pressure. Stain is hematoxylin/eosin(×150).
Assessment of chest radiographs obtained before any surfactant administration showed severe RDS in all 30 animals, with diffuse opacification of the lung fields, indistinct cardiac shadow and diaphragm margins, and prominent air bronchograms. The radiographic RDS severity score was 4.83± 0.07 (mean ± SEM) for the group before treatment. Rapid improvement in the radiographic appearance occurred within 3-5 h after KL4-Surfactant treatment. At approximately 10 h of age, the RDS scores of the treated monkeys had improved to 2.31 ± 0.13. Figure 4 shows the typical radiographic appearance of the lungs before and after treatment with KL4-Surfactant.
Chest radiographs of monkey no. 7 at 0.3(left) and 9.3 (right) h of age. This animal received 133 mg/kg of KL4-Surfactant at 3.1 h of age. The granular, hazy appearance of the lung fields and the presence of air bronchograms at 0.3 h is consistent with respiratory distress syndrome. By 9.3 h, clearing of the lung fields, with the appearance of a distinct cardiac shadow and diaphragmatic surfaces, reveals improvement in lung expansion.
Six additional fetal rhesus monkeys were given two doses of KL4-Surfactant, with the time of the second dose varying from 1 to 10 h after the first dose. The second dose averaged 139 mg/kg. The clinical response of these animals was no greater than that of those receiving a single dose (data not shown).
Low versus high dose. The monkeys received one instillation of 200 mg/kg (n = 24), 133 mg/kg (n = 5), or 99 mg/kg(n = 1) KL4-Surfactant. Separation of the efficacy data into subpopulations receiving either low dose (99-133 mg/mL with a mean of 127 mg/kg, n = 6) or high dose (all receiving 200 mg/kg, n = 24) allows a comparison of the two doses, Figure 5 shows the result of this comparison. The monkeys receiving the higher dose (200 mg/kg) responded faster, more consistently, and to a greater extent than did those receiving the lower dose (127 mg/kg). At 4-5 h of age, 14/24 (58.3%) of the high dose animals had an a/A ≥ 0.20, as compared with 1/6 (16.7%) of the low dose animals. At 20-21 h of age, 94% of the high dose but none of the low dose animals had a/A above 0.4. As shown in Figure 5A, the a/A were statistically higher in the high dose group at 6 of the 11 time points analyzed. Fio2 was comparable in the two groups until approximately 12 h of age (Fig. 5B). Required Fio2 was significantly lower (p < 0.05) in the high dose group at 14, 16, 18, 20, and 22 h after treatment. At 18 h of age, one of the three animals remaining in the low dose group necessitated a substantial increase in Fio2; the resultant rise in the mean value can be seen in the graph. MAP, although initially higher in the high dose group, was lower at all time points posttreatment than the values in the low dose group (Fig. 5C); however, statistical significance (p< 0.05) was achieved at only two of the time points.
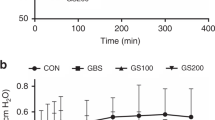
The a/A (panel A), Fio2 (panel B), and the MAP (panel C), as a function of time, for six rhesus monkeys that received a low dose (mean dose = 127 mg/kg, dotted line) and 24 animals that received a high dose (200 mg/kg, solid line) of KL4-Surfactant. Data are expressed as the mean ± SEM. The larger error bars for the later time points of the low dose animals in Panels A and B are reflective of the smaller number of data points available as well as the greater variability in the individual animals' responses to the dose. Asterisks denote those points for which there is a statistical difference (p < 0.05) between the two groups.
