Key Points
-
Most patients with faecal incontinence are managed with conservative measures and biofeedback techniques
-
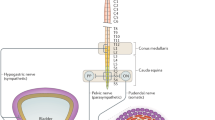
Sacral nerve stimulation has dramatically changed the management of patients with faecal incontinence who do not respond to conservative measures
-
Sacral nerve stimulation is a minimally invasive procedure with low morbidity and good medium-term to long-term results; a test period of stimulation enables identification of those patients likely to benefit
-
Creation of a neosphincter can be performed with either muscle (dynamic graciloplasty) or an artificial device (artificial bowel sphincter)
-
Both neosphincter techniques are associated with substantial morbidity and reoperation rates, although new devices (for example the magnetic anal sphincter) have been developed and are currently under assessment
-
Injection of bulking agents into the anal canal or sphincter complex offers good results for patients with mild-to-moderate symptoms or predominantly passive faecal incontinence
Abstract
Faecal incontinence is a common condition and is associated with considerable morbidity and economic cost. The majority of patients are managed with conservative interventions. However, for those patients with severe or refractory incontinence, surgical treatment might be required. Over the past 20 years, numerous developments have been made in the surgical therapies available to treat such patients. These surgical therapies can be classified as techniques of neuromodulation, neosphincter creation (muscle or artificial) and injection therapy. Techniques of neuromodulation, particularly sacral nerve stimulation, have transformed the management of these patients with a minimally invasive procedure that offers good results and low morbidity. By contrast, neosphincter procedures are characterized by being more invasive and associated with considerable morbidity, although some patients will experience substantial improvements in their continence. Injection of bulking agents into the anal canal can improve symptoms and quality of life in patients with mild-to-moderate incontinence, and the use of autologous myoblasts might be a future therapy. Further research and development is required not only in terms of the devices and procedures, but also to identify which patients are likely to benefit most from such interventions.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Nelson, R., Norton, N., Cautley, E. & Furner, S. Community-based prevalence of anal incontinence. JAMA 274, 559–561 (1995).
Perry, S. et al. Prevalence of faecal incontinence in adults aged 40 years or more living in the community. Gut 50, 480–484 (2002).
Nelson, R., Furner, S. & Jesudason, V. Fecal incontinence in Wisconsin nursing homes: prevalence and associations. Dis. Colon Rectum 41, 1226–1229 (1998).
NICE. NICE clinical guideline 49. Faecal incontince: the management of faecal incontinence in adults. NICE [online]
Read, M., Read, N. W., Barber, D. C. & Duthie, H. L. Effects of loperamide on anal sphincter function in patients complaining of chronic diarrhea with fecal incontinence and urgency. Dig. Dis. Sci. 27, 807–814 (1982).
Brown, S. R., Wadhawan, H. & Nelson, R. L. Surgery for faecal incontinence in adults. Cochrane Database of Systematic Reviews. Issue 7. Art. no.: CD001757 http://dx.doi.org/10.1002.14651858.CD001757.pub4.
Fang, D. T. et al. Overlapping sphincteroplasty for acquired anal incontinence. Dis. Colon Rectum 27, 720–722 (1984).
Oliveira, L., Pfeifer, J. & Wexner, S. D. Physiological and clinical outcome of anterior sphincteroplasty. Br. J. Surg. 83, 502–505 (1996).
Brown, S. R. in Contemporary Coloproctology (eds Brown, S. R., Hartley, J. E., Hill, J. Scott, N. & Williams, J. G.) 369–387 (Springer-Verlag, 2012).
Gladman, M. A., Scott, S. M., Lunniss, P. J. & Williams, N. S. Systematic review of surgical options for idiopathic megarectum and megacolon. Ann. Surg. 241, 562–574 (2005).
D'Hoore, A., Cadoni, R. & Penninckx, F. Long-term outcome of laparoscopic ventral rectopexy for total rectal prolapse. Br. J. Surg. 91, 1500–1505 (2004).
Matzel, K. E., Stadelmaier, U., Hohenfellner, M. & Gall, F. P. Electrical stimulation of sacral spinal nerves for treatment of faecal incontinence. Lancet 346, 1124–1127 (1995).
Gourcerol, G. et al. How sacral nerve stimulation works in patients with faecal incontinence. Colorectal Dis. 13, e203–e211 (2011).
