Key Points
-
Intradiverticular bladder tumours (IDBT) are rare, accounting for approximately 1% of all bladder tumours; the true prevalence of bladder diverticula is not known as most are asymptomatic
-
Urine cytology, ultrasonography, and cystoscopy should be used in the initial assessment of a suspected IDBT; cross-sectional imaging can complement these techniques, and is also important in staging
-
Bladder-conserving treatments including transurethral resection, diverticulectomy, or partial cystectomy with or without intravesical adjuvant therapy can be used in patients with low-grade, low-volume, noninvasive disease
-
Radical cystectomy, with or without systemic neoadjuvant or adjuvant therapy, is required for patients with large, invasive tumours, or tumours that are associated with poor bladder function (chronic retention)
-
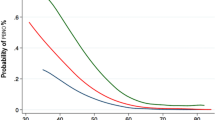
5-year survival rates of 72% and 45% have been reported for patients with IDBT and, specifically, T3 IDBTs, respectively; these rates are comparable to those for intravesical bladder cancer
Abstract
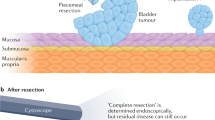
Intradiverticular bladder tumours (IDBT) account for approximately 1% of all urinary bladder tumours. The risk of developing a tumour within a bladder diverticulum is considered to be greater than in the main bladder, possibly owing to prolonged contact of potential carcinogens with the mucosal lining from urinary stasis. Patients with these tumours most commonly present with visible haematuria. Diagnostic tests include urine cytology, cystoscopy, ultrasonography, CT, MRI, and biopsy. Lack of muscle in the diverticula increases the risk of bladder perforation during biopsy and makes pathological staging difficult as there is no T2 stage; instead, data suggest that any invasion beyond the lamina propria should be described as T3. IDBT can be managed by transurethral resection and adjuvant intravesical therapy, diverticulectomy, or cystectomy (partial or radical), as outlined by the only guidelines to specifically address the management of IDBT, which were published by the Cancer Committee of the French Association of Urology (CCAFU) in 2012. The prognosis of patients with intradiverticular bladder tumours has always been perceived to be worse than those with intravesical tumours; however, the only study of 5-year survival rates for patients with IDBT suggests that prognosis might be comparable for these conditions.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Kong, M. X. et al. Histopathologic and clinical features of vesical diverticula. Urology 82, 142–147 (2013).
Tamas, E. F. et al. Histopathologic features and clinical outcomes in 71 cases of bladder diverticula. Arch. Pathol. Lab. Med. 133, 791–796 (2009).
Wein, A. J., Kavoussi, L. R., Novick, A. C., Partin, A. W. & Peters, C. A. Campbell-Walsh Urology 10th edn (Elsevier Health Sciences, 2011).
Melekos, M. D., Asbach, H. W. & Barbalias, G. A. Vesical diverticula: aetiology, diagnosis, tumorigenesis, and treatment. Analysis of 74 cases. Urology 30, 453–457 (1987).
Whitefield, B. Urinary bladder diverticulum and its association with malignancy: an anatomical study on cadavers. Rom. J. Morphol. Embryol. 51, 543–545 (2010).
Idrees, M. T., Alexander, R. E., Kum, J. B. & Cheng, L. The spectrum of histopathologic findings in vesical diverticulum: implications for pathogenesis and staging. Hum. Pathol. 44, 1223–1232 (2013).
Viana, R. et al. The development of the bladder trigone, the centre of the anti-reflux mechanism. Development 134, 3763–3769 (2007).
Yucel, S. & Baskin, L. S. An anatomical description of the male and female urethral sphincter complex. J. Urol. 171, 1890–1897 (2004).
Stage, K. H. K. & Tank, E. S. E. Primary congenital bladder diverticula in boys. Urology 40, 536–538 (1992).
Sarihan, H. H. & Abes, M. M. Congenital bladder diverticula in infants. Eur. Urol. 33, 101–103 (1998).