Peptide-containing versus non-peptide-containing surfactants. The 30 fetal monkeys treated with the peptide-containing KL4-Surfactant at a mean age of 1.45 h were compared with nine similar fetal monkeys treated with a non-peptide-containing surfactant (Exosurf) at a mean age of 2.22 h. One of the nine animals receiving the non-peptide-containing surfactant received two doses; all in the KL4-Surfactant group received a single dose. The a/A for the two groups are presented in Figure 6. Additional information reflecting the response of the monkeys to the two surfactants is given in Table 2. Clinical data were tabulated and compared at approximately 9 h of age. The mean a/A at this time point was 0.38 ± 0.02 for the KL4-Surfactant-treated animals as compared with 0.15 ± 0.03 for those receiving the non-peptide-containing surfactant (p = 0.0001). Mirroring these results, the mean Fio2 at this same time point was 0.41 ± 0.03 for the KL4-Surfactant group and 0.66 ± 0.07 for the non-peptide surfactant (p = 0.0002). The mean Pco2 for the two groups were 5.01 ± 0.21 and 8.67 ± 1.51 kPa (37.6 ± 1.6 and 65.1± 11.3 mm Hg), respectively (p = 0.0002), and the pH values of the blood at the given time points were 7.36 ± 0.01 and 7.22± 0.04 (p = 0.0001). All of these values suggest that the group treated with KL4-Surfactant had clinically improved to a greater extent than the group treated with a non-peptide-containing surfactant when the two groups were compared at approximately 9 h of age. Two (22%) of the monkeys treated with the non-peptide-containing surfactant did not survive past 9 h; all animals treated with KL4-Surfactant survived.
The responses of 30 prematurely delivered rhesus monkeys to a single dose of KL4-Surfactant (solid bars) are compared with those of nine similar monkeys treated with a non-peptide-containing surfactant (hatched bars). Plotted are the a/A pretreatment and at 5 time points after surfactant treatment. Each bar represents the mean ± SEM of all available data points within 0.5 h of the stated time. Asterisks indicate statistical difference(p < 0.05) between the two groups.
RDS severity based on analyses of chest radiographs was assessed for both groups; the data are presented in Table 2. Pretreatment scores averaged 4.83 ± 0.07 (mean ± SEM) and 5.00 ± 0 for the KL4-Surfactant and non-peptide-containing surfactant groups, respectively. Radiographs taken approximately 9 h after administration of KL4-Surfactant yielded a mean RDS severity score of 2.31 ± 0.13, whereas those taken 9 h after treatment with the non-peptide-containing surfactant averaged 4.25 ± 0.25 (p = 0.0001). Several of the animals in each group were killed at <13 h of age, and the expansion of the lungs at necropsy and microscopic alveolar expansion were assessed. Mean values are included in Table 2. Figure 3 shows the appearance of representative sections from one monkey in each group. A quantitative morphometric analysis of air space/interstitial space was also performed on the lung sections from the killed animals in each group and confirmed the gross and histologic scoring. The ratios of air space to interstitial space for the two groups were 1.06 ± 0.14 and 0.31± 0.02, respectively (p = 0.0016).
Concern that the overall earlier treatment of the group receiving KL4-Surfactant, mean time of 1.45 h as compared with a mean time of 2.22 h for the group receiving the nonpeptide-containing surfactant, might have influenced the magnitude of the differences seen prompted an analysis of a subset of the KL4-Surfactant animals having times of dosing closer to the 2.22-h dosing time of the comparison group. The results (data not shown) were very similar to those presented above; thus, the poorer response obtained with the non-peptide-containing surfactant was judged not to be due to the 46-min difference in dosing times.
Toxicity. To assess potential toxicity of KL4-Surfactant when administered to prematurely delivered rhesus monkeys, additional data were collected from 11 of the animals which received the higher dose (200 mg/kg). The animals were treated at an average age of 1.36 h. All the monkeys developed severe RDS as evidenced by low a/A levels and by opalescent densities throughout the lung fields demonstrated in radiographs. Responses to KL4-Surfactant, monitored until the animals were 19-24 h of age, occurred in all monkeys with a rise in a/A, lowered Fio2 and mean airway pressures, and clearing of the lung fields in radiographs, similar to those previously described above. There was no mortality among the 11 monkeys throughout the study period. Blood samples were taken for hematologic and biochemical analyses before administration of KL4-Surfactant and at the time of sacrifice. The data showed most values falling near or within the normal range for 127-131-d gestation infant rhesus monkeys. Creatinine and blood urea nitrogen levels rose in the 19-24-h period, reflecting a shift from maternal clearance to neonatal clearance of these substances. Glucose, albumin, and total protein levels varied with the instillation of dextrose/water and saline as part of fluid and electrolyte therapy. White blood cell counts, and in particular, neutrophils, rose moderately in all monkeys by 19-24 h, possibly as a result of the minor surgical procedures involved with the insertion of tracheal and arterial cannulas, but remained within normal limits. One of 11 animals developed elevated aspartate aminotransferase, alanine aminotransferase, and creatinine phosphokinase at 24 h.