Jarrett, M. E. et al. Systematic review of sacral nerve stimulation for faecal incontinence and constipation. Br. J. Surg. 91, 1559–1569 (2004).
Leroi, A. M. et al. Efficacy of sacral nerve stimulation for fecal incontinence: results of a multicenter double-blind crossover study. Ann. Surg. 242, 662–669 (2005).
Tjandra, J. J., Chan, M. K., Yeh, C. H. & Murray-Green, C. Sacral nerve stimulation is more effective than optimal medical therapy for severe fecal incontinence: a randomized, controlled study. Dis. Colon Rectum 51, 494–502 (2008).
Chan, M. K. & Tjandra, J. J. Sacral nerve stimulation for fecal incontinence: external anal sphincter defect vs. intact anal sphincter. Dis. Colon Rectum 51, 1015–1024 (2008).
Mellgren, A. et al. Long-term efficacy and safety of sacral nerve stimulation for fecal incontinence. Dis. Colon Rectum 54, 1065–1075 (2011).
Uludag, O. et al. Sacral neuromodulation: long-term outcome and quality of life in patients with faecal incontinence. Colorectal Dis. 13, 1162–1166 (2011).
Shafik, A., Ahmed, I., El-Sibai, O. & Mostafa, R. M. Percutaneous peripheral neuromodulation in the treatment of fecal incontinence. Eur. Surg. Res. 35, 103–107 (2003).
Queralto, M. et al. Preliminary results of peripheral transcutaneous neuromodulation in the treatment of idiopathic fecal incontinence. Int. J. Colorectal Dis. 21, 670–672 (2006).
Vitton, V., Damon, H., Roman, S. & Mion, F. Transcutaneous electrical posterior tibial nerve stimulation for faecal incontinence: effects on symptoms and quality of life. Int. J. Colorectal Dis. 25, 1017–1020 (2010).
Eleouet, M. et al. Chronic posterior tibial nerve transcutaneous electrical nerve stimulation (TENS) to treat fecal incontinence (FI). Int. J. Colorectal Dis. 25, 1127–1132 (2010).
Leroi, A. M. et al. Transcutaneous electrical tibial nerve stimulation in the treatment of fecal incontinence: a randomized trial (CONSORT 1a). Am. J. Gastroenterol. 107, 1888–1896 (2012).
Mentes, B. B. et al. Posterior tibial nerve stimulation for faecal incontinence after partial spinal injury: preliminary report. Tech. Coloproctol. 11, 115–119 (2007).
de la Portilla, F. et al. Evaluation of the use of posterior tibial nerve stimulation for the treatment of fecal incontinence: preliminary results of a prospective study. Dis. Colon Rectum 52, 1427–1433 (2009).
Govaert, B. et al. A prospective multicentre study to investigate percutaneous tibial nerve stimulation for the treatment of faecal incontinence. Colorectal Dis. 12, 1236–1241 (2010).
Boyle, D. J., Prosser, K., Allison, M. E., Williams, N. S. & Chan, C. L. Percutaneous tibial nerve stimulation for the treatment of urge fecal incontinence. Dis. Colon Rectum 53, 432–437 (2010).
Findlay, J. M., Yeung, J. M., Robinson, R., Greaves, H. & Maxwell-Armstrong, C. Peripheral neuromodulation via posterior tibial nerve stimulation—a potential treatment for faecal incontinence? Ann. R. Coll. Surg. Engl. 92, 385–390 (2010).
Allison, M. Percutaneous tibial nerve stimulation for patients with faecal incontinence. Nurs. Stand. 25, 44–48 (2011).
Hotouras, A. et al. Short-term outcome following percutaneous tibial nerve stimulation for faecal incontinence: a single-centre prospective study. Colorectal Dis. 14, 1101–1105 (2012).
George, A. T. et al. A prospective single blinded placebo controlled study into the role of percutaneous and transcutaneous for the treatment of faecal incontinence. Colorectal Dis. 54 (Suppl. 4), 1–14 (2011).
Jorge, J. M. & Wexner, S. D. Etiology and management of fecal incontinence. Dis. Colon Rectum 36, 77–97 (1993).
