Abstract
Background:
To investigate the impact of body mass index (BMI) on tumor characteristics and biochemical recurrence (BCR) after radical prostatectomy (RP) for prostate cancer (PCa) in Japanese men.
Methods:
We evaluated data from consecutive patients who had undergone RP. Data analyzed included age, preoperative serum PSA, prostatic volume, BMI (continuous or categorized (⩽25 kg/m2) values), clinical and pathological findings including index tumor volume (ITV), and current status in areas such as smoker or nonsmoker and presence or absence of diabetes. We analyzed association between BMI and BCR, especially based on ITV using univariate and multivariate analysis.
Results:
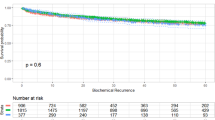
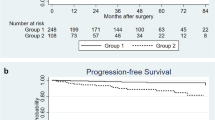
We analyzed data from a total of 703 patients. The median follow-up time was 38.4 months. BCR was diagnosed in 154 patients (21.9%) at a median of 9.7 months postoperatively. Multivariate linear regression analysis adjusted for preoperative variables showed a significant positive association between BMI and ITV (continuous BMI: P=0.002; categorical BMI: P<0.001, respectively), especially for higher-grade tumors (Gleason score ⩾ 7). Cox proportional hazards analysis showed a significant association between continuous BMI and BCR after surgery (preoperative variables, hazard ratio (HR) 1.09, 95% confidence interval (CI) 1.02–1.16, P=0.008), independent of clinical and pathological findings. In patients with high-risk cancer, the positive association between BMI and BCR was strengthened (preoperative variables, continuous BMI, HR 1.16, 95% CI 1.07–1.26, P<0.001; categorical BMI, HR 2.11, 95% CI 1.29–3.45, P=0.003, respectively).
Conclusions:
Greater BMI significantly correlates with higher rates of BCR after surgery; BMI is a preoperative variable associated with high-grade ITV. Our results suggest that the biological environment created by greater BMI may contribute to increasing tumor aggressiveness.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 4 print issues and online access
$259.00 per year
only $64.75 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Calle EE, Rodriguez C, Walker-Thurmond K, Thun MJ . Overweight, obesity, and mortality from cancer in a prospectively studied cohort of U.S. adults. N Engl J Med 2003; 348: 1625–1638.
Okayasu M, Takahashi H, Furusato B, Egawa S . Comparison of latent prostate cancer detected at autopsy between pre-and post-prostatic specific antigen (PSA) era. Mod Pathol 2012; 25: 231A.
Kadota A, Miura K, Ueshima H . [The trend of metabolic syndrome in Japanese National Health and Nutrition Survey]. Nihon Rinsho 2011; 69 (Suppl 1): 35–39.
Cullen J, Elsamanoudi S, Brassell SA, Chen Y, Colombo M, Srivastava A et al. The burden of prostate cancer in Asian nations. J Carcinog 2012; 11: 7.
Albertsen PC . What is the risk posed by prostate cancer? J Natl Cancer Inst Monogr 2012; 2012: 169–174.
Raldow A, Hamstra DA, Kim SN, Yu JB . Adjuvant radiotherapy after radical prostatectomy: evidence and analysis. Cancer Treat Rev 2011; 37: 89–96.
Hayashi N, Urashima M, Ikemoto I, Kuruma H, Arai Y, Kuwao S et al. Prostate-specific antigen adjusted for total prostatic tumor volume as a predictor for outcome after radical prostatectomy. Prostate Cancer Prostatic Dis 2007; 10: 60–65.
Freedman JE, Larson MG, Tanriverdi K, O'Donnell CJ, Morin K, Hakanson AS et al. Relation of platelet and leukocyte inflammatory transcripts to body mass index in the Framingham heart study. Circulation 2010; 122: 119–129.
Kanahara (ed.) General Rule for Clinical and Pathological Studies on Prostatic Cancer 3 edn. Japanese Urological Association and Japanese Pathological Society: Tokyo, 2001.
Sbin L, W. C ed UICC International Union Against Cancer 2002; Wiley-Liss: New York.
D'Amico AV, Whittington R, Malkowicz SB, Schultz D, Blank K, Broderick GA et al. Biochemical outcome after radical prostatectomy, external beam radiation therapy, or interstitial radiation therapy for clinically localized prostate cancer. JAMA 1998; 280: 969–974.