Evangelidis, A. et al. Surgical management of primary bladder diverticula in children. J. Paediatr. Surg. 40, 701–703 (2005).
Hutch, J. A. J. Saccule formation at the ureterovesical junction in smooth walled bladders. J. Urol. 86, 390–399 (1961).
Golijanin, D., Yossepowitch, O., Beck, S. D., Sogani, P. & Dalbagni, G. Carcinoma in a bladder diverticulum: presentation and treatment outcome. J. Urol. 170, 1761–1764 (2003).
Baniel, J. & Vishna, T. Primary transitional cell carcinoma in vesical diverticula. Urology 50, 697–699 (1997).
Childs, M. A. et al. Pathogenesis of bladder calculi in the presence of urinary stasis. J. Urol. 189, 1347–1351 (2013).
Vecchioli Scaldazza, C. Incidence of urothelial carcinoma of the bladder in males with chronic urinary retention. Arch. Esp. Urol. 45, 523–525 (1992).
Burger, M. et al. Epidemiology and risk factors of urothelial bladder cancer. Eur. Urol. 63, 234–241 (2013).
Das, S. S. & Amar, A. D. A. Vesical diverticulum associated with bladder carcinoma: therapeutic implications. J. Urol. 136, 1013–1014 (1986).
Mic´ic´, S. & Ilic´, V. Incidence of neoplasm in vesical diverticula. J. Urol. 129, 734–735 (1983).
Neuzillet, Y. et al. Intradiverticular bladder tumours: review of the Cancer Committee of the French Association of Urology. Prog. Urol. 22, 495–502 (2012).
Babjuk, M. et al. EAU guidelines on non-muscle-invasive urothelial carcinoma of the bladder: update Eur. Urol. 64, 639–653 (2013).
Stenzl, A. et al. Treatment of muscle-invasive and metastatic bladder cancer: update of the EAU guidelines. Eur. Urol. 59, 1009–1018 (2011).
Lokeshwar, V. B. et al. Bladder tumour markers beyond cytology: International Consensus Panel on bladder tumour markers. Urology 66, 35–63 (2005).
Raitanen M.-P. et al. Differences between local and review urinary cytology in diagnosis of bladder cancer. An interobserver multicentre analysis. Eur. Urol. 41, 284–289 (2002).
Haecker, A., Riedasch, G., Langbein, S., Alken, P. & Michel, M. S. Diverticular carcinoma of the urinary bladder: diagnosis and treatment problems. A case report. Med. Princ. Pract. 14, 121–124 (2005).
Knappenberger, S. T., Uson, A. C. & Melicow, M. M. Primary neoplasms occurring in vesical diverticula: a report of 18 cases. J. Urol. 83, 153–159 (1960).
Fekak, H. et al. Intradiverticular bladder tumours. Three case reports. Ann. Urol. (Paris) 36, 53–57 (2002).
Durfee, S. M., Schwartz, L. H., Panicek, D. M. & Russo, P. MR imaging of carcinoma within urinary bladder diverticulum. Clin. Imag. 21, 290–292 (1997).
Dondalski, M., White, E. M., Ghahremani, G. G. & Patel, S. K. Carcinoma arising in urinary bladder diverticula: imaging findings in six patients. AJR Am. J. Roentgenol. 161, 817–820 (1993).
Croitoru, S., Moskovitz, B., Nativ, O., Barmeir, E. & Hiller, N. Diagnostic potential of virtual pneumoendoscopy of the urinary tract. Abdom. Imag. 33, 717–723 (2008).
Khan, M. S., Thornhill, J. A., Gaffney, E., Loftus, B. & Butler, M. R. Keratinising squamous metaplasia of the bladder: natural history and rationalization of management based on review of 54 years experience. Eur. Urol. 42, 469–474 (2002).
Garzotto, M. G., Tewari, A. & Wajsman, Z. Multimodal therapy for neoplasms arising from a vesical diverticulum. J. Surg. Oncol. 62, 46–48 (1996).