Knowles, C. H. Protocol 11PRT/4126: Control of faecal incontinence using distal neuromodulation—CONFIDeNT Trial: a phase III clinical trial (ISRCTN8855947). The Lancet [online].
Chetwood, C. H. Plastic operation of the sphincter ani with report of a case. Med. Rec. 61, 529 (1902).
Hultman, C. S., Zenn, M. R., Agarwal, T. & Baker, C. C. Restoration of fecal continence after functional gluteoplasty: long-term results, technical refinements, and donor-site morbidity. Ann. Plast. Surg. 56, 65–70 (2006).
Baeten, C., Spaans, F. & Fluks, A. An implanted neuromuscular stimulator for fecal continence following previously implanted gracilis muscle. Report of a case. Dis. Colon Rectum 31, 134–137 (1988).
Williams, N. S., Patel, J., George, B. D., Hallan, R. I. & Watkins, E. S. Development of an electrically stimulated neoanal sphincter. Lancet 338, 1166–1169 (1991).
Belyaev, O., Muller, C. & Uhl, W. Neosphincter surgery for fecal incontinence: a critical and unbiased review of the relevant literature. Surg. Today 36, 295–303 (2006).
Rongen, M. J. et al. Long-term follow-up of dynamic graciloplasty for fecal incontinence. Dis. Colon Rectum 46, 716–721 (2003).
Penninckx, F. Belgian experience with dynamic graciloplasty for faecal incontinence. Br. J. Surg. 91, 872–878 (2004).
Baeten, C. G. et al. Safety and efficacy of dynamic graciloplasty for fecal incontinence: report of a prospective, multicenter trial. Dynamic Graciloplasty Therapy Study Group. Dis. Colon Rectum 43, 743–751 (2000).
Christiansen, J. & Lorentzen, M. Implantation of artificial sphincter for anal incontinence. Lancet 2, 244–245 (1987).
Wong, W. D. et al. The safety and efficacy of the artificial bowel sphincter for fecal incontinence: results from a multicenter cohort study. Dis. Colon Rectum 45, 1139–1153 (2002).
Wexner, S. D., Jin, H. Y., Weiss, E. G., Nogueras, J. J. & Li, V. K. Factors associated with failure of the artificial bowel sphincter: a study of over 50 cases from Cleveland Clinic Florida. Dis. Colon Rectum 52, 1550–1557 (2009).
O'Brien, P. E. et al. A prospective, randomized, controlled clinical trial of placement of the artificial bowel sphincter (Acticon Neosphincter) for the control of fecal incontinence. Dis. Colon Rectum 47, 1852–1860 (2004).
Schrag, H. J. et al. German artificial sphincter system: first report of a novel and highly integrated sphincter prosthesis for therapy of major fecal incontinence. Dis. Colon Rectum 47, 2215–2217 (2004).
Finlay, I. G., Richardson, W. & Hajivassiliou, C. A. Outcome after implantation of a novel prosthetic anal sphincter in humans. Br. J. Surg. 91, 1485–1492 (2004).
Lehur, P. A. et al. Magnetic anal sphincter augmentation for the treatment of fecal incontinence: a preliminary report from a feasibility study. Dis. Colon Rectum 53, 1604–1610 (2010).
Wong, M. T., Meurette, G., Stangherlin, P. & Lehur, P. A. The magnetic anal sphincter versus the artificial bowel sphincter: a comparison of 2 treatments for fecal incontinence. Dis. Colon Rectum 54, 773–779 (2011).
Wong, M. T., Meurette, G., Wyart, V. & Lehur, P. A. Does the magnetic anal sphincter device compare favourably with sacral nerve stimulation in the management of faecal incontinence? Colorectal Dis. 14, e323–e329 (2012).
Mercer-Jones, M. in Pelvic Floor Disorders for the Colorectal Surgeon (eds Lindsey, I., Nugent, K. & Dixon, T.) 237–250 (Oxford University Press, 2010).
Luo, C., Samaranayake, C. B., Plank, L. D. & Bissett, I. P. Systematic review on the efficacy and safety of injectable bulking agents for passive faecal incontinence. Colorectal Dis. 12, 296–303 (2010).