Amling CL, Riffenburgh RH, Sun L, Moul JW, Lance RS, Kusuda L et al. Pathologic variables and recurrence rates as related to obesity and race in men with prostate cancer undergoing radical prostatectomy. J Clin Oncol 2004; 22: 439–445.
Freedland SJ, Aronson WJ, Kane CJ, Presti JC Jr, Amling CL, Elashoff D et al. Impact of obesity on biochemical control after radical prostatectomy for clinically localized prostate cancer: a report by the Shared Equal Access Regional Cancer Hospital database study group. J Clin Oncol 2004; 22: 446–453.
Freedland SJ, Isaacs WB, Mangold LA, Yiu SK, Grubb KA, Partin AW et al. Stronger association between obesity and biochemical progression after radical prostatectomy among men treated in the last 10 years. Clin Cancer Res 2005; 11: 2883–2888.
Freedland SJ, Terris MK, Presti JC Jr., Amling CL, Kane CJ, Trock B et al. Obesity and biochemical outcome following radical prostatectomy for organ confined disease with negative surgical margins. J Urol 2004; 172: 520–524.
Jayachandran J, Banez LL, Aronson WJ, Terris MK, Presti JC Jr, Amling CL et al. Obesity as a predictor of adverse outcome across black and white race: results from the Shared Equal Access Regional Cancer Hospital (SEARCH) Database. Cancer 2009; 115: 5263–5271.
Wilson KM, Giovannucci EL, Mucci LA . Lifestyle and dietary factors in the prevention of lethal prostate cancer. Asian J Androl 2012; 14: 365–374.
Nutrition NIoHa. Section of the National Health and Nutrition Survey. National Insutitute of Health and Nutrition.
Ma J, Li H, Giovannucci E, Mucci L, Qiu W, Nguyen PL et al. Prediagnostic body-mass index, plasma C-peptide concentration, and prostate cancer-specific mortality in men with prostate cancer: a long-term survival analysis. Lancet Oncol 2008; 9: 1039–1047.
Rowlands MA, Holly JM, Gunnell D, Gilbert R, Donovan J, Lane JA et al. The relation between adiposity throughout the life course and variation in IGFs and IGFBPs: evidence from the ProtecT (Prostate testing for cancer and Treatment) study. Cancer Causes Control 2010; 21: 1829–1842.
Keto CJ, Aronson WJ, Terris MK, Presti JC, Kane CJ, Amling CL et al. Obesity is associated with castration-resistant disease and metastasis in men treated with androgen deprivation therapy after radical prostatectomy: results from the SEARCH database. BJU Int 2012; 110: 492–498.
Capitanio U, Suardi N, Briganti A, Gallina A, Abdollah F, Lughezzani G et al. Influence of obesity on tumour volume in patients with prostate cancer. BJU Int 2012; 109: 678–684.
Freedland SJ, Banez LL, Sun LL, Fitzsimons NJ, Moul JW . Obese men have higher-grade and larger tumors: an analysis of the duke prostate center database. Prostate Cancer Prostatic Diseases 2009; 12: 259–263.
Hayashi N, Matsushima M, Yamamoto T, Sasaki H, Takahashi H, Egawa S . The impact of hypertriglyceridemia on prostate cancer development in patients aged >/=60 years. BJU Int 2012; 109: 515–519.
Lee DJ, Ritch C, Desai M, Benson MC, McKiernan JM . The interaction of body mass index and race in predicting biochemical failure after radical prostatectomy. BJU Int 2011; 107: 1741–1747.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Hayashi, N., Matsushima, M., Kido, M. et al. BMI is associated with larger index tumors and worse outcome after radical prostatectomy. Prostate Cancer Prostatic Dis 17, 233–237 (2014). https://doi.org/10.1038/pcan.2014.15
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/pcan.2014.15
This article is cited by
-
Obesity and biochemical recurrence in clinically localised prostate cancer: a systematic review and meta-analysis of 86,490 patients
Prostate Cancer and Prostatic Diseases (2022)
-
Body mass index is associated with higher Gleason score and biochemical recurrence risk following radical prostatectomy in Chinese men: a retrospective cohort study and meta-analysis
World Journal of Surgical Oncology (2015)