All animals were autopsied. Samples from sixteen organs were taken for gross and microscopic examination. All organs and tissues were found to be normal by gross and microscopic analysis, with the exception of the monkey noted above with the elevated aspartate aminotransferase, alanine aminotransferase, and creatinine phosphokinase. This animal was found to have a small, single infarction in the liver. Review of its records indicated a cessation of fluid flow in the umbilical artery catheter for a period of time which may have allowed for the formation and passage into the celiac artery of a small blood clot. The lungs, in particular, aside from residual atelectasis associated with the RDS and attendent hyaline membranes, showed no evidence of injury, white cell accumulation, or vascular alterations 19-24 h after instillation of the KL4-Surfactant.
DISCUSSION
The data from this study demonstrate that a 21-residue peptide, KL4-, modeled from the pattern of SP-B, when dispersed in the phospholipids DPPC and POPG, confers surfactant activity to the phospholipids.In vitro assays using a bubble surfactometer showed the ability of KL4- and RL4-Surfactants to lower the surface tension at an air-liquid interface. In 30 premature (127-131 d of gestation) infant rhesus monkeys, treatment with KL4-Surfactant expanded the lungs and improved pulmonary function within 1-2 h of treatment. By 10-16 h after treatment, indices of pulmonary function were in the normal range. Chest radiographs showed clearing beginning 1-2 h after treatment. Gross and microscopic examination of the lungs confirmed the expansion of alveoli. The results indicate that the synthetic peptide surfactant (KL4-Surfactant) successfully expanded the pulmonary alveoli, promoting gas exchange. The expansion was maintained over the 20-24-h period of the study, indicating durability of the peptide surfactant. Such durability would be provided by both intrinsic strength of the KL4 peptide-phospholipid layer and resistance to inactivation by extrinsic plasma proteins and oxidants that may be present in the alveolar space. Strong resistance to inactivation of KL4-Surfactant by these agents has been reported(36, 37). The widespread pulmonary distribution of KL4-Surfactant in monkeys has been recorded(38). However, data are not yet available on the pharmacokinetics of KL4-Surfactant in the lungs and the potential capacity of KL4-Surfactant to stimulate intrinsic production of surfactant. Historical data, confirmed in this study, indicate that untreated premature monkeys do not spontaneously produce sufficient native surfactant to expand the alveoli within the initial 24 h of life.
Two dose levels of KL4-Surfactant were compared. Infant monkeys receiving 200 mg/kg were found to respond faster, more consistently, and to a greater extent than did those receiving a dose of approximately 127 mg/kg. It was noteworthy that the monkeys responded to a single dose of KL4-Surfactant. Providing a second dose of surfactant between 100 and 200 mg/kg did not improve the response within the first 24 h of age beyond that resulting from a single dose.
Monkeys given a non-peptide-containing surfactant, i.e. phospholipids without peptide or protein, showed little or no response, with two of nine monkeys so treated becoming moribund by 7-9 h of age. A comparison of KL4-Surfactant-treated animals with a non-peptide-containing surfactant showed a significantly better physiologic response, greater clearing of the lungs assessed radiographically, and a greater degree of alveolar expansion in the group treated with the peptide-containing surfactant. It should be noted, however, that the monkeys receiving the non-peptide-containing surfactant receiving the manufacturer's recommended dosage of 67.5 mg/kg phospholipid, whereas the KL4-Surfactant was given at a phospholipid dosage of 99, 133, or 200 mg/kg (mean = 185 mg/kg). Human clinical trials of KL4-Surfactant have used a dose of 133 or 200 mg/kg(29).