Maeda, Y., Laurberg, S. & Norton, C. Perianal injectable bulking agents as treatment for faecal incontinence in adults. Cochrane Database of Systematic Reviews Issue 2. Art. no.: CD007959 http://dx.doi.org/10.1002/14651858.CD007959.pub3.
Graf, W. et al. Efficacy of dextranomer in stabilised hyaluronic acid for treatment of faecal incontinence: a randomised, sham-controlled trial. Lancet 377, 997–1003 (2011).
Tjandra, J. J., Lim, J. F., Hiscock, R. & Rajendra, P. Injectable silicone biomaterial for fecal incontinence caused by internal anal sphincter dysfunction is effective. Dis. Colon Rectum 47, 2138–2146 (2004).
Maslekar, S., Smith, K., Harji, D., Griffiths, B. & Sagar, P. M. Injectable collagen for the treatment of fecal incontinence: long-term results. Dis. Colon Rectum 56, 354–359 (2013).
Smaldone, M. C. & Chancellor, M. B. Muscle derived stem cell therapy for stress urinary incontinence. World J. Urol. 26, 327–332 (2008).
Kajbafzadeh, A. M., Elmi, A., Talab, S. S., Esfahani, S. A. & Tourchi, A. Functional external anal sphincter reconstruction for treatment of anal incontinence using muscle progenitor cell auto grafting. Dis. Colon Rectum 53, 1415–1421 (2010).
Kang, S. B. et al. Sphincter contractility after muscle-derived stem cells autograft into the cryoinjured anal sphincters of rats. Dis. Colon Rectum 51, 1367–1373 (2008).
Frudinger, A. et al. Muscle-derived cell injection to treat anal incontinence due to obstetric trauma: pilot study with 1 year follow-up. Gut 59, 55–61 (2010).
Romaniszyn, M. et al. Successful implantation of autologous muscle-derived stem cells in treatment of faecal incontinence due to external sphincter rupture. Int. J. Colorectal Dis. 28, 1035–1036 (2013).
Takahashi, T. et al. Radio-frequency energy delivery to the anal canal for the treatemnt of fecal incontinence. Dis. Colon Rectum 45, 915–922 (2002).
Takahashi-Monroy, T. et al. SECCA procedure for the treatment of fecal incontinence: results of five-year follow-up. Dis. Colon Rectum 51, 355–359 (2008).
Malone, P. S., Ransley, P. G. & Kiely, E. M. Preliminary report: the antegrade continence enema. Lancet 336, 1217–1218 (1990).
Poirier, M., Abcarian, H. & Nelson, R. Malone antegrade continent enema: an alternative to resection in severe defecation disorders. Dis. Colon Rectum 50, 22–28 (2007).
Worsøe, J., Christensen, P., Krogh, K., Buntzen, S. & Laurberg, S. Long-term results of antegrade colonic enema in adult patients: assessment of functional results. Dis. Colon Rectum 51, 1523–1528 (2008).
Thomas, G. P., Dudding, T. C., Rahbour, G., Nicholls, R. J. & Vaizey, C. J. A review of posterior tibial nerve stimulation for faecal incontinence. Colorectal Dis. 15, 519–526 (2013).
Chapman, A. E. et al. Systematic review of dynamic graciloplasty in the treatment of faecal incontinence. Br. J. Surg. 89, 138–153 (2002).
Author information
Authors and Affiliations
Contributions
Both authors contributed to all aspects of this manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Rights and permissions
About this article
Cite this article
Mitchell, P., Sagar, P. Emerging surgical therapies for faecal incontinence. Nat Rev Gastroenterol Hepatol 11, 279–286 (2014). https://doi.org/10.1038/nrgastro.2013.220
Published:
Issue Date:
DOI: https://doi.org/10.1038/nrgastro.2013.220
This article is cited by
-
Management of functional constipation in children and adults
Nature Reviews Gastroenterology & Hepatology (2020)
-
Exhausted implanted pulse generator in sacral nerve stimulation for faecal incontinence: What next in daily practice for patients?
International Journal of Colorectal Disease (2016)
-
Pregnancy and Postpartum Bowel Changes: Constipation and Fecal Incontinence
American Journal of Gastroenterology (2015)
-
Implantation of autologous muscle-derived stem cells in treatment of fecal incontinence: results of an experimental pilot study
Techniques in Coloproctology (2015)