Montague, D. K. & Boltuch, R. L. Primary neoplasms in vesical diverticula: report of 10 cases. J. Urol. 116, 41–42 (1976).
Redman, J. F., McGinnis, T. B. & Bissada, N. K. Management of neoplasms in vesical diverticula. Urology 7, 492–494 (1976).
Raheem, O. A., Besharatian, B. & Hickey, D. P. Surgical management of bladder transitional cell carcinoma in a vesicular diverticulum: case report. Can. Urol. Assoc. J. 5, E60–E64 (2011).
Brausi, M. et al. Variability in the recurrence rate at first follow-up cystoscopy after TUR in stage Ta T1 transitional cell carcinoma of the bladder: a combined analysis of seven EORTC studies. Eur. Urol. 41, 523–531 (2002).
Brausi, M. Transurethral resection of bladder cancer: a simple and diffusely-performed technique but with controversial outcomes. Urologia 80, 127–129 (2013).
Mariappan, P., Zachou, A. & Grigor, K. M. Edinburgh Uro-Oncology Group. Detrusor muscle in the first, apparently complete transurethral resection of bladder tumour specimen is a surrogate marker of resection quality, predicts risk of early recurrence, and is dependent on operator experience. Eur. Urol. 57, 843–849 (2010).
Balbay, M. D. et al. The actual incidence of bladder perforation following transurethral bladder surgery. J. Urol. 174, 2260–2263 (2005).
Herkommer, K., Hofer, C., Gschwend, J. E., Kron, M. & Treiber, U. Gender and body mass index as risk factors for bladder perforation during primary transurethral resection of bladder tumours. J. Urol. 187, 1566–1570 (2012).
Gan, C. et al. Snapshot of transurethral resection of bladder tumours in the United Kingdom Audit (STUKA). BJU Int. 112, 930–935 (2013).
Skolarikos, A. et al. Does the management of bladder perforation during transurethral resection of superficial bladder tumours predispose to extravesical tumour recurrence? J. Urol. 173, 1908–1911 (2005).
Golan, S., Baniel, J., Lask, D., Livne, P. M. & Yossepowitch, O. Transurethral resection of bladder tumour complicated by perforation requiring open surgical repair—clinical characteristics and oncological outcomes. BJU Int. 107, 1065–1068 (2011).
Collado, A., Chéchile, G. E., Salvador, J. & Vicente, J. Early complications of endoscopic treatment for superficial bladder tumours. J. Urol. 164, 1529–1532 (2000).
Thomas, K. & O'Brien, T. Improving transurethral resection of bladder tumour: the gold standard for diagnosis and treatment of bladder tumours. Eur. Urol. 7, 524–528 (2008).
Traxer, O., Pasqui, F., Gattegno, B. & Pearle, M. S. Technique and complications of transurethral surgery for bladder tumours. BJU Int. 94, 492–496 (2004).
Myer, E. G. & Wagner, J. R. Robotic assisted laparoscopic bladder diverticulectomy. J. Urol. 178, 2406–2410 (2007).
Thüroff, J. W., Roos, F. C., Thomas, C., Kamal, M. M. & Hampel, C. Surgery illustrated-surgical atlas: robot-assisted laparoscopic bladder diverticulectomy. BJU Int. 110, 1820–1836 (2012).
Porpiglia, F. et al. Is laparoscopic bladder diverticulectomy after transurethral resection of the prostate safe and effective? Comparison with open surgery. J. Endourol. 18, 73–76 (2004).
Magera, J. S. Jr, Adam Childs, M. & Frank, I. Robot-assisted laparoscopic transvesical diverticulectomy and simple prostatectomy. J. Robotic Surg. Springer-Verlag 2, 205–208 (2008).
Eyraud, R. et al. Robot-assisted laparoscopic bladder diverticulectomy. Curr. Urol. Rep. 14, 46–51 (2013).
Sullivan, J. W., Grabstald, H. & Whitmore, W. F. Complications of ureteroileal conduit with radical cystectomy: review of 336 cases. J. Urol. 124, 797–801 (1980).