Blood chemistry and hematologic analyses performed at 19-24 h after administration of KL4-Surfactant showed no abnormal effects associated with administration of the peptide surfactant. Likewise, gross and microscopic examination of the major body organs/tissues showed no associated toxicity. In summary of the toxicity studies, there was no evidence of toxicity after treatment with 200 mg/kg KL4-Surfactant given intratracheally to premature infant rhesus monkeys as demonstrated by physiologic, hematologic, biochemical, and pathologic data.
Thus, the data in this study support the hypothesis that peptides consisting of hydrophilic basic residues that form electrostatic interactions with the phospholipid polar head groups, with intermittent stretches of hydrophobic residues that bond with the hydrophobic acyl side chains, when mixed with appropriate phospholipids can induce and maintain expansion of pulmonary alveoli over at least a 20-24-h period. The data also show that the KL4-Surfactant has no discernible toxicity associated with a dose of 200 mg/kg.
These studies establish the efficacy and safety in primates of a synthetic peptide-containing surfactant based upon an understanding of the mechanism of interaction of its lipid and peptide components. Studies, reported separately, using KL4-Surfactant in the treatment of RDS in human infants, have also shown efficacy and safety of the synthetic peptide-containing surfactant(29).
Abbreviations
- a/A:
-
ratio of arterial to alveolar oxygen tension
- DPPC:
-
dipalmitoyl-sn-glycero-3-phosphocholine
- Fio2:
-
fraction of inspired oxygen
- MAP:
-
mean airway pressure
- PG:
-
phosphatidyl glycerol
- POPG:
-
1-palmitoyl-2-oleoyl-sn-glycero-3-phosphoglycerol
- RDS:
-
respiratory distress syndrome
- SP:
-
surfactant protein
References
Yu S-H, Possmayer F 1988 Comparative studies on the biophysical activities of the low-molecular-weight hydrophobic proteins purified from bovine pulmonary surfactant. Biochim Biophys Acta 961: 337–350.
Revak SD, Merritt TA, Degryse E, Stefani L, Courtney M, Hallman M, Cochrane CG 1988 Use of human surfactant low molecular weight apoprotein in the reconstitution of surfactant biologic activity. J Clin Invest 81: 826–833.
Curstedt T, Jornvall H, Robertson B, Bergman T, Berggren P 1987 The hydrophobic low-molecular mass protein fractions of pulmonary surfactant: characterization and biophysical activity. Eur J Biochem 168: 255–262.
Sarin VK, Gupta S, Leung TK, Taylor VE, Ohning BL, Whitsett JA, Fox JL 1990 Biophysical and biological activity of a synthetic 8.7 kD hydrophobic pulmonary surfactant protein SP-B. Proc Natl Acad Sci USA 87: 2633–2637.
Nogee LM, de Mello DE, Dehner LP, Colten HR 1993 Brief report: deficiency of pulmonary surfactant protein B in congenital alveolar proteinosis. N Engl J Med 328: 406–410.
Fujita Y, Kogishi K, Suzuki Y 1988 Pulmonary damage induced in mice by a monoclonal antibody to proteins associated with pig pulmonary surfactant. Exp Lung Res 14: 247–260.
Kobayashi T, Nitta K, Takahashi R, Kurashima K, Robertson B, Suzuki Y 1991 Activity of pulmonary surfactant after blocking the associated proteins SP-A and SP-B. J Appl Physiol 71: 530–536.
Robertson B, Kobayashi T, Ganzuka M, Grossmann G, Li WZ, Suzuki Y 1991 Experimental neonatal respiratory failure induced by a monoclonal antibody to the hydrophobic surfactant-associated protein SP-B. Pediatr Res 30: 239–243.
Hawgood S, Benson JB, Schilling J, Damm D, Clements JA, White RT 1987 Nucleotide and amino acid sequences of pulmonary surfactant protein SP18. Proc Natl Acad Sci USA 84: 66–70.
Glasser SW, Korfhagen TR, Weaver T, Pilot-Matias T, Fox JL, Whitsett JA 1987 cDNA and deduced amino acid sequence of pulmonary surfactant-associated proteolipid SPL (Phe). Proc Natl Acad Sci USA 84: 4007–4011.