Thomas, D. M. & Riddle, P. R. Morbidity and mortality in 100 consecutive radical cystectomies. Br. J. Urol. 54, 716–719 (1982).
Skinner, D. G., Crawford, E. D. & Kaufman, J. J. Complications of radical cystectomy for carcinoma of the bladder. J. Urol. 123, 640–643 (1980).
Johnson, D. E. & Lamy, S. M. Complications of a single stage radical cystectomy and ileal conduit diversion: review of 214 cases. J. Urol. 117, 171–173 (1977).
Charbit, L., Beurton, D. & Cukier, J. Mortalité et morbidité après cystectomie totale pour cancer. J. Urol. (Paris) 90, 39–46 (1984).
Boström, P. J., Kössi, J., Laato, M. & Nurmi, M. Risk factors for mortality and morbidity related to radical cystectomy. BJU Int. 103, 191–196 (2009).
Lawrentschuk, N. et al. Prevention and management of complications following radical cystectomy for bladder cancer. Eur. Urol. 57, 983–1001 (2010).
McCabe, J. E., Jibawi, A. & Javle, P. M. Radical cystectomy: defining the threshold for a surgeon to achieve optimum outcomes. Postgrad. Med. J. 83, 556–560 (2007).
Fairey, A. et al. Associations among age, comorbidity and clinical outcomes after radical cystectomy: results from the Alberta Urology Institute radical cystectomy database. J. Urol. 180, 128–134 (2008).
Corica, F. A. et al. Intestinal metaplasia is not a strong risk factor for bladder cancer: study of 53 cases with long-term follow-up. Urology 50, 427–431 (1997).
Smith, A. K., Hansel, D. E. & Jones, J. S. Role of cystitis cystica et glandularis and intestinal metaplasia in development of bladder carcinoma. Urology 71, 915–918 (2008).
Faysal, M. H. & Freiha, F. S. Primary neoplasm in vesical diverticula. A report of 12 cases. Br. J. Urol. 53, 141–143 (1981).
Boylan, R. N., Greene, L. F. & Mcdonald, J. R. Epithelial neoplasms arising in diverticula of the urinary bladder. J. Urol. 65, 1041–1049 (1951).
Kelalis, P. P. & McLean, P. The treatment of diverticulum of the bladder. J. Urol. 98, 349–352 (1967).
American Cancer Society. Cancer Treatment and Survivorship Facts & Figures 2012–2013 [online], (2013).
Shipley, W. U. et al. Selective bladder preservation by combined modality protocol treatment: long-term outcomes of 190 patients with invasive bladder cancer. Urology 60, 62–67 (2002).
Author information
Authors and Affiliations
Contributions
All authors made substantial contributions towards writing, editing, reviewing, and discussing the manuscript with colleagues. N.F.W. researched the literature for this article.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
PowerPoint slides
Rights and permissions
About this article
Cite this article
Walker, N., Gan, C., Olsburgh, J. et al. Diagnosis and management of intradiverticular bladder tumours. Nat Rev Urol 11, 383–390 (2014). https://doi.org/10.1038/nrurol.2014.131
Published:
Issue Date:
DOI: https://doi.org/10.1038/nrurol.2014.131
This article is cited by
-
Updated pathology reporting standards for bladder cancer: biopsies, transurethral resections and radical cystectomies
World Journal of Urology (2022)
-
Cancer risk in bladder diverticula: a large institutional analysis of risk and management
International Urology and Nephrology (2022)
-
Imaging spectrum of common and rare infections affecting the lower genitourinary tract
Abdominal Radiology (2021)
-
Dataset for the reporting of carcinoma of the bladder—cystectomy, cystoprostatectomy and diverticulectomy specimens: recommendations from the International Collaboration on Cancer Reporting (ICCR)
Virchows Archiv (2020)
-
Imaging of non-traumatic urinary bladder emergencies
Emergency Radiology (2019)