Curstedt T, Johansson J, Barros-Soderling J, Robertson B, Nilsson G, Westberg M, Jornvall H 1988 Low-molecular-mass surfactant protein type 1: the primary structure of a hydrophobic 8-kDa polypeptide with eight half-cystine residues. Eur J Biochem 172: 521–525.
Olafson RW, Rink U, Kielland S, Yu SH, Chung J, Harding PG, Possmayer F 1987 Protein sequence analysis studies on the low molecular weight hydrophobic proteins associated with bovine pulmonary surfactant. Biochem Biophys Res Commun 148: 1406–1411.
Yu S-H, Possmayer F 1986 Reconstitution of surfactant activity by using 6 kDa apoprotein associated with pulmonary surfactant. Biochem J 236: 85–89.
Whitsett JA, Ohning BL, Ross G, Meuth J, Weaver T, Holm BA, Shapiro DL, Notter RH 1986 Hydrophobic surfactant-associated protein in whole lung surfactant and its importance for biophysical activity in lung surfactant extracts used for replacement therapy. Pediatr Res 20: 460–467.
Benson B, Hawgood S, Schilling J, Clements J, Damm D, Cordell B, White RT 1985 Structure of canine pulmonary surfactant apoprotein cDNA and complete amino acid sequence. Proc Natl Acad Sci USA 82: 6379–6383.
Emrie PA, Shannon JM, Mason RJ, Fisher JH 1989 cDNA and deduced amino acid sequence for the rat hydrophobic pulmonary surfactant-associated protein, SP-B. Biochim Biophys Acta 994: 215–221.
Jacobs KA, Phelps DS, Steinbrink R, Fisch J, Kriz R, Mitsock L, Dougherty JP, Taeusch HW, Flores J 1987 Isolation of a cDNA clone encoding a high molecular weight precurser to a 6-kDa pulmonary surfactant-associated protein. J Biol Chem 262: 9808–9811.
Revak SD, Merritt TA, Hallman M, Heldt G, La Polla RJ, Hoey K, Houghten RA, Cochrane CG 1991 The use of synthetic peptides in the formation of biophysically and biologically active pulmonary surfactants. Pediatr Res 29: 460–465.
Waring A, Taeusch W, Bruni R, Amirkhanian J, Fan B, Stevens R, Young J 1989 Synthetic amphipathic sequences of surfactant protein-B mimic several physicochemical and in vivo properties of native pulmonary surfactant proteins. Peptide Res 2: 308–313.
McLean LR, Krstenansky JL, Jackson RL, Hagaman KA, Olsen KF, Lewis JE 1992 Mixtures of synthetic peptides and dipalmitoylphosphatidylcholine as lung surfactants. Am J Physiol 262:L292–L300.
McLean LR, Lewis JE, Krstenansky JL, Hagaman KA, Cope AS, Olsen KF, Matthews ER, Uhrhammer DC, Owen TJ, Payne MH 1993 An Amphipathic -helical decapeptide in phosphatidylcholine is an effective synthetic lung surfactant. Am Rev Respir Dis 147: 462–465.
Cochrane CG, Revak SD 1990 Surfactant protein SP-B. Pediatr Res 27: 297A (abstr)
Cochrane CG, Revak SD 1991 Pulmonary surfactant protein B (SP-B): structure-function relationships. Science 254: 566–568.
Vandenbussche G, Clercx A, Clercx M, Curstedt T, Johansson J, Jornvall H, Ruysschaert JM 1992 Secondary structure and orientation of the surfactant protein SP-B in a lipid environment. A Fourier transform infrared spectroscopy study. Biochemistry 31: 9169–9176.
Vincent JS, Revak SD, Cochrane CG, Levin IW 1991 Raman spectroscopic studies of model human pulmonary surfactant systems: phospholipid interactions with peptide paradigms for the surfactant protein SP-B. Biochemistry 30: 8395–8401.
Baatz JE, Elledge B, Whitsett JA 1990 Surfactant protein SP-B induces ordering at the surface of model membrane bilayers. Biochemistry 29: 6714–6720.
Bruni R, Taeusch HW, Waring AJ 1991 Surfactant protein B: lipid interactions of synthetic peptides representing the amino-terminal amphipathic domain. Proc Natl Acad Sci USA 88: 7451–7455.
Tanaka Y, Takei T, Aiba T, Masuda K, Kiuchi A, Fujiwara T 1986 Development of synthetic lung surfactants. J Lipid Res 27: 475–485.
Cochrane CG, Revak SD, Merritt TA, Heldt GP, Hallman M, Cunningham MD, Easa D, Pramanik A, Edwards DK, Alberts MS 1996 The efficacy and safety of KL4-Surfactant in preterm infants with RDS. Am J Respir Crit Care Med 153: 404–410.
Hallman M, Merritt TA, Schneider H, Epstein BL, Mannino F, Edwards DK, Gluck L 1983 Isolation of human surfactant from amniotic fluid and a pilot study of its efficacy in respiratory distress syndrome. Pediatrics 71: 473–482.
Revak SD, Merritt TA, Hallman M, Cochrane CG 1986 Reconstitution of surfactant activity using purified human apoprotein and phospholipids measured in vitro and in vivo. Am Rev Respir Dis 134: 1258–1265.
Epstein NE, Farrell PM, Chez RA 1976 Fetal lung lecithin metabolism and the amniotic fluid L/S ratio in rhesus monkey gestations. Am J Obstet Gynecol 125: 545–549.
Edwards DK, Hilton SvW, Merritt TA, Hallman M, Mannino F, Boynton F 1985 Respiratory distress syndrome treated with human surfactant: radiographic findings. Radiology 157: 329–334.
Harker LC, Kirkpatrick SE, Friedman WF, Bloor CM 1981 Effects of indomethacin on fetal rat lungs: a possible cause of persistent fetal circulation (PFC). Pediatr Res 15: 147–151.
Goetzman BW, Read LC, Plopper CG, Tarantal AF, George-Nascimento C, Merritt TA, Whitsett JA, Styne D 1994 Prenatal exposure to epidermal growth factor attenuates respiratory distress syndrome in rhesus infants. Pediatr Res 35: 30–36.
Merritt TA, Amirkhanian JD, Helbock H, Halliwell B, Cross CE 1993 Reduction of the surface-tension-lowering ability of surfactant after exposure to hypochlorous acid. Biochem J 295: 19–22.
Amirkhanian JD, Kheiter A, Merritt TA 1994 Comparative Evaluation of Reduction in surface-tension lowering ability of Survanta and KL4-Surfactant by some serum components. Pediatr Res 35: 324A
Merritt TA, Kheiter A, Cochrane C 1995 Positive end expiratory pressure during instillation enhances distribution of exogenous KL4-Surfactant in Simian respiratory distress syndrome. Pediatr Res 38: 211–217.
Acknowledgements
The authors are grateful to Kenway Hoey, Tom Madden, and Pete Glavinos for preparation of synthetic peptides and many of the batches of peptide containing surfactant. We thank Dr. Colin Bloor for the morphometric analyses of lung histologic sections. We also thank Sarah Davis and the staff of the California Regional Primate Research Center in Davis, CA, without whose expert assistance these studies could not have been performed.
Author information
Authors and Affiliations
Additional information
Supported by Grant HL-23584 from the Public Health Service, Grant N00014 from the Office of Naval Research, Primate Research Center Grant National Institutes of Health RR00169, and by the R. W. Johnson Pharmaceutical Research Institute.This is publication number 9057-IMM from the Department of Immunology, The Scripps Research Institute.
Rights and permissions
About this article
Cite this article
Revak, S., Merritt, T., Cochrane, C. et al. Efficacy of Synthetic Peptide-Containing Surfactant in the Treatment of Respiratory Distress Syndrome in Preterm Infant Rhesus Monkeys. Pediatr Res 39, 715–724 (1996). https://doi.org/10.1203/00006450-199604000-00025
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/00006450-199604000-00025
This article is cited by
-
Evolution of surfactant therapy for respiratory distress syndrome: past, present, and future
Pediatric Research (2017)
-
Synthetic surfactants: where are we? Evidence from randomized, controlled clinical trials
Journal of Perinatology (2009)
-
Prognose extrem unreifer Frühgeborener
Monatsschrift Kinderheilkunde (